Hearing and Vestibular Disorders in the Workplace
Total Page:16
File Type:pdf, Size:1020Kb

Load more
Recommended publications
-
HEARING LOSS, DEAFNESS Ear32 (1)
HEARING LOSS, DEAFNESS Ear32 (1) Hearing Loss, Deafness Last updated: May 11, 2019 CLASSIFICATION, DIAGNOSIS ................................................................................................................. 1 METHODS OF COMMUNICATION FOR DEAF ............................................................................................ 2 MANAGEMENT ......................................................................................................................................... 2 HEARING AIDS (S. AMPLIFICATION) ....................................................................................................... 2 COCHLEAR IMPLANTS ............................................................................................................................ 2 AUDITORY BRAINSTEM IMPLANTS .......................................................................................................... 4 PREVENTION .......................................................................................................................................... 4 PEDIATRIC HEARING DEFICITS ............................................................................................................... 4 ETIOLOGY .............................................................................................................................................. 4 DIAGNOSIS ............................................................................................................................................. 6 TREATMENT .......................................................................................................................................... -

Pediatric Sensorineural Hearing Loss, Part 2: Syndromic And
Published May 19, 2011 as 10.3174/ajnr.A2499 Pediatric Sensorineural Hearing Loss, Part 2: REVIEW ARTICLE Syndromic and Acquired Causes B.Y. Huang SUMMARY: This article is the second in a 2-part series reviewing neuroimaging in childhood SNHL. C. Zdanski Previously, we discussed the clinical work-up of children with hearing impairment, the classification of inner ear malformations, and congenital nonsyndromic causes of hearing loss. Here, we review and M. Castillo illustrate the most common syndromic hereditary and acquired causes of childhood SNHL, with an emphasis on entities that demonstrate inner ear abnormalities on cross-sectional imaging. Syndromes discussed include BOR syndrome, CHARGE syndrome, Pendred syndrome, Waardenburg syndrome, and X-linked hearing loss with stapes gusher. We conclude the article with a review of acquired causes of childhood SNHL, including infections, trauma, and neoplasms. ABBREVIATIONS: BOR ϭ branchio-oto-renal; CISS ϭ constructive interference in steady state; IAC ϭ internal auditory canal; NF-2 ϭ neurofibromatosis type II; SCC ϭ semicircular canal; SNHL ϭ sensorineural hearing loss; T1WI ϭ T1-weighted image; T2 WI ϭ T2-weighted image he estimated prevalence of SNHL in patients younger than Table 1: Selected hereditary syndromes commonly associated with 1 T18 years of age is 6 per 1000, making it one of the leading SNHL causes of childhood disability and a common reason for oto- Inner Ear Malformations on Inner Ear Malformations laryngology referrals. Cross-sectional imaging is now rou- Imaging Not Common on Imaging tinely performed in these patients because it provides impor- Alagille syndrome Alport syndrome tant information about potential etiologies for hearing loss, Branchio-oto-renal syndrome Biotinidase deficiency defines the anatomy of the temporal bone and the central au- CHARGE syndrome Jervell and Lange-Nielsen syndrome ditory pathway, and identifies additional intracranial abnor- Klippel-Feil syndrome Norrie syndrome malities that may require further work-up. -
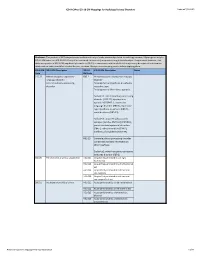
ICD-9/10 Mapping Spreadsheet
ICD-9-CM to ICD-10-CM Mappings for Audiology Related Disorders Updated 7/16/2015 Disclaimer: This product is NOT comprehensive and consists only of codes commonly related to audiology services. Mappings are only to ICD-10-CM codes, not ICD-10-PCS. Every effort was made to accurately map codes using detailed analysis. Keep in mind, however, that while many codes in ICD-9-CM map directly to codes in ICD-10, in some cases, additional clinical analysis may be required to determine which code or codes should be selected for your situation. Always review mapping results before applying them. ICD-9-CM ICD-9-CM Description ICD-10- ICD-10-CM Description Notes Code CM Code 315.32 Mixed receptive-expressive F80.2 Mixed receptive-expressive language language disorder disorder Central auditory processing Developmental dysphasia or aphasia, disorder receptive type Developmental Wernicke's aphasia Excludes1: central auditory processing disorder (H93.25), dysphasia or aphasia NOS (R47.-), expressive language disorder (F80.1), expressive type dysphasia or aphasia (F80.1), word deafness (H93.25) Excludes2: acquired aphasia with epilepsy [Landau-Kleffner] (G40.80-), pervasive developmental disorders (F84.-), selective mutism (F94.0), intellectual disabilities (F70-F79) H93.25 Central auditory processing disorder Congenital auditory imperception Word deafness Excludes1: mixed receptive-epxressive language disorder (F80.2) 380.00 Perichondritis of pinna, unspecified H61.001 Unspecified perichondritis of right external ear H61.002 Unspecified perichondritis -

