Antibiotic Guideline
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Medical Review(S) Clinical Review
CENTER FOR DRUG EVALUATION AND RESEARCH APPLICATION NUMBER: 200327 MEDICAL REVIEW(S) CLINICAL REVIEW Application Type NDA Application Number(s) 200327 Priority or Standard Standard Submit Date(s) December 29, 2009 Received Date(s) December 30, 2009 PDUFA Goal Date October 30, 2010 Division / Office Division of Anti-Infective and Ophthalmology Products Office of Antimicrobial Products Reviewer Name(s) Ariel Ramirez Porcalla, MD, MPH Neil Rellosa, MD Review Completion October 29, 2010 Date Established Name Ceftaroline fosamil for injection (Proposed) Trade Name Teflaro Therapeutic Class Cephalosporin; ß-lactams Applicant Cerexa, Inc. Forest Laboratories, Inc. Formulation(s) 400 mg/vial and 600 mg/vial Intravenous Dosing Regimen 600 mg every 12 hours by IV infusion Indication(s) Acute Bacterial Skin and Skin Structure Infection (ABSSSI); Community-acquired Bacterial Pneumonia (CABP) Intended Population(s) Adults ≥ 18 years of age Template Version: March 6, 2009 Reference ID: 2857265 Clinical Review Ariel Ramirez Porcalla, MD, MPH Neil Rellosa, MD NDA 200327: Teflaro (ceftaroline fosamil) Table of Contents 1 RECOMMENDATIONS/RISK BENEFIT ASSESSMENT ......................................... 9 1.1 Recommendation on Regulatory Action ........................................................... 10 1.2 Risk Benefit Assessment.................................................................................. 10 1.3 Recommendations for Postmarketing Risk Evaluation and Mitigation Strategies ........................................................................................................................ -

Ladenburg Thalmann Healthcare Conference
Ladenburg Thalmann Healthcare Conference July 13, 2021 Forward-looking Statements This presentation contains forward-looking statements as defined in the Private Securities Litigation Reform Act of 1995 regarding, among other things, the design, initiation, timing and submission to the U.S. Food and Drug Administration (FDA) of a New Drug Application (NDA) for tebipenem HBr and the potential approval of tebipenem HBr by the FDA; future commercialization, the potential number of patients who could be treated by tebipenem HBr and market demand for tebipenem HBr generally; expected broad access across payer channels for tebipenem HBr; the expected pricing of tebipenem HBr and the anticipated shift in treating patients from intravenous to oral administration; the initiation, timing, progress and results of the Company’s preclinical studies and clinical trials and its research and development programs, including management’s assessment of such results; the direct and indirect impact of the pandemic caused by an outbreak of a new strain of coronavirus on the Company’s business and operations; the timing of the availability of data from the Company’s clinical trials; the timing of the Company’s filings with regulatory agencies; product candidate benefits; competitive position; business strategies; objectives of management; potential growth opportunities; potential market size; reimbursement matters; possible or assumed future results of operations; projected costs; and the Company’s cash forecast and the availability of additional non-dilutive funding from governmental agencies beyond any initially funded awards. In some cases, forward-looking statements can be identified by terms such as “may,” “will,” “should,” “expect,” “plan,” “aim,” “anticipate,” “could,” “intent,” “target,” “project,” “contemplate,” “believe,” “estimate,” “predict,” “potential” or “continue” or the negative of these terms or other similar expressions. -
