Breast and Pelvic Anatomy Dwight E
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-
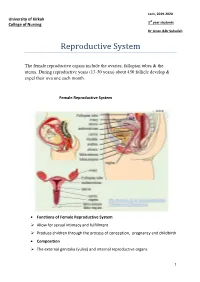
Reproductive System
Lec1, 2019-2020 University of Kirkuk 3rd year students College of Nursing Dr Jenan &Dr Suhailah Reproductive System The female reproductive organs include the ovaries, fallopian tubes & the uterus. During reproductive years (13-50 years) about 450 follicle develop & expel their ova one each month. Female Reproductive System Functions of Female Reproductive System Allow for sexual intimacy and fulfillment Produce children through the process of conception, pregnancy and childbirth Composition The external genitalia (vulva) and internal reproductive organs 1 External genitalia of the female reproductive system: Mons pubis Labia majora Labia minora Clitoris Vestibule Perineum Internal Reproductive Organs Vagina (Birth canal) - A muscular tube that leads from the vulva to the uterus Uterus (Womb) A hollow, pear-shaped muscular structure Functions of the uterus: 1. Prepare for pregnancy each month 2. Protect and nourish the growing child Four sections: Cervix - Connect the vagina and uterus - Outer os Uterine Isthmus - Connects the cervix to the main body of the uterus - Thinnest portion of the uterus, and does not participate in the muscular Contractions of labor - Most likely to rupture during childbirth Corpus (Body) - Main body of the uterus 2 Fundus Topmost section of the uterus Walls of the corpus and fundus have three layers - Perimetrium - Myometrium - Endometrium Paired fallopian tubes - Tiny, muscular corridors 8-14 cm long 3 sections 1. Isthmus 2. Ampulla 3. Infundibulum Ovaries Two sex glands homologous to the male testes; located on either side of the uterus Functions: - Produce the female hormones estrogen and progesterone - Store ova and help them to mature - Regulate the menstrual cycle in response to anterior pituitary hormones 3 Regulation of Reproductive function: Puberty - The time of life in which an individual become capable of sexual reproduction. -

Impotence Due to External Iliac Steal Syndrome
Case Report http://dx.doi.org/10.3348/kjr.2013.14.1.81 pISSN 1229-6929 · eISSN 2005-8330 Korean J Radiol 2013;14(1):81-85 Impotence due to External Iliac Steal Syndrome: Treatment with Percutaneous Transluminal Angioplasty and Stent Placement Serkan Gür, MD1, Levent Oguzkurt, MD2, Bilal Kaya, MD2, Güven Tekbas, MD2, Ugur Ozkan, MD2 1Sifa University, Department of Radiology, 35240 Basmane, Izmir, Turkey; 2Baskent University, Faculty of Medicine, Department of Radiology, 01250, Yüregir, Adana, Turkey We report a case of erectile dysfunction caused by external iliac artery occlusion, associated with pelvic steal syndrome; bilateral internal iliac arteries were patent. The patient stated that he had experienced erectile dysfunction at similar times along with claudication, but he did not mention it before angiography. He expressed that the erectile dysfunction did not last long and that he felt completely okay after the interventional procedure, in addition to his claudication. Successful treatment of the occlusion, by percutaneous transluminal angioplasty and stent implantation, helped resolve erectile dysfunction completely and treat the steal syndrome. Index terms: Erectile dysfunction; Pelvic steal syndrome; Percutaneous angioplasty INTRODUCTION and obstructive disease of the penile arteries are two main vascular causes of impotence. Obstructive arterial diseases Erectile dysfunction (ED) affects 10% of men between cause impotence by obstructing blood supply to the penis, the ages of 40 and 70 (1). ED includes multiple negative and impotence also occurs when the rare entities do not consequences; it was once believed to be a primarily obstruct the blood flow to the penis rather divert blood flow psychological problem. However, it has been estimated away from it. -