Vestibular Neuritis and Labyrinthitis
Vestibular Neuritis and DISORDERS Labyrinthitis: Infections of the Inner Ear By Charlotte L. Shupert, PhD with contributions from Bridget Kulick, PT and the Vestibular Disorders Association INFECTIONS Result in damage to inner ear and/or nerve. ARTICLE 079 DID THIS ARTICLE HELP YOU? SUPPORT VEDA @ VESTIBULAR.ORG Vestibular neuritis and labyrinthitis are disorders resulting from an 5018 NE 15th Ave. infection that inflames the inner ear or the nerves connecting the inner Portland, OR 97211 ear to the brain. This inflammation disrupts the transmission of sensory 1-800-837-8428 information from the ear to the brain. Vertigo, dizziness, and difficulties [email protected] with balance, vision, or hearing may result. vestibular.org Infections of the inner ear are usually viral; less commonly, the cause is bacterial. Such inner ear infections are not the same as middle ear infections, which are the type of bacterial infections common in childhood affecting the area around the eardrum. VESTIBULAR.ORG :: 079 / DISORDERS 1 INNER EAR STRUCTURE AND FUNCTION The inner ear consists of a system of fluid-filled DEFINITIONS tubes and sacs called the labyrinth. The labyrinth serves two functions: hearing and balance. Neuritis Inflamation of the nerve. The hearing function involves the cochlea, a snail- shaped tube filled with fluid and sensitive nerve Labyrinthitis Inflamation of the labyrinth. endings that transmit sound signals to the brain. Bacterial infection where The balance function involves the vestibular bacteria infect the middle organs. Fluid and hair cells in the three loop-shaped ear or the bone surrounding semicircular canals and the sac-shaped utricle and Serous the inner ear produce toxins saccule provide the brain with information about Labyrinthitis that invade the inner ear via head movement. -

Vestibular Neuritis, Labyrinthitis, and a Few Comments Regarding Sudden Sensorineural Hearing Loss Marcello Cherchi
Vestibular neuritis, labyrinthitis, and a few comments regarding sudden sensorineural hearing loss Marcello Cherchi §1: What are these diseases, how are they related, and what is their cause? §1.1: What is vestibular neuritis? Vestibular neuritis, also called vestibular neuronitis, was originally described by Margaret Ruth Dix and Charles Skinner Hallpike in 1952 (Dix and Hallpike 1952). It is currently suspected to be an inflammatory-mediated insult (damage) to the balance-related nerve (vestibular nerve) between the ear and the brain that manifests with abrupt-onset, severe dizziness that lasts days to weeks, and occasionally recurs. Although vestibular neuritis is usually regarded as a process affecting the vestibular nerve itself, damage restricted to the vestibule (balance components of the inner ear) would manifest clinically in a similar way, and might be termed “vestibulitis,” although that term is seldom applied (Izraeli, Rachmel et al. 1989). Thus, distinguishing between “vestibular neuritis” (inflammation of the vestibular nerve) and “vestibulitis” (inflammation of the balance-related components of the inner ear) would be difficult. §1.2: What is labyrinthitis? Labyrinthitis is currently suspected to be due to an inflammatory-mediated insult (damage) to both the “hearing component” (the cochlea) and the “balance component” (the semicircular canals and otolith organs) of the inner ear (labyrinth) itself. Labyrinthitis is sometimes also termed “vertigo with sudden hearing loss” (Pogson, Taylor et al. 2016, Kim, Choi et al. 2018) – and we will discuss sudden hearing loss further in a moment. Labyrinthitis usually manifests with severe dizziness (similar to vestibular neuritis) accompanied by ear symptoms on one side (typically hearing loss and tinnitus). -

