Spinal Cord, Spinal Nerves, and Somatic Reflexes
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

NS201C Anatomy 1: Sensory and Motor Systems
NS201C Anatomy 1: Sensory and Motor Systems 25th January 2017 Peter Ohara Department of Anatomy [email protected] The Subdivisions and Components of the Central Nervous System Axes and Anatomical Planes of Sections of the Human and Rat Brain Development of the neural tube 1 Dorsal and ventral cell groups Dermatomes and myotomes Neural crest derivatives: 1 Neural crest derivatives: 2 Development of the neural tube 2 Timing of development of the neural tube and its derivatives Timing of development of the neural tube and its derivatives Gestational Crown-rump Structure(s) age (Weeks) length (mm) 3 3 cerebral vesicles 4 4 Optic cup, otic placode (future internal ear) 5 6 cerebral vesicles, cranial nerve nuclei 6 12 Cranial and cervical flexures, rhombic lips (future cerebellum) 7 17 Thalamus, hypothalamus, internal capsule, basal ganglia Hippocampus, fornix, olfactory bulb, longitudinal fissure that 8 30 separates the hemispheres 10 53 First callosal fibers cross the midline, early cerebellum 12 80 Major expansion of the cerebral cortex 16 134 Olfactory connections established 20 185 Gyral and sulcul patterns of the cerebral cortex established Clinical case A 68 year old woman with hypertension and diabetes develops abrupt onset numbness and tingling on the right half of the face and head and the entire right hemitrunk, right arm and right leg. She does not experience any weakness or incoordination. Physical Examination: Vitals: T 37.0° C; BP 168/87; P 86; RR 16 Cardiovascular, pulmonary, and abdominal exam are within normal limits. Neurological Examination: Mental Status: Alert and oriented x 3, 3/3 recall in 3 minutes, language fluent. -

The Brain Stem Medulla Oblongata
Chapter 14 The Brain Stem Medulla Oblongata Copyright © The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Central sulcus Parietal lobe • embryonic myelencephalon becomes Cingulate gyrus leaves medulla oblongata Corpus callosum Parieto–occipital sulcus Frontal lobe Occipital lobe • begins at foramen magnum of the skull Thalamus Habenula Anterior Epithalamus commissure Pineal gland • extends for about 3 cm rostrally and ends Hypothalamus Posterior commissure at a groove between the medulla and Optic chiasm Mammillary body pons Cerebral aqueduct Pituitary gland Fourth ventricle Temporal lobe • slightly wider than spinal cord Cerebellum Midbrain • pyramids – pair of external ridges on Pons Medulla anterior surface oblongata – resembles side-by-side baseball bats (a) • olive – a prominent bulge lateral to each pyramid • posteriorly, gracile and cuneate fasciculi of the spinal cord continue as two pair of ridges on the medulla • all nerve fibers connecting the brain to the spinal cord pass through the medulla • four pairs of cranial nerves begin or end in medulla - IX, X, XI, XII Medulla Oblongata Associated Functions • cardiac center – adjusts rate and force of heart • vasomotor center – adjusts blood vessel diameter • respiratory centers – control rate and depth of breathing • reflex centers – for coughing, sneezing, gagging, swallowing, vomiting, salivation, sweating, movements of tongue and head Medulla Oblongata Nucleus of hypoglossal nerve Fourth ventricle Gracile nucleus Nucleus of Cuneate nucleus vagus -

