The Anatomy of the Aging Face: a Review
Total Page:16
File Type:pdf, Size:1020Kb

Load more
Recommended publications
-

Questions on Human Anatomy
Standard Medical Text-books. ROBERTS’ PRACTICE OF MEDICINE. The Theory and Practice of Medicine. By Frederick T. Roberts, m.d. Third edi- tion. Octavo. Price, cloth, $6.00; leather, $7.00 Recommended at University of Pennsylvania. Long Island College Hospital, Yale and Harvard Colleges, Bishop’s College, Montreal; Uni- versity of Michigan, and over twenty other medical schools. MEIGS & PEPPER ON CHILDREN. A Practical Treatise on Diseases of Children. By J. Forsyth Meigs, m.d., and William Pepper, m.d. 7th edition. 8vo. Price, cloth, $6.00; leather, $7.00 Recommended at thirty-five of the principal medical colleges in the United States, including Bellevue Hospital, New York, University of Pennsylvania, and Long Island College Hospital. BIDDLE’S MATERIA MEDICA. Materia Medica, for the Use of Students and Physicians. By the late Prof. John B Biddle, m.d., Professor of Materia Medica in Jefferson Medical College, Phila- delphia. The Eighth edition. Octavo. Price, cloth, $4.00 Recommended in colleges in all parts of the UnitedStates. BYFORD ON WOMEN. The Diseases and Accidents Incident to Women. By Wm. H. Byford, m.d., Professor of Obstetrics and Diseases of Women and Children in the Chicago Medical College. Third edition, revised. 164 illus. Price, cloth, $5.00; leather, $6.00 “ Being particularly of use where questions of etiology and general treatment are concerned.”—American Journal of Obstetrics. CAZEAUX’S GREAT WORK ON OBSTETRICS. A practical Text-book on Midwifery. The most complete book now before the profession. Sixth edition, illus. Price, cloth, $6.00 ; leather, $7.00 Recommended at nearly fifty medical schools in the United States. -

CME Anatomy of Aging Face
Published online: 2020-01-15 Free full text on www.ijps.org CME Anatomy of aging face Rakesh Khazanchi, Aditya Aggarwal, Manoj Johar1 Department of Plastic and Cosmetic Surgery, Sir Ganga Ram Hospital, New Delhi - 110 060, 1Fortis Hospital, Noida, UP, India Address for correspondence: Dr. Rakesh Khazanchi, Department of Plastic and Cosmetic Surgery, Sir Ganga Ram Hospital, New Delhi - 110 060, India. E-mail: [email protected] ejuvenation of the face is evolving into a common deposition in regions of body called ‘depots’ procedure in India. This may be attempted by f) Fascial and ligament laxity Reither surgical or non surgical means. Surgical g) Shrinkage of glandular tissue (Salivary glands) rejuvenation of face includes a large variety of procedures h) Skeletal resorption to revert the changes of aging. In the past, face lift operation was done to simply lift the sagging skin rather Facial soft tissues are arranged in concentric layers. than shaping the face. However it often ended up in Skin is the outermost layer and then the basic building giving the patient an ‘operated on’ look producing tight blocks-fat, superficial fascia also known as superficial appearing face. The surgeons have now learnt that aging musculoaponeurotic system (SMAS), deep fascia and the process is a complex process that involves soft tissues as periosteum that covers the facial skeleton. Interspersed well as skeleton of face and is not just sagging of skin. in these layers are vessels, nerves, facial muscles and Therefore in order to get a good result after surgical retaining ligaments. Knowledge of these layers allows facial rejuvenation, it is paramount to understand these the surgeon to dissect in a given anatomic plane without anatomical structures and the effect of aging process on damaging important structures. -

