Scale up of Platelet Production from Human Pluripotent Stem Cells for Developing Targeted Therapies: Advances and Challenges
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Comments on August 1, 2018 Planning Commission Agenda Items, Received July 26-30
Comments on August 1, 2018 Planning Commission agenda items, received July 26-30 Items 1a/b, South Nashville Community Plan Amendment/Fairgrounds Mixed-Use District -----Original Message----- From: John Bernatavitz [mailto:[email protected]] Sent: Monday, July 30, 2018 10:30 AM To: Planning Commissioners Subject: Major League Soccer is what Nashville needs; so please support the proposed stadium! Dear Members of the Planning Commission, The 2018 World Cup said it all. What a great event! Nashville could also potentially share in the sport the binds the world together. I support the proposed Major League Soccer Stadium and renovation to the Fairgrounds Nashville. Professional sports teams in Nashville have turned into major brands that are recognized across their various leagues. The Predators not only hosted the NHL All Star weekend not long ago but are widely hailed as having the best home ice advantage in hockey. The Titans, on the heels of their incredible new uniform update ceremony, were selected to host next year's NFL draft at Ascend Amphitheater. Professional sports always have, and always will greatly benefit not only the neighborhoods where they play, but the city as a whole. I would ask that you seize this opportunity to make history with us and vote to approve this soccer stadium as well as the accompanying fairgrounds renovations. I recently went on a trip to Belize, and in the small village of Hopkins, Belize, I and my wife had the privilege of experiencing the World Cup final between Croatia and France with many people throughout the world in this village. -

U.S. Military Fatal Casualties of the Korean War for Home-State-Of-Record: New York
U.S. Military Fatal Casualties of the Korean War for Home-State-of-Record: New York Name Service Rank / Birthdate Home of Record: Incident or Remains Rate (YYYYMMDD) City County Death Date Recovered (YYYYMMDD) AARON GEORGE AIR FORCE CAPT 19170716 NEW YORK NEW YORK 19510412 Y ABLONDI BRUNO FRANK ARMY CPL 19270000 UNKNOWN ROCKLAND 19510602 Y ABRAHAMSEN HARALD ARMY PFC 19300000 NEW YORK KINGS 19521015 Y ACKERMANN WILLIAM C ARMY PVT 19300000 NEW YORK RICHMOND 19520416 Y ACKLEY EDWIN F ARMY PVT 19320000 UNKNOWN CHEMUNG 19501126 N ACOSTA PABLO MARINE CORPS PFC 19300307 NEW YORK BRONX 19521013 Y ADAMEC GEORGE E AIR FORCE 1STLT 19180131 BROADALBIN FULTON 19510105 Y ADAMO JOSEPH JOHN ARMY PFC 19310000 UNKNOWN NASSAU 19501130 N ADAMOWICZ WALTER J ARMY PFC 19330000 UNKNOWN STEUBEN 19510714 Y ADAMS HOLLIS J ARMY SGT 19310000 UNKNOWN TOMPKINS 19510914 Y ADAMS RAYMOND A ARMY CPL 19310000 UNKNOWN ONEIDA 19500901 Y ADAMS RONALD HUNTER ARMY PFC 19320329 UNKNOWN MADISON 19501102 N AGNELLI JUNIUS B JR ARMY PFC 19280000 UNKNOWN WESTCHESTER 19510519 Y AGOSTINI JORGE L ARMY PFC 19280000 NEW YORK KINGS 19510212 Y AGRAIT RICARDO A ARMY PFC 19290000 NEW YORK NEW YORK 19500921 Y AGUAYO RICHARD ARMY MSG 19230000 NEW YORK BRONX 19510407 Y AHLSTROM ERIC L JR ARMY PFC 19320000 NEW YORK RICHMOND 19530624 Y Source of data: the Korean War Extract Data File, as of April 29, 2008, of the Defense Casualty Analysis System (DCAS) Files, part of Record Group 330: Records of the Office of the Secretary of Defense. You can view the full DCAS record for an individual named in the list via the Access to Archival Databases resource, or AAD. -

