Management of Unicameral Bone Cyst of Proximal Femur: Experience of 14 Cases and Review of Literature
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Percutaneous Injection of Calcium Phosphate Composite in Pediatric Unicameral Bone Cysts: a Minimum 5-Year Follow-Up Study
Sport Sciences for Health (2019) 15:207–213 https://doi.org/10.1007/s11332-018-0513-7 ORIGINAL ARTICLE Percutaneous injection of calcium phosphate composite in pediatric unicameral bone cysts: a minimum 5-year follow-up study Marco Turati1,2 · Marco Bigoni2,3 · Lilia Brahim1 · Emeline Bourgeois1 · Giovanni Zatti2,3 · Ahmad Eid1 · Jacques Griffet1 · Aurélien Courvoisier1 Received: 4 September 2018 / Accepted: 9 November 2018 / Published online: 24 November 2018 © Springer-Verlag Italia S.r.l., part of Springer Nature 2018 Abstract Background Unicameral bone cyst (UBC) is a common lesion in skeletally immature patients. Multiple treatments are pro- posed as curettage and autologous bone graft, percutaneous local corticoids injections, decompression with internal fixation, and injection of bioresorbable cement. Decompression, curettage, and percutaneous bioresorbable cement injection showed interesting results, but until now, no long-term follow-up was reported in pediatric patients with UBC. Methods We retrospectively evaluated 13 pediatric patients with UBC treated with curettage, decompression, and injection of a calcium phosphate composite (CPC) at a single institution with an average F-U of 5.46 years (range 5–7 years). Func- tional outcomes were evaluated according to the Musculoskeletal Tumour Society (MSTS) Score. Radiographic healing was assessed with the modified Neer Outcome Rating System. Complications were recorded. Results The mean MSTS score was 29.61 (range 28–30). No joint limitation or any pain was recorded. All patients returned to their previous level of activity. Complete healed cysts were observed in 76.9% of patients (10 of 13) and partially healed in 23.1% (3 of 13). Three fractures of the humerus occurred without any further consequence. -

Treatment of Aneurysmal Bone Cysts with Titanium Elastic Nails in Children
Treatment of Aneurysmal Bone Cysts with Titanium Elastic Nails in Children Yi-chen Wang Children's Hospital of Shanghai Xing Jia Children's Hospital of Shanghai Yang Shen Children's Hospital of Shanghai Sun Wang Children's Hospital of Shanghai Liang-chao Dong Children's Hospital of Shanghai Jing Ren Children's Hospital of Shanghai Li-hua Zhao ( [email protected] ) Research Keywords: Primary aneurysmal bone cyst, Titanium Elastic Nails, recurrence, ecacy Posted Date: July 6th, 2020 DOI: https://doi.org/10.21203/rs.3.rs-38776/v1 License: This work is licensed under a Creative Commons Attribution 4.0 International License. Read Full License Page 1/16 Abstract Background: The main treatment method of the primary aneurysmal bone cyst (ABC) is to curettage and bone grafts with high-speed burring, radiotherapy, sclerotherapy, arterial embolism and hormone therapy can be used for the lesions whose location cannot be easily exposed by the surgery. Regardless of the method, high recurrence rates are a common problem. The purpose of this study was to evaluate retrospectively the use of titanium elastic nails as a internal xation in the treatment of aneurysmal bone cysts in children. Methods: Children with histological primary aneurysmal bone cyst were evaluated between 2010 to 2017. The patients were divided into 2 groups according to the treatment plan. Patients in the study group operated with curettage and bone grafts with high-speed burring + internal xation of titanium elastic nails (TEN), and patients in the control group operated with curettage and bone grafts with high-speed burring. The curative effect of the children in the 2 groups were analyzed statistically according to the imaging results (Neer grading) and MSTS functional evaluation. -

Case Report Chondroblastoma of The
CASE REPORT CHONDROBLASTOMA OF THE PATELLA ASSOCIATED WITH AN ANEURYSMAL BONE CYST R. TREBŠE1, A. ROTTER2,V. PIŠOT1 Chondroblastoma is a rare, benign tumor of bone, cartilage germ cells, and they redefined the tumor accounting for about 1% of all bone tumor cases. It as “benign chondroblastoma”. tends to affect the epiphyseal ends of long bones, Chondroblastoma is rare, representing about 1% most often in males during the first and second of all primary bone tumors (1, 5, 9). It is typically decades of life. It has well-characterized radio- centered in an epiphysis. Although it occurs most graphic and histologic features but despite its histo- often in the end of a long tubular bone, it can logically benign appearance a few cases of metastases appear in any secondary center of ossification. It is have been reported. Local recurrences after curet- tage and bone grafting occur in 11% to 25% of cases. most probably a tumor of cartilaginous origin and The features of a patellar chondroblastoma are the is more common in males by a ratio of about 2-to- same as for other locations. In reviewing the litera- 1 (1, 5, 9). Seventy percent of chondroblastomas ture we found an unusually high male-to-female occur during active epiphyseal plate growth, and ratio. It is interesting that the usual treatment of the about two-thirds of the patients are in the second patellar chondroblastoma has been patellectomy, decade of life (5). whereas curettage and bone grafting has predomi- Local pain of several months’ duration and nated in the other locations. -

