Ashton-Manual.Pdf
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

NHS Fife Guidelines for Benzodiazepine Prescribing in Benzodiazepine Dependence
NHS Fife Guidelines for Benzodiazepine Prescribing in Benzodiazepine Dependence Dr. A. Baldacchino, Liz. Hutchings, Addiction Services Issued: April 2013 Review Date: April 2016 1 Approved by NHS Fife ADTC on behalf of NHS Fife Date June 2013 Contents Flowchart for Benzodiazepine Withdrawal ……………………………………………………………3 Establishing type of dependence. ........................................................................................... 4 Assessment of Benzodiazepine Dependence .............................................................................. 5 Management of dependence in therapeutic dose users ........................................................... 6 Management of dependence in prescribed high dose users. ................................................... 7 Management of dependence in illicit and recreational users. .................................................. 8 Psychological support. ................................................................................................................. 9 Pharmacological support............................................................................................................ 10 Appendices Appendix 1 Example Patient Letter (regular user) ................................................. 11 Appendix 2 Information leaflets and advice from the internet ................................ 13 Appendix 3 DRUG DIARY ..................................................................................... 14 Appendix 4 Benzodiazepine conversion table ...................................................... -

The Diagnosis and Management of Benzodiazepine Dependence Heather Ashton
The diagnosis and management of benzodiazepine dependence Heather Ashton Purpose of review Abbreviation Despite repeated recommendations to limit GABA g -aminobutyric acid benzodiazepines to short-term use (2–4 weeks), doctors worldwide are still prescribing them for months or years. # 2005 Lippincott Williams & Wilkins This over-prescribing has resulted in large populations of 0951-7367 long-term users who have become dependent on benzodiazepines and has also led to leakage of benzodiazepines into the illicit drug market. This review Introduction outlines the risks of long-term benzodiazepine use, gives Since their introduction in the 1950s, benzodiazepines guidelines on the management of benzodiazepine appear to have passed their zenith of medical popularity. withdrawal and suggests ways in which dependence can However, they are still prescribed excessively and often be prevented. inappropriately. With their reputation perhaps approach- Recent findings ing a nadir, at least as prescribed medications for Recent literature shows that benzodiazepines have all the long-term use, it is timely to review approaches to the characteristics of drugs of dependence and that they are diagnosis and management of dependence on these inappropriately prescribed for many patients, including drugs. those with physical and psychiatric problems, elderly residents of care homes and those with comorbid alcohol The benzodiazepine bonanza and substance abuse. Many trials have investigated In the late 1970s benzodiazepines became the most methods of benzodiazepine -

The BENZODIAZEPINE TOOLKIT
the BENZODIAZEPINE TOOLKIT By Reconnexion Acknowledgements The 2018 edition of the Beyond Benzodiazepines toolkit has been revised from the 1997 original updated in 2000 and again in 2010. For this version thanks to Erin Oldenhof, James Szeto and Jane Anderson-Wurf. The 2010 version was updated by Tomi Redman and Gwenda Cannard with additional material by Janet Haynes, Jo Marston and Laurence Hennessey. Reconnexion (now a service of EACH) is grateful for the support of ExxonMobil Australia for enabling the revision and update on the 2010 manual. The 1997 original manual was written by Elin Ree and supported by ExxonMobil for which Reconnexion is grateful. Thanks to the Psychotropic Expert Group, Therapeutic Guidelines Limited for permission to use the Comparative Information for Benzodiazepines, Zolpidem and Zopiclone table in Chapter Four. Updates, revisions and feedback retained in the revised version were provided by Therese Barry (Alcohol & Drug Counsellor, Western Region Community Health Centre), Dr Robert Cummins (Deakin University), Hilde Edward (Swinburne University), Lisa Frank (University of Melbourne), Melanie Hands (Project Manager, Drug & Alcohol Clinical Advisory Service, Turning Point Alcohol & Drug Centre), Terrie Hollingsworth (Counsellor, Sunbury Community Health), Dr Peter Johnson (GP), Dr Len Klimans (Chemical Dependency Unit, Royal Women’s Hospital), Dr Nic Lintzeris (Turning Point Alcohol & Drug Centre), Dr Mike McDonough (Consultant, St. Vincent’s Alcohol & Drug Program, Western General Hospital Alcohol & Drug Program), Peter McManus (Secretary, Drug Utilisation Sub Committee, Pharmaceutical Benefits Scheme, Department of Health & Ageing), Dr Robert Moulds (Director, Department of Clinical Pharmacology & Therapeutics, Royal Melbourne Hospital), Jackie Shaw (Manager, Depaul House, St Vincent’s Hospital, Melbourne), Lyn Walker (Manager, CASA House, Royal Women’s Hospital, Melbourne) and Dr Sally Wilkins (North East Melbourne Psychiatric Services, Department of Human Services, Victoria). -

Social Networking and Benzodiazepine Withdrawal: The
Catherine M. Pittman, Ph.D. William Youngs, Ph.D. Elizabeth (Lisa) Karle, MLIS Saint Mary’s College Notre Dame, Indiana ADAA Conference April 5, 2013 No Disclosures. Thank you We would like to begin by expressing our thanks to all those who completed the survey and shared their experiences with us. We also owe a great debt to the founder of BenzoBuddies as well as a skilled technician assistant associated with the group. They provided invaluable advice and assistance, and without their help, the survey would not have been as valid or successful. Finally, we want to thank research assistant Carla Leal for her patient assistance in the creation and coding of the survey. Note: This survey was reviewed and approved by the Institutional Review Board at Saint Mary’s College. When individuals have difficulty with anxiety, what is the most typical response? Often they approach their family doctor, who attempts to treat the anxiety or refers them to a psychiatrist. In either case, it is very likely that a medical (psychopharmalogical) solution may be offered. The solution offered is often benzodiazepines. The United States has the highest rate of benzodiazepine prescription in the world (Rivas- Vazquez, 2003). If the person is prescribed benzodiazepines, short term relief is obtained, but tolerance develops and increasing dosages may be required. Dependence on benzodiazepines is very likely, and how do we help individuals facing benzodiazepine dependence? The truth is we don’t. And this is the reason that Social Networking is important to them. -
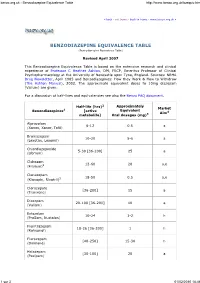
Benzodiazepine Equivalence Table
benzo.org.uk : Benzodiazepine Equivalence Table http://www.benzo.org.uk/bzequiv.htm « back exit frame back to frame www.benzo.org.uk » BENZODIAZEPINE EQUIVALENCE TABLE (Benzodiazepine Equivalency Table) Revised April 2007 This Benzodiazepine Equivalence Table is based on the extensive research and clinical experience of Professor C Heather Ashton , DM, FRCP, Emeritus Professor of Clinical Psychopharmacology at the University of Newcastle upon Tyne, England. Sources: NRHA Drug Newsletter , April 1985 and Benzodiazepines: How they Work & How to Withdraw (The Ashton Manual ), 2002. The approximate equivalent doses to 10mg diazepam (Valium) are given. For a discussion of half-lives and equivalencies see also the Benzo FAQ document . 2 Approximately Half-life (hrs) Market Benzodiazepines 1 [active Equivalent Aim4 metabolite] Oral dosages (mg) 3 Alprazolam 6-12 0.5 a (Xanax, Xanor, Tafil) Bromazepam 10-20 5-6 a (Lexotan, Lexomil) Chlordiazepoxide 5-30 [36-200] 25 a (Librium) Clobazam 12-60 20 a,e (Frisium) 5 Clonazepam 18-50 0.5 a,e (Klonopin, Rivotril) 5 Clorazepate [36-200] 15 a (Tranxene) Diazepam 20-100 [36-200] 10 a (Valium) Estazolam 10-24 1-2 h (ProSom, Nuctalon) Flunitrazepam 18-26 [36-200] 1 h (Rohypnol) Flurazepam [40-250] 15-30 h (Dalmane) Halazepam [30-100] 20 a (Paxipam) 1 sur 3 01/02/2010 18:46 benzo.org.uk : Benzodiazepine Equivalence Table http://www.benzo.org.uk/bzequiv.htm Ketazolam 30-100 [36-200] 15-30 a (Anxon) Loprazolam 6-12 1-2 h (Dormonoct) Lorazepam 10-20 1 a (Ativan, Temesta, Tavor) Lormetazepam 10-12 1-2 h (Noctamid) Medazepam 36-200 10 a (Nobrium) Nitrazepam 15-38 10 h (Mogadon) Nordazepam 36-200 10 a (Nordaz, Calmday) Oxazepam (Serax, Serenid, 4-15 20 a Serepax, Seresta) Prazepam [36-200] 10-20 a (Centrax, Lysanxia) Quazepam (Doral) 25-100 20 h Temazepam (Restoril, Normison, 8-22 20 h Euhypnos) Triazolam 2 0.5 h (Halcion) Non-benzodiazepines with similar effects 1, 6 Zaleplon 2 20 h (Sonata) Zolpidem (Ambien, Stilnoct, 2 20 h Stilnox) Zopiclone 5-6 15 h (Zimovane, Imovane) Eszopiclone 6 3 h (Lunesta) (9 in elderly) 1. -

