Making Therapeutic Sense of Severe Deficit
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Cognitive Emotional Sequelae Post Stroke
11/26/2019 The Neuropsychology of Objectives 1. Identify various cognitive sequelae that may result from stroke Stroke: Cognitive & 2. Explain how stroke may impact emotional functioning, both acutely and long-term Emotional Sequelae COX HEALTH STROKE CONFERENCE BRITTANY ALLEN, PHD, ABPP, MBA 12/13/2019 Epidemiology of Stroke Stroke Statistics • > 795,000 people in the United States have a stroke • 5th leading cause of death for Americans • ~610,000 are first or new strokes • Risk of having a first stroke is nearly twice as high for blacks as whites • ~1/4 occur in people with a history of prior stroke • Blacks have the highest rate of death due to stroke • ~140,000 Americans die every year due to stroke • Death rates have declined for all races/ethnicities for decades except that Hispanics have seen • Approximately 87% of all strokes are ischemic an increase in death rates since 2013 • Costs the United States an estimated $34 billion annually • Risk for stroke increases with age, but 34% of people hospitalized for stroke were < 65 years of • Health care services age • Medicines to treat stroke • Women have a lower stroke risk until late in life when the association reverses • Missed days of work • Approximately 15% of strokes are heralded by a TIA • Leading cause of long-term disability • Reduces mobility in > 50% of stroke survivors > 65 years of age Source: Centers for Disease Control Stroke Death Rates Neuropsychological Assessment • Task Engagement • Memory • Language • Visuospatial Functioning • Attention/Concentration • Executive -

Lack of Motivation: Akinetic Mutism After Subarachnoid Haemorrhage
Netherlands Journal of Critical Care Submitted October 2015; Accepted March 2016 CASE REPORT Lack of motivation: Akinetic mutism after subarachnoid haemorrhage M.W. Herklots1, A. Oldenbeuving2, G.N. Beute3, G. Roks1, G.G. Schoonman1 Departments of 1Neurology, 2Intensive Care Medicine and 3Neurosurgery, St. Elisabeth Hospital, Tilburg, the Netherlands Correspondence M.W. Herklots - [email protected] Keywords - akinetic mutism, abulia, subarachnoid haemorrhage, cingulate cortex Abstract Akinetic mutism is a rare neurological condition characterised by One of the major threats after an aneurysmal SAH is delayed the lack of verbal and motor output in the presence of preserved cerebral ischaemia, caused by cerebral vasospasm. Cerebral alertness. It has been described in a number of neurological infarction on CT scans is seen in about 25 to 35% of patients conditions including trauma, malignancy and cerebral ischaemia. surviving the initial haemorrhage, mostly between days 4 and We present three patients with ruptured aneurysms of the 10 after the SAH. In 77% of the patients the area of cerebral anterior circulation and akinetic mutism. After treatment of the infarction corresponded with the aneurysm location. Delayed aneurysm, the patients lay immobile, mute and were unresponsive cerebral ischaemia is associated with worse functional outcome to commands or questions. However, these patients were awake and higher mortality rate.[6] and their eyes followed the movements of persons around their bed. MRI showed bilateral ischaemia of the medial frontal Cases lobes. Our case series highlights the risk of akinetic mutism in Case 1: Anterior communicating artery aneurysm patients with ruptured aneurysms of the anterior circulation. It A 28-year-old woman with an unremarkable medical history is important to recognise akinetic mutism in a patient and not to presented with a Hunt and Hess grade 3 and Fisher grade mistake it for a minimal consciousness state. -

