Understanding Neurogenic Bladder Supported by an Unrestricted Educational Grant from Hollister Incorporated
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Urinary Incontinence: Impact on Long Term Care
Urinary Incontinence: Impact on Long Term Care Muhammad S. Choudhury, MD, FACS Professor and Chairman Department of Urology New York Medical College Director of Urology Westchester Medical Center 1 Urinary Incontinence: Overview • Definition • Scope • Anatomy and Physiology of Micturition • Types • Diagnosis • Management • Impact on Long Term Care 2 Urinary Incontinence: Definition • Involuntary leakage of urine which is personally and socially unacceptable to an individual. • It is a multifactorial syndrome caused by a combination of: • Genito urinary pathology. • Age related changes. • Comorbid conditions that impair normal micturition. • Loss of functional ability to toilet oneself. 3 Urinary Incontinence: Scope • Prevalence of Urinary incontinence increase with age. • Affects more women than men (2:1) up to age 80. • After age 80, both women and men are equally affected. • Urinary Incontinence affect 15% to 30% of the general population > 65 years. • > 50% of 1.5 million Long Term Care residents may be incontinent. • The cost to care for this group is >5 billion per year. • The total cost of care for Urinary Incontinence in the U.S. is estimated to be over $36 billion. Ehtman et al., 2012. 4 Urinary Incontinence: Impact on Quality of Life • Loss of self esteem. • Avoidance of social activity and interaction. • Decreased ability to maintain independent life style. • Increased dependence on care givers. • One of the most common reason for long term care placement. Grindley et al. Age Aging. 1998; 22: 82-89/Harris T. Aging in the eighties. NCHS # 121 1985. Noelker L. Gerontologist 1987; 27: 194-200. 5 Health related consequences of Urinary Incontinence • Increased propensity for fall/fracture. -

Urinary Incontinence
GLICKMAN UROLOGICAL & KIDNEY INSTITUTE Urinary Incontinence What is it? can lead to incontinence, as can prostate cancer surgery or Urinary incontinence is the inability to control when you radiation treatments. Sometimes the cause of incontinence pass urine. It’s a common medical problem. As many as isn’t clear. 20 million Americans suffer from loss of bladder control. The condition is more common as men get older, but it’s Where can I get help? not an inevitable part of aging. Often, embarrassment stops Talking to your doctor is the first step. You shouldn’t feel men from seeking help, even when the problem is severe ashamed; physicians regularly help patients with this prob- and affects their ability to leave the house, spend time with lem and are comfortable talking about it. Many patients family and friends or take part in everyday activities. It’s can be evaluated and treated after a simple office visit. possible to cure or significantly improve urinary inconti- Some patients may require additional diagnostic tests, nence, once its underlying cause has been identified. But which can be done in an outpatient setting and aren’t pain- it’s important to remember that incontinence is a symp- ful. Once these tests have determined the cause of your tom, not a disease. Its cause can be complex and involve incontinence, your doctor can recommend specific treat- many factors. Your doctor should do an in-depth evaluation ments, many of which do not require surgery. No matter before starting treatment. how serious the problem seems, urinary incontinence is a condition that can be significantly relieved and, in many What might be causing my incontinence? cases, cured. -

