Male Reproductive System
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-
Reproductive System
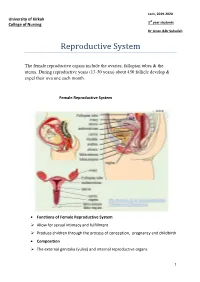
Lec1, 2019-2020 University of Kirkuk 3rd year students College of Nursing Dr Jenan &Dr Suhailah Reproductive System The female reproductive organs include the ovaries, fallopian tubes & the uterus. During reproductive years (13-50 years) about 450 follicle develop & expel their ova one each month. Female Reproductive System Functions of Female Reproductive System Allow for sexual intimacy and fulfillment Produce children through the process of conception, pregnancy and childbirth Composition The external genitalia (vulva) and internal reproductive organs 1 External genitalia of the female reproductive system: Mons pubis Labia majora Labia minora Clitoris Vestibule Perineum Internal Reproductive Organs Vagina (Birth canal) - A muscular tube that leads from the vulva to the uterus Uterus (Womb) A hollow, pear-shaped muscular structure Functions of the uterus: 1. Prepare for pregnancy each month 2. Protect and nourish the growing child Four sections: Cervix - Connect the vagina and uterus - Outer os Uterine Isthmus - Connects the cervix to the main body of the uterus - Thinnest portion of the uterus, and does not participate in the muscular Contractions of labor - Most likely to rupture during childbirth Corpus (Body) - Main body of the uterus 2 Fundus Topmost section of the uterus Walls of the corpus and fundus have three layers - Perimetrium - Myometrium - Endometrium Paired fallopian tubes - Tiny, muscular corridors 8-14 cm long 3 sections 1. Isthmus 2. Ampulla 3. Infundibulum Ovaries Two sex glands homologous to the male testes; located on either side of the uterus Functions: - Produce the female hormones estrogen and progesterone - Store ova and help them to mature - Regulate the menstrual cycle in response to anterior pituitary hormones 3 Regulation of Reproductive function: Puberty - The time of life in which an individual become capable of sexual reproduction. -

Normal Imaging Findings of the Uterus 3
Normal Image Findings of the Uterus 37 Normal Imaging Findings of the Uterus 3 Claudia Klüner and Bernd Hamm CONTENTS the strong muscle coat forming the mass of the organ. The myometrium is mostly comprised of spindle- 3.1 Embryonic Development and shaped smooth muscle cells and additionally con- Normal Anatomy of the Uterus 37 tains reserve connective tissue cells, which give rise 3.2 Imaging Findings: Uterine Corpus 40 to additional myometrial cells in pregnancy through 3.3 Imaging Findings: Uterine Cervix 44 hyperplasia. The uterine cavity is only a thin cleft and References 47 is lined by endometrium (Fig. 3.2). Functionally, the endometrium consists of basal and functional layers. The isthmus of uterus (lower uterine segment), 3.1 together with the internal os, forms the junction be- Embryonic Development and tween the corpus and cervix. In nonpregnant wom- Normal Anatomy of the Uterus en the isthmus is only about 5 mm high and is less muscular than the corpus. Unlike the uterine cervix, During embryonal life, fusion of the two Müllerian the isthmus becomes overproportionally large in the ducts gives rise to the uterine corpus, isthmus, cervix, course of pregnancy and serves as a kind of reserve and the upper third of the vagina. The Müllerian ducts for fetal development in addition to the uterine cor- are of mesodermal origin and arise in the 4th week pus. The endometrium of the isthmus consists of a of gestation. They course on both sides lateral to the single layer of columnar epithelium and only under- ducts of the mesonephros (Wolffi an ducts). -

