Fetal Renal Cystic Diseases
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Educational Paper Ciliopathies
Eur J Pediatr (2012) 171:1285–1300 DOI 10.1007/s00431-011-1553-z REVIEW Educational paper Ciliopathies Carsten Bergmann Received: 11 June 2011 /Accepted: 3 August 2011 /Published online: 7 September 2011 # The Author(s) 2011. This article is published with open access at Springerlink.com Abstract Cilia are antenna-like organelles found on the (NPHP) . Ivemark syndrome . Meckel syndrome (MKS) . surface of most cells. They transduce molecular signals Joubert syndrome (JBTS) . Bardet–Biedl syndrome (BBS) . and facilitate interactions between cells and their Alstrom syndrome . Short-rib polydactyly syndromes . environment. Ciliary dysfunction has been shown to Jeune syndrome (ATD) . Ellis-van Crefeld syndrome (EVC) . underlie a broad range of overlapping, clinically and Sensenbrenner syndrome . Primary ciliary dyskinesia genetically heterogeneous phenotypes, collectively (Kartagener syndrome) . von Hippel-Lindau (VHL) . termed ciliopathies. Literally, all organs can be affected. Tuberous sclerosis (TSC) . Oligogenic inheritance . Modifier. Frequent cilia-related manifestations are (poly)cystic Mutational load kidney disease, retinal degeneration, situs inversus, cardiac defects, polydactyly, other skeletal abnormalities, and defects of the central and peripheral nervous Introduction system, occurring either isolated or as part of syn- dromes. Characterization of ciliopathies and the decisive Defective cellular organelles such as mitochondria, perox- role of primary cilia in signal transduction and cell isomes, and lysosomes are well-known -

Potter Syndrome: a Case Study
Case Report Clinical Case Reports International Published: 22 Sep, 2017 Potter Syndrome: A Case Study Konstantinidou P1,2, Chatzifotiou E1,2, Nikolaou A1,2, Moumou G1,2, Karakasi MV2, Pavlidis P2 and Anestakis D1* 1Laboratory of Forensic and Toxicology, Department of Histopathology, Aristotle University of Thessaloniki, Greece 2Laboratory of Forensic Sciences, Department of Histopathology, Democritus University of Thrace School, Greece Abstract Potter syndrome (PS) is a term used to describe a typical physical appearance, which is the result of dramatically decreased amniotic fluid volume secondary to renal diseases such as bilateral renal agenesis (BRA). Other causes are abstraction of the urinary tract, autosomal recessive polycystic kidney disease (ARPKD), autosomal dominant polycystic kidney disease (ADPKD) and renal hypoplasia. In 1946, Edith Potter characterized this prenatal renal failure/renal agenesis and the resulting physical characteristics of the fetus/infant that result from oligohydramnios as well as the complete absence of amniotic fluid (anhydramnios). Oligohydramnios and anhydramnios can also be due to the result of leakage of amniotic fluid from rupturing of the amniotic membranes. The case reported concerns of stillborn boy with Potter syndrome. Keywords: Potter syndrome; Polycystic kidney disease; Oligohydramnios sequence Introduction Potter syndrome is not technically a ‘syndrome’ as it does not collectively present with the same telltale characteristics and symptoms in every case. It is technically a ‘sequence’, or chain of events - that may have different beginnings, but ends with the same conclusion. Below are the different ways that Potter syndrome (A.K.A Potter sequence) can begin due to various causes of renal failure. They gave numbers to differentiate the different forms, but this system had not caught in the medical and scientific communities [1]. -