Neuropsychological Aspects of Frontal Lobe Epilepsy
Neuropsychological aspects of frontal lobe epilepsy. Dominic Upton, Doctor of Philosophy. Institute of Neurology. University of London. LONDON, WON 36G ROCKEFELLER MEOICAL LIBRARY INSTITUTE OF NEUROLOGY THE NATIONAL HOSPITAL QUEEN SQUARE, LONDON, WCIN 33G CLASS ACCN No. d a t e W c ProQuest Number: 10017771 All rights reserved INFORMATION TO ALL USERS The quality of this reproduction is dependent upon the quality of the copy submitted. In the unlikely event that the author did not send a complete manuscript and there are missing pages, these will be noted. Also, if material had to be removed, a note will indicate the deletion. uest. ProQuest 10017771 Published by ProQuest LLC(2016). Copyright of the Dissertation is held by the Author. All rights reserved. This work is protected against unauthorized copying under Title 17, United States Code. Microform Edition © ProQuest LLC. ProQuest LLC 789 East Eisenhower Parkway P.O. Box 1346 Ann Arbor, Ml 48106-1346 Abstract. This study sought to increase our understanding of the neuropsychological consequences of frontal lobe epilepsy and surgery for this condition. In so doing, some suggestions were made on the role of the frontal lobes, and ways of assessing possible dysfunction in this area. The performance of a large group of subjects with clearly defined frontal lobe epilepsy (n=74), was examined on a comprehensive battery of neuropsychological measures. The performance of this group was compared to a control group of subjects with clearly defined temporal lobe epilepsy (n=57). There were few consistent group differences in test performance. Neither were there any strong relationships between test scores and epilepsy related variables. -

Co-Morbidities and Dementia
VOLUME 21 ISSUE 1 SPRING- SUMMER 2011 Published by the National Association of Professional Geriatric Care of Managers 3275 West Ina Road Suite 130 Tucson, Arizona Geriatric Care Management 85741 520.881.8008 / phone 520.325.7925 / fax www.caremanager.org Co-Morbidities and Dementia Guest Editor’s Message .............................................................................2 By Karen Knutson, MSN, MBA Dementia, Diabetes, Hypertension, and Alcohol Abuse: A Case Study of Medical Co-morbidities ....................................................3 By Karen Knutson, MSN, MBA Alzheimer’s Disease Co-morbidities ............................................................7 By M. Reza Bolouri, M.D. Frontal Lobe Disorders and Dementia.........................................................9 By Patricia Gross, Ph.D., ABPP-CN A Different Dementia: Different Challenges ...............................................13 By Sharon Mayfield, BSN of Geriatric Care Management Spring/Summer 2011 Guest Editor’s Message Coordinating the Complex Care of Clients with Dementia and Co-Morbidities By Karen Knutson, MSN, MBA, RN Care managers play a pivotal role in in psychiatric classification, co- options available for our clients? coordinating the care of their clients. morbidity does not necessarily imply Selected articles have been chosen As people live longer, the complexity the presence of multiple diseases, to provide more understanding of of life will continue and the increasing but rather an inability of a single the co-morbidities associated with prevalence of chronic disease will diagnosis to account for all of the dementia. Hopefully you will find pose many challenges for coordinating individual’s symptoms. new insights and approaches to such complex care. While the experts hash out integrate into your practice. In health care, co-morbidity is definitions of co-morbidity there The first article which I authored, defined in two different ways. -
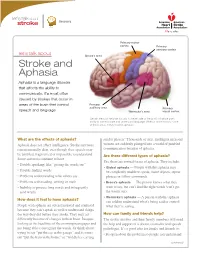
Stroke and Aphasia Aphasia Is a Language Disorder That Affects the Ability to Communicate
Recovery Primary motor cortex Primary sensory cortex let’s talk about Broca’s area Stroke and Aphasia Aphasia is a language disorder that affects the ability to communicate. It’s most often caused by strokes that occur in areas of the brain that control Primary auditory area Primary speech and language. Wernicke’s area visual cortex Certain areas of the brain (usually in the left side of the brain) influence one’s ability to communicate and understand language. When a stroke occurs in one of these areas, it may result in aphasia. What are the effects of aphasia? sender plissen.” Thousands of alert, intelligent men and Aphasia does not affect intelligence. Stroke survivors women are suddenly plunged into a world of jumbled remain mentally alert, even though their speech may communication because of aphasia. be jumbled, fragmented or impossible to understand. Are there different types of aphasia? Some survivors continue to have: Yes, there are several forms of aphasia. They include: • Trouble speaking, like “getting the words out” • Global aphasia — People with this aphasia may • Trouble finding words be completely unable to speak, name objects, repeat • Problems understanding what others say phrases or follow commands. • Problems with reading, writing or math • Broca’s aphasia — The person knows what they • Inability to process long words and infrequently want to say, but can’t find the right words (can’t get used words the words out). • Wernicke’s aphasia — A person with this aphasia How does it feel to have aphasia? can seldom understand what’s being said or control People with aphasia are often frustrated and confused what they’re saying. -

