A Simple Bone Cyst
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Oralmedicine
116 Test 98.2 ORAL MEDICINE Developmental Mandibular Salivary Gland Defect The Importance of Clinical Evaluation developmental mandibular salivary gland defect (also known as static A bone cyst, static bone defect, Stafne bone cavity, latent bone cyst, latent bone defect, idiopathic bone cavity, developmen- tal submandibular gland defect of the mandible, aberrant salivary gland defect in the mandible, and lingual mandibular bone Sako Ohanesian, concavity) is a deep, well-defined depression DDS in the lingual surface of the posterior body of the mandible. More precisely, the most common location is within the submandibu- lar gland fossa and often close to the inferi- or border of the mandible. In developmental bone defects investigated surgically, an aberrant lobe of the submandibular gland extends into the bony depression. First recognized by Dr. Edward Stafne in 1942, numerous cases of developmental mandibular salivary gland defect have since been reported, and the lesion should not be considered rare.1 In a study of 4963 pan- Most authorities now agree that this entity is a congenital defect, although it has rarely been observed in children and its precise anatomic nature is still uncertain. oramic images of adult patients, 18 cases of Figure 1. CT slices/panoramic views showing a well-defined radiolucent lesion in the right mandible. salivary gland depression were found by Karmiol and Walsh2, an incidence of nearly 0.4%. Most authorities now agree that this The margins of the radiolucent defect are around an extension of salivary tissue. This entity is a congenital defect, although it has well-defined by a dense radiopaque line. -

Peripheral Giant Cell Reparative Granuloma of Maxilla in a Patient with Aggressive Periodontitis
Peripheral Giant Cell Reparative Granuloma of Maxilla in a Patient with Aggressive Periodontitis E Cayci1, B Kan2, E Guzeldemir-Akcakanat1, B Muezzinoglu3 1Department of Periodontology, Kocaeli University, Faculty of Dentistry, Kocaeli, Turkey. 2Department of Oral and Maxillofacial Surgery, Kocaeli University, Faculty of Dentistry, Kocaeli, Turkey. 3Department of Pathology, Kocaeli University, School of Medicine, Kocaeli, Turkey. Abstract Peripheral giant cell reparative granuloma is a reactive and rare lesion of oral cavity with unknown etiology which is derived from periosteum and periodontal ligament and occurs frequently in young adults. Inflammation or trauma is underlying causative factor of reactive proliferation. In the present case report, a 35 year-old male with aggressive periodontitis and peripheral giant cell reparative granuloma is presented. The patient applied to our clinic with a complaining about a big nodule at his palate. The lesion was pedunculated and localized at his right maxilla between #16 and #17 which arose from distal aspect of #16, and the surface of the lesion was hyperkeratotic and the lesion was measured 22 x 30 mm at the largest diameter. He also had severe generalized aggressive periodontitis and hypertension. Amoxicillin clavulanate 625 mg, three times a day, metronidazole 500 mg three times a day and 0.2% chlorhexidine digluconate oral rinse, twice a day for a week, were prescribed to the patient. Then, scaling and root planing were performed along with systemic antibiotic treatment and he scheduled for surgery. The lesion was excised completely and #16 was extracted. After the healing period, periodontal surgery was planned for the treatment of aggressive periodontitis. Obtained tissue specimen was sent for histopathological examination. -

Iii Bds Oral Pathology and Microbiology
III BDS ORAL PATHOLOGY AND MICROBIOLOGY Theory: 120 Hours ORAL PATHOLOGY MUST KNOW 1. Benign and Malignant Tumours of the Oral Cavity (30 hrs) a. Benign tumours of epithelial tissue origin - Papilloma, Keratoacanthoma, Nevus b. Premalignant lesions and conditions: - Definition, classification - Epithelial dysplasia - Leukoplakia, Carcinoma in-situ, Erythroplakia, Palatal changes associated with reverse smoking, Oral submucous fibrosis c. Malignant tumours of epithelial tissue origin - Basal Cell Carcinoma, Epidermoid Carcinoma (Including TNM staging), Verrucous carcinoma, Malignant Melanoma. d. Benign tumours of connective tissue origin : - Fibroma, Giant cell Fibroma, Peripheral and Central Ossifying Fibroma, Lipoma, Haemangioma (different types). Lymphangioma, Chondroma, Osteoma, Osteoid Osteoma, Benign Osteoblastoma, Tori and Multiple Exostoses. e. Tumour like lesions of connective tissue origin : - Peripheral & Central giant cell granuloma, Pyogenic granuloma, Peripheral ossifying fibroma f. Malignant Tumours of Connective tissue origin : - Fibrosarcoma, Chondrosarcoma, Kaposi's Sarcoma Ewing's sarcoma, Osteosarcoma Hodgkin's and Non Hodgkin's L ymphoma, Burkitt's Lymphoma, Multiple Myeloma, Solitary Plasma cell Myeloma. g. Benign Tumours of Muscle tissue origin : - Leiomyoma, Rhabdomyoma, Congenital Epulis of newborn, Granular Cell tumor. h. Benign and malignant tumours of Nerve Tissue Origin - Neurofibroma & Neurofibromatosis-1, Schwannoma, Traumatic Neuroma, Melanotic Neuroectodermal tumour of infancy, Malignant schwannoma. i. Metastatic -

