Tamoxifen Resistance: Emerging Molecular Targets
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Hedgehog Signaling Is Evolutionarily Conserved Cilium-Independent
Downloaded from genesdev.cshlp.org on August 14, 2009 - Published by Cold Spring Harbor Laboratory Press Cilium-independent regulation of Gli protein function by Sufu in Hedgehog signaling is evolutionarily conserved Miao-Hsueh Chen, Christopher W. Wilson, Ya-Jun Li, et al. Genes Dev. 2009 23: 1910-1928 Access the most recent version at doi:10.1101/gad.1794109 Supplemental http://genesdev.cshlp.org/content/suppl/2009/07/23/23.16.1910.DC1.html Material References This article cites 97 articles, 47 of which can be accessed free at: http://genesdev.cshlp.org/content/23/16/1910.full.html#ref-list-1 Email alerting Receive free email alerts when new articles cite this article - sign up in the box at the service top right corner of the article or click here To subscribe to Genes & Development go to: http://genesdev.cshlp.org/subscriptions Copyright © 2009 by Cold Spring Harbor Laboratory Press Downloaded from genesdev.cshlp.org on August 14, 2009 - Published by Cold Spring Harbor Laboratory Press Cilium-independent regulation of Gli protein function by Sufu in Hedgehog signaling is evolutionarily conserved Miao-Hsueh Chen,1,3 Christopher W. Wilson,1,3 Ya-Jun Li,1 Kelvin King Lo Law,2 Chi-Sheng Lu,1 Rhodora Gacayan,1 Xiaoyun Zhang,2 Chi-chung Hui,2 and Pao-Tien Chuang1,4 1Cardiovascular Research Institute, University of California at San Francisco, San Francisco, California 94158, USA; 2Program in Developmental and Stem Cell Biology, The Hospital for Sick Children, and Department of Molecular Genetics, University of Toronto, Toronto, Ontario M5G 1L7, Canada A central question in Hedgehog (Hh) signaling is how evolutionarily conserved components of the pathway might use the primary cilium in mammals but not fly. -

Gli Transcription Factors Mediate the Oncogenic Transformation of Prostate Basal Cells Induced by a Kras-Androgen Receptor Axis*
crossmark THE JOURNAL OF BIOLOGICAL CHEMISTRY VOL. 291, NO. 49, pp. 25749–25760, December 2, 2016 © 2016 by The American Society for Biochemistry and Molecular Biology, Inc. Published in the U.S.A. Gli Transcription Factors Mediate the Oncogenic Transformation of Prostate Basal Cells Induced by a Kras-Androgen Receptor Axis*□S Received for publication, August 12, 2016, and in revised form, September 28, 2016 Published, JBC Papers in Press, October 19, 2016, DOI 10.1074/jbc.M116.753129 Meng Wu‡, Lishann Ingram‡, Ezequiel J. Tolosa§, Renzo E. Vera§, Qianjin Li‡, Sungjin Kim‡, Yongjie Ma‡, Demetri D. Spyropoulos¶, Zanna Beharryʈ, Jiaoti Huang**, Martin E. Fernandez-Zapico§, and Houjian Cai‡1 From the ‡Department of Pharmaceutical and Biomedical Sciences, College of Pharmacy, University of Georgia, Athens, Georgia 30602, the §Schulze Center for Novel Therapeutics, Division of Oncology Research, Mayo Clinic, Rochester, Minnesota 55905, the ¶Department of Pathology and Laboratory Medicine, Medical University of South Carolina, Charleston, South Carolina 29425, the ʈDepartment of Chemistry and Physics, Florida Gulf Coast University, Fort Myers, Florida 33965, and the **Department of Pathology, School of Medicine, Duke University, Durham, North Carolina 27710 Edited by Eric Fearon Although the differentiation of oncogenically transformed cer progression has been characterized with multiple stages, 2 basal progenitor cells is one of the key steps in prostate tumori- including benign, prostatic intraepithelial neoplasia (PIN), Downloaded from genesis, the mechanisms mediating this cellular process are still invasive adenocarcinoma, and metastatic cancer (2). Numerous ؉ largely unknown. Here we demonstrate that an expanded p63 oncogenic driver genes, including loss of tumor suppressors, ؉ and CK5 basal/progenitor cell population, induced by the con- overexpression, and/or activation of oncogenes, have been comitant activation of oncogenic Kras(G12D) and androgen identified based on genetic analysis of clinical prostate tumors. -

