The Impact of Star Physicians on Diffusion
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Primary Epiploic Appendagitis☆
J COLOPROCTOL. 2013;33(3):161–166 Journal of Coloproctology www.jcol.org.br Case report Primary epiploic appendagitis☆ Carlos Augusto Real Martineza,*, Rogério Tadeu Palmab, Paulo Pedroso Silveira Júnior c, Daniela Tiemi Satoc, Murilo Rocha Rodriguesc, Hermínio Cabral de Resende Júniorb, René Crepaldi Filhod,e a Graduate Program in Health Sciences of Universidade São Francisco (USF), Bragança Paulista, SP, Brazil b Discipline of Digestive System Surgery of Faculdade de Medicina da Fundação ABC (FUABC), Santo André, SP, Brazil c School of Medicine, USF, Bragança Paulista, SP, Brazil d Discipline of Digestive System Surgery of Faculdade de Medicina da Fundação ABC (FUABC), Santo André, SP, Brazil e Discipline of Digestive System Surgery of Universidade Nove de Julho (UNIVOVE), São Paulo, SP, Brazil article info abstract Article history: Primary epiploic appendagitis (PEA) is a seldom reported disease caused by spontaneous Received 2 February 2013 torsion of one or more epiploic appendices. The aim of this study is to describe two cases Accepted 15 March 2013 of PEA reviewing the main aspects of the diagnosis and treatment of disease. Case report: Case 1) Male patient, 55 years old, obese, with abdominal right iliac fossa (RIF) pain for two Keywords: days. Abdominal examination showed pain on palpation in the RIF with rebound tenderness. Appendicitis Abdominal computed tomography identifi ed lobulated lesion in the cecum, measuring 4.5 Cecal diseases cm in diameter, which was suggestive of PEA or early neoplasm of the colon wall. The lapa- Infl ammation roscopic assessment confi rmed the diagnosis of PEA and the appendix was removed. The pa- Colon tient had a satisfactory outcome, being discharged on the second postoperative day. -

Multimodal Analgesia for Colorectal Surgery: a Retrospective Evaluation of an Enhanced Recovery Protocol
10/10/2020 Multimodal Analgesia for Colorectal Surgery: A Retrospective Evaluation of an Enhanced Recovery Protocol Andrew Candelore, DNP, CRNA Andrea Mazzei, DNP, CRNA Robert Wolfrom, DNP, CRNA 1 Introduction and Background Traditional Colorectal Surgery Laparoscopic Surgery ● Large abdominal incisions • Reduced complications ● High rates of adverse • Significantly shortened LOS outcomes • Decreased readmission rates ○ PONV ○ Increased pain Continued Challenges ○ Decreased mobility • Opioids used as primary ○ Delayed gastric motility analgesic modality ○ Urinary dysfunction • Troublesome side effects: ○ 78% increase in LOS • PONV, respiratory depression, ○ Readmission rates as high sedation, constipation, as 35.4% addiction 2 1 10/10/2020 Significance • The Opioid Epidemic • 99% of adult surgical patients receive an opioid • 6-10% of opioid-naïve patients have continued dependence • 14.4% of colorectal surgical patients report chronic use pattern postoperatively • Anesthetic Pain Management • Aim to limit opioids • Adopt alternative approaches • Provide effective analgesia while promoting optimal patient outcomes 3 Purpose and Objectives • Project Purpose Evaluate the perioperative care improvement initiative implemented at Christiana Care by the Department of Anesthesia which aimed to improve the quality of recovery from colorectal surgery through the utilization of multimodal analgesia. • Determine if multimodal analgesia, as compared to traditional anesthesia care, reduced: • Pain scores • Opioid consumption • PONV • Hospital LOS -

