Nail Disorders: Anatomy, Pathology, Therapy
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Development and Maintenance of Epidermal Stem Cells in Skin Adnexa
International Journal of Molecular Sciences Review Development and Maintenance of Epidermal Stem Cells in Skin Adnexa Jaroslav Mokry * and Rishikaysh Pisal Medical Faculty, Charles University, 500 03 Hradec Kralove, Czech Republic; [email protected] * Correspondence: [email protected] Received: 30 October 2020; Accepted: 18 December 2020; Published: 20 December 2020 Abstract: The skin surface is modified by numerous appendages. These structures arise from epithelial stem cells (SCs) through the induction of epidermal placodes as a result of local signalling interplay with mesenchymal cells based on the Wnt–(Dkk4)–Eda–Shh cascade. Slight modifications of the cascade, with the participation of antagonistic signalling, decide whether multipotent epidermal SCs develop in interfollicular epidermis, scales, hair/feather follicles, nails or skin glands. This review describes the roles of epidermal SCs in the development of skin adnexa and interfollicular epidermis, as well as their maintenance. Each skin structure arises from distinct pools of epidermal SCs that are harboured in specific but different niches that control SC behaviour. Such relationships explain differences in marker and gene expression patterns between particular SC subsets. The activity of well-compartmentalized epidermal SCs is orchestrated with that of other skin cells not only along the hair cycle but also in the course of skin regeneration following injury. This review highlights several membrane markers, cytoplasmic proteins and transcription factors associated with epidermal SCs. Keywords: stem cell; epidermal placode; skin adnexa; signalling; hair pigmentation; markers; keratins 1. Epidermal Stem Cells as Units of Development 1.1. Development of the Epidermis and Placode Formation The embryonic skin at very early stages of development is covered by a surface ectoderm that is a precursor to the epidermis and its multiple derivatives. -

Nail Anatomy and Physiology for the Clinician 1
Nail Anatomy and Physiology for the Clinician 1 The nails have several important uses, which are as they are produced and remain stored during easily appreciable when the nails are absent or growth. they lose their function. The most evident use of It is therefore important to know how the fi ngernails is to be an ornament of the hand, but healthy nail appears and how it is formed, in we must not underestimate other important func- order to detect signs of pathology and understand tions, such as the protective value of the nail plate their pathogenesis. against trauma to the underlying distal phalanx, its counterpressure effect to the pulp important for walking and for tactile sensation, the scratch- 1.1 Nail Anatomy ing function, and the importance of fi ngernails and Physiology for manipulation of small objects. The nails can also provide information about What we call “nail” is the nail plate, the fi nal part the person’s work, habits, and health status, as of the activity of 4 epithelia that proliferate and several well-known nail features are a clue to sys- differentiate in a specifi c manner, in order to form temic diseases. Abnormal nails due to biting or and protect a healthy nail plate [1 ]. The “nail onychotillomania give clues to the person’s emo- unit” (Fig. 1.1 ) is composed by: tional/psychiatric status. Nail samples are uti- • Nail matrix: responsible for nail plate production lized for forensic and toxicology analysis, as • Nail folds: responsible for protection of the several substances are deposited in the nail plate nail matrix Proximal nail fold Nail plate Fig. -
Pediatrics-EOR-Outline.Pdf
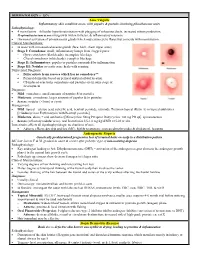
DERMATOLOGY – 15% Acne Vulgaris Inflammatory skin condition assoc. with papules & pustules involving pilosebaceous units Pathophysiology: • 4 main factors – follicular hyperkeratinization with plugging of sebaceous ducts, increased sebum production, Propionibacterium acnes overgrowth within follicles, & inflammatory response • Hormonal activation of pilosebaceous glands which may cause cyclic flares that coincide with menstruation Clinical Manifestations: • In areas with increased sebaceous glands (face, back, chest, upper arms) • Stage I: Comedones: small, inflammatory bumps from clogged pores - Open comedones (blackheads): incomplete blockage - Closed comedones (whiteheads): complete blockage • Stage II: Inflammatory: papules or pustules surrounded by inflammation • Stage III: Nodular or cystic acne: heals with scarring Differential Diagnosis: • Differentiate from rosacea which has no comedones** • Perioral dermatitis based on perioral and periorbital location • CS-induced acne lacks comedones and pustules are in same stage of development Diagnosis: • Mild: comedones, small amounts of papules &/or pustules • Moderate: comedones, larger amounts of papules &/or pustules • Severe: nodular (>5mm) or cystic Management: • Mild: topical – azelaic acid, salicylic acid, benzoyl peroxide, retinoids, Tretinoin topical (Retin A) or topical antibiotics [Clindamycin or Erythromycin with Benzoyl peroxide] • Moderate: above + oral antibiotics [Minocycline 50mg PO qd or Doxycycline 100 mg PO qd], spironolactone • Severe (refractory nodular acne): oral -

