Prioritization of Health Services
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Refusal to Undergo a Cesarean Section: a Woman's Right Or a Criminal Act ? Monica K
Health Matrix: The Journal of Law- Medicine Volume 15 | Issue 2 2005 Refusal to Undergo a Cesarean Section: A Woman's Right or a Criminal Act ? Monica K. Miller Follow this and additional works at: https://scholarlycommons.law.case.edu/healthmatrix Part of the Health Law and Policy Commons Recommended Citation Monica K. Miller, Refusal to Undergo a Cesarean Section: A Woman's Right or a Criminal Act ?, 15 Health Matrix 383 (2005) Available at: https://scholarlycommons.law.case.edu/healthmatrix/vol15/iss2/6 This Article is brought to you for free and open access by the Student Journals at Case Western Reserve University School of Law Scholarly Commons. It has been accepted for inclusion in Health Matrix: The ourJ nal of Law-Medicine by an authorized administrator of Case Western Reserve University School of Law Scholarly Commons. REFUSAL TO UNDERGO A CESAREAN SECTION: A WOMAN'S RIGHT OR A CRIMINAL ACT? Monica K. Millert INTRODUCTION In March, 2004, Melissa Ann Rowland, a twenty-eight-year-old woman from Salt Lake City, gained national media attention when she was arrested on charges of homicide relating to the death of her son. Although there are many child homicide cases that occur regularly across the country that do not attract wide-spread media attention, this case was exceptional because her son died before he was ever born. 1 Rowland had sought medical treatment several times between late December 2003 and January 9, 2004. Each time, she was allegedly advised to get immediate medical treatment, including a cesarean sec- tion (c-section), because her twin fetuses were in danger of death or serious injury. -

Oregon Health Plan Changes Effective January 1, 2017
HEALTH SYSTEMS DIVISION Kate Brown, Governor 500 Summer St NE E44 Salem, OR, 97301 Date: December 8, 2016 Voice: 1-800-336-6016 FAX: 503-945-6873 To: Oregon Health Plan providers TTY: 711 www.oregon.gov/OHA/healthplan From: Don Ross, Physical and Oral Health Programs manager Integrated Health Programs, Health Systems Division Subject: Oregon Health Plan changes effective January 1, 2017 To meet federal health plan requirements, the Oregon Health Authority (OHA) is making the following changes to Oregon Health Plan (OHP) benefits and copayment requirements, subject to approval by the federal Centers for Medicare & Medicaid Services. The changes apply to services covered by OHA and all coordinated care organizations on and after January 1, 2017. OHP Plus benefit changes OHA will update the Prioritized List of Health Services and related administrative rules to add these benefits effective January 1, 2017: A wig benefit of at least $150 per year for patients with hair loss related to chemotherapy or radiation therapy. Separate limits for habilitative and rehabilitative services under Guideline Note 6, which covers physical, occupational and speech therapy for adults with physical health conditions. Guideline Note 106 on Preventive Services has been modified to reflect that OHP coverage will continue to follow federal requirements for coverage of preventive services including: Services with A and B recommendations from the United States Preventive Services Task Force, Immunizations recommended by the Advisory Committee on Immunization Practices, The Health Resources & Services Administration’s Women’s Preventive Services guidelines, and The American Academy of Pediatrics Bright Futures Guidelines. Removal of OHP copayments Copays will be removed from all OHP services, including pharmacy, professional, and outpatient hospital services. -