Spinal Cord Organization
Lecture 4 Spinal Cord Organization The spinal cord . Afferent tract • connects with spinal nerves, through afferent BRAIN neuron & efferent axons in spinal roots; reflex receptor interneuron • communicates with the brain, by means of cell ascending and descending pathways that body form tracts in spinal white matter; and white matter muscle • gives rise to spinal reflexes, pre-determined gray matter Efferent neuron by interneuronal circuits. Spinal Cord Section Gross anatomy of the spinal cord: The spinal cord is a cylinder of CNS. The spinal cord exhibits subtle cervical and lumbar (lumbosacral) enlargements produced by extra neurons in segments that innervate limbs. The region of spinal cord caudal to the lumbar enlargement is conus medullaris. Caudal to this, a terminal filament of (nonfunctional) glial tissue extends into the tail. terminal filament lumbar enlargement conus medullaris cervical enlargement A spinal cord segment = a portion of spinal cord that spinal ganglion gives rise to a pair (right & left) of spinal nerves. Each spinal dorsal nerve is attached to the spinal cord by means of dorsal and spinal ventral roots composed of rootlets. Spinal segments, spinal root (rootlets) nerve roots, and spinal nerves are all identified numerically by th region, e.g., 6 cervical (C6) spinal segment. ventral Sacral and caudal spinal roots (surrounding the conus root medullaris and terminal filament and streaming caudally to (rootlets) reach corresponding intervertebral foramina) collectively constitute the cauda equina. Both the spinal cord (CNS) and spinal roots (PNS) are enveloped by meninges within the vertebral canal. Spinal nerves (which are formed in intervertebral foramina) are covered by connective tissue (epineurium, perineurium, & endoneurium) rather than meninges. -

The Degenerations Kesulting from Lesions of Posterior
THE DEGENERATIONS KESULTING FROM Downloaded from LESIONS OF POSTERIOR NERVE ROOTS AND FROM TRANSVERSE LESIONS OF THE SPINAL CORD IN MAN. A STUDY OF TWENTY CASES. http://brain.oxfordjournals.org/ BY JAMES COLLIEB, M.D., B.Sc, F.E.C.P. Assistant Physician to the National Hospital, E. FARQUHAR BUZZARD, M.D., M.R.C.P. Pathologist to the National Hospital, and Assistant Physician to the Royal Free Hospital. HAVING held successively the post of pathologist to the at Florida Atlantic University on March 21, 2016 National Hospital we have had the opportunity of examin- ing (1) two cases in which there were isolated lesions of the posterior roots in the cervical or lumbo-sacral region, and (2) twelve cases of transverse lesion of the spinal cord, at various levels. In all of these cases the method of Marchi was applicable. In connection with the descending systems of the pos- terior columns we have also made use of several cases of transverse lesion of the spinal cord, which we have examined by the Weigert-Pal method. For the Marchi method we have invariably used Busch's sodium-iodate process. Inasmuch as the literature of the subject is very extensive, we have deemed it convenient to refer only to the more recent investigations concerning such anatomical and physiological points as have been but lately brought to light, or as are still debatable, and to which our observations may add some further information. A bibliography of the more recent literature upon these subjects is appended. 560 ORIGINAL ARTICLES AND CLINICAL CASES The subject matter of this paper is arranged as follows : — The posterior roots.—(1) The descending intraspinal pro- longations and their relations to the coma tract, to the septo-marginal system, and to other posterior descending systems. -