Annual Report 2018
2018 Annual Report 4 A Message from the Chair 5 A Message from the Director & President 6 Remembering Keith L. Sachs 10 Collecting 16 Exhibiting & Conserving 22 Learning & Interpreting 26 Connecting & Collaborating 30 Building 34 Supporting 38 Volunteering & Staffing 42 Report of the Chief Financial Officer Front cover: The Philadelphia Assembled exhibition joined art and civic engagement. Initiated by artist Jeanne van Heeswijk and shaped by hundreds of collaborators, it told a story of radical community building and active resistance; this spread, clockwise from top left: 6 Keith L. Sachs (photograph by Elizabeth Leitzell); Blocks, Strips, Strings, and Half Squares, 2005, by Mary Lee Bendolph (Purchased with the Phoebe W. Haas fund for Costume and Textiles, and gift of the Souls Grown Deep Foundation from the William S. Arnett Collection, 2017-229-23); Delphi Art Club students at Traction Company; Rubens Peale’s From Nature in the Garden (1856) was among the works displayed at the 2018 Philadelphia Antiques and Art Show; the North Vaulted Walkway will open in spring 2019 (architectural rendering by Gehry Partners, LLP and KXL); back cover: Schleissheim (detail), 1881, by J. Frank Currier (Purchased with funds contributed by Dr. Salvatore 10 22 M. Valenti, 2017-151-1) 30 34 A Message from the Chair A Message from the As I observe the progress of our Core Project, I am keenly aware of the enormity of the undertaking and its importance to the Museum’s future. Director & President It will be transformative. It will not only expand our exhibition space, but also enhance our opportunities for community outreach. -

State of New Jersey Medicaid Fraud Division Provider Exclusion Report
State of New Jersey 1 Medicaid Fraud Division Provider Exclusion Report Updated on: 8/23/2021 **ADDITIONAL NPI NUMBERS MAY BE ASSOCIATED WITH THE LISTED INDIVIDUALS/ENTITIES** PROVIDER NAME TITLE DATE OF NPI NUMBER STREET CITY STA ZIP ACTION EFFECTIVE EXPIRATION BIRTH TE DATE DATE 2258 PHARMACY, INC. 2258 THIRD AVENUE NEW YORK NY 10035 SUSPENSION 7/20/2003 6522 VENTNOR AVE. 6522 VENTNOR AVENUE VENTNOR NJ 08406 DISQUALIFICATION PHARMACY, INC. ABARCA, CHERYL R. LPN 8/15/1962 528 3RD STREET NEWARK NJ 07107 SUSPENSION 6/20/2005 ABASHKIN, ROMAN CHHA 12/21/1981 72 RIDGEVIEW TERRACE WAYNE NJ 07470 DISQUALIFICATION 5/29/2015 ABASHKIN, ROMAN CHHA 12/21/1981 72 RIDGEVIEW TERRACE WAYNE NJ 07470 DISQUALIFICATION 6/3/2016 ABBASSI, JADAN MD 9/19/1944 1194807255 1618 MAIN AVENUE CLIFTON NJ 07011 DISQUALIFICATION 11/21/2016 PERMANENT ABBASSI, JADAN MD 9/19/1944 1194807255 115 NELLIS DRIVE WAYNE NJ 07470 DISQUALIFICATION 6/20/2018 PERMANENT ABDALLA, IZZELDIN 4/5/1967 1116 ANNE STREET ELIZABETH NJ 07201 DISQUALIFICATION 11/10/1999 ABDELGANI, AMIR ALLENWOOD USP WHITE DEER PA 17887 DISQUALIFICATION 11/26/2001 ABDELGANI, FADIL TERRE HAUTE USP TERRE HAUTE IN 47808 DISQUALIFICATION 11/26/2001 ABDELHAMID, MANAL RPH 5/28/1969 7100 BOULEVARD EAST, 11G GUTTENBERG NJ 07093 DEBARMENT 3/15/2001 ABDOLLAHI, MITRA DMD 8/31/1966 1033329230 646 N. SARATOGA DRIVE MOORESTOWN NJ 08057 DISQUALIFICATION 11/5/2007 7/19/2019 ABERBACH, STEVEN RPH 8/5/1944 23 STONEGATE DRIVE WATCHUNG NJ 07069 DEBARMENT 12/19/2003 ABOOD, ABDOLMAID S. 1/20/1966 64 BEVAN STREET JERSEY CITY NJ 07306 SUSPENSION 5/7/1997 ABOODS MEDICAL LIVERY 64 BEVAN STREET JERSEY CITY NJ 07306 DISQUALIFICATION 5/22/1994 ABOUELHODA, AHMED RPH 3/23/1974 33-17 60TH STREET, APT. -

