Childcare Exclusion List
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Roseola Fact Sheet
Sixth Disease/ Exanthem Subitum DISTRICT OF COLUMBIA DEPARTMENT OF HEALTH Division of Epidemiology, Disease Surveillance and Investigation 899 N. Capitol Street, NE, Suite 580 Washington, D.C. 20002 202-442-9371 Fax 202-442-8060 * www.dchealth.dc.gov What is Roseola? medications. Frequent hand washing may Roseola is an acute, febrile rash illness caused by a limit transmission (spread). Women who are virus. pregnant and have been exposed to this illness should discuss the exposure with Who gets Fifth Disease? their doctor. Roseola occurs in children usually under four years of age. It is most common in children under the age Should a child with Roseola be excluded of two. from Child-care? Yes, a child with fever and rash should be What are the symptoms of Roseola? excluded from child-care until seen by a The symptoms of roseola include a high fever that health-care provider. The child may return lasts for three to five days. A runny nose, irritability, to child-care once the fever has gone, even if eyelid swelling, and tiredness may also be present. the rash is present. When the fever disappears, a rash appears, mainly on the face and body. How can Roseola be prevented? There is no vaccine or medicine that How is Roseola spread? prevents roseola. Frequent and thorough Roseola is spread from person to person but the hand washing is recommended as a practical exact way is not known. It appears that saliva may be and effective method of preventing most an important way for the spread of the virus. -

Communicable Disease Chart
COMMON INFECTIOUS ILLNESSES From birth to age 18 Disease, illness or organism Incubation period How is it spread? When is a child most contagious? When can a child return to the Report to county How to prevent spreading infection (management of conditions)*** (How long after childcare center or school? health department* contact does illness develop?) To prevent the spread of organisms associated with common infections, practice frequent hand hygiene, cover mouth and nose when coughing and sneezing, and stay up to date with immunizations. Bronchiolitis, bronchitis, Variable Contact with droplets from nose, eyes or Variable, often from the day before No restriction unless child has fever, NO common cold, croup, mouth of infected person; some viruses can symptoms begin to 5 days after onset or is too uncomfortable, fatigued ear infection, pneumonia, live on surfaces (toys, tissues, doorknobs) or ill to participate in activities sinus infection and most for several hours (center unable to accommodate sore throats (respiratory diseases child’s increased need for comfort caused by many different viruses and rest) and occasionally bacteria) Cold sore 2 days to 2 weeks Direct contact with infected lesions or oral While lesions are present When active lesions are no longer NO Avoid kissing and sharing drinks or utensils. (Herpes simplex virus) secretions (drooling, kissing, thumb sucking) present in children who do not have control of oral secretions (drooling); no exclusions for other children Conjunctivitis Variable, usually 24 to Highly contagious; -

Clinical Impact of Primary Infection with Roseoloviruses
Available online at www.sciencedirect.com ScienceDirect Clinical impact of primary infection with roseoloviruses 1 2 1 Brenda L Tesini , Leon G Epstein and Mary T Caserta The roseoloviruses, human herpesvirus-6A -6B and -7 (HHV- infection in different cell types, have the ability to reac- 6A, HHV-6B and HHV-7) cause acute infection, establish tivate, and may be intermittently shed in bodily fluids [3]. latency, and in the case of HHV-6A and HHV-6B, whole virus Unlike other human herpesviruses, HHV-6A and HHV- can integrate into the host chromosome. Primary infection with 6B are also found integrated into the host genome HHV-6B occurs in nearly all children and was first linked to the (ciHHV-6). Integration has been documented in 0.2– clinical syndrome roseola infantum. However, roseolovirus 1% of the general population and along with latency infection results in a spectrum of clinical disease, ranging from has confounded the ability to correlate the presence of asymptomatic infection to acute febrile illnesses with severe viral nucleic acid with active disease [4]. neurologic complications and accounts for a significant portion of healthcare utilization by young children. Recent advances The syndrome known as roseola infantum was reported as have underscored the association of HHV-6B and HHV-7 early as 1809 by Robert Willan in his textbook ‘On primary infection with febrile status epilepticus as well as the cutaneous diseases’ [5]. This clinical entity is also com- role of reactivation of latent infection in encephalitis following monly referred to as exanthem subitum and early pub- cord blood stem cell transplantation. -