Outcomes of Prophylactic Intramedullary Fixation for Benign Bone Lesions
Orginal Article 364 Outcomes of prophylactic intramedullary fixation for benign bone lesions İyi huylu kemik lezyonlarında profilaktik intramedüller fiksasyon sonuçları Çağrı Neyişci, Yusuf Erdem, Ahmet Burak Bilekli Gülhane Training and Research Hospital, Department of Orthopedics and Traumatology, Ankara, Turkey Dergiye Ulaşma Tarihi: 26.09.2019 Dergiye Kabul Tarihi: 29.09.2019 Doi: 10.5505/aot.2019.64325 ÖZET Amaç: Bu çalışmada benign kemik lezyonu sebebiyle profilaktik intramedüller tespit ameliyatı yaptığımız hastaların sonuçlarını sunmayı amaçladık. Gereç ve Yöntem: Bu çalışmaya 2008-2017 yılları arasında benign kemik lezyonu nedeni ile küretaj, greftleme ve profilaktik intramedüller tespit ameliyatı yaptığımız 22 hasta dâhil edilmiştir. Lezyonlar preoperatif dönemde Mirels sınıflamasına göre incelenerek patolojik kırık riski belirlenmiştir. Tüm hastaların tedavisinde küretaj, greftleme ve intramedüller tespit yöntemi kullanılmıştır. Kontrol muayenelerinde hastalar; eklem hareket açıklıklarına, ağrı durumuna, lezyonun ve implantın radyolojik görüntüsüne göre değerlendirilmiştir. Bulgular: Hastaların yaş ortalaması 24,8 (aralık, 7-38) yıldı. Hastalar ortalama 35,8 (aralık, 13-80) ay takip edildi. Çalışmaya dâhil edilen 21 hastanın ilk başvuru nedeni ağrı olup 2 hastada ağrı fonksiyon kaybına neden olmaktaydı. Patolojik humerus kırığı olan bir hasta akut ağrı ve fonksiyon kaybı ile başvurdu, iki ay konservatif olarak takip edildi ve ardından profilaktik cerrahi yapıldı. Hastaların ortalama Mirels skoru 9,3 (aralık, 9-10)’tü. Takiplerde tüm hastaların ekstremite fonksiyonları tamdı. Ameliyat sonrası ortalama VAS 8,09'dan 2,54'e gerilemiştir. Sonuç:9 veya daha fazla Mirels skoruna sahip olan iyi huylu kemik lezyonları için profilaktik fiksasyonun, olası patolojik kırık riskini azalttığı, VAS skorlarını azalttığı, ayrıca fonksiyon kaybını önlediği ve daha erken normal aktivitesine geri dönüşe olanak sağladığı sonucuna vardık. -

Benign Bone Tumors of the Foot and Ankle
CHAPTER 20 BENIGN BONE TUMORS OF THE FOOT AND ANKLE, Robert R. Miller, D.P.M. Stephen V. Corey, D.P.M. Benign bone tumors of the foot and ankle typically Table 1 displays the percentage of each lesion present both a diagnostic and therapeutic challenge found in the leg and foot. The lesions represent a to podiatric surgeons. These lesions have a percentage of local lesions compared to the total relatively low incidence of occuffence in the foot number of lesions reported for the studies. It does and ankle when compared to other regions of the seem apparent that the overall incidence of foot body, and the behavior of these lesions may mimic and ankle involvement is relatively low, but some malignant tumors. Not only is it impofiant to tumors do occur with a somewhat frequent rate. recognize a specific lesion to insure proper treat- Primarily, enchondroma, osteochondroma, osteoid ment, but the ability to differentiate a benign from osteoma, simple (unicameral) bone cysts, and malignant process is of utmost importance. aneurysmal bone cysts are somewhat common in It is difficult to determine the true incidence of the foot and ankle. benign bone tumors of the foot and ankle. Most large studies do not distinguish individual tarsal RADIOGRAPHIC CHARACTERISTICS OF bones, nor is there a distinction made befween BENIGN BONE TUMORS proximal and distal aspects of the tibia and fibula. Dahlin's Bone Tumors has reported findings of the Several radiographic parameters have been Mayo Clinic up until 7993.' total 2334 Of a of described to differentiate between benign and benign bone tumors affecting the whole body, malignant bone tumors. -