Mir-338-3P Is Regulated by Estrogens Through GPER in Breast Cancer Cells and Cancer-Associated Fibroblasts (Cafs)
cells Article miR-338-3p Is Regulated by Estrogens through GPER in Breast Cancer Cells and Cancer-Associated Fibroblasts (CAFs) Adele Vivacqua 1,*, Anna Sebastiani 1, Anna Maria Miglietta 2, Damiano Cosimo Rigiracciolo 1, Francesca Cirillo 1, Giulia Raffaella Galli 1, Marianna Talia 1, Maria Francesca Santolla 1, Rosamaria Lappano 1, Francesca Giordano 1, Maria Luisa Panno 1 and Marcello Maggiolini 1,* 1 Department of Pharmacy, Health and Nutritional Sciences, University of Calabria, 87036 Rende, Italy; [email protected] (A.S.); [email protected] (D.C.R.); [email protected] (F.C.); [email protected] (G.R.G.); [email protected] (M.T.); [email protected] (M.F.S.); [email protected] (R.L.); [email protected] (F.G.); [email protected] (M.L.P.) 2 Regional HospitalCosenza, 87100 Cosenza, Italy; [email protected] * Correspondence: [email protected] (A.V.); [email protected] (M.M.); Tel.: +39-0984-493-048 (A.V.); +39-0984-493-076 (M.M.) Received: 12 October 2018; Accepted: 7 November 2018; Published: 9 November 2018 Abstract: Estrogens acting through the classic estrogen receptors (ERs) and the G protein estrogen receptor (GPER) regulate the expression of diverse miRNAs, small sequences of non-coding RNA involved in several pathophysiological conditions, including breast cancer. In order to provide novel insights on miRNAs regulation by estrogens in breast tumor, we evaluated the expression of 754 miRNAs by TaqMan Array in ER-negative and GPER-positive SkBr3 breast cancer cells and cancer-associated fibroblasts (CAFs) upon 17β-estradiol (E2) treatment. Various miRNAs were regulated by E2 in a peculiar manner in SkBr3 cancer cells and CAFs, while miR-338-3p displayed a similar regulation in both cell types. -

Non-Canonical Activation of Hedgehog in Prostate Cancer Cells Mediated by the Interaction of Transcriptionally Active Androgen Receptor Proteins with Gli3
Oncogene (2018) 37:2313–2325 https://doi.org/10.1038/s41388-017-0098-7 ARTICLE Non-canonical activation of hedgehog in prostate cancer cells mediated by the interaction of transcriptionally active androgen receptor proteins with Gli3 1 1,2 2 1 1 1 2,3 Na Li ● Sarah Truong ● Mannan Nouri ● Jackson Moore ● Nader Al Nakouzi ● Amy Anne Lubik ● Ralph Buttyan Received: 19 July 2017 / Revised: 18 October 2017 / Accepted: 29 November 2017 / Published online: 12 February 2018 © The Author(s) 2018. This article is published with open access Abstract Hedgehog (Hh) is an oncogenic signaling pathway that regulates the activity of Gli transcription factors. Canonical Hh is a Smoothened-(Smo-) driven process that alters the post-translational processing of Gli2/Gli3 proteins. Though evidence supports a role for Gli action in prostate cancer (PCa) cell growth and progression, there is little indication that Smo is involved. Here we describe a non-canonical means for activation of Gli transcription in PCa cells mediated by the binding of transcriptionally-active androgen receptors (ARs) to Gli3. Androgens stimulated reporter expression from a Gli-dependent promoter in a variety of AR + PCa cells and this activity was suppressed by an anti-androgen, Enz, or by AR knockdown. 1234567890();,: Androgens also upregulated expression of endogenous Gli-dependent genes. This activity was associated with increased intranuclear binding of Gli3 to AR that was antagonized by Enz. Fine mapping of the AR binding domain on Gli2 showed that AR recognizes the Gli protein processing domain (PPD) in the C-terminus. Mutations in the arginine-/serine repeat elements of the Gli2 PPD involved in phosphorylation and ubiquitinylation blocked the binding to AR. -