Upper Lid Orbicularis Oculi Muscle Strip and Sequential Brow Suspension with Autologous Fascia Lata Is Beneficial for Selected P
Eye (2009) 23, 1549–1553 & 2009 Macmillan Publishers Limited All rights reserved 0950-222X/09 $32.00 www.nature.com/eye Upper lid orbicularis B Patil and AJE Foss CLINICAL STUDY oculi muscle strip and sequential brow suspension with autologous fascia lata is beneficial for selected patients with essential blepharospasm Abstract Introduction Purpose Severe cases of blepharospasm Patients with severe blepharospasm, whose resistant to botulinum toxin represent a symptoms are not controlled by botulinum challenging clinical problem. Over the toxin injections, are a difficult management last 10 years, we have adopted a staged problem for whom a number of surgical options surgical management of these cases have been tried. with an initial upper lid orbicularis Two operations, in particular, have been tried; myectomy (combined with myectomy the orbicularis myectomy (or strip) and brow of procerus and corrugator supercilius as suspension. The choice of the procedure appropriate) and then 4–6 months later classically depends upon the clinical a brow suspension with autologous fascia presentation, with all types being offered the Department of lata. The aim of this study was to orbicularis myectomy except for the apraxic (also Ophthalmology, assess the outcome of this staged surgical called the pre-tarsal) type. The proposed Queen’s Medical Centre, approach. aetiology of the apraxic type is considered to Nottingham University, Materials and methods A questionnaire differ and to represent a failure of eyelid opening Nottingham, UK was sent to all patients who had undergone and is clinically characterized by the eyebrows Correspondence: AJE Foss, the procedure and the clinical records going up and not down with the spasms. -

Head & Neck Muscle Table
Robert Frysztak, PhD. Structure of the Human Body Loyola University Chicago Stritch School of Medicine HEAD‐NECK MUSCLE TABLE PROXIMAL ATTACHMENT DISTAL ATTACHMENT MUSCLE INNERVATION MAIN ACTIONS BLOOD SUPPLY MUSCLE GROUP (ORIGIN) (INSERTION) Anterior floor of orbit lateral to Oculomotor nerve (CN III), inferior Abducts, elevates, and laterally Inferior oblique Lateral sclera deep to lateral rectus Ophthalmic artery Extra‐ocular nasolacrimal canal division rotates eyeball Inferior aspect of eyeball, posterior to Oculomotor nerve (CN III), inferior Depresses, adducts, and laterally Inferior rectus Common tendinous ring Ophthalmic artery Extra‐ocular corneoscleral junction division rotates eyeball Lateral aspect of eyeball, posterior to Lateral rectus Common tendinous ring Abducent nerve (CN VI) Abducts eyeball Ophthalmic artery Extra‐ocular corneoscleral junction Medial aspect of eyeball, posterior to Oculomotor nerve (CN III), inferior Medial rectus Common tendinous ring Adducts eyeball Ophthalmic artery Extra‐ocular corneoscleral junction division Passes through trochlea, attaches to Body of sphenoid (above optic foramen), Abducts, depresses, and medially Superior oblique superior sclera between superior and Trochlear nerve (CN IV) Ophthalmic artery Extra‐ocular medial to origin of superior rectus rotates eyeball lateral recti Superior aspect of eyeball, posterior to Oculomotor nerve (CN III), superior Elevates, adducts, and medially Superior rectus Common tendinous ring Ophthalmic artery Extra‐ocular the corneoscleral junction division -

Blepharoplasty
Blepharoplasty Bobby Tajudeen Brow position • medial brow as having its medial origin at the level of a vertical line drawn to the nasal alar-facial junction • lateral extent of the brow should reach a point on a line drawn from the nasal alar-facial junction through the lateral canthus of the eye • brow should arch superiorly, well above the supraorbital rim, with the highest point lying at the lateral limbus • Less arched in men • midpupillary line and the inferior brow border should be approximately 2.5 cm. The distance from the superior border of the brow to the anterior hairline should be 5 cm Eyelid aesthetics • The highest point of the upper eyelid is at the medial limbus, and the lowest point of the lower eyelid is at the lateral limbus. • Sharp canthal angles should exist, especially at the lateral canthus. • The upper eyelid orbicularis muscle should be smooth and flat, and the upper eyelid crease should be crisp. The upper lid crease should lie between 8 and 12 mm from the lid margin in the Caucasian patient. • The upper lid margin should cover 1 to 2 mm of the superior limbus, and the lower lid margin should lie at the inferior limbus or 1 mm below the inferior limbus • The lower eyelid should closely appose the globe without any drooping of the lid away from the globe (ectropion) or in toward the globe (entropion) Lid laxity and excess • A pinch test helps determine the degree of excess lid skin that is present. The snap test helps determine the degree of lower lid laxity and is useful in preoperative planning Evaluation • -