Brainstem and Its Associated Cranial Nerves
Brainstem and its Associated Cranial Nerves Anatomical and Physiological Review By Sara Alenezy With appreciation to Noura AlTawil’s significant efforts Midbrain (Mesencephalon) External Anatomy of Midbrain 1. Crus Cerebri (Also known as Basis Pedunculi or Cerebral Peduncles): Large column of descending “Upper Motor Neuron” fibers that is responsible for movement coordination, which are: a. Frontopontine fibers b. Corticospinal fibers Ventral Surface c. Corticobulbar fibers d. Temporo-pontine fibers 2. Interpeduncular Fossa: Separates the Crus Cerebri from the middle. 3. Nerve: 3rd Cranial Nerve (Oculomotor) emerges from the Interpeduncular fossa. 1. Superior Colliculus: Involved with visual reflexes. Dorsal Surface 2. Inferior Colliculus: Involved with auditory reflexes. 3. Nerve: 4th Cranial Nerve (Trochlear) emerges caudally to the Inferior Colliculus after decussating in the superior medullary velum. Internal Anatomy of Midbrain 1. Superior Colliculus: Nucleus of grey matter that is associated with the Tectospinal Tract (descending) and the Spinotectal Tract (ascending). a. Tectospinal Pathway: turning the head, neck and eyeballs in response to a visual stimuli.1 Level of b. Spinotectal Pathway: turning the head, neck and eyeballs in response to a cutaneous stimuli.2 Superior 2. Oculomotor Nucleus: Situated in the periaqueductal grey matter. Colliculus 3. Red Nucleus: Red mass3 of grey matter situated centrally in the Tegmentum. Involved in motor control (Rubrospinal Tract). 1. Inferior Colliculus: Nucleus of grey matter that is associated with the Tectospinal Tract (descending) and the Spinotectal Tract (ascending). Tectospinal Pathway: turning the head, neck and eyeballs in response to a auditory stimuli. 2. Trochlear Nucleus: Situated in the periaqueductal grey matter. Level of Inferior 3. -
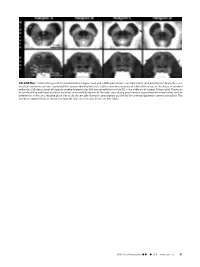
ON-LINE FIG 1. Selected Images of the Caudal Midbrain (Upper Row
ON-LINE FIG 1. Selected images of the caudal midbrain (upper row) and middle pons (lower row) from 4 of 13 total postmortem brains illustrate excellent anatomic contrast reproducibility across individual datasets. Subtle variations are present. Note differences in the shape of cerebral peduncles (24), decussation of superior cerebellar peduncles (25), and spinothalamic tract (12) in the midbrain of subject D (top right). These can be attributed to individual anatomic variation, some mild distortion of the brain stem during procurement at postmortem examination, and/or differences in the axial imaging plane not easily discernable during its prescription parallel to the anterior/posterior commissure plane. The numbers in parentheses in the on-line legends refer to structures in the On-line Table. AJNR Am J Neuroradiol ●:●●2019 www.ajnr.org E1 ON-LINE FIG 3. Demonstration of the dentatorubrothalamic tract within the superior cerebellar peduncle (asterisk) and rostral brain stem. A, Axial caudal midbrain image angled 10° anterosuperior to posteroinferior relative to the ACPC plane demonstrates the tract traveling the midbrain to reach the decussation (25). B, Coronal oblique image that is perpendicular to the long axis of the hippocam- pus (structure not shown) at the level of the ventral superior cerebel- lar decussation shows a component of the dentatorubrothalamic tract arising from the cerebellar dentate nucleus (63), ascending via the superior cerebellar peduncle to the decussation (25), and then enveloping the contralateral red nucleus (3). C, Parasagittal image shows the relatively long anteroposterior dimension of this tract, which becomes less compact and distinct as it ascends toward the thalamus. ON-LINE FIG 2. -