600 Technology (Applied Sciences)
600 600 Technology (Applied sciences) Class here inventions See also 303.48 for technology as a cause of cultural change; also 306.4 for sociology of technology; also 338.1–338.4 for economic aspects of industries based on specific technologies; also 338.9 for technology transfer, appropriate technology See Manual at 300 vs. 600; also at 363 vs. 302–307, 333.7, 570–590, 600; also at 363.1 vs. 600; also at 583–585 vs. 600 SUMMARY 601–609 Standard subdivisions and technical drawing, hazardous materials technology, patents 610 Medicine and health 620 Engineering and allied operations 630 Agriculture and related technologies 640 Home and family management 650 Management and auxiliary services 660 Chemical engineering and related technologies 670 Manufacturing 680 Manufacture of products for specific uses 690 Construction of buildings 601 Philosophy and theory 602 Miscellany Do not use for patents; class in 608 Class interdisciplinary works on trademarks and service marks in 929.9 Interdisciplinary collections of standards relocated to 389 .9 Commercial miscellany Class commercial miscellany of products and services used in individual and family living in 640.29; class commercial miscellany of manufactured products in 670.29; class interdisciplinary commercial miscellany in 381.029 603 Dictionaries, encyclopedias, concordances 604 Technical drawing, hazardous materials technology; groups of people 657 604 Dewey Decimal Classification 604 .2 Technical drawing Including arrangement and organization of drafting rooms, preservation and storage of drawings; specific drafting procedures and conventions (e.g., production illustration, dimensioning; lettering, titling; shades, shadows, projections); preparation and reading of copies Class here engineering graphics, mechanical drawing For architectural drawing, see 720.28. -

Coloduodenal Fistula in Right Colorectal Cancer: Case Report and Review of the Literature
Journal of Medical Research and Health Sciences Received 5 Dec 2020 | Accepted 12 Jan 2021 | Published Online 16 Jan 2021 DOI: https://doi.org/10.15520/jmrhs.v4i1.303 JMRHS 4 (1), 1135−1138 (2020) ISSN (O) 2589-9031 | (P) 2589-9023 CASE REPORTS Coloduodenal Fistula in Right Colorectal Cancer: Case Report and Review of the Literature ∗ Patricia Ciriano Hernández 1 Carlos Martínez Pinedo Rafael Picón Rodríguez Elisa Jiménez Higuera Daniel Sánchez Peláez Ángel Fernández Camuñas Jesús Martín Fernández 1General and Digestive System Abstract Surgery Hospital General In spite of the high incidence of colorectal cancer, cases of right colon Universitario de Ciudad Real Calle Obispo Rafael Torija 13005 cancer presenting with local invasion are not common. This is even Ciudad Real, Castilla la Mancha, more infrequent if we focus on duodenal invasion and presence of Spain duodenal fistula. We present the case of a patient admitted to our hospital due to severe weight loss, malnutrition and bowel obstruction. The patient was diagnosed of advanced right colon cancer with coloduodenal fistula and concomitant liver metastasis. According to diagnosis, palliative surgery was performed. 1 INTRODUCTION mia, diarrhea or feculent vomiting. (1)(5) Diagnosis is based on upper endoscopy and olorectal cancer is one of the most frequent colonoscopy, which can also provide the biopsy for malignancies among developed countries. CLocally advanced cases range from 5 to 25%. histopathological confirmation. The gold standard The specific invasion of the duodenum has been radiology test is the CT scan. reported to account for 0, 4 %. ((1),(2) Management of malignant duodenal fistula poses a This clinical entity has become a rare event in present dilemma to surgeons. -