Atlas of the Facial Nerve and Related Structures
Rhoton Yoshioka Atlas of the Facial Nerve Unique Atlas Opens Window and Related Structures Into Facial Nerve Anatomy… Atlas of the Facial Nerve and Related Structures and Related Nerve Facial of the Atlas “His meticulous methods of anatomical dissection and microsurgical techniques helped transform the primitive specialty of neurosurgery into the magnificent surgical discipline that it is today.”— Nobutaka Yoshioka American Association of Neurological Surgeons. Albert L. Rhoton, Jr. Nobutaka Yoshioka, MD, PhD and Albert L. Rhoton, Jr., MD have created an anatomical atlas of astounding precision. An unparalleled teaching tool, this atlas opens a unique window into the anatomical intricacies of complex facial nerves and related structures. An internationally renowned author, educator, brain anatomist, and neurosurgeon, Dr. Rhoton is regarded by colleagues as one of the fathers of modern microscopic neurosurgery. Dr. Yoshioka, an esteemed craniofacial reconstructive surgeon in Japan, mastered this precise dissection technique while undertaking a fellowship at Dr. Rhoton’s microanatomy lab, writing in the preface that within such precision images lies potential for surgical innovation. Special Features • Exquisite color photographs, prepared from carefully dissected latex injected cadavers, reveal anatomy layer by layer with remarkable detail and clarity • An added highlight, 3-D versions of these extraordinary images, are available online in the Thieme MediaCenter • Major sections include intracranial region and skull, upper facial and midfacial region, and lower facial and posterolateral neck region Organized by region, each layered dissection elucidates specific nerves and structures with pinpoint accuracy, providing the clinician with in-depth anatomical insights. Precise clinical explanations accompany each photograph. In tandem, the images and text provide an excellent foundation for understanding the nerves and structures impacted by neurosurgical-related pathologies as well as other conditions and injuries. -

MBB Lab 5: Anatomy of the Face and Ear
MBB Lab 5: Anatomy of the Face and Ear PowerPoint Handout Review ”The Basics” and ”The Details” for the following cranial nerves in the Cranial Nerve PowerPoint Handout. • Mandibular division trigeminal (CN V3) • Facial nerve (CN VII) Slide Title Slide Number Slide Title Slide Number Blood Supply to Neck, Face, and Scalp: External Carotid Artery Slide3 Parotid Gland Slide 22 Scalp: Layers Slide4 Scalp and Face: Sensory Innervation Slide 23 Scalp: Blood Supply Slide 5 Scalp and Face: Sensory Innervation (Continued) Slide 24 Regions of the Ear Slide 6 Temporomandibular joint Slide 25 External Ear Slide 7 Temporal and Infratemporal Fossae: Introduction Slide 26 Temporal and Infratemporal Fossae: Muscles of Tympanic Membrane Slide 8 Slide 27 Mastication Tympanic Membrane (Continued) Slide 9 Temporal and Infratemporal Fossae: Muscles of Sensory Innervation: Auricle, EAC, and Tympanic Membrane Slide 10 Slide 28 Mastication (Continued) Middle Ear Cavity Slide 11 Summary of Muscles of Mastication Actions Slide 29 Middle Ear Cavity (Continued) Slide 12 Infratemporal Fossae: Mandibular Nerve Slide 30 Mastoid Antrum Slide 13 Inferior Alveolar Nerve Block Slide 31 Eustachian (Pharyngotympanic or Auditory) Tube Slide 14 Palatine Nerve Block Slide 32 Otitis Media Slide 15 Infratemporal Fossae: Maxillary Artery & Pterygoid Plexus Auditory Ossicles Slide 16 Slide 33 Chorda Tympani Nerve and Middle Ear Slide 17 Infratemporal Fossa: Maxillary Artery Slide 34 Superficial Facial Muscles: Muscles of Facial Expression Slide 18 Infratemporal Fossa: Pterygoid Plexus Slide 35 Superficial Facial Muscles: Muscles of Facial Expression Slide 19 Infratemporal Fossa: Otic Ganglion Slide 36 (Continued) Superficial Facial Muscles: Innervation Slide 20 Infratemporal Fossa: Chorda Tympani Nerve Slide 37 Superficial Facial Muscles: Innervation (Continued) Slide 21 Blood Supply to Neck, Face, and Scalp: External Carotid Artery The common carotid artery branches into the internal and external carotid arteries at the level of the superior edge of the thyroid cartilage. -

