Non-Specific Immunity Defense Mechanisms First Line of Defense
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Guidelines on the Diagnosis and Management of Pericardial
European Heart Journal (2004) Ã, 1–28 ESC Guidelines Guidelines on the Diagnosis and Management of Pericardial Diseases Full Text The Task Force on the Diagnosis and Management of Pericardial Diseases of the European Society of Cardiology Task Force members, Bernhard Maisch, Chairperson* (Germany), Petar M. Seferovic (Serbia and Montenegro), Arsen D. Ristic (Serbia and Montenegro), Raimund Erbel (Germany), Reiner Rienmuller€ (Austria), Yehuda Adler (Israel), Witold Z. Tomkowski (Poland), Gaetano Thiene (Italy), Magdi H. Yacoub (UK) ESC Committee for Practice Guidelines (CPG), Silvia G. Priori (Chairperson) (Italy), Maria Angeles Alonso Garcia (Spain), Jean-Jacques Blanc (France), Andrzej Budaj (Poland), Martin Cowie (UK), Veronica Dean (France), Jaap Deckers (The Netherlands), Enrique Fernandez Burgos (Spain), John Lekakis (Greece), Bertil Lindahl (Sweden), Gianfranco Mazzotta (Italy), Joa~o Morais (Portugal), Ali Oto (Turkey), Otto A. Smiseth (Norway) Document Reviewers, Gianfranco Mazzotta, CPG Review Coordinator (Italy), Jean Acar (France), Eloisa Arbustini (Italy), Anton E. Becker (The Netherlands), Giacomo Chiaranda (Italy), Yonathan Hasin (Israel), Rolf Jenni (Switzerland), Werner Klein (Austria), Irene Lang (Austria), Thomas F. Luscher€ (Switzerland), Fausto J. Pinto (Portugal), Ralph Shabetai (USA), Maarten L. Simoons (The Netherlands), Jordi Soler Soler (Spain), David H. Spodick (USA) Table of contents Constrictive pericarditis . 9 Pericardial cysts . 13 Preamble . 2 Specific forms of pericarditis . 13 Introduction. 2 Viral pericarditis . 13 Aetiology and classification of pericardial disease. 2 Bacterial pericarditis . 14 Pericardial syndromes . ..................... 2 Tuberculous pericarditis . 14 Congenital defects of the pericardium . 2 Pericarditis in renal failure . 16 Acute pericarditis . 2 Autoreactive pericarditis and pericardial Chronic pericarditis . 6 involvement in systemic autoimmune Recurrent pericarditis . 6 diseases . 16 Pericardial effusion and cardiac tamponade . -

WHITE BLOOD CELLS Formation Function ~ TEST YOURSELF
Chapter 9 Blood, Lymph, and Immunity 231 WHITE BLOOD CELLS All white blood cells develop in the bone marrow except Any nucleated cell normally found in blood is a white blood for some lymphocytes (they start out in bone marrow but cell. White blood cells are also known as WBCs or leukocytes. develop elsewhere). At the beginning of leukopoiesis all the When white blood cells accumulate in one place, they grossly immature white blood cells look alike even though they're appear white or cream-colored. For example, pus is an accu- already committed to a specific cell line. It's not until the mulation of white blood cells. Mature white blood cells are cells start developing some of their unique characteristics larger than mature red blood cells. that we can tell them apart. There are five types of white blood cells. They are neu- Function trophils, eosinophils, basophils, monocytes and lymphocytes (Table 9-2). The function of all white blood cells is to provide a defense White blood cells can be classified in three different ways: for the body against foreign invaders. Each type of white 1. Type of defense function blood cell has its own unique role in this defense. If all the • Phagocytosis: neutrophils, eosinophils, basophils, mono- white blood cells are functioning properly, an animal has a cytes good chance of remaining healthy. Individual white blood • Antibody production and cellular immunity: lympho- cell functions will be discussed with each cell type (see cytes Table 9-2). 2. Shape of nucleus In providing defense against foreign invaders, the white • Polymorphonuclear (multilobed, segmented nucleus): blood cells do their jobs primarily out in the tissues. -