Measles Diagnostic Tool
Measles Prodrome and Clinical evolution E Fever (mild to moderate) E Cough E Coryza E Conjunctivitis E Fever spikes as high as 105ºF Koplik’s spots Koplik’s Spots E E Viral enanthem of measles Rash E Erythematous, maculopapular rash which begins on typically starting 1-2 days before the face (often at hairline and behind ears) then spreads to neck/ the rash. Appearance is similar to “grains of salt on a wet background” upper trunk and then to lower trunk and extremities. Evolution and may become less visible as the of rash 1-3 days. Palms and soles rarely involved. maculopapular rash develops. Rash INCUBATION PERIOD Fever, STARTS on face (hairline & cough/coryza/conjunctivitis behind ears), spreads to trunk, Average 8-12 days from exposure to onset (sensitivity to light) and then to thighs/ feet of prodrome symptoms 0 (average interval between exposure to onset rash 14 day [range 7-21 days]) -4 -3 -2 -1 1234 NOT INFECTIOUS higher fever (103°-104°) during this period rash fades in same sequence it appears INFECTIOUS 4 days before rash and 4 days after rash Not Measles Rubella Varicella cervical lymphadenopathy. Highly variable but (Aka German Measles) (Aka Chickenpox) Rash E often maculopapular with Clinical manifestations E Clinical manifestations E Generally mild illness with low- Mild prodrome of fever and malaise multiforme-like lesions and grade fever, malaise, and lymph- may occur one to two days before may resemble scarlet fever. adenopathy (commonly post- rash. Possible low-grade fever. Rash often associated with painful edema hands and feet. auricular and sub-occipital). -
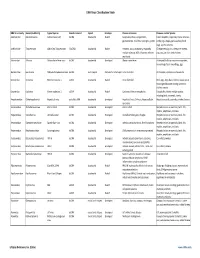
Virus Classification Tables V2.Vd.Xlsx
DNA Virus Classification Table DNA Virus Family Genera (Subfamily) Typical Species Genetic material Capsid Envelope Disease in Humans Diseases in other Species Adenoviridae Mastadenovirus Adenoviruses 1‐47 dsDNA Icosahedral Naked Respiratory illness; conjunctivitis, Canine hepatitis, respiratory illness in horses, gastroenteritis, tonsillitis, meningitis, cystitis cattle, pigs, sheep, goats, sea lions, birds dogs, squirrel enteritis Anelloviridae Torqueviruses Alpha‐Zeta Torqueviruses (‐)ssDNA Icosahedral Naked Hepatitis, lupus, pulmonary, myopathy, Chimpanzee, pig, cow, sheep, tree shrews, multiple sclerosis; 90% of humans infected pigs, cats, sea lions and chickens worldwide Asfarviridae Asfivirus African Swine fever virus dsDNA Icosahedral Enveloped African swine fever Arthropod (tick) transmission or ingestion; hemorrhagic fever in warthogs, pigs Baculoviridae Baculovirus Alpha‐Gamma Baculoviruses dsDNA Stick shaped Occluded or Enveloped none identified Arthropods, Lepidoptera, crustaceans Circoviridae Circovirus Porcine circovirus 1 ssDNA Icosahedral Naked none identified Birds, pigs, dogs; bats; rodents; causes post‐ weaning multisystem wasting syndrome, chicken anemia Circoviridae Cyclovirus Human cyclovirus 1 ssDNA Icosahedral Naked Cyclovirus Vietnam encephalitis Encephalitis; infects multiple species including birds, mammals, insects Hepadnaviridae Orthohepadnavirus Hepatitis B virus partially ssDNA Icosahedral Enveloped Hepatitis B virus; Cirrhosis, Hepatocellular Hepatitis in ducks, squirrels, primates, herons carcinoma Herpesviridae -

Fundamentals of Dermatology Describing Rashes and Lesions
Dermatology for the Non-Dermatologist May 30 – June 3, 2018 - 1 - Fundamentals of Dermatology Describing Rashes and Lesions History remains ESSENTIAL to establish diagnosis – duration, treatments, prior history of skin conditions, drug use, systemic illness, etc., etc. Historical characteristics of lesions and rashes are also key elements of the description. Painful vs. painless? Pruritic? Burning sensation? Key descriptive elements – 1- definition and morphology of the lesion, 2- location and the extent of the disease. DEFINITIONS: Atrophy: Thinning of the epidermis and/or dermis causing a shiny appearance or fine wrinkling and/or depression of the skin (common causes: steroids, sudden weight gain, “stretch marks”) Bulla: Circumscribed superficial collection of fluid below or within the epidermis > 5mm (if <5mm vesicle), may be formed by the coalescence of vesicles (blister) Burrow: A linear, “threadlike” elevation of the skin, typically a few millimeters long. (scabies) Comedo: A plugged sebaceous follicle, such as closed (whitehead) & open comedones (blackhead) in acne Crust: Dried residue of serum, blood or pus (scab) Cyst: A circumscribed, usually slightly compressible, round, walled lesion, below the epidermis, may be filled with fluid or semi-solid material (sebaceous cyst, cystic acne) Dermatitis: nonspecific term for inflammation of the skin (many possible causes); may be a specific condition, e.g. atopic dermatitis Eczema: a generic term for acute or chronic inflammatory conditions of the skin. Typically appears erythematous, -