Profiling G Protein-Coupled Receptors of Fasciola Hepatica Identifies Orphan Rhodopsins Unique to Phylum Platyhelminthes
bioRxiv preprint doi: https://doi.org/10.1101/207316; this version posted October 23, 2017. The copyright holder for this preprint (which was not certified by peer review) is the author/funder, who has granted bioRxiv a license to display the preprint in perpetuity. It is made available under aCC-BY-NC-ND 4.0 International license. 1 Profiling G protein-coupled receptors of Fasciola hepatica 2 identifies orphan rhodopsins unique to phylum 3 Platyhelminthes 4 5 Short title: Profiling G protein-coupled receptors (GPCRs) in Fasciola hepatica 6 7 Paul McVeigh1*, Erin McCammick1, Paul McCusker1, Duncan Wells1, Jane 8 Hodgkinson2, Steve Paterson3, Angela Mousley1, Nikki J. Marks1, Aaron G. Maule1 9 10 11 1Parasitology & Pathogen Biology, The Institute for Global Food Security, School of 12 Biological Sciences, Queen’s University Belfast, Medical Biology Centre, 97 Lisburn 13 Road, Belfast, BT9 7BL, UK 14 15 2 Institute of Infection and Global Health, University of Liverpool, Liverpool, UK 16 17 3 Institute of Integrative Biology, University of Liverpool, Liverpool, UK 18 19 * Corresponding author 20 Email: [email protected] 21 1 bioRxiv preprint doi: https://doi.org/10.1101/207316; this version posted October 23, 2017. The copyright holder for this preprint (which was not certified by peer review) is the author/funder, who has granted bioRxiv a license to display the preprint in perpetuity. It is made available under aCC-BY-NC-ND 4.0 International license. 22 Abstract 23 G protein-coupled receptors (GPCRs) are established drug targets. Despite their 24 considerable appeal as targets for next-generation anthelmintics, poor understanding 25 of their diversity and function in parasitic helminths has thwarted progress towards 26 GPCR-targeted anti-parasite drugs. -

The Role of Gli3 in Inflammation
University of New Hampshire University of New Hampshire Scholars' Repository Doctoral Dissertations Student Scholarship Winter 2020 THE ROLE OF GLI3 IN INFLAMMATION Stephan Josef Matissek University of New Hampshire, Durham Follow this and additional works at: https://scholars.unh.edu/dissertation Recommended Citation Matissek, Stephan Josef, "THE ROLE OF GLI3 IN INFLAMMATION" (2020). Doctoral Dissertations. 2552. https://scholars.unh.edu/dissertation/2552 This Dissertation is brought to you for free and open access by the Student Scholarship at University of New Hampshire Scholars' Repository. It has been accepted for inclusion in Doctoral Dissertations by an authorized administrator of University of New Hampshire Scholars' Repository. For more information, please contact [email protected]. THE ROLE OF GLI3 IN INFLAMMATION BY STEPHAN JOSEF MATISSEK B.S. in Pharmaceutical Biotechnology, Biberach University of Applied Sciences, Germany, 2014 DISSERTATION Submitted to the University of New Hampshire in Partial Fulfillment of the Requirements for the Degree of Doctor of Philosophy In Biochemistry December 2020 This dissertation was examined and approved in partial fulfillment of the requirement for the degree of Doctor of Philosophy in Biochemistry by: Dissertation Director, Sherine F. Elsawa, Associate Professor Linda S. Yasui, Associate Professor, Northern Illinois University Paul Tsang, Professor Xuanmao Chen, Assistant Professor Don Wojchowski, Professor On October 14th, 2020 ii ACKNOWLEDGEMENTS First, I want to express my absolute gratitude to my advisor Dr. Sherine Elsawa. Without her help, incredible scientific knowledge and amazing guidance I would not have been able to achieve what I did. It was her encouragement and believe in me that made me overcome any scientific struggles and strengthened my self-esteem as a human being and as a scientist. -
