Differentiating Common from Uncommon Pediatric Joint Pain
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Netter's Musculoskeletal Flash Cards, 1E
Netter’s Musculoskeletal Flash Cards Jennifer Hart, PA-C, ATC Mark D. Miller, MD University of Virginia This page intentionally left blank Preface In a world dominated by electronics and gadgetry, learning from fl ash cards remains a reassuringly “tried and true” method of building knowledge. They taught us subtraction and multiplication tables when we were young, and here we use them to navigate the basics of musculoskeletal medicine. Netter illustrations are supplemented with clinical, radiographic, and arthroscopic images to review the most common musculoskeletal diseases. These cards provide the user with a steadfast tool for the very best kind of learning—that which is self directed. “Learning is not attained by chance, it must be sought for with ardor and attended to with diligence.” —Abigail Adams (1744–1818) “It’s that moment of dawning comprehension I live for!” —Calvin (Calvin and Hobbes) Jennifer Hart, PA-C, ATC Mark D. Miller, MD Netter’s Musculoskeletal Flash Cards 1600 John F. Kennedy Blvd. Ste 1800 Philadelphia, PA 19103-2899 NETTER’S MUSCULOSKELETAL FLASH CARDS ISBN: 978-1-4160-4630-1 Copyright © 2008 by Saunders, an imprint of Elsevier Inc. All rights reserved. No part of this book may be produced or transmitted in any form or by any means, electronic or mechanical, including photocopying, recording or any information storage and retrieval system, without permission in writing from the publishers. Permissions for Netter Art figures may be sought directly from Elsevier’s Health Science Licensing Department in Philadelphia PA, USA: phone 1-800-523-1649, ext. 3276 or (215) 239-3276; or e-mail [email protected]. -

Elbow Arthroscopy for Osteochondral Lesions in Athletes
SPORTS SURGERY ELBOW ARTHROSCOPY FOR OSTEOCHONDRAL LESIONS IN ATHLETES – Written by Luigi Pederzini et al, Italy Several sports specific injuries of the elbow OSTEOCHONDRAL DEFECT have been well-described. For example, Definition and symptoms the prevalence of medial elbow instability Osteochondral defect is a detachment is high in throwing athletes such as of bone and cartilage in a joint that can Osteochondral baseball players. Similarly, javelin throwers, cause pain. The clinical presentation defect is a volleyball players and tennis players are is characterised by an acute or chronic frequently complaining about elbow pain. onset of symptoms. The majority of detachment of This can be the result of intensive training patients with osteochondral defects of or chronic overuse which results in an the elbow complain of pain. In some bone and cartilage acute or chronic injury. Some of these patients the defect is associated with injuries can be osteochondral lesions such a loose body, and the patient presents in a joint that as osteochondral defects, osteochondrosis clinically with pain, giving way, swelling, can cause pain... of the capitulum humeri or osteochondritis catching, clicking, crepitus and elbow dissecans (OCD). stiffness aggravated by joint movements. characterised Standard X-rays are the initial studies of choice, but sometimes are negative. by an acute or Magnetic resonance imaging (MRI) and 3D computed tomography (CT) scan can chronic onset of be extremely useful in establishing an symptoms. accurate diagnosis and to add in pre- operative planning. 210 OSTEOCHONDROSIS OF CAPITULUM HUMERI (PANNER’S DISEASE) Definition and symptoms Panner’s disease, an ostechondrosis of the capitellum, is a rare disorder that usually affects the dominant elbow in individuals younger than 10 years old. -

