Infantile Spasms Parent Information Booklet
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Epilepsy in Childhood
Psychogenic Non-epileptic Seizures Dr Katharina Junejo Consultant Child and Adolescent Psychiatrist Aim Overview of basic principles in childhood epilepsy PNES Diagnosis of epilepsy Every child’s brain is capable of generating seizures with certain pro-convulsive drugs, acute metabolic disturbance, CNS infection, acute head trauma Risk of epilepsy after acute and provoked seizure is 3-5% Emotional stress is not considered provoking factor Henri Gastaut and colleagues proposed a classification of seizures: “all attempts at classification of seizures are hampered by our limited knowledge of the underlying pathological processes within the brain and that any classification must of necessity be a tentative one and will be subject to change with every advance in scientific understanding of epilepsy” (Gastaut et al 1964). Epilepsy has variable clinical presentations Convulsions (tonic- Staring spells clonic seizures) (absences) Period with confusion with or without Variants of automatism (complex paroxysmal events partial seizures) during sleep (common frontal lobe seizures) Limb or body jerk movements (myoclonus) Loss of speech/decline in Spasms (infantile or social, cognitive function Falls or drops epileptic spasms) (Landau-Kleffner (atonic but also syndrome) tonic seizures) ILAE Revised Terminology for Organization of Seizures and Epilepsies 2011 ‐ 2013 Classification of seizures: generalised and focal seizures Electroclinical syndromes and other epilepsies grouped by specificity of diagnosis (arranged by typical age of onset) Major conceptual changes: using aetiological classification of epilepsy-genetic, metabolic, immune, infectious and unknown causes Changes in terminology Operational diagnosis of epilepsy: occurrence of 2 or more unprovoked seizures, irrespective of seizure type (as recurrence risk is 80-90%) Careful history is only diagnostic test as many paroxysmal disorders that mimic epileptic seizures (most common vasovagal syncope or reflex anoxic seizure) Limitations of EEG: approx. -

Prognostic Utility of Hypsarrhythmia Scoring in Children with West
Clinical Neurology and Neurosurgery 184 (2019) 105402 Contents lists available at ScienceDirect Clinical Neurology and Neurosurgery journal homepage: www.elsevier.com/locate/clineuro Prognostic utility of hypsarrhythmia scoring in children with West syndrome T after ketogenic diet ⁎ Yunjian Zhang1, Lifei Yu1, Yuanfeng Zhou, Linmei Zhang, Yi Wang, Shuizhen Zhou Department of Pediatric Neurology, Children’s Hospital of Fudan University, China ARTICLE INFO ABSTRACT Keywords: Objective: The aim of this study was to evaluate the clinical efficacy and electroencephalographic (EEG) changes West syndrome of West syndrome after ketogenic diet (KD) therapy and to explore the correlation of EEG features and clinical Ketogenic diet efficacy. EEG Patients and methods: We retrospectively studied 39 patients with West syndrome who accepted KD therapy from Hypsarrhythmia May 2011 to October 2017. Outcomes including clinical efficacy and EEG features with hypsarrhythmia severity scores were analyzed. Results: After 3 months of treatment, 20 patients (51.3%) had ≥50% seizure reduction, including 4 patients (10.3%) who became seizure-free. After 6 months of treatment, 4 patients remained seizure free, 12 (30.8%) had 90–99% seizure reduction, 8 (20.5%) had a reduction of 50–89%, and 15 (38.5%) had < 50% reduction. Hypsarrhythmia scores were significantly decreased at 3 months of KD. They were associated with seizure outcomes at 6 months independent of gender, the course of disease and etiologies. Patients with a hypsar- rhythmia score ≥8 at 3 months of therapy may not be benefited from KD. Conclusion: Our findings suggest a potential benefit of KD for patients with drug-resistant West syndrome. Early change of EEG after KD may be a predictor of a patient’s response to the therapy. -