CMS Manual System Human Services (DHHS) Pub
Department of Health & CMS Manual System Human Services (DHHS) Pub. 100-07 State Operations Centers for Medicare & Provider Certification Medicaid Services (CMS) Transmittal 8 Date: JUNE 28, 2005 NOTE: Transmittal 7, of the State Operations Manual, Pub. 100-07 dated June 27, 2005, has been rescinded and replaced with Transmittal 8, dated June 28, 2005. The word “wound” was misspelled in the Interpretive Guidance section. All other material in this instruction remains the same. SUBJECT: Revision of Appendix PP – Section 483.25(d) – Urinary Incontinence, Tags F315 and F316 I. SUMMARY OF CHANGES: Current Guidance to Surveyors is entirely replaced by the attached revision. The two tags are being combined as one, which will become F315. Tag F316 will be deleted. The regulatory text for both tags will be combined, followed by this revised guidance. NEW/REVISED MATERIAL - EFFECTIVE DATE*: June 28, 2005 IMPLEMENTATION DATE: June 28, 2005 Disclaimer for manual changes only: The revision date and transmittal number apply to the red italicized material only. Any other material was previously published and remains unchanged. However, if this revision contains a table of contents, you will receive the new/revised information only, and not the entire table of contents. II. CHANGES IN MANUAL INSTRUCTIONS: (N/A if manual not updated.) (R = REVISED, N = NEW, D = DELETED) – (Only One Per Row.) R/N/D CHAPTER/SECTION/SUBSECTION/TITLE R Appendix PP/Tag F315/Guidance to Surveyors – Urinary Incontinence D Appendix PP/Tag F316/Urinary Incontinence III. FUNDING: Medicare contractors shall implement these instructions within their current operating budgets. IV. ATTACHMENTS: Business Requirements x Manual Instruction Confidential Requirements One-Time Notification Recurring Update Notification *Unless otherwise specified, the effective date is the date of service. -

Urinary Tract Infection (Uti) Fact Sheet
URINARY TRACT INFECTION (UTI) FACT SHEET Overview A urinary tract infection (UTI) is an infection that involves any part of the urinary tract, including the kidneys, bladder and urethra. It is usually caused by exposure of the urinary tract to a fecal organism such as Escherichia coli (E. coli) but also may be caused by other organisms. An indwelling urinary catheter is a drainage tube that is inserted into the urinary bladder through the urethra, is left in place and is connected to a closed urine collection system. Urinary tract infections in patients with an indwelling urinary catheter are called catheter-associated UTIs, or CAUTIs. Signs and Symptoms Common symptoms of UTI include: • fever; • pain or burning in the lower abdomen; • burning during urination; • an increase in the frequency of urination; and • cloudy appearing urine. Causes and Transmission A UTI occurs when germs (usually bacteria) enter the urinary tract through the meatus (the opening of the urinary tract). These germs then cause infection. The urinary tract is normally sterile, meaning it contains no germs. A CAUTI occurs when germs (usually bacteria) enter the urinary tract through the urinary catheter and cause infection. This can occur when health care worker hands are not properly cleaned before the insertion of a catheter or during the process of cleaning or emptying of the urine collection system. Risk Factors Sexually active women, people with blockages in the urinary tract, such as prostate enlargement, and women using certain types of birth control, such as diaphragms, or those who are undergoing menopause are at higher risk of UTI. -

STRESS INCONTINENCE by JOHN BEATTIE, M.D., F.R.C.S., F.R.C.O.G
Postgrad Med J: first published as 10.1136/pgmj.32.373.527 on 1 November 1956. Downloaded from s27 STRESS INCONTINENCE By JOHN BEATTIE, M.D., F.R.C.S., F.R.C.O.G. Gynaecological Surgeon, St. Bartholomew's Hospital So far the mist has cleared very little from around obtain such a history, otherwise a patient may be this difficult subject despite the original work operated upon for urethrocele when the symptoms which has been carried out during the last io are due to something else or if true stress incon- years. Operations for the cure of stress incon- tinence develops after child bearing in such a tinence have been described from time to time patient the results of operation may be dis- during the last 50 years, but until recently most appointing. gynaecologists considered that a modified anterior Other abnormalities of bladder function which colporrhaphy was all that was necessary to achieve must be differentiated from a case of true stress a lasting cure. incontinence are as follows: One of the most important things in dealing with this subject is first to differentiate true stress The Neurogenic Bladder incontinence from inability to control the passage The bladder is often a most sensitive indicator Protected by copyright. of urine from the bladder when the urge to mic- of neurological disease and, of course, there may turate becomes great. There is also the leak which be, and often is, vaginal prolapse present at the occurs in retention with overflow to consider and onset of such a condition. The most often quoted other conditions which cause weakness of the instance of the neurogenic bladder is disseminated bladder sphincterwithout a true stress incontinence sclerosis, and, indeed, it is the commonest neuro- being present. -