SAS Journal of Surgery (SASJS) Panner's Disease: About a Case
SAS Journal of Surgery (SASJS) ISSN 2454-5104 Abbreviated Key Title: SAS J. Surg. ©Scholars Academic and Scientific Publishers (SAS Publishers) A Unit of Scholars Academic and Scientific Society, India Panner's Disease: About A Case Mohamed Ben-Aissi1, Redouane Hani1, Mohammed Kadiri1, Mouad Beqqali-Hassani1, Paolo Palmari2, Moncef Boufettal1, Mohamed Kharmaz1, Moulay Omar Lamrani1, Ahmed El Bardouni1, Mustapha Mahfoud1, Mohamed Saleh Berrada1 1Orthopedic surgery and traumatology department, Ibn Sina Hospital, Rabat, Morocco 2Orthopedic surgery and traumatology departemnt, Robert Ballanger Hospital, Paris, France Abstract: Panner's disease, or osteochondrosis of the lateral condylar nucleus, is an Case Report avascular necrosis leading to subchondral bone loss, it was first described in 1927. We report a case of Panner's disease, which has been evolving since 1 month, in a child of 8 *Corresponding author years sportsman practicing karate. The evolution was favorable with restitution ad Mohamed Ben-Aissi integrum in 8 months after a short anti-inflammatory treatment and a sports rest of 3 months, without any immobilization of the neither elbow nor surgical intervention. Article History Keywords: Osteochondrosis, Panner’s disease, Treatment. Received: 03.10.2018 Accepted: 06.10.2018 INTRODUCTION Published: 30.10.2018 Panner's disease, or osteochondrosis of the lateral condylar nucleus, is an avascular necrosis leading to a loss of subchondral bone fissuring the radio-humeral DOI: articular surfaces, occurring in the hyperspottive child, in connection with an overuse of 10.21276/sasjs.2018.4.10.7 the elbow [1, 2]. It was first described in 1927 by Dane Panner, a Danish orthopedic surgeon [2, 3]. -

Physical Esxam
Pearls in the Musculoskeletal Exam Frank Caruso MPS, PA-C, EMT-P Skin, Bones, Hearts & Private Parts 2019 Examination Key Points • Area that needs to be examined, gown your patients - well exposed • Understand normal functional anatomy • Observe normal activity • Palpation • Range of Motion • Strength/neuro-vascular assessment • Special Tests General Exam Musculoskeletal Overview Physical Exam Preview Watch Your Patients Walk!! Inspection • Posture – Erectness – Symmetry – Alignment • Skin and subcutaneous tissues – Swelling – Redness – Masses Inspection • Extremities – Size – Deformities – Enlargement – Alignment – Contour – Symmetry Inspection • Muscles – Bilateral symmetry – Hypertrophy – Atrophy – Fasciculations – Spasms Palpation • Palpate bones, joints, and surrounding muscles for the following: – Heat – Tenderness – Swelling – Fluctuation – Crepitus – Resistance to pressure – Muscle tone Muscles • Size and strength affected by the following: – Genetics – Exercise – Nutrition • Muscles move joints through range of motion (ROM). Muscle Strength • Compare bilateral muscles – Strength – Symmetry – Equality – Resistance End Feel Think About It!! • The sensation the examiner feels in the joint as it reaches the end of the range of motion of each passive movement • Bone to bone: This is hard, unyielding – normal would be elbow extension. • Soft–tissue approximation: yielding compression that stops further movement – elbow and knee flexion. End Feel • Tissue stretch: hard – springy type of movement with a slight give – toward the end of range of motion – most common type of normal end feel : knee extension and metacarpophalangeal joint extension. Abnormal End Feel • Muscle spasm: invoked by movement with a sudden dramatic arrest of movement often accompanied by pain - sudden hard – “vibrant twang” • Capsular: Similar to tissue stretch but it does not occur where one would expect – range of motion usually reduced. -
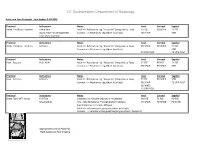