Treatment for Unicameral Bone Cysts in Long Bones: an Evidence Based
Orthopedic Reviews 2010; volume 2:e13 Treatment for unicameral bone unknown, it is estimated that approximately 75% of children present with pathological frac- Correspondence: Sandra Donaldson, cysts in long bones: ture.1 Cysts heal in less than 15% of children Orthopaedic Surgery, The Hospital for Sick an evidence based review following fracture.2 Although unicameral bone Children, S107-555 University Ave, cysts are believed to resolve with skeletal Toronto, Ontario, M5G 1X8, Canada. E-mail: [email protected] Sandra Donaldson,1 Josie Chundamala,2 maturity, without treatment these children are 3 2 Suzanne Yandow, James G. Wright at risk for pain, or recurrent fracture leading to Key words: unicameral bone cyst, pediatrics, 1Orthopaedic Surgery, The Hospital for activity restriction for many years. treatment, levels of evidence. Unicameral bone cysts may also lead to Sick Children, Toronto, Ontario, Canada; growth disturbance. Growth arrest, a relatively Contributions: SD and JC, analysis and interpreta- 2Department of Surgery, The Hospital for uncommon complication, may occur through tion of data, drafting the article, final approval of Sick Children, Toronto, Ontario, Canada; many mechanisms. The disruptive, hydrody- the version to be published; SY, analysis and inter- 3 Orthopaedic Surgery, Central Texas namic assault of cyst fluid on the physis may in pretation of data, revising article for important intellectual content, final approval of the version to Pediatric Orthopedics, Austin, Texas, itself result in growth disturbances.3 Other USA be published; JGW, conception and design; analy- rare causes for growth arrest include multiple sis and interpretation of data, revising article for fractures through the cyst that damage the important intellectual content, final approval of the physis, direct extension of the cyst through the version to be published and funding. -

Tuberculosis – the Masquerader of Bone Lesions in Children MN Rasool FCS(Orth) Department of Orthopaedics, University of Kwazulu-Natal
SAOJ Autumn 2009.qxd 2/27/09 11:11 AM Page 21 CLINICAL ARTICLE SA ORTHOPAEDIC JOURNAL Autumn 2009 / Page 21 C LINICAL A RTICLE Tuberculosis – the masquerader of bone lesions in children MN Rasool FCS(Orth) Department of Orthopaedics, University of KwaZulu-Natal Reprint requests: Dr MN Rasool Department of Orthopaedics University of KwaZulu-Natal Private Bag 7 Congella 4001 Tel: (031) 260 4297 Fax: (031) 260 4518 Email: [email protected] Abstract Fifty-three children with histologically confirmed tuberculous osteomyelitis were treated between 1989 and 2007. The age ranged from 1–12 years. There were 65 osseous lesions (excluding spinal and synovial). Seven had mul- tifocal bone involvement. Four basic types of lesions were seen: cystic (n=46), infiltrative (n=7), focal erosions (n=6) and spina ventosa (n=7). The majority of lesions were in the metaphyses (n=36); the remainder were in the diaphysis, epiphysis, short tubular bones, flat bones and small round bones. Bone lesions resembled chronic infections, simple and aneurysmal bone cysts, cartilaginous tumours, osteoid osteoma, haematological bone lesions and certain osteochondroses seen during the same period of study. Histological confirmation is man- datory to confirm the diagnosis of tuberculosis as several bone lesions can mimic tuberculous osteomyelitis. Introduction The variable radiological appearance of isolated bone Tuberculous osteomyelitis is less common than skeletal lesions in children can resemble various bone lesions tuberculosis involving the spine and joints. The destruc- including subacute and chronic osteomyelitis, simple and tive bone lesions of tuberculosis, the disseminated and the aneurysmal bone cysts, cartilaginous tumours, osteoid multifocal forms, are less common now than they were 50 osteoma, granulomatous lesions, haematological disease, 6,7,12 years ago.1-7 However, in recent series, solitary involve- and certain malignant tumours. -