What a Difference a Delay Makes! CT Urogram: a Pictorial Essay
Abdominal Radiology (2019) 44:3919–3934 https://doi.org/10.1007/s00261-019-02086-0 SPECIAL SECTION : UROTHELIAL DISEASE What a diference a delay makes! CT urogram: a pictorial essay Abraham Noorbakhsh1 · Lejla Aganovic1,2 · Noushin Vahdat1,2 · Soudabeh Fazeli1 · Romy Chung1 · Fiona Cassidy1,2 Published online: 18 June 2019 © This is a U.S. Government work and not under copyright protection in the US; foreign copyright protection may apply 2019 Abstract Purpose The aim of this pictorial essay is to demonstrate several cases where the diagnosis would have been difcult or impossible without the excretory phase image of CT urography. Methods A brief discussion of CT urography technique and dose reduction is followed by several cases illustrating the utility of CT urography. Results CT urography has become the primary imaging modality for evaluation of hematuria, as well as in the staging and surveillance of urinary tract malignancies. CT urography includes a non-contrast phase and contrast-enhanced nephrographic and excretory (delayed) phases. While the three phases add to the diagnostic ability of CT urography, it also adds potential patient radiation dose. Several techniques including automatic exposure control, iterative reconstruction algorithms, higher noise tolerance, and split-bolus have been successfully used to mitigate dose. The excretory phase is timed such that the excreted contrast opacifes the urinary collecting system and allows for greater detection of flling defects or other abnormali- ties. Sixteen cases illustrating the utility of excretory phase imaging are reviewed. Conclusions Excretory phase imaging of CT urography can be an essential tool for detecting and appropriately characterizing urinary tract malignancies, renal papillary and medullary abnormalities, CT radiolucent stones, congenital abnormalities, certain chronic infammatory conditions, and perinephric collections. -

Renal Agenesis, Renal Tubular Dysgenesis, and Polycystic Renal Diseases
Developmental & Structural Anomalies of the Genitourinary Tract DR. Alao MA Bowen University Teach Hosp Ogbomoso Picture test Introduction • Congenital Anomalies of the Kidney & Urinary Tract (CAKUT) Objectives • To review the embryogenesis of UGS and dysmorphogenesis of CAKUT • To describe the common CAKUT in children • To emphasize the role of imaging in the diagnosis of CAKUT Introduction •CAKUT refers to gross structural anomalies of the kidneys and or urinary tract present at birth. •Malformation of the renal parenchyma resulting in failure of normal nephron development as seen in renal dysplasia, renal agenesis, renal tubular dysgenesis, and polycystic renal diseases. Introduction •Abnormalities of embryonic migration of the kidneys as seen in renal ectopy (eg, pelvic kidney) and fusion anomalies, such as horseshoe kidney. •Abnormalities of the developing urinary collecting system as seen in duplicate collecting systems, posterior urethral valves, and ureteropelvic junction obstruction. Introduction •Prevalence is about 3-6 per 1000 births •CAKUT is one of the commonest anomalies found in human. •It constitute approximately 20 to 30 percent of all anomalies identified in the prenatal period •The presence of CAKUT in a child raises the chances of finding congenital anomalies of other organ-systems Why the interest in CAKUT? •Worldwide, CAKUT plays a causative role in 30 to 50 percent of cases of end-stage renal disease (ESRD), •The presence of CAKUT, especially ones affecting the bladder and lower tract adversely affects outcome of kidney graft after transplantation Why the interest in CAKUT? •They significantly predispose the children to UTI and urinary calculi •They may be the underlying basis for urinary incontinence Genes & Environment Interact to cause CAKUT? • Tens of different genes with role in nephrogenesis have been identified. -

Potter Syndrome, a Rare Entity with High Recurrence Risk in Women with Renal Malformations – Case Report and a Review of the Literature
CASE PRESENTATIONS Ref: Ro J Pediatr. 2017;66(2) DOI: 10.37897/RJP.2017.2.9 POTTER SYNDROME, A RARE ENTITY WITH HIGH RECURRENCE RISK IN WOMEN WITH RENAL MALFORMATIONS – CASE REPORT AND A REVIEW OF THE LITERATURE George Rolea1, Claudiu Marginean1, Vladut Stefan Sasaran2, Cristian Dan Marginean2, Lorena Elena Melit3 1Obstetrics and Gynecology Clinic 1, Tirgu Mures 2University of Medicine and Pharmacy, Tirgu Mures 3Pediatrics Clinic 1, Tirgu Mures ABSTRACT Potter syndrome represents an association between a specific phenotype and pulmonary hypoplasia as a result of oligohydramnios that can appear in different pathological conditions. Thus, Potter syndrome type 1 or auto- somal recessive polycystic renal disease is a relatively rare pathology and with poor prognosis when it is diag- nosed during the intrauterine life. We present the case of a 24-year-old female with an evolving pregnancy, 22/23 gestational weeks, in which the fetal ultrasound revealed oligohydramnios, polycystic renal dysplasia and pulmonary hypoplasia. The personal pathological history revealed the fact that 2 years before this pregnancy, the patient presented a therapeutic abortion at 16 gestational weeks for the same reasons. The maternal ultra- sound showed unilateral maternal renal agenesis. Due to the fact that the identified fetal malformation was in- compatible with life, we decided to induce the therapeutic abortion. The particularity of the case consists in di- agnosing Potter syndrome in two successive pregnancies in a 24-year-old female, without any significant -