The Incidence and Anatomy of Accessory Pudendal Arteries As
The Incidence and Anatomy of Accessory Pudendal Arteries as Depicted on Multidetector-Row CT Angiography: Clinical Implications of Preoperative Evaluation for Laparoscopic and Robot-Assisted Radical Prostatectomy Beom Jin Park, MD1 Objective: To help preserve accessory pudendal arteries (APAs) and to Deuk Jae Sung, MD1 ensure optimal postoperative sexual function after a laparoscopic or robot-assist- Min Ju Kim, MD1 ed radical prostatectomy, we have evaluated the incidence of APAs as detected Sung Bum Cho, MD1 on multidetector-row CT (MDCT) angiography and have provided a detailed 1 Yun Hwan Kim, MD anatomical description. Kyoo Byung Chung, MD1 Materials and Methods: The distribution of APAs was evaluated in 121 con- Seok Ho Kang, MD2 secutive male patients between February 2006 and July 2007 who underwent 64- Jun Cheon, MD2 channel MDCT angiography of the lower extremities. We defined an APA as any artery located within the periprostatic region running parallel to the dorsal vascu- lar complex. We also subclassified APAs into lateral and apical APAs. Two radiol- ogists retrospectively evaluated the origin, course and number of APAs; the final Index terms: Accessory pudendal arteries APA subclassification based on MDCT angiography source data was determined Computed tomography (CT) by consensus. Angiography Results: We identified 44 APAs in 36 of 121 patients (30%). Two distinct vari- Laparoscopy Prostatectomy eties of APAs were identified. Thirty-three APAs (75%) coursed near the antero- lateral region of the prostatic apex, termed apical APAs. The remaining 11 APAs DOI:10.3348/kjr.2009.10.6.587 (25%) coursed along the lateral aspect of the prostate, termed lateral APAs. -

Vaginal Health After Breast Cancer: a Guide for Patients
Information Sheet Vaginal health after breast cancer: A guide for patients Key points • Women who have had breast cancer treatment before menopause may develop a range of symptoms related to low oestrogen levels, while post-menopausal women may have a worsening of their symptoms. • These symptoms relate to both the genital and urinary tracts. • A range of both non-prescription/lifestyle and prescription treatments is available. Discuss your symptoms with your specialist or general practitioner as they will be able to advise you, based on your individual situation. • Women who have had breast cancer treatment before menopause might find they develop symptoms such as hot flushes, night sweats, joint aches and vaginal dryness. • These are symptoms of low oestrogen, which occur naturally with age, but may also occur in younger women undergoing treatment for breast cancer. These changes are called the genito-urinary syndrome of menopause (GSM), which was previously known as atrophic vaginitis. • Unlike some menopausal symptoms, such as hot flushes, which may go away as time passes, vaginal dryness, discomfort with intercourse and changes in sexual function often persist and may get worse with time. • The increased use of adjuvant treatments (medications that are used after surgery/chemotherapy/radiotherapy), which evidence shows reduce the risk of the cancer recurring, unfortunately leads to more side-effects. • Your health and comfort are important, so don’t be embarrassed about raising these issues with your doctor. • This Information Sheet offers some advice for what you can do to maintain the health of your vagina, your vulva (the external genitals) and your urethra (outlet from the bladder), with special attention to the needs of women who have had breast cancer treatment. -

Normal Imaging Findings of the Uterus 3
Normal Image Findings of the Uterus 37 Normal Imaging Findings of the Uterus 3 Claudia Klüner and Bernd Hamm CONTENTS the strong muscle coat forming the mass of the organ. The myometrium is mostly comprised of spindle- 3.1 Embryonic Development and shaped smooth muscle cells and additionally con- Normal Anatomy of the Uterus 37 tains reserve connective tissue cells, which give rise 3.2 Imaging Findings: Uterine Corpus 40 to additional myometrial cells in pregnancy through 3.3 Imaging Findings: Uterine Cervix 44 hyperplasia. The uterine cavity is only a thin cleft and References 47 is lined by endometrium (Fig. 3.2). Functionally, the endometrium consists of basal and functional layers. The isthmus of uterus (lower uterine segment), 3.1 together with the internal os, forms the junction be- Embryonic Development and tween the corpus and cervix. In nonpregnant wom- Normal Anatomy of the Uterus en the isthmus is only about 5 mm high and is less muscular than the corpus. Unlike the uterine cervix, During embryonal life, fusion of the two Müllerian the isthmus becomes overproportionally large in the ducts gives rise to the uterine corpus, isthmus, cervix, course of pregnancy and serves as a kind of reserve and the upper third of the vagina. The Müllerian ducts for fetal development in addition to the uterine cor- are of mesodermal origin and arise in the 4th week pus. The endometrium of the isthmus consists of a of gestation. They course on both sides lateral to the single layer of columnar epithelium and only under- ducts of the mesonephros (Wolffi an ducts). -

