Non-Small-Cell Lung Cancer?
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Successful Chemotherapy Is Possible for Seemingly Inoperable Anaplastic Thyroid Cancer
® Clinical Thyroidology for the Public VOLUME 12 | ISSUE 12 | DECEMBER 2019 THYROID CANCER Successful chemotherapy is possible for seemingly inoperable anaplastic thyroid cancer BACKGROUND form of standard chemotherapy and 2 received another While the vast majority of thyroid cancers are slow tyrosine kinase inhibitor called pembrolizumab. Of the 6 growing and have an excellent prognosis, anaplastic patients that had surgery after this treatment, 4 patients thyroid cancer, which makes up <1% of all thyroid cancer, had the entire primary cancer removed and the other 2 is one of the most aggressive of all cancers, with a survival patients only had microscopic pieces of cancer left after averaging ~6 months after diagnosis. Surgery, radiation the surgery. After the surgery, 5 of 6 patients received and single drug chemotherapy is all ineffective in most standard chemotherapy and radiation to the surgical area. cases. The aim of this study is to study if combination Of the 6 patients, 4 patients had no evidence of cancer at chemotherapy will make previously inoperable anaplastic the last check, some over 2 years after surgery. The 2 other thyroid cancers safe to remove with surgery. patients did pass away from anaplastic cancer; however, there was no re-growth of cancer in the area where surgery THE FULL ARTICLE TITLE occurred. Wang JR et al 2019 Complete surgical resection following neoadjuvant dabrafenib plus trametinib in BRAFV600E- WHAT ARE THE IMPLICATIONS mutated anaplastic thyroid carcinoma. Thyroid 29:1036– OF THIS STUDY? 1043. PMID: 31319771. In selected patients with anaplastic thyroid cancer with the BRAF V600E mutation, treatment with dabrafenib SUMMARY OF THE STUDY and trametinib may increase the chance of having a In this study from the MD Anderson Cancer Center successful surgery of the primary tumor. -

Combined BRAF and MEK Inhibition with Vemurafenib and Cobimetinib for Patients with Advanced Melanoma
Review Melanoma Combined BRAF and MEK Inhibition with Vemurafenib and Cobimetinib for Patients with Advanced Melanoma Antonio M Grimaldi, Ester Simeone, Lucia Festino, Vito Vanella and Paolo A Ascierto Melanoma, Cancer Immunotherapy and Innovative Therapy Unit, Istituto Nazionale Tumori Fondazione “G. Pascale”, Napoli, Italy cquired resistance is the most common cause of BRAF inhibitor monotherapy treatment failure, with the majority of patients experiencing disease progression with a median progression-free survival of 6-8 months. As such, there has been considerable A focus on combined therapy with dual BRAF and MEK inhibition as a means to improve outcomes compared with monotherapy. In the COMBI-d and COMBI-v trials, combined dabrafenib and trametinib was associated with significant improvements in outcomes compared with dabrafenib or vemurafenib monotherapy, in patients with BRAF-mutant metastatic melanoma. The combination of vemurafenib and cobimetinib has also been investigated. In the phase III CoBRIM study in patients with unresectable stage III-IV BRAF-mutant melanoma, treatment with vemurafenib and cobimetinib resulted in significantly longer progression-free survival and overall survival (OS) compared with vemurafenib alone. One-year OS was 74.5% in the vemurafenib and cobimetinib group and 63.8% in the vemurafenib group, while 2-year OS rates were 48.3% and 38.0%, respectively. The combination was also well tolerated, with a lower incidence of cutaneous squamous-cell carcinoma and keratoacanthoma compared with monotherapy. Dual inhibition of both MEK and BRAF appears to provide a more potent and durable anti-tumour effect than BRAF monotherapy, helping to prevent acquired resistance as well as decreasing adverse events related to BRAF inhibitor-induced activation of the MAPK-pathway. -

