Intermenstrual and Post-Coital Bleeding
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-
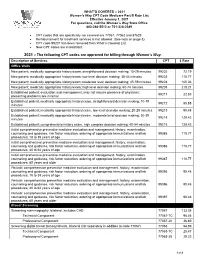

2021 – the Following CPT Codes Are Approved for Billing Through Women’S Way
WHAT’S COVERED – 2021 Women’s Way CPT Code Medicare Part B Rate List Effective January 1, 2021 For questions, call the Women’s Way State Office 800-280-5512 or 701-328-2389 • CPT codes that are specifically not covered are 77061, 77062 and 87623 • Reimbursement for treatment services is not allowed. (See note on page 8). • CPT code 99201 has been removed from What’s Covered List • New CPT codes are in bold font. 2021 – The following CPT codes are approved for billing through Women’s Way. Description of Services CPT $ Rate Office Visits New patient; medically appropriate history/exam; straightforward decision making; 15-29 minutes 99202 72.19 New patient; medically appropriate history/exam; low level decision making; 30-44 minutes 99203 110.77 New patient; medically appropriate history/exam; moderate level decision making; 45-59 minutes 99204 165.36 New patient; medically appropriate history/exam; high level decision making; 60-74 minutes. 99205 218.21 Established patient; evaluation and management, may not require presence of physician; 99211 22.83 presenting problems are minimal Established patient; medically appropriate history/exam, straightforward decision making; 10-19 99212 55.88 minutes Established patient; medically appropriate history/exam, low level decision making; 20-29 minutes 99213 90.48 Established patient; medically appropriate history/exam, moderate level decision making; 30-39 99214 128.42 minutes Established patient; comprehensive history exam, high complex decision making; 40-54 minutes 99215 128.42 Initial comprehensive -

Endometrial Biopsy | Memorial Sloan Kettering Cancer Center
PATIENT & CAREGIVER EDUCATION Endometrial Biopsy This information describes what to expect during and after your endometrial biopsy. About Your Endometrial Biopsy During your endometrial biopsy, your doctor will remove a small piece of tissue from the lining of your uterus. The lining of your uterus is called your endometrium. This tissue is sent to the pathology department to be examined under a microscope. The pathologist will look for abnormal cells or signs of cancer. Before Your Procedure Tell your doctor or nurse if: You’re allergic to iodine. You’re allergic to latex. There’s a chance that you’re pregnant. If you still get your period and are between ages 11 and 50, you will need to take a urine pregnancy test to make sure you’re not pregnant. You won’t need to do anything to get ready for this procedure. During Your Procedure You will have your endometrial biopsy done in an exam room. You will lie on your back as you would for a routine pelvic exam. You will be awake during the procedure. Endometrial Biopsy 1/3 First, your doctor will put a speculum into your vagina. A speculum is a tool that will gently spread apart your vaginal walls, so your doctor can see your cervix (the bottom part of your uterus). Next, your doctor will clean your cervix with a cool, brown solution of povidone- iodine (Betadine® ). Then, they will put a thin, flexible tool, called a pipelle, through your cervix and into your uterus to take a small amount of tissue from your endometrium. -

Vaginitis and Abnormal Vaginal Bleeding
UCSF Family Medicine Board Review 2013 Vaginitis and Abnormal • There are no relevant financial relationships with any commercial Vaginal Bleeding interests to disclose Michael Policar, MD, MPH Professor of Ob, Gyn, and Repro Sciences UCSF School of Medicine [email protected] Vulvovaginal Symptoms: CDC 2010: Trichomoniasis Differential Diagnosis Screening and Testing Category Condition • Screening indications – Infections Vaginal trichomoniasis (VT) HIV positive women: annually – Bacterial vaginosis (BV) Consider if “at risk”: new/multiple sex partners, history of STI, inconsistent condom use, sex work, IDU Vulvovaginal candidiasis (VVC) • Newer assays Skin Conditions Fungal vulvitis (candida, tinea) – Rapid antigen test: sensitivity, specificity vs. wet mount Contact dermatitis (irritant, allergic) – Aptima TMA T. vaginalis Analyte Specific Reagent (ASR) Vulvar dermatoses (LS, LP, LSC) • Other testing situations – Vulvar intraepithelial neoplasia (VIN) Suspect trich but NaCl slide neg culture or newer assays – Psychogenic Physiologic, psychogenic Pap with trich confirm if low risk • Consider retesting 3 months after treatment Trichomoniasis: Laboratory Tests CDC 2010: Vaginal Trichomoniasis Treatment Test Sensitivity Specificity Cost Comment Aptima TMA +4 (98%) +3 (98%) $$$ NAAT (like GC/Ct) • Recommended regimen Culture +3 (83%) +4 (100%) $$$ Not in most labs – Metronidazole 2 grams PO single dose Point of care – Tinidazole 2 grams PO single dose •Affirm VP III +3 +4 $$$ DNA probe • Alternative regimen (preferred for HIV infected -