Pediatric MSK Protocols
UT Southwestern Department of Radiology Ankle and Foot Protocols - Last Update 5-18-2015 Protocol Indications Notes Axial Coronal Sagittal Ankle / Midfoot - Routine Ankle Pain Axial = In Relation to Leg "Footprint" (Long Axis to Foot) T1 FSE PD SPAIR T1 FSE Injury, Internal Derangement Coronal = In Relation to Leg (Short Axis Foot) PD SPAIR STIR Talar OCD, Coalition Protocol Indications Notes Axial Coronal Sagittal Ankle / Midfoot - Arthritis Arthritis Axial = In Relation to Leg "Footprint" (Long Axis to Foot) PD SPAIR PD SPAIR T1 FSE Coronal = In Relation to Leg (Short Axis Foot) STIR T1 SPIR POST T1 SPIR POST Protocol Indications Notes Axial Coronal Sagittal Foot - Routine Pain, AVN Axial = In Relation to Leg "Footprint" (Long Axis to Foot) T1 FSE PD FSE T1 FSE Coronal = In Relation to Leg (Short Axis Foot) PD SPAIR PD SPAIR STIR Protocol Indications Notes Axial Coronal Sagittal Foot - Arthritis Arthritis Axial = In Relation to Leg "Footprint" (Long Axis to Foot) T1 FSE PD SPAIR STIR Coronal = In Relation to Leg (Short Axis Foot) PD SPAIR T1 SPIR POST 3D WATS T1 SPIR POST Protocol Indications Notes Axial Coronal Sagittal Great Toe / MTP Joints Turf Toe Smallest Coil Possible (Microcoil if Available) PD FSE T1 FSE PD FSE Sesamoiditis FoV = Mid Metatarsal Through Distal Phalanges PD SPAIR PD SPAIR PD SPAIR Slice thickness = 2-3 mm, 10% gap Axial = In relation to the great toe (short axis foot) Coronal = In relation to the great toe (long axis foot / footprint) Appropriate Coronal Plane for Both Ankle and Foot Imaging UT Southwestern Department -
Musculoskeletal Clinical Vignettes a Case Based Text
Leading the world to better health MUSCULOSKELETAL CLINICAL VIGNETTES A CASE BASED TEXT Department of Orthopaedic Surgery, RCSI Department of General Practice, RCSI Department of Rheumatology, Beaumont Hospital O’Byrne J, Downey R, Feeley R, Kelly M, Tiedt L, O’Byrne J, Murphy M, Stuart E, Kearns G. (2019) Musculoskeletal clinical vignettes: a case based text. Dublin, Ireland: RCSI. ISBN: 978-0-9926911-8-9 Image attribution: istock.com/mashuk CC Licence by NC-SA MUSCULOSKELETAL CLINICAL VIGNETTES Incorporating history, examination, investigations and management of commonly presenting musculoskeletal conditions 1131 Department of Orthopaedic Surgery, RCSI Prof. John O'Byrne Department of Orthopaedic Surgery, RCSI Dr. Richie Downey Prof. John O'Byrne Mr. Iain Feeley Dr. Richie Downey Dr. Martin Kelly Mr. Iain Feeley Dr. Lauren Tiedt Dr. Martin Kelly Department of General Practice, RCSI Dr. Lauren Tiedt Dr. Mark Murphy Department of General Practice, RCSI Dr Ellen Stuart Dr. Mark Murphy Department of Rheumatology, Beaumont Hospital Dr Ellen Stuart Dr Grainne Kearns Department of Rheumatology, Beaumont Hospital Dr Grainne Kearns 2 2 Department of Orthopaedic Surgery, RCSI Prof. John O'Byrne Department of Orthopaedic Surgery, RCSI Dr. Richie Downey TABLE OF CONTENTS Prof. John O'Byrne Mr. Iain Feeley Introduction ............................................................. 5 Dr. Richie Downey Dr. Martin Kelly General guidelines for musculoskeletal physical Mr. Iain Feeley examination of all joints .................................................. 6 Dr. Lauren Tiedt Dr. Martin Kelly Upper limb ............................................................. 10 Department of General Practice, RCSI Example of an upper limb joint examination ................. 11 Dr. Lauren Tiedt Shoulder osteoarthritis ................................................. 13 Dr. Mark Murphy Adhesive capsulitis (frozen shoulder) ............................ 16 Department of General Practice, RCSI Dr Ellen Stuart Shoulder rotator cuff pathology ................................... -

SPR 2015 the Good, the Bad and the Ugly
SPR 2015 The Good, the Bad and the Ugly Diego Jaramillo, M.D., M.P.H. Department of Radiology Children’s Hospital of Philadelphia University of Pennsylvania Pearlman School of Medicine Variants, small abnormalities, and disease are closelyo related Little holes in the humeral head? Developmental proximal humeral cyst Posterior, adjacent to union between greater and lesser tuberosity Cyst related to rotator cuff injury (courtesy of Tal Laor, MD) • Anterior, adjacent to footprint (insertion) Intertuberosity Cysts vs. Rotator Cuff Cyts Intertuberosity Rotator Cuff Cysts Cysts Age (yr) <15 >10 Location Posterior Anterior Rotator Cuff Not usually Yes Disease Little hole in the capitellum? Osteochondral injury with loose body Acute Osteochondral Injuries • Anterior capitellum • Fragment usually detaches at o-c junction • Only acute changes in the bone Persistent pain after a fall 13-year-old competitive tennis player Osteochondritis Dissecans 6 month follow up Osteochondritis Dissecans • Anterior to inferior capitellum • Bone marrow edema • Cystic changes • Findings similar to those of OCD in the knee 8-year-old with elbow pain Panner’s Disease • Osteonecrosis of the capitellum • First decade • Repetitive trauma 17 “Pseudo Panner”: Irregular ossification variant Regarding elbow OCD and Panner’s disease, which of these statements is true: 1. Both affect the same age group 2. The trochlea is the structure most frequently affected by Panner’s disease 3. The capitellum is the structure most frequently affected by OCD 4. The articular cartilage is disrupted in Panner’s disease Regarding elbow OCD and Panner’s disease, which of these statements is true: 1. Both affect the same age group 2. -