US 2017/0020926 A1 Mata-Fink Et Al
US 20170020926A1 (19) United States (12) Patent Application Publication (10) Pub. No.: US 2017/0020926 A1 Mata-Fink et al. (43) Pub. Date: Jan. 26, 2017 (54) METHODS AND COMPOSITIONS FOR 62/006,825, filed on Jun. 2, 2014, provisional appli MMUNOMODULATION cation No. 62/006,829, filed on Jun. 2, 2014, provi sional application No. 62/006,832, filed on Jun. 2, (71) Applicant: RUBIUS THERAPEUTICS, INC., 2014, provisional application No. 61/991.319, filed Cambridge, MA (US) on May 9, 2014, provisional application No. 61/973, 764, filed on Apr. 1, 2014, provisional application No. (72) Inventors: Jordi Mata-Fink, Somerville, MA 61/973,763, filed on Apr. 1, 2014. (US); John Round, Cambridge, MA (US); Noubar B. Afeyan, Lexington, (30) Foreign Application Priority Data MA (US); Avak Kahvejian, Arlington, MA (US) Nov. 12, 2014 (US) ................. PCT/US2O14/0653O4 (21) Appl. No.: 15/301,046 Publication Classification (22) PCT Fed: Mar. 13, 2015 (51) Int. Cl. A6II 35/28 (2006.01) (86) PCT No.: PCT/US2O15/02O614 CI2N 5/078 (2006.01) (52) U.S. Cl. S 371 (c)(1), CPC ............. A61K 35/28 (2013.01); C12N5/0641 (2) Date: Sep. 30, 2016 (2013.01): CI2N 5/0644 (2013.01); A61 K Related U.S. Application Data 2035/122 (2013.01) (60) Provisional application No. 62/059,100, filed on Oct. (57) ABSTRACT 2, 2014, provisional application No. 62/025,367, filed on Jul. 16, 2014, provisional application No. 62/006, Provided are cells containing exogenous antigen and uses 828, filed on Jun. 2, 2014, provisional application No. -

San Diego County Treasurer-Tax Collector 2019-2020 Returned Property Tax Bills
SAN DIEGO COUNTY TREASURER-TAX COLLECTOR 2019-2020 RETURNED PROPERTY TAX BILLS TO SEARCH, PRESS "CTRL + F" CLICK HERE TO CHANGE MAILING ADDRESS PARCEL/BILL OWNER NAME 8579002100 11-11 GIFT TRUST 04-01-96 8579002104 11-11 GIFT TRUST 04-01-96 8579002112 11-11 GIFT TRUST 04-01-96 8679002101 11-11 GIFT TRUST 04-01-96 8679002105 11-11 GIFT TRUST 04-01-96 8679002113 11-11 GIFT TRUST 04-01-96 8779002102 11-11 GIFT TRUST 04-01-96 8779002106 11-11 GIFT TRUST 04-01-96 8779002114 11-11 GIFT TRUST 04-01-96 8879002103 11-11 GIFT TRUST 04-01-96 8879002107 11-11 GIFT TRUST 04-01-96 8879002115 11-11 GIFT TRUST 04-01-96 5331250200 1141 LAGUNA AVE L L C 2224832400 1201 VIA RAFAEL LTD 3172710300 12150 FLINT PLACE LLC 2350405100 1282 PACIFIC OAKS LLC 4891237400 1360 E MADISON AVENUE L L C 1780235100 138 SUN VILLA CT LLC 8894504458 138 SUN VILLA CT LLC 2222400700 1488 SAN PABLO L L C 1300500500 15195 HWY 76 TRUST 04-084 1473500900 152 S MYERS LLC 4230941300 1550 GARNET LLC 2754610900 15632 POMERADO ROAD L L C 1678 COUNTRY CLUB DR ESCONDIDO CA 92029 TRUST 05-07- 2325114700 18 1678 COUNTRY CLUB DR ESCONDIDO CA 92029 TRUST 05-07- 8894616148 18 2542212300 1697A LA COSTA MEADOWS L L C 2542212400 1697A LA COSTA MEADOWS L L C 6461901900 1704 CACTUS ROAD LLC 5333021200 1750 FIFTH AVENUE L L C 2542304001 180 PHOEBE STREET LLC 5392130600 1815-19 GRANADA AVENUE LLC 5392130700 1815-19 GRANADA AVENUE LLC 2643515400 18503 CALLE LA SERRA L L C 2263601300 1991 TRUST 12-02-91 AND W J K FAMILY LTD PARTNERSHIP 5650321400 1998 ENG FAMILY L L C 5683522300 1998 ENG FAMILY L L -

Genome Editing: Scientific Opportunities, Public Interests and Policy Options in the European Union