Clinical Research of Effects of Retaining the Uterine Blood Supply Hysterectomy on Ovarian Function
BIO Web of Conferences 8 , 01038 (2017)DOI: 10.1051/bioconf/201 70801038 ICMSB2016 Clinical research of effects of retaining the uterine blood supply hysterectomy on ovarian function Yufei Cai 1 and Hongxia Sun 2,a 1Obstetrics and Gynecology Department,Affiliated Hospital of Beihua University 2 Pharmacological Department, Pharmacy, Beihua University jilin jilin 132011, China Abstract. Objective To evaluate the effect of hysterectomy for reserving the uterine blood supply on ovarian endocrine function and on symptoms of menopausal transition. Methods Uterine benign lesions should be line the uterus times total resection in 100 patients were randomly divided into hysterectomy group of retaining uterus vascular supply group(research group,n=50) and traditional total hysterectomy group (the control group, n=50), comparing two groups in operation time, intraoperative bleeding ,postoperative fever and residual polyp, blood tests were taken to check the serum sex hormone levels change and clinical observation for perimenopausal symptoms before and postoperative three months, six months, one year and two years at the same time respectively. Results There was no significant difference between two groups in operation time, intraoperative blood loss, postoperative fever and residual polyp (P>0.05). There was no significant difference among research group before and after operation in serum sex hormones(P>0.05),the symptoms of the menopausal transition hardly appear; postoperative FSH, LH increased significantly in control group (P<0.05),E2 decrease (P<0.05), perimenopausal symptoms appeared more often. Conclusion The effect of uterus hysterectomy for retaining vascular supply on ovarian endocrine function is less than the traditional total hysterectomy, this operation has a certain importance to preserve ovarian function and delay the occurrence of premature ovarian aging. -

CHAPTER 6 Perineum and True Pelvis
193 CHAPTER 6 Perineum and True Pelvis THE PELVIC REGION OF THE BODY Posterior Trunk of Internal Iliac--Its Iliolumbar, Lateral Sacral, and Superior Gluteal Branches WALLS OF THE PELVIC CAVITY Anterior Trunk of Internal Iliac--Its Umbilical, Posterior, Anterolateral, and Anterior Walls Obturator, Inferior Gluteal, Internal Pudendal, Inferior Wall--the Pelvic Diaphragm Middle Rectal, and Sex-Dependent Branches Levator Ani Sex-dependent Branches of Anterior Trunk -- Coccygeus (Ischiococcygeus) Inferior Vesical Artery in Males and Uterine Puborectalis (Considered by Some Persons to be a Artery in Females Third Part of Levator Ani) Anastomotic Connections of the Internal Iliac Another Hole in the Pelvic Diaphragm--the Greater Artery Sciatic Foramen VEINS OF THE PELVIC CAVITY PERINEUM Urogenital Triangle VENTRAL RAMI WITHIN THE PELVIC Contents of the Urogenital Triangle CAVITY Perineal Membrane Obturator Nerve Perineal Muscles Superior to the Perineal Sacral Plexus Membrane--Sphincter urethrae (Both Sexes), Other Branches of Sacral Ventral Rami Deep Transverse Perineus (Males), Sphincter Nerves to the Pelvic Diaphragm Urethrovaginalis (Females), Compressor Pudendal Nerve (for Muscles of Perineum and Most Urethrae (Females) of Its Skin) Genital Structures Opposed to the Inferior Surface Pelvic Splanchnic Nerves (Parasympathetic of the Perineal Membrane -- Crura of Phallus, Preganglionic From S3 and S4) Bulb of Penis (Males), Bulb of Vestibule Coccygeal Plexus (Females) Muscles Associated with the Crura and PELVIC PORTION OF THE SYMPATHETIC -

Modified Radical Abdominal Trachelectomy in Cervical Cancer in Young Women. J. Life Sci. Biomed. 8(1): 19-23;
2018 SCIENCELINE Journal of Life Science and Biomedicine J Life Sci Biomed, 8(1): 19-23, 2018 License: CC BY 4.0 ISSN 2251-9939 Modified Radical Abdominal Trachelectomy in Cervical Cancer in Young Women Visola Sarimbekovna NAVRUZOVA (MD) National Center for Cancer Research under the MoH Tashkent, Uzbekistan Corresponding author’s Email: [email protected] ABSTRACT Original Article A modification of traditional fertility-sparing abdominal radical trachelectomy PII: S225199391800004-8 (ART) has been developed to reduce the opportunity for intra-operative injuries to occur through better management of the surgical field. The technique is similar to Rec. 03 Nov. 2017 the standard abdominal radical trachelectomy. The ART modification developed by Acc. 16 Jan. 2018 us enables to perform total or partial resection of the affected part of the uterine Pub. 25 Jan. 2018 cervix after total mobilization of the cervix and excision of the upper and middle Keywords parts of the vagina. We have performed 204 modified fertility-sparing ARTs for CC Cervical Cancer, women of reproductive age (27 to 37 years) at the early stage of the disease (T1A, Squamous Cells, T1B). On average the surgery lasted 140 ± 28.7 min, blood loss was 420 ± 50 ml. Dynamic Monitoring, Epithelization of the uterine stump after surgery lasted 5 - 8 weeks. No intra- Fertility-Sparing Surgery, operative injuries of the nearby organs occurred. The follow-up period has lasted for Abdominal Radical 42 months. Oncological outcomes. No patient had CC recurrence and metastasis (till Trachelectomy, 42 months after the first surgery). Quality of Life INTRODUCTION Cervical cancer (CC) is known to be the second most common malignancy in women worldwide [1]. -

