Selective Esophagogastric Devascularization in the Modified
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

CASE REPORT Spinal Cord Infarction Following Endoscopic Variceal Ligation
Spinal Cord (2008) 46, 241–242 & 2008 International Spinal Cord Society All rights reserved 1362-4393/08 $30.00 www.nature.com/sc CASE REPORT Spinal cord infarction following endoscopic variceal ligation K Tofuku, H Koga, T Yamamoto, K Yone and S Komiya Department of Orthopaedic Surgery, Kagoshima Graduate School of Medical and Dental Sciences, Kagoshima, Japan Study design: A case report of spinal cord infarction following endoscopic variceal ligation. Objectives: To describe an exceedingly rare case of spinal cord infarction following endoscopic variceal ligation. Setting: Department of Orthopaedic Surgery, Kagoshima, Japan. Methods: A 75-year-old woman with cirrhosis caused by hepatitis C virus, who was admitted to our hospital for the treatment of esophageal varices, experienced numbness of the hands and lower extremities bilaterally following an endoscopic variceal ligation procedure. Sensory and motor dysfunction below C6 level progressed rapidly, resulting in inability to move the lower extremities the following day. Magnetic resonance imaging of the spine revealed abnormal spinal cord signal on T2-weighted images from approximately C6 through T5 levels, which was diagnosed as spinal cord infarction. Results: The patient underwent hyperbaric oxygen treatment. Her symptoms and signs related to spinal cord infarction gradually remitted, and nearly complete disappearance of neurological deficits was noted within 3 months after the start of treatment. Conclusion: We speculate that the pathogenesis of the present case may have involved congestion of the abdominal–epidural–spinal cord venous network owing to ligation of esophageal varices and increased thoracoabdominal cavity pressure. Spinal Cord (2008) 46, 241–242; doi:10.1038/sj.sc.3102092; published online 19 June 2007 Keywords: endoscopic variceal ligation; hyperbaric oxygen; spinal cord infarction Introduction The spectrum of etiologies of spinal cord infarction is as On physical examination, her right upper extremity diverse as that for cerebral infarction. -

Vessels and Circulation
CARDIOVASCULAR SYSTEM OUTLINE 23.1 Anatomy of Blood Vessels 684 23.1a Blood Vessel Tunics 684 23.1b Arteries 685 23.1c Capillaries 688 23 23.1d Veins 689 23.2 Blood Pressure 691 23.3 Systemic Circulation 692 Vessels and 23.3a General Arterial Flow Out of the Heart 693 23.3b General Venous Return to the Heart 693 23.3c Blood Flow Through the Head and Neck 693 23.3d Blood Flow Through the Thoracic and Abdominal Walls 697 23.3e Blood Flow Through the Thoracic Organs 700 Circulation 23.3f Blood Flow Through the Gastrointestinal Tract 701 23.3g Blood Flow Through the Posterior Abdominal Organs, Pelvis, and Perineum 705 23.3h Blood Flow Through the Upper Limb 705 23.3i Blood Flow Through the Lower Limb 709 23.4 Pulmonary Circulation 712 23.5 Review of Heart, Systemic, and Pulmonary Circulation 714 23.6 Aging and the Cardiovascular System 715 23.7 Blood Vessel Development 716 23.7a Artery Development 716 23.7b Vein Development 717 23.7c Comparison of Fetal and Postnatal Circulation 718 MODULE 9: CARDIOVASCULAR SYSTEM mck78097_ch23_683-723.indd 683 2/14/11 4:31 PM 684 Chapter Twenty-Three Vessels and Circulation lood vessels are analogous to highways—they are an efficient larger as they merge and come closer to the heart. The site where B mode of transport for oxygen, carbon dioxide, nutrients, hor- two or more arteries (or two or more veins) converge to supply the mones, and waste products to and from body tissues. The heart is same body region is called an anastomosis (ă-nas ′tō -mō′ sis; pl., the mechanical pump that propels the blood through the vessels. -
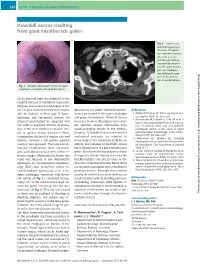
Downhill Varices Resulting from Giant Intrathoracic Goiter
E40 UCTN – Unusual cases and technical notes Downhill varices resulting from giant intrathoracic goiter Fig. 2 Sagittal com- puted tomography of the chest. The goiter was immense, reaching the aortic arch, sur- rounding the trachea and partially compres- sing the upper esopha- gus. The esophagus was additionally com- pressed by anterior spinal spondylophytes. Fig. 1 Multiple submucosal veins in the upper esophagus, consistent with downhill varices. An 82-year-old man was admitted to the hospital because of substernal chest pain, dyspnea, and occasional dysphagia to sol- ids. His past medical history was remark- geal varices are called “downhill varices”, References able for diabetes mellitus type II, hyper- as they are located in the upper esophagus 1 Kotfila R, Trudeau W. Extraesophageal vari- – lipidemia, and Parkinson’s disease. On and project downwards. Downhill varices ces. Dig Dis 1998; 16: 232 241 2 Basaranoglu M, Ozdemir S, Celik AF et al. A occur as a result of shunting in cases of up- physical examination he appeared frail case of fibrosing mediastinitis with obstruc- but with no apparent distress. Examina- per systemic venous obstruction from tion of superior vena cava and downhill tion of the neck showed no masses, stri- space-occupying lesions in the medias- esophageal varices: a rare cause of upper dor or jugular venous distension. Heart tinum [2,3]. Downhill varices as a result of gastrointestinal hemorrhage. J Clin Gastro- – examination disclosed a regular rate and mediastinal processes are reported to enterol 1999; 28: 268 270 3 Calderwood AH, Mishkin DS. Downhill rhythm; however a 2/6 systolic ejection occur in up to 50% of patients [3,4]. -