Oral Path Questions
Oral Pathology Oral Pathology • Developmental Conditions • Mucosal Lesions—Reactive • Mucosal Lesions—Infections • Mucosal Lesions—Immunologic Diseases • Mucosal Lesions—Premalignant • Mucosal Lesions—Malignant • CT Tumors—Benign • CT Tumors—Malignant • Salivary Gland Diseases—Reactive • Salivary Gland Diseases—Benign • Salivary Gland Diseases—Malignant • Lymphoid Neoplasms • Odontogenic Cysts • Odontogenic Tumors • Bone Lesions—Fibro-Osseous • Bone Lesions—Giant Cell • Bone Lesions—Inflammatory • Bone Lesions—Malignant • Hereditary Conditions #1 One of the primary etiologic agents of aphthous stomatitis is proposed to be: A. Cytomegalovirus B. Staphylococcus C. Herpes simplex D. Human leukocyte antigen E. Candidiasis #1 One of the primary etiologic agents of aphthous stomatitis is proposed to be: A. Cytomegalovirus B. Staphylococcus C. Herpes simplex D. Human leukocyte antigen E. Candidiasis #2 Intracellular viral inclusions are seen in tissue specimens of which of the following? A. Solar cheilitis B. Minor aphthous ulcers C. Geographic tongue D. Hairy leukoplaKia E. White sponge nevus #2 Intracellular viral inclusions are seen in tissue specimens of which of the following? A. Solar cheilitis B. Minor aphthous ulcers C. Geographic tongue D. Hairy leukoplakia E. White sponge nevus #3 Sjogren’s Syndrome has been linKed to which of the following malignancies? A. Leukemia B. Lymphoma C. Pleomorphic adenoma D. Osteosarcoma #3 Sjogren’s Syndrome has been linKed to which of the following malignancies? A. Leukemia B. Lymphoma C. Pleomorphic adenoma D. Osteosarcoma #4 Acantholysis, resulting from desmosome weaKening by autoantibodies directed against the protein desmoglein, is the disease mechanism attributed to which of the following? A. Epidermolysis bullosa B. Mucous membrane pemphigoid C. Pemphigus vulgaris D. Herpes simplex infections E. -

Benign Bone Tumors of the Foot and Ankle
CHAPTER 20 BENIGN BONE TUMORS OF THE FOOT AND ANKLE, Robert R. Miller, D.P.M. Stephen V. Corey, D.P.M. Benign bone tumors of the foot and ankle typically Table 1 displays the percentage of each lesion present both a diagnostic and therapeutic challenge found in the leg and foot. The lesions represent a to podiatric surgeons. These lesions have a percentage of local lesions compared to the total relatively low incidence of occuffence in the foot number of lesions reported for the studies. It does and ankle when compared to other regions of the seem apparent that the overall incidence of foot body, and the behavior of these lesions may mimic and ankle involvement is relatively low, but some malignant tumors. Not only is it impofiant to tumors do occur with a somewhat frequent rate. recognize a specific lesion to insure proper treat- Primarily, enchondroma, osteochondroma, osteoid ment, but the ability to differentiate a benign from osteoma, simple (unicameral) bone cysts, and malignant process is of utmost importance. aneurysmal bone cysts are somewhat common in It is difficult to determine the true incidence of the foot and ankle. benign bone tumors of the foot and ankle. Most large studies do not distinguish individual tarsal RADIOGRAPHIC CHARACTERISTICS OF bones, nor is there a distinction made befween BENIGN BONE TUMORS proximal and distal aspects of the tibia and fibula. Dahlin's Bone Tumors has reported findings of the Several radiographic parameters have been Mayo Clinic up until 7993.' total 2334 Of a of described to differentiate between benign and benign bone tumors affecting the whole body, malignant bone tumors. -