Automatic System for Differential Blood Counting
ISSN (Print) : 2320 – 3765 ISSN (Online): 2278 – 8875 International Journal of Advanced Research in Electrical, Electronics and Instrumentation Engineering (An ISO 3297: 2007 Certified Organization) Vol. 5, Issue 4, April 2016 Automatic System for Differential Blood Counting 1 2 Manisha Shirvoikar , Dr.H.G.Virani PG Student [ECI], Dept. of ETC, Goa College of Engineering, Ponda, Goa, India1 Professor & Head of Department, Dept. of ETC, Goa College of Engineering, Ponda, Goa, India2 ABSTRACT: For detecting various diseases, Doctor first suggests the patient to undergo blood test which is used as a health indicator. Differential Blood Count (DBC) provides haematologist with valuable information about health of the patient. DBC determines the percentage of types of WBC this is important because it give exact count of five types of WBC such as neutrophil, lymphocyte, monocyte, eosinophil and basophile. Increase or decrease of DBC than the ideal count indicated that our body is not healthy. Precise counting of type of WBC is very important. Manual counting of White blood cells is time consuming and can lead to human error with increase in number of samples. Automatic cell counter sometimes misclassifies the cells having different morphology. Even they are very expensive and unaffordable by remote area health centres and hospitals. These problems are overcome by developing a system which is image based, cost effective, fast and accurate which has the capability to identify, classify the different type of white blood cell and perform DBC. Implementation is done using MATLABR2014b. KEYWORDS: MATLAB, peripheral blood smear, RBC, Thresholding, WBC, DBC. I.INTRODUCTION Total volume of blood in human is 5-6 litres i.e 8% of body weight or 80 mL/kg body weight. -

NLRP3 Inflammasome Cutting Edge
Cutting Edge: Nitric Oxide Inhibits the NLRP3 Inflammasome Eduardo Hernandez-Cuellar, Kohsuke Tsuchiya, Hideki Hara, Rendong Fang, Shunsuke Sakai, Ikuo Kawamura, This information is current as Shizuo Akira and Masao Mitsuyama of September 25, 2021. J Immunol published online 24 October 2012 http://www.jimmunol.org/content/early/2012/10/24/jimmun ol.1202479 Downloaded from Supplementary http://www.jimmunol.org/content/suppl/2012/10/24/jimmunol.120247 Material 9.DC1 http://www.jimmunol.org/ Why The JI? Submit online. • Rapid Reviews! 30 days* from submission to initial decision • No Triage! Every submission reviewed by practicing scientists • Fast Publication! 4 weeks from acceptance to publication by guest on September 25, 2021 *average Subscription Information about subscribing to The Journal of Immunology is online at: http://jimmunol.org/subscription Permissions Submit copyright permission requests at: http://www.aai.org/About/Publications/JI/copyright.html Email Alerts Receive free email-alerts when new articles cite this article. Sign up at: http://jimmunol.org/alerts The Journal of Immunology is published twice each month by The American Association of Immunologists, Inc., 1451 Rockville Pike, Suite 650, Rockville, MD 20852 Copyright © 2012 by The American Association of Immunologists, Inc. All rights reserved. Print ISSN: 0022-1767 Online ISSN: 1550-6606. Published October 24, 2012, doi:10.4049/jimmunol.1202479 Cutting Edge: Nitric Oxide Inhibits the NLRP3 Inflammasome Eduardo Hernandez-Cuellar,*,† Kohsuke Tsuchiya,* Hideki Hara,* Rendong Fang,* Shunsuke Sakai,* Ikuo Kawamura,* Shizuo Akira,† and Masao Mitsuyama* Although the NLRP3 inflammasome plays a pivotal role in that NLRP3 inflammasome contributes to host defense against host defense, its uncontrolled activation is associated with microbialpathogens,excessiveactivationduetomutationsinthe inflammatory disorders, suggesting that regulation of the NLRP3 gene has been associated with a spectrum of autoin- inflammasome is important to prevent detrimental effects. -