Cervical Polypectomy
Cervical Polypectomy Author: Consultant Department: Gynaecology/ Colposcopy Document Number: STHK1225 Version: 4 Review date: 01/10/2022 What is a polyp? Your doctor/nurse has advised you to have a polypectomy, which is the removal of a polyp. A polyp is a flesh-like structure (often described as looking like a cherry on a stalk or a skin tag), which can develop in many places in the body, including the cervix and uterus. It may have blood vessels running through it, which can often be the cause of bleeding. If it is thought the polyp is in your uterus, you will need to have a hysteroscopy (a procedure that uses a narrow camera to look inside the cavity of the uterus). This procedure is carried out as a gynaecology outpatient appointment at the Women’s Centre, and is performed in a special clinic in the Diagnostic Suite. You will receive a further appointment for this treatment and be given a different leaflet to explain the hysteroscopy procedure. If for any reason the polyp cannot be removed or fully removed during either of these treatments, the doctor will advise you of other options. Reasons for the procedure As you know you have been referred to the Colposcopy Clinic because you have a polyp on the cervix. Sometimes the cervical polyp is broad based, where it does not have a stalk but sits on the cervix. Often they cause no symptoms and are found as a result of other examinations. Polyps are usually benign (non-cancerous). Less than 1 % (1 in 100) may have pre-cancerous or cancerous changes within them; it is therefore advisable to have them removed. -

A Review on the Outcome of Patient Managed in One Stop Postmenopausal Bleeding Clinic in New Territories East Cluster, NTEC
A Review on the Outcome of Patient managed in One Stop Postmenopausal Bleeding Clinic in New Territories East Cluster, NTEC Principal Investigator: Dr. CHEUNG Chun Wai Co-investigators: Dr. FUNG Wen Ying, Linda Dr. CHAN Wai Yin, Winnie Prof. Lao Tzu Hsi, Terence Department of Obstetrics and Gynaecology, the Chinese University of Hong Kong, Shatin, New Territories, Hong Kong. Version: 1 Date: 24 Jul 2017 1 Introduction: Postmenopausal bleeding (PMB) is a common gynaecological complaint, accounting for up to 5 to 10 % of postmenopausal women being referred to gynaecological outpatient clinic (1, 2). It also comprised of up to 10% of our outpatient gynaecological referral. In general, 60 % of women with postmenopausal bleeding have no organic causes identified, whilst benign causes of PMB includes atrophic vaginitis, endometrial polyp, submucosal fibroid and functional endometrium. However, between 5.7 to 11.5% of women with postmenopausal bleeding have endometrial carcinoma (3, 4, 5), which is the fourth most common cancer among women (6), therefore, it is important to investigate carefully to exclude genital tract cancer. In the past, often women with PMB require multiple clinic visits in order to reach a final diagnosis. This not only increase the medical cost as a whole, but also imposes an enormous stress and burden on patients, concerning about delayed or overlooked diagnosis of genital tract cancer. A One-stop postmenopausal bleeding clinic has been established since February, 2002 by the Department of Obstetrics and Gynaecology, New Territories East cluster (NTEC) aiming at providing immediate assessment of women with postmenopausal bleeding in one single outpatient clinic assessment. -