Tuberculosis – the Masquerader of Bone Lesions in Children MN Rasool FCS(Orth) Department of Orthopaedics, University of Kwazulu-Natal
SAOJ Autumn 2009.qxd 2/27/09 11:11 AM Page 21 CLINICAL ARTICLE SA ORTHOPAEDIC JOURNAL Autumn 2009 / Page 21 C LINICAL A RTICLE Tuberculosis – the masquerader of bone lesions in children MN Rasool FCS(Orth) Department of Orthopaedics, University of KwaZulu-Natal Reprint requests: Dr MN Rasool Department of Orthopaedics University of KwaZulu-Natal Private Bag 7 Congella 4001 Tel: (031) 260 4297 Fax: (031) 260 4518 Email: [email protected] Abstract Fifty-three children with histologically confirmed tuberculous osteomyelitis were treated between 1989 and 2007. The age ranged from 1–12 years. There were 65 osseous lesions (excluding spinal and synovial). Seven had mul- tifocal bone involvement. Four basic types of lesions were seen: cystic (n=46), infiltrative (n=7), focal erosions (n=6) and spina ventosa (n=7). The majority of lesions were in the metaphyses (n=36); the remainder were in the diaphysis, epiphysis, short tubular bones, flat bones and small round bones. Bone lesions resembled chronic infections, simple and aneurysmal bone cysts, cartilaginous tumours, osteoid osteoma, haematological bone lesions and certain osteochondroses seen during the same period of study. Histological confirmation is man- datory to confirm the diagnosis of tuberculosis as several bone lesions can mimic tuberculous osteomyelitis. Introduction The variable radiological appearance of isolated bone Tuberculous osteomyelitis is less common than skeletal lesions in children can resemble various bone lesions tuberculosis involving the spine and joints. The destruc- including subacute and chronic osteomyelitis, simple and tive bone lesions of tuberculosis, the disseminated and the aneurysmal bone cysts, cartilaginous tumours, osteoid multifocal forms, are less common now than they were 50 osteoma, granulomatous lesions, haematological disease, 6,7,12 years ago.1-7 However, in recent series, solitary involve- and certain malignant tumours. -

Management of Unicameral Bone Cyst of Proximal Femur: Experience of 14 Cases and Review of Literature
202 KUWAIT MEDICAL JOURNAL September 2008 Original Article Management of Unicameral Bone Cyst of Proximal Femur: Experience of 14 Cases and Review of Literature Magdy M Abdel-Mota’al, Abdul Salam Othman Mohamad, Kenneth Chukwuka Katchy, Amarnath A Mallur, Fawzy Hamido Ahmad, Barakat El-Alfy Kuwait Medical Journal 2008, 40 (3): 202-210 ABSTRACT Objective: To assess the results of surgical treatment Main Outcome Measures: Patients were followed up of unicameral bone cyst (UBC) involving the proximal post-operatively for an average period of 42 months (range femur = 9–120 months). They were observed for recurrence, Design: Retrospective study of 14 cases of UBC of complications and fracture healing. proximal femur Results: Recurrence was observed in one case while other Setting: Al-Razi Orthopedic Hospital, Kuwait cases showed healing of the cyst with consolidation and Subjects and Methods: Fourteen cases of UBC seen and varying degrees of remodeling in one years time. A case treated at Al-Razi hospital were included in the study. developed mal-union and growth arrest with subsequent Their presentation and the method of treatment were shortening. Avascular necrosis and coxa vara was recorded. detected in another case. All the fractures healed in the Intervention: Thirteen cases were treated surgically using usual expected time according to age. intra-lesional excision (ILE). The cavity was filled with Conclusion: UBC of the proximal femur exhibits unique autogenous bone graft in three cases, hydroxyapatite characters and complications. Hydroxyapatite matrix matrix (HA) in eight cases, and combined autogenous is a useful and effective bone substitute. Post-excision graft and hydroxyapatite matrix in two cases. -