Childhood Diseases and Potential Risks During Pregnancy: (All Information Available on the March of Dimes Web Site.)
Childhood Diseases and potential risks during pregnancy: (All information available on the March of Dimes Web Site.) http://www.modimes.org/ Fifth disease (erythema infectiosum) is a common, mild, childhood illness caused by parvovirus B19. It causes a “slapped-cheek” rash on the face and, less commonly, fever, headache, sore throat and joint pain in children. Infected adults often have joint pain and swelling, and sometimes mild flu-like symptoms, but usually no rash. Women with young children and those who work with them (for example, child care providers and teachers) are at greatest risk of exposure and infection. About 60 percent of adults have had the infection as children and, therefore, are immune as adults. Most unborn babies are unaffected if their mother gets infected. Some unborn babies, however, do become infected. The virus can disrupt the ability to produce red blood cells, leading to a dangerous form of anemia, heart failure and, in about 2-9 percent of fetal infections, death of the unborn child. What you can do: If you are pregnant and unsure of your immune status, you can help protect yourself from infection by: * Washing your hands thoroughly and often, especially after touching tissues used by children who might be infected * Not sharing drinking glasses and utensils with any one who has or was exposed to the illness If you think you have been exposed to fifth disease, call your health care provider right away. Chickenpox (varicella) is a viral illness that mainly affects children. Its symptoms include an itchy rash and fever. Between 85 and 95 percent of pregnant women are immune to chickenpox, meaning that they cannot catch it. -

Infectious Disease in Childcare Settings Manual
INFECTIOUS DISEASES IN CHILDCARE SETTINGS Informational Guidelines for Directors, Caregivers, and Parents Third Edition July 2013 Department of Health and Social Services Delaware Division of Public Health Office of Infectious Disease Epidemiology Thomas Collins Building 540 S. DuPont Highway Dover, Delaware 19901 302-744-1033 888-295-5156 Childcare Manual Table of Contents Page About this book 5 Chapter 1 Introduction: Keeping Children Healthy 6 Chapter 2 Health History and Immunizations for Children 7-8 Health History and Immunizations for Caregivers 9 Immunization Schedule 10 Things You Need to Know about Immunizations 11-12 Chapter 3 Infection Overview: 13-14 Infection Spread by Direct Contact with People or Objects Infection Spread by the Fecal-Oral Route Infection Spread by the Respiratory Route Infection Spread through Blood, Urine, and Saliva Chapter 4 Infection Control Measures: Sanitation and Disinfection 15 Washing and Disinfecting Bathrooms and other Surfaces 16 Washing and Disinfecting Diaper Changing Areas 16 Washing Potty Chairs and Toilets 16-17 Washing and Disinfecting Clothing, Linen and Furnishings 17 Washing and Disinfecting Toys 17-18 Cleaning up Body Fluids 18 Handwashing 19-21 Hand Washing Steps and Diagram 21 Diaper Changing Steps 22-23 Food Safety and Sanitation 24-25 Breast Milk and Infectious Disease Exposure 26 Proper Handling and Storage of Breast Milk 27 Pets in the Childcare Setting 28-29 Chapter 5 Health of Childcare Providers Health Appraisals 30 Health Limitations of Staff 30 Health Risks for Pregnant -

Pathogenic Viruses Commonly Present in the Oral Cavity and Relevant Antiviral Compounds Derived from Natural Products
medicines Review Pathogenic Viruses Commonly Present in the Oral Cavity and Relevant Antiviral Compounds Derived from Natural Products Daisuke Asai and Hideki Nakashima * Department of Microbiology, St. Marianna University School of Medicine, Kawasaki 216-8511, Japan * Correspondence: [email protected]; Tel.: +81-44-977-8111 Received: 24 October 2018; Accepted: 7 November 2018; Published: 12 November 2018 Abstract: Many viruses, such as human herpesviruses, may be present in the human oral cavity, but most are usually asymptomatic. However, if individuals become immunocompromised by age, illness, or as a side effect of therapy, these dormant viruses can be activated and produce a variety of pathological changes in the oral mucosa. Unfortunately, available treatments for viral infectious diseases are limited, because (1) there are diseases for which no treatment is available; (2) drug-resistant strains of virus may appear; (3) incomplete eradication of virus may lead to recurrence. Rational design strategies are widely used to optimize the potency and selectivity of drug candidates, but discovery of leads for new antiviral agents, especially leads with novel structures, still relies mostly on large-scale screening programs, and many hits are found among natural products, such as extracts of marine sponges, sea algae, plants, and arthropods. Here, we review representative viruses found in the human oral cavity and their effects, together with relevant antiviral compounds derived from natural products. We also highlight some recent emerging pharmaceutical technologies with potential to deliver antivirals more effectively for disease prevention and therapy. Keywords: anti-human immunodeficiency virus (HIV); antiviral; natural product; human virus 1. Introduction The human oral cavity is home to a rich microbial flora, including bacteria, fungi, and viruses. -

