Hysteroscopy an Internal Examination of Your Womb
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Hysteroscopy with Dilation and Curretage (D & C)
501 19th Street, Trustees Tower FORT SANDERS WOMEN’S SPECIALISTS 1924 Pinnacle Point Way Suite 401, Knoxville Tn 37916 P# 865-331-1122 F# 865-331-1976 Suite 200, Knoxville Tn 37922 Dr. Curtis Elam, M.D., FACOG, AIMIS, Dr. David Owen, M.D., FACOG, Dr. Brooke Foulk, M.D., FACOG Dr. Dean Turner M.D., FACOG, ASCCP, Dr. F. Robert McKeown III, M.D., FACOG, AIMIS, Dr. Steven Pierce M.D., Dr. G. Walton Smith, M.D., FACOG, Dr. Susan Robertson, M.D., FACOG HYSTEROSCOPY WITH DILATION AND CURRETAGE (D & C) Please read and sign the following consent form when you feel that you completely understand the surgical procedure that is to be performed and after you have asked all of your questions. If you have any further questions or concerns, please contact our office prior to your procedure so that we may clarify any pertinent issues. Definition: HysterosCopy is an outpatient procedure that allows your doctor direct visualization of the inside of the uterine cavity (womb) by inserting a thin lighted telescope (hysteroscope) through the vagina (birth canal) and cervix, without making an abdominal incision. This procedure enables your doctor to examine the lining of the uterus, look for polyps, fibroids, scar tissue, blockages of the fallopian tubes, and abnormal partitions. In addition, this procedure allows your doctor to remove or surgically treat many of the abnormalities seen. Dilation and Curettage (D&C) allows your doctor to take a sample of the tissue that lines your uterus (endometrium) and/or to remove polyps, fibroid tumors, or hyperplasia. Suction D&C is used in cases of miscarriage. -

Risks of Hysteroscopy and Fractional Dilation and Curettage South Care Women's Florida
Risks of Hysteroscopy and Fractional Dilation and Curettage South Florida Women's Care The Procedure I will be undergoing is ______________________________________________________ _________________________________________________________________________________________. 1. Damage to uterus, bowel, bladder, urinary organs: Perforation of the uterus is a small risk. If that were to occur, laparoscopy (placing a camera in the umbilicus) may need to be done to make sure the uterus wasn’t bleeding and repair any damage. Cervical stenosis (inability of the cervix to dilate) can increase the rise of uterine perforation. 2. Fluid overload: Special attention is taken to monitor exactly how much fluid goes into your uterus during the hysteroscopy. Rarely, extra fluid can accumulate in your lungs, called pulmonary edema. 3. Damage to nerves, skin: We are very careful to position your legs very gently before surgery. Rarely, the nerves in your legs can “go to sleep” during surgery and can have temporary nerve damage. 4. Infection: You are given an antibiotic during surgery to decrease any risk of infection. Rarely, infection can occur after surgery and need medicine, and even surgery to correct. 5. Need for further surgery: If your procedure involves treatment for heavy bleeding (i.e. Removing a polyp or endometrial ablation), it is possible that these procedures will not cure your underlying problem and further surgery will be needed. 6. Risks for endometrial ablation: Sometimes your cervix will not close over the device and cause the procedure to be abandoned for safety reasons. There is also risk of damage to abdominal organs. About 5-10% of ablations done need further surgery (hysterectomy) to stop heavy bleeding. -

Dilation and Curettage (D&C)
Fact Sheet From ReproductiveFacts.org The Patient Education Website of the American Society for Reproductive Medicine Dilation and Curettage (D&C) This fact sheet was developed in collaboration with The Society of Reproductive Surgeons “Dilation and curettage” (D&C) is a short surgical as intestines, bladder, or blood vessels, are injured. If procedure that removes tissue from your uterus (womb). any of these organs are injured, they must be repaired You may need this procedure if you have unexplained with surgery. However, if no other organs have been or abnormal bleeding, or if you have delivered a baby injured, long-term complications from a perforation are and placental tissue remains in your womb. D&C also is extremely rare and the uterus heals on its own. performed to remove pregnancy tissue remaining from can occur after a D&C. If you are not a miscarriage or an abortion. Infections pregnant at the time of your D&C, this complication How is the procedure done? is extremely rare. However, 10% of women who were D&C can be done in a doctor’s office or in the hospital. pregnant before their D&C can get an infection, usually You may be given medications to relax you or to put you within 1 week of the procedure. It may be related to a to sleep for a short time. Your doctor will slowly widen sexually transmitted infection or due to normal bacteria the opening to your uterus (cervix). Opening your cervix that pass from the vagina into the uterus during or can cause cramping. -