Tariff of Fees for Insured Medical Services Regulations (O.I.C. 81-379)
0 Certified to be a true copy of an Order of his Honour the Governor of Nova Scotia in Council made the EXCUTVE coUNCIL Lieutenant 24th day of March A. D. 1981 N. S. Reuhton NOVA scoriA _3i/_’) 81-379 / The Governor in Council on the report and recommendation of the Minister of Health dated the 13th day of March, A... D., 1981, and pursuant to clause (a) of subection (1) of Section 11 of Chapter 8 of the Statutes of Nova Scotia, 1973, the Health Services and Insurance Act, and subsection (3) of Section 4 of Chapter 15 of the Statutes of Nova Scotia, 1973, the Regulations Act, is pleased to: (a) approve and authorize payments by the Health Services and Insurance Commission in respect of the tariff of fees for insured medical services attached to and forming part of the report and recommendation, and marked Schedule “A”, effective for a period of one year, comrnencing.on the 1st day of April, A. D., 1980, at a rate of 85% of the fee so calculated; and (b) order that the publication of this regulation be dispense4 with due to the length of the Schedule attached to and forming part of the report and recommendation. 1-3. H F. G. STEVEiS, Q..C., CLEKOF THE EXECUTIVE COUNCIL. 5/1 SCHEDULE “A” TABLE OF CONTENTS PREAMBLE 2 UNIT VALUE SYSTEM 21 MISCELLANEOUS FEES 22 FAMILY PRACTICE 24 ANAESTHESIA 26 DERMATOLOGY 29 INTERNAL MEDICINE 31 NEUROLOGY 33 PHYSICAL MEDICINE AND REHABILITATION 35 PABDIATRICS 37 PSYCHIATRY 39 DIAGNOSTIC AND THERAPEUTIC PROCEDURES 41 GENERAL SURGERY 51 NEUROSURGERY 75 OBSTETRICS AND GYNAECOLOGY 82 OPHTHALMOLOGY 87 OTOLARYNGOLOGY 92 ORTHOPAEDIC SURGERY 98 PLASTIC SURGERY 116 UROLOGY 124 RADIATION ONCOLOGY 133 PATHOLOGY CONSULTATIONS 134 INDEX 150 —- — — e • r. -

Table of Contents
TABLE OF CONTENTS 4 GENERAL INFORMATION ABOUT THE MEETING Communications at the 4 Registration Information SAGES Meeting 6 SCHEDULE AT A GLANCE 8, 10 SAGES Meeting Leaders You will be able to reach the world and the world will be able to reach you while you are in attendance at the 12 Wednesday, March 31, 2004 Program SAGES meeting. 19 Thursday, April 1, 2004 Program Option 1: 31 Friday, April 2, 2004 Program A message can be left for you at either of the following 40 Saturday, April 3, 2004 Program phone numbers. A fax message can be sent using the number below. The phone or fax message will be posted for you on 2004 HANDS-ON COURSES SAGES Message Board outside the Main Session Room. 16 Advanced Laparoscopic Techniques Registration: 303-228-8293 20 Surgeons in the Digital Age SAGES On-Site Office: 303-228-8291 2004 POSTGRADUATE COURSES SAGES On-Site Office Fax: 303-228-8292 14 Complications in Bariatric Surgery and Option 2: How to Manage Them Five email stations will be available at which attendees 22 Top to Bottom: GERD can check and send email. Two stations will be placed in the Exhibit hall, one in the Olympus booth (309) and one 24 Top to Bottom: Colon adjacent to booth 230. An additional two stations will be 26 Minimally Invasive Surgery in HPB Tumors located outside the Main Session room. A final station will be located in the Foundation Donors booth (accessible to 17 Primer on Establishing and Running a MIS/GI Foundation donors only). Fellowship Program 18 Evening Video Session 21 Allied Health Professionals Course Thanks to our 28 RESIDENT & FELLOW SCIENTIFIC SESSION Corporate Supporters! 30 Industry Education Events Platinum Level Donors 31 Industry Breakfast 32 2004 SCIENTIFIC SESSION Auto Suture Ethicon Endo-Surgery, Inc. -

Hospital and Day Surgery 2017 National Institute for Health Development
Hospital and day surgery 2017 National Institute for Health Development Hospital and day surgery 2017 Merike Rätsep Tallinn 2019 The mission of the National Institute for Health Development is to create and share knowledge for influencing the attitudes, behaviour, policies and the environment with evidence-based information with an aim of improving the well-being of the people in Estonia. When using the information presented in this report, refer to the publication. Recommended reference: Rätsep M. Hospital and day surgery 2017. Tallinn: National Institute for Health Development; 2019. Contents Definitions ................................................................................................................................................................................................. 4 Abbreviations .......................................................................................................................................................................................... 4 Summary .................................................................................................................................................................................................... 5 Introduction ............................................................................................................................................................................................. 6 1 Results .................................................................................................................................................................................................. -