Orthopaedic Examination Spinal Cord / Nerves
9/6/18 OBJECTIVES: • Identify the gross anatomy of the upper extremities, spine, and lower extremities. • Perform a thorough and accurate orthopaedic ORTHOPAEDIC EXAMINATION examination of the upper extremities, spine, and lower extremities. • Review the presentation of common spine and Angela Pearce, MS, APRN, FNP-C, ONP-C extremity diagnoses. Robert Metzger, DNP, APRN, FNP - BC • Determine appropriate diagnostic tests for common upper extremity, spine, and lower extremity problems REMEMBER THE BASIC PRINCIPLES OF MUSCULOSKELETAL EXAMINATION Comprehensive History Comprehensive Physical Exam THE PRESENTERS • Chief Complaint • Inspection • HPI OLDCART • Palpation HAVE NO CONFLICTS OF INTEREST • PMH • Range of Motion TO REPORT • PSH • Basic principles use a goniometer to assess joint ROM until you can • PFSH safely eyeball it • ROS • Muscle grading • Physical exam one finger point • Sensation to maximum pain • Unusual findings winging and atrophy SPINAL COLUMN SPINAL CORD / NERVES • Spinal cord • Begins at Foramen Magnum and • Consists of the Cervical, Thoracic, continues w/ terminus at Conus Medullaris near L1 and Lumbar regions. • Cauda Equina • Collection of nerves which run from • Specific curves to the spinal column terminus to end of Filum Terminale • Lordosis: Cervical and Lumbar • Nerve Roots • Kyphosis: Thoracic and Sacral • Canal is broader in cervical/ lumbar regions due to large number of nerve roots • Vertebrae are the same throughout, • Branch off the spinal cord higher except for C1 & C2, therefore same than actual exit through -

Sports Injuries in Children Continued
Me d i c i n eT o d a y PEER REVIEWED ARTICLE POINTS: 2 CPD/1 PDP Sports injuries in childre n The number of children with sports injuries seen in sports medicine practices is increasing. The usual outcome is full recovery, but the consequence of a missed diagnosis of a more serious condition may be significant for the child. The important issue of encouraging children to be injuries seen in sports medicine practices appears more active in an effort to improve their overall to be actually increasing.1 , 2 health is a complex public health problem.1 , 2 Fortunately, many of the sports injuries that Childhood sports participation in Australia has occur in children are self-limited and full recovery unfortunately declined over the past few decades. is the usual outcome. However, more serious con- Some 86% of children aged 5 to 14 years were ditions may occasionally occur and the conse- active in sport in 1985, but by 2003, the level of quence of a missed diagnosis, especially during the participation had fallen to 54% for girls and 69% rapid pubertal growth phase, may be significant for boys.1 During this time period, the number of for the child. overweight and obese children has been increas- Pain in a child should not be dismissed as ‘grow- TOM CROSS ing. At the other end of the spectrum, more active ing pains’. If an informed systematic approach FACSP, MBBS, DCH children are training more intensively and for is followed, the clinical assessment of a child will longer periods of time in one or several sports. -