Pediatric Disorders
Neurological Disorder Part 3 - Pediatric Disorders CDKL5 Disorder • Characteristics: • Rare x-linked genetic disorder • CDLK5 mutations cause deficiencies in the protein needed for normal brain development • More common in females; however males with the disorder are affected much more severely than females © Trusted Neurodiagnostics Academy CDKL5 Disorder • Characteristics • CDKL5D mutations can be found in children who have been diagnosed with infantile spasms, Lennox Gastaut syndrome, Rett Syndrome, West Syndrome and autism © Trusted Neurodiagnostics Academy CDKL5 Disorder • Symptoms: • Infantile spasms beginning the first 3 - 6 months of life • Neurodevelopmental impairment • Patients cannot walk, talk, or feed themselves • Repetitive hand movements (stereotypies) © Trusted Neurodiagnostics Academy CDKL5 Disorder • Seizures: • Early onset • Infantile spasms, myoclonic, tonic, tonic-clonic seizures • Status epilepticus and non convulsive status epilepticus can occur © Trusted Neurodiagnostics Academy CDKL5 Disorder • Diagnosis: • Genetic blood testing to confirm the change or mutation on the CDKL5 gene • EEG © Trusted Neurodiagnostics Academy CDKL5 Disorder • EEG Findings: • Early in the disorder • EEG may be normal or slightly abnormal • During progression of the disorder • Some background activity is slow and epileptic discharges can be seen in one or more areas • Burst Suppression • Atypical hypsarrhythmia © Trusted Neurodiagnostics Academy CDKL5 Disorder © Trusted Neurodiagnostics Academy CDKL5 Disorder • Treatment: • Seizures -

“Seizures (Epilepsy)” a Seizure: Partial – Start in a Specific Part of the Brain, Not in the Whole � Is a Symptom of an Electrical Disturbance in the Brain Brain
“Seizures (Epilepsy)” A seizure: Partial – start in a specific part of the brain, not in the whole Is a symptom of an electrical disturbance in the brain brain. Unlike generalized seizures, partial seizures can have a Is a rare event warning before they occur (aura). Auras are actually a kind of Has a typical beginning (best clue for accurate diagnosis) seizure. There are several different kinds of partial seizures: Is involuntary simple (motor, sensory or psychological), complex, partial Lasts only a short time (90% complete in 90 seconds) seizure with secondary generalization. May cause post seizure impairments. Most seizures do not involve convulsions. Accurate seizure diagnosis by the health care provider is very The most common type of seizure is one mostly involving important because the medications used to treat seizures often vary loss of awareness. depending on the type. There are 20 types of seizures in the Seizures can be very subtle and hard to notice. International Classification of Seizures (over 2,000 types reported in the literature). Examples of post-seizure impairments: A detailed description of the seizure by the person observing the Post ictal confusion (length is individual) seizure is necessary for accurate diagnosing. Having a seizure while in Initial difficulty speaking the doctor’s office is very rare. Confusion about when, where, or what was just happening Memory disturbance which can last a while (behaving Seizure observation: - 3 important ones to make (in order of usual normally but can’t retain/absorb information) importance): Headache with some kinds of seizures What happened right as the seizure was beginning? What is epilepsy? What happened after the seizure was over? What happened during the seizure? Epilepsy is a condition where a person has “recurrent, unprovoked” seizures. -

Operational Classification of Seizure Types by the International League Against Epilepsy: Position Paper of the ILAE Commission
ILAE POSITION PAPER Operational classification of seizure types by the International League Against Epilepsy: Position Paper of the ILAE Commission for Classification and Terminology *Robert S. Fisher, †J. Helen Cross, ‡Jacqueline A. French, §Norimichi Higurashi, ¶Edouard Hirsch, #Floor E. Jansen, **Lieven Lagae, ††Solomon L. Moshe, ‡‡Jukka Peltola, §§Eliane Roulet Perez, ¶¶Ingrid E. Scheffer, and ##***Sameer M. Zuberi Epilepsia, 58(4):522–530, 2017 doi: 10.1111/epi.13670 SUMMARY The International League Against Epilepsy (ILAE) presents a revised operational clas- sification of seizure types. The purpose of such a revision is to recognize that some sei- zure types can have either a focal or generalized onset, to allow classification when the onset is unobserved, to include some missing seizure types, and to adopt more trans- parent names. Because current knowledge is insufficient to form a scientifically based classification, the 2017 Classification is operational (practical) and based on the 1981 Classification, extended in 2010. Changes include the following: (1) “partial” becomes “focal”; (2) awareness is used as a classifier of focal seizures; (3) the terms dyscognitive, simple partial, complex partial, psychic, and secondarily generalized are eliminated; Dr. Robert S. Fisher, (4) new focal seizure types include automatisms, behavior arrest, hyperkinetic, auto- past president of nomic, cognitive, and emotional; (5) atonic, clonic, epileptic spasms, myoclonic, and American Epilepsy tonic seizures can be of either focal or generalized onset; (6) focal to bilateral tonic– Society and editor of clonic seizure replaces secondarily generalized seizure; (7) new generalized seizure Epilepsia and types are absence with eyelid myoclonia, myoclonic absence, myoclonic–atonic, epilepsy.com, led the myoclonic–tonic–clonic; and (8) seizures of unknown onset may have features that can Seizure Classification still be classified. -