A Critical Systematic Review and Meta-Analyses of Risk Factors for Fertility Problems in a Globalized World
medRxiv preprint doi: https://doi.org/10.1101/2021.05.06.21256676; this version posted May 8, 2021. The copyright holder for this preprint (which was not certified by peer review) is the author/funder, who has granted medRxiv a license to display the preprint in perpetuity. It is made available under a CC-BY-NC-ND 4.0 International license . Looking beyond the obvious: a critical systematic review and meta-analyses of risk factors for fertility problems in a globalized world Authors: R.R. Bayoumi1*, J. Boivin2*, H.M. Fatemi3, L. Hurt4, G.I. Serour5, S. van der Poel6 and C. Venetis7. 1* Corresponding author: PhD Student, School of Psychology, Cardiff University, Cardiff, Wales, UK; Takemi Fellow, Takemi Program in International Health, Harvard T.H. Chan School of Public Health, Boston, USA, [email protected] 2* Corresponding author: Professor of Psychology, School of Psychology, Cardiff University, Cardiff, Wales, UK, [email protected] 3: Professor of Obstetrics and Gynecology, Group Medical Director, ART Fertility Clinics, Abu Dhabi, UAE 4: Senior Lecturer, Division of Population Medicine, Cardiff University School of Medicine, Cardiff, Wales, UK 5: Professor of Obstetrics and Gynecology, Al Azhar University, Cairo, Egypt 6: Independent Consultant, Route de la Capite, Geneva, Switzerland 7: Associate Professor, Centre for Big Data Research in Health, University of New South Wales, Sydney, Australia Abstract Background: Well-established risk factors for fertility problems such as smoking have been included in fertility awareness efforts globally. However, these efforts neglect risks that women in low and middle-income countries (LMIC) face. Objective: To address this gap, we identified eight risk factors affecting women in LMIC and the aim of the current review was to estimate the impact of these risks on fertility. -

Hysteroscopy Vs. Transvaginal Ultraultrasonography in the Diagnosis of Endometrial Lesions
Caspian J Reprod Med, 2016, 2(1): 21-26 Caspian Journal of Reproductive Medicine Journal homepage: www.caspjrm.ir Original article Hysteroscopy vs. transvaginal ultraultrasonography in the diagnosis of endometrial lesions Zinatossadat Bouzari 1, Shahla Yazdani2, Sedigheh Esmailzadeh 2,*, Roza Shahhoseini3, Ali Fazli4, Mojgan Naeimi rad4 1Cellular & Molecular Biology Research Center, Department of Obstetrics & Gynecology, Babol University of Medical Sciences, Babol, Iran 2Infertility and Reproductive Health Research Center, Health Research Institute & Department of Obstetrics & Gynecology, Clinical Research Development Unit of Rouhani Hospital, Babol University of Medical Sciences, Babol, Iran 3Department of Obstetrics & Gynecology, Faculty of Medicine, Babol University of Medical Sciences, Babol, Iran 4Clinical Research Development Unit of Rouhani Hospital, Babol University of Medical Sciences, Babol-Iran Received: 11 Dec 2015 Accepted: 10 Mar 2016 Abstract Background: Abnormal uterine bleeding (AUB) is the most common gynecological problems that many factors are involved in its creation. Two common methods used to diagnose uterine lesions are vaginal ultraultrasonography and hysteroscopy. The aim of this study was to evaluate the diagnostic value of transvaginal ultraultrasonography and hysteroscopy in the diagnosis of intrauterine lesions leading to the AUB. Methods: A cross-sectional study was performed on 203 premenopausal post-menopausal women with complaints of abnormal uterine bleeding. A transvaginal ultraultrasonography was performed from the eligible subjects. In the second visit, a hysteroscopy was done and during the hysteroscopy procedure an endometrial biopsy was obtained from all the women. Pathology was considered as the gold standard and sensitivity, specificity, positive predictive value and negative predictive value were calculated for both methods using the Cat maker software. -