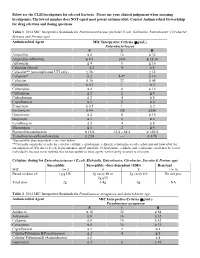
Below Are the CLSI Breakpoints for Selected Bacteria. Please Use Your Clinical Judgement When Assessing Breakpoints
Below are the CLSI breakpoints for selected bacteria. Please use your clinical judgement when assessing breakpoints. The lowest number does NOT equal most potent antimicrobial. Contact Antimicrobial Stewardship for drug selection and dosing questions. Table 1: 2014 MIC Interpretive Standards for Enterobacteriaceae (includes E.coli, Klebsiella, Enterobacter, Citrobacter, Serratia and Proteus spp) Antimicrobial Agent MIC Interpretive Criteria (g/mL) Enterobacteriaceae S I R Ampicillin ≤ 8 16 ≥ 32 Ampicillin-sulbactam ≤ 8/4 16/8 ≥ 32/16 Aztreonam ≤ 4 8 ≥ 16 Cefazolin (blood) ≤ 2 4 ≥ 8 Cefazolin** (uncomplicated UTI only) ≤ 16 ≥ 32 Cefepime* ≤ 2 4-8* ≥ 16 Cefotetan ≤ 16 32 ≥ 64 Ceftaroline ≤ 0.5 1 ≥ 2 Ceftazidime ≤ 4 8 ≥ 16 Ceftriaxone ≤ 1 2 ≥ 4 Cefpodoxime ≤ 2 4 ≥ 8 Ciprofloxacin ≤ 1 2 ≥ 4 Ertapenem ≤ 0.5 1 ≥ 2 Fosfomycin ≤ 64 128 ≥256 Gentamicin ≤ 4 8 ≥ 16 Imipenem ≤ 1 2 ≥ 4 Levofloxacin ≤ 2 4 ≥ 8 Meropenem ≤ 1 2 ≥ 4 Piperacillin-tazobactam ≤ 16/4 32/4 – 64/4 ≥ 128/4 Trimethoprim-sulfamethoxazole ≤ 2/38 --- ≥ 4/76 *Susceptibile dose-dependent – see chart below **Cefazolin can predict results for cefaclor, cefdinir, cefpodoxime, cefprozil, cefuroxime axetil, cephalexin and loracarbef for uncomplicated UTIs due to E.coli, K.pneumoniae, and P.mirabilis. Cefpodoxime, cefinidir, and cefuroxime axetil may be tested individually because some isolated may be susceptible to these agents while testing resistant to cefazolin. Cefepime dosing for Enterobacteriaceae ( E.coli, Klebsiella, Enterobacter, Citrobacter, Serratia & Proteus spp) Susceptible Susceptible –dose-dependent (SDD) Resistant MIC </= 2 4 8 >/= 16 Based on dose of: 1g q12h 1g every 8h or 2g every 8 h Do not give 2g q12 Total dose 2g 3-4g 6g NA Table 2: 2014 MIC Interpretive Standards for Pseudomonas aeruginosa and Acinetobacter spp. -

Principles of Antimicrobial Drugs
Cephalosporins LECTURE 22 DR.SUHEIL DONE BY: 7ALA RAED Cephalosporins Derivatives of 7-aminocephalosporanic acid β- lactam antibiotics, Cidal effect ,Semisynthetic, from funges Broad spectrum Inhibitors of microbial cell wall synthesis (similar way to penicillin) Differ in pharmacokinetic properties and spectrum of activity Classified into 1st 2nd 3rd 4th and 5th generations ركزوا First generation * على الملون بالزهري Cefadroxil Cefalexin Oral Cefazolin IM, IV Cephapirin Cephradine Cephaloridine * Second generation Cefaclor Oral Cephamandole IM, IV ركزوا على الزهري )اﻷصفر الي حكى عنهم الدكتور ( Cephmetazole Cefonicid Cefotetan Cefoxitin Cefprozil Cefuroxime Cefuroxime axetil Loracarbef * Third generation Cefixime Oral Cefoperazone IM, IV Cefdinir Cefpodoxime Cefotaxims Ceftazidime Ceftriaxone Ceftibuten Ceftizoxime * Fourth generation Cefepime IM, IV * Fifth generation Ceftaroline IV 1st generation cephalosporins have the best activity against G+ve microorganisms, less resistant to β- lactamases, and do not cross readily the BBB as compared to 2nd, 3rd and 4h generations Cephalosporins never considered drugs of choice for any infection, however they are highly effective in upper and lower respiratory infection, H. influenza, UTI’s, dental infections, severe systemic infection... كله حفظ يعني ** Among cephalosporins: - Cefoxitin (2nd) has the best activity against Bacteroides fragilis - Cefamandole (2nd) has the best activity against H. influenza - Cefoperazone (3rd), Ceftazidine (3rd) and Cefepime (4th) have the best activity against P. -

