Pediatric Quick Notes
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Genes in Eyecare Geneseyedoc 3 W.M
Genes in Eyecare geneseyedoc 3 W.M. Lyle and T.D. Williams 15 Mar 04 This information has been gathered from several sources; however, the principal source is V. A. McKusick’s Mendelian Inheritance in Man on CD-ROM. Baltimore, Johns Hopkins University Press, 1998. Other sources include McKusick’s, Mendelian Inheritance in Man. Catalogs of Human Genes and Genetic Disorders. Baltimore. Johns Hopkins University Press 1998 (12th edition). http://www.ncbi.nlm.nih.gov/Omim See also S.P.Daiger, L.S. Sullivan, and B.J.F. Rossiter Ret Net http://www.sph.uth.tmc.edu/Retnet disease.htm/. Also E.I. Traboulsi’s, Genetic Diseases of the Eye, New York, Oxford University Press, 1998. And Genetics in Primary Eyecare and Clinical Medicine by M.R. Seashore and R.S.Wappner, Appleton and Lange 1996. M. Ridley’s book Genome published in 2000 by Perennial provides additional information. Ridley estimates that we have 60,000 to 80,000 genes. See also R.M. Henig’s book The Monk in the Garden: The Lost and Found Genius of Gregor Mendel, published by Houghton Mifflin in 2001 which tells about the Father of Genetics. The 3rd edition of F. H. Roy’s book Ocular Syndromes and Systemic Diseases published by Lippincott Williams & Wilkins in 2002 facilitates differential diagnosis. Additional information is provided in D. Pavan-Langston’s Manual of Ocular Diagnosis and Therapy (5th edition) published by Lippincott Williams & Wilkins in 2002. M.A. Foote wrote Basic Human Genetics for Medical Writers in the AMWA Journal 2002;17:7-17. A compilation such as this might suggest that one gene = one disease. -

Cutaneous Manifestations of Newborns in Omdurman Maternity Hospital
ﺑﺴﻢ اﷲ اﻟﺮﺣﻤﻦ اﻟﺮﺣﻴﻢ Cutaneous Manifestations of Newborns in Omdurman Maternity Hospital A thesis submitted in the partial fulfillment of the degree of clinical MD in pediatrics and child health University of Khartoum By DR. AMNA ABDEL KHALIG MOHAMED ATTAR MBBS University of Khartoum Supervisor PROF. SALAH AHMED IBRAHIM MD, FRCP, FRCPCH Department of Pediatrics and Child Health University of Khartoum University of Khartoum The Graduate College Medical and Health Studies Board 2008 Dedication I dedicate my study to the Department of Pediatrics University of Khartoum hoping to be a true addition to neonatal care practice in Sudan. i Acknowledgment I would like to express my gratitude to my supervisor Prof. Salah Ahmed Ibrahim, Professor of Peadiatric and Child Health, who encouraged me throughout the study and provided me with advice and support. I am also grateful to Dr. Osman Suleiman Al-Khalifa, the Dermatologist for his support at the start of the study. Special thanks to the staff at Omdurman Maternity Hospital for their support. I am also grateful to all mothers and newborns without their participation and cooperation this study could not be possible. Love and appreciation to my family for their support, drive and kindness. ii Table of contents Dedication i Acknowledgement ii Table of contents iii English Abstract vii Arabic abstract ix List of abbreviations xi List of tables xiii List of figures xiv Chapter One: Introduction & Literature Review 1.1 The skin of NB 1 1.2 Traumatic lesions 5 1.3 Desquamation 8 1.4 Lanugo hair 9 1.5 -