Hearing Loss, Vertigo and Tinnitus
HEARING LOSS, VERTIGO AND TINNITUS Jonathan Lara, DO April 29, 2012 Hearing Loss Facts S Men are more likely to experience hearing loss than women. S Approximately 17 percent (36 million) of American adults report some degree of hearing loss. S About 2 to 3 out of every 1,000 children in the United States are born deaf or hard-of-hearing. S Nine out of every 10 children who are born deaf are born to parents who can hear. Hearing Loss Facts S The NIDCD estimates that approximately 15 percent (26 million) of Americans between the ages of 20 and 69 have high frequency hearing loss due to exposure to loud sounds or noise at work or in leisure activities. S Only 1 out of 5 people who could benefit from a hearing aid actually wears one. S Three out of 4 children experience ear infection (otitis media) by the time they are 3 years old. Hearing Loss Facts S There is a strong relationship between age and reported hearing loss: 18 percent of American adults 45-64 years old, 30 percent of adults 65-74 years old, and 47 percent of adults 75 years old or older have a hearing impairment. S Roughly 25 million Americans have experienced tinnitus. S Approximately 4,000 new cases of sudden deafness occur each year in the United States. Hearing Loss Facts S Approximately 615,000 individuals have been diagnosed with Ménière's disease in the United States. Another 45,500 are newly diagnosed each year. S One out of every 100,000 individuals per year develops an acoustic neurinoma (vestibular schwannoma). -

Hearing Loss
Randal W. Swenson, M.D. Joshua G. Yorgason, M.D. David K. Palmer, M.D. Wesley R. Brown, M.D. John E. Butler, M.D. Nancy J. Stevenson, PA-C Justin D. Gull, M.D. ENT SPECIALISTS Kristin G. Hoopes, PA-C www.entslc.com Hearing Loss Approximately one in ten persons in the United may result from blockage of the ear canal (wax), States has some degree of hearing loss. Hearing is from a perforation (hole) in the ear drum, or from measured in decibels (dB), and a hearing level of 0- infection or disease of any of the three middle ear 25 dB is considered normal hearing. Your level is: bones. With a conductive loss only, the patient will never go deaf, but will always be able to hear, either Right ear _______ dB Left ear _______dB with reconstructive ear surgery or by use of a properly fitted hearing aid. Some patients who are Hearing Severity / % Loss not candidates for surgery, may benefit from a new 25 dB (normal).….0% 65dB(Severe)……...60% technology, the Baha (bone-anchored hearing aid). 35 dB (mild)……..15% 75dB(Severe)……...75% When there is a problem with the inner ear or 45 dB (moderate)..30% >85dB (Profound)..>90% nerve of hearing, a sensori-neural hearing loss occurs. This is most commonly from normal aging, Normal speech discrimination is 88-100%. Yours is: is usually worse in high frequencies, and can progress to total deafness. Noise exposure is another Right ear _______ % Left ear_______% common cause of high frequency hearing loss. Patients with sensori-neural hearing loss usually complain of difficulty hearing in loud environments. -

