Approach to Hematemesis and Gastrointestinal Bleeding Clinical Presentation of GI Bleeding
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Lower Gastrointestinal Bleeding
Journal of Experimental and Clinical Medicine https://dergipark.org.tr/omuJecm Re view Article J Exp Clin Med 2021; 38(S1): 23-32 doi: 10.52142/omujecm.38.si.gastro.3 Lower gastrointestinal bleeding Serkan ÖCAL1,* , Mehmet Mutlu ÇATLI2 1 Department of Gastroenterology, University of Health Sciences Antalya Training and Research Hospital, Antalya, Turkey 2Departmant of Internal Medicine, Antalya Training and Research Hospital, Antalya, Turkey Received: 13.12.2020 • Accepted/Published Online: 09.01.2021 • Final Version: 18.03.2021 Abstract Bleeding from the lower part of the digestive system that appears as hematocheZia (fresh blood, clot or cherry-colored stool) or melena (dark- colored tarry stool) is called lower gastrointestinal tract bleeding (lower GI bleeding) (or colonic bleeding). In the traditional definition, lower GI bleeding was generally classified as bleeding distal to the TreitZ ligament (duodenojejunal junction) as the border. In the last decade, GI bleeding has adopted three categories in some recent publications: Upper, middle, and lower. According to this category, bleeding from a source between the TreitZ ligament and the ileocecal valve is classified as middle GI bleeding, bleeding from the distal of the ileocecal valve is classified lower GI bleeding. Lower GI bleeding and hospitalization rates increase with aging. Currently, physicians managing lower GI bleeding have many different diagnostic and therapeutic options ranging from colonoscopy and flexible sigmoidoscopy to radiographic interventions such as scintigraphy or angiography. Lower GI bleeding often stops spontaneously and less common than upper GI bleeding. Even though no modality has emerged as the gold standard in the treatment of lower GI bleeding, colonoscopy has several advantages and is generally considered as the preferred initial test in most of the cases. -

Clinical Audit on Management of Hematemesis in Children Admitted to Pediatric Gastroenterology and Hepatology Unit of Assiut
Med. J. Cairo Univ., Vol. 86, No. 8, December: 4531-4536, 2018 www.medicaljournalofcairouniversity.net Clinical Audit on Management of Hematemesis in Children Admitted to Pediatric Gastroenterology and Hepatology Unit of Assiut University Children Hospital ESRAA T. AHMED, M.Sc.; FATMA A. ALI, M.D. and NAGLA H. ABU FADDAN, M.D. The Department of Pediatrics, Faculty of Medicine, Assiut University, Assiut, Egypt Abstract Hematemesis: Indicates that the bleeding origin is above the Treitz angle, i.e., that it constitutes an Background: Hematemesis is an uncommon but potentially Upper Gastrointestinal Bleeding (UGIB) [3] . serious and life-threatening clinical condition in children. It indicates that the bleeding origin is above the Treitz angle, The etiology of upper GI bleeding varies by i.e., that it constitutes an Upper Gastrointestinal Bleeding (UGIB). age. The pathophysiology of upper GI bleeding is related to the source of the bleeding. Most clinically Aim of Study: To assess for how much the adopted proto- significant causes of upper GI bleeds are associated cols of management of children with upper gastrointestinal bleeding were applied at Gastroenterology & Hepatology Unit with ulcers, erosive esophagitis, gastritis, varices, of Assiut University Children Hospital. and/or Mallory-Weiss tears. While Physiologic Patients and Methods: This study is a an audit on man- stress, NSAIDs such as aspirin and ibuprofen, and agement of children with upper gastrointestinal bleeding infection with Helicobacter pylori are few of the admitted to pediatric Gastroenterology and Hepatology Unit, factors contributing to the imbalance leading to Assiut University Children Hospital during the period from ulcers and erosions in the GI tract [4] . -