Clinical Management of Cutaneous Adverse Events in Patients on Chemotherapy 449
Actas Dermosifiliogr. 2019;110(6):448---459 CONSENSUS DOCUMENT Clinical Management of Cutaneous Adverse Events in Patients on Chemotherapy: A National Consensus Statement by the Spanish Academy of Dermatology and Venereology and the Spanish Society of Medical Oncologyଝ a b c d e f O. Sanmartín, C. Beato, H. Jin Suh-Oh, I. Aragón, A. Espana,˜ M. Majem, g h i,∗ j S. Segura, A. Gúrpide, R. Botella, C. Grávalos a Servicio de Dermatología, Instituto Valenciano de Oncología, Valencia, Espana˜ b Departamento de Oncología Médica, Hospital Universitario Virgen Macarena, Sevilla, Espana˜ c Servicio de Dermatología, Complejo Hospitalario Universitario de Pontevedra, Pontevedra, Espana˜ d Departamento de Oncología Médica, Complejo Hospitalario Universitario de Huelva, Huelva, Espana˜ e Servicio de Dermatología, Clínica Universitaria de Navarra, Pamplona, Espana˜ f Departamento de Oncología Médica, Hospital de la Santa Creu i Sant Pau, Barcelona, Espana˜ g Servicio de Dermatología, Hospital del Mar, Barcelona, Espana˜ h Departamento de Oncología Médica, Clínica Universitaria de Navarra, Pamplona, Espana˜ i Servicio de Dermatología, Hospital Universitario La Fe, Facultad de Medicina, Universidad de Valencia, Valencia, Espana˜ j Servicio de Oncología Médica, Hospital Universitario Doce de Octubre, Madrid, Espana˜ KEYWORDS Abstract Although the arrival of new chemotherapy drugs and combinations has brought Chemotherapy; progress in terms of cancer patient survival, they entail many adverse effects that can Photosensitivity; compromise treatment, and hence -

Nutritional Dermatoses in the Hospitalized Patient
HOSPITAL CONSULT IN PARTNERSHIP WITH THE SOCIETY FOR DERMATOLOGY HOSPITALISTS Nutritional Dermatoses in the Hospitalized Patient Melissa Hoffman, MS; Robert G. Micheletti, MD; Bridget E. Shields, MD Nutritional deficiencies may arise from inadequate nutrient intake, abnormal nutrient absorption, or improper nutrient PRACTICE POINTS utilization.4 Unfortunately, no standardized algorithm for • Nutritional deficiencies are common in hospitalized screening and diagnosing patients with malnutrition exists, patients and often go unrecognized. making early physical examination findings of utmost • Awareness of the risk factors predisposing patients importance. Herein, we present a review of acquired nutri- to nutritional deficiencies and the cutaneous manifes- tional deficiency dermatoses in the inpatient setting. tations associated with undernutrition can promote copy early diagnosis. Protein-Energy Malnutrition • When investigating cutaneous findings, undernutri- tion should be considered in patients with chronic Protein-energy malnutrition (PEM) refers to a set of infections, malabsorptive states, psychiatric illness, related disorders that include marasmus, kwashiorkor and strict dietary practices, as well as in those using (KW), and marasmic KW. These conditions frequently are certain medications. seen in developing countries but also have been reported 5 • Prompt nutritional supplementation can prevent patient in developed nations. Marasmus occurs from a chronic morbidity and mortality and reverse skin disease. deficiencynot of protein and calories. Decreased insulin pro- duction and unopposed catabolism result in sarcopenia and loss of bone and subcutaneous fat.6 Affected patients include children who are less than 60% ideal body weight Cutaneous disease may be the first manifestation of an underlying nutri- 7 tional deficiency, highlighting the importance of early recognition by der- (IBW) without edema or hypoproteinemia. -