Smoothened Variants Explain the Majority of Drug Resistance in Basal Cell Carcinoma
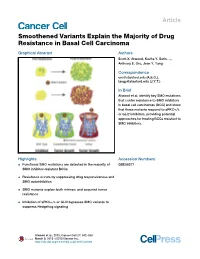
Article Smoothened Variants Explain the Majority of Drug Resistance in Basal Cell Carcinoma Graphical Abstract Authors Scott X. Atwood, Kavita Y. Sarin, ..., Anthony E. Oro, Jean Y. Tang Correspondence [email protected] (A.E.O.), [email protected] (J.Y.T.) In Brief Atwood et al. identify key SMO mutations that confer resistance to SMO inhibitors in basal cell carcinomas (BCC) and show that these mutants respond to aPKC-i/l or GLI2 inhibitors, providing potential approaches for treating BCCs resistant to SMO inhibitors. Highlights Accession Numbers d Functional SMO mutations are detected in the majority of GSE58377 SMO inhibitor-resistant BCCs d Resistance occurs by suppressing drug responsiveness and SMO autoinhibition d SMO mutants explain both intrinsic and acquired tumor resistance d Inhibition of aPKC-i/l or GLI2 bypasses SMO variants to suppress Hedgehog signaling Atwood et al., 2015, Cancer Cell 27, 342–353 March 9, 2015 ª2015 Elsevier Inc. http://dx.doi.org/10.1016/j.ccell.2015.02.002 Cancer Cell Article Smoothened Variants Explain the Majority of Drug Resistance in Basal Cell Carcinoma Scott X. Atwood,1,2 Kavita Y. Sarin,1,2 Ramon J. Whitson,1 Jiang R. Li,1 Geurim Kim,1 Melika Rezaee,1 Mina S. Ally,1 Jinah Kim,1 Catherine Yao,1 Anne Lynn S. Chang,1,3 Anthony E. Oro,1,3,* and Jean Y. Tang1,3,* 1Program in Epithelial Biology and Department of Dermatology, Stanford University School of Medicine, Stanford, CA 94305, USA 2Co-first author 3Co-senior author *Correspondence: [email protected] (A.E.O.), [email protected] (J.Y.T.) http://dx.doi.org/10.1016/j.ccell.2015.02.002 SUMMARY Advanced basal cell carcinomas (BCCs) frequently acquire resistance to Smoothened (SMO) inhibitors through unknown mechanisms. -

GLI3 Knockdown Decreases Stemness, Cell Proliferation and Invasion in Oral Squamous Cell Carcinoma
2458 INTERNATIONAL JOURNAL OF ONCOLOGY 53: 2458-2472, 2018 GLI3 knockdown decreases stemness, cell proliferation and invasion in oral squamous cell carcinoma MARIA FERNANDA SETÚBAL DESTRO RODRIGUES1,2, LUCYENE MIGUITA2, NATHÁLIA PAIVA DE ANDRADE2, DANIELE HEGUEDUSCH2, CAMILA OLIVEIRA RODINI3, RAQUEL AJUB MOYSES4, TATIANA NATASHA TOPORCOV5, RICARDO RIBEIRO GAMA6, ELOIZA ELENA TAJARA7 and FABIO DAUMAS NUNES2 1Postgraduate Program in Biophotonics Applied to Health Sciences, Nove de Julho University (UNINOVE), São Paulo 01504000; 2Department of Oral Pathology, School of Dentistry, University of São Paulo, São Paulo 05508000; 3Department of Biological Sciences, Bauru School of Dentistry, Bauru 17012901; 4Department of Head and Neck Surgery, School of Medicine, 5School of Public Health, University of São Paulo, São Paulo 03178200; 6Department of Head and Neck Surgery, Barretos Cancer Hospital, Barretos 014784400; 7Department of Molecular Biology, School of Medicine of São José do Rio Preto, São José do Rio Preto 15090000, Brazil Received February 28, 2018; Accepted June 29, 2018 DOI: 10.3892/ijo.2018.4572 Abstract. Oral squamous cell carcinoma (OSCC) is an expression of the Involucrin (IVL) and S100A9 genes. Cellular extremely aggressive disease associated with a poor prognosis. proliferation and invasion were inhibited following GLI3 Previous studies have established that cancer stem cells (CSCs) knockdown. In OSCC samples, a high GLI3 expression was actively participate in OSCC development, progression and associated with tumour size but not with prognosis. On the resistance to conventional treatments. Furthermore, CSCs whole, the findings of this study demonstrate for the first time, frequently exhibit a deregulated expression of normal stem at least to the best of our knowledge, that GLI3 contributes cell signalling pathways, thereby acquiring their distinctive to OSCC stemness and malignant behaviour. -