Acne in Childhood: an Update Wendy Kim, DO; and Anthony J
FEATURE Acne in Childhood: An Update Wendy Kim, DO; and Anthony J. Mancini, MD cne is the most common chron- ic skin disease affecting chil- A dren and adolescents, with an 85% prevalence rate among those aged 12 to 24 years.1 However, recent data suggest a younger age of onset is com- mon and that teenagers only comprise 36.5% of patients with acne.2,3 This ar- ticle provides an overview of acne, its pathophysiology, and contemporary classification; reviews treatment op- tions; and reviews recently published algorithms for treating acne of differing levels of severity. Acne can be classified based on le- sion type (morphology) and the age All images courtesy of Anthony J. Mancini, MD. group affected.4 The contemporary Figure 1. Comedonal acne. This patient has numerous closed comedones (ie, “whiteheads”). classification of acne based on sev- eral recent reviews is addressed below. Acne lesions (see Table 1, page 419) can be divided into noninflammatory lesions (open and closed comedones, see Figure 1) and inflammatory lesions (papules, pustules, and nodules, see Figure 2). The comedone begins with Wendy Kim, DO, is Assistant Professor of In- ternal Medicine and Pediatrics, Division of Der- matology, Loyola University Medical Center, Chicago. Anthony J. Mancini, MD, is Professor of Pediatrics and Dermatology, Northwestern University Feinberg School of Medicine, Ann and Robert H. Lurie Children’s Hospital of Chi- cago. Address correspondence to: Anthony J. Man- Figure 2. Moderate mixed acne. In this patient, a combination of closed comedones, inflammatory pap- ules, and pustules can be seen. cini, MD, Division of Dermatology Box #107, Ann and Robert H. -
Mongolian Spot
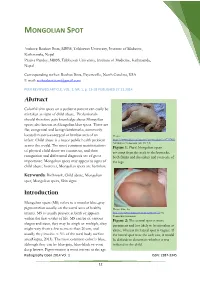
MONGOLIAN SPOT Authors: Roshan Bista, MBBS, Tribhuvan University, Institute of Medicine, Kathmandu, Nepal Prativa Pandey, MBBS, Tribhuvan University, Institute of Medicine, Kathmandu, Nepal Corresponding author: Roshan Bista, Fayetteville, North Carolina, USA E-mail: [email protected] PEER REVIEWED ARTICLE, VOL. 1, NR. 1, p. 12-18 PUBLISHED 27.11.2014 Abstract Colorful skin spots on a pediatric patient can easily be mistaken as signs of child abuse. Professionals should therefore gain knowledge about Mongolian spots; also known as Mongolian blue spots. These are flat, congenital and benign birthmarks, commonly located in sacro-coccygeal or lumbar area of an Photo: infant. Child abuse is a major public health problem https://www.flickr.com/photos/geowombats/1667757455 Attribution 2.0 Generic (CC BY 2.0) across the world. The most common manifestations Figure 1: Plural Mongolian spots of physical child abuse are cutaneous, and their covering from the neck to the buttocks, recognition and differential diagnosis are of great both flanks and shoulders and even one of importance. Mongolian spots may appear as signs of the legs. child abuse; however, Mongolian spots are harmless. Keywords: Birthmark, Child abuse, Mongolian spot, Mongolian spots, Skin signs Introduction Mongolian spots (MS) refers to a macular blue-gray pigmentation usually on the sacral area of healthy Photo: Abby Lu infants. MS is usually present at birth or appears http://creativecommons.org/licenses/by/2.0 via Wikimedia Commons within the first weeks of life. MS can be of various Figure 2: The central spot is more shapes and sizes, they may be single or multiple, they prominent and less likely to be mistaken as might vary from a few to more than 20 cm, and abuse, whereas the lateral spot is vaguer. -

Child Abuse: Skin Markers and Differential Diagnosis
527 527 REVISÃO L Violência contra a criança: indicadores dermatológicos e diagnósticos diferenciais* Child abuse: skin markers and differential diagnosis Roberta Marinho Falcão Gondim 1 Daniel Romero Muñoz 2 Valeria Petri 3 Resumo: As denúncias de abuso contra a criança têm sido frequentes e configuram grave problema de saúde pública. O tema é desconfortável para muitos médicos, seja pelo treinamento insuficiente, seja pelo desconhecimento das dimensões do problema. Uma das formas mais comuns de violência contra a criança é o abuso físico. Como órgão mais exposto e extenso, a pele é o alvo mais sujeito aos maus- tratos. Equimoses e queimaduras são os sinais mais visíveis. Médicos (pediatras, clínicos-gerais e derma- tologistas) costumam ser os primeiros profissionais a observar e reconhecer sinais de lesões não aciden- tais ou intencionais. Os dermatologistas podem auxiliar na distinção entre lesões traumáticas inten- cionais, acidentais e doenças cutâneas que mimetizam maus-tratos. Palavras-chave: Contusões; Equimose; Queimaduras; Violência doméstica; Violência sexual Abstract: Reports of child abuse have increased significantly. The matter makes most physicians uncom- fortable for two reasons: a) Little guidance or no training in recognizing the problem; b - Not under- standing its true dimension. The most common form of child violence is physical abuse. The skin is the largest and frequently the most traumatized organ. Bruises and burns are the most visible signs. Physicians (pediatricians, general practitioners and dermatologists) -