Ectopic Kidney
Ectopic Kidney We normally have two kidneys which each have a single tube (called a ureter) that connects to the bladder. This tube drains urine from the kidneys into the bladder (see below). In some pregnancies, the kidneys do not develop normally. One such variation is known as an ECTOPIC KIDNEY. An ectopic kidney means that the kidney is not in the usual position. You may be told that your baby has an ectopic kidney, during your pregnancy ultrasound scan or after your baby’s birth. You may need to go back to the hospital for further tests during the pregnancy and after birth. You may instead be told your child has an ectopic kidney if he / she has had investigations due to urine tract infections or abdominal pain. About the urinary system The kidneys are part of the urinary system, which gets rid of things that the body no longer needs so that we can grow and stay healthy. The kidneys are bean-shaped organs. They filter blood and remove extra water, salt and waste in urine (wee). Most of us have two kidneys, which are at the back on either side of our spine (backbone), near the bottom edge of our ribs. Other parts of the urinary system are: two ureters– long tubes that carry urine from the kidneys to the bladder bladder– muscular bag that stores urine until we are ready to pass urine urethra– tube that carries urine from the bladder out of the body. <More information about the urinary system and kidneys> Ectopic Kidney About Ectopic kidney Ectopic kidneys are one type of congenital renal anomaly: • ectopic – in an abnormal place or position • congenital – the problem is present at birth • renal – to do with the kidneys • anomaly– different from normal Ectopic kidneys occur due to an abnormality in the way the growing baby’s urinary system is developing while a baby is growing in the uterus (womb). -

Evolving Concepts in Human Renal Dysplasia
DISEASE OF THE MONTH J Am Soc Nephrol 15: 998–1007, 2004 EBERHARD RITZ, FEATURE EDITOR Evolving Concepts in Human Renal Dysplasia ADRIAN S. WOOLF, KAREN L. PRICE, PETER J. SCAMBLER, and PAUL J.D. WINYARD Nephro-Urology and Molecular Medicine Units, Institute of Child Health, University College London, London, United Kingdom Abstract. Human renal dysplasia is a collection of disorders in correlating with perturbed cell turnover and maturation. Mu- which kidneys begin to form but then fail to differentiate into tations of nephrogenesis genes have been defined in multiorgan normal nephrons and collecting ducts. Dysplasia is the princi- dysmorphic disorders in which renal dysplasia can feature, pal cause of childhood end-stage renal failure. Two main including Fraser, renal cysts and diabetes, and Kallmann syn- theories have been considered in its pathogenesis: A primary dromes. Here, it is possible to begin to understand the normal failure of ureteric bud activity and a disruption produced by nephrogenic function of the wild-type proteins and understand fetal urinary flow impairment. Recent studies have docu- how mutations might cause aberrant organogenesis. mented deregulation of gene expression in human dysplasia, Congenital anomalies of the kidney and urinary tract and the main renal pathology is renal dysplasia (RD). In her (CAKUT) account for one third of all anomalies detected by landmark book Normal and Abnormal Development of the routine fetal ultrasonography (1). A recent UK audit of child- Kidney published in 1972 (7), Edith Potter emphasized that one hood end-stage renal failure reported that CAKUT was the must understand normal development to generate realistic hy- cause in ~40% of 882 individuals (2). -
Renal Agenesis: Difficulties and Pitfalls of Antenatal Diagnosis in 5
Scholars International Journal of Obstetrics and Gynecology Abbreviated Key Title: Sch Int J Obstet Gynec ISSN 2616-8235 (Print) |ISSN 2617-3492 (Online) Scholars Middle East Publishers, Dubai, United Arab Emirates Journal homepage: https://saudijournals.com Original Research Article Renal Agenesis: Difficulties and Pitfalls of Antenatal Diagnosis in 5 Cases and Review of the Literature Imane Attar1*, Hekmat Chaara1, Sofia Jayi1, Fatima-Zahra Fdili Alaoui1, Moulay Abdelilah Melhouf1 1Department of Gynecology and Obstetrics II, Chu Hassan II Fes, Morocco DOI: 10.36348/sijog.2021.v04i04.006 | Received: 07.03.2021 | Accepted: 06.04.2021 | Published: 15.04.2021 *Corresponding author: Imane Attar Abstract Renal agenesis is the absence of any trace of kidney, ureter, and therefore the absence of fetal renal function. It constitutes a major field of antenatal screening which presents until now certain limits during ultrasound diagnosis which remains the only accessible, inexpensive and reproducible means of exploration for making the diagnosis with a sensitivity of 85%. The neonatal prognosis is considered better in the unilateral Renal agenesis with functional contralateral kidney, but is always fatal in its bilateral form. The objective of our study is to clarify the ultrasound strategy that must be adopted in antenatal to make the diagnosis while highlighting the technical difficulties that can misdiagnose. An update on the epidemiological and etiopathogenetic nature of the anomaly will also be discussed. Keywords: Renal agenesis; antenatal diagnosis; Topography; prognosis. Copyright © 2021 The Author(s): This is an open-access article distributed under the terms of the Creative Commons Attribution 4.0 International License (CC BY-NC 4.0) which permits unrestricted use, distribution, and reproduction in any medium for non-commercial use provided the original author and source are credited. -