Clinical Pelvic Anatomy
SECTION ONE • Fundamentals 1 Clinical pelvic anatomy Introduction 1 Anatomical points for obstetric analgesia 3 Obstetric anatomy 1 Gynaecological anatomy 5 The pelvic organs during pregnancy 1 Anatomy of the lower urinary tract 13 the necks of the femora tends to compress the pelvis Introduction from the sides, reducing the transverse diameters of this part of the pelvis (Fig. 1.1). At an intermediate level, opposite A thorough understanding of pelvic anatomy is essential for the third segment of the sacrum, the canal retains a circular clinical practice. Not only does it facilitate an understanding cross-section. With this picture in mind, the ‘average’ of the process of labour, it also allows an appreciation of diameters of the pelvis at brim, cavity, and outlet levels can the mechanisms of sexual function and reproduction, and be readily understood (Table 1.1). establishes a background to the understanding of gynae- The distortions from a circular cross-section, however, cological pathology. Congenital abnormalities are discussed are very modest. If, in circumstances of malnutrition or in Chapter 3. metabolic bone disease, the consolidation of bone is impaired, more gross distortion of the pelvic shape is liable to occur, and labour is likely to involve mechanical difficulty. Obstetric anatomy This is termed cephalopelvic disproportion. The changing cross-sectional shape of the true pelvis at different levels The bony pelvis – transverse oval at the brim and anteroposterior oval at the outlet – usually determines a fundamental feature of The girdle of bones formed by the sacrum and the two labour, i.e. that the ovoid fetal head enters the brim with its innominate bones has several important functions (Fig. -

Download Article
Advances in Social Science, Education and Humanities Research, volume 356 2nd International Conference on Contemporary Education, Social Sciences and Ecological Studies (CESSES 2019) A New Exploration of the Combined Treatment of Symptoms and Social Work Psychology in Male Sexual Addiction Patients Chengchung Tsai Minyi Li School of Management School of Social Sciences Putian University University of Macau Putian, China Macau, China Abstract—Post-Orgasmic Illness Syndrome (POIS) was progesterone, low cholesterol, low dehydroepiandrosterone, first discovered by Professor Waldinger and Schweitzerl in low cortisol, high prolactin or hypothyroidism. Some cases 2002. After publishing several papers such as "POIS Records encountered by the author team indicate that when the of Emotional, Psychological and Behavioral Changes in Male mother was pregnant in the early years, she or her family had Patients" and "POIS Patients", "Clinical Observation Records smoking habits. Some mothers had long-term use of of Psychological and Behavioral Changes" and "POIS Male contraceptives or were used to eating animal internal organs. Disease Self-reports and Treatment Methods", in this paper, Even some cases were diagnosed as male gynecomastia. the author will cite the views of Chinese medicine practitioners on the treatment of POIS, and hope to provide more practical treatment methods and references for future research. TABLE I. SEVEN GROUPS OF POIS SYMPTOMS FOUND BY WALDINGER AND OTHER MEDICAL TEAMS Keywords—POIS; male; ejaculation; mental state; disorder; Body parts Various local sensations emotion Behavioral symptoms extreme fatigue, exhaustion, palpitations, forgetting words, being too lazy to talk, incoherent, inattention, irritability, I. INTRODUCTION photophobia, depression The main research objects of this paper are journalists, Flu symptoms fever, cold, hot, sweaty, trembling writers and other text workers, as well as creative designers Head symptoms head dizziness, groggy, confused and heavy who take creativity as the selling point as the research object. -