Prevalence of Non-Infectious Dermatoses in Patients Attending a Tertiary Care Center in Rajasthan
International Journal of Research in Dermatology Singh B et al. Int J Res Dermatol. 2019 Feb;5(1):192-196 http://www.ijord.com DOI: http://dx.doi.org/10.18203/issn.2455-4529.IntJResDermatol20190244 Original Research Article Prevalence of non-infectious dermatoses in patients attending a tertiary care center in Rajasthan 1 2 Bhagirath Singh , Indira Subhadarshini Paul * 1Department of Skin and V. D., 2Department of Paediatrics, Pacific Medical College and Hospital Udaipur, Rajasthan, India Received: 03 November 2018 Revised: 10 December 2018 Accepted: 12 December 2018 *Correspondence: Dr. Indira Subhadarshini Paul, E-mail: [email protected] Copyright: © the author(s), publisher and licensee Medip Academy. This is an open-access article distributed under the terms of the Creative Commons Attribution Non-Commercial License, which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited. ABSTRACT Background: Pediatric dermatoses require a separate view from adult dermatoses as there are important differences in clinical presentation, treatment and prognosis. There is very little epidemiological study available on non-infectious childhood dermatoses in India. The aims of the study were to find the prevalence, clinical profile and various etiological factors associated with childhood non-infectious dermatoses and to determine the prevalence of most common non-infectious childhood dermatoses. Methods: This cross-sectional observational study conducted at tertiary care centre in Rajasthan, India. Children with age 13 years and below with clinical evidence of cutaneous disorders were studied. Parents who have not given consent for the study, acutely ill children, Children having infectious dermatoses (bacterial, fungal, viral, arthropods, parasitic and protozoal infection) were excluded from the study. -

Hand Blisters in Major League Baseball Pitchers: Current Concepts and Management
A Review Paper Hand Blisters in Major League Baseball Pitchers: Current Concepts and Management Andrew R. McNamara, MD, Scott Ensell, MS, ATC, and Timothy D. Farley, MD Abstract Friction blisters are a common sequela of spent time on the DL due to blisters. More- many athletic activities. Their significance can over, there have been several documented range from minor annoyance to major per- and publicized instances of professional formance disruptions. The latter is particularly baseball pitchers suffering blisters that did true in baseball pitchers, who sustain repeat- not require placement on the DL but did ed trauma between the baseball seams and result in injury time and missed starts. the fingers of the pitching hand, predominate- The purpose of this article is to review ly at the tips of the index and long fingers. the etiology and pathophysiology of friction Since 2010, 6 Major League Baseball blisters with particular reference to baseball (MLB) players accounted for 7 stints on the pitchers; provide an overview of past and disabled list (DL) due to blisters. These inju- current prevention methods; and discuss ries resulted in a total of 151 days spent on our experience in treating friction blisters the DL. Since 2012, 8 minor league players in MLB pitchers. riction blisters result from repetitive friction of rubbing (erythroderma). This is followed by a and strain forces that develop between the pale, narrow demarcation, which forms around the F skin and various objects. Blisters form in reddened region. Subsequently, this pale area fills areas where the stratum corneum and stratum in toward the center to occupy the entire affected granulosum are sufficiently robust (Figure), such area, which becomes the blister lesion.1,2 as the palmar and plantar surfaces of the hand and Hydrostatic pressure then causes blister fluid feet. -