Massive Axial and Appendicular Skeletal Deformities in Connection with Gorham-Stout Syndrome
Case Report Massive Axial and Appendicular Skeletal Deformities in Connection with Gorham-Stout Syndrome Ali Al Kaissi 1,2,*, Sami Bouchoucha 3, Mohammad Shboul 4, Vladimir Kenis 5, Franz Grill 2, Rudolf Ganger 2 and Susanne Gerit Kircher 6 1 Ludwig Boltzmann Institute of Osteology, at the Hanusch Hospital of WGKK and, AUVA Trauma Centre Meidling, First Medical Department, Hanusch Hospital, 1090 Vienna, Austria 2 Orthopaedic Hospital of Speising, Paediatric department, 1090 Vienna, Austria; [email protected] (F.G.); [email protected] (R.G.) 3 Paediatric Orthopedic Surgery—Children Hospital, Tunis 1029, Tunis-Tunisia; [email protected] 4 Department of Medical Laboratory Sciences, Jordan University of Science and Technology, Irbid 22110, Jordan; [email protected] 5 Department of Foot and Ankle Surgery, Neuroorthopaedics and Systemic Disorders, Pediatric Orthopedic Institute n.a. H. Turner, Parkovaya str., 64-68, Pushkin, Saint Petersburg, Russia; [email protected] 6 Department of Medical Chemistry, Medical University of Vienna, 1090 Vienna, Austria; [email protected] * Correspondence: [email protected]; Tel. (Fax): +43-180-182-1260 Received: 26 March 2019; Accepted: 5 May 2019; Published: 7 May 2019 Abstract: Background: Etiological understanding is the corner stone in the management of skeletal deformities. Methods: Multi-centre study of patients with deformities in connection with diverse etiological backgrounds. We aimed to study four patients (one boy and three girls) with variable axial and appendicular deformities in connection with a vanishing bone disorder. Results: Axial deformities such as scoliosis, kyphoscoliosis, compressed fused vertebrae, appendicular fractures, dislocations, and vicious disorganization deformities of the joints were in connection with the vanishing bone disorder, namely Gorham-Stout syndrome. -
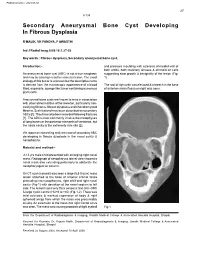
Secondary Aneurysmal Bone Cyst Developing in Fibrous Dysplasia
Published online: 2021-08-02 27 9-135 Secondary Aneurysmal Bone Cyst Developing In Fibrous Dysplasia R MALIK, VK PANDYA, P AWASTHI Ind J Radiol Imag 2006 16:1:27-28 Key words : Fibrous dysplasia, Secondary aneurysmal bone cyst. Introduction:- and pressure moulding with sclerosis of medial wall of both orbits, both maxillary sinuses & ethmoid air cells An aneurysmal bone cyst (ABC) is not a true neoplasm suggesting slow growth & benignitity of the lesion (Fig and may be a benign reactive vascular lesion. The exact 1). etiology of this tumor is unknown but the descriptive name is derived from the microscopic appearance of a blood The roof of right orbit was elevated & a breech in the base filled, expansile, sponge like tumor containing numerous of anterior cranial fossa on right was seen. giant cells. Aneurysmal bone cysts are known to arise in association with other abnormalities of the skeleton, particularly non ossifying fibroma, fibrous dysplasia and chondromyxoid fibroma. Such lesions have been described as secondary ABCs [1]. They have also been recorded following fractures [1]. The ABCs most commonly involve the metaphyses of long bones or the posterior elements of vertebrae, but the nasal cavity is the extremely rare site [2]. We report an interesting and rare case of secondary ABC developing in fibrous dysplasia in the nasal cavity & nasopharynx. Material and method:- A 13 yrs male child presented with enlarging right nasal mass. Radiograph of nasopharynx lateral view showed a nasal mass also extending posteriorly to obliterate the nasopharyngeal air column. On CT scan (coronal) was seen a large (5.5 X 6cm) mass lesion attached to the base of anterior cranial fossa protruding into nasopharynx, right orbit and right nasal cavity (Fig-1) with deviation of the nasal septum to left side. -

Oral Pathology Final Exam Review Table Tuanh Le & Enoch Ng, DDS
Oral Pathology Final Exam Review Table TuAnh Le & Enoch Ng, DDS 2014 Bump under tongue: cementoblastoma (50% 1st molar) Ranula (remove lesion and feeding gland) dermoid cyst (neoplasm from 3 germ layers) (surgical removal) cystic teratoma, cyst of blandin nuhn (surgical removal down to muscle, recurrence likely) Multilocular radiolucency: mucoepidermoid carcinoma cherubism ameloblastoma Bump anterior of palate: KOT minor salivary gland tumor odontogenic myxoma nasopalatine duct cyst (surgical removal, rare recurrence) torus palatinus Mixed radiolucencies: 4 P’s (excise for biopsy; curette vigorously!) calcifying odontogenic (Gorlin) cyst o Pyogenic granuloma (vascular; granulation tissue) periapical cemento-osseous dysplasia (nothing) o Peripheral giant cell granuloma (purple-blue lesions) florid cemento-osseous dysplasia (nothing) o Peripheral ossifying fibroma (bone, cartilage/ ossifying material) focal cemento-osseous dysplasia (biopsy then do nothing) o Peripheral fibroma (fibrous ct) Kertocystic Odontogenic Tumor (KOT): unique histology of cyst lining! (see histo notes below); 3 important things: (1) high Multiple bumps on skin: recurrence rate (2) highly aggressive (3) related to Gorlin syndrome Nevoid basal cell carcinoma (Gorlin syndrome) Hyperparathyroidism: excess PTH found via lab test Neurofibromatosis (see notes below) (refer to derm MD, tell family members) mucoepidermoid carcinoma (mixture of mucus-producing and squamous epidermoid cells; most common minor salivary Nevus gland tumor) (get it out!) -