Non-Penicillin Beta-Lactam Drugs: a CGMP Framework for Preventing Cross- Contamination
Guidance for Industry Non-Penicillin Beta-Lactam Drugs: A CGMP Framework for Preventing Cross- Contamination U.S. Department of Health and Human Services Food and Drug Administration Center for Drug Evaluation and Research (CDER) April 2013 Current Good Manufacturing Practices (CGMPs) Guidance for Industry Non-Penicillin Beta-Lactam Drugs: A CGMP Framework for Preventing Cross- Contamination Additional copies are available from: Office of Communications Division of Drug Information, WO51, Room 2201 Center for Drug Evaluation and Research Food and Drug Administration 10903 New Hampshire Ave. Silver Spring, MD 20993-0002 Phone: 301-796-3400; Fax: 301-847-8714 [email protected] http://www.fda.gov/Drugs/GuidanceComplianceRegulatoryInformation/Guidances/default.htm U.S. Department of Health and Human Services Food and Drug Administration Center for Drug Evaluation and Research (CDER) April 2013 Current Good Manufacturing Practices (CGMP) Contains Nonbinding Recommendations TABLE OF CONTENTS I. INTRODUCTION....................................................................................................................1 II. BACKGROUND ......................................................................................................................2 III. RECOMMENDATIONS.........................................................................................................7 i Contains Nonbinding Recommendations Guidance for Industry1 Non-Penicillin Beta-Lactam Drugs: A CGMP Framework for Preventing Cross-Contamination This guidance -

The Effects of Combination Antibiotic Therapy on Methicillin-Resistant Staphylococcus Aureus Presented by Kasra Nick Fallah In
View metadata, citation and similar papers at core.ac.uk brought to you by CORE provided by UT Digital Repository The Effects of Combination Antibiotic Therapy on Methicillin-Resistant Staphylococcus aureus Presented by Kasra Nick Fallah in partial fulfillment of the requirements for completion of the Health Science Scholars honors program in the College of Natural Sciences at The University of Texas at Austin Spring 2018 Gregory C. Palmer, Ph.D. Date Supervising Professor Texas Institute for Discovery Education in Science Department of Medical Education Ruth Buskirk, Ph.D. Date Biology Honors Advisor Biological Sciences, College of Natural Sciences Table of Contents Abstract (3) Chapter 1: Literature Review (4) 1.1: The History of Antibiotics (4) 1.1.1: The Discovery of Penicillin (4) 1.1.2: The Different Classes of Antibiotics (7) 1.1.3: The Mechanisms of Action of Antibiotics (13) 1.2: Antibiotic Resistance (16) 1.2.1: The Rise of Antibiotic Resistance (16) 1.2.2: Mechanisms of Resistance (17) 1.2.3: How Antibiotic Resistance Spreads (20) 1.2.4: Methicillin-Resistant Staphylococcus aureus (21) 1.3: Streptomyces (24) 1.3.1: Selman Waksman (24) 1.3.2: Streptomyces: A Possible Solution to Antibiotic Resistance (25) 1.4: Combination Antibiotic Therapy (27) 1.4.1: The Positive/Negative Effects of Combination Antibiotic Therapy (27) 1.4.2: Drug Interactions (29) 1.4.3: Antibiotic Stewardship (30) Chapter 2: Research Manuscript (32) 2.1: Introduction (32) 1 2.2: Methods (35) 2.2.1: Strains, Media, and Growth Conditions (35) 2.2.2: Bacterial Strain Isolation and Identification (35) 2.2.3: Ethyl acetate Extractions (36) 2.2.4: Disc Assays (36) 2.3: Results & Discussion (38) 2.3.1: Isolation of Bacteria (38) 2.3.2: Organic Extractions (41) 2.3.3: Inhibition of MSSA and MRSA (41) 2.3.4: Inhibitory effect of the antibiotic produced by S. -

ARCH-Vet Anresis.Ch