Breast and Pelvic Anatomy Dwight E
Breast and Pelvic Anatomy Dwight E. Hooper, MD, MBA The Female Breast This bilateral organ that lies anterior to the pectoral muscles is typically asymmetrical in size. The anatomy of the breasts is quite variable in terms of the overall size including the size and color of the areola (pronounced either: a REE la or air ree O la). Size is also relative in terms of diameter and anterior projection of the nipple. While the breast is often circular in shape, quite often there is a projection of the breasts tissue extending into the axilla. This projection is referred to as the Axillary Tail (of Spence). Beneath the skin of the breast is a layer of corium, and beneath it is what makes the greatest volume of the breast ‐ fat lobules. There is also glandular and stromal tissue within the substance of the breast. Diving from the nipple deep into the breast are lactiferous ducts. Supporting the breasts positioning on the chest are the ligaments of Cooper. Frequently, following repeated extension and retraction of the ligaments of Cooper (during the change in breast size from pregnancy or other instances of dramatic weight/ fat changes) the ligaments become more lax thereby altering the breasts position (pre‐ versus post‐pregnancy/ weight change). The Female Pelvis Description of the female pelvis can be divided into three categories: the bony pelvis, external anatomy, and internal (or surgical anatomy). The bony pelvis consisting of bilateral iliac, ischium, and pubic bones anchored to the sacrum, results in several typical shapes. The shape most often found in adult females is the gynecoid pelvis which is of a configuration most consistent with vaginal childbirth as distinguished from the android (the typical male pelvis) or platypeloid pelvises. -

The Female Reproductive Organs Include the Ovaries, Fallopian Tubes & the Uterus. During Reproductive Years (13-50 Years) Ab
University of Kirkuk Lec 2 College of Nursing Reproductive System 3rd Class2019-2020 Dr. jenan, Dr Suhailah The female reproductive organs include the ovaries, fallopian tubes & the uterus. During reproductive years (13-50 years) about 450 follicle develop & expel their ova one each month. Female Reproductive System Functions of Female Reproductive System Allow for sexual intimacy and fulfillment Produce children through the process of conception, pregnancy and childbirth Composition The external genitalia (vulva) and internal reproductive organs 1 External genitalia of the female reproductive system: Mons pubis Labia majora Labia minora Clitoris Vestibule Perineum Internal Reproductive Organs Vagina (Birth canal) - A muscular tube that leads from the vulva to the uterus Uterus (Womb) A hollow, pear-shaped muscular structure Functions of the uterus: 1. Prepare for pregnancy each month 2. Protect and nourish the growing child Four sections: Cervix - Connect the vagina and uterus - Outer os Uterine Isthmus - Connects the cervix to the main body of the uterus - Thinnest portion of the uterus, and does not participate in the muscular Contractions of labor - Most likely to rupture during childbirth Corpus (Body) - Main body of the uterus 2 Fundus Top most section of the uterus Walls of the corpus and fundus have three layers - Perimetrium - Myometrium - Endometrium Paired fallopian tubes - Tiny, muscular corridors 8-14 cm long 3 sections 1. Isthmus 2. Ampulla 3. Infundibulum Ovaries Two sex glands homologous to the male testes; located on either side of the uterus Functions: - Produce the female hormones estrogen and progesterone - Store ova and help them to mature - Regulate the menstrual cycle in response to anterior pituitary hormones 3 Regulation of Reproductive function: Puberty - The time of life in which an individual become capable of sexual reproduction. -