Anatomy of the Periorbital Region Review Article Anatomia Da Região Periorbital
RevSurgicalV5N3Inglês_RevistaSurgical&CosmeticDermatol 21/01/14 17:54 Página 245 245 Anatomy of the periorbital region Review article Anatomia da região periorbital Authors: Eliandre Costa Palermo1 ABSTRACT A careful study of the anatomy of the orbit is very important for dermatologists, even for those who do not perform major surgical procedures. This is due to the high complexity of the structures involved in the dermatological procedures performed in this region. A 1 Dermatologist Physician, Lato sensu post- detailed knowledge of facial anatomy is what differentiates a qualified professional— graduate diploma in Dermatologic Surgery from the Faculdade de Medician whether in performing minimally invasive procedures (such as botulinum toxin and der- do ABC - Santo André (SP), Brazil mal fillings) or in conducting excisions of skin lesions—thereby avoiding complications and ensuring the best results, both aesthetically and correctively. The present review article focuses on the anatomy of the orbit and palpebral region and on the important structures related to the execution of dermatological procedures. Keywords: eyelids; anatomy; skin. RESU MO Um estudo cuidadoso da anatomia da órbita é muito importante para os dermatologistas, mesmo para os que não realizam grandes procedimentos cirúrgicos, devido à elevada complexidade de estruturas envolvidas nos procedimentos dermatológicos realizados nesta região. O conhecimento detalhado da anatomia facial é o que diferencia o profissional qualificado, seja na realização de procedimentos mini- mamente invasivos, como toxina botulínica e preenchimentos, seja nas exéreses de lesões dermatoló- Correspondence: Dr. Eliandre Costa Palermo gicas, evitando complicações e assegurando os melhores resultados, tanto estéticos quanto corretivos. Av. São Gualter, 615 Trataremos neste artigo da revisão da anatomia da região órbito-palpebral e das estruturas importan- Cep: 05455 000 Alto de Pinheiros—São tes correlacionadas à realização dos procedimentos dermatológicos. -

The Relationship of the Fronto-Temporal Branches of The
Neurosurg Rev DOI 10.1007/s10143-006-0053-5 REVIEW The relationship of the fronto-temporal branches of the facial nerve to the fascias of the temporal region: a literature review applied to practical anatomical dissection Niklaus Krayenbühl & Gustavo Rassier Isolan & Ahmad Hafez & M. Gazi Yaşargil Received: 26 June 2006 /Revised: 13 September 2006 /Accepted: 14 September 2006 # Springer-Verlag 2006 Abstract The understanding of the course of the facial anterior cranial fossa lesions with wider exposures, includ- nerve and its relationship to the different connective tissue ing partial removal or mobilization of the orbit or the layers in the temporal area is paramount to preserving this zygomatic arch made protection of the fronto-temporal nerve during surgery. But the use of different nomencla- branches of the facial nerve a bigger issue [3–5, 12, 29, 47, tures for anatomical structures such as for the different 55]. Moreover, the advances in plastic, reconstructive and fascial layers or fat pads in the temporal region as well as maxillofacial surgery have improved the understanding of the difference in description of the course of the fronto- the relationship between the different fascial layers and the temporal branches of the facial nerve in relationship to the nerves in the temporal region [2, 9, 20, 21, 45, 53, 56]. fascial layers can lead to confusion. Therefore we have A clear understanding of the course of the facial nerve reviewed the literature about this topic and tried to apply and its relationship to the different galeal-fascial layers is the information to practical anatomical dissection. paramount to preserve this nerve during surgery. -