Pharmacology and Effects of Cannabis: a Brief Review
BRITISH JOURNAL OF PSYCHIATRY $2001), 178, 101^106 Pharmacology and effects of cannabis: Health Organization, 1997; Solowij, 1998). This fact is important since the ef- abriefreview{{ fects of THC are dose-related and most of the research on cannabis was carried out in the 1970s using doses of 5±25 mg THC C. HEATHER ASHTON !World Health Organization, 1997). Gold !1991, p. 356) remarks: ``This single fact has made obsolete much of what we once knew about the risks and consequences of marijuana use''. In the UK at present, many recreational users grow their own supplies of high- Background Increasing prevalence of Herbal cannabis contains over 400 com- potency cannabis !exact details of how to recreational cannabis use among the pounds including over 60 cannabinoids, grow it can be obtained on the internet). which are aryl-substituted meroterpenes Another main source is imports from Holland young population has stimulated debate unique to the plant genus CannabisCannabis..The The !also high-potency) and home growers can ononthe the possible effects of acute andlong-and long- pharmacology of most of the cannabinoids obtain seeds in Amsterdam at £10±£50 term use.use.term is largely unknown but the most potent for 10 seeds, depending on potency. Canna- psychoactive agent, DD99-tetrahydrocannabi- bis can be smoked as joints, from pipes, or Aims TohighlightrecentknowledgeofTohighlightrecent knowledge of nol !nol!DD99-THC, or THC), has been isolated, from `buckets', by inhaling from a mass of mechanisms of action, effects on synthesised and much studied. Other plant plant or resin ignited in a sawn-off plastic psychomotor and cognitive performance, cannabinoids include DD88-THC, cannabinol bottle. -
Perils in Benzodiazepine Withdrawal: Case Report
EJMED, European Journal of Medical and Health Sciences Vol. 2, No. 3, June 2020 Perils in Benzodiazepine Withdrawal: Case Report V. F. H Macfarlane, L. J. Moore obstructive sleep apnea resolved on repeat testing after Abstract — The discovery that clonazepam prescribed for conversion to lorazepam. Lorazepam was substituted the treatment of migraines caused obstructive sleep apnea led because it is short acting with no active metabolites and is to a rapid taper of clonazepam and substitution of lorazepam. considered favorable for use in the elderly. A very rapid Lack of accurate knowledge about the different pharmacokinetics and actions of different benzodiazepines at conversion and an inadequate substitution were made and GABA-A receptors and the risks associated with rapid the patient developed multiple physical symptoms. It took benzodiazepine withdrawal resulted in the development of the more than four months before an addiction specialist benzodiazepine protracted withdrawal syndrome. Moderately instituted appropriate treatment with a low dose of diazepam severe disability continued after 2 years. Insufficient and recognised the symptoms were due to the knowledge about benzodiazepines and their withdrawal is a benzodiazepine protracted withdrawal syndrome. None of serious problem as doctors across the world are under extreme pressure to stop prescribing them but do not have an the patient’s previous doctors had any understanding of understanding of the potential perils involved. The benzodiazepine withdrawal or recognised the challenges pathophysiology of protracted withdrawal syndrome remains associated with conversion of one benzodiazepine for poorly understood and there is no recognised treatment. another. A very slow titration of 0.5 to 1 mg diazepam every Information about appropriate management of withdrawal 2-3 months was recommended by the addiction specialist; and the protracted withdrawal syndrome are available on however, a new treating doctor reduced the dose of Professor Ashton’s website at www.benzo.org.uk. -