Clinical Characteristics of Congenital Cervical Atresia Based on Anatomy
Xie et al. European Journal of Medical Research 2014, 19:10 http://www.eurjmedres.com/content/19/1/10 EUROPEAN JOURNAL OF MEDICAL RESEARCH RESEARCH Open Access Clinical characteristics of congenital cervical atresia based on anatomy and ultrasound: a retrospective study of 32 cases Zhihong Xie1*, Xiaoping Zhang1, Jiandong Liu2, Ningzhi Zhang1, Hong Xiao1, Yongying Liu1, Liang Li1 and Xiaoying Liu3 Abstract Background: To explore the clinical characteristics of congenital cervical atresia. Methods: This retrospective analysis included 32 cases of congenital cervical atresia treated from March 1984 to September 2010. The anatomic location, ultrasonic features, surgical treatments, and outcomes were recorded. Results: Based on clinical characteristics observed during preoperative ultrasound and intraoperative exploration, congenital cervical atresia was divided into four types. Type I (n = 22/32, 68.8%) is incomplete cervical atresia. Type II (n = 5/32, 15.6%) defines a short and solid cervix with a round end; the structure lacked uterosacral and cardinal ligament attachments to the lower uterine body. Type III (n = 2/32, 6.3%) is complete cervical atresia, in which the lowest region of the uterus exhibited a long and solid cervix. Type IV (n = 3/32, 9.4%) defines the absence of a uterine isthmus, in which no internal os was detected, and a blind lumen was found under the uterus. Conclusions: Observations of clinical characteristics of congenital cervical atresia based on the anatomy and ultrasound may inform diagnosis and treatment strategy. Keywords: cervicovaginal operation, congenital cervical atresia, Müllerian duct anomaly Background system, which is based on the ‘tumor nodes metastases’ Congenital cervical atresia is a relatively rare Müllerian principle in oncology [8]; and the new European Society of duct anomaly of the female reproductive tract that was Human Reproduction and Embryology/European Society first reported by Ludwig in 1900. -

The Female Reproductive Organs Include the Ovaries, Fallopian Tubes & the Uterus
University of Kirkuk Lec 1 College of Nursing Reproductive System 3rd Class2020-2021 Dr. jenan, Dr Suhailah The female reproductive organs include the ovaries, fallopian tubes & the uterus. During reproductive years (13-50 years) about 450 follicle develop & expel their ova one each month. Female Reproductive System ● Functions of Female Reproductive System ⮚ Allow for sexual intimacy and fulfillment ⮚ Produce children through the process of conception, pregnancy and childbirth ● Composition ⮚ The external genitalia (vulva) and internal reproductive organs 1 External genitalia of the female reproductive system: ● Mons pubis ● Labia majora ● Labia minora ● Clitoris ● Vestibule ● Perineum Internal Reproductive Organs ● Vagina (Birth canal) - A muscular tube that leads from the vulva to the uterus ● Uterus (Womb) A hollow, pear-shaped muscular structure Functions of the uterus: 1. Prepare for pregnancy each month 2. Protect and nourish the growing child Four sections: ⮚ Cervix - Connect the vagina and uterus - Outer os ⮚ Uterine Isthmus - Connects the cervix to the main body of the uterus - Thinnest portion of the uterus, and does not participate in the muscular Contractions of labor - Most likely to rupture during childbirth ⮚ Corpus (Body) - Main body of the uterus 2 Fundus Top most section of the uterus Walls of the corpus and fundus have three layers - Perimetrium - Myometrium - Endometrium ⮚ Paired fallopian tubes - Tiny, muscular corridors 8-14 cm long 3 sections 1. Isthmus 2. Ampulla 3. Infundibulum ⮚ Ovaries Two sex glands homologous to the male testes; located on either side of the uterus Functions: - Produce the female hormones estrogen and progesterone - Store ova and help them to mature 3 - Regulate the menstrual cycle in response to anterior pituitary hormones Regulation of Reproductive function: ● Puberty - The time of life in which an individual become capable of sexual reproduction. -