System, Method and Software for Calculation of a Cannabis Drug Efficiency Index for the Reduction of Inflammation
International Journal of Molecular Sciences Article System, Method and Software for Calculation of a Cannabis Drug Efficiency Index for the Reduction of Inflammation Nicolas Borisov 1,† , Yaroslav Ilnytskyy 2,3,†, Boseon Byeon 2,3,4,†, Olga Kovalchuk 2,3 and Igor Kovalchuk 2,3,* 1 Moscow Institute of Physics and Technology, 9 Institutsky lane, Dolgoprudny, Moscow Region 141701, Russia; [email protected] 2 Department of Biological Sciences, University of Lethbridge, Lethbridge, AB T1K 3M4, Canada; [email protected] (Y.I.); [email protected] (B.B.); [email protected] (O.K.) 3 Pathway Rx., 16 Sandstone Rd. S., Lethbridge, AB T1K 7X8, Canada 4 Biomedical and Health Informatics, Computer Science Department, State University of New York, 2 S Clinton St, Syracuse, NY 13202, USA * Correspondence: [email protected] † First three authors contributed equally to this research. Abstract: There are many varieties of Cannabis sativa that differ from each other by composition of cannabinoids, terpenes and other molecules. The medicinal properties of these cultivars are often very different, with some being more efficient than others. This report describes the development of a method and software for the analysis of the efficiency of various cannabis extracts to detect the anti-inflammatory properties of the various cannabis extracts. The method uses high-throughput gene expression profiling data but can potentially use other omics data as well. According to the signaling pathway topology, the gene expression profiles are convoluted into the signaling pathway activities using a signaling pathway impact analysis (SPIA) method. The method was tested by inducing inflammation in human 3D epithelial tissues, including intestine, oral and skin, and then exposing these tissues to various extracts and then performing transcriptome analysis. -

Emerging Role of Tumor Cell Plasticity in Modifying Therapeutic Response
Signal Transduction and Targeted Therapy www.nature.com/sigtrans REVIEW ARTICLE OPEN Emerging role of tumor cell plasticity in modifying therapeutic response Siyuan Qin1, Jingwen Jiang1,YiLu 2,3, Edouard C. Nice4, Canhua Huang1,5, Jian Zhang2,3 and Weifeng He6,7 Resistance to cancer therapy is a major barrier to cancer management. Conventional views have proposed that acquisition of resistance may result from genetic mutations. However, accumulating evidence implicates a key role of non-mutational resistance mechanisms underlying drug tolerance, the latter of which is the focus that will be discussed here. Such non-mutational processes are largely driven by tumor cell plasticity, which renders tumor cells insusceptible to the drug-targeted pathway, thereby facilitating the tumor cell survival and growth. The concept of tumor cell plasticity highlights the significance of re-activation of developmental programs that are closely correlated with epithelial–mesenchymal transition, acquisition properties of cancer stem cells, and trans- differentiation potential during drug exposure. From observations in various cancers, this concept provides an opportunity for investigating the nature of anticancer drug resistance. Over the years, our understanding of the emerging role of phenotype switching in modifying therapeutic response has considerably increased. This expanded knowledge of tumor cell plasticity contributes to developing novel therapeutic strategies or combination therapy regimens using available anticancer drugs, which are likely to -