Periorbital Anatomy - an Essential Foundation for Blepharoplasty
PERIORBITAL ANATOMY - AN ESSENTIAL FOUNDATION FOR BLEPHAROPLASTY William M. Ramsdell, M.D. 102 Westlake Dr, Ste 100 Austin, TX 78746 [email protected] 512-327-7779 Private Practice Periorbital Anatomy - An Essential Foundation for Blepharoplasty ABSTRACT Background Mastery of anatomy is fundamental to all surgeons. The anatomy of the eyelids and periorbital regions is unique. Because the eyes and periorbital areas are so essential to cosmetic appearance, blepharoplasty is a popular procedure. Successful blepharoplasty requires thorough knowledge of anatomical concepts. These concepts continue to evolve. Objective To develop thorough knowledge of the anatomy necessary to perform blepharoplasty. To understand anatomical relationships and age-related anatomical changes based upon physical examination. Conclusion The acquistion of knowledge regarding the structure of periorbital tissues is achievable by cosmetic surgeons dedicated to the best in patient care. Such knowledge results in a mutually beneficial surgical experience for surgeons and patients alike. Periorbital Anatomy - An Essential Foundation for Blepharoplasty PERIORBITAL ANATOMY - AN ESSENTIAL FOUNDATION FOR BLEPHAROPLASTY Comprehensive knowledge of anatomy is fundamental to any successful surgery. The anatomy of the periorbital region is unique. Successful management of this region requires not only a thorough knowledge of basic anatomical elements but also how the aging process affects these structures. The study of anatomy is a dynamic process with development of new insights on an ongoing basis. Our understanding has increased significantly over the past 20 years. This article will address fundamental anatomy of the periorbital region. UPPER EYELID ANATOMY The upper eyelid can be divided into two layers or lamellae. The anterior lamella consists of skin, orbicularis oculi muscle and the orbital septum (Figure 1). -

Temporal Branch of the Facial Nerve and Its Relationship to Fascial Layers
ORIGINAL ARTICLE Temporal Branch of the Facial Nerve and Its Relationship to Fascial Layers Seda T. Babakurban, MD; Ozcan Cakmak, MD; Simel Kendir, MD; Alaittin Elhan, PhD, MD; Vito C. Quatela, MD Objectives: To eliminate the inconsistency in the no- 3 (14.3%), and 4 (14.3%) twigs in the specimens. The menclature, to anatomically and definitively describe the temporoparietal fascia had no attachment to the zygo- topographic relationship of the temporal branch of the matic arch and continued caudally as the superficial mus- facial nerve to the fascial layers and the fat pads, and to culoaponeurotic system. Adhesions were between the tem- create an effective algorithm to define the safest ap- poroparietal fascia and the superficial layer of the deep proaches and planes for surgical procedures in this area. temporal fascia around the zygomatic arch. In most speci- mens, the superficial layer of the deep temporal fascia con- Methods: The study was performed using 18 hemifa- tinued as the parotideomasseterica fascia, and a deep layer cial cadaveric specimens. In 12 hemifacial specimens, the abutted the posterosuperior edge of the zygomatic arch. facial halves were coronally sectioned and dissected. In 6 hemifacial specimens, planar dissection was per- Conclusion: An easy and safe surgical approach in this formed layer by layer. area is to elevate the superficial layer deep to the inter- mediate fat pad directly on the deep layer of the deep tem- Results: The temporal branch of the facial nerve that tra- poral fascia descending to the periosteum along the zy- versed inside the deep layers of the temporoparietal fas- gomatic arch. -
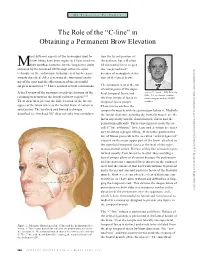
The Role of the “C-Line” in Obtaining a Permanent Brow Elevation
My Practice To Yours The Role of the “C-line” in Obtaining a Permanent Brow Elevation any different aspects of the techniques used for tion the lateral portion of brow lifting have been explored. I have not been the eyebrow but will often fully satisfied, however, by the long-term results lift the medial brow to give M Downloaded from https://academic.oup.com/asj/article/19/2/148/227917 by guest on 23 September 2021 obtained by the forehead lift through either the open the “surprised look” technique or the endoscopic technique as it has been pre- because of inadequate eleva- viously described. After reviewing the functional anato- tion of the lateral brow. my of the area and the effectiveness of the successful surgical maneuvers,1-5 I have reached several conclusions. The temporal crest is the site of convergence of the super- A brief review of the anatomy reveals the location of the ficial temporal fascia and Adrien E. Aiache, MD, Beverly 6-10 Hills, CA, is a board-certified retaining structures in the lateral eyebrow region. the deep temporal fascia or plastic surgeon and an ASAPS These structures prevent the full elevation of the lateral temporal fascia proper. member. aspect of the brow whereas the medial brow elevation is These fasciae enclose the satisfactory. The localized and limited technique temporalis muscle with the periosteum below it. Medially described as “forehead lift” does not take into considera- the fascial elements enclosing the frontalis muscle are the fascia superiorly and the frontal muscle fascia and the periosteum inferiorly. These convergences create the so- called “line of fusion.” Its release and elevation are neces- sary to obtain a proper lifting.