Abadie's Sign Abadie's Sign Is the Absence Or Diminution of Pain Sensation When Exerting Deep Pressure on the Achilles Tendo
A.qxd 9/29/05 04:02 PM Page 1 A Abadie’s Sign Abadie’s sign is the absence or diminution of pain sensation when exerting deep pressure on the Achilles tendon by squeezing. This is a frequent finding in the tabes dorsalis variant of neurosyphilis (i.e., with dorsal column disease). Cross References Argyll Robertson pupil Abdominal Paradox - see PARADOXICAL BREATHING Abdominal Reflexes Both superficial and deep abdominal reflexes are described, of which the superficial (cutaneous) reflexes are the more commonly tested in clinical practice. A wooden stick or pin is used to scratch the abdomi- nal wall, from the flank to the midline, parallel to the line of the der- matomal strips, in upper (supraumbilical), middle (umbilical), and lower (infraumbilical) areas. The maneuver is best performed at the end of expiration when the abdominal muscles are relaxed, since the reflexes may be lost with muscle tensing; to avoid this, patients should lie supine with their arms by their sides. Superficial abdominal reflexes are lost in a number of circum- stances: normal old age obesity after abdominal surgery after multiple pregnancies in acute abdominal disorders (Rosenbach’s sign). However, absence of all superficial abdominal reflexes may be of localizing value for corticospinal pathway damage (upper motor neu- rone lesions) above T6. Lesions at or below T10 lead to selective loss of the lower reflexes with the upper and middle reflexes intact, in which case Beevor’s sign may also be present. All abdominal reflexes are preserved with lesions below T12. Abdominal reflexes are said to be lost early in multiple sclerosis, but late in motor neurone disease, an observation of possible clinical use, particularly when differentiating the primary lateral sclerosis vari- ant of motor neurone disease from multiple sclerosis. -

THE CLINICAL ASSESSMENT of the PATIENT with EARLY DEMENTIA S Cooper, J D W Greene V15
J Neurol Neurosurg Psychiatry: first published as 10.1136/jnnp.2005.081133 on 16 November 2005. Downloaded from THE CLINICAL ASSESSMENT OF THE PATIENT WITH EARLY DEMENTIA S Cooper, J D W Greene v15 J Neurol Neurosurg Psychiatry 2005;76(Suppl V):v15–v24. doi: 10.1136/jnnp.2005.081133 ementia is a clinical state characterised by a loss of function in at least two cognitive domains. When making a diagnosis of dementia, features to look for include memory Dimpairment and at least one of the following: aphasia, apraxia, agnosia and/or disturbances in executive functioning. To be significant the impairments should be severe enough to cause problems with social and occupational functioning and the decline must have occurred from a previously higher level. It is important to exclude delirium when considering such a diagnosis. When approaching the patient with a possible dementia, taking a careful history is paramount. Clues to the nature and aetiology of the disorder are often found following careful consultation with the patient and carer. A focused cognitive and physical examination is useful and the presence of specific features may aid in diagnosis. Certain investigations are mandatory and additional tests are recommended if the history and examination indicate particular aetiologies. It is useful when assessing a patient with cognitive impairment in the clinic to consider the following straightforward questions: c Is the patient demented? c If so, does the loss of function conform to a characteristic pattern? c Does the pattern of dementia conform to a particular pattern? c What is the likely disease process responsible for the dementia? An understanding of cognitive function and its anatomical correlates is necessary in order to ascertain which brain areas are affected. -

Dementia and Aphasia in Motor Neuron Disease: an Underrecognised Association?
J Neurol Neurosurg Psychiatry 1998;65:881–889 881 J Neurol Neurosurg Psychiatry: first published as 10.1136/jnnp.65.6.881 on 1 December 1998. Downloaded from Dementia and aphasia in motor neuron disease: an underrecognised association? Wojtek P Rakowicz, John R Hodges Abstract predominantly sporadic, cases have subse- Objectives—To determine the prevalence quently been found in western countries.6–9 and nature of global cognitive dysfunction The most common pattern of cognitive and language deficits in an unselected decline in MND is a progressive dementia of population based cohort of patients with the frontal lobe type.10 It is unclear whether this motor neuron disease (MND). MND-frontal lobe dementia syndrome consti- Methods——A battery of neuropsycho- tutes the extreme end of a range of disease or logical and language tests was adminis- alternatively whether it represents a separate tered to patients presenting consecutively nosological entity. Whereas some early studies overa3yearperiodtoaregional neurol- which looked for intermediate degrees of ogy service with a new diagnosis of cognitive dysfunction in clinically non- sporadic motor neuron disease. demented patients with MND found no evidence of widespread impairment,11 others Results—The 18 patients could be divided reported poor performance in isolated tests of on the basis of their performance into 12 13 three groups: Three patients were de- memory or concentration. The emerging picture is of consistent abnormalities on tests of mented and had impaired language func- so-called “frontal executive” function, most tion (group 1); two non-demented patients notably decreased verbal fluency, aVecting a had an aphasic syndrome characterised large proportion of non-demented patients with Y by word finding di culties and anomia MND. -