Hysteroscopy Dilation and Curettage
Hysteroscopy Dilation and Curettage Technique Procedure involves using a hysteroscope to place microinserts within the opening of the fallopian tubes from within the uterus. These inserts block the fallopian tubes for the purpose of permanent sterilization. Incisions No incisions are required for this procedure Operative Time Operative times vary greatly depending on the findings at the time of surgery. Your surgeon will proceed with safety as his/her first priority. Average times range from 15-30 minutes. Anesthesia • Local anesthesia or • Local anesthesia + IV sedation Preoperative Care • Schedule your case immediately after your period. • Your doctor will recommend that you take a hormonal medicine to thin the lining of your uterus prior to this procedure. • Nothing by mouth after midnight Hospital Stay • Office procedure • Day surgery Postoperative Care These guidelines are intended to give you a general idea of your postoperative course. Since every patient is unique and has a unique procedure, your recovery may differ. • Anti-inflammatory pain medicine, such as ibuprofen, naproxen, etc., is usually required for the first several days. Most patients do not need narcotics. • Driving is allowed once you have cleared anesthesia. • If they desire, patients may return to work on the day of the procedure. • You must use a form of reversible contraception until you undergo a hysterosalpingogram (HSG). This x-ray test will be performed 3 months after your procedure and will confirm that your fallopian tubes are occluded. 1700 6th Avenue South ● Birmingham, AL 35249 ● (205) 934-9999 . -
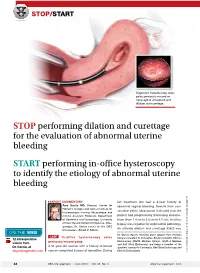
STOP Performing Dilation and Curettage for the Evaluation Of
STOP/START Diagnostic hysteroscopy spies polyp previously missed on transvaginal ultrasound and dilation and curettage. STOP performing dilation and curettage for the evaluation of abnormal uterine bleeding START performing in-office hysteroscopy to identify the etiology of abnormal uterine bleeding }expert commentary her treatment she had a 3-year history of Amy Garcia mD, Director, Center for abnormal vaginal bleeding. Results from con- Women’s Surgery and Garcia Institute for management secutive pelvic ultrasounds indicated that the Hysteroscopic Training, Albuquerque, and Clinical Assistant Professor, Department patient had progressively thickening endome- obg r of Obstetrics and Gynecology, University trium (from 1.4 cm to 2.5 cm to 4.7 cm). In-office O r f of New Mexico School of Medicine, Albu- E biopsy was negative for endometrial pathology. f querque. Dr. Garcia serves on the OBG ie An ultimate dilation and curettage (D&C) was K ManageMent Board of Editors. On the Web aig Dr. Garcia reports receiving grant support from Hologic; CASe In-office hysteroscopy spies being a consultant to Conceptus, Boston Scientific, Ethicon : Cr 12 intraoperative Endosurgery, IOGYN, Minerva, Hologic, Smith & Nephew, previously missed polyp ation videos from and Karl Storz Endoscopy; and being a member of the r A 51-year-old woman with a history of breast Dr. Garcia, at speakers’ bureau for Conceptus, Karl Storz Endoscopy, and ust ll obgmanagement.com cancer completed 5 years of tamoxifen. During Ethicon Endosurgery. I 44 OBG Management | June 2013 | Vol. 25 No. 6 obgmanagement.com performed with negative histologic diagnosis. FIGURE consecutive ultrasounds evaluating The patient is seen in consultation, and abnormal bleeding the ultrasound images are reviewed (FIGURE). -