Phagocytosis References
9025 Technology Dr. Fishers, IN 46038 • www.bangslabs.com • [email protected] • 800.387.0672 PHAGOCYTOSIS REFERENCES GENERAL BEAD SELECTION & PHAGOCYTOSIS RATES Thiele L, Diederichs JE, Reszka R, Merkle HP, Walter E. (2003) Competitive adsorption of serum proteins at microparticles affects phagocytosis by dendritic cells. Biomaterials; 24(8):1409-18. (1µm Polybead® and Fluoresbrite® Carboxylate microspheres) Ahsan F, Rivas IP, Khan MA, Torres Suarez AI. (2002) Targeting to macrophages: role of physicochemical properties of particulate carriers-- liposomes and microspheres--on the phagocytosis by macrophages. J Controlled Release; 79:29-40. Thiele L, Rothen-Rutishauser B, Jilek S, Wunderli-Allenspach H, Merkle HP, Walter E. (2001) Evaluation of particle uptake in human blood monocyte-derived cells in vitro. Does phagocytosis activity of dendritic cells measure up with macrophages? J Controlled Release; 76:59-71. Koval M, Preiter K, Adles C, Stahl PD, Steinberg TH. (1998) Size of IgG-opsonized particles determines macrophage response during internalization. Exp Cell Res; 242(1):265-73. (0.2-0.3µm Polybead® microspheres; trypan blue quenching) Tabata Y, Ikada Y. (1988) Effect of the size and surface charge of polymer microspheres on their phagocytosis by macrophage. Biomaterials; 9(4):356-62. MONOCYTES Gu BJ, Duce JA, Valova VA, Wong B, Bush AI, Petrou S, Wiley JS. (2012) P2X7 receptor-mediated scavenger activity of mononuclear phagocytes toward non-opsonized particles and apoptotic cells is inhibited by serum glycoproteins but remains active in cerebrospinal fluid.Journal of Biological Chemistry. May 18;287:17318-30. (1µm Fluoresbrite® YG microspheres) Dumrese C, Slomianka L, Ziegler U, Choi SS, Kalia A, Fulurija A, Lu W, Berg DE, Benghezal M, Marshall B, Mittl PR. -

Digitalcommons@UNMC Granulocytopenia
University of Nebraska Medical Center DigitalCommons@UNMC MD Theses Special Collections 5-1-1936 Granulocytopenia Howard E. Mitchell University of Nebraska Medical Center This manuscript is historical in nature and may not reflect current medical research and practice. Search PubMed for current research. Follow this and additional works at: https://digitalcommons.unmc.edu/mdtheses Part of the Medical Education Commons Recommended Citation Mitchell, Howard E., "Granulocytopenia" (1936). MD Theses. 457. https://digitalcommons.unmc.edu/mdtheses/457 This Thesis is brought to you for free and open access by the Special Collections at DigitalCommons@UNMC. It has been accepted for inclusion in MD Theses by an authorized administrator of DigitalCommons@UNMC. For more information, please contact [email protected]. G PA~lULOCYTOPENI A SENIOR THESIS By Howard E. Mitchell April 17, 1936 TABLE OF CONT'ENTS Introduction Definition • · 1 History . • • • 1 Nomenclature • • • • • 4 ClassificBtion • • • • 6 Physiology • • • • .10 Etiology • • 22 Geographic Distribution • 23 Age, Sex, and R9ce • • ·• 23 Occupation • .. • • • • .. • 23 Ba.cteria • • • • .. 24 Glandu18.r Dysfunction • • • 27 Radiation • • • • 28 Allergy • • • 28 Chemotactic and Maturation Factors • • 28 Chemicals • • • • • 30 Pathology • • • • • 36 Symptoms • • • • • • • 43 DiEtgnosis • • • • • .. • • • • • .. • 4'7 Prognosis 48 '" • • • • • • • • • • • • Treatment • • • • • • • • 49 Non"'specific Therapy • • • • .. 50 Transfusion • • • • .. 51 X-Ray • • • • • • • • • 52 Liver ·Extract • • • • • • • 53 Nucleotides • • • • • • • • • • • 53 General Ca.re • • • • • • • • 57 Conclusion • • • • • • • • • 58 480805 INTHODUCTION Although t~ere is reference in literature of the Nineteenth Century to syndromes similating the disease (granulocytopenia) 9.8 W(~ know it todes, it "vas not un til the year 1922 that Schultz 8ctually described his C8se as a disease entity and by so doing, stimulated the interest of tne medical profession to further in vestigation. -