Details of the Available Literature on Sex for Induction of Labour
Appendix 1: Details of the available literature on sex for induction of labour At term, nipple and genital stimulation have been advocated as a way of naturally promoting the release of endogenous oxytocin. 1 In 2005, a Cochrane Review examined the evidence for breast stimulation as a method for inducing labour and found six trials of 719 women, showing a decrease in the number of women not in labour at 72 hours with nipple stimulation compared with no intervention. 2 However, this finding was only significant among women who already had a favourable Bishop score (a cervical assessment used to predict the success of achieving a vaginal delivery). When breast stimulation was compared with intravenous oxytocin in the review, there was no difference in rates of cesarean delivery, number of women in labour at 72 hours or rates of meconium staining. However, the included studies did not look at time to vaginal delivery as an outcome. Overall, nipple stimulation seems to have minimal or no effect for women with an unripe cervix, but may be helpful for inducing labour in those with a ripe cervix. Few studies have looked at the role of intercourse as a cervical-ripening technique. However, prostaglandin concentrations have been shown to be 10 to 50 times higher in the cervical mucous of pregnant women two to four hours after intercourse, compared with concentrations before intercourse. 3 In a study of 47 women who had sex at term compared with 46 who abstained, there was no significant difference in Bishop scores. On average, the sexually active group delivered four days earlier, which was not considered clinically significant. -

Clinical Research of Effects of Retaining the Uterine Blood Supply Hysterectomy on Ovarian Function
BIO Web of Conferences 8 , 01038 (2017)DOI: 10.1051/bioconf/201 70801038 ICMSB2016 Clinical research of effects of retaining the uterine blood supply hysterectomy on ovarian function Yufei Cai 1 and Hongxia Sun 2,a 1Obstetrics and Gynecology Department,Affiliated Hospital of Beihua University 2 Pharmacological Department, Pharmacy, Beihua University jilin jilin 132011, China Abstract. Objective To evaluate the effect of hysterectomy for reserving the uterine blood supply on ovarian endocrine function and on symptoms of menopausal transition. Methods Uterine benign lesions should be line the uterus times total resection in 100 patients were randomly divided into hysterectomy group of retaining uterus vascular supply group(research group,n=50) and traditional total hysterectomy group (the control group, n=50), comparing two groups in operation time, intraoperative bleeding ,postoperative fever and residual polyp, blood tests were taken to check the serum sex hormone levels change and clinical observation for perimenopausal symptoms before and postoperative three months, six months, one year and two years at the same time respectively. Results There was no significant difference between two groups in operation time, intraoperative blood loss, postoperative fever and residual polyp (P>0.05). There was no significant difference among research group before and after operation in serum sex hormones(P>0.05),the symptoms of the menopausal transition hardly appear; postoperative FSH, LH increased significantly in control group (P<0.05),E2 decrease (P<0.05), perimenopausal symptoms appeared more often. Conclusion The effect of uterus hysterectomy for retaining vascular supply on ovarian endocrine function is less than the traditional total hysterectomy, this operation has a certain importance to preserve ovarian function and delay the occurrence of premature ovarian aging. -

Parts of the Body 1) Head – Caput, Capitus 2) Skull- Cranium Cephalic- Toward the Skull Caudal- Toward the Tail Rostral- Toward the Nose 3) Collum (Pl
BIO 3330 Advanced Human Cadaver Anatomy Instructor: Dr. Jeff Simpson Department of Biology Metropolitan State College of Denver 1 PARTS OF THE BODY 1) HEAD – CAPUT, CAPITUS 2) SKULL- CRANIUM CEPHALIC- TOWARD THE SKULL CAUDAL- TOWARD THE TAIL ROSTRAL- TOWARD THE NOSE 3) COLLUM (PL. COLLI), CERVIX 4) TRUNK- THORAX, CHEST 5) ABDOMEN- AREA BETWEEN THE DIAPHRAGM AND THE HIP BONES 6) PELVIS- AREA BETWEEN OS COXAS EXTREMITIES -UPPER 1) SHOULDER GIRDLE - SCAPULA, CLAVICLE 2) BRACHIUM - ARM 3) ANTEBRACHIUM -FOREARM 4) CUBITAL FOSSA 6) METACARPALS 7) PHALANGES 2 Lower Extremities Pelvis Os Coxae (2) Inominant Bones Sacrum Coccyx Terms of Position and Direction Anatomical Position Body Erect, head, eyes and toes facing forward. Limbs at side, palms facing forward Anterior-ventral Posterior-dorsal Superficial Deep Internal/external Vertical & horizontal- refer to the body in the standing position Lateral/ medial Superior/inferior Ipsilateral Contralateral Planes of the Body Median-cuts the body into left and right halves Sagittal- parallel to median Frontal (Coronal)- divides the body into front and back halves 3 Horizontal(transverse)- cuts the body into upper and lower portions Positions of the Body Proximal Distal Limbs Radial Ulnar Tibial Fibular Foot Dorsum Plantar Hallicus HAND Dorsum- back of hand Palmar (volar)- palm side Pollicus Index finger Middle finger Ring finger Pinky finger TERMS OF MOVEMENT 1) FLEXION: DECREASE ANGLE BETWEEN TWO BONES OF A JOINT 2) EXTENSION: INCREASE ANGLE BETWEEN TWO BONES OF A JOINT 3) ADDUCTION: TOWARDS MIDLINE -