On the Interrnedio-Lateral Tract. Literature
On the Interrnedio-lateral Tract. Literature. The intermedio-;ateral tract was described for the first time "by Lockhart Clarke in the Philosophical Transactions, 1851, P. 613, where he states that "at the outer border of the grey matter, between the anterior and posterior cornua, is to be found a small column of vesicular matter which is softer and more transparent than the rest. According to Clarke's original account, the column in question resembled the substantia gelatinosa of the posterior horn. It was found in the upper part of the lumbar enlargement, extended upwards through the dorsal region, where it distinctly increased in siae, to the lower part of the cervical enlargement. Here it disappeared almost entirely. In the upper cervical enlargement it was again seen, and could be traced upwards into the medulla oblongata, where, in the space immediately behind the central canal, it blended with its fellow of the opposite side. In a second paper, published in 1859, he gave a more complete account of this tract. He here proposed to calx it the "tract,us intermedio-lateralis" on account of its position. Its component cells are described as in part oval, fusiform, pyriform or triangular, smaller' and more uniform in siae than those of the anterior cornu. In the mid-dorsal .region they are least numerous and are found only near the lateral margin of the grey matter^ With the exception of some cells which lie among the white fibres beyond the margin of the grey substance. In the upper dorsal region the tract is larger, not only projecting further outwards into the lateral column of the white fibres, but also tapering inwards across the grey substance, almost to the front of Clarke's coliimn. -
The Nervous System: Sensory and Motor Tracts of the Spinal Cord
15 The Nervous System: Sensory and Motor Tracts of the Spinal Cord PowerPoint® Lecture Presentations prepared by Steven Bassett Southeast Community College Lincoln, Nebraska © 2012 Pearson Education, Inc. Introduction • Millions of sensory neurons are delivering information to the CNS all the time • Millions of motor neurons are causing the body to respond in a variety of ways • Sensory and motor neurons travel by different tracts within the spinal cord © 2012 Pearson Education, Inc. Sensory and Motor Tracts • Communication to and from the brain involves tracts • Ascending tracts are sensory • Deliver information to the brain • Descending tracts are motor • Deliver information to the periphery © 2012 Pearson Education, Inc. Sensory and Motor Tracts • Naming the tracts • If the tract name begins with “spino” (as in spinocerebellar), the tract is a sensory tract delivering information from the spinal cord to the cerebellum (in this case) • If the tract name ends with “spinal” (as in vestibulospinal), the tract is a motor tract that delivers information from the vestibular apparatus (in this case) to the spinal cord © 2012 Pearson Education, Inc. Sensory and Motor Tracts • There are three major sensory tracts • The posterior column tract • The spinothalamic tract • The spinocerebellar tract © 2012 Pearson Education, Inc. Sensory and Motor Tracts • The three major sensory tracts involve chains of neurons • First-order neuron • Delivers sensations to the CNS • The cell body is in the dorsal or cranial root ganglion • Second-order neuron • An interneuron with the cell body in the spinal cord or brain • Third-order neuron • Transmits information from the thalamus to the cerebral cortex © 2012 Pearson Education, Inc. -

Reorganization of Intact Descending Motor Circuits to Replace Lost Connections After Injury
Neurotherapeutics (2016) 13:370–381 DOI 10.1007/s13311-016-0422-x REVIEW Reorganization of Intact Descending Motor Circuits to Replace Lost Connections After Injury Kathren L. Fink1 & William B. J. Cafferty 1 Published online: 3 February 2016 # The Author(s) 2016. This article is published with open access at Springerlink.com Abstract Neurons have a limited capacity to regenerate in the molecular mechanisms that drive plasticity within intact cir- adult central nervous system (CNS). The inability of damaged cuits is crucial in developing novel, potent, and specific ther- axons to re-establish original circuits results in permanent apeutics to restore function after SCI. In this review we dis- functional impairment after spinal cord injury (SCI). Despite cuss the evidence supporting a focus on exploring the capacity abortive regeneration of axotomized CNS neurons, limited of intact motor circuits to functionally repair the damaged spontaneous recovery of motor function emerges after partial CNS after SCI. SCI in humans and experimental rodent models of SCI. It is hypothesized that this spontaneous functional recovery is the result of the reorganization of descending motor pathways Keywords Spinal cord injury . Plasticity . Regeneration . spared by the injury, suggesting that plasticity of intact circuits Repair . Axon . Neuron is a potent alternative conduit to enhance functional recovery after SCI. In support of this hypothesis, several studies have shown that after unilateral corticospinal tract (CST) lesion (unilateral pyramidotomy), -

Cerebral Cortex
Cerebral Cortex • Research on the structure and function of the brain reveals that there are both specialized and diffuse areas of function • Motor and sensory areas are localized in discrete cortical areas called domains • Many higher mental functions such as memory and language appear to have overlapping domains and are more diffusely located • Broadmann areas are areas of localized function Cerebral Cortex - Generalizations • The cerebral cortex has three types of functional areas – Motor areas / control voluntary motor function – Sensory areas / provide conscious awareness of sensation – Association areas / act mainly to integrate diverse information for purposeful action • Each hemisphere is chiefly concerned with the sensory and motor functions of the opposite (contralateral) side of the body Motor Areas • Cortical areas controlling motor functions lie in the posterior part of the frontal lobes • Motor areas include the primary motor cortex, the premotor cortex, Broca’s area, and the front eye field Primary Motor Cortex • The primary motor cortex is located in the precentral gyrus of the frontal lobe of each hemisphere • Large neurons (pyramidal cells) in these gyri allow us to consciously control the precise or skill voluntary movements of our skeletal muscles Pyramidal cells • These long axons, which project to the spinal cord, form the massive Dendrites voluntary motor tracts called the pyramidal, or corticospinal tracts • All other descending motor tracts issue from brain stem nuclei and consists of chains of two, three, or -