1019 2 Feb 11 Weisbrode FINAL.Pages
The Armed Forces Institute of Pathology Department of Veterinary Pathology Wednesday Slide Conference 2010-2011 Conference 19 2 February 2011 Conference Moderator: Steven E. Weisbrode, DVM, PhD, Diplomate ACVP CASE I: 2173 (AFIP 2790938). Signalment: 3.5-month-old, male intact, Chow-Rottweiler cross, canine (Canis familiaris). History: This 3.5-month-old male Chow-Rottweiler mixed breed dog was presented to a veterinary clinic with severe neck pain. No cervical vertebral lesions were seen radiographically. The dog responded to symptomatic treatment. A week later the dog again presented with neck pain and sternal recumbency. The nose was swollen, and the submandibular and popliteal lymph nodes were moderately enlarged. The body temperature was normal. A complete blood count (CBC) revealed a marked lymphocytosis (23,800 lymphocytes/uI). Over a 3-4 hour period there was a noticeable increase in the size of all peripheral lymph nodes. Treatment included systemic antibiotics and corticosteroids. The dog became ataxic and developed partial paralysis. The neurologic signs waxed and waned over a period of 7 days, and the lymphadenopathy persisted. The peripheral blood lymphocyte count 5 days after the first CBC was done revealed a lymphocyte count of 6,000 lymphocytes/uI. The clinical signs became progressively worse, and the dog was euthanized two weeks after the initial presentation. Laboratory Results: Immunohistochemical (IHC) staining of bone marrow and lymph node sections revealed that tumor cells were negative for CD3 and CD79α. Gross Pathology: Marked generalized lymph node enlargement was found. Cut surfaces of the nodes bulged out and had a white homogeneous appearance. The spleen was enlarged and meaty. -

Musculoskeletal Radiology
MUSCULOSKELETAL RADIOLOGY Developed by The Education Committee of the American Society of Musculoskeletal Radiology 1997-1998 Charles S. Resnik, M.D. (Co-chair) Arthur A. De Smet, M.D. (Co-chair) Felix S. Chew, M.D., Ed.M. Mary Kathol, M.D. Mark Kransdorf, M.D., Lynne S. Steinbach, M.D. INTRODUCTION The following curriculum guide comprises a list of subjects which are important to a thorough understanding of disorders that affect the musculoskeletal system. It does not include every musculoskeletal condition, yet it is comprehensive enough to fulfill three basic requirements: 1.to provide practicing radiologists with the fundamentals needed to be valuable consultants to orthopedic surgeons, rheumatologists, and other referring physicians, 2.to provide radiology residency program directors with a guide to subjects that should be covered in a four year teaching curriculum, and 3.to serve as a “study guide” for diagnostic radiology residents. To that end, much of the material has been divided into “basic” and “advanced” categories. Basic material includes fundamental information that radiology residents should be able to learn, while advanced material includes information that musculoskeletal radiologists might expect to master. It is acknowledged that this division is somewhat arbitrary. It is the authors’ hope that each user of this guide will gain an appreciation for the information that is needed for the successful practice of musculoskeletal radiology. I. Aspects of Basic Science Related to Bone A. Histogenesis of developing bone 1. Intramembranous ossification 2. Endochondral ossification 3. Remodeling B. Bone anatomy 1. Cellular constituents a. Osteoblasts b. Osteoclasts 2. Non cellular constituents a. -