CHAPTER 6 Perineum and True Pelvis
193 CHAPTER 6 Perineum and True Pelvis THE PELVIC REGION OF THE BODY Posterior Trunk of Internal Iliac--Its Iliolumbar, Lateral Sacral, and Superior Gluteal Branches WALLS OF THE PELVIC CAVITY Anterior Trunk of Internal Iliac--Its Umbilical, Posterior, Anterolateral, and Anterior Walls Obturator, Inferior Gluteal, Internal Pudendal, Inferior Wall--the Pelvic Diaphragm Middle Rectal, and Sex-Dependent Branches Levator Ani Sex-dependent Branches of Anterior Trunk -- Coccygeus (Ischiococcygeus) Inferior Vesical Artery in Males and Uterine Puborectalis (Considered by Some Persons to be a Artery in Females Third Part of Levator Ani) Anastomotic Connections of the Internal Iliac Another Hole in the Pelvic Diaphragm--the Greater Artery Sciatic Foramen VEINS OF THE PELVIC CAVITY PERINEUM Urogenital Triangle VENTRAL RAMI WITHIN THE PELVIC Contents of the Urogenital Triangle CAVITY Perineal Membrane Obturator Nerve Perineal Muscles Superior to the Perineal Sacral Plexus Membrane--Sphincter urethrae (Both Sexes), Other Branches of Sacral Ventral Rami Deep Transverse Perineus (Males), Sphincter Nerves to the Pelvic Diaphragm Urethrovaginalis (Females), Compressor Pudendal Nerve (for Muscles of Perineum and Most Urethrae (Females) of Its Skin) Genital Structures Opposed to the Inferior Surface Pelvic Splanchnic Nerves (Parasympathetic of the Perineal Membrane -- Crura of Phallus, Preganglionic From S3 and S4) Bulb of Penis (Males), Bulb of Vestibule Coccygeal Plexus (Females) Muscles Associated with the Crura and PELVIC PORTION OF THE SYMPATHETIC -

Leading Article Sexuality and Women with Complete Spinal Cord Injury
Spinal Cord (1997) 35, 136 ± 138 1997 International Medical Society of Paraplegia All rights reserved 1362 ± 4393/97 $12.00 Leading Article Sexuality and women with complete spinal cord injury Beverly Whipple1 and Barry R Komisaruk2 1College of Nursing Rutgers, The State University of New Jersey, 180 University Ave, Newark, NJ 07102; 2Psychology, Rutgers, The State University of NJ, 101 Warren Street, Newark, NJ 07102, USA Keywords: spinal cord injury; sexual aspects; women Introduction There is very little known about sexual response in brain.7 However, women who have been diagnosed as women with SCI.1 Although it is well documented that having `complete' SCI reported to us anecdotally that women with spinal cord injury (SCI) are able to they experience orgasms. menstruate, conceive and give birth,1 the literature This led us to hypothesize that in women with concerning orgasm in women with SCI is scant. complete SCI, there may still exist intact genital Money2 referred to orgasms that people with SCI sensory pathways from the peripheral sensory recep- reported during their dreams; he called these orgasms tors to the brain. This hypothesis is based on studies in `phantom'. The term `phantom orgasm' is still used in laboratory animals that demonstrate multiple sensory the literature and rehabilitation settings today. How- pathways from the genital system to dierent levels of ever, this term is misleading, because it confuses the spinal cord as well as directly to the brain. perception of orgasm, which is real, with the absent or denervated peripheral sensory receptor, which is Nerve Pathways `phantom'. For example, in the case of `phantom limb pain', the pain is real but the limb is `phantom'.