Vestibular Neuritis and Labyrinthitis: Infections of the Inner
PO BOX 13305 · PORTLAND, OR 97213 · FAX: (503) 229-8064 · (800) 837-8428 · [email protected] · WWW.VESTIBULAR.ORG Vestibular Neuritis and Labyrinthitis Infections of the Inner Ear By Charlotte L. Shupert, PhD with contributions from Bridget Kulick, PT and the Vestibular Disorders Association Vestibular neuritis and labyrinthitis are Infections of the inner ear are usually disorders resulting from an infection that viral; less commonly, the cause is inflames the inner ear or the nerves bacterial. Such inner ear infections are connecting the inner ear to the brain. This not the same as middle ear infections, inflammation disrupts the transmission of which are the type of bacterial infections sensory information from the ear to the common in childhood affecting the area brain. Vertigo, dizziness, and difficulties around the eardrum. with balance, vision, or hearing may result. Inner ear structure and function The inner ear consists of a system of fluid-filled tubes and sacs (see diagram © Vestibular Disorders Association ◦ www.vestibular.org ◦ Page 1 of 6 on page 2) called the labyrinth. The Labyrinthitis (inflammation of the labyrinth serves two functions: hearing labyrinth) occurs when an infection and balance. affects both branches of the vestibulo- cochlear nerve, resulting in hearing The hearing function involves the cochlea, changes as well as dizziness or vertigo. a snail-shaped tube filled with fluid and sensitive nerve endings that transmit Bacterial and viral infections sound signals to the brain. Inner ear infections that cause vestibular neuritis or labyrinthitis are usually viral The balance function involves the rather than bacterial. Although the vestibular organs. Fluid and hair cells in symptoms of bacterial and viral infections the three loop-shaped semicircular canals may be similar, the treatments are very and the sac-shaped utricle and saccule different, so proper diagnosis by a provide the brain with information about physician is essential. -

Good Practice Guide for Social Workers in England and Wales Working with Adults with Acquired Hearing Loss
Good Practice Guide for Social Workers in England and Wales Working with Adults with Acquired Hearing Loss Brian Crellin, Peter Simcock & Jacqui Bond www.basw.co.uk Contents Forewords ..................................................................................................................................... 3 About the Authors ...................................................................................................................... 4 Introduction ................................................................................................................................. 5 Definitions ................................................................................................................................... 6 What is acquired hearing loss? ...................................................................................................... 6 Types of Acquired Hearing Loss ................................................................................................... 9 Registration and Acquired Hearing Loss ..................................................................................... 9 Incidence and Prevalence of Acquired Hearing Loss ........................................................ 10 Medical Assessment of Hearing Loss ....................................................................................12 Tinnitus and its Treatment .............................................................................................................13 Meniere’s Disease and its Treatment ......................................................................................... -

Resources Resources
RESOURCES RESOURCES Pediatric audiological Service ProviderS For Children with Hearing Loss In Central Ohio Columbus City Schools Phone: 614-365-5977 Huy Elementary/A. G. Bell Program FAX: 614-365-5491 Columbus Hearing Impaired Program (C.H.I.P.) TTY: 614-365-5977 1545 Huy Road Columbus, Ohio 43224 Website: Columbus.k12.oh.us/agbell Diagnostic Audiological Evaluation: Infants Screenings (Birth–12 Months) or OAE o ABR 0-6 7-23 24-36 (months) Hearing Aid Services: OAE or or ro o Hearing Aids ro Loaner Hearing Aids ABR o o o o Monitored Sedation o Medical/ENT Evaluation ASSR o o o Tympanometry o or ro ro FM technology in the classroom Cochlear Implant Services: (Check all that applies to your services) o Comprehensive Cochlear Implant Program – Medical team; ENT Cochlear Implant, Surgeon, CI Coordinator, Audiologist, Speech & Language Pathologist, Psychologist, Social Worker, Occupational Therapist, Physical Therapist o Cochlear Implant Candidacy Evaluation o ENT Cochlear Implant Surgeon ro Psychologist ro Audiologist ro Speech & Language Pathologist ro Counselor ro Occupational Therapy ro Physical Therapy Financial: N/A – School System o Insurance Accepted o Medicaid Provider o BCMH (Ohio) Provider o Financial Assistance We are part of a school system and only serve those children enrolled in Columbus City Schools or in the Regional Infant Hearing Program (ages 0-3 years). If you have any questions or would like to discuss please call Rachel Nadal, Au.D. 614-365-5977. 154 Pediatric Audiological Service Providers Information in this section was provided by the individual service providers. If a provider is not listed, they did not submit information. -