Hair Loss in Infancy
SCIENCE CITATIONINDEXINDEXED MEDICUS INDEX BY (MEDLINE) EXPANDED (ISI) OFFICIAL JOURNAL OF THE SOCIETÀ ITALIANA DI DERMATOLOGIA MEDICA, CHIRURGICA, ESTETICA E DELLE MALATTIE SESSUALMENTE TRASMESSE (SIDeMaST) VOLUME 149 - No. 1 - FEBRUARY 2014 Anno: 2014 Lavoro: 4731-MD Mese: Febraury titolo breve: Hair loss in infancy Volume: 149 primo autore: MORENO-ROMERO No: 1 pagine: 55-78 Rivista: GIORNALE ITALIANO DI DERMATOLOGIA E VENEREOLOGIA Cod Rivista: G ITAL DERMATOL VENEREOL G ITAL DERMATOL VENEREOL 2014;149:55-78 Hair loss in infancy J. A. MORENO-ROMERO 1, R. GRIMALT 2 Hair diseases represent a signifcant portion of cases seen 1Department of Dermatology by pediatric dermatologists although hair has always been Hospital General de Catalunya, Barcelona, Spain a secondary aspect in pediatricians and dermatologists 2Universitat de Barcelona training, on the erroneous basis that there is not much in- Universitat Internacional de Catalunya, Barcelona, Spain formation extractable from it. Dermatologists are in the enviable situation of being able to study many disorders with simple diagnostic techniques. The hair is easily ac- cessible to examination but, paradoxically, this approach is often disregarded by non-dermatologist. This paper has Embryology and normal hair development been written on the purpose of trying to serve in the diag- nostic process of daily practice, and trying to help, for ex- ample, to distinguish between certain acquired and some The full complement of hair follicles is present genetically determined hair diseases. We will focus on all at birth and no new hair follicles develop thereafter. the data that can be obtained from our patients’ hair and Each follicle is capable of producing three different try to help on using the messages given by hair for each types of hair: lanugo, vellus and terminal. -

The Integumentary System
CHAPTER 5: THE INTEGUMENTARY SYSTEM Copyright © 2010 Pearson Education, Inc. OVERALL SKIN STRUCTURE 3 LAYERS Copyright © 2010 Pearson Education, Inc. Figure 5.1 Skin structure. Hair shaft Dermal papillae Epidermis Subpapillary vascular plexus Papillary layer Pore Appendages of skin Dermis Reticular • Eccrine sweat layer gland • Arrector pili muscle Hypodermis • Sebaceous (oil) gland (superficial fascia) • Hair follicle Nervous structures • Hair root • Sensory nerve fiber Cutaneous vascular • Pacinian corpuscle plexus • Hair follicle receptor Adipose tissue (root hair plexus) Copyright © 2010 Pearson Education, Inc. EPIDERMIS 4 (or 5) LAYERS Copyright © 2010 Pearson Education, Inc. Figure 5.2 The main structural features of the skin epidermis. Keratinocytes Stratum corneum Stratum granulosum Epidermal Stratum spinosum dendritic cell Tactile (Merkel) Stratum basale Dermis cell Sensory nerve ending (a) Dermis Desmosomes Melanocyte (b) Melanin granule Copyright © 2010 Pearson Education, Inc. DERMIS 2 LAYERS Copyright © 2010 Pearson Education, Inc. Figure 5.3 The two regions of the dermis. Dermis (b) Papillary layer of dermis, SEM (22,700x) (a) Light micrograph of thick skin identifying the extent of the dermis, (50x) (c) Reticular layer of dermis, SEM (38,500x) Copyright © 2010 Pearson Education, Inc. Figure 5.3a The two regions of the dermis. Dermis (a) Light micrograph of thick skin identifying the extent of the dermis, (50x) Copyright © 2010 Pearson Education, Inc. Q1: The type of gland which secretes its products onto a surface is an _______ gland. 1) Endocrine 2) Exocrine 3) Merocrine 4) Holocrine Copyright © 2010 Pearson Education, Inc. Q2: The embryonic tissue which gives rise to muscle and most connective tissue is… 1) Ectoderm 2) Endoderm 3) Mesoderm Copyright © 2010 Pearson Education, Inc. -