Oncology 101 Dictionary
ONCOLOGY 101 DICTIONARY ACUTE: Symptoms or signs that begin and worsen quickly; not chronic. Example: James experienced acute vomiting after receiving his cancer treatments. ADENOCARCINOMA: Cancer that begins in glandular (secretory) cells. Glandular cells are found in tissue that lines certain internal organs and makes and releases substances in the body, such as mucus, digestive juices, or other fluids. Most cancers of the breast, pancreas, lung, prostate, and colon are adenocarcinomas. Example: The vast majority of rectal cancers are adenocarcinomas. ADENOMA: A tumor that is not cancer. It starts in gland-like cells of the epithelial tissue (thin layer of tissue that covers organs, glands, and other structures within the body). Example: Liver adenomas are rare but can be a cause of abdominal pain. ADJUVANT: Additional cancer treatment given after the primary treatment to lower the risk that the cancer will come back. Adjuvant therapy may include chemotherapy, radiation therapy, hormone therapy, targeted therapy, or biological therapy. Example: The decision to use adjuvant therapy often depends on cancer staging at diagnosis and risk factors of recurrence. BENIGN: Not cancerous. Benign tumors may grow larger but do not spread to other parts of the body. Also called nonmalignant. Example: Mary was relieved when her doctor said the mole on her skin was benign and did not require any further intervention. BIOMARKER TESTING: A group of tests that may be ordered to look for genetic alterations for which there are specific therapies available. The test results may identify certain cancer cells that can be treated with targeted therapies. May also be referred to as genetic testing, molecular testing, molecular profiling, or mutation testing. -

Original Research Paper In-Silico FDA-Approved Drug Repurposing to Find
Original Research Paper In-silico FDA-approved drug repurposing to find the possible treatment of Coronavirus Disease-19 (COVID-19) Kumar Sharp1, Dr. Shubhangi Dange2* 12nd MBBS undergraduate student, Government Medical College and Hospital, Jalgaon 2Associate Professor, Dept. of Microbiology, Government Medical College and Hospital, Jalgaon *Corresponding author: - Dr. Shubhangi Dange, Associate Professor, Department of Microbiology, Government Medical College and Hospital, Jalgaon Email: [email protected] Abstract Identification of potential drug-target interaction for approved drugs serves as the basis of repurposing drugs. Studies have shown polypharmacology as common phenomenon. In-silico approaches help in screening large compound libraries at once which could take years in a laboratory. We screened a library of 1050 FDA-approved drugs against spike glycoprotein of SARS-CoV2 in-silico. Anti-cancer drugs have shown good binding affinity which is much better than hydroxychloroquine and arbidol. We have also introduced a hypothesis named “Bump” hypothesis which and be developed further in field of computational biology. Keywords: spike glycoprotein; FDA; drug repurposing; anti-cancer; hydroxychloroquine Introduction Identification of potential drug-target interaction for approved drugs serves as the basis of repurposing drugs. Studies have shown polypharmacology as common phenomenon [1][2]. Since the three-dimensional structures of proteins of SARS-CoV2 have been mapped it opens opportunity for in-silico approaches of either novel drug discovery or drug repurposing. In the absence of an exact cure or vaccine, coronavirus disease-19 has taken a huge toll of humanity. Our study of target specific drug docking and novel hypothesis contributes in this fight. In-silico approaches help in screening large compound libraries at once which could take years in a laboratory. -

Tafinlar, INN-Dabrafenib
ANNEX I SUMMARY OF PRODUCT CHARACTERISTICS 1 1. NAME OF THE MEDICINAL PRODUCT Tafinlar 50 mg hard capsules Tafinlar 75 mg hard capsules 2. QUALITATIVE AND QUANTITATIVE COMPOSITION Tafinlar 50 mg hard capsules Each hard capsule contains dabrafenib mesilate equivalent to 50 mg of dabrafenib. Tafinlar 75 mg hard capsules Each hard capsule contains dabrafenib mesilate equivalent to 75 mg of dabrafenib. For the full list of excipients, see section 6.1. 3. PHARMACEUTICAL FORM Hard capsule (capsule). Tafinlar 50 mg hard capsules Opaque dark red capsules, approximately 18 mm long, with capsule shell imprinted with “GS TEW” and “50 mg”. Tafinlar 75 mg hard capsules Opaque dark pink capsules, approximately 19 mm long, with capsule shell imprinted with “GS LHF” and “75 mg”. 4. CLINICAL PARTICULARS 4.1 Therapeutic indications Melanoma Dabrafenib as monotherapy or in combination with trametinib is indicated for the treatment of adult patients with unresectable or metastatic melanoma with a BRAF V600 mutation (see sections 4.4 and 5.1). Adjuvant treatment of melanoma Dabrafenib in combination with trametinib is indicated for the adjuvant treatment of adult patients with Stage III melanoma with a BRAF V600 mutation, following complete resection. Non-small cell lung cancer (NSCLC) Dabrafenib in combination with trametinib is indicated for the treatment of adult patients with advanced non-small cell lung cancer with a BRAF V600 mutation. 2 4.2 Posology and method of administration Treatment with dabrafenib should be initiated and supervised by a qualified physician experienced in the use of anticancer medicinal products. Before taking dabrafenib, patients must have confirmation of tumour BRAF V600 mutation using a validated test. -