Usage of Antibiotics and Occurrence of Antibiotic Resistance in Bacteria from Humans and Animals in Switzerland Joint report 2013 ARCH-Vet anresis.ch Publishing details © Federal Office of Public Health FOPH Published by: Federal Office of Public Health FOPH Publication date: November 2015 Editors: Federal Office of Public Health FOPH, Division Communicable Diseases. Elisabetta Peduzzi, Judith Klomp, Virginie Masserey Design and layout: diff. Marke & Kommunikation GmbH, Bern FOPH publication number: 2015-OEG-17 Source: SFBL, Distribution of Publications, CH-3003 Bern www.bundespublikationen.admin.ch Order number: 316.402.eng Internet: www.bag.admin.ch/star www.blv.admin.ch/gesundheit_tiere/04661/04666 Table of contents 1 Foreword 4 Vorwort 5 Avant-propos 6 Prefazione 7 2 Summary 10 Zusammenfassung 12 Synthèse 14 Sintesi 17 3 Introduction 20 3.1 Antibiotic resistance 20 3.2 About anresis.ch 20 3.3 About ARCH-Vet 21 3.4 Guidance for readers 21 4 Abbreviations 24 5 Antibacterial consumption in human medicine 26 5.1 Hospital care 26 5.2 Outpatient care 31 5.3 Discussion 32 6 Antibacterial sales in veterinary medicines 36 6.1 Total antibacterial sales for use in animals 36 6.2 Antibacterial sales – pets 37 6.3 Antibacterial sales – food producing animals 38 6.4 Discussion 40 7 Resistance in bacteria from human clinical isolates 42 7.1 Escherichia coli 42 7.2 Klebsiella pneumoniae 44 7.3 Pseudomonas aeruginosa 48 7.4 Acinetobacter spp. 49 7.5 Streptococcus pneumoniae 52 7.6 Enterococci 54 7.7 Staphylococcus aureus 55 Table of contents 1 8 Resistance in zoonotic bacteria 58 8.1 Salmonella spp. -

HKUST 2011 Igem Team
HKUST 2011 iGEM Team E. trojan – Boosting the effectiveness of antibiotics through quorum- sensing disruption INTRODUCTION Mistakes… Penicillin G Amikacin, Gentamicin, Kanamycin, Neomycin, Netilmicin, Tobramycin, Paromomycin, Loracarbef, Ertapenem, Doripenem, Imipenem, Meropenem, Cefadroxil, Cefazolin, Cefalotin, Cefalexin, Cefaclor, Cefamandole, Cefoxitin, Cefprozil, Cefuroxime, Cefixime, Cefdinir, Cefditoren, Cefoperazone, Cefotaxime, Cefpodoxime, Ceftazidime, Ceftibuten, Ceftizoxime, Ceftriaxone, Cefepime, Ceftobiprole, Teicoplanin, Vancomycin, Telavancin, Clindamycin, Lincomycin, Daptomycin, Azithromycin, Clarithromycin, Dirithromycin, Erythromycin, Roxithromycin, Troleandomycin, Telithromycin, Spectinomycin, Aztreonam, Furazolidone, Nitrofurantoin, Amoxicillin, Ampicillin, Azlocillin, Carbenicillin, Cloxacillin, Dicloxacillin, Flucloxacillin, Mezlocillin, Methicillin, Nafcillin, Oxacillin, Penicillin, Piperacillin, Temocillin, Ticarcillin, Bacitracin, Colistin, Polymyxin B … Charity Indole Signalling Rearm Antibiotics ReduceAntibiotic Antibiotic-Free Disruption (T4MO) E. TROJAN SelectionUsage E. CRAFT – AN ALTERNATIVE TRANSFORMATION METHOD Essential- gene- based selection method: E. CRAFT Eschericia coli Re-engineered for Antibiotic- Free Transformation Deletion of an essential gene from E. CRAFT’s genome Addiction to extragenomic source of the gene pCarrier, a heat- insensitive analog of pDummy TRANSFORMATION TRANSFORMATION The selection, comparison between successful and unsuccessful transformation PLASMID SHUFFLING Development -

Vs. Long-Course Antibiotic Treatment for Acute Streptococcal Pharyngitis: Systematic Review and Meta-Analysis of Randomized Controlled Trials