Nomina Histologica Veterinaria, First Edition
NOMINA HISTOLOGICA VETERINARIA Submitted by the International Committee on Veterinary Histological Nomenclature (ICVHN) to the World Association of Veterinary Anatomists Published on the website of the World Association of Veterinary Anatomists www.wava-amav.org 2017 CONTENTS Introduction i Principles of term construction in N.H.V. iii Cytologia – Cytology 1 Textus epithelialis – Epithelial tissue 10 Textus connectivus – Connective tissue 13 Sanguis et Lympha – Blood and Lymph 17 Textus muscularis – Muscle tissue 19 Textus nervosus – Nerve tissue 20 Splanchnologia – Viscera 23 Systema digestorium – Digestive system 24 Systema respiratorium – Respiratory system 32 Systema urinarium – Urinary system 35 Organa genitalia masculina – Male genital system 38 Organa genitalia feminina – Female genital system 42 Systema endocrinum – Endocrine system 45 Systema cardiovasculare et lymphaticum [Angiologia] – Cardiovascular and lymphatic system 47 Systema nervosum – Nervous system 52 Receptores sensorii et Organa sensuum – Sensory receptors and Sense organs 58 Integumentum – Integument 64 INTRODUCTION The preparations leading to the publication of the present first edition of the Nomina Histologica Veterinaria has a long history spanning more than 50 years. Under the auspices of the World Association of Veterinary Anatomists (W.A.V.A.), the International Committee on Veterinary Anatomical Nomenclature (I.C.V.A.N.) appointed in Giessen, 1965, a Subcommittee on Histology and Embryology which started a working relation with the Subcommittee on Histology of the former International Anatomical Nomenclature Committee. In Mexico City, 1971, this Subcommittee presented a document entitled Nomina Histologica Veterinaria: A Working Draft as a basis for the continued work of the newly-appointed Subcommittee on Histological Nomenclature. This resulted in the editing of the Nomina Histologica Veterinaria: A Working Draft II (Toulouse, 1974), followed by preparations for publication of a Nomina Histologica Veterinaria. -

Sweat Glands • Oil Glands • Mammary Glands
Chapter 4 The Integumentary System Lecture Presentation by Steven Bassett Southeast Community College © 2015 Pearson Education, Inc. Introduction • The integumentary system is composed of: • Skin • Hair • Nails • Sweat glands • Oil glands • Mammary glands © 2015 Pearson Education, Inc. Introduction • The skin is the most visible organ of the body • Clinicians can tell a lot about the overall health of the body by examining the skin • Skin helps protect from the environment • Skin helps to regulate body temperature © 2015 Pearson Education, Inc. Integumentary Structure and Function • Cutaneous Membrane • Epidermis • Dermis • Accessory Structures • Hair follicles • Exocrine glands • Nails © 2015 Pearson Education, Inc. Figure 4.1 Functional Organization of the Integumentary System Integumentary System FUNCTIONS • Physical protection from • Synthesis and storage • Coordination of immune • Sensory information • Excretion environmental hazards of lipid reserves response to pathogens • Synthesis of vitamin D3 • Thermoregulation and cancers in skin Cutaneous Membrane Accessory Structures Epidermis Dermis Hair Follicles Exocrine Glands Nails • Protects dermis from Papillary Layer Reticular Layer • Produce hairs that • Assist in • Protect and trauma, chemicals protect skull thermoregulation support tips • Nourishes and • Restricts spread of • Controls skin permeability, • Produce hairs that • Excrete wastes of fingers and supports pathogens prevents water loss provide delicate • Lubricate toes epidermis penetrating epidermis • Prevents entry of -