General Signs and Symptoms of Abdominal Diseases
General signs and symptoms of abdominal diseases Dr. Förhécz Zsolt Semmelweis University 3rd Department of Internal Medicine Faculty of Medicine, 3rd Year 2018/2019 1st Semester • For descriptive purposes, the abdomen is divided by imaginary lines crossing at the umbilicus, forming the right upper, right lower, left upper, and left lower quadrants. • Another system divides the abdomen into nine sections. Terms for three of them are commonly used: epigastric, umbilical, and hypogastric, or suprapubic Common or Concerning Symptoms • Indigestion or anorexia • Nausea, vomiting, or hematemesis • Abdominal pain • Dysphagia and/or odynophagia • Change in bowel function • Constipation or diarrhea • Jaundice “How is your appetite?” • Anorexia, nausea, vomiting in many gastrointestinal disorders; and – also in pregnancy, – diabetic ketoacidosis, – adrenal insufficiency, – hypercalcemia, – uremia, – liver disease, – emotional states, – adverse drug reactions – Induced but without nausea in anorexia/ bulimia. • Anorexia is a loss or lack of appetite. • Some patients may not actually vomit but raise esophageal or gastric contents in the absence of nausea or retching, called regurgitation. – in esophageal narrowing from stricture or cancer; also with incompetent gastroesophageal sphincter • Ask about any vomitus or regurgitated material and inspect it yourself if possible!!!! – What color is it? – What does the vomitus smell like? – How much has there been? – Ask specifically if it contains any blood and try to determine how much? • Fecal odor – in small bowel obstruction – or gastrocolic fistula • Gastric juice is clear or mucoid. Small amounts of yellowish or greenish bile are common and have no special significance. • Brownish or blackish vomitus with a “coffee- grounds” appearance suggests blood altered by gastric acid. -

Outpatient Services
Outpatient Services Coverage of Certain Services in the OUTPATIENT setting only* EFFECTIVE MARCH 9, 2015 bmchp.org | 888-566-0008 TO FIND A CODE OR WORD - While holding down the CTRL key, press the F key, type in Code, then press ENTER key Procedure Code Description 0213T Injection(s), diagnostic or therapeutic agent, paravertebral facet (zygapophyseal) joint (or nerves innervating that joint) with ultrasound guidance, cervical or thoracic; single level 0214T Injection(s), diagnostic or therapeutic agent, paravertebral facet (zygapophyseal) joint (or nerves innervating that joint) with ultrasound guidance, cervical or thoracic; second level (List separately in addition to code for primary procedure) 0215T Injection(s), diagnostic or therapeutic agent, paravertebral facet (zygapophyseal) joint (or nerves innervating that joint) with ultrasound guidance, cervical or thoracic; third and any additional level(s) (List separately in addition to code for primary procedure) 0216T Injection(s), diagnostic or therapeutic agent, paravertebral facet (zygapophyseal) joint (or nerves innervating that joint) with ultrasound guidance, lumbar or sacral; single level 0217T Injection(s), diagnostic or therapeutic agent, paravertebral facet (zygapophyseal) joint (or nerves innervating that joint) with ultrasound guidance, lumbar or sacral; second level (List separately in addition to code for primary procedure) 0218T Injection(s), diagnostic or therapeutic agent, paravertebral facet (zygapophyseal) joint (or nerves innervating that joint) with ultrasound -

Hemosuccus Pancreaticus: a Rare Cause of Upper Gastrointestinal Bleeding During Pregnancy Rani Akhil Bhat,1 Vani Ramkumar,1 K
Hemosuccus Pancreaticus: A Rare Cause Of Upper Gastrointestinal Bleeding During Pregnancy Rani Akhil Bhat,1 Vani Ramkumar,1 K. Akhil Krishnanand Bhat, 2 Rajgopal Shenoy2 Abstract Upper gastrointestinal bleeding is most commonly caused by From the 1Department of Department of Obstetrics and Gynaecology, Oman Medical 2 lesions in the esophagus, stomach or duodenum. Bleeding which College, Sohar, Sultanate of Oman, Department of Surgery, Oman Medical College, Sohar, Sultanate of Oma. originates from the pancreatic duct is known as hemosuccus pancreaticus. Only a few scattered case reports of hemosuccus Received: 06 Nov 2009 pancreaticus during pregnancy have been recorded in literature. Accepted: 31 Dec 2009 This is a case of a primigravida with 37 weeks of gestation Address correspondence and reprint request to: Dr. Rani A. Bhat,Department of with hemosuccus pancreaticus and silent chronic pancreatitis. Obstetrics and Gynaecology, Oman Medical College, P. O. Box 391, P. C. 321, Al- Evaluating pregnant women with upper gastrointestinal Tareef, Sohar, Sultanate of Oman. bleeding differs from that of non pregnant women as diagnostic E-mail: [email protected] modalities using radiation cannot be used. Therefore, Esophagogastroduodenoscopy should be performed at the time of active bleeding to diagnose hemosuccus pancreaticus. Bhat RA, et al. OMJ. 25 (2010); doi:10.5001/omj.2010.21 Introduction examination showed a combination of dark red blood and melena. Laboratory investigations revealed hemoglobin of 6.3 grams/dL, Hemosuccus pancreaticus is the term used to describe the liver function tests, serum amylase, glucose and prothrombin time syndrome of gastrointestinal bleeding into the pancreatic duct were within the normal range. -