Abductor Pollicis Brevis 5, 66, 68 Acetabular Dysplasia 199 Achilles
Cambridge University Press 978-0-521-86241-7 - Advanced Examination Techniques in Orthopaedics Edited by Nick Harris Index More information 13Harris(Ind)-cpp 25/9/02 11:34 am Page 219 Index abductor pollicis brevis 5, 66, 68 dislocation 156 acetabular dysplasia 199 paediatric patients 205 achilles tendinitis 165 shoulder instability 99, 101, 207 achilles tendon 167 apprentice’s spine (thoraco-lumbar Scheuermann’s disruption 182 disease) 214 acromegaly 4 arachnodactyly 207 acromioclavicular joint arcade of Frohse 73 impingement signs/tests 96–97 arcade of Struthers 71 inspection 85 arthrogryposis multiplex congenita 191, 206 palpation 85, 88 ataxic gait 197 acromioclavicular joint disorders 81 axillary nerve damage 88, 114, 118 impingement 96, 97 axonotmesis 66 adolescent acetabular dysplasia 193 adolescent disc syndrome 213, 217 back kneeing 197 adolescent idiopathic scoliosis 197 back pain 125, 126 Adson’s manoeuvre 131 paediatric patients 214 Allen’s test 5, 19 ballotment test (Reagan) 35, 36 anconeous epitrochlearis 71 Barlow’s test 203 ankle 165–187 belly press test (Napoleon’s sign) 91, 95 anatomy 170, 173 benign essential tremor 4 examination 167–182 biceps brachii 117 history 165 function testing 92 inspection 167 rupture instability 165, 182 insertion tendon 46, 47 movement 176–179 long head 47, 85 muscle strength grading 206 biceps reflex 88 neurovascular assessment 180 bicipital tendonitis 88, 92 paediatric examination 205–206 biro test see tactile adherence test cerebral palsy 209 block test 199, 200, 201 pain 165 Blount’s -

Physical Examination of Knee Ligament Injuries..Pdf
Review Article Physical Examination of Knee Ligament Injuries Abstract Robert D. Bronstein, MD The knee is one of the most commonly injured joints in the body. Joseph C. Schaffer, MD A thorough history and physical examination of the knee facilitates accurate diagnosis of ligament injury. Several examination techniques for the knee ligaments that were developed before advanced imaging remain as accurate or more accurate than these newer imaging modalities. Proper use of these examination techniques requires an understanding of the anatomy and pathophysiology of knee ligament injuries. Advanced imaging can be used to augment a history and examination when necessary, but should not replace a thorough history and physical examination. he knee joint is one of the most injuries because the current injury may Tcommonly injured joints in the be the sequela of a previous injury. body. Knee ligament injury and sub- Here, we present specific tech- sequent instability can cause consid- niques for the ligamentous exami- erable disability. Diagnosis of knee nation, including identifying injuries ligament injuries requires a thorough of the anterior cruciate ligament understanding of the anatomy and (ACL), the medial collateral liga- the biomechanics of the joint. Many ment (MCL), the lateral collateral specific examination techniques were ligament (LCL), the posterolateral cor- developed before advanced imaging, ner (PLC), and the posterior cruciate and several techniques remain as ligament (PCL), and describe the asso- accurate or more accurate than the ciated anatomy and biomechanics and From the Division of Sports Medicine, new imaging modalities. Advanced the methods that allow for increased Department of Orthopaedics, University of Rochester School of Medicine and imaging (eg, MRI) is appropriate to diagnostic sensitivity and accuracy. -

Elbow, Forearm, Wrist & Hand
Orthopedic Physical Assessment with Special Tests | Elbow, Forearm, Wrist & Hand COURSE DESCRIPTION Detailed video demonstrations of tests and procedures common in musculoskeletal assessment are supplemented by high-quality full-color clinical photographs and illustrations of each test and assessment for the Elbow, Forearm, Wrist & Hand. LEARNING OBJECTIVES Module 1 | Selected Movements- Elbow At the end of this module the learner will be able to: • Correctly instruct patients in performing active movements of the elbow including flexion,extension, pronation, and supination. • Identify positive indications of flexion, extension, pronation, and supination of the elbow. • Correctly perform and identify positive indications of passive movements of the elbow. • Correctly perform and identify positive indications of resisted isometric movements of the elbow including elbow flexion, elbow extension, pronation, supination, wrist flexion, and wrist extension. Module 2 | Special Tests for Ligamentous Instability At the end of this module the learner will be able to: • Define and describe ligamentous instability including suspected injury, epidemiology and demographics, relevant history, and relevant signs, symptoms and mechanism of injury for dislocation/subluxation and repetitive stress injuries. • Correctly perform and identify positive indications of a ligamentous valgus instability test. • Correctly perform and identify positive indications of a ligamentous varus instability test. • Correctly perform and identify positive indications of a milking maneuver. • Correctly perform and identify positive indications of a moving valgus stress test. • Correctly perform and identify positive indications of a lateral pivot-shift test. • Correctly perform and identify positive indications of a posterolateral rotary drawer test. • Correctly perform and identify positive indications of a posterolateral rotary apprehension test. Page 1 of 4 Accelerated Online Learning Orthopedic Phys.