Nails Develop from Thickened Areas of Epidermis at the Tips of Each Digit Called Nail Fields
Nail Biology: The Nail Apparatus Nail plate Proximal nail fold Nail matrix Nail bed Hyponychium Nail Biology: The Nail Apparatus Lies immediately above the periosteum of the distal phalanx The shape of the distal phalanx determines the shape and transverse curvature of the nail The intimate anatomic relationship between nail and bone accounts for the bone alterations in nail disorders and vice versa Nail Apparatus: Embryology Nail field develops during week 9 from the epidermis of the dorsal tip of the digit Proximal border of the nail field extends downward and proximally into the dermis to create the nail matrix primordium By week 15, the nail matrix is fully developed and starts to produce the nail plate Nails develop from thickened areas of epidermis at the tips of each digit called nail fields. Later these nail fields migrate onto the dorsal surface surrounded laterally and proximally by folds of epidermis called nail folds. Nail Func7on Protect the distal phalanx Enhance tactile discrimination Enhance ability to grasp small objects Scratching and grooming Natural weapon Aesthetic enhancement Pedal biomechanics The Nail Plate Fully keratinized structure produced throughout life Results from maturation and keratinization of the nail matrix epithelium Attachments: Lateral: lateral nail folds Proximal: proximal nail fold (covers 1/3 of the plate) Inferior: nail bed Distal: separates from underlying tissue at the hyponychium The Nail Plate Rectangular and curved in 2 axes Transverse and horizontal Smooth, although -

There Are 25 Questions, Each Worth 3 Points and a Short Essay Worth 25 Points. DO YOUR OWN WORK !! Use Your Time Wisely 1. T
Mr. Holder Integumentary System – Unit 5 December 3, 2015 ARC TEST 1.0 DO NOT MARK OR WRITE ON THIS QUIZ !! There are 25 questions, each worth 3 points and a short essay worth 25 points. DO YOUR OWN WORK !! Use Your Time Wisely 1. The Integumentary System is divided into how many layers? a) 2 b) 3 c) 4 d) 6 2. What are the two major groups of membranes covering the human body? a) Epithelial & Mucus b) Cutaneous & Mucus c) Epithelial & Connective Tissue d) None of these 3. Which internal membrane provides protection for your joints? a) Serous b) Synovial c) Cutaneous d) Mucus 4. These membranes line internal cavities exposed to air & excrete a gooey substance. a) Serous b) Synovial c) Cutaneous d) Mucus 5. The Integumentary System protects the human body from … a) Friction b) Hot & Cold Temperature c) Bacteria d) All of These 6. Which stratum of the epidermis is full of keratin, cornified to prevent water loss? a) Basale b) Granulosum c) Corneum d) None of These 7. Which body system extends into the dermis to provide information to your brain? a) Cardiovascular b) Immune c) Integumentary d) Nervous 8. Subcutaneous tissue includes adipose tissue or fat. It is also known as the … a) Dermis b) Papillary Layer c) Hypodermis d) Reticular Layer 9. The dermis is divided into two layers. Which of these is the thickest? a) Papillary b) Reticular c) Basale d) Hypodermis 10. Which stratum of the epidermis is responsible for new cell production? a) Corneum b) Basale c) Granulosum d) Spinosum Page 1 Mr. -

Nail Involvement in Alopecia Areata
212 CLINICAL REPORT Nail Involvement in Alopecia Areata: A Questionnaire-based Survey on DV Clinical Signs, Impact on Quality of Life and Review of the Literature 1 2 2 1 cta Yvonne B. M. ROEST , Henriët VAN MIDDENDORP , Andrea W. M. EVERS , Peter C. M. VAN DE KERKHOF and Marcel C. PASCH1 1 2 A Department of Dermatology, Radboud University Nijmegen Medical Center, Nijmegen, and Health, Medical and Neuropsychology Unit, Institute of Psychology, Leiden University, Leiden, The Netherlands Alopecia areata (AA) is an immune-mediated disease at any age, but as many as 60% of patients with AA will causing temporary or permanent hair loss. Up to 46% present with their first patch before 20 years of age (4), and of patients with AA also have nail involvement. The prevalence peaks between the 2nd and 4th decades of life (1). aim of this study was to determine the presence, ty- AA is a lymphocyte cell-mediated inflammatory form pes, and clinical implications of nail changes in pa- of hair loss in which a complex interplay between genetic enereologica tients with AA. This questionnaire-based survey eva- factors and underlying autoimmune aetiopathogenesis V luated 256 patients with AA. General demographic is suggested, although the exact aetiological pathway is variables, specific nail changes, nail-related quality of unknown (5). Some studies have shown association with life (QoL), and treatment history and need were evalu- other auto-immune diseases, including asthma, atopic ated. Prevalence of nail involvement in AA was 64.1%. dermatitis, and vitiligo (6). ermato- The specific nail signs reported most frequently were Many patients with AA also have nail involvement, D pitting (29.7%, p = 0.008) and trachyonychia (18.0%).