Venous Drainage from the Tail of the Pancreas to the Lienal Vein and Its Relationship with the Distal Splenorenal Shunt Selectivity1
20 – ORIGINAL ARTICLE Surgical Anatomy Venous drainage from the tail of the pancreas to the lienal vein and its relationship with the distal splenorenal shunt selectivity1 Drenagem venosa da cauda do pâncreas para a veia lienal e sua relação com a seletividade da anastomose esplenorrenal Cláudio PirasI, Danilo Nagib Salomão PauloII, Isabel Cristina Andreatta Lemos PauloIII, Hildegardo RodriguesIV, Alcino Lázaro da SilvaV I Associate Professor, Department of Surgery, School of Sciences, EMESCAM, Espirito Santo, Brazil. II Full Professor of Surgery, Department of Surgery, School of Sciences, EMESCAM, Espirito Santo, Brazil. III Associate Professor, Department of Surgery, School of Sciences, EMESCAM, Espirito Santo, Brazil. IV Professor of Anatomy, Department of Morphology, School of Sciences, EMESCAM, Espirito Santo, Brazil. V Emeritus Professor of Surgery, School of Medicine, Federal University of Minas Gerais, Brazil. ABSTRACT Purpose: To identify the veins draining from the pancreatic tail to the lienal vein and its possible relationship with the loss of the distal splenorenal shunt selectivity. Methods: Thirty eight human blocks including stomach, duodenum, spleen, colon and pancreas, removed from fresh corpses, were studied with the replenish and corrosion technique, using vinilic resin and posterior corrosion of the organic tissue with commercial hydrochloric acid, in order to study the lienal vein and its tributaries. Results: The number of veins flowing directly to the splenic vein varied from seven to twenty two (14.52 ± 3.53). Pancreatic branches of the pancreatic tail flowing to the segmentary veins of the spleen were found in 25 of the anatomical pieces studied (65.79%). These branches varied from one to four, predominating one branch (60%) and two branches (24%). -

Blood Vessels and Circulation
19 Blood Vessels and Circulation Lecture Presentation by Lori Garrett © 2018 Pearson Education, Inc. Section 1: Functional Anatomy of Blood Vessels Learning Outcomes 19.1 Distinguish between the pulmonary and systemic circuits, and identify afferent and efferent blood vessels. 19.2 Distinguish among the types of blood vessels on the basis of their structure and function. 19.3 Describe the structures of capillaries and their functions in the exchange of dissolved materials between blood and interstitial fluid. 19.4 Describe the venous system, and indicate the distribution of blood within the cardiovascular system. © 2018 Pearson Education, Inc. Module 19.1: The heart pumps blood, in sequence, through the arteries, capillaries, and veins of the pulmonary and systemic circuits Blood vessels . Blood vessels conduct blood between the heart and peripheral tissues . Arteries (carry blood away from the heart) • Also called efferent vessels . Veins (carry blood to the heart) • Also called afferent vessels . Capillaries (exchange substances between blood and tissues) • Interconnect smallest arteries and smallest veins © 2018 Pearson Education, Inc. Module 19.1: Blood vessels and circuits Two circuits 1. Pulmonary circuit • To and from gas exchange surfaces in the lungs 2. Systemic circuit • To and from rest of body © 2018 Pearson Education, Inc. Module 19.1: Blood vessels and circuits Circulation pathway through circuits 1. Right atrium (entry chamber) • Collects blood from systemic circuit • To right ventricle to pulmonary circuit 2. Pulmonary circuit • Pulmonary arteries to pulmonary capillaries to pulmonary veins © 2018 Pearson Education, Inc. Module 19.1: Blood vessels and circuits Circulation pathway through circuits (continued) 3. Left atrium • Receives blood from pulmonary circuit • To left ventricle to systemic circuit 4. -