Subcellular Localization of MC4R with ADCY3 at Neuronal Primary Cilia Underlies a Common Pathway for Genetic Predisposition to Obesity
HHS Public Access Author manuscript Author ManuscriptAuthor Manuscript Author Nat Genet Manuscript Author . Author manuscript; Manuscript Author available in PMC 2018 July 08. Published in final edited form as: Nat Genet. 2018 February ; 50(2): 180–185. doi:10.1038/s41588-017-0020-9. Subcellular localization of MC4R with ADCY3 at neuronal primary cilia underlies a common pathway for genetic predisposition to obesity Jacqueline E. Siljee1,*, Yi Wang1,*, Adelaide A. Bernard1, Baran A. Ersoy1, Sumei Zhang1, Aaron Marley2, Mark Von Zastrow2, Jeremy F. Reiter3, and Christian Vaisse1,** 1Department of Medicine and Diabetes Center, University of California, San Francisco, California, USA 2Department of Psychiatry and Cellular & Molecular Pharmacology, University of California, San Francisco, California, USA 3Department of Biochemistry and Biophysics, Cardiovascular Research Institute, University of California, San Francisco, California, USA MAIN TEXT Most monogenic cases of obesity in humans have been linked to mutations in genes of the leptin-melanocortin pathway. Specifically, mutations in the Melanocortin-4 Receptor (MC4R), account for 3–5% of all severe obesity cases in humans1–3. Recently, adenylate cyclase 3 (ADCY3) mutations have been implicated in obesity4,5. ADCY3 is expressed at the primary cilia of neurons6, organelles that function as hubs for select signaling pathways. Mutations that disrupt the functions of primary cilia cause ciliopathies, rare recessive pleiotropic diseases, of which obesity is a cardinal manifestation7. We demonstrate that MC4R co-localizes with ADCY3 at the primary cilium of a subset of hypothalamic neurons, that obesity-associated MC4R mutations can impair ciliary localization and that inhibition of adenylyl-cyclase signaling at the primary cilia of these neurons increases body weight. -

GLI2 but Not GLI1/GLI3 Plays a Central Role in the Induction of Malignant Phenotype of Gallbladder Cancer
ONCOLOGY REPORTS 45: 997-1010, 2021 GLI2 but not GLI1/GLI3 plays a central role in the induction of malignant phenotype of gallbladder cancer SHU ICHIMIYA1, HIDEYA ONISHI1, SHINJIRO NAGAO1, SATOKO KOGA1, KUKIKO SAKIHAMA2, KAZUNORI NAKAYAMA1, AKIKO FUJIMURA3, YASUHIRO OYAMA4, AKIRA IMAIZUMI1, YOSHINAO ODA2 and MASAFUMI NAKAMURA4 Departments of 1Cancer Therapy and Research, 2Anatomical Pathology, 3Otorhinolaryngology and 4Surgery and Oncology, Graduate School of Medical Sciences, Kyushu University, Fukuoka 812‑8582, Japan Received August 10, 2020; Accepted December 7, 2020 DOI: 10.3892/or.2021.7947 Abstract. We previously reported that Hedgehog (Hh) signal Introduction was enhanced in gallbladder cancer (GBC) and was involved in the induction of malignant phenotype of GBC. In recent Gallbladder cancer (GBC) is the seventh most common gastro- years, therapeutics that target Hh signaling have focused on intestinal carcinoma and accounts for 1.2% of all cancer cases molecules downstream of smoothened (SMO). The three tran- and 1.7% of all cancer-related deaths (1). GBC develops from scription factors in the Hh signal pathway, glioma-associated metaplasia to dysplasia to carcinoma in situ and then to invasive oncogene homolog 1 (GLI1), GLI2, and GLI3, function down- carcinoma over 5‑15 years (2). During this time, GBC exhibits stream of SMO, but their biological role in GBC remains few characteristic symptoms, and numerous cases have already unclear. In the present study, the biological significance of developed into locally advanced or metastasized cancer by the GLI1, GLI2, and GLI3 were analyzed with the aim of devel- time of diagnosis. Gemcitabine (GEM), cisplatin (CDDP), and oping novel treatments for GBC.