Congenital Kidney and Urinary Tract Anomalies: a Review for Nephrologists
REVIEW ARTICLE Port J Nephrol Hypert 2018; 32(4): 385-391 • Advance Access publication 4 January 2019 Congenital kidney and urinary tract anomalies: a review for nephrologists Marina Vieira, Aníbal Ferreira, Fernando Nolasco Nephrology Department, Hospital Curry Cabral, Centro Hospitalar Lisboa Central, Lisboa, Portugal Received for publication: Sep 7, 2018 Accepted in revised form: Dec 7, 2018 ABSTRACT Kidney and urinary tract development disorder are two of the most prevalent congenital malformations and the main cause of chronic kidney disease in pediatric age patients. As such, it is very important that the neph‑ rologist understands these pathologies to improve transition and ensure a good continuity between pediatric and adult nephrological care. The purpose of this article is to present a brief review of congenital anomalies of the kidney and urinary tract (CAKUT). Kidney malformations are classified according to macroscopic and microscopic anatomic features, and are the result of the following abnormal renal developmental processes: malformations of the renal parenchyma, abnor‑ malities of the embryonic migration of the kidneys and abnormalities of the developing urinary collecting system. Keys words: congenital anomalies of the kidneys and urinary tract, dysplasia, ciliopathies, posterior urethral valves, vesicoureteral reflux. INTRODUCTION are more likely to require dialysis6. Kidney malforma‑ tions are classified according to macroscopic and micro‑ Kidney and urinary tract development disorders scopic anatomic features, and -

The Presentation and Management of Neonatal Obstructive Uropathies J
Postgrad Med J: first published as 10.1136/pgmj.48.562.486 on 1 August 1972. Downloaded from Postgraduate Medical Journal (August 1972) 48, 486 -492. The presentation and management of neonatal obstructive uropathies J. H. JOHNSTON F.R.C.S. Alder Hey Children's Hospital, Liverpool Presentation urinary, alimentary and genital tracts share a The existence of a congenital urinary obstruction common evacuatory channel is similarly frequently may be suggested when routine examination of the associated with upper urinary tract lesions. newborn infant reveals such signs as enlargement of one or both kidneys, distension of the bladder or (3) Anomalies of the female genital tract slow, dribbling micturition. The paediatrician should Congenital absence of the vagina is associated also be alerted to the possibility of obstructive uro- with urinary tract anomalies in some 500 of cases pathy when there are present non-urological con- (Bryan, Nigro & Counsellor, 1949). A similar high genital anomalies which often secondarily involve incidence occurs with such conditions as duplication the urinary tract or which are known commonly to ofthe vagina and uterus but these may not be obvious co-exist with congenital urinary tract lesions. clinically in the young child. Secondary involvement, with obstruction, of the urinary tract occurs with space-occupying masses in Deficient abdominal mucsculature (4) by copyright. the pelvis such as hydrometrocolpos or a large intra- Urinary tract anomalies of various degrees of pelvic component of a sacrococcygeal teratoma. are The pelvic tumour, by displacing the bladder, leads severity always present. to chronic urinary retention and upper tract dilata- Cardiac anomalies tion. -