Editorial Has the Time Come for Cyanoacrylate Injection to Become the Standard-Of-Care for Gastric Varices?
Tropical Gastroenterology 2010;31(3):141–144 Editorial Has the time come for cyanoacrylate injection to become the standard-of-care for gastric varices? Radha K. Dhiman, Narendra Chowdhry, Yogesh K Chawla The prevalence of gastric varices varies between 5% and 33% among patients with portal Department of Hepatology, hypertension with a reported incidence of bleeding of about 25% in 2 years and with a higher Postgraduate Institute of Medical bleeding incidence for fundal varices.1 Risk factors for gastric variceal hemorrhage include the education Research (PGIMER), size of fundal varices [more with large varices (as >10 mm)], Child class (C>B>A), and endoscopic Chandigarh, India presence of variceal red spots (defined as localized reddish mucosal area or spots on the mucosal surface of a varix).2 Gastric varices bleed less commonly as compared to esophageal Correspondence: Dr. Radha K. Dhiman, varices (25% versus 64%, respectively) but they bleed more severely, require more blood E-mail: [email protected] transfusions and are associated with increased mortality.3,4 The approach to optimal treatment for gastric varices remains controversial due to a lack of large, randomized, controlled trials and no clear clinical consensus. The endoscopic treatment modalities depend to a large extent on an accurate categorization of gastric varices. This classification categorizes gastric varices on the basis of their location in the stomach and their relationship with esophageal varices.1,5 Gastroesophageal varices are associated with varices along -

Chapter 156: Upper Gastrointestinal Bleeding
8/23/2018 Principles and Practice of Hospital Medicine, 2e > Chapter 156: Upper Gastrointestinal Bleeding Stephen R. Rotman; John R. Saltzman INTRODUCTION Key Clinical Questions What is the timing and treatment of peptic ulcer disease? What are the factors in diagnosis and treatment of aortoenteric fistula? What treatments are available for each etiology of upper GI bleeding? What is the appropriate management and follow-up of variceal bleeding? How do you estimate the severity of bleeding so that you can triage appropriate patients to the ICU, medical floor, or observation unit? Which patients are more likely to rebleed and hence require continued observation in the hospital aer their bleeding has apparently stopped, and for how long? Upper gastrointestinal (GI) bleeding is responsible for over 300,000 hospitalizations per year in the United States. An additional 100,000 to 150,000 patients develop upper GI bleeding during hospitalizations. The annual cost of treating nonvariceal acute upper GI bleeding in the United States exceeds $7 billion. Upper GI bleeding is defined as a bleeding source in the GI tract proximal to the ligament of Treitz. The presentation varies depending on the nature and severity of bleeding and includes hematemesis, melena, hematochezia (in rapid upper GI bleeding), and anemia with heme-positive stools. Bleeding can be associated with changes in vital signs, including tachycardia and hypotension including orthostatic hypotension. Given the range of presentations, pinpointing the nature and severity of GI bleeding may be a challenging task. The natural history of nonvariceal upper GI bleeding is that 80% of patients will stop bleeding spontaneously and no further urgent intervention will be needed. -