Clinical Policy: Fetal Surgery in Utero for Prenatally Diagnosed
Clinical Policy: Fetal Surgery in Utero for Prenatally Diagnosed Malformations Reference Number: CP.MP.129 Effective Date: 01/18 Coding Implications Last Review Date: 09/18 Revision Log Description This policy describes the medical necessity requirements for performing fetal surgery. This becomes an option when it is predicted that the fetus will not live long enough to survive delivery or after birth. Therefore, surgical intervention during pregnancy on the fetus is meant to correct problems that would be too advanced to correct after birth. Policy/Criteria I. It is the policy of Pennsylvania Health and Wellness® (PHW) that in-utero fetal surgery (IUFS) is medically necessary for any of the following: A. Sacrococcygeal teratoma (SCT) associated with fetal hydrops related to high output heart failure : SCT resecton: B. Lower urinary tract obstruction without multiple fetal abnormalities or chromosomal abnormalities: urinary decompression via vesico-amniotic shunting C. Ccongenital pulmonary airway malformation (CPAM) and extralobar bronchopulmonary sequestration with hydrops (hydrops fetalis): resection of malformed pulmonary tissue, or placement of a thoraco-amniotic shunt; D. Twin-twin transfusion syndrome (TTTS): treatment approach is dependent on Quintero stage, maternal signs and symptoms, gestational age and the availability of requisite technical expertise and include either: 1. Amnioreduction; or 2. Fetoscopic laser ablation, with or without amnioreduction when member is between 16 and 26 weeks gestation; E. Twin-reversed-arterial-perfusion (TRAP): ablation of anastomotic vessels of the acardiac twin (laser, radiofrequency ablation); F. Myelomeningocele repair when all of the following criteria are met: 1. Singleton pregnancy; 2. Upper boundary of myelomeningocele located between T1 and S1; 3. -

Fetal Surgery in Utero for Prenatally Diagnosed Malformations
Clinical Policy: Fetal Surgery in Utero for Prenatally Diagnosed Malformations Reference Number: PA.CP.MP.129 Effective Date: 01/18 Coding Implications Last Review Date: 12/18 Revision Log Description This policy describes the medical necessity requirements for performing fetal surgery. This becomes an option when it is predicted that the fetus will not live long enough to survive delivery or after birth. Therefore, surgical intervention during pregnancy on the fetus is meant to correct problems that would be too advanced to correct after birth. Policy/Criteria I. It is the policy of Pennsylvania Health and Wellness® (PHW) that in-utero fetal surgery (IUFS) is medically necessary for any of the following: A. Sacrococcygeal teratoma (SCT) associated with fetal hydrops related to high output heart failure : SCT resection; B. Lower urinary tract obstruction without multiple fetal abnormalities or chromosomal abnormalities: urinary decompression via vesico-amniotic shunting C. Congenital pulmonary airway malformation (CPAM) and extralobar bronchopulmonary sequestration with hydrops (hydrops fetalis): resection of malformed pulmonary tissue, or placement of a thoraco-amniotic shunt; D. Twin-twin transfusion syndrome (TTTS): treatment approach is dependent on Quintero stage, maternal signs and symptoms, gestational age and the availability of requisite technical expertise and include either: 1. Amnioreduction; or 2. Fetoscopic laser ablation, with or without amnioreduction when member is between 16 and 26 weeks gestation; E. Twin-reversed-arterial-perfusion (TRAP): ablation of anastomotic vessels of the acardiac twin (laser, radiofrequency ablation); F. Myelomeningocele repair when all of the following criteria are met: 1. Singleton pregnancy; 2. Upper boundary of myelomeningocele located between T1 and S1; 3. -
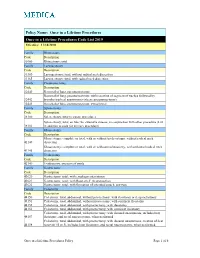
Once in a Lifetime Procedures Code List 2019 Effective: 11/14/2010
Policy Name: Once in a Lifetime Procedures Once in a Lifetime Procedures Code List 2019 Effective: 11/14/2010 Family Rhinectomy Code Description 30160 Rhinectomy; total Family Laryngectomy Code Description 31360 Laryngectomy; total, without radical neck dissection 31365 Laryngectomy; total, with radical neck dissection Family Pneumonectomy Code Description 32440 Removal of lung, pneumonectomy; Removal of lung, pneumonectomy; with resection of segment of trachea followed by 32442 broncho-tracheal anastomosis (sleeve pneumonectomy) 32445 Removal of lung, pneumonectomy; extrapleural Family Splenectomy Code Description 38100 Splenectomy; total (separate procedure) Splenectomy; total, en bloc for extensive disease, in conjunction with other procedure (List 38102 in addition to code for primary procedure) Family Glossectomy Code Description Glossectomy; complete or total, with or without tracheostomy, without radical neck 41140 dissection Glossectomy; complete or total, with or without tracheostomy, with unilateral radical neck 41145 dissection Family Uvulectomy Code Description 42140 Uvulectomy, excision of uvula Family Gastrectomy Code Description 43620 Gastrectomy, total; with esophagoenterostomy 43621 Gastrectomy, total; with Roux-en-Y reconstruction 43622 Gastrectomy, total; with formation of intestinal pouch, any type Family Colectomy Code Description 44150 Colectomy, total, abdominal, without proctectomy; with ileostomy or ileoproctostomy 44151 Colectomy, total, abdominal, without proctectomy; with continent ileostomy 44155 Colectomy, -