Guidelines for Schools and Child Care Centres on Communicable
Guidelines for Schools and Child Care Centres on Communicable Diseases and Other Childhood Health Issues This resource is intended to provide school principals, teachers, directors of child care centres (CCCs) and health care professionals with guidelines on communicable disease prevention and control in schools and CCCs. Any child who is ill and unable to participate fully in regular activities should be cared for at home. Ottawa Public Health recommends that individuals who may have been exposed to a communicable disease and have specific health concerns, such as pregnancy and immunosuppression, be assessed by a health care professional. Proper hand hygiene is the most effective way to prevent the spread of communicable diseases. May 2017 CRITERIA FOR REPORTING OUTBREAKS TO OTTAWA PUBLIC HEALTH For reporting of gastroenteritis outbreaks, see page 5. For reporting of respiratory infection outbreaks, see page 11. Schools must report when they have greater than 10% absenteeism due to similar symptoms in the school on the same day OR a sudden or unusual increase in absenteeism due to similar symptoms in students/staff in a class or school on the same day. Child care centres must report when they have 10% or more children/staff ill with similar symptoms or absent on the same day. Report all outbreaks immediately to the Outbreak Reporting Line at 613-580-6744, ext 26325, Monday to Friday 8:30 a.m. to 4:30 p.m. or 3-1-1 after hours. 1 Period of Reporting Disease Cause/Symptoms Transmission Incubation Exclusion Communicability Requirements Amebiasis Parasite. Fecal-oral route. Few days to several During the period that CCCs: exclude Report to 613-580-6744, Abdominal distension, Food and water months to years, most cysts are passed, which symptomatic cases ext. -

Fifth Disease (Erythema Infectiosum) Fact Sheet
Fifth Disease (Erythema Infectiosum) Fact Sheet Fifth disease is a mild rash illness It is caused by a human virus called parvovirus B19 and primarily affects school age children. Many people already have had fifth disease Most people get infected between 5 and 14 years of age. It is estimated that about half the adults in the United States have been infected with parvovirus B19 and therefore can not get it again. A red, patchy, "slapped cheek" rash on the face is common during infection The rash may appear on other parts of the body (such as the arms, trunk, buttocks, and thighs). Other symptoms such as fever, headache, body ache, sore throat, congestion, runny nose, cough, nausea, or diarrhea may come before the rash. In adults, joint pains or arthritis may occur. Symptoms usually start 4 to 20 days after a person has been exposed. About 25% of all cases have no symptoms. In both children and adults, the disease is usually mild and recovery occurs without problems. A person with fifth disease usually spreads the virus before the rash starts The virus is spread by exposure to airborne droplets from the nose and throat of infected people. The virus can also be transmitted by blood or blood products. There is a blood test, but it is not widely available A blood test for antibodies is used to see if a person is currently infected or was infected in the past. The blood test is used primarily for pregnant women exposed to fifth disease. In most cases, the disease is diagnosed based on the appearance of a typical rash. -

Communicable Disease Guide
Introduction This guide was developed by the Illinois Department of Public Health (IDPH) to furnish school officials, health care providers and other interested persons with information on the control of communicable diseases. It provides information on 48 common reportable and non-reportable communicable diseases and conditions. More detailed information on many of these diseases can be obtained from the IDPH Web site (www.idph.state.il.us) or from the Web site of the U.S. Centers for Disease Control and Prevention (CDC) (www.cdc.gov). Both sites have a topics listing that affords easy access to communicable disease-related information. Those diseases or conditions marked with an asterisk must be reported to a local health department or to IDPH. Time frames for reporting to the health authority are designated for each reportable disease. Prompt reporting to the local health authority of all cases of communicable diseases can greatly reduce opportunities for these diseases to be spread. Information related to exclusion from day care and school attendance is noted in bold in the “Control of Case” and “Contact” sections under each disease. For more information, refer to the following IDPH rules and regulations: Control of Communicable Diseases (77 Ill. Adm. Code 690) Child Health Examination Code (77 Ill. Adm. Code 665) Immunization Code (77 Ill. Adm. Code 695) College Immunization Code (77 Ill. Adm. Code 694) Control of Sexually Transmissible Diseases Code (77 Ill. Adm. Code 693) Control of Tuberculosis Code (77 Ill. Adm. Code 696) They can all be accessed through the IDPH Web site, <www.idph.state.il.us/rulesregs/rules-index.htm>.