233 the Use of Absorbent Pads Increases the Risk For
233 Omli R1, Skotnes L H1, Romild U1, Kuhry E1 1. Namsos Hospital THE USE OF ABSORBENT PADS INCREASES THE RISK FOR LOWER URINARY TRACT INFECTIONS IN NURSING HOMES RESIDENTS. Hypothesis / aims of study Urinary incontinence is a common medical problem in the nursing home population. The aim of this study was to determine whether use of absorbent pads is a risk factor for the development of lower urinary tract infections in nursing home residents. Introduction Lower urinary tract infections (UTIs) are a common medical problem in the elderly. Different kinds of absorbent products, such as diapers, pad and pant combinations, are used in incontinence care. In some cases, indwelling catheters, external condom catheters or in-and-out catheterisation are options for managing bladder dysfunction. About 23% of the residents in nursing homes don’t need toilet assistance. That means that the majority of residents is dependent on help from nursing staff for toileting and help to change soiled absorbent pads. Transmission of bacteria during incontinence care is associated with UTIs in elderly. In the vulnerable nursing home population, UTIs are a frequent problem and can lead to increased morbidity and even mortality. The prevalence of UTIs in nursing home residents is approximately 30%. Improving hand hygiene among staffing in nursing homes is one of the most important and effective methods to reduce hand born transmission of pathological microbes. Studies in long-term-care facilities document a lack of hand hygiene in connection to staff-resident interactions. This study studies the association between the use of absorbent pads and symptomatic UTIs in the nursing home population. -

35-40 Institute of Normal Anatomy
35 Lymphology 28 (1995) 35-40 Institute of Normal Anatomy (PP,AT), Institute of Histology and General Embryology (CM), and Department of Human Pathology (RS), University of Pavia, Italy ABSTRACT light and electron microscopy (2,3). To clarify vesical lymph drainage, we now examined the After endoscopic transurethral biopsies of fine structure of small lymphatic vessels (SL V) normal human urinary bladder, an extensive and their distribution in the normal human network of small initial lymphatic vessels was urinary bladder. Particular attention was depicted by means of light and electron directed to the structure and composition of microscopy. Using light microscopy, lymphatic the connective matrix that surrounds the vessels were seen in the mucosa and lymphatic vessels in the different regions of submucosa and formed a complex network in the bladder wall. the detrusor muscular coat. These lymphatics were characterized by an irregular and MATERIALS AND METHODS attenuated wall and increased in number and size from the superficial to the deeper region of Ten male subjects (40 to 60 years of age) the bladder. Ultrastructurally, the lymphatic who had symptoms of bladder outlet wall was characterized by endothelial cells obstruction were utilized for this investigation. joined together end-to-end or by complicated Two endoscopic transurethral biopsies from interdigitations. Often intercellular channels the lateral wall of the normal urinary bladder and gaps between two contiguous endothelial were performed under a constant bladder cells were present. A broad network of elastic distention after introduction of physiological and collagen fibers joined the lymphatic saline at 50 cm H20 constant pressure. The endothelial wall to the neighboring connective biopsy trocar was regulated to obtain vesical tissue. -