Prioritization of Health Services
PRIORITIZATION OF HEALTH SERVICES A Report to the Governor and the 72nd Oregon Legislative Assembly Oregon Health Services Commission Office for Oregon Health Policy and Research Department of Administrative Services 2003 TABLE OF CONTENTS List of Tables . iii Health Services Commission and Staff . .v Acknowledgments . .vii Executive Summary . xi CHAPTER ONE: HISTORY OF THE OREGON HEALTH PLAN Legislative Framework . 3 Implementation of the Medicaid Demonstration . .. 5 Accomplishments . 7 CHAPTER TWO: PRIORITIZATION OF HEALTH SERVICES Charge to the Health Services Commission . .. 21 Prioritization Methodology . 22 Biennial Review . 23 Interim Modifications . 31 Technical Changes . 32 Advancements in Medical Technology . .33 Solid Organ Transplantation . 34 Intrathecal Baclofen Therapy . 36 CHAPTER THREE: CLARIFICATIONS TO THE PRIORITIZED LIST OF HEALTH SERVICES Practice Guidelines . 39 Hysterectomy for Benign Conditions . 40 Adenomyosis . 42 Comfort Care . 44 Spinal Deformities . 45 Cancer of the Esophagus, Liver, Pancreas, and Gallbladder . 45 Intrathecal Baclofen Therapy . 46 Prevention Guidelines . 47 Coding Specifications . 48 Seminoma . 48 Breast Reconstruction Post-Mastectomy for Breast Cancer . 49 Statements of Intent . 49 Medical Codes Not Appearing on the Prioritized List . 50 CHAPTER FOUR: SUBCOMMITTEES, TASK FORCES, AND WORKGROUPS Health Outcomes Subcommittee . 55 Mental Health Care and Chemical Dependency Subcommittee . 56 Workgroup on Public Outreach . 57 Oncology Task Force . 58 CHAPTER FIVE: RECOMMENDATIONS . .61 i TABLE -

Overview of Surgical Techniques in Gender-Affirming Genital Surgery
208 Review Article Overview of surgical techniques in gender-affirming genital surgery Mang L. Chen1, Polina Reyblat2, Melissa M. Poh2, Amanda C. Chi2 1GU Recon, Los Angeles, CA, USA; 2Southern California Permanente Medical Group, Los Angeles, CA, USA Contributions: (I) Conception and design: ML Chen, AC Chi; (II) Administrative support: None; (III) Provision of study materials or patients: All authors; (IV) Collection and assembly of data: None; (V) Data analysis and interpretation: None; (VI) Manuscript writing: All authors; (VII) Final approval of manuscript: All authors. Correspondence to: Amanda C. Chi. 6041 Cadillac Ave, Los Angeles, CA 90034, USA. Email: [email protected]. Abstract: Gender related genitourinary surgeries are vitally important in the management of gender dysphoria. Vaginoplasty, metoidioplasty, phalloplasty and their associated surgeries help patients achieve their main goal of aligning their body and mind. These surgeries warrant careful adherence to reconstructive surgical principles as many patients can require corrective surgeries from complications that arise. Peri- operative assessment, the surgical techniques employed for vaginoplasty, phalloplasty, metoidioplasty, and their associated procedures are described. The general reconstructive principles for managing complications including urethroplasty to correct urethral bulging, vaginl stenosis, clitoroplasty and labiaplasty after primary vaginoplasty, and urethroplasty for strictures and fistulas, neophallus and neoscrotal reconstruction after phalloplasty are outlined as well. Keywords: Transgender; vaginoplasty; phalloplasty; metoidioplasty Submitted May 30, 2019. Accepted for publication Jun 20, 2019. doi: 10.21037/tau.2019.06.19 View this article at: http://dx.doi.org/10.21037/tau.2019.06.19 Introduction the rectum and the lower urinary tract, formation of perineogenital complex for patients who desire a functional The rise in social awareness of gender dysphoria has led vaginal canal, labiaplasty, and clitoroplasty. -