Step by Step Guide to Reducing from Benzodiazepines
STEP BY STEP GUIDE Reducing from Benzodiazepines & Recovery from Withdrawal 1 Table of Contents Introduction ........................................................................................................ ...3 List of Benzodiazepines .......................................................................................... 5 Dose Equivalents .................................................................................................... 6 Stabilising and Reducing the Dose ......................................................................... 7 Example of a Reduction Regime .......................................................................... 11 Benzodiazepine Withdrawal Symptoms .............................................................. 13 Management of Withdrawal Symptoms .............................................................. 14 Tips to Help with Withdrawal Symptoms ............................................................ 15 Suggestions for your Diet whilst withdrawing ..................................................... 17 Staying off Tranquillisers and Sleeping Pills ......................................................... 18 Relaxation ............................................................................................................. 19 Breathing Exercise ................................................................................................ 22 Resources for Further Assistance ......................................................................... 23 2 Introduction These -
Risks of Dependence on Benzodiazepine Drugs: a Major Problem of Long Term Treatment
Risks of dependence on benzodiazepine drugs: a major problem of long term treatment Heather Ashton BMJ: first published as 10.1136/bmj.298.6666.103 on 14 January 1989. Downloaded from Phlegmatic people dislike taking benzodiazepine drugs. In those with low'anxiety traits benzodiazepines Profiles of dependence on drugs are dysphoric and may paradoxically increase anxiety.' In normal subjects benzodiazepines improve perform- People who become dependent on drugs are suggested ance under experimental stress but worsen it under to be two different populations at the extremes of a conditions of low stress.2 Benzodiazepines relieve pre- normal distribution. Those who take drugs for pro- operative anxiety in patients with high anticipatory tection are anxious, have high scores for neuroticism but not in those with low anxiety.3 (N),46 17 are highly susceptible to punishment,'4 tender anxiety anticipatory minded, and socially compliant.4 Their preferred Thus like 0i receptor blocking agents benzodiazepines drugs are benzodiazepine tranquillosedatives, which require some underlying tone upon which to exert their they tend to take long term in low, prescribed doses. anxiolytic effects. In general, the greater the anxiety They are sensitive to withdrawal largely because of the greater the anxiolytic efficacy. their anxiety and poor abilities in coping with stress. It follows that most people who take benzodiazepines In contrast, those who take drugs for kicks have are anxious. In students a history of prescribed high scores for psychoticism (P),'7 are highly sensitive benzodiazepines correlates with a high anxiety trait.4 to reward,'4 impulsive, tough minded, antisocial, and Long term users likewise have high scores for neuroti- seek sensation.4 '7 They tend to abuse hard and soft cism. -
Fife Guidelines for Benzodiazepine Prescribing in Benzodiazepine Dependence
NHS Fife Guidelines for Benzodiazepine Prescribing in Benzodiazepine Dependence Dr. A. Baldacchino, Liz. Hutchings, Addiction Services Issued: April 2013 Review Date: April 2016 1 Approved by NHS Fife ADTC on behalf of NHS Fife Date June 2013 Contents Flowchart for Benzodiazepine Withdrawal ……………………………………………………………3 Establishing type of dependence. ...........................................................................................4 Assessment of Benzodiazepine Dependence..............................................................................5 Management of dependence in therapeutic dose users............................................................6 Management of dependence in prescribed high dose users. ...................................................7 