Levetiracetam-Associated Psychogenic Non-Epileptic Seizures
Original Research DOI: 10.22374/1710-6222.25.2.1 LEVETIRACETAM-ASSOCIATED PSYCHOGENIC NON-EPILEPTIC SEIZURES: A HIDDEN PARADOX Shaik Afshan Jabeen,1 Padmaja Gaddamanugu,1 Ajith Cherian,2 Kandadai Rukmini Mridula,2 Dasari Uday Kumar,1 Angamuttu kanikannan Meena1 1Deptartment of Neurology Nizam’s Institute of Medical Sciences, Hyderabad, India. 2Department of Neurology, Sree Chitra Tirunal Institute of Medical Sciences. Thiruvananthapuram, India. Corresponding Author: [email protected] Submitted: August 16, 2017. Accepted: May 31, 2018. Published: June 15, 2018. ABSTRACT Objectives To study the clinical profile and outcome in patients with epilepsy who developed psychogenic non-epileptic seizures (PNES) associated with levetiracetam (LEV) use. Methods In this prospective observational study, conducted over 1 year, 13 patients with epilepsy and PNES, docu- mented by video electroencephalogram (VEEG) while on LEV, were included. Those with past history of psychiatric illnesses were excluded. VEEG, high-resolution magnetic resonance imaging, neuropsychologi- cal and psychiatric evaluation were performed. Patients in Group I (07) were treated with psychotherapy, psychiatric medications and immediate withdrawal of LEV while, those in Group II (06) received psy- chotherapy, anxiolytics and LEV for initial 2 months after which it was stopped. Follow-up period was six months. Results Mean (±SD) age of patients was 25 ± 12.28 years; there were 11 (84.62%) females. All were on antiepileptic agents which included LEV >1000 mg/day, except one. Mean dose of LEV was 1269.23 ± 483.71 mg/day. J Popul Ther Clin Pharmacol Vol 25(2):1-11; June 15, 2018. This article is distributed under the terms of the Creative Commons Attribution-Non Commercial 4.0 International License. -

Understanding Seizures and Epilepsy
Understanding Sei zures & Epilepsy Selim R. Benbadis, MD Leanne Heriaud, RN Comprehensive Epilepsy Program Table of Contents * What is a seizure and what is epilepsy?....................................... 3 * Who is affected by epilepsy? ......................................................... 3 * Types of seizures ............................................................................. 3 * Types of epilepsy ............................................................................. 6 * How is epilepsy diagnosed? .......................................................... 9 * How is epilepsy treated? .............................................................. 10 Drug therapy ......................................................................... 10 How medication is prescribed ............................................ 12 Will treatment work?............................................................ 12 How long will treatment last?............................................. 12 Other treatment options....................................................... 13 * First aid for a person having a seizure ....................................... 13 * Safety and epilepsy ....................................................................... 14 * Epilepsy and driving..................................................................... 15 * Epilepsy and pregnancy ............................................................... 15 * More Information .......................................................................... 16 Comprehensive -