Lung Cancer 2020 Fact Sheet
Lung Cancer 2020 Fact Sheet Lung cancer: the most fatal cancer • The most frequently diagnosed cancer is lung cancer (11.6 percent), followed by female breast (11.6 percent) and colorectal cancers (10.2 percent). • Worldwide lung cancer incidents are on track to increase by 38 percent to 2.89 million by 2030. • Lung cancer is the leading cause of death from cancer at 1.74 million (18.4 percent), followed by colorectal (9.2 percent) and stomach cancers (8.2 percent). • Lung cancer deaths exceed breast cancer mortality for women in 28 countries. • Lung cancer mortality is projected to reach 2.45 million worldwide by 2030, a 39 percent increase since 2018. • About 80 percent of lung cancer deaths are as a result of smoking tobacco. Smokers exposed to other known risk factors such as radon and asbestos are at an even higher risk. • For men, lung cancer is the most prevalent form of cancer, it is third for women. • The five-year cancer survival rate in middle-income countries for all types of lung cancer (19 percent) is lower than many other leading cancer sites, such as the colon (71 percent), breast (85 percent) and prostate (98.9 percent). Treating lung cancer • In lower-income countries, access to care and cost-effective treatments can reduce the human burden and societal impact of lung cancer. • Screening with CT scans compared with chest radiography resulted in a 20 percent reduction in lung cancer-specific deaths, but much cheaper and more accessible methods are needed for low-income settings. • Early-stage lung cancer is treated with curative-intent surgery or radiation therapy. -

Epidemiology and Clinical Aspects of Malignant Pleural Mesothelioma
cancers Review Epidemiology and Clinical Aspects of Malignant Pleural Mesothelioma Fraser Brims 1,2,3 1 Curtin Medical School, Curtin University, Perth, WA 6845, Australia; [email protected] 2 Department of Respiratory Medicine, Sir Charles Gairdner Hospital, Perth, WA 6009, Australia 3 National Centre for Asbestos Related Diseases, Institute for Respiratory Health, Perth, WA 6009, Australia Simple Summary: Mesothelioma is a cancer of the lining of the lungs caused by breathing in asbestos fibres. Asbestos was widely used in industry in the last century in most developed countries and is still present in many older buildings to this day. There is no known safe level of asbestos exposure. Symptoms of mesothelioma can include worsening breathlessness, chest pain and loss of weight. There is no cure, and the treatment of mesothelioma is limited, although there have been some recent improvements in therapy. Survival is very variable although most people live for around one year after diagnosis. Efforts to improve and maintain the quality of life for patients with mesothelioma remain a priority. Abstract: Mesothelioma is a cancer predominantly of the pleural cavity. There is a clear association of exposure to asbestos with a dose dependent risk of mesothelioma. The incidence of mesothelioma in different countries reflect the historical patterns of commercial asbestos utilisation in the last century and predominant occupational exposures mean that mesothelioma is mostly seen in males. Modern imaging techniques and advances in immunohistochemical staining have contributed to an improved diagnosis of mesothelioma. There have also been recent advances in immune checkpoint inhibition, however, mesothelioma remains very challenging to manage, especially Citation: Brims, F. -

Oncology Drug Shortage Update
] ] [ News ] Analysis ] Commentary ] Controversy ] June 25, 2013 Vol. 35 No. 12 oncology-times.com ONCOLOGY e 5 Y ars 3 of g P in u t b a l r i s b h e i l n e g IMES C 35 TThe Independent Hem/Onc News Source Oncology Drug Shortage Update BY HEATHER LINDSEY new survey documents that cancer drug shortages have occurred A frequently, led to treatment delays, increased the risks of errors and adverse outcomes, complicated research, and increased the costs of medications� The survey, by the Hematology-Oncology Pharmacy Association, is the first to focus specifically on oncology� Page 14 • Advanced NSCLC: 60 Gy Standard • Seminoma: Opting Out of Adjuvant Therapy Safe LUNG CANCER: • Immunotherapy ‘Poised to Change Treatment Paradigm’ Leukemia Researcher Lukas Meeting Spotlights • DLBCL: CT Surveillance Adds Little Value Wartman Describes 10-Year Progress in Molecularly • CLL: Enthusiasm for Idelalisb Personal Battle Against Guided Therapy p.10 • Fitness & Cancer Prognosis pp.18, 25, 28, 33, 36, 37 Adult ALL p.20 [ALSO] SHOP TALK �� � � � � � � � � � � � � � � � � � � � � � � � � � � � � � � � � � � � � � � � � � � � �3 EDITH PEREZ: How I Treat Patients with Advanced HER2-Positive Breast Cancer � � � � � � � � � � �5 Exercise, Estrogen, & Breast Cancer Risk: New Data �� � � � � � � � � � � � � � � � � � � � � � � � � � � � � � � � � �11 JOE SIMONE: Changing Views of Leaders and Leadership � � � � � � � � � � � � � � � � � � � � � � � � � � � � �16 Science Symposium for ACS’s 100th Anniversary �� � � � � � � � � � � � � � � � � � � � � � � � -