• Classifications of Aphasia Expressive Vs. Receptive Fluent Vs
12/7/2018 APHASIA Aphasia is an acquired communication disorder that impairs a person’s ability to process LANGUAGE, but DOES NOT AFFECT intelligence. Aphasia impairs the ability to speak and understand others. -National Aphasia Association LANGUAGE Language is a system of communication that uses symbolism. K L U $ + M – Phonemes: perceptually distinct unit of sounds Words: sounds combined & given meaning Sentences: combination of syntax (rules) and semantics (meaning). • CLASSIFICATIONS OF APHASIA EXPRESSIVE VS. RECEPTIVE FLUENT VS. NON- FLUENT 1 12/7/2018 -NATIONAL APHASIA ASSOCIATION -COURTESY OF MY-MS.ORG MCA DISTRIBUTION -SLIDESHARE.NET 2 12/7/2018 BROCA’S APHASIA * short utterances * limited vocabulary * halting, effortful speech *mild comprehension deficits Lesion * Inferior frontal gyrus Choose Sentence Speech Coordinate Speak Idea Words Structure Sounds Articulate Pragmatics Muscles Fluently (Semantics) (Syntax) (Phonology) SAMPLE OF BROCA’S THERAPY FROM TACTUS THERAPY 3 12/7/2018 WERNICKE’S APHASIA • Comprehension is poor (auditory & reading) • Fluent, intact prosody • Logorrhea, press of speech • Neologisms, Paraphasias • Lack of awareness Lesion Temporo-Parietal, Posterior section of the superior temporal gyrus near the auditory cortex Auditory Preparation Attach Input Perception Recognition Phonological For Meaning Analysis Output WERNICKE’S APHASIA FROM TACTUS THERAPY 4 12/7/2018 GLOBAL APHASIA * severe language deficit * responds to personally relevant language * responds to non-verbal cues * some automatic speech Lesion -

Number Reading in Pure Alexiaâ
Neuropsychologia 49 (2011) 2283–2298 Contents lists available at ScienceDirect Neuropsychologia jo urnal homepage: www.elsevier.com/locate/neuropsychologia Reviews and perspectives Number reading in pure alexia—A review a,∗ b Randi Starrfelt , Marlene Behrmann a Center for Visual Cognition, Department of Psychology, Copenhagen University, O. Farimagsgade 2A, DK-1353 Copenhagen K, Denmark b Department of Psychology, Carnegie Mellon University, Pittsburgh, PA, USA a r t i c l e i n f o a b s t r a c t Article history: It is commonly assumed that number reading can be intact in patients with pure alexia, and that this Received 25 October 2010 dissociation between letter/word recognition and number reading strongly constrains theories of visual Received in revised form 31 March 2011 word processing. A truly selective deficit in letter/word processing would strongly support the hypothesis Accepted 22 April 2011 that there is a specialized system or area dedicated to the processing of written words. To date, however, Available online 4 May 2011 there has not been a systematic review of studies investigating number reading in pure alexia and so the status of this assumed dissociation is unclear. We review the literature on pure alexia from 1892 to Keywords: 2010, and find no well-documented classical dissociation between intact number reading and impaired Pure alexia letter identification in a patient with pure alexia. A few studies report strong dissociations, with number Alexia without agraphia reading less impaired than letter reading, but when we apply rigorous statistical criteria to evaluate Letter-by-letter reading Visual recognition these dissociations, the difference in performance across domains is not statistically significant. -