Occipital and Parietal Lobe Epilepsies
Chapter 15 Occipital and parietal lobe epilepsies JOHN S. DUNCAN UCL Institute of Neurology, National Hospital for Neurology and Neurosurgery, Queen Square, London Epileptic seizures of parietal and occipital origin are heterogeneous and mainly characterised by the presenting auras, although the most dramatic clinical manifestations may reflect spread, and overshadow the focal origin. The two lobes serve mainly sensory functions, and the characteristic seizure phenomena are therefore subjective sensations. The incidence of these seizures is not well known, but they are generally considered rare. Occipital seizures have been reported to constitute 8% and parietal seizures 1.4% of total seizures in the prevalent population with epilepsy1,2. The pattern of seizures is most commonly focal seizures without impairment of awareness, with occasional secondary generalisation. Focal seizures with impairment of awareness are rare and usually indicate spread of the seizure into the temporal lobe. Seizures with somatosensory symptomatology1-3 Somatosensory seizures may arise from any of the three sensory areas of the parietal lobe, but the post-central gyrus is most commonly involved. Seizures present with contralateral, or rarely ipsilateral, or bilateral sensations. All sensory modalities may be represented, most commonly tingling and numbness, alone or together. There may be prickling, tickling or crawling sensations, or a feeling of electric shock in the affected body part. The arms and the face are the most common sites, but any segment or region may be affected. The paraesthesia may spread in a Jacksonian manner, and when this occurs motor activity in the affected body member follows the sensations in about 50% of cases. -
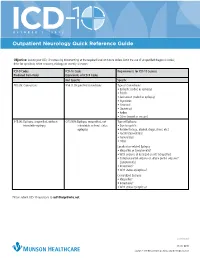
Outpatient Neurology Quick Reference Guide
OCTOBER 1, 2015 Outpatient Neurology Quick Reference Guide Objective: Ensure your ICD-10 success by documenting at the required level on future orders. Limit the use of unspecified diagnosis codes; drive for specificity when anatomy, etiology, or severity is known. ICD-9 Codes ICD-10 Code Requirements for ICD-10 Success Produced from Order Equivalents of ICD-9 Codes Not Specific Specific 780.39: Convulsions R56.9: Unspecified convulsions Type of Convulsions: • Epileptic (coded as epilepsy) • Febrile • Jacksonian (coded as epilepsy) • Myoclonic • Neonatal • Obstetrical • Reflex • Other (coded as seizure) 345.90: Epilepsy, unspecified, without G40.909: Epilepsy, unspecified, not Type of Epilepsy: intractable epilepsy intractable, without status • Due to syphilis epileptus • Related to (e.g., alcohol, drugs, stress, etc.) • Localization-related • Generalized • Other Localization-related Epilepsy • Idiopathic or Symptomatic? • With seizures of localized onset? (idiopathic) • Complex partial seizures or simple partial seizures? (symptomatic) • Intractable? • With status epilepticus? Generalized Epilepsy • Idiopathic? • Intractable? • With status epilepticus? Please submit ICD-10 questions to [email protected]. continued 11372 08/15 Copyright © 2015 Munson Healthcare, Traverse City, MI. All rights reserved. OCTOBER 1, 2015 Outpatient Neurology Quick Reference Guide Specific ICD-10-CM Codes Code Definition Convulsions R56.01 Complex febrile convulsions R53.00 Simple febrile convulsions G25.3 Myoclonus R25.8 Other abnormal involuntary movements -

Investigation of Seizures in Infants
Chapter 23 Investigation of seizures in infants RICHARD E. APPLETON1 and AILSA McLELLAN2 1The Roald Dahl EEG Unit, Paediatric Neurosciences Foundation, Alder Hey Children’s NHS Foundation Trust, Liverpool, and 2Department of Paediatric Neurosciences, Royal Hospital for Sick Children, Edinburgh The investigation of seizures in infancy (i.e. within the first year of life) begins with establishing whether the seizures are epileptic or non-epileptic in origin. The ‘broad’ differential diagnosis of possible seizures and ‘epilepsy’ is multiple and is particularly difficult under the age of 12 months and includes: Gastro-oesophageal reflux (Sandifer’s syndrome) Pallid syncopal attacks (reflex anoxic seizures) Cyanotic breath-holding attacks Cardiac arrhythmias Münchausen syndrome by proxy (passive or active both representing a form of child abuse) Shuddering spells and jitteriness Hyperekplexia Benign neonatal sleep myoclonus Benign myoclonus of infancy Tonic reflex activity and involuntary movements (seen in children with neurological impairment including cerebral palsy or hydrocephalus). Once a non-epileptic disorder has been excluded or the episodes are considered to be obviously epileptic, then the following conditions/investigations should be considered on a chronological basis. Perinatal (first week of life) and neonatal (first month of life) seizures The newborn period is the time of life with the highest risk of seizures1-3. This is because of the relative lack, and immature development of inhibitory neurotransmitters and their pathways. The immature and developing brain is susceptible to a large number of both cerebral and systemic insults including: Asphyxia (hypoxic-ischaemic encephalopathy) the most common and also most serious cause of neonatal seizures – particularly in term infants Intra- and periventricular haemorrhage – particularly in pre-term infants Metabolic dysfunction (e.g. -