MEKINIST (Trametinib) Tablets for Oral Use Are Supplied As 0.5 Mg and 2 Mg Tablets for Oral Administration
HIGHLIGHTS OF PRESCRIBING INFORMATION Colitis and Gastrointestinal Perforation: Colitis and gastrointestinal These highlights do not include all the information needed to use perforation can occur in patients receiving MEKINIST. (5.3) MEKINIST safely and effectively. See full prescribing information for Venous Thromboembolism: Deep vein thrombosis and pulmonary MEKINIST. embolism can occur in patients receiving MEKINIST. (5.4, 2.7) MEKINIST® (trametinib) tablets, for oral use Cardiomyopathy: Assess LVEF before treatment, after one month of Initial U.S. Approval: 2013 treatment, then every 2 to 3 months thereafter. (5.5, 2.7) ------------------------------RECENT MAJOR CHANGES------------------------ Ocular Toxicities: Perform ophthalmologic evaluation for any visual Indications and Usage (1.1-1.3) 4/2018 disturbances. For Retinal Vein Occlusion (RVO), permanently Indications and Usage (1.4, 1.5) 5/2018 discontinue MEKINIST. (5.6, 2.7) Dosage and Administration Interstitial Lung disease (ILD): Withhold MEKINIST for new or (2.2, 2.3, 2.4) 4/2018 progressive unexplained pulmonary symptoms. Permanently discontinue (2.1, 2.5, 2.6, 2.7) 5/2018 MEKINIST for treatment-related ILD or pneumonitis. (5.7, 2.7) Warnings and Precautions (5) 4/2018 Serious Febrile Reactions: Can occur when MEKINIST is used with dabrafenib. (5.8, 2.7) ------------------------------INDICATIONS AND USAGE------------------------- Serious Skin Toxicity: Monitor for skin toxicities and for secondary MEKINIST is a kinase inhibitor indicated as a single agent for the treatment infections. Discontinue MEKINIST for intolerable Grade 2, or Grade 3 of patients with unresectable or metastatic melanoma with BRAF V600E or or 4 rash not improving within 3 weeks despite interruption of V600K mutations as detected by an FDA-approved test. -