The Woman with Postmenopausal Bleeding
THEME Gynaecological malignancies The woman with postmenopausal bleeding Alison H Brand MD, FRCS(C), FRANZCOG, CGO, BACKGROUND is a certified gynaecological Postmenopausal bleeding is a common complaint from women seen in general practice. oncologist, Westmead Hospital, New South Wales. OBJECTIVE [email protected]. This article outlines a general approach to such patients and discusses the diagnostic possibilities and their edu.au management. DISCUSSION The most common cause of postmenopausal bleeding is atrophic vaginitis or endometritis. However, as 10% of women with postmenopausal bleeding will be found to have endometrial cancer, all patients must be properly assessed to rule out the diagnosis of malignancy. Most women with endometrial cancer will be diagnosed with early stage disease when the prognosis is excellent as postmenopausal bleeding is an early warning sign that leads women to seek medical advice. Postmenopausal bleeding (PMB) is defined as bleeding • cancer of the uterus, cervix, or vagina (Table 1). that occurs after 1 year of amenorrhea in a woman Endometrial or vaginal atrophy is the most common cause who is not receiving hormone therapy (HT). Women of PMB but more sinister causes of the bleeding such on continuous progesterone and oestrogen hormone as carcinoma must first be ruled out. Patients at risk for therapy can expect to have irregular vaginal bleeding, endometrial cancer are those who are obese, diabetic and/ especially for the first 6 months. This bleeding should or hypertensive, nulliparous, on exogenous oestrogens cease after 1 year. Women on oestrogen and cyclical (including tamoxifen) or those who experience late progesterone should have a regular withdrawal bleeding menopause1 (Table 2). -

SJH Procedures
SJH Procedures - Gynecology and Gynecology Oncology Services New Name Old Name CPT Code Service ABLATION, LESION, CERVIX AND VULVA, USING CO2 LASER LASER VAPORIZATION CERVIX/VULVA W CO2 LASER 56501 Destruction of lesion(s), vulva; simple (eg, laser surgery, Gynecology electrosurgery, cryosurgery, chemosurgery) 56515 Destruction of lesion(s), vulva; extensive (eg, laser surgery, Gynecology electrosurgery, cryosurgery, chemosurgery) 57513 Cautery of cervix; laser ablation Gynecology BIOPSY OR EXCISION, LESION, FACE AND NECK EXCISION/BIOPSY (MASS/LESION/LIPOMA/CYST) FACE/NECK General, Gynecology, Plastics, ENT, Maxillofacial BIOPSY OR EXCISION, LESION, FACE AND NECK, 2 OR MORE EXCISE/BIOPSY (MASS/LESION/LIPOMA/CYST) MULTIPLE FACE/NECK 11102 Tangential biopsy of skin (eg, shave, scoop, saucerize, curette); General, Gynecology, single lesion Aesthetics, Urology, Maxillofacial, ENT, Thoracic, Vascular, Cardiovascular, Plastics, Orthopedics 11103 Tangential biopsy of skin (eg, shave, scoop, saucerize, curette); General, Gynecology, each separate/additional lesion (list separately in addition to Aesthetics, Urology, code for primary procedure) Maxillofacial, ENT, Thoracic, Vascular, Cardiovascular, Plastics, Orthopedics 11104 Punch biopsy of skin (including simple closure, when General, Gynecology, performed); single lesion Aesthetics, Urology, Maxillofacial, ENT, Thoracic, Vascular, Cardiovascular, Plastics, Orthopedics 11105 Punch biopsy of skin (including simple closure, when General, Gynecology, performed); each separate/additional lesion -

Icd-9-Cm (2010)
ICD-9-CM (2010) PROCEDURE CODE LONG DESCRIPTION SHORT DESCRIPTION 0001 Therapeutic ultrasound of vessels of head and neck Ther ult head & neck ves 0002 Therapeutic ultrasound of heart Ther ultrasound of heart 0003 Therapeutic ultrasound of peripheral vascular vessels Ther ult peripheral ves 0009 Other therapeutic ultrasound Other therapeutic ultsnd 0010 Implantation of chemotherapeutic agent Implant chemothera agent 0011 Infusion of drotrecogin alfa (activated) Infus drotrecogin alfa 0012 Administration of inhaled nitric oxide Adm inhal nitric oxide 0013 Injection or infusion of nesiritide Inject/infus nesiritide 0014 Injection or infusion of oxazolidinone class of antibiotics Injection oxazolidinone 0015 High-dose infusion interleukin-2 [IL-2] High-dose infusion IL-2 0016 Pressurized treatment of venous bypass graft [conduit] with pharmaceutical substance Pressurized treat graft 0017 Infusion of vasopressor agent Infusion of vasopressor 0018 Infusion of immunosuppressive antibody therapy Infus immunosup antibody 0019 Disruption of blood brain barrier via infusion [BBBD] BBBD via infusion 0021 Intravascular imaging of extracranial cerebral vessels IVUS extracran cereb ves 0022 Intravascular imaging of intrathoracic vessels IVUS intrathoracic ves 0023 Intravascular imaging of peripheral vessels IVUS peripheral vessels 0024 Intravascular imaging of coronary vessels IVUS coronary vessels 0025 Intravascular imaging of renal vessels IVUS renal vessels 0028 Intravascular imaging, other specified vessel(s) Intravascul imaging NEC 0029 Intravascular -