Diagnosis and Management of Urinary Incontinence in Childhood
Committee 9 Diagnosis and Management of Urinary Incontinence in Childhood Chairman S. TEKGUL (Turkey) Members R. JM NIJMAN (The Netherlands), P. H OEBEKE (Belgium), D. CANNING (USA), W.BOWER (Hong-Kong), A. VON GONTARD (Germany) 701 CONTENTS E. NEUROGENIC DETRUSOR A. INTRODUCTION SPHINCTER DYSFUNCTION B. EVALUATION IN CHILDREN F. SURGICAL MANAGEMENT WHO WET C. NOCTURNAL ENURESIS G. PSYCHOLOGICAL ASPECTS OF URINARY INCONTINENCE AND ENURESIS IN CHILDREN D. DAY AND NIGHTTIME INCONTINENCE 702 Diagnosis and Management of Urinary Incontinence in Childhood S. TEKGUL, R. JM NIJMAN, P. HOEBEKE, D. CANNING, W.BOWER, A. VON GONTARD In newborns the bladder has been traditionally described as “uninhibited”, and it has been assumed A. INTRODUCTION that micturition occurs automatically by a simple spinal cord reflex, with little or no mediation by the higher neural centres. However, studies have indicated that In this chapter the diagnostic and treatment modalities even in full-term foetuses and newborns, micturition of urinary incontinence in childhood will be discussed. is modulated by higher centres and the previous notion In order to understand the pathophysiology of the that voiding is spontaneous and mediated by a simple most frequently encountered problems in children the spinal reflex is an oversimplification [3]. Foetal normal development of bladder and sphincter control micturition seems to be a behavioural state-dependent will be discussed. event: intrauterine micturition is not randomly distributed between sleep and arousal, but occurs The underlying pathophysiology will be outlined and almost exclusively while the foetus is awake [3]. the specific investigations for children will be discussed. For general information on epidemiology and During the last trimester the intra-uterine urine urodynamic investigations the respective chapters production is much higher than in the postnatal period are to be consulted. -

STRESS INCONTINENCE of URINE in the FEMALE by TERENCE MILLIN, M.CH., F.R.C.S., and CHARLES D
Postgrad Med J: first published as 10.1136/pgmj.24.267.3 on 1 January 1948. Downloaded from 3 STRESS INCONTINENCE OF URINE IN THE FEMALE By TERENCE MILLIN, M.CH., F.R.C.S., and CHARLES D. READ, M.B. F.R.C.S.(E), F.R.A.C.S., F.R.C.O.G. London PART I The distressing condition for which Sir Eardley genital prolapse, but the condition is encountered Holland coined the term stress incontinence is not infrequently in nulliparae about the meno- variously known as orthostatic, exertional or pausal age. It has long been recognized that little diurnal incontinence. relationship exists between the degree of genital The diagnosis presents little difficulty as a rule. prolapse and the severity of the urinary incon- The history varies according to the severity of the tinence. In fact, many women with an extreme condition. In its mildest form the patient is degree of descensus.have no stress incontinence, conscious of an escape of a small quantity of urine and conversely, patients exhibiting marked urinary in any movement which entails a rise of intra- loss may reveal little or no evidence of urethrocoele abdominal pressure when in the upright position or cystocoele. On several occasions we have -sneezing, coughing, walking up or down stairs. encountered stress incontinence which has by copyright. In its most severe form it may be evidenced by developed after the successful repair of a prolapse almost complete incontinence while in the up- in patients who previously had been completely right position. Almost invariably there is adequate continent of urine. -