ea sac Genome editing: scientific opportunities, public interests and policy options in the European Union EASAC policy report 31 March 2017 ISBN: 978-3-8047-3727-3 This report can be found at www.easac.eu Science Advice for the Benefit of Europe EASAC EASAC – the European Academies' Science Advisory Council – is formed by the national science academies of the EU Member States to enable them to collaborate with each other in giving advice to European policy-makers. It thus provides a means for the collective voice of European science to be heard. EASAC was founded in 2001 at the Royal Swedish Academy of Sciences. Its mission reflects the view of academies that science is central to many aspects of modern life and that an appreciation of the scientific dimension is a pre-requisite to wise policy-making. This view already underpins the work of many academies at national level. With the growing importance of the European Union as an arena for policy, academies recognise that the scope of their advisory functions needs to extend beyond the national to cover also the European level. Here it is often the case that a trans-European grouping can be more effective than a body from a single country. The academies of Europe have therefore formed EASAC so that they can speak with a common voice with the goal of building science into policy at EU level. Through EASAC, the academies work together to provide independent, expert, evidence-based advice about the scientific aspects of public policy to those who make or influence policy within the European institutions. -
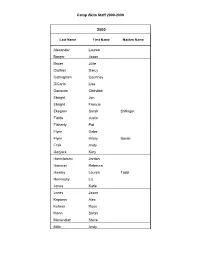
2000-2009 List.Xlsx
Camp Akita Staff 2000-2009 2000 Last Name First Name Maiden Name Alexander Lauren Barger Jason Bauer Julie Clothier Darcy Cottingham Courtney DiCarlo Lisa Donovan Christian Ebright Jon Ebright Francie Ekegren Sarah Stillinger Fields Justin Flaherty Pat Flynn Gabe Flynn Hilary Bosler Frick Andy Gozjack Kory Hanhilammi Jordan Hanscel Rebecca Hawley Lauren Todd Hennessy Liz Jones Katie Jones Jason Kaparos Alex Kuhner Russ Mann Sarah Menendian Steve Mills Andy Camp Akita Staff 2000-2009 Moore Heidi Nicoll Ryan Steele Nicoll Scot Noone Kim Ottney Andy Page Carissa Patterson Karen Franklin Poe Adam Popa JW Porterfield Jodi Lee Rankin Molly Revelle Chuck Rohrer Katie Ross John Schlacter Daniel Smith Ben Smith Jenny Smith Shawn Spurbeck Stephanie Starr Krissy Talmage Scott Trainer Amy Tutt Nathanial Wilkinson PJ Wing Bria Camp Akita Staff 2000-2009 2001 Last Name First Name Maiden Name Albert Katie Bain Austin Barger Jason Bedell Ashley Benes Livvy Bernard John Brownfield Ryan Burke Megan Cottingham Courtney Creech Steve Davidson Joel Dixon Liz Ebright Jon Falkenberg Katie Fields Justin Fleishman Amy Flynn Gabe Flynn Hilary Bosler Franklin Julie Gozjack Kory Hanhilammi Jordan Hawley Lauren Todd Irene Jessi Jones Jason Jones Kyle Kidwell Tabitha Kinsey Connor Camp Akita Staff 2000-2009 Laubenthal Amanda Yant Marshall Vanessa McGauvren Heather Menendian Steve Mulgrew Brent Nicoll Scot Noone Kim Oberle Katy Sebastian Poe Adam Pond Ashley Popovich Katie Porter Sam Porter, III Samuel Porterfield Jodi Lee Rankin Tom Rohrer Katie Ross John Smith Ben -

Human Platelet Lysate As a Functional Substitute for Fetal Bovine Serum in the Culture of Human Adipose Derived Stromal/Stem Cells