Overview of Esophageal and Gastric Varices
pISSN 2287-2728 eISSN 2287-285X https://doi.org/10.3350/cmh.2020.0022 Review Clinical and Molecular Hepatology 2020;26:444-460 Managing liver cirrhotic complications: Overview of esophageal and gastric varices Cosmas Rinaldi Adithya Lesmana1,2, Monica Raharjo1, and Rino A. Gani1 1Division of Hepatobiliary, Department of Internal Medicine, Dr. Cipto Mangunkusumo National General Hospital, Medical Faculty Universitas Indonesia, Jakarta; 2Digestive Disease & GI Oncology Centre, Medistra Hospital, Jakarta, Indonesia Managing liver cirrhosis in clinical practice is still a challenging problem as its progression is associated with serious complications, such as variceal bleeding that may increase mortality. Portal hypertension (PH) is the main key for the development of liver cirrhosis complications. Portal pressure above 10 mmHg, termed as clinically significant portal hypertension, is associated with formation of varices; meanwhile, portal pressure above 12 mmHg is associated with variceal bleeding. Hepatic vein pressure gradient measurement and esophagogastroduodenoscopy remain the gold standard for assessing portal pressure and detecting varices. Recently, non-invasive methods have been studied for evaluation of portal pressure and varices detection in liver cirrhotic patients. Various guidelines have been published for clinicians’ guidance in the management of esophagogastric varices which aims to prevent development of varices, acute variceal bleeding, and variceal rebleeding. This writing provides a comprehensive review on development of PH and varices in liver cirrhosis patients and its management based on current international guidelines and real experience in Indonesia. (Clin Mol Hepatol 2020;26:444-460) Keywords: Liver cirrhosis; Hypertension, Portal; Esophageal and gastric varices INTRODUCTION tes, hepatic encephalopathy, coagulation dysfunction, hepatorenal syndrome, and even cardiac and pulmonary complications. -

Flexible Video-Endsocopic Injection Sclerotherapy for Second and Third Degree Internal Hemorrhoids
Published online: 2019-09-26 ORIGINAL ARTICLE Flexible Video-Endsocopic Injection Sclerotherapy for Second and Third Degree Internal Hemorrhoids Sandeep Nijhawan, Udawat H, Gaurav Gupta, Anil Sharma, Amit Mathur, Bharat Sapra, Subhash Nepalia Department of Gastroenterology, SMS Medical College, Jaipur, Rajasthan, India ABSTRACT Background and objectives: Bleeding from hemorrhoids is the commonest cause of rectal bleeding in adults. Injection sclerotherapy of internal hemorrhoids is one of the non-surgical treatments, and is simple, safe and feasible. Conventionally sclerotherapy is performed with rigid proctoscope which has limitations of maneuverability, narrower field of vision and documentation compared to flexible videoendoscope. Therefore, we assessed the efficacy and safety of video-colonoscopic sclerotherapy for bleeding internal hemorrhides. Methods: Seventy-nine patients of bleeding internal hemorrhoids were subjected to colonoscopic sclerotherapy using 1.5% polidocanol in retroflexed or forward viewing positions. Success of treatment was defined as cessation of bleeding for six weeks. Patients were observed for complications and were followed up regularly for 3 months. Results: A total of 79 evaluable patients, 61 had grade II and 18 had grade III hemorrhoids. There was no statistically significant differences in achieving excellent or good results for control of bleeding between patients with grade II and grade III hemorrhoids (100% vs 94,5%; p>0.05). The number of sessions of sclerotherapy required were significantly more in grade II than grade III hemorrhoids (1.1 ± 0.3 vs 1.3 ± 0.7; p = 0.04). No significant complications were noted except for bloating in ten patients (12.6 %) and rectal pain in 6 (7.6%) patients. -
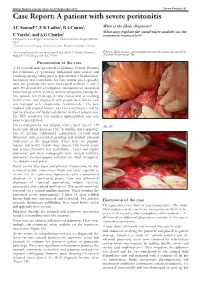
Case Report: a Patient with Severe Peritonitis
Malawi Medical Journal; 25(3): 86-87 September 2013 Severe Peritonitis 86 Case Report: A patient with severe peritonitis J C Samuel1*, E K Ludzu2, B A Cairns1, What is the likely diagnosis? 2 1 What may explain the small white nodules on the C Varela , and A G Charles transverse mesocolon? 1 Department of Surgery, University of North Carolina, Chapel Hill NC USA 2 Department of Surgery, Kamuzu Central Hospital, Lilongwe Malawi Corresponding author: [email protected] 4011 Burnett Womack Figure1. Intraoperative photograph showing the transverse mesolon Bldg CB 7228, Chapel Hill NC 27599 (1a) and the pancreas (1b). Presentation of the case A 42 year-old male presented to Kamuzu Central Hospital for evaluation of worsening abdominal pain, nausea and vomiting starting 3 days prior to presentation. On admission, his history was remarkable for four similar prior episodes over the previous five years that lasted between 3 and 5 days. He denied any constipation, obstipation or associated hematemesis, fevers, chills or urinary symptoms. During the first episode five years ago, he was evaluated at an outlying health centre and diagnosed with peptic ulcer disease and was managed with omeprazole intermittently . His past medical and surgical history was non contributory and he had no allergies and he denied alcohol intake or tobacco use. His HIV serostatus was negative approximately one year prior to presentation. On examination he was afebrile, with a heart rate of 120 (Fig 1B) beats/min, blood pressure 135/78 mmHg and respiratory rate of 22/min. Abdominal examination revealed mild distension with generalized guarding and marked rebound tenderness in the epigastrium. -