Comparison of Hysterosalpingography and Hysteroscopy in Evaluating the Uterine Cavity in Infertile Women
MOJ Women’s Health Research Article Open Access Comparison of hysterosalpingography and hysteroscopy in evaluating the uterine cavity in infertile women Abstract Volume 8 Issue 1 - 2019 Background: Infertility in women is predominantly associated with uterine cavity Baydaa F Alsannan,1 Ghadeer S Akbar,2 abnormalities. Uterine cavity anomalies and damage to the fallopian tubes may occur 3 due to various reasons such as endometriosis, polyps, adhesions and scar tissues. Anthony P Cheung 1Department of Obstetrics and Gynecology, University of Objective: To investigate the diagnostic value of hysterosalpingography (HSG) in Kuwait, Kuwait comparison to hysteroscopy (HSC) for various structural and intracavitary uterine 2Department of Obstetrics and Gynecology, Ministry of Health, pathologies in women with infertility. Kuwait 3Department of Reproductive Endocrinology and Infertility, Materials and methods: An observational study of 280 women with infertility was University of British Colombia, Canada carried out to compare the diagnostic values of HSG and HSC in the diagnosis of uterine pathologies in women enduring infertility. The specific uterine conditions Correspondence: Baydaa Al Sannan, Department of evaluated were intrauterine synechiae, intrauterine fibroids/polyps and Mullerian Obstetrics and Gynecology, Faculty of medicine, Kuwait congenital anomalies. The main outcome measures were sensitivity, specificity, University, Kuwait, Tel +965 25319601, positive and negative predictive values of HSG relative to hysteroscopy in diagnosing Email the following uterine pathologies: intrauterine synechiae, intrauterine fibroids/polyps Received: December 18, 2018 | Published: January 16, 2019 and Mullerian anomalies. Results: HSG had a sensitivity of 75% in detecting intrauterine synechiae, specificity of 86.5%, positive predictive value of 63% and negative predictive value of 91.8%. -

Shurooq Abid Abdulhadi* ABSTRACT KEYWORDS INTERNATIONAL
ORIGINAL RESEARCH PAPER Volume-9 | Issue-1 | January-2020 | PRINT ISSN No. 2277 - 8179 | DOI : 10.36106/ijsr INTERNATIONAL JOURNAL OF SCIENTIFIC RESEARCH THE MANAGEMENT OF POLYPS IN FEMALE GENITAL MUTILATION Gynaecology Manal Sabri Hasan High Diploma In Gynecology And Obstetrics/Abu Ghraib Hospital, Baghdad, Iraq Shurooq Abid High Diploma In Gynecology And Obstetrics/Abu Ghraib Hospital, Baghdad, Iraq Abdulhadi* *Corresponding Author ABSTRACT Polyps of the decrease reproductive canton are discovered between 7.8 to 50% of women. It has been hypothesized up to expectation cytogenetic modifications about chromosomes 6,7 or 12 so well namely epigenetic elements involving enzyme and metabolic activities may motive polyps in imitation of develop. Cervical polyps found into 2e5% concerning cases are of ignoble clinical significance or do cause, although rarely, submit coital bleedings. Cervical polyps develop at some stage in pregnancy or mucorrhoea. Trans vaginal ultrasound (TVU) presents an excellent diagnostic approach according to longevity diagnose the size and the anatomic vicinity on endometrial polyps (EPs). In asymptomatic young womanwith tiny EPs <10 min size, conservative administration perform be safely observed by using limit the polyp growth. EPs positioned at the fundal or tubocornual areas robotically affect plenty then buck up ordinary mobile characteristic due after chronic inflammation. In instances where Eps are a reason over subfertility mechanical hysteroscopic resection is advisable. When the sheer purpose because infertility is an EP, the affected person repeatedly becomes effortlessly with young shortly after removal. EP Detection into either peri- or post-menopausal age, among evidential and longevity asymptomatic patients calls because meticulous hysteroscopic analysis and polypectomy is mandatory.