Instant Notes: Immunology, Second Edition
Immunology Second Edition The INSTANT NOTES series Series Editor: B.D. Hames School of Biochemistry and Molecular Biology, University of Leeds, Leeds, UK Animal Biology 2nd edition Biochemistry 2nd edition Bioinformatics Chemistry for Biologists 2nd edition Developmental Biology Ecology 2nd edition Immunology 2nd edition Genetics 2nd edition Microbiology 2nd edition Molecular Biology 2nd edition Neuroscience Plant Biology Chemistry series Consulting Editor: Howard Stanbury Analytical Chemistry Inorganic Chemistry 2nd edition Medicinal Chemistry Organic Chemistry 2nd edition Physical Chemistry Psychology series Sub-series Editor: Hugh Wagner Dept of Psychology, University of Central Lancashire, Preston, UK Psychology Cognitive Psychology Forthcoming title Physiological Psychology Immunology Second Edition P.M. Lydyard Department of Immunology and Molecular Pathology, Royal Free and University College Medical School, University College London, London, UK A. Whelan Department of Immunology, Trinity College and St James’ Hospital, Dublin, Ireland and M.W. Fanger Department of Microbiology and Immunology, Dartmouth Medical School, Lebanon, New Hampshire, USA © Garland Science/BIOS Scientific Publishers Limited, 2004 First published 2000 This edition published in the Taylor & Francis e-Library, 2005. “To purchase your own copy of this or any of Taylor & Francis or Routledge’s collection of thousands of eBooks please go to www.eBookstore.tandf.co.uk.” Second edition published 2004 All rights reserved. No part of this book may be reproduced or -

Ingenuity Pathway Analysis of Human Facet Joint Tissues: Insight Into Facet Joint Osteoarthritis
EXPERIMENTAL AND THERAPEUTIC MEDICINE 19: 2997-3008, 2020 Ingenuity pathway analysis of human facet joint tissues: Insight into facet joint osteoarthritis CHU CHEN*, SHENGYU CUI*, WEIDONG LI, HURICHA JIN, JIANBO FAN, YUYU SUN and ZHIMING CUI Department of Spine Surgery, The Second Affiliated Hospital of Nantong University, Nantong, Jiangsu 226001, P.R. China Received August 17, 2019; Accepted January 30, 2020 DOI: 10.3892/etm.2020.8555 Abstract. Facet joint osteoarthritis (FJOA) is a common the top 5 IPA networks (with a score >30). The present study degenerative joint disorder with high prevalence in the elderly. provides insight into the pathological processes of FJOA from FJOA causes lower back pain and lower extremity pain, and a genetic perspective and may thus benefit the clinical treat- thus severely impacts the quality of life of affected patients. ment of FJOA. Emerging studies have focused on the histomorphological and histomorphometric changes in FJOA. However, the dynamic Introduction genetic changes in FJOA have remained to be clearly deter- mined. In the present study, previously obtained RNA deep Facet joint osteoarthritis (FJOA) is a common degenerative sequencing data were subjected to an ingenuity pathway joint disorder that causes the degeneration and breakdown analysis (IPA) and canonical signaling pathways of differ- of cartilage and restricts the movement of joints (1). It has entially expressed genes (DEGs) in FJOA were studied. The been reported that lumbar FJOA occurs at high prevalence top 25 enriched canonical signaling pathways were identified and the presence of FJOA is highly associated with age (2,3). and canonical signaling pathways with high absolute values A community-based cross-sectional study indicated that of z-scores, specifically leukocyte extravasation signaling, in populations aged <50 years, the prevalence of FJOA was Tec kinase signaling and osteoarthritis pathway, were inves- <45%, while it was ~75% in populations aged >50 years (4). -