Esophageal Varices
View metadata, citation and similar papers at core.ac.uk brought to you by CORE provided by Crossref Hindawi Publishing Corporation Case Reports in Critical Care Volume 2016, Article ID 2370109, 4 pages http://dx.doi.org/10.1155/2016/2370109 Case Report A Rare but Reversible Cause of Hematemesis: (Downhill) Esophageal Varices Lam-Phuong Nguyen,1,2,3 Narin Sriratanaviriyakul,1,2,3 and Christian Sandrock1,2,3 1 Division of Pulmonary, Critical Care, and Sleep Medicine, University of California, Davis, Suite #3400, 4150 V Street, Sacramento, CA 95817, USA 2Department of Internal Medicine, University of California, Davis, Sacramento, USA 3VA Northern California Health Care System, Mather, USA Correspondence should be addressed to Lam-Phuong Nguyen; [email protected] Received 12 December 2015; Accepted 1 February 2016 Academic Editor: Kurt Lenz Copyright © 2016 Lam-Phuong Nguyen et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. “Downhill” varices are a rare cause of acute upper gastrointestinal bleeding and are generally due to obstruction of the superior vena cava (SVC). Often these cases of “downhill” varices are missed diagnoses as portal hypertension but fail to improve with medical treatment to reduce portal pressure. We report a similar case where recurrent variceal bleeding was initially diagnosed as portal hypertension but later found to have SVC thrombosis presenting with recurrent hematemesis. A 39-year-old female with history of end-stage renal disease presented with recurrent hematemesis. Esophagogastroduodenoscopy (EGD) revealed multiple varices. -

Palliative Care in Advanced Liver Disease (Marsano 2018)
Palliative Care in Advanced Liver Disease Luis Marsano, MD 2018 Mortality in Cirrhosis • Stable Cirrhosis: – Prognosis determined by MELD-Na score – Provides 90 day mortality. – http://www.mdcalc.com/meldna-meld-na-score-for-liver-cirrhosis/ • Acute on Chronic Liver Failure (ACLF) – Mortality Provided by CLIF-C ACLF Calculator – Provides mortality at 1, 3, 6 and 12 months. – http://www.clifresearch.com/ToolsCalculators.aspx • Acute Decompensation (without ACLF): – Mortality Provided by CLIF-C Acute decompensation Calculator – Provides mortality at 1, 3, 6 and 12 months. – http://www.clifresearch.com/ToolsCalculators.aspx • Survival of Ambulatory Patients with HCC (MESIAH) – Provides survival at 1, 3, 6, 12, 24 and 36 months. – https://www.mayoclinic.org/medical-professionals/model-end-stage-liver- disease/model-estimate-survival-ambulatory-hepatocellular-carcinoma-patients- mesiah Acute Decompensation Type and Mortality Organ Failure in Acute-on-Chronic Liver Failure Organ Failure Mortality Impact Frequency of Organ Failure 48% have >/= 2 Organ Failures The MESIAH Score Model of Estimated Survival In Ambulatory patients with HCC Complications of Cirrhosis Affecting Palliative Care • Ascites and Hepatic Hydrothorax. • Hyponatremia. • Hepatorenal syndrome. • Hepatic Encephalopathy. • Malnutrition/ Anorexia. • GI bleeding: Varices, Portal gastropathy & Gastric Antral Vascular Ectasia • Pruritus • Hepatopulmonary Syndrome. Difficult Decisions with Shifting Balance • Is patient a liver transplant candidate? • Effect of illness in: – patient’s survival – patient’s Quality of Life • patient’s relation to family • family’s Quality of Life • Effect of therapy in: – patient’s survival – patient’s Quality of Life • patient’s relation to family • family’s Quality of life Ascites and Palliation • PATHOGENESIS • CONSEQUENCES • Hepatic sinusoidal HTN • Abdominal distention with early stimulates hepatic satiety.