Brief Report Human Platelet Lysate as a Functional Substitute for Fetal Bovine Serum in the Culture of Human Adipose Derived Stromal/Stem Cells Mathew Cowper 1,†, Trivia Frazier 1,2,3, Xiying Wu 2,3, Lowry Curley 2,4, Michelle H. Ma 3, Omair A. Mohuiddin 1, Marilyn Dietrich 5, Michelle McCarthy 1, Joanna Bukowska 1,6 and Jeffrey M. Gimble 1,2,3,* 1 School of Medicine, Tulane University, New Orleans, LA 70112, USA 2 LaCell LLC, New Orleans, LA 70148, USA 3 Obatala Sciences Inc., New Orleans, LA 70148, USA 4 Axosim Sciences Inc., New Orleans, LA 70803, USA 5 Louisiana State University School of Veterinary Medicine, Baton Rouge, LA 70803, USA 6 Institute for Animal Reproduction and Food Research, Polish Academy of Science, 10-748 Olsztyn, Poland * Correspondence: [email protected]; Tel.: 1-(504)-300-0266 † Current Affiliations: Department of Urology, Bowman Gray School of Medicine, Wake Forest University, Winston Salem, NC 27101, USA. Received: 15 May 2019; Accepted: 9 July 2019; Published: 15 July 2019 Abstract: Introduction: Adipose derived stromal/stem cells (ASCs) hold potential as cell therapeutics for a wide range of disease states; however, many expansion protocols rely on the use of fetal bovine serum (FBS) as a cell culture nutrient supplement. The current study explores the substitution of lysates from expired human platelets (HPLs) as an FBS substitute. Methods: Expired human platelets from an authorized blood center were lysed by freeze/thawing and used to examine human ASCs with respect to proliferation using hematocytometer cell counts, colony forming unit- fibroblast (CFU-F) frequency, surface immunophenotype by flow cytometry, and tri-lineage (adipocyte, chondrocyte, osteoblast) differentiation potential by histochemical staining. -

Review Article the Roles of Platelets in Inflammation, Immunity, Wound Healing and Malignancy
Int J Clin Exp Med 2016;9(3):5347-5358 www.ijcem.com /ISSN:1940-5901/IJCEM0021296 Review Article The roles of platelets in inflammation, immunity, wound healing and malignancy Ymer H Mekaj1,2 1Institute of Pathophysiology, Faculty of Medicine, University of Prishtina, Prishtina, Kosovo; 2Department of Hemostasis and Thrombosis, National Blood Transfusion Center of Kosovo, Prishtina, Kosovo Received December 6, 2015; Accepted March 10, 2016; Epub March 15, 2016; Published March 30, 2016 Abstract: The roles of platelets as essential effector cells in hemostasis have been known for over a century. Platelets also have many other functions, which are facilitated by their complex morphological structures and their ability to synthesize and store a variety of biochemical substances. These substances are released via the platelet release re- action in response to tissue/cell damage. The aim of the current study was to review the reported functions of plate- lets in inflammation, immunity, wound healing and malignancy. For this purpose, we used relevant data from the latest numerous scientific studies, including review articles, and original research articles. Platelets physiologically respond to inflammation by recruiting inflammatory cells to repair and resolve injuries. This response is facilitated by the ability of platelets to promote vascular permeability under inflammatory conditions. Platelets have critical roles in innate and adaptive immune responses and extensively interact with endothelial cells, various pathogens, and almost all known immune cell types, including neutrophils, monocytes, macrophages and lymphocytes. Additionally, platelets affect wound healing by integrating complex cascades between their mediators, which include multiple cytokines, transforming growth factors, platelet growth factors, and vascular endothelial growth factors, among oth- ers. -