Journal of Neurological Disorders DOI: 10.4172/2329-6895.1000309 ISSN: 2329-6895
olog eur ica N l D f i o s l o a r n d r e u r s o J Lee, et al., J Neurol Disord 2016, 4:7 Journal of Neurological Disorders DOI: 10.4172/2329-6895.1000309 ISSN: 2329-6895 Case Report Open Access Two Cases with Cerebral Infarction in the Left Middle Frontal Lobe Presented as Gerstmann's Syndrome Eun-Ju Lee, Hye-Young Shin, Young Noh, Ki-Hyung Park, Hyeon-Mi Park, Yeong-Bae Lee, Dong-Jin Shin, Young Hee Sung and Dong Hoon Shin* Department of Neurology, Gil Hospital, Gachon University Gil Medical Center, Incheon, South Korea *Corresponding author: Dong Hoon Shin, Department of Neurology, Gil Hospital, Gachon University Gil Medical Center, South Korea, Tel: +82-32-460-3346; Fax: +83-32-460-3344; E-mail: [email protected] Rec date: Oct 08, 2016, Acc date: Oct 18, 2016, Pub date: Oct 22, 2016 Copyright: © 2016 Lee, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. Abstract Gerstmann's syndrome is a neuropsychological disorder characterized by four symptoms, namely, acalculia, finger agnosia, left-right disorientation, and agraphia suggesting the presence of a lesion in the inferior parietal lobule of the dominant hemisphere, especially at the angular gyrus. Several descriptions of Gerstmann's syndrome have been reported in associated with a lesion to the left frontal lobe, but none of these reports fulfilled the full tetrad of diagnostic criteria. -

Read the 2013 PSHA Journal
1 PSHA JOURNAL ANNUAL PUBLICATION OF THE PENNSYLVANIA SPEECH-LANGUAGE-HEARING ASSOCIATION DECEMBER 2013 EDITION 2 JOURNAL IS AN ANNUAL PUBLICATION OF THE PENNSYLVANIA SPEECH-LANGUAGE-HEARING ASSOCIATION 700 McKnight Park Drive, Suite 708 Pittsburgh, PA 15237 412.366.9858 (Phone) 412.366.8804 (Fax) [email protected] THE PENNSYLVANIA SPEECH-LANGUAGE-HEARING ASSOCIATION (PSHA), FOUNDED IN 1960, IS A PROFESSIONAL ORGANIZATION OF SPEECH-LANGUAGE PATHOLOGISTS, AUDIOLOGISTS, AND TEACHERS OF THE HEARING-IMPAIRED. AS SUCH, PSHA: Serves as a liaison between the American Speech-Language-Hearing Association and its Pennsylvania members. Represents its’ members interests in legislative affairs. Recommends standards for training and practices. Provides information about effective services and programs and services in communication disorders and other related fields. Works to inform the public about the professions, careers, programs, and services in the field of communication disorders. Encourages basic scientific study of the process of individual human communication. Monitors state Licensure Board activities. 2013-2014 PSHA EXECUTIVE BOARD PRESIDENT: Kathleen Helfrich-Miller PRESIDENT-ELECT: Amy Goldman PAST PRESIDENT: Craig Coleman VICE-PRESIDENT – PROFESSIONAL PRACTICE (SPEECH-LANGUAGE PATHOLOGY): Susan Hough VICE-PRESIDENT – PROFESSIONAL PRACTICE (AUDIOLOGY/EDUCATION): Jennifer Rakers VICE-PRESIDENT – PROFESSIONAL PREPARATION/CONTINUING EDUCATION: Joan Luckhurst VICE-PRESIDENT – MEMBERSHIP/ETHICAL PRACTICES: Nancy Carlino VICE-PRESIDENT – PUBLIC INFORMATION/PROFESSIONAL COMMUNICATION: Eileen Cirelli VICE-PRESIDENT – CONVENTION PLANNING/PROGRAMMING: Mary Beth Mason-Baughman VICE-PRESIDENT – GOVERNMENTAL RELATIONS: Caterina Stalteri VICE-PRESIDENT – PUBLICATIONS/EDITOR: Cheryl Gunter SECRETARY: Emily Katzaman TREASURER: Hunter Manasco Ex Officio STUDENT REPRESENTATIVE: Kathryn Young BUSINESS MANAGER: Diane Yenerall ACCOUNT MANAGER: Amy Caye 3 JOURNAL EDITOR Cheryl D. Gunter, Ph.D.