antibiotics Review Short- vs. Long-Course Antibiotic Treatment for Acute Streptococcal Pharyngitis: Systematic Review and Meta-Analysis of Randomized Controlled Trials Anna Engell Holm * , Carl Llor, Lars Bjerrum and Gloria Cordoba Research Unit for General Practice and Section of General Practice, Department of Public Health, Øster Farimagsgade 5, 1014 Copenhagen, Denmark; [email protected] (C.L.); [email protected] (L.B.); [email protected] (G.C.) * Correspondence: [email protected]; Tel.: +45-261-110-54 Received: 9 September 2020; Accepted: 21 October 2020; Published: 26 October 2020 Abstract: BACKGROUND: To evaluate the effectiveness of short courses of antibiotic therapy for patients with acute streptococcal pharyngitis. METHODS: Randomized controlled trials comparing short-course antibiotic therapy ( 5 days) with long-course antibiotic therapy ( 7 days) for patients with ≤ ≥ streptococcal pharyngitis were included. Two primary outcomes: early clinical cure and early bacterial eradication. RESULTS: Fifty randomized clinical trials were included. Overall, short-course antibiotic treatment was as effective as long-course antibiotic treatment for early clinical cure (odds ratio (OR) 0.85; 95% confidence interval (CI) 0.79 to 1.15). Subgroup analysis showed that short-course penicillin was less effective for early clinical cure (OR 0.43; 95% CI, 0.23 to 0.82) and bacteriological eradication (OR 0.34; 95% CI, 0.19 to 0.61) in comparison to long-course penicillin. Short-course macrolides were equally effective, compared to long-course penicillin. Finally, short-course cephalosporin was more effective for early clinical cure (OR 1.48; 95% CI, 1.11 to 1.96) and early microbiological cure (OR 1.60; 95% CI, 1.13 to 2.27) in comparison to long-course penicillin. -

Guidelines for Atcvet Classification 2012
Guidelines for ATCvet classification 2012 ISSN 1020-9891 ISBN 978-82-8082-479-0 Suggested citation: WHO Collaborating Centre for Drug Statistics Methodology, Guidelines for ATCvet classification 2012. Oslo, 2012. © Copyright WHO Collaborating Centre for Drug Statistics Methodology, Oslo, Norway. Use of all or parts of the material requires reference to the WHO Collaborating Centre for Drug Statistics Methodology. Copying and distribution for commercial purposes is not allowed. Changing or manipulating the material is not allowed. Guidelines for ATCvet classification 14th edition WHO Collaborating Centre for Drug Statistics Methodology Norwegian Institute of Public Health P.O.Box 4404 Nydalen N-0403 Oslo Norway Telephone: +47 21078160 Telefax: +47 21078146 E-mail: [email protected] Website: www.whocc.no Previous editions: 1992: Guidelines on ATCvet classification, 1st edition1) 1995: Guidelines on ATCvet classification, 2nd edition1) 1999: Guidelines on ATCvet classification, 3rd edition1) 2002: Guidelines for ATCvet classification, 4th edition2) 2003: Guidelines for ATCvet classification, 5th edition2) 2004: Guidelines for ATCvet classification, 6th edition2) 2005: Guidelines for ATCvet classification, 7th edition2) 2006: Guidelines for ATCvet classification, 8th edition2) 2007: Guidelines for ATCvet classification, 9th edition2) 2008: Guidelines for ATCvet classification, 10th edition2) 2009: Guidelines for ATCvet classification, 11th edition2) 2010: Guidelines for ATCvet classification, 12th edition2) 2011: Guidelines for ATCvet classification, 13th edition2) 1) Published by the Nordic Council on Medicines 2) Published by the WHO Collaborating Centre for Drug Statistics Methodology Preface The Anatomical Therapeutic Chemical classification system for veterinary medicinal products, ATCvet, has been developed by the Nordic Council on Medicines (NLN) in collaboration with the NLN’s ATCvet working group, consisting of experts from the Nordic countries. -

Glycopeptide Antibiotics: Structure and Mechanisms of Action