The Expanding Horizons in Thrombosis and Hemostasis
The Expanding Horizons in Thrombosis and Hemostasis Vivian Xiaoyan Du The Expanding Horizons in Thrombosis and Hemostasis Thesis University Utrecht ISBN: 978-90-8891-881-0 Cover design: Andrea Almering Layout: Vivian X. Du Printing: Uitgeverij BOXPress Copy right © X.Du, Utrecht 2014 The Expanding Horizons in Thrombosis and Hemostasis De Uitbreiding van de Horizon van Trombose en Hemostase (met een samenvatting in het Nederlands) 血栓与凝血新进展 (含中文概要) Proefschrift ter verkrijging van de graad van doctor aan de Universiteit Utrecht op gezag van de rector magnificus, prof. dr. G. J. van der Zwaan, ingevolge het besluit van het collage voor promoties in het openbaar te verdedigen op maandag 16 juni 2014 des middags te 2.30 uur door Xiaoyan Du geboren op 23 september 1980 te Dongping county, China Promotor: Prof. dr. Ph. G. de Groot Co-promotor: Dr. B. de Laat The studies described in this thesis were supported by a grant from Sanquin Blood Supply awarded to Dr. Bas de Laat . Financial support by the Netherlands Heart Foundation for the publication of this thesis is gratefully acknowledged. Financial support by Synapse B.V. and Phenom-World for publication of this thesis is gratefully acknowledged. Additional financial support by Stago BNL, CASLO ApS, Bayer B.V. and ChipSoft B.V. is gratefully acknowledged. “As far as we can discern, the sole purpose of human existence is to kindle a light in the darkness of mere being.” Carl Jung To Iwan My father Pa en Ma Fernhout Dear Uncle and Aunt Du Beoordelingscommissie: prof. dr. J. A. G. van Strijp prof. -

Would Like to Wish You a Warm Welcome to the 2016-2017
ADDRESSING THE NEEDS OF OUR STUDENTS & PLANTING THE SEEDS FOR A SECURE FUTURE . I believe 2016-2017 is going to be a As always, you are would like to wish you a great year for EOF. We started with our and all warm welcome to the a newly revamped office that is con- our services and support 2016-2017 academic year. ducive of a welcoming academic envi- are only here to see you So far, we are off to a ronment with new furniture and up- all succeed, graduate great start and we are dated computers, which we hope will and transfer to a four seeing many of you al- help in your academic endeavors. We year institution or go out ready coming in and out have prepared a variety of activities into the workforce. Remember through- of the office and getting and workshops throughout the Fall to out the term to stay connected, meet nicely settled. First, I would make sure you stay on top of your with your counselor regularly, ask like to congratulate all of you studies, while building new skills that questions, get tutoring, and keep up who completed summer will contribute to your success here with your assignments. Make a good courses with such superior at CCM. Additionally, you will have impression with your professors, chat grades. You definitely gave opportunities to partake in through- with them during office hours and do your GPA a boost, and got moving in out the term and become involved not wait until things get too difficult the right direction.