Diagnosis and Management in Most Frequent Congenital Defects Of
Prof. dr hab. Anna Wasilewska ~ 10% born with potentially significant malformation of urinary tract, but congenital renal disease much less common 1. Anomalies of the number a. Renal agenesis b. Supernumerary kidney 2. Anomalies of the size a. Renal hypoplasia 3. Anomalies of kidney structure a. Polcystic kidney b. Medullary sponge kidney 4. Anomalies of position • Ectopic pelvic kidney • Ectopic thoracic kidney • Crossed ectopic kidney with and without fusion 5. Anomalies of fusion • Horseshoe kidney • Crossed ectopic kidney with fusion 6. Anomalies of the renal collecting system a. Calcyeal diverticulum b. Ureterpelvic junction stenosis 7. Anomalies of the renal vasculature a. Arteriovenous malformations and fistulae b. Aberrant and accessory vessels. c. Renal artery stenosis The distinction between severe unilateral hydronephrosis and a multicystic dysplastic kidney may be unclear bilaterally enlarged echogenic kidneys, associated with hepatobiliary dilatation and oligohydroamnios suggests autosomal recessive polycystic kidney disease. Simple cysts Autosomal Dominant Polycystic Kidney Disease Autosomal Recessive Polycystic Kidney Disease Multicystic Dysplastic Kidney Disease cysts may be › solitary or multiple › unilateral or bilateral › congenital (hereditary or not) or acquired common increasing incidence with age single or multiple few mms to several cms smooth lining, clear fluid no effect on renal function occasionally haemorrhage, causing pain only real issue is distinction from tumour Characterized by cystic -
Angiotensin Converting Enzyme (ACE) Inhibitors
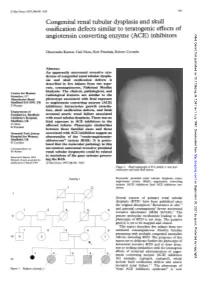
J Med Genet 1997;34:541-545 541 Congenital renal tubular dysplasia and skull ossification defects similar to teratogenic effects of J Med Genet: first published as 10.1136/jmg.34.7.541 on 1 July 1997. Downloaded from angiotensin converting enzyme (ACE) inhibitors Dhavendra Kumar, Gail Moss, Rob Primhak, Robert Coombs Abstract An apparently autosomal recessive syn- drome of congenital renal tubular dyspla- sia and skull ossification defects is described in five infants from two sepa- rate, consanguineous, Pakistani Muslim kindreds. The clinical, pathological, and Centre for Human Genetics, 117 radiological features are similar to the Manchester Road, phenotype associated with fetal exposure Sheffield S1O 5DN, UK to angiotensin converting enzyme (ACE) D Kumar inhibitors: intrauterine growth retarda- Department of tion, skull ossification defects, and fetal/ Paediatrics, Sheffield neonatal anuric renal failure associated Children's Hospital, with renal tubular dysplasia. There was no Sheffield, UK fetal exposure to ACE inhibitors in the G Moss affected infants. similarities R Primhak Phenotypic between these familial cases and those Neonatal Unit, Jessop associated with ACE inhibition suggest an Hospital for Women, abnormality of the "renin-angiotensin- Sheffield, UK aldosterone" system (RAS). It is postu- R Coombs lated that the molecular pathology in this Correspondence to: uncommon autosomal recessive proximal Dr Kumar. renal tubular dysgenesis could be related http://jmg.bmj.com/ to mutations of the Received 4 March 1996 gene systems govern- Revised version accepted for ing the RAS. publication 6 March 1997 (JMed Genet 1997;34:541-545) Figure 2 Skull radiograph ofIV.5,family 1: note poor ossification and wide skull sutures.