Uterine Anomalies in Infertility - an Evaluation by Diagnostic Hysterolaparoscopy
Jebmh.com Original Research Article Uterine Anomalies in Infertility - An Evaluation by Diagnostic Hysterolaparoscopy Benudhar Pande1, Soumyashree Padhan2, Pranati Pradhan3 1, 2, 3 Department of Obstetrics and Gynaecology, Veer Surendra Sai Institute of Medical Science and Research, Burla, Odisha, India. ABSTRACT BACKGROUND About 10 - 15 % of reproductive age couples are affected by infertility.1 According Corresponding Author: Dr. Pranati Pradhan, to WHO 60 - 80 million couples currently suffer from infertility.2 Prevalence of Assistant Professor, infertility is rapidly increasing globally.3 Uterine factors of infertility include uterine Department of O & G, anomalies, fibroid uterus, synechiae, Asherman’s syndrome, and failure of VIMSAR, Burla – 768017, implantation without any known primary causes. Congenital uterine malformations Odisha, India. are seen in 10 % cases of infertile women. We wanted to evaluate the anomalies E-mail: [email protected] of uterus in case of primary and secondary infertility by DHL (diagnostic hysterolaperoscopy). DOI: 10.18410/jebmh/2020/580 METHODS How to Cite This Article: Pande B, Padhan S, Pradhan P. Uterine This is a hospital-based, observational study, conducted in the Department of anomalies in infertility-an evaluation by Obstetrics and Gynaecology, VIMSAR, Burla, from November 2017 to October diagnostic hysterolaparoscopy. J Evid 2019. Diagnostic hysterolaparoscopy was done in 100 infertility cases. Based Med Healthc 2020; 7(48), 2831- 2835. DOI: 10.18410/jebmh/2020/580 RESULTS In our study, uterine anomaly i.e. septate uterus was the most common Submission 03-09-2020, hysteroscopic abnormaly found in 23 cases followed by submucous fibroid, polyp, Peer Review 10-09-2020, Acceptance 17-10-2020, synechiae and bicornuate uterus. -

ICD-9-CM and ICD-10-CM Codes for Gynecology and Obstetrics
Diagnostic Services ICD-9-CM and ICD-10-CM Codes for Gynecology and Obstetrics ICD-9 ICD-10 ICD-9 ICD-10 Diagnoses Diagnoses Code Code Code Code Menstral Abnormalities 622.12 Moderate Dysplasia Of Cervix (CIN II) N87.2 625.3 Dysmenorrhea N94.6 Menopause 625.4 Premenstrual Syndrome N94.3 627.1 Postmenopausal Bleeding N95.0 626.0 Amenorrhea N91.2 627.2 Menopausal Symptoms N95.1 626.1 Oligomenorrhea N91.5 627.3 Senile Atrophic Vaginitis N95.2 626.2 Menorrhagia N92.0 627.4 Postsurgical Menopause N95.8 626.4 Irregular Menses N92.6 627.8 Perimenopausal Bleeding N95.8 626.6 Metrorrhagia N92.1 Abnormal Pap Smear Results 626.8 Dysfunctional Uterine Bleeding N93.8 795.00 Abnormal Pap Smear Result, Cervix R87.619 Disorders Of Genital Area 795.01 ASC-US, Cervix R87.610 614.9 Pelvic Inflammatory Disease (PID) N73.9 795.02 ASC-H, Cervix R87.611 616.1 Vaginitis, Unspecified N76.0 795.03 LGSIL, Cervix R87.612 616.2 Bartholin’s Cyst N75.0 795.04 HGSIL, Cervix R87.613 Cervical High-Risk HPV DNA 616.4 Vulvar Abscess N76.4 795.05 R87.810 Test Positive 616.5 Ulcer Of Vulva N76.6 Unsatisfactory Cervical 795.08 R87.615 616.89 Vaginal Ulcer N76.5 Cytology Sample 623.1 Leukoplakia Of Vagina N89.4 795.10 Abnormal Pap Smear Result, Vagina R87.628 Vaginal High-Risk HPV DNA 623.5 Vaginal Discharge N89.8 795.15 R87.811 Test Positive 623.8 Vaginal Bleeding N93.9 Disorders Of Uterus And Ovary 623.8 Vaginal Cyst N89.8 218.9 Uterine Fibroid/Leiomyoma D25.9 Noninflammatory Disorder 623.9 N89.9 Of Vagina 256.39 Ovarian Failure E28.39 624.8 Vulvar Lesion N90.89 256.9 Ovarian -