Clinical and Functional Anatomy of the Urethral Sphincter
Review Article International Neurourology Journal Int Neurourol J 2012;16:102-106 http://dx.doi.org/10.5213/inj.2012.16.3.102 pISSN 2093-4777 · eISSN 2093-6931 INJ Clinical and Functional Anatomy of the Urethral Sphincter Junyang Jung, Hyo Kwang Ahn, Youngbuhm Huh Department of Anatomy, Kyung Hee University School of Medicine, Seoul, Korea Continence and micturition involve urethral closure. Especially, insufficient strength of the pelvic floor muscles including the urethral sphincter muscles causes urinary incontinence (UI). Thus, it is most important to understand the main mechanism causing UI and the relationship of UI with the urethral sphincter. Functionally and anatomically, the urethral sphincter is made up of the internal and the external sphincter. We highlight the basic and clinical anatomy of the internal and the external sphinc- ter and their clinical meaning. Understanding these relationships may provide a novel view in identifying the main mechanism causing UI and surgical techniques for UI. Keywords: Urethral sphincters; Pudendal nerve; Autonomic nervous system; Urinary incontinence; Urination INTRODUCTION tomical damage to the ligaments, facial support, and pelvic floor musculature, including the levator ani [8]. The pudendal nerve The urethral sphincter is crucial for the maintenance of urinary innervating the EUS is susceptible to injury during vaginal birth continence [1,2]. The urethral sphincter refers to one of the fol- because it travels between the sacrospinous and sacrotuberous lowing muscles [3]: 1) the internal urethral sphincter (IUS), ligaments [9]. In this article, we discuss the basic and clinical which consists of smooth muscle and is continuous with the anatomy of the urethral sphincter and the relationship between detrusor muscle and under involuntary control, and 2) the ex- the urethral sphincter and UI. -
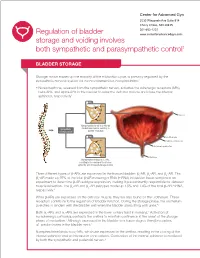
Regulation of Bladder Storage and Voiding Involves Both Sympathetic
Center for Advanced Gyn 5530 Wisconsin Ave Suite 914 Chevy Chase, MD 20815 301-652-1231 Regulation of bladder www.centerforadvancedgyn.com storage and voiding involves both sympathetic and parasympathetic control1 BLADDER STORAGE Storage, which makes up the majority of the micturition cycle, is primarily regulated by the sympathetic nervous system via the neurotransmitter, norepinephrine.2 • Norepinephrine, released from the sympathetic nerves, activates the adrenergic receptors (ARs), beta-ARs, and alpha-ARs in the bladder to relax the detrusor muscle and close the internal sphincter, respectively2 β-ARs Norepinephrine Ureter β-AR Norepinephrine binds to β-ARs on Sympathetic the detrusor muscle, resulting in nervous system bladder relaxation α-ARs Urothelium -AR α1 Detrusor muscle Internal sphincter Norepinephrine Urethra Norepinephrine binds to α1-ARs, resulting in the closing of the internal sphincter and increased storage of urine Three different types of b-ARs are expressed in the human bladder: b1-AR, b2-AR, and b3-AR. The b3-AR made up 97% of the total b-AR messenger RNA (mRNA) in bladder tissue samples in an experiment to determine b-AR subtype expression, making it predominantly responsible for detrusor muscle relaxation. The b1-AR and b2-AR subtypes made up 1.5% and 1.4% of the total b-AR mRNA, respectively.3 While b-ARs are expressed on the detrusor muscle, they are also found on the urothelium. These receptors contribute to the regulation of bladder function. During the storage phase, the urothelium stretches in tandem with the bladder wall when the bladder starts filling with urine.4,5 6 Both a1-ARs and a2-ARs are expressed in the lower urinary tract in humans. -

Urinary Retention in Women Workshop Chair: David Castro-Diaz, Spain 07 October 2015 08:30 - 11:30
W16: Urinary Retention in Women Workshop Chair: David Castro-Diaz, Spain 07 October 2015 08:30 - 11:30 Start End Topic Speakers 08:30 08:45 Urinary retention in women: concepts and pathophysiology David Castro-Diaz 08:45 08:50 Discussion All 08:50 09:05 Evaluation Tufan Tarcan 09:05 09:10 Discussion All 09:10 09:30 Conservative management Cristina Naranjo-Ortiz 09:30 09:35 Discussion All 09:35 09:55 Medical and surgical management Christopher Chapple 09:55 10:00 Discussion All 10:00 10:30 Break None 10:30 11:20 Typical clinical cases discussion All 11:20 11:30 Take home messages David Castro-Diaz Aims of course/workshop Urinary retention in women is rare and diverse. Diagnostic criteria are not agreed and epidemiology is not well known. Forms of urinary retention in women include: complete retention, incomplete or insufficient emptying and elevated post-void residual. It may be acute or chronic, symptomatic or asymptomatic. Etiology is multifactorial including anatomic or functional bladder outlet obstruction and bladder dysfunction related to neurological diseases, diabetes mellitus, aging, pharmacotherapy, pain and infective/inflammatory disease and idiopathic or unknown aetiology. This workshop will analyse and discuss physiopathology, evaluation and management of urinary retention in women from an integral, practical and evidence based approach. Learning Objectives 1. Identify urinary retention in women, its etiology and risk factors. 2. Carry out proper diagnosis of urinary retention in women as well as its relationship with risk and influent factors. 3. Properly manage female acute and chronic acute and chronic urinary retention with the different approaches including conservative, medical and surgical therapies.