Simplified White Blood Cell Differential: an Inexpensive, Smartphone- and Paper-Based Blood Cell Count
Simplified White Blood Cell Differential: An Inexpensive, Smartphone- and Paper-Based Blood Cell Count Item Type Article Authors Bills, Matthew V.; Nguyen, Brandon T.; Yoon, Jeong-Yeol Citation M. V. Bills, B. T. Nguyen and J. Yoon, "Simplified White Blood Cell Differential: An Inexpensive, Smartphone- and Paper-Based Blood Cell Count," in IEEE Sensors Journal, vol. 19, no. 18, pp. 7822-7828, 15 Sept.15, 2019. doi: 10.1109/JSEN.2019.2920235 DOI 10.1109/jsen.2019.2920235 Publisher IEEE-INST ELECTRICAL ELECTRONICS ENGINEERS INC Journal IEEE SENSORS JOURNAL Rights © 2019 IEEE. Download date 25/09/2021 12:19:07 Item License http://rightsstatements.org/vocab/InC/1.0/ Version Final accepted manuscript Link to Item http://hdl.handle.net/10150/634549 > REPLACE THIS LINE WITH YOUR PAPER IDENTIFICATION NUMBER (DOUBLE-CLICK HERE TO EDIT) < 1 Simplified White Blood Cell Differential: An Inexpensive, Smartphone- and Paper-Based Blood Cell Count Matthew V. Bills, Brandon T. Nguyen, and Jeong-Yeol Yoon or trained lab specialist to prepare blood smear slides, stain Abstract— Sorting and measuring blood by cell type is them, and then manually count different WBC types using a extremely valuable clinically and provides physicians with key hemocytometer under a microscope [3]. To do this they must information for diagnosing many different disease states dilute specimens in a red blood cell (RBC) lysing solution to including: leukemia, autoimmune disorders, bacterial infections, remove RBCs and count WBCs. Manually counting WBCs is etc. Despite the value, the present methods are unnecessarily laborious and requires specialized medical equipment and costly and inhibitive particularly in resource poor settings, as they require multiple steps of reagent and/or dye additions and trained personnel. -

Cd47-Sirpα Interaction and IL-10 Constrain Inflammation-Induced Macrophage Phagocytosis of Healthy Self-Cells
Cd47-Sirpα interaction and IL-10 constrain inflammation-induced macrophage phagocytosis of healthy self-cells Zhen Biana,b, Lei Shia, Ya-Lan Guoa, Zhiyuan Lva, Cong Tanga, Shuo Niua, Alexandra Tremblaya, Mahathi Venkataramania, Courtney Culpeppera, Limin Lib, Zhen Zhoub, Ahmed Mansoura, Yongliang Zhangc, Andrew Gewirtzd, Koby Kiddera,e, Ke Zenb, and Yuan Liua,d,1 aProgram of Immunology and Cell Biology, Department of Biology, Center for Diagnostics & Therapeutics, Georgia State University, Atlanta, GA 30302; bState Key Laboratory of Pharmaceutical Biotechnology, Nanjing Advanced Institute for Life Sciences, Nanjing University, Nanjing, Jiangsu 210093, China; cDepartment of Microbiology and Immunology, Yong Loo Lin School of Medicine, Life Science Institute (LSI) Immunology Programme, National University of Singapore, Singapore 117456; dCenter for Inflammation, Immunity and Infection, Georgia State University, Atlanta, GA 30303; and eDepartment of Cell Biology, Rutgers University, New Brunswick, NJ 08901 Edited by Jason G. Cyster, University of California, San Francisco, CA, and approved July 11, 2016 (received for review October 28, 2015) − − Rapid clearance of adoptively transferred Cd47-null (Cd47 / ) cells in The CD47-SIRPα mechanism was first reported by Oldenborg congeneic WT mice suggests a critical self-recognition mechanism, et al. (1), who had demonstrated in red blood cell (RBC) in which CD47 is the ubiquitous marker of self, and its interaction transfusion experiments that WT mice rapidly eliminate syngeneic − with macrophage signal regulatory protein α (SIRPα) triggers inhib- Cd47-null (Cd47 ) RBCs through erythrophagocytosis in the itory signaling through SIRPα cytoplasmic immunoreceptor tyrosine- spleen and that the lack of tyrosine phosphorylation in SIRPα based inhibition motifs and tyrosine phosphatase SHP-1/2. -