The Role of Hysteroscopy in Diagnosing Endometrial Cancer
The role of hysteroscopy in diagnosing endometrial cancer Certain hysteroscopic findings correlate with the likelihood of endometrial carcinoma—and the absence of pathology. Here is a breakdown of hysteroscopic morphologic findings and hysteroscopic-directed biopsy techniques. Amy L. Garcia, MD or more than 45 years, gynecologists He demonstrated the advantages of using have used hysteroscopy to diagnose hysteroscopy and directed biopsy in the eval- F endometrial carcinoma and to asso- uation of abnormal uterine bleeding (AUB) to ciate morphologic descriptive terms with obtain a more accurate diagnosis compared visual findings.1 Today, considerably more with dilation and curettage (D&C) alone clinical evidence supports visual pattern rec- (sensitivity, 98% vs 65%, respectively).2 ognition to assess the risk for and presence of Also derived from this work is the clini- IN THIS endometrial carcinoma, improving observer- cal application of the “negative hysteroscopic ARTICLE dependent biopsy of the most suspect lesions view” (NHV). Loffer used the following cri- (VIDEO 1). teria to define the NHV: good visualization Hysteroscopic In this article, I discuss the clinical evo- of the entire uterine cavity, no structural classification lution of hysteroscopic pattern recognition abnormalities of the cavity, and a uniformly of endometrial Ca of endometrial disease and review the visual thin, homogeneous-appearing endometrium findings that correlate with the likelihood of without variations in thickness (TABLE 1). The this page endometrial carcinoma. In addition, I have last criterion can be expected to occur only in provided 9 short videos that show hystero- the early proliferative phase or in postmeno- Negative scopic views of various endometrial patholo- pausal women. -

Having a Cervical Polypectomy
Gynaecology information Having a cervical polypectomy Introduction This leaflet gives you advice and information about having a cervical polypectomy (removal of polyps from the neck of the womb). Please read it before you go home so that you can have your questions answered before you leave. Feel free to discuss any questions or concerns with your nurse or telephone the Colposcopy Clinic on 0118 322 7197 or Sonning Ward on: 0118 322 7181. What is a cervical polypectomy and why do I need one? A cervical polyp is a small piece of tissue, usually on a stalk, that grows on the cervix (neck of the womb). Sometimes the cervical polyp is broad-based, where it does not have a stalk but sits on the cervix. Often they cause no symptoms and are found as a result of other examinations. Polyps are usually benign (non-cancerous). Less than 1% may have pre- cancerous or cancerous changes within them; it is therefore advisable to have them removed. A polypectomy is the removal of polyps. What are the risks of a cervical polypectomy? The procedure is very low risk, but may cause an infection or heavier bleeding. Before being sent for a polypectomy your doctor will have carried out a full pelvic examination, including an examination of your cervix using a speculum and you may have had an ultrasound or scan. What happens during a cervical polypectomy? This is normally done in the outpatient clinic. You will be asked to undress from the waist down and lie down on an examination couch. A speculum (the instrument used to open up the vagina) is passed into the vagina to expose the cervix. -

Menstrual Disorder
Menstrual Disorder N.SmidtN.Smidt--AfekAfek MD MHPE Lake Placid January 2011 The Menstrual Cycle two phases: follicular and luteal Normal Menstruation Regular menstruation 28+/28+/--7days;7days; Flow 4 --7d. 40ml loss Menstrual Disorders Abnormal Beleding –– Menorrhagia ,Metrorrhagia, Polymenorrhagia, Oligomenorrhea, Amenorrhea -- Dysmenorrhea –– Primary Dysmenorrhea, secondary Dysmenorrhea Pre Menstrual Tension –– PMD, PMDD Abnormal Uterine Beleeding Abnormal Bleeding Patterns Menorrhagia --bleedingbleeding more than 80ml or lasting >7days Metrorrhagia --bleedingbleeding between periods Polymenorrhagia -- menses less than 21d apart Oligomenorrhea --mensesmenses greater than 35 dasy apart. (in majority is anovulatory) Amenorrhea --NoNo menses for at least 6months Dysfunctional Uterine Bleeding Clinical term referring to abnormal bleeding that is not caused by identifiable gynecological pathology "Anovulatory Uterine Bleeding“ is usually the cause Diagnosis of exclusion Anovulatory Bleeding Most common at either end of reproductive life Chronic spotting Intermittent heavy bleeding Post Coital Bleeding Cervical ectropion ( most common in pregnancy) Cervicitis Vaginal or cervical malignancy Polyp Common Causes by age Neonatal Premenarchal ––EstrogenEstrogen withdrawal ––ForeignForeign body ––Trauma,Trauma, including sexual abuse Infection ––UrethralUrethral prolapse ––Sarcoma botryoides ––Ovarian tumor ––PrecociousPrecocious puberty Common Causes by age Early postmenarche Anovulation (hypothalamic immaturity) Bleeding -