The Gastrointestinal Tract Frank A
91731_ch13 12/8/06 8:55 PM Page 549 13 The Gastrointestinal Tract Frank A. Mitros Emanuel Rubin THE ESOPHAGUS Bezoars Anatomy THE SMALL INTESTINE Congenital Disorders Anatomy Tracheoesophageal Fistula Congenital Disorders Rings and Webs Atresia and Stenosis Esophageal Diverticula Duplications (Enteric Cysts) Motor Disorders Meckel Diverticulum Achalasia Malrotation Scleroderma Meconium Ileus Hiatal Hernia Infections of the Small Intestine Esophagitis Bacterial Diarrhea Reflux Esophagitis Viral Gastroenteritis Barrett Esophagus Intestinal Tuberculosis Eosinophilic Esophagitis Intestinal Fungi Infective Esophagitis Parasites Chemical Esophagitis Vascular Diseases of the Small Intestine Esophagitis of Systemic Illness Acute Intestinal Ischemia Iatrogenic Cancer of Esophagitis Chronic Intestinal Ischemia Esophageal Varices Malabsorption Lacerations and Perforations Luminal-Phase Malabsorption Neoplasms of the Esophagus Intestinal-Phase Malabsorption Benign tumors Laboratory Evaluation Carcinoma Lactase Deficiency Adenocarcinoma Celiac Disease THE STOMACH Whipple Disease Anatomy AbetalipoproteinemiaHypogammaglobulinemia Congenital Disorders Congenital Lymphangiectasia Pyloric Stenosis Tropical Sprue Diaphragmatic Hernia Radiation Enteritis Rare Abnormalities Mechanical Obstruction Gastritis Neoplasms Acute Hemorrhagic Gastritis Benign Tumors Chronic Gastritis Malignant Tumors MénétrierDisease Pneumatosis Cystoides Intestinalis Peptic Ulcer Disease THE LARGE INTESTINE Benign Neoplasms Anatomy Stromal Tumors Congenital Disorders Epithelial Polyps -

Stomach, Thick Muscular Wall Called Pyloric Sphincter and the Cavity of Pylorus Is Pyloric Canal (Length of Canal 2.5 Cm)
Divisions: 1)Fundus: is dome-shaped projects upward , It is usually full of gas. 2)Body: This extends from level of cardiac orifice to incisura angularis ( constant notch in lower part of lesser curvature ). 3) Antrum: extends from incisura angularis to pylorus. 4) Pylorus: This is the most tubular part of stomach, thick muscular wall called pyloric sphincter and the cavity of pylorus is pyloric canal (length of canal 2.5 cm). Two Openings : *Cardiac orifice. *Pyloric orifice. Two Curvatures : * Greater curvature. *Lesser curvature. Two Surfaces : *Anterior surface. *posterior surface. The cardiac orifice is where esophagus enters stomach & it has a physiologic sphincter exists that prevents regurgitation of stomach contents into esophagus . The circular muscle coat of pylorus is much thicker here and forms anatomical pyloric sphincter Lesser curvature forms right border of stomach extends from cardiac orifice to pylorus. Greater curvature is much longer than lesser curvature ,extends from left of cardiac orifice over dome of fundus & along left border of stomach to pylorus . 1)Lesser omentum: suspended lesser curvature to liver. 2)Greater omentum: extends from the greater curvature to the transverse colon. 3) Gastrosplenic ligament : extends from upper part of greater curvature to spleen . Relations: Anteriorly: Anterior abdominal wall Left costal margin Left pleura and lung Diaphragm Left lobe of the liver . Posteriorly: The lesser sac Diaphragm spleen , splenic artery left suprarenal gland upper part of left kidney pancreas transverse mesocolon. transverse colon Arteries: 1) The left gastric artery : arises from celiac artery. It passes upward & to the left reach esophagus and then descends along the lesser curvature of stomach. -