Journal of Bacteriology and Virology 2015. Vol. 45, No. 2 p.67 – 78 http://dx.doi.org/10.4167/jbv.2015.45.2.67 Review Article Glycopeptide Antibiotics: Structure and Mechanisms of Action * Hee-Kyoung Kang1 and Yoonkyung Park1,2 1Department of Biomedical Sciences, Chosun University, Gwangju; 2Research Center for Proteinaceous Materials, Chosun University, Gwangju, Korea Glycopeptides of the clinically important antibiotic drugs are glycosylated cyclic or polycyclic nonribosomal peptides. Glycopeptides such as vancomycin and teicoplanin are often used for the treatment of gram-positive bacteria in patients. The increased incidence of drug resistance and inadequacy of these therapeutics against gram-positive bacterial infections would be the formation and clinical development of more variable second generation of glycopeptide antibiotics: semisynthetic lipoglycopeptide analogs such as telavancin, dalbavancin, and oritavancin with improved activity and better pharmacokinetic properties. In this review, we describe the development of and bacterial resistance to vancomycin, teicoplanin, and semisynthetic glycopeptides (teicoplanin, dalbavancin, and oritavancin). The clinical influence of resistance to glycopeptides, particularly vancomycin, are also discussed. Key Words: Glycopeptide; Resistance; Vancomycin; Teicoplanin; Dalbavancin (vancomycin-intermediate S. aureus, VISA or glycopeptide- INTRODUCTION intermediate S. aureus, GISA) has caused researchers to develop the second-generation glycopeptides and caused a Glycopeptides are the most prevalent class of thera- flurry of activity targeted at understanding the mechanisms peutics that are used for the treatment against as severe of bacterial resistance and the evolution of glycopeptide infections caused by Gram-positive pathogens, such as antibiotics (1, 2). enterococci, methicillin-resistant Staphylococcus aureus Glycopeptides are glycosylated cyclic or polycyclic non- (MRSA), and Clostridium difficile. -

1 Cephalosporins and Vancomycin
Alice Prince CEPHALOSPORINS AND VANCOMYCIN CEPHALOSPORINS These compounds are closely related in structure, mechanism of action, spectrum of activity and pharmacology to the penicillins. They are produced by fungi and synthetic modification. I. CHEMISTRY Contains 6-membered dihydrothiazine ring. Substitutions at position 3 generally affect pharmacology; substitutions at position 7 affect antibacterial activity, but this is not invariably true. 1 II. MECHANISM OF ACTION Cephalosporins are bactericidal. They inhibit enzymatic reactions necessary for stable bacterial cell walls by binding to PBPs. Bacterial cells must be growing. III. PHARMACOLOGIC PROPERTIES OF CEPHALOSPORINS Peak blood level Percentage Drug (µg/ml) Protein Binding T½ (hr) [CSF] µg/ml Cefazolin 1g 188 70 - 85% 1.4 ---------------- Cefuroxime 1.5g 100 50% 1.3 1.1 - 18 Cefoxitin 1g 110 70% 0.7-0.9 ---------------- Cefotaxime 1g 100 13 - 38% 1.0 6 – 11 (2g)* Ceftriaxone 1g 150 83 - 96% 5.8-8.7 1.3 - 44 Ceftazidime 1g 90 < 10% 1.9 2 – 42 *non-inflamed meninges CSF level 0.01-0.7 µg/ml IV. MECHANISM OF RESISTANCE TO CEPHALOSPORINS A. Failure to reach receptor sites, permeability. B. Destroyed by β-lactamase. Some gram-negative bacteria produce large amounts of β- lactamase constitutively. C. Failure to bind to penicillin binding proteins, in gram negative and gram positive organisms. V. ANTIMICROBIAL ACTIVITY The cephalosporins have been grouped into "generations" corresponding to their development by the pharmaceutical industry in response to clinical needs. In general, the later generations of cephalosporins have greater gram-negative activity at the expense of gram-positive activity. A. First generation agents Cefazolin Cephalothin Cephalexin (oral) Cefaclor (oral) All of these drugs inhibit gram-positive cocci (S.