Cervical Cancer
Cervical Cancer Ritu Salani, M.D., M.B.A. Assistant Professor, Dept. of Obstetrics & Gynecology Division of Gynecologic Oncology The Ohio State University Estimated gynecologic cancer cases United States 2010 Jemal, A. et al. CA Cancer J Clin 2010; 60:277-300 1 Estimated gynecologic cancer deaths United States 2010 Jemal, A. et al. CA Cancer J Clin 2010; 60:277-300 Decreasing Trends of Cervical Cancer Incidence in the U.S. • With the advent of the Pap smear, the incidence of cervical cancer has dramatically declined. • The curve has been stable for the past decade because we are not reaching the unscreened population. Reprinted by permission of the American Cancer Society, Inc. 2 Cancer incidence worldwide GLOBOCAN 2008 Cervical Cancer New cases Deaths United States 12,200 4,210 Developing nations 530,000 275,000 • 85% of cases occur in developing nations ¹Jemal, CA Cancer J Clin 2010 GLOBOCAN 2008 3 Cervical Cancer • Histology – Squamous cell carcinoma (80%) – Adenocarcinoma (15%) – Adenosquamous carcinoma (3 to 5%) – Neuroendocrine or small cell carcinoma (rare) Human Papillomavirus (HPV) • Etiologic agent of cervical cancer • HPV DNA sequences detected is more than 99% of invasive cervical carcinomas • High risk types: 16, 18, 45, and 56 • Intermediate types: 31, 33, 35, 39, 51, 52, 55, 58, 59, 66, 68 HPV 16 accounts for ~80% of cases HPV 18 accounts for 25% of cases Walboomers JM, Jacobs MV, Manos MM, et al. J Pathol 1999;189(1):12-9. 4 Viral persistence and Precancerous progression Normal lesion cervix Regression/ clearance Invasive cancer Risk factors • Early age of sexual activity • Cigggarette smoking • Infection by other microbial agents • Immunosuppression – Transplant medications – HIV infection • Oral contraceptive use • Dietary factors – Deficiencies in vitamin A and beta carotene 5 Multi-Stage Cervical Carcinogenesis Rosenthal AN, Ryan A, Al-Jehani RM, et al. -

Oregon Health Plan
Background Brief on… Oregon Health Plan Prepared by: Rick Berkobien May 2004 Background Volume 2, Issue 1 From 1989 to 1999, the Oregon Legislature passed a series of laws collectively known as the Oregon Health Plan (OHP). OHP expanded access to health care using a combi- Inside this Brief nation of public and private insurance plans and a prioritized list of health care services. Currently, more than 450,000 • Background Oregonians have access to health care under the OHP. The Department of Human Services (DHS), Office of Medi- • OHP Plus cal Assistance Programs (OMAP) administers the public insurance components of OHP, including Medicaid and the State Children’s Health Insurance Program (SCHIP). SCHIP • OHP Standard is a separate federal/state funded program to provide health care services to certain low-income children. • Family Health Insurance The Family Health Insurance Assistance Program (FHIAP), Assistance Program created by the 1997 Legislature, provides subsidies for the purchase of private health insurance by low-income workers. As part of OHP, FHIAP is currently funded solely with state • Proof for OHP Eligibility dollars—about $20 million in tobacco settlement funds—and the number of people served is capped at around 4,000. FHIAP currently provides services to people with incomes • The Insurance Pool up to 170 percent of the federal poverty level (FPL). Subsi- Governing Board dies range from 70 percent up to 95 percent of the premium costs depending on family size and income. • Staff and Agency Contacts House Bill 2519 (2001) modified the program to provide coverage to more uninsured Oregonians, have more flexibil- ity in the program’s benefits, secure more federal dollars, and help control the program’s rising medical costs. -