Massive Axial and Appendicular Skeletal Deformities in Connection with Gorham-Stout Syndrome
Case Report Massive Axial and Appendicular Skeletal Deformities in Connection with Gorham-Stout Syndrome Ali Al Kaissi 1,2,*, Sami Bouchoucha 3, Mohammad Shboul 4, Vladimir Kenis 5, Franz Grill 2, Rudolf Ganger 2 and Susanne Gerit Kircher 6 1 Ludwig Boltzmann Institute of Osteology, at the Hanusch Hospital of WGKK and, AUVA Trauma Centre Meidling, First Medical Department, Hanusch Hospital, 1090 Vienna, Austria 2 Orthopaedic Hospital of Speising, Paediatric department, 1090 Vienna, Austria; [email protected] (F.G.); [email protected] (R.G.) 3 Paediatric Orthopedic Surgery—Children Hospital, Tunis 1029, Tunis-Tunisia; [email protected] 4 Department of Medical Laboratory Sciences, Jordan University of Science and Technology, Irbid 22110, Jordan; [email protected] 5 Department of Foot and Ankle Surgery, Neuroorthopaedics and Systemic Disorders, Pediatric Orthopedic Institute n.a. H. Turner, Parkovaya str., 64-68, Pushkin, Saint Petersburg, Russia; [email protected] 6 Department of Medical Chemistry, Medical University of Vienna, 1090 Vienna, Austria; [email protected] * Correspondence: [email protected]; Tel. (Fax): +43-180-182-1260 Received: 26 March 2019; Accepted: 5 May 2019; Published: 7 May 2019 Abstract: Background: Etiological understanding is the corner stone in the management of skeletal deformities. Methods: Multi-centre study of patients with deformities in connection with diverse etiological backgrounds. We aimed to study four patients (one boy and three girls) with variable axial and appendicular deformities in connection with a vanishing bone disorder. Results: Axial deformities such as scoliosis, kyphoscoliosis, compressed fused vertebrae, appendicular fractures, dislocations, and vicious disorganization deformities of the joints were in connection with the vanishing bone disorder, namely Gorham-Stout syndrome. -
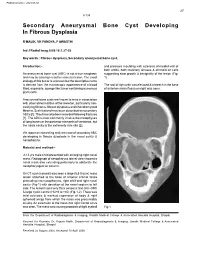
Secondary Aneurysmal Bone Cyst Developing in Fibrous Dysplasia
Published online: 2021-08-02 27 9-135 Secondary Aneurysmal Bone Cyst Developing In Fibrous Dysplasia R MALIK, VK PANDYA, P AWASTHI Ind J Radiol Imag 2006 16:1:27-28 Key words : Fibrous dysplasia, Secondary aneurysmal bone cyst. Introduction:- and pressure moulding with sclerosis of medial wall of both orbits, both maxillary sinuses & ethmoid air cells An aneurysmal bone cyst (ABC) is not a true neoplasm suggesting slow growth & benignitity of the lesion (Fig and may be a benign reactive vascular lesion. The exact 1). etiology of this tumor is unknown but the descriptive name is derived from the microscopic appearance of a blood The roof of right orbit was elevated & a breech in the base filled, expansile, sponge like tumor containing numerous of anterior cranial fossa on right was seen. giant cells. Aneurysmal bone cysts are known to arise in association with other abnormalities of the skeleton, particularly non ossifying fibroma, fibrous dysplasia and chondromyxoid fibroma. Such lesions have been described as secondary ABCs [1]. They have also been recorded following fractures [1]. The ABCs most commonly involve the metaphyses of long bones or the posterior elements of vertebrae, but the nasal cavity is the extremely rare site [2]. We report an interesting and rare case of secondary ABC developing in fibrous dysplasia in the nasal cavity & nasopharynx. Material and method:- A 13 yrs male child presented with enlarging right nasal mass. Radiograph of nasopharynx lateral view showed a nasal mass also extending posteriorly to obliterate the nasopharyngeal air column. On CT scan (coronal) was seen a large (5.5 X 6cm) mass lesion attached to the base of anterior cranial fossa protruding into nasopharynx, right orbit and right nasal cavity (Fig-1) with deviation of the nasal septum to left side. -

Bone Marrow Injection for Treatment of Aneurysmal Bone Cyst
MOJ Orthopedics & Rheumatology Bone Marrow Injection for Treatment of Aneurysmal Bone Cyst Research Article Abstract Volume 5 Issue 3 - 2016 Study design: Patients had Aneurysmal bone cyst lesion that underwent to be treated by Injection of Autologous Bone Marrow Aspirates (ABM) and follow up of this case for the final results. Patients and Methods: Sixteen patients had had Aneurysmal bone cyst had been treated by ABM injections. Study have 16 patients 11 females (68.75 %) and 5 Department of Orthopedics, Faculty of Medicine, Egypt Mahmoud I Abdel-Ghany, Assistant male (31.25 %). Age ranged from 3-14 years with average age 7.5 years. Number *Corresponding author: study including 5 cases (31.25 %) with proximal femoral cyst, 9 cases (56.25 %) Professor of Orthopedic and Trauma Surgery Faculty of of injections for every patient ranged from 2-6 times with average 4.4 times. This had tibial cyst (2 distal and 7 proximal tibiea) and 2 cases (12.5 %) had proximal Medicine for Girls, Egypt, Email: humeral cyst. All patients treated by injection of Autologous Bone Marrow Aspirates which obtained from the iliac crest. The bone marrow aspirates was Received: February 26, 2016 | Published: July 29, 2016 obtained percutaneous by bone marrow aspiration needle, According to follow up X-ray during injections we decide continuity of injections. Average size of the defect was 2.3 cm. and average amount bone marrow/inj. Was 10.2 cc. Results: Pain Score according to VAS ranged from 3-9 with average 5.7 which was improved to average 1.5 at final follow up.