Download Download
Doi: 10.32677/IJCH.2017.v04.i04.024 Original Article Prevalence and presentation of cutaneous lesions in healthy neonates: A single-center study from Eastern India Mishra Shubhankar1, Mishra Pravakar2, Bhol Deepak Ranjan2, Agarwalla Sunil K2, Panigrahy Sambedana1, Mishra Swayamsiddha3 From Departments of Pediatrics, 1Kalinga Institute of Medical Sciences, Bhubaneswar, 2Maharaja Krushna Chandra Gajapati Medical College, Berhampur, Odisha, 3Department of Dermatology, Vydehi Institute of Medical Sciences, Bangalore, Karnataka, India Correspondence to: Dr. Pravakar Mishra, Department of Pediatrics, 1456 B, Sector 6, CDA, Markatnagar, Cuttack - 753 014, Odisha, India. Phone: +91-8908130041/+91-9437028882. E-mail: [email protected] Received – 06 March 2017 Initial Review – 06 April 2017 Published Online – 10 September 2017 ABSTRACT Background: Skin lesions are much common and specific to neonates. They vary according to age, sex, and geographic region. Objectives: The objective of this study was to determine the prevalence of different cutaneous lesions in newborns and their association with the type of delivery, age, sex, and maturity. Materials and Methods: This study was done in neonatal follow-up clinic of department of Pediatrics, Maharaja Krushna Chandra Gajapati Medical College, Berhampur, Odisha. All the healthy newborns coming to the OPD from January 2015 to December 2016 were included in this prospective study, and their details were recorded in case recording format after taking informed consent from their guardians. Admitted patients were excluded from the study. Statistical assessments were the done by SPSS software. Results: Out of 500 neonates, skin lesions were found in 366 (73.2%) patients. Physiological cutaneous lesions were most common, consisting 259 (70.7%) neonates. -

Orange Plaque on the Scalp P.33 6
DERM CASE Test your knowledge with multiple-choice cases This month – 10 cases: 1. Orange Plaque on the Scalp p.33 6. Generalized Pruritis in an Infant p.38 2. Slowly Enlarging Plaque p.34 7. Intensely Pruritic Lesions p.40 3. Painful Rash on Chest p.35 8. A Thick, Pruritic Growth p.41 4. Asymptomatic, Erythematous Papules p.36 9. Rough Spots on the Palms and Soles p.42 5. A Stain on the Forehead p.37 10. Oral, White Patches p.44 © right ibution py istr ad, Co l D ownlo Case 1 rcia can d me users use om orised sonal r C . Auth or per e o hibited copy f Sal se pro ingle for ised u rint a s ot author and p N Un y, view Orangedis pPla laque on the Scalp An 8-year-old female presents with an asympto - matic orange plaque on her scalp that has been pre - sent since birth. The plaque has grown as she has grown What is your diagnosis? a. Congenital melanocytic nevus b. Port wine stain c. Xanthoma d. Nevus sebaceous e. Xanthogranuloma Answer Nevus sebaceous (answer d) is a sharply circum - scribed yellow-orange plaque that presents at birth, It is a clinical diagnosis, although occasionally a most commonly on the face or scalp. It is less common biopsy is needed to verify the diagnosis. Full-thickness for the neck and face to be affected. Lesions are hairless excision has been the traditional treatment of choice, and persist throughout life. although watchful waiting and observation are also rea - With age, a nevus sebaceous becomes more verru - sonable options. -