Management of dependence in illicit and recreational users. ..................................................8 Psychological support. .................................................................................................................9 Pharmacological support............................................................................................................10 Appendices Appendix 1 Example Patient Letter (regular user).................................................11 Appendix 2 Information leaflets and advice from the internet................................13 Appendix 3 DRUG DIARY.....................................................................................14 Appendix 4 Benzodiazepine conversion table.......................................................15 -

Risks of Dependence on Benzodiazepine Drugs: a Major Problem of Long Term Treatment
Risks of dependence on benzodiazepine drugs: a major problem of long term treatment Heather Ashton BMJ: first published as 10.1136/bmj.298.6666.103 on 14 January 1989. Downloaded from Phlegmatic people dislike taking benzodiazepine drugs. In those with low'anxiety traits benzodiazepines Profiles of dependence on drugs are dysphoric and may paradoxically increase anxiety.' In normal subjects benzodiazepines improve perform- People who become dependent on drugs are suggested ance under experimental stress but worsen it under to be two different populations at the extremes of a conditions of low stress.2 Benzodiazepines relieve pre- normal distribution. Those who take drugs for pro- operative anxiety in patients with high anticipatory tection are anxious, have high scores for neuroticism but not in those with low anxiety.3 (N),46 17 are highly susceptible to punishment,'4 tender anxiety anticipatory minded, and socially compliant.4 Their preferred Thus like 0i receptor blocking agents benzodiazepines drugs are benzodiazepine tranquillosedatives, which require some underlying tone upon which to exert their they tend to take long term in low, prescribed doses. anxiolytic effects. In general, the greater the anxiety They are sensitive to withdrawal largely because of the greater the anxiolytic efficacy. their anxiety and poor abilities in coping with stress. It follows that most people who take benzodiazepines In contrast, those who take drugs for kicks have are anxious. In students a history of prescribed high scores for psychoticism (P),'7 are highly sensitive benzodiazepines correlates with a high anxiety trait.4 to reward,'4 impulsive, tough minded, antisocial, and Long term users likewise have high scores for neuroti- seek sensation.4 '7 They tend to abuse hard and soft cism. -

Guidance for the Use and Reduction of Misuse of Benzodiazepines and Other Hypnotics and Anxiolytics in General Practice
Guidance for the use and reduction of misuse of benzodiazepines and other hypnotics and anxiolytics in general practice Chris Ford and Fergus Law Guidance for the use and reduction of misuse of benzodiazepines and other hypnotics and anxiolytics in general practice Chris Ford and Fergus Law with support from Jean-Claude Barjolin, Jo Betterton, Tom Carnwath, Clare Gerada, Steve Iliffe, Mick McKernan, Graham Parsons, Stephen Pick and Muriel Simmonte Final draft: July 2014 CONTENTS SUMMARY PART 1: SECTION 1: INTRODUCTION 1.1 Background 1.2 History of benzodiazepines and other hypnotics and anxiolytics 1.3 Prevalence of benzodiazepine use and other hypnotics and anxiolytics SECTION 2: CLINICAL PHARMACOLOGY 2.1 Properties and clinical actions 2.2 Speed of onset and peak effects 2.3 Duration of action 2.4 Metabolism 2.5 Mechanism of action 2.6 Tolerance 2.7 Equivalence SECTION 3: TREATMENT OF INSOMNIA AND ANXIETY 3.1 Insomnia, anxiety, panic disorder and related conditions 3.2 Practical prescribing SECTION 4: ADVERSE EFFECTS & PROBLEMS WITH, MANAGEMENT OF AND WITHDRAWAL FROM LONG-TERM USE 4.1 Specific problems with long-term use 4.2 Withdrawal from long-term use 4.3 Other pharmacological treatments that may sometimes be useful 4.4 Longer-term prescribing PART 2: SECTION 5: ADDITIONAL INFORMATION ABOUT CERTAIN GROUPS 5.1 People with mental illness 5.2 People who use alcohol 5.3 Involuntary addiction 5.4 People who use drugs 5.5 Women 5.6 Pregnant women, neonates and breast-feeding mothers 5.7 Parents and carers 5.8 Children and young people