Lecture (6) Internal Structures of the Brainstem.Pdf
Internal structures of the Brainstem Neuroanatomy block-Anatomy-Lecture 6 Editing file Objectives At the end of the lecture, students should be able to: ● Distinguish the internal structure of the components of the brain stem in different levels and the specific criteria of each level. 1. Medulla oblongata (closed, mid and open medulla) 2. Pons (caudal and rostral). 3. Midbrain ( superior and inferior colliculi). Color guide ● Only in boys slides in Green ● Only in girls slides in Purple ● important in Red ● Notes in Grey Medulla oblongata Caudal (Closed) Medulla Traversed by the central canal Motor decussation (decussation of the pyramids) ● Formed by pyramidal fibers, (75-90%) cross to the opposite side ● They descend in the lateral white column of the spinal cord as the lateral corticospinal tract. ● The uncrossed fibers form the ventral corticospinal tract Trigeminal sensory nucleus. ● it is the larger sensory nucleus. ● The Nucleus Extends Through the whole length of the brainstem and its note :All CN V afferent sensory information enters continuation of the substantia gelatinosa of the spinal cord. the brainstem through the nerve itself located in the pons. Thus, to reach the spinal nucleus (which ● It lies in all levels of M.O, medial to the spinal tract of the trigeminal. spans the entire brain stem length) in the Caudal ● It receives pain and temperature from face, forehead. Medulla those fibers have to "descend" in what's known as the Spinal Tract of the Trigeminal ● Its tract present in all levels of M.O. is formed of descending (how its sensory and descend?see the note) fibers that terminate in the trigeminal nucleus. -

Fig. 13.1 Copyright © Mcgraw-Hill Education
Fig. 13.1 Copyright © McGraw-Hill Education. Permission required for reproduction or display. C1 Cervical Cervical enlargement spinal nerves C7 Dural sheath Subarachnoid space Thoracic spinal Spinal cord nerves Vertebra (cut) Lumbar Spinal nerve enlargement T12 Spinal nerve rootlets Medullary cone Posterior median sulcus Lumbar Subarachnoid space Cauda equina spinal nerves Epidural space Posterior root ganglion L5 Rib Arachnoid mater Terminal Sacral Dura mater filum spinal nerves S5 Col (b) (a) 1 Fig. 13.2 Copyright © McGraw-Hill Education. Permission required for reproduction or display. Posterior Spinous process of vertebra Meninges: Dura mater (dural sheath) Arachnoid mater Fat in epidural space Pia mater Subarachnoid space Spinal cord Denticulate ligament Posterior root ganglion Spinal nerve Vertebral body (a) Spinal cord and vertebra (cervical) Anterior Posterior Gray matter: Central canal median sulcus White matter: Posterior horn Posterior column Gray commissure Lateral column Lateral horn Anterior column Anterior horn Posterior root of spinal nerve Posterior root ganglion Spinal nerve Anterior median fissure Anterior root of spinal nerve Meninges: Pia mater Arachnoid mater Dura mater (dural sheath) (b) Spinal cord and meninges (thoracic) (c) Lumbar spinal cord c: ©Ed Reschke/Getty Images 2 Table 13.1 3 Fig. 13.4 Copyright © McGraw-Hill Education. Permission required for reproduction or display. Ascending Descending tracts tracts Posterior column: Gracile fasciculus Cuneate fasciculus Anterior corticospinal tract Lateral Posterior spinocerebellar tract corticospinal tract Lateral reticulospinal tract Anterior spinocerebellar tract Tectospinal tract Anterolateral system (containing Medial reticulospinal tract spinothalamic and spinoreticular tracts) Lateral vestibulospinal tract Medial vestibulospinal tract 4 Fig. 13.5 Copyright © McGraw-Hill Education. Permission required for reproduction or display.