Thermographic Imaging in Cats and Dogs Usability As a Clinical Method
Recent Publications in this Series MARI VAINIONPÄÄ 1/2014 Hanna Rajala Molecular Pathogenesis of Large Granular Lymphocytic Leukemia DISSERTATIONES SCHOLAE DOCTORALIS AD SANITATEM INVESTIGANDAM UNIVERSITATIS HELSINKIENSIS 2/2014 Thermographic Imaging in Cats and Dogs Usability as a Clinical Method MARI VAINIONPÄÄ Thermographic Imaging in Cats and Dogs Usability as a Clinical Method DEPARTMENT OF EQUINE AND SMALL ANIMAL MEDICINE FACULTY OF VETERINARY MEDICINE AND DOCTORAL PROGRAMME IN CLINICAL VETERINARY MEDICINE UNIVERSITY OF HELSINKI 2/2014 Helsinki 2014 ISSN 2342-3161 ISBN 978-952-10-9941-0 Department of Equine and Small Animal Medicine University of Helsinki Finland Thermographic imaging in cats and dogs Usability as a clinical method Mari Vainionpää, DVM ACADEMIC DISSERTATION To be presented, with the permission of the Faculty of Veterinary Medicine of the University of Helsinki, for public examination in Walter Hall, University EE building, on June 6th 2014, at noon. Helsinki 2014 SUPERVISED BY: Outi Vainio, DVM, PhD, Dipl. ECVPT, Professor Marja Raekallio, DVM, PhD, University Lecturer Marjatta Snellman, DVM, PhD, Dipl. ECVDI, Professor Emerita Department of Equine and Small Animal Medicine Faculty of Veterinary Medicine University of Helsinki Helsinki, Finland REVIEWED BY: Francis Ring, DSc, MSc, Professor Medical Imaging Research Unit Faculty of Advanced Technology University of South Wales Pontypridd, Wales, UK Ram Purohit DVM, PhD, Dipl. ACT, Professor Emeritus Department of Clinical Science College of Veterinary Medicine Auburn -

Neonatal and Infantile Acne
Neonatal and infantile acne Also known as neonatal acne, neonatal cephalic pustulosis What‘s the differene etween neonatal and infantile ane? Neonatal acne affects babies in the first 3 months of life. About 20% of healthy newborn babies may develop superficial pustules mostly on the face but also on the neck and upper trunk. There are no comedones (whiteheads or blackheads) present. Neonatal acne usually resolves without treatment. Infantile acne is the development of comedones (blackheads and whiteheads) with papules and pustules and occasionally nodules and cysts that may lead to scarring. It may occur in children from a few months of age and may last till 2 years of age. It is more common in boys. What causes infantile acne? Infantile acne is thought to be a result of testosterone temporarily causing an over-activity of the ski’s oil glads. I suseptile hildre this ay stiulate the development of acne. Most children are however otherwise healthy with no hormonal problem. The acne reaction usually subsides within 2 years. What does infantile acne look like? Infantile acne presents with whiteheads, blackheads, red papules and pustules, nodules and sometimes cysts that may lead to long term scarring. It most commonly affects the cheeks, chin and forehead with less frequent involvement of the body. How is infantile acne diagnosed? The diagnosis is made clinically and investigations are not usually required. However, if older children (2 to 6 years) develop acne and other symptoms such as body odour, breast and genital development, then hormonal screening blood tests should be considered. How is infantile acne treated? Treatment is usually with topical agents such as benzoyl peroxide, retinoid cream (adapalene) or antibiotic gel (erythromycin). -

OIICS Manual 2012
SECTION 4 Alphabetical Indices SECTION CONTENTS 4.1 Nature of Injury or Illness 4.2 Part of Body Affected 4.3 Source of Injury or Illness; Secondary Source of Injury or Illness 4.4 Event or Exposure *-Asterisks denote a summary level code not assigned to individual cases. _____________________________________________________________________________________________ 01/12 446 SECTION 4.1 Nature of Injury or Illness Index *-Asterisks denote a summary level code not assigned to individual cases. _____________________________________________________________________________________________ 01/12 447 NATURE CODE INDEX A 2831 Acne 2831 Acne varioliformis 3221 Abacterial meningitis 3211 Acquired immune deficiency syndrome 253 Abdominal hernia from repeated exertions (AIDS)—diagnosed 124 Abdominal hernia from single or short term 3199 Actinomycotic infections exertion 2819 Acute abscess of lymph gland or node 5174 Abdominal pain, unspecified 2359 Acute and subacute endocarditis 521 Abnormal blood-gas level 241 Acute bronchitis and bronchiolitis 521 Abnormal blood-lead level 2341 Acute cor pulmonale 525 Abnormal electrocardiogram (EKG, ECG), 195* Acute dermatitis electroencephalogram (EEG), 2819 Acute lymphadenitis electroretinogram (ERG) 2351 Acute myocarditis 52* Abnormal findings 2359 Acute pericarditis 521 Abnormal findings from examination of 2342 Acute pulmonary artery or vein embolism, blood nontraumatic 522 Abnormal findings from examination of 241 Acute respiratory infections (including urine common cold) 525 Abnormal findings from function