First-Line Treatment Options for Patients with Stage IV Non-Small Cell Lung Cancer with Driver Alterations
First-Line Treatment Options for Patients with Stage IV Non-Small Cell Lung Cancer with Driver Alterations Patients with stage IV non-small cell lung cancer Nonsquamous cell carcinoma and squamous cell carcinoma Activating EGFR mutation other Sensitizing (L858R/exon 19 MET exon 14 skipping than exon 20 insertion mutations, EGFR exon 20 mutation ALK rearrangement ROS1 rearrangement BRAF V600E mutation RET rearrangement NTRK rearrangement mutations KRAS alterations HER2 alterations NRG1 alterations deletion) EGFR mutation T790M, L858R or Ex19Del PS 0-2 Treatment Options PS 0-2 Treatment Options PS 0-2 Treatment Options PS 0-2 Treatment Options PS 0-2 Treatment Options Treatment Options PS 0-2 Treatment Options PS 0-2 Treatment Options PS 0-2 Treatment Options Emerging target; no Emerging target; no Emerging target; no Platinum doublet † † † Osimertinib monotherapy S Afatinib monotherapy M M Alectinib S Entrectinib M Dabrafenib/trametinib M Capmatinib M Selpercatinib M Entrectinib M conclusions available conclusions available conclusions available chemotherapy ± bevacizumab Gefitinib with doublet Standard treatment based on Standard treatment based on Standard treatment based on M M M Brigatinib S Crizotinib M M Tepotinib M Pralsetinib* W Larotrectinib M chemotherapy non-driver mutation guideline non-driver mutation guideline non-driver mutation guideline If alectinib or brigatinib are not available If entrectinib or crizotinib are not available Standard treatment based on Standard treatment based on Standard treatment based on Dacomitinib monotherapy M Osimertinib W M M M Ceritinib S Ceritinib W non-driver mutation guideline non-driver mutation guideline non-driver mutation guideline Monotherapy with afatinib M Crizotinib S Lortlatinib W Standard treatment based on Erlotinib/ramucirumab M M non-driver mutation guideline Erlotinib/bevacizumab M Monotherapy with erlotinib M Strength of Recommendation Monotherapy with gefitinib M S Strong M Moderate W Weak Monotherapy with icotinib M Notes. -
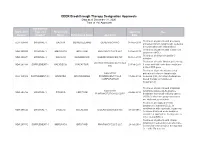
CDER Breakthrough Therapy Designation Approvals Data As of December 31, 2020 Total of 190 Approvals
CDER Breakthrough Therapy Designation Approvals Data as of December 31, 2020 Total of 190 Approvals Submission Application Type and Proprietary Approval Use Number Number Name Established Name Applicant Date Treatment of patients with previously BLA 125486 ORIGINAL-1 GAZYVA OBINUTUZUMAB GENENTECH INC 01-Nov-2013 untreated chronic lymphocytic leukemia in combination with chlorambucil Treatment of patients with mantle cell NDA 205552 ORIGINAL-1 IMBRUVICA IBRUTINIB PHARMACYCLICS LLC 13-Nov-2013 lymphoma (MCL) Treatment of chronic hepatitis C NDA 204671 ORIGINAL-1 SOVALDI SOFOSBUVIR GILEAD SCIENCES INC 06-Dec-2013 infection Treatment of cystic fibrosis patients age VERTEX PHARMACEUTICALS NDA 203188 SUPPLEMENT-4 KALYDECO IVACAFTOR 21-Feb-2014 6 years and older who have mutations INC in the CFTR gene Treatment of previously untreated NOVARTIS patients with chronic lymphocytic BLA 125326 SUPPLEMENT-60 ARZERRA OFATUMUMAB PHARMACEUTICALS 17-Apr-2014 leukemia (CLL) for whom fludarabine- CORPORATION based therapy is considered inappropriate Treatment of patients with anaplastic NOVARTIS lymphoma kinase (ALK)-positive NDA 205755 ORIGINAL-1 ZYKADIA CERITINIB 29-Apr-2014 PHARMACEUTICALS CORP metastatic non-small cell lung cancer (NSCLC) who have progressed on or are intolerant to crizotinib Treatment of relapsed chronic lymphocytic leukemia (CLL), in combination with rituximab, in patients NDA 206545 ORIGINAL-1 ZYDELIG IDELALISIB GILEAD SCIENCES INC 23-Jul-2014 for whom rituximab alone would be considered appropriate therapy due to other co-morbidities -

MAP Kinase Signaling and Inhibition in Melanoma
Oncogene (2013) 32, 2373–2379 & 2013 Macmillan Publishers Limited All rights reserved 0950-9232/13 www.nature.com/onc REVIEW MAP kinase signaling and inhibition in melanoma RJ Sullivan and K Flaherty The mitogen-activated protein kinase (MAPK) pathway is critical to oncogenic signaling in the majority of patients with malignant melanoma. Driver mutations in both NRAS and BRAF have important implications for prognosis and treatment. The development of inhibitors to mediators of the MAPK pathway, including those to CRAF, BRAF, and MEK, has led to major advances in the treatment of patients with melanoma. In particular, the selective BRAF inhibitor vemurafenib has been shown to improve overall survival in patients with tumors harboring BRAF mutations. However, the duration of benefit is limited in many patients and highlights the need for understanding the limitations of therapy in order to devise more effective strategies. MEK inhibitors have proven to particularly active in BRAF mutant melanomas also. Emerging knowledge about mechanisms of resistance as well as a more complete understanding of the biology of MAPK pathway signaling provides insight into rational combination regimens and sequences of molecularly targeted therapies. Oncogene (2013) 32, 2373–2379; doi:10.1038/onc.2012.345; published online 3 September 2012 Keywords: melanoma; targeted therapy; BRAF INTRODUCTION activation. The RAS GTPases are a critical link between activated The mitogen-activated protein kinase (MAPK) pathway is activated growth factor receptors and downstream signal transduction in the great majority of melanomas and typically occurs through pathways. In light of this central role, it is not surprising that three activating mutations of either NRAS (15–20% cutaneous melano- RAS isoforms (HRAS, KRAS and NRAS) collectively represent the mas) or BRAF (40–50%).1 These mutations can be identified in most commonly mutated oncogene in human malignancies and 13,14 benign melanocytic proliferation and all stages of invasive and distribute across a variety of cancers.