Esophageal Varices
ESOPHAGEAL VARICES The esophagus is the flexible tube that carries food from the mouth to the stomach. Through the neck and the chest. Varicose veins, whatever there are legs or esophagus, are irregularly dilated veins with a thin wall. Those in the legs, which are common, visible, and well known, developed under the skin. Those of the esophagus, invisible from the outside, thrive under the lining of the gastrointestinal tract in contact with the food. This lining is called the mucosa. Varicose veins are in the lining of the esophagus itself, between the mucous membrane and the muscles that form the outer wall of the esophagus. The contraction of these muscles is responsible for moving food down the esophagus. Esophageal Varices Similar to varices in the legs, esophageal varicose veins results from poor blood circulation. Like legs varicose, they can crack and leak blood, a process that is inappropriately called a rupture. Esophageal varicose veins are just normal esophageal veins which are enlarged and increase the pressure of the blood they carry. The main cause of this increase pressure is portal hypertension (see 2016 news letter). The veins of the portal system carry blood to the liver. Portal hypertension therefore occurs when the passage of blood through the liver is obstructed by a portal vein thrombosis, or by an obstruction of the small vessels of the liver, or by a thrombosis of the hepatic veins (Budd-Chiari syndrome). The obstruction of the small vessels of the liver is mainly due to a chronic disease leading to cirrhosis (diabetes, viral hepatitis, alcohol). -

HEMORRHAGE • It Is a Blood Escaping from the Circulatory System HEMORRHAGE
LECTURE 6 HEMORRHAGE • It is a blood escaping from the circulatory system HEMORRHAGE HAEMORRHAGIA EXTERNA DIRECT INDIRECT (VULNUS) (ESOPHAGEAL VARICES) INTERNAL HEMORRHAGE (FROM HEART) - HEMOPERICARDIUM VARICES • Dilated tortuous vessels, usually submucosal, that develop due to portal hypertension (prolonged or severe), which induces formation of collaterals between portal and caval systems VARICES • Collaterals in lower esophagus divert flow from portal vein, through coronary veins of stomach, into esophageal veins, then azygous veins, then into vena cava VARICES in the lower esophagus (which has been turned inside out at autopsy) are linear dark blue submucosal dilated veins known as varices: in patients with portal hypertension ORIGIN OF HEMORRHAGES HEMORRHAGE FROM HEART ARTERIAL HEMORRHAGE VENOUS HEMORRHAGE-varices PARENCHYMATOUS HEMORRHAGE MECHANISMS OF HEMORRHAGES HEMORRHAGIA PER RHEXIN - RUPTURE HEMORRHAGIA PER DIABROSIN - ARROSION HEMORRHAGIA PER DIAPEDESIN - DIAPEDESIS CLASSIFICATION OF HEMORRHAGES WITH REGARD TO THE MECHANISM • 1. TRAUMATIC HEMORRHAGES • 2. SPONTANEOUS HEMORRHAGES • A. PER RHEXIN (RUPTURE) • B. PER DIABROSIN (ARROSION) • C. PER DIAPEDESIN (DIAPEDESIS) TYPES OF HEMORRHAGIC CHANGES B. C. B. and D. PURPURA A. SIZE D. A. PETECHIA (SKIN) 1-5 mm C. PETECHIA (BRAIN) HEMORRHAGIC SUGGILLATIONS SKIN BRUISE A BRUISE IS THE EPICARDIAL BRUISE UNDER EXTRAVASATION OF BLOOD TO BRUISE EPICARDIUM – SURROUNDING INTACT TISSUES OFTEN AS A RESULT OF A DAMAGE OF BRAIN STEM ECCHYMOSIS Ecchymosis is the medical term for a bruise that -