Appendix I: Chronology of the Evolution of Family Practice As a Specialty in the United States
Appendix I: Chronology of the Evolution of Family Practice as a Specialty in the United States Robert B. Taylor Year Event Significance 1900 At least 80% of American physicians were General practice was the predominant model of general practitioners: one general practitioner medical care. for every 600 people. 1910 Publication of the Flexner Report by the Prompted changes in methods and quality of Carnegie Foundation with cooperation of the medical education: premedical education, American Medical Association (AMA). biomedical research, and postgraduate training. 1940 Generalists comprised 76% of private medical Decline of general ism paralleled the rise of specialty practitioners. practice. 1950-62% of practitioners were generalists 1960-45% of practitioners were generalists 1970-21 % of practitioners were generalists AMA petitioned to approve a general practice Request refused. specialty board. 1941 General Practice Certifying Board proposed at First call for a certifying board for general ists. AMA House of Delegates. 1946 Section on General Practice of the AMA An early organization of generalists with nationwide organized. representation. 1947 American Academy of General Practice (MGP) First major medical organization to require founded. continuing medical education as a condition of membership. 1950 First residency training programs in general Signified need for postgraduate generalist training practice established. beyond the internship year. Publication of journal GP. First scientific journal for generalists. 1958 Family Health Foundation of America Early funding for conferences on family medicine incorporated. education. 1154 Robert B. Taylor Year Event Significance 1960 American Board of General Practice formed. First effort to obtain general practice board status. 1964 19% of U.S. medical graduates entered general Continued decline in numbers of general practice. -

4Th Quarter 2001 Medicare a Bulletin
In This Issue... Medicare Guidelines on Telehealth Services Benefit Expansion, Coverage and Conditions for Reimbursement of These Services ............... 5 Medicare eNews Now Available Join Florida Medicare eNews Mailing List to Receive Important News and Information ........ 9 Expansion of Coverage on Percutaneous Transluminal Angioplasty Coverage Expansion and Claim Processing Instructions for Hospital Inpatient Services ..... 12 Skilled Nursing Facility Consolidated Billing Clarification to Health Insurance Prospective Payment System Coding and Billing Guidelines .............................................................................................................................. 15 Final Medical Review Policies 10060, 55873, 67221, 71250, 74150, 84155, 85007, 88141, 92225, 93303, A0430, G0030,G0104, G0108, J1561, J1745, J9212, and M0302 ...................................... 22 Outpatient Prospective Payment System Update and Changes to the Hospital Outpatient Prospective Payment System ...................... 87 Bulletin Reader Survey Provide your Comments and Feedback on the Medicare Part A Publication and/or our Provider Web Site ................................................................................................................ 103 Features From the Medical Director 3 he Medicare A Bulletin should be shared with all Administrative 4 T health care practitioners and General Information 5 managerial members of the General Coverage 11 provider/supplier staff. Publications issued after End Stage Renal Disease 13 -

Estimation of Physiologic Ability and Surgical Stress Scoring System Appraises Laparoscopy-Assisted and Open Distal Gastrectomy in Treatment of Early Gastric Cancer*
Journal of Cancer Therapy, 2013, 4, 1-5 1 http://dx.doi.org/10.4236/jct.2013.49A1001 Published Online October 2013 (http://www.scirp.org/journal/jct) Estimation of Physiologic Ability and Surgical Stress Scoring System Appraises Laparoscopy-Assisted and Open Distal Gastrectomy in Treatment of Early Gastric Cancer* Hideki Bou1#, Hideyuki Suzuki1, Kentaro Maejima1, Hidetsugu Hanawa1, Masanori Watanabe1, Eiji Uchida2 1Institute of Gastroenterology, Nippon Medical School Musashi-kosugi Hospital, Kawasaki, Japan; 2Department of Surgery, Nippon Medical School, Tokyo, Japan. Email: #[email protected] Received July 24th, 2013; revised August 23rd, 2013; accepted August 30th, 2013 Copyright © 2013 Hideki Bou et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. ABSTRACT Laparoscopy-assisted distal gastrectomy (LADG) has been widely used to treat early gastric cancer (EGC). The Esti- mation of Physiologic Ability and Surgical Stress (E-PASS) scoring system predicts the risk of fatal postoperative com- plications by quantifying the patient’s reserve and degree of surgical stress, but there have been a few reports of use of the E-PASS scoring system to assess the risk of mortality following special types of surgical procedures such as LADG. In this study we assessed the feasibility of LADG versus open distal gastrectomy (ODG) by the E-PASS scoring system. The subjects of this study consisted of 69 stage IA gastric cancer patients who underwent LADG (LADG group) and 69 stage IA gastric cancer patients who underwent ODG (ODG group). -