Part II: Reproductive System Outlines • Revision of Anatomy & Physiology
Part II: Reproductive System Outlines Revision of anatomy & physiology of reproductive system (male& female). Menstrual Cycle. Learning Objectives At the end of this chapter, the student should be able to: 1. Explain two major functions of the reproductive system. 2. Label an anatomic drawing of the female and male reproductive systems, including external genitalia and internal anatomy. 3. Discuss major functions of each reproductive structure, gland, and organ. 4. Trace the path of sperm through the male reproductive system, from the site of formation to ejaculation from the body. 5. Describe the process of semen production. 6. Compare hormonal regulation of male reproductive function with that of the female. 7. Illustrate the inter-relationships of the ovarian and uterine cycles and the overall menstrual cycle. 8. Describe and compare the male and female sexual response cycles. Reproductive Systems • External and internal parts. • Main purpose – produce offspring. • Secondary functions. – Allow for sexual intimacy and fulfillment. – Provide a conduit for urinary elimination. • Most structures paired. • Male and female systems complementary. Male Reproductive System • Testes produce gametes (sperm). • Contains one half of genetic material needed to produce human baby. • Urinary tract and reproductive system closely connected. Male External Genitalia • Penis – Composed of a bulbous head, called the glans penisor glans, and a shaft. – Serves a dual role as the male organ of reproduction and as the external organ of urinary elimination. • Scrotum – An external sac that houses the testes in two internal compartments. – Protects the testes from trauma and regulates the temperature within the testes. Male Internal Reproductive Organs: • Testes – Two oval organs, one within each scrotal sac. -
Laparoscopic Correction of the Uterine Muscle Loss in the Scar After a Caesarean Section Delivery
Case report Videosurgery Laparoscopic correction of the uterine muscle loss in the scar after a Caesarean section delivery Michał Ciebiera, Grzegorz Jakiel, Aneta Słabuszewska-Jóźwiak 1st Department of Obstetrics and Gynaecology, Medical Centre of Postgraduate Education, Warsaw, Poland Videosurgery Miniinv 2013; 8 (4): 342–345 DOI: 10.5114/wiitm.2013.39514 Abstract Caesarean section is the most frequently c onducted surgery in modern obstetrics. It involves a significant risk of com - plications; also disorders in the area of the scar after hysterotomy may lead to menstrual disorders, pain and sec - ondary infertility. In light of the presented facts the significance of a good uterus muscle correction method is high. We present a case of a 28-year-old patient after Caesarean section with further reproductive plans. In the ultrasono - graphic examination the residual thickness of the uterine wall was approx. 2.5–3 mm. The patient was operated on using laparoscopy and the fibrotic scar tissue was removed. During the follow-up examination in transvaginal ultra - sonography the uterine muscularis was continuous on the whole surface. Laparoscopic treatment ensures the appro - priate visibility which makes the risk of damage to the adjacent organs lower, and the time of convalescence is short. It provides repetitive good results from the anatomical and functional points of view. Key words: Caesarean section, laparoscopy, uterine scar, minimally invasive surgery. Introduction and the dehiscence of the scar after a Caesarean sec - A Caesarean section is the most frequently con - tion [4–9]. Disorders within the area of a scar after ducted surgery in modern obstetrics and it consists a Caesarean section delivery may constitute aetiolog - in a surgical incision of skin integuments, as well as ical factors for menstrual disorders, painful menstru - an incision of the anterior wall of the uterus, after ations, intermenstrual bleeding, and also the cause of which a child is delivered. -
The Structure and Function of the Cervix During Pregnancy Translational
Translational Research in Anatomy 2 (2016) 1e7 Contents lists available at ScienceDirect Translational Research in Anatomy journal homepage: http://www.journals.elsevier.com/translational- research-in-anatomy The structure and function of the cervix during pregnancy James P. Nott a, Elizabeth A. Bonney b, James D. Pickering c, Nigel A.B. Simpson a, * a Division of Women's and Children's Health, School of Medicine, University of Leeds, Leeds, UK b Leeds Teaching Hospitals NHS Trust, Leeds, UK c Division of Anatomy, School of Medicine, University of Leeds, Leeds, UK article info abstract Article history: The structure of the cervix is integral to the maintenance of pregnancy, keeping the developing baby in Received 8 December 2015 utero and forming a barrier to the ascent of microorganisms from the vagina. Weakness of the cervix may Received in revised form lead to deficiency of this barrier and is associated with subsequent preterm birth. The underlying cause 25 January 2016 of this structural weakness is poorly understood. In this paper we review the structure and function of Accepted 29 February 2016 the cervix before and during pregnancy. The causes of mechanical failure of the cervix during pregnancy Available online 2 March 2016 are described, with a specific focus on the internal cervical os. We highlight the role of the internal cervical os in causing preterm birth and discuss research techniques that may provide further insight into Keywords: Cervix its function during pregnancy. It is hoped that clinical translation of this knowledge will enable the early fi fi Pregnancy and appropriate identi cation of women who will bene t from strategies to reinforce the internal os and Preterm birth so reduce the incidence of preterm birth.