Genes of Early-Onset Epileptic Encephalopathies: from Genotype to Phenotype
Pediatric Neurology 46 (2012) 24e31 Contents lists available at ScienceDirect Pediatric Neurology journal homepage: www.elsevier.com/locate/pnu Review Article Genes of Early-Onset Epileptic Encephalopathies: From Genotype to Phenotype Mario Mastrangelo MD, Vincenzo Leuzzi MD * Division of Child Neurology, Department of Pediatrics, Child Neurology, and Psychiatry, Sapienza University of Rome, Rome, Italy article information abstract Article history: Early-onset epileptic encephalopathies are severe disorders in which cognitive, sensory, and motor Received 26 July 2011 development is impaired by recurrent clinical seizures or prominent interictal epileptiform discharges Accepted 24 October 2011 during the neonatal or early infantile periods. They include Ohtahara syndrome, early myoclonic epileptic encephalopathy, West syndrome, Dravet syndrome, and other diseases, e.g., X-linked myoclonic seizures, spasticity and intellectual disability syndrome, idiopathic infantile epileptic-dyskinetic encephalopathy, epilepsy and mental retardation limited to females, and severe infantile multifocal epilepsy. We summarize recent updates on the genes and related clinical syndromes involved in the pathogenesis of early-onset epileptic encephalopathies: Aristaless-related homeobox (ARX), cyclin- dependent kinase-like 5 (CDKL5), syntaxin-binding protein 1 (STXBP1), solute carrier family 25 member 22 (SLC25A22), nonerythrocytic a-spectrin-1 (SPTAN1), phospholipase Cb1(PLCb1), membrane- associated guanylate kinase inverted-2 (MAGI2), polynucleotide kinase -

Infantile Spasms: an Update on Pre-Clinical Models and EEG Mechanisms
children Review Infantile Spasms: An Update on Pre-Clinical Models and EEG Mechanisms Remi Janicot, Li-Rong Shao and Carl E. Stafstrom * Division of Pediatric Neurology, The Johns Hopkins University School of Medicine, Baltimore, MD 21287, USA; [email protected] (R.J.); [email protected] (L.-R.S.) * Correspondence: [email protected]; Tel.: +1-(410)-955-4259; Fax: +1-(410)-614-2297 Received: 19 November 2019; Accepted: 23 December 2019; Published: 6 January 2020 Abstract: Infantile spasms (IS) is an epileptic encephalopathy with unique clinical and electrographic features, which affects children in the middle of the first year of life. The pathophysiology of IS remains incompletely understood, despite the heterogeneity of IS etiologies, more than 200 of which are known. In particular, the neurobiological basis of why multiple etiologies converge to a relatively similar clinical presentation has defied explanation. Treatment options for this form of epilepsy, which has been described as “catastrophic” because of the poor cognitive, developmental, and epileptic prognosis, are limited and not fully effective. Until the pathophysiology of IS is better clarified, novel treatments will not be forthcoming, and preclinical (animal) models are essential for advancing this knowledge. Here, we review preclinical IS models, update information regarding already existing models, describe some novel models, and discuss exciting new data that promises to advance understanding of the cellular mechanisms underlying the specific EEG changes seen in IS—interictal hypsarrhythmia and ictal electrodecrement. Keywords: infantile spasms; West syndrome; epilepsy; childhood; epileptic encephalopathy; electroencephalogram (EEG); hypsarrhythmia; electrodecrement; animal model 1. Introduction Epileptic encephalopathies (EEs) are a spectrum of disorders that mostly begin during infancy and have poor neurological and behavioral outcomes.