Surgical-Site Infection Risk in Oncologic Digestive Surgery
ARTICLE Surgical-site infection risk in oncologic ORIGINAL digestive surgery ABSTRACT Authors Paulo de Tarso Oliveira e Surgical-site infection (SSI) is the most prevalent type of hospital infection in surgical patients and is as- Castro1 2 sociated with an increase in hospital stay, costs and morbidity/lethality. The knowledge of the main risk André Lopes Carvalho Stela Verzinhasse Peres3 factors for this type of infection is important for the establishment of prevention measures regarding mod- Milene Mitsuyuki ifiable risks factors. The objective of the preset study was to assess the occurrence of SSI and study the risk Foschini4 factors in oncologic surgeries of the digestive system at Hospital de Câncer in Barretos, São Paulo, Brazil. Afonso Dinis Costa Passos5 Individuals undergoing oncologic surgeries of the digestive system in the period of 08/01/2007 to 08/10/2008 were prospectively followed for 30 days after surgery. Possible risk factors related to the 1Infectologist , Hospital de patient and to the surgical procedure were also studied. A total of 210 surgeries were analyzed, with Câncer de Barretos, São Paulo, Brazil a global SSI incidence of 23.8%. The following variables were independently associated with SSI: time 2Prof. Dr., Hospital de and type of surgery, radiotherapy before surgery and surgeon’s years of experience. The risk factors Câncer de Barretos, São Paulo, Brazil found in this study have been described by other authors and are not amenable to intervention for 3Epidemiologist, Hospital SSI prevention. Further studies are recommended with the objective of investigating interventions de Câncer de Barretos, São that could reduce the risk for SSI in this type of surgery. -
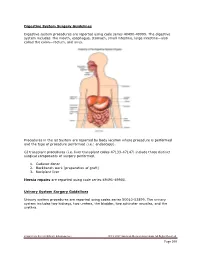
Page 100 Digestive System Surgery Guidelines Digestive System
Digestive System Surgery Guidelines Digestive system procedures are reported using code series 40490-49999. The digestive system includes the mouth, esophagus, stomach, small intestine, large intestine—also called the colon—rectum, and anus. Procedures in the GI System are reported by body location where procedure is performed and the type of procedure performed (i.e.: endoscopy). GI transplant procedures (i.e. liver transplant codes 47133-47147) include three distinct surgical components of surgery performed. 1. Cadaver donor 2. Backbench work (preparation of graft) 3. Recipient liver Hernia repairs are reported using code series 49491-49900. Urinary System Surgery Guidelines Urinary system procedures are reported using codes series 50010-53899. The urinary system includes two kidneys, two ureters, the bladder, two sphincter muscles, and the urethra. Proprietary Xact Healthcare Solutions, Inc. CPT© 2017 American Medical Association. All Rights Reserved Page 100 Male Genital System Surgery Guidelines Male genital system procedures are reported using codes series 54000-55899. The male genital system includes the penis, scrotum and testicles. Female Genital System Surgery Guidelines Female genital system procedures are reported using code series 56405-58999. The female genital system includes the external organs: the labia majora, labia manora, Bartholin's glands, the clitoris and the internal organs: vagina, uterus, ovaries and fallopian tubes. Proprietary Xact Healthcare Solutions, Inc. CPT© 2017 American Medical Association. All Rights Reserved Page 101 Maternity Care and Delivery procedure codes are reported using code series 59000- 59899 and include all procedures performed antepartum, delivery and postpartum. Antepartum procedures are those procedures that occur just prior to childbirth and include any patient history and exam, record of weight, BP, routine urinalysis and all monthly visits up to twenty-eight weeks of pregnancy, biweekly visits up to thirty-six weeks of pregnancy and weekly visits up to the date of delivery.