A Case Simultaneously Presenting with a Rare Portal Collateral Pathway and Left Gastric Venous Anomaly It Is Known, That When Th
A Case Simultaneously Presenting with a Rare Portal Collateral Pathway and Left Gastric Venous Anomaly By Masato OHKUBO and Akira IIMURA Department of Anatomy, Tokyo Medical College, 6-1-1 Shinjuku, Shinjuku-ku, Tokyo 160, Japan -Received for Publication, June 4,1997- Key Words: Portal vein, Left gastric vein, Renal vein, Collateral vein, Anomaly Summary: We had the opportunity to dissect an autopsy case who had developed a rare portal collateral pathway due to increased portal pressure resulting from liver cirrhosis and simultaneous abnormal left gastric venous distribution. The portal collateral pathway consisted of a well-developed communicating branch located between the left renal vein and the left gastric vein. The left gastric vein did not merge into the portal vein, but directly entered the liver after bifurcating near the hepatic hilum. One branch had an anastomosis to the left branch of portal vein in the liver and the other distributed in the hepatic quadrate lobe. We considered this aberrant left gastric vein to be a congenital residue of the embryological left portal vein. The present case is the third Japanese case to have been described minutely in the literature, following the two cases reported by Miyaki et al. (1987). Persistence of the umbilical vein and the absence of the celiac trunk were also observed. It is known, that when the portal vein is oc- nal vein and left gastric vein. The left gastric vein cluded, various collateral routes are developed. did not merge into the portal vein, showing direct Representative examples listed in the textbooks of entry into the liver. -

Therapeutic Approach To" Downhill" Esophageal Varices Bleeding Due to Superior Vena Cava Syndrome in Behcet's Disease: a Case Report
BMC Gastroenterology BioMed Central Case report Open Access Therapeutic approach to "downhill" esophageal varices bleeding due to superior vena cava syndrome in Behcet's disease: a case report Hamid Tavakkoli*1, Mehrnaz Asadi1, Mahshid Haghighi1 and Abbas Esmaeili2 Address: 1Alzahra Hospital, Isfahan University of Medical Sciences, Isfahan, Iran and 2Poursina Hakim Research Institute, Isfahan, Iran Email: Hamid Tavakkoli* - [email protected]; Mehrnaz Asadi - [email protected]; Mahshid Haghighi - [email protected]; Abbas Esmaeili - [email protected] * Corresponding author Published: 27 December 2006 Received: 14 September 2006 Accepted: 27 December 2006 BMC Gastroenterology 2006, 6:43 doi:10.1186/1471-230X-6-43 This article is available from: http://www.biomedcentral.com/1471-230X/6/43 © 2006 Tavakkoli et al; licensee BioMed Central Ltd. This is an Open Access article distributed under the terms of the Creative Commons Attribution License (http://creativecommons.org/licenses/by/2.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. Abstract Background: One of the rare presentations of superior vena cava syndrome is bleeding of "downhill" esophageal varices (DEV) and different approaches have been used to control it. This is a case report whose DEV was eradicated by band ligation for the first time. Case presentation: We report a 42-year-old man who is a known case of Behcet's disease. The patient's first presentation was superior vena cava syndrome due to thrombosis followed by bipolar ulcers and arthralgia. He received warfarin, prednisolone and azathioprine. The clinical course of the patient was complicated by one episode of hematemesis without abdominal pain when the patient's PT was in therapeutic range. -

Liver Disease and Portal Hypertension Fact Sheet
FACT SHEET FOR PATIENTS AND FAMILIES Liver Disease and Portal Hypertension What is portal hypertension and How is it diagnosed? what causes it? Depending on your symptoms, your doctor may The portal vein is a major blood vessel that leads order tests to see if you have portal hypertension. to the liver. Portal hypertension [hi-per-TEN-shun] • An endoscopy [en-DOS-kuh-pee] is a when a thin, is when the blood pressure inside the portal vein flexible tube with a camera and a light on the end increases. Increased pressure in the portal vein can is placed in your esophagus while you are sleeping. cause blood to back up. This can cause other medical This allows your doctor to see if you have problems problems, such as: with your esophageal veins. • Esophageal [ee-sof-uh-JEE-al] varices [VAIR-uh-sees], • An angiogram [AN-jee-uh-gram] can tell your doctor if when the veins in the esophagus (the tube that there is a blockage in the portal vein and you need a carries food to your stomach) become enlarged. shunt (a device to help lower portal hypertension). • Ascites [ah-SITE-eez], or fluid build-up in your During this test, a dye is placed in a vein. The dye abdomen (belly). makes your veins visible on a special x-ray called a fluoroscope[FLOOR-oh-scope] • Splenomegaly [splen-oh-MEG-ah-lee], when your . spleen becomes enlarged. • Other imaging tests, such as a CT (computed • Edema [eh-DEEM-ah], or swelling in the lower legs. tomography) scan may also be needed.