A Giant, Deceptive Cervical Polyp
Interventions in Gynaecology & Women’s Healthcare DOI: 10.32474/IGWHC.2020.04.000183 ISSN: 2637-4544 Case Report A Giant, Deceptive Cervical Polyp Mounia Bennani*, Hanane Baybay, Jihane Ziani, Sara Elloudi, Zakia Douhi and Fatima Zahra Mernissi Department of dermatology and venerology, Hassan II hospital university, Morocco *Corresponding author: Mounia Bennani Department of dermatology and venerology, Hassan II Hospital University, FES Received: February 29,2020 Published: March 05, 2020 Case Report This is the case of a 48-year-old patient, no Medical or pink-reddish, with a smooth surface (Figure 2), the vaginal touch pharmacological history referred in Our dermatology consultation protruding through the vagina (Figure1). The mass was firm, the tumor was in continuity with the cervix, while the vulva was for management of a lesion evolving for 6 years, increasing in intact. A dermoscopic examination was carried out objectifying size, becoming bleeding on contact, the patient did not complain the presence of a polymorphic vascularization made of vessels in of pain, but rather an unpleasant feeling of heaviness. On local points, irregular linear, and hairpins in place, associated with the examination, a multi-lobed tumor of approximately 10 cm was presence of bright white areas without structures (Figure 3). Figure 1: Image showing a 10cm Multilobed tumor protruding through the vagina. Copyright © All rights are reserved by Mounia Bennani. 384 Int Gyn & Women’s Health Volume 4 - Issue 2 Copyrights @ Mounia Bennani. Figure 2: Image showing a firm, pinkish-reddish, multiloped mass with a smooth surface. Figure 3: Dermoscopic image showing polymorphic vascularity and bright white structures. -
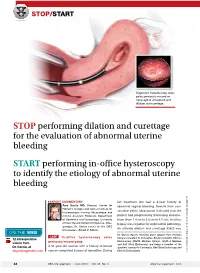
STOP Performing Dilation and Curettage for the Evaluation Of
STOP/START Diagnostic hysteroscopy spies polyp previously missed on transvaginal ultrasound and dilation and curettage. STOP performing dilation and curettage for the evaluation of abnormal uterine bleeding START performing in-office hysteroscopy to identify the etiology of abnormal uterine bleeding }expert commentary her treatment she had a 3-year history of Amy Garcia mD, Director, Center for abnormal vaginal bleeding. Results from con- Women’s Surgery and Garcia Institute for management secutive pelvic ultrasounds indicated that the Hysteroscopic Training, Albuquerque, and Clinical Assistant Professor, Department patient had progressively thickening endome- obg r of Obstetrics and Gynecology, University trium (from 1.4 cm to 2.5 cm to 4.7 cm). In-office O r f of New Mexico School of Medicine, Albu- E biopsy was negative for endometrial pathology. f querque. Dr. Garcia serves on the OBG ie An ultimate dilation and curettage (D&C) was K ManageMent Board of Editors. On the Web aig Dr. Garcia reports receiving grant support from Hologic; CASe In-office hysteroscopy spies being a consultant to Conceptus, Boston Scientific, Ethicon : Cr 12 intraoperative Endosurgery, IOGYN, Minerva, Hologic, Smith & Nephew, previously missed polyp ation videos from and Karl Storz Endoscopy; and being a member of the r A 51-year-old woman with a history of breast Dr. Garcia, at speakers’ bureau for Conceptus, Karl Storz Endoscopy, and ust ll obgmanagement.com cancer completed 5 years of tamoxifen. During Ethicon Endosurgery. I 44 OBG Management | June 2013 | Vol. 25 No. 6 obgmanagement.com performed with negative histologic diagnosis. FIGURE consecutive ultrasounds evaluating The patient is seen in consultation, and abnormal bleeding the ultrasound images are reviewed (FIGURE).