Update on Prenatal Diagnosis and Fetal Surgery for Myelomeningocele
Review Arch Argent Pediatr 2021;119(3):e215-e228 / e215 Update on prenatal diagnosis and fetal surgery for myelomeningocele César Meller, M.D.a, Delfina Covini, M.D.b, Horacio Aiello, M.D.a, Gustavo Izbizky, M.D.a, Santiago Portillo Medina, M.D.c and Lucas Otaño, M.D.a ABSTRACT This powered research in two A seminal study titled Management of critical areas. On the one side, prenatal Myelomeningocele Study, from 2011, demonstrated that prenatal myelomeningocele defect repaired myelomeningocele diagnosis within before 26 weeks of gestation improved the therapeutic window became a neurological outcomes; based on this study, fetal mandatory goal; therefore, research surgery was introduced as a standard of care efforts on screening strategies were alternative. Thus, prenatal myelomeningocele diagnosis within the therapeutic window became intensified, especially in the first a mandatory goal; therefore, research efforts on trimester. On the other side, different screening strategies were intensified, especially fetal surgery techniques were assessed in the first trimester. In addition, different fetal to improve neurological outcomes and surgery techniques were developed to improve neurological outcomes and reduce maternal reduce maternal risks. The objective risks. The objective of this review is to provide an of this review is to provide an update update on the advances in prenatal screening and on the advances in prenatal screening diagnosis during the first and second trimesters, and diagnosis and in fetal surgery for and in open and fetoscopic fetal surgery for myelomeningocele. myelomeningocele. Key words: myelomeningocele, fetal therapies, spina bifida, fetoscopy, antenatal care. EPIDEMIOLOGY The prevalence of spina bifida http://dx.doi.org/10.5546/aap.2021.eng.e215 varies markedly worldwide based on ethnic and geographic To cite: Meller C, Covini D, Aiello H, Izbizky G, characteristics.8,9 In Argentina, since et al. -

Application for Oregon Health Plan and Healthy Kids
Application for Oregon Health Plan and Healthy Kids Read this before you start. You can get this application in other formats. • This is for the Oregon Health Plan and Healthy Kids. You • This document can be provided upon request in alternative can apply for one or both programs with this application. formats for individuals with disabilities. Other formats may • Please answer all questions so we have the information include (but are not limited to) large print, Braille, audio we need to see if you qualify. recordings, Web-based communications and other electronic formats. Email [email protected], or call • Read the Green Booklet by clicking here. 1-800-699-9075 (voice) or TTY 711 to arrange for the It includes more information about the questions asked. alternative format that will work best for you. When you see this arrow, it means you may have to • You can get this application in another language or you send documents that show us the information you gave can get an interpreter. Call 1-800-699-9075 or TTY 711. is correct. Please mail copies of these documents along with your application to: For more information about: OHP Processing Center, • Healthy Kids or to find local application assistance, PO Box 14520, Salem, OR 97309-5044 click here: www.oregonhealthykids.gov or fax to 503-373-7493 • Oregon Health Plan, click here: www.oregon.gov/OHA/healthplan 1 About you. Please tell us about yourself, even if you are only applying for benefits for your children. You may need to send proof of immigration status or tribal affiliation if you are applying for yourself (see the checklist on page 16). -

MSC 5504 PEBB Open Enrollment and Correction Form
Open Enrollment Form Office use only October 1 – October 31, 2021 Approved by: Approved date: Open Enrollment Corrections (see dates below) Effective date: See the Summary Plan Description for more information on benefits at www.pebbinfo.com Section 1: Enrollment Type F Open Enrollment – October 1, to October 31, 2021 F Open Enrollment Correction – May be submitted through February 28, 2022. **HEM is not correctable** F Newly hired in October and November 2021 Section 2: Employee information PEBB benefit number (P########), OR#, University ID or Lottery ID Gender Date of birth (mm/dd/yyyy) F M F F F Other Last name First name M.I. Work phone number Home phone number (optional) Cell phone number (Optional) F Check if new address Address Apartment or space# City State ZIP County Personal email (Optional) Work email Are you Medicare eligible? F Yes F No Are you serving or did you ever serve in the military? F Yes F No If “Yes,” do you authorize PEBB to send your name and address to the Oregon Department of Veterans’ Affairs (ODVA) for the purpose of receiving benefit information? F Yes F No Ethnicity (Select one): F Hispanic F Non-Hispanic/Non-Latino F Refused F Unknown Race (Select at least one. If selecting more than one, circle one as primary): F Asian F Black/African American F American Indian/Alaska Native F Native Hawaiian/Other Pacific Islander F White F Other F Refused F Unknown Page 1 of 8 MSC 5504 (09/2021) Section 3: Dependent information 1. List all eligible family members you want to provide coverage for.