Quantitative Studies of the Inflammatory Process in Fatal Viral Meningoencephalitis
Quantitative Studies of the Inflammatory Process in Fatal Viral Meningoencephalitis P. C. Doherty, MVSc, PhD The pathogenesis of acute meningoencephalitis induced in adult mice by in- travenous inoculation with Semliki Forest virus has been assessed by counting cells in cerebrospinal fluid (CSF). Meningitis was first apparent on day 4 and, by the time that animals were moribund 2 days later, each microliter of CSF contained in excess of 10,000 mononuclear cells. The following conclusions were made concerning this very considerable inflammatory response: a) Complete suppression of cellular infiltration makes no difference to the clinical disease. b) No correlation is apparent between inflammation and levels of circulating antibody. c) Participation of thymus-derived lymphocytes (T cells) is essential for full expression, though not for initiation, of cellular invasion. d) There is evidently no requirement for lymphocytes recently derived from thymus or for any humoral factor secreted by thymus tissue. e) T cells entering the recirculating pool more than 6 weeks or less than about 1 week prior to inoculation of virus are equally effective in promoting inflammation. f) The T cells apparently act directly by enhancing infiltration of other blood-borne mononuclears into the brain and CSF (Am J Pathol 73:607-622, 1973). A PROTECTIVE ROLE for the inflammatory response has been clearly demonstrated in several acute infectious diseases. The marked cellular infiltration occurring in ectromelia 1,2 and listeriosis 3'4 is associated with elimination of the parasite from the liver and sur- vival of the host. Inflammation is implicated in reducing virus titers in the nonfatal meningoencephalitis caused by intracerebral injec- tion of Sindbis virus." In a few conditions, however, the overall effect of the inflammatory process is deleterious. -
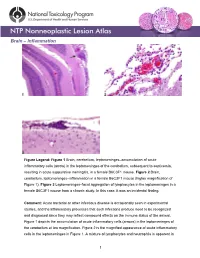
Brain – Inflammation
Brain – Inflammation Figure Legend: Figure 1 Brain, cerebellum, leptomeninges–accumulation of acute inflammatory cells (arrow) in the leptomeninges of the cerebellum, subsequent to septicemia, resulting in acute suppurative meningitis, in a female B6C3F1 mouse. Figure 2 Brain, cerebellum, leptomeninges–inflammation in a female B6C3F1 mouse (higher magnification of Figure 1). Figure 3 Leptomeninges–focal aggregation of lymphocytes in the leptomeninges in a female B6C3F1 mouse from a chronic study. In this case, it was an incidental finding. Comment: Acute bacterial or other infectious disease is occasionally seen in experimental studies, and the inflammatory processes that such infections produce need to be recognized and diagnosed since they may reflect compound effects on the immune status of the animal. Figure 1 depicts the accumulation of acute inflammatory cells (arrows) in the leptomeninges of the cerebellum at low magnification. Figure 2 is the magnified appearance of acute inflammatory cells in the leptomeninges in Figure 1. A mixture of lymphocytes and neutrophils is apparent in 1 Brain – Inflammation this exudate. Figure 3 shows the focal aggregation of lymphocytes in the leptomeninges of a mouse. In this case, it was an incidental finding. The occurrence of such a lesion may, however, indicate a response to a recent viral infection in the nervous system. Occasionally, a small, apparently inert cluster of mononuclear cells without any other reactive responses in the vicinity may be referred to as inflammatory infiltrate. However, the presence of neutrophils should alert the pathologist to conduct a diligent evaluation for other complementary signs of inflammation. In NTP studies, there are five standard categories of inflammation: acute, suppurative, chronic, chronic-active, and granulomatous.