Pathologic Femoral Neck Fractures in Children
An Original Study Pathologic Femoral Neck Fractures in Children M. Wade Shrader, MD, Joseph H. Schwab, MD, William J. Shaughnessy, MD, and David J. Jacofsky, MD more common in adults and usually are caused by meta- ABSTRACT static disease. These fractures are typically treated with Pathologic fractures in children occur in a variety of internal fixation, intramedullary fixation, or arthroplasty.1 malignant and benign pathologic processes. Pediatric Fractures in the femoral neck of children are extremely pathologic femoral neck fractures are particularly rare and require special treatment considerations because rare. Until now, all reported cases have been isolated of growth issues and the possibility of avascular necrosis cases, small series, or cases reported in series of (AVN).2 adult pathologic hip fractures. The present article is the first report of a relatively large series of patho- The literature includes very little on pathologic femoral logic femoral neck fractures in a pediatric population. neck fractures in children. Fractures in FD have received We identified pathologic femoral neck fractures, the most attention. In their series on femoral neck insuf- including 2 basicervical fractures, in 15 children (9 ficiency fractures in FD, Enneking and Gearen3 indicated boys, 6 girls) ranging in age from 18 months to 15 years that 6 of the 15 patients were children. Funk and Wells4 (mean age, 9 years) and treated between 1960 and reported on 4 pediatric patients with FD, 2 of whom had 2000. The pathologic diagnoses were fibrous dysplasia pathologic femoral neck fractures. In addition, several (5 children), unicameral bone cyst (2), Ewing’s sarcoma other authors have documented single cases of pathologic (2), osteomyelitis (2), leukemia (1), rhabdomyosarcoma hip fracture in patients with simple bone cysts, aneurysmal (1), osteogenesis imperfecta (1), and osteopetrosis (1). -

Vanishing Bone Disease
Journal of Regenerative Biology and Medicine ISSN: 2582-385X Tamilthangam P, et al., 2021- J Regen Bio Med Review Article Vanishing Bone Disease: The unseen 1Senior lecturer, Department of Oral Seen Pathology and Microbiology, 1 2 Periyasamy Tamilthangam, * Jeyaraman Swathiraman Vivekanandha Dental College for Women, Thangavelu kavin3, Aravind RJ4, Ramesh Narendar5, India 6 7 S.P.Indra kumar and Meyyappan Suruthi keerthana 2Senior lecturer, Department of Oral Pathology and Microbiology, Vivekanandha Dental College for Women, Abstract India Vanishing bone disease (Gorham disease) is an uncommon bone pathology that is characterized by a continuous replacement of bone 3Professor and Head, Department of oral with the abundance of endothelial cells. It is usually nonfamilial, but and maxillofacial surgery, Vivekanandha Dental College for Women, India maybe familial and occurs periodically in children and young adults. The lesion is usually nonexpansile and monocentric, rarely polyostotic, 4Professor, Department of oral and but locally aggressive. Though asymptomatic cases have been maxillofacial surgery, Vivekanandha Dental College for Women, India reported, clinical symptoms include pain, functional disability and swelling of the involved area. Pathologic fracture of the involved bone 5Reader, Department of oral and has also been noted in some patients. Surgical treatment, as well as maxillofacial surgery, Vivekanandha radiotherapy, forms the main basis of treatment modality. Dental College for Women, India 6Senior lecturer, Department of oral and Keywords: Gorham disease; Pathology; Surgical treatment; maxillofacial surgery, Vivekanandha Radiotherapy; Endothelial cells. Dental College for Women, India 7Intern, Vivekanandha Dental College for Introduction Women, India Vanishing bone disease (Gorham disease) is an uncommon bone pathology that is characterized by a continuous *Corresponding Author: Tamilthangam P, et al, 1Senior lecturer, Department of replacement of bone with the abundance of endothelial cells.