Radiology in Vertigo and Dizziness
10.5005/jp-journals-10003-1092 DeepakREVIEW Patkar ARTICLE et al Radiology in Vertigo and Dizziness Deepak Patkar, Girish Yevankar, Rashmi Parikh ABSTRACT • Cerebellopontine angle tumor Objective: Vertigo may or may not be associated with hearing • Cerebrovascular disease, such as transient ischemic loss. In addition, the imaging findings are often subtle. attack or stroke Underdiagnosis of cause of vertigo on imaging can lead to long • Migraine standing annoying symptom of vertigo. • Multiple sclerosis Conclusion: This article reviews the radiologic findings of • Other causes vertigo. After completing this article, the readers should have • Cervical vertigo an improved ability to diagnose the common causes of vertigo, • Drug-induced vertigo using the optimal imaging tools to achieve this goal. • Psychological Keywords: American College of Radiology, Magnetic The appropriate imaging modality depends upon the resonance imaging, Magnetic resonance angiogram. associated symptoms and is guided by ACR criterion as How to cite this article: Patkar D, Yevankar G, Parikh R. given in Table 1 (ACR Appropriateness Criteria)**.9 Radiology in Vertigo and Dizziness. Otorhinolaryngol Clin Int J 2012;4(2):86-92. Labyrinthitis Source of support: Nil Labyrinthitis is an inflammation of the membranous Conflict of interest: None declared labyrinth10 and can be divided according to etiology as follows: INTRODUCTION • Tympanogenic Imaging plays an important role in the diagnosis and • Post-traumatic treatment of the patients with vestibular abnormalities. • Meningogenic There are multiple imaging tools available for the • Hematogenic patients with vestibular and temporal bone abnormalities • Autoimmune viz computed tomography (CT) scan, magnetic resonance Prior to MRI, no imaging findings were described; imaging (MRI) including MR angiography and digital however, now enhancement of the labyrinth on postcontrast subtraction angiography. -

Education Labyrinthitis and Vestibular Neuritis
Education Labyrinthitis and Vestibular Neuritis What are labyrinthitis and vestibular neuritis? Labyrinthitis is an inflammation of the inner ear. Vestibular neuritis is an inflammation of the nerves connecting the inner ear to the brain. The inner ear is made up of a system of fluid-filled tubes and sacs called the labyrinth. The labyrinth contains an organ for hearing called the cochlea. It also contains the vestibular system, which helps you keep your balance. How do they occur? Generally viruses cause the inflammation. In vestibular neuritis, a virus similar to the herpes virus causes an infection. This infection causes swelling and inflammation of the vestibular nerves or the labyrinth. Sometimes bacteria from a middle ear infection cause labyrinthitis. What are the symptoms? Symptoms of vestibular neuritis and labyrinthitis are: dizziness or vertigo (feeling like the room is spinning) trouble keeping your balance nausea. Vestibular neuritis and labyrinthitis are rarely painful. If you have pain, get treatment right away. After a few days, the symptoms may decrease so that you have symptoms only when you move suddenly. A sudden turn of the head is the most common movement that causes symptoms. How are they diagnosed? Your health care provider will ask about your symptoms and examine you. Often, no other testing is needed. However, if your symptoms last for more than a month, see your health care provider again. Let your health care provider know if your symptoms are getting worse. You may have the following tests: A hearing test. An electronystagmogram (ENG). The ENG checks eye movements as a way to get information about the vestibular system.