Differences Between Amlodipine and Lisinopril in Control of Clinic and Twenty- Four Hour Ambulatory Blood Pressures
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

A Comparison of the Tolerability of the Direct Renin Inhibitor Aliskiren and Lisinopril in Patients with Severe Hypertension
Journal of Human Hypertension (2007) 21, 780–787 & 2007 Nature Publishing Group All rights reserved 0950-9240/07 $30.00 www.nature.com/jhh ORIGINAL ARTICLE A comparison of the tolerability of the direct renin inhibitor aliskiren and lisinopril in patients with severe hypertension RH Strasser1, JG Puig2, C Farsang3, M Croket4,JLi5 and H van Ingen4 1Technical University Dresden, Heart Center, University Hospital, Dresden, Germany; 2Department of Internal Medicine, La Paz Hospital, Madrid, Spain; 31st Department of Internal Medicine, Semmelweis University, Budapest, Hungary; 4Novartis Pharma AG, Basel, Switzerland and 5Novartis Institutes for Biomedical Research, Cambridge, MA, USA Patients with severe hypertension (4180/110 mm Hg) LIS 3.4%). The most frequently reported AEs in both require large blood pressure (BP) reductions to reach groups were headache, nasopharyngitis and dizziness. recommended treatment goals (o140/90 mm Hg) and At end point, ALI showed similar mean reductions from usually require combination therapy to do so. This baseline to LIS in msDBP (ALI À18.5 mm Hg vs LIS 8-week, multicenter, randomized, double-blind, parallel- À20.1 mm Hg; mean treatment difference 1.7 mm Hg group study compared the tolerability and antihyperten- (95% confidence interval (CI) À1.0, 4.4)) and mean sitting sive efficacy of the novel direct renin inhibitor aliskiren systolic blood pressure (ALI À20.0 mm Hg vs LIS with the angiotensin converting enzyme inhibitor À22.3 mm Hg; mean treatment difference 2.8 mm Hg lisinopril in patients with severe hypertension (mean (95% CI À1.7, 7.4)). Responder rates (msDBPo90 mm Hg sitting diastolic blood pressure (msDBP)X105 mm Hg and/or reduction from baselineX10 mm Hg) were 81.5% and o120 mm Hg). -

Potentially Harmful Drugs in the Elderly: Beers List
−This Clinical Resource gives subscribers additional insight related to the Recommendations published in− March 2019 ~ Resource #350301 Potentially Harmful Drugs in the Elderly: Beers List In 1991, Dr. Mark Beers and colleagues published a methods paper describing the development of a consensus list of medicines considered to be inappropriate for long-term care facility residents.12 The “Beers list” is now in its sixth permutation.1 It is intended for use by clinicians in outpatient as well as inpatient settings (but not hospice or palliative care) to improve the care of patients 65 years of age and older.1 It includes medications that should generally be avoided in all elderly, used with caution, or used with caution or avoided in certain elderly.1 There is also a list of potentially harmful drug-drug interactions in seniors, as well as a list of medications that may need to be avoided or have their dosage reduced based on renal function.1 This information is not comprehensive; medications and interactions were chosen for inclusion based on potential harm in relation to benefit in the elderly, and availability of alternatives with a more favorable risk/benefit ratio.1 The criteria no longer address drugs to avoid in patients with seizures or insomnia because these concerns are not unique to the elderly.1 Another notable deletion is H2 blockers as a concern in dementia; evidence of cognitive impairment is weak, and long-term PPIs pose risks.1 Glimepiride has been added as a drug to avoid. Some drugs have been added with cautions (dextromethorphan/quinidine, trimethoprim/sulfamethoxazole), and some have had cautions added (rivaroxaban, tramadol, SNRIs). -

Ace Inhibitors (Angiotensin-Converting Enzyme)
Medication Instructions Ace Inhibitors (Angiotensin-Converting Enzyme) Generic Brand Benazepril Lotensin Captopril Capoten Enalapril Vasotec Fosinopril Monopril Lisinopril Prinivil, Zestril Do not Moexipril Univasc Quinapril Accupril stop taking Ramipril Altace this medicine Trandolapril Mavik About this Medicine unless told ACE inhibitors are used to treat both high blood pressure (hypertension) and heart failure (HF). They block an enzyme that causes blood vessels to constrict. This to do so allows the blood vessels to relax and dilate. Untreated, high blood pressure can damage to your heart, kidneys and may lead to stroke or heart failure. In HF, using by your an ACE inhibitor can: • Protect your heart from further injury doctor. • Improve your health • Reduce your symptoms • Can prevent heart failure. Generic forms of ACE Inhibitors (benazepril, captopril, enalapril, fosinopril, and lisinopril) may be purchased at a lower price. There are no “generics” for Accupril, Altace Mavik, and of Univasc. Thus their prices are higher. Ask your doctor if one of the generic ACE Inhibitors would work for you. How to Take Use this drug as directed by your doctor. It is best to take these drugs, especially captopril, on an empty stomach one hour before or two hours after meals (unless otherwise instructed by your doctor). Side Effects Along with needed effects, a drug may cause some unwanted effects. Many people will not have any side effects. Most of these side effects are mild and short-lived. Check with your doctor if any of the following side effects occur: • Fever and chills • Hoarseness • Swelling of face, mouth, hands or feet or any trouble in swallowing or breathing • Dizziness or lightheadedness (often a problem with the first dose) Report these side effects if they persist: • Cough – dry or continuing • Loss of taste, diarrhea, nausea, headache or unusual fatigue • Fast or irregular heartbeat, dizziness, lightheadedness • Skin rash Special Guidelines • Sodium in the diet may cause you to retain fluid and increase your blood pressure. -

Guideline for Preoperative Medication Management
Guideline: Preoperative Medication Management Guideline for Preoperative Medication Management Purpose of Guideline: To provide guidance to physicians, advanced practice providers (APPs), pharmacists, and nurses regarding medication management in the preoperative setting. Background: Appropriate perioperative medication management is essential to ensure positive surgical outcomes and prevent medication misadventures.1 Results from a prospective analysis of 1,025 patients admitted to a general surgical unit concluded that patients on at least one medication for a chronic disease are 2.7 times more likely to experience surgical complications compared with those not taking any medications. As the aging population requires more medication use and the availability of various nonprescription medications continues to increase, so does the risk of polypharmacy and the need for perioperative medication guidance.2 There are no well-designed trials to support evidence-based recommendations for perioperative medication management; however, general principles and best practice approaches are available. General considerations for perioperative medication management include a thorough medication history, understanding of the medication pharmacokinetics and potential for withdrawal symptoms, understanding the risks associated with the surgical procedure and the risks of medication discontinuation based on the intended indication. Clinical judgement must be exercised, especially if medication pharmacokinetics are not predictable or there are significant risks associated with inappropriate medication withdrawal (eg, tolerance) or continuation (eg, postsurgical infection).2 Clinical Assessment: Prior to instructing the patient on preoperative medication management, completion of a thorough medication history is recommended – including all information on prescription medications, over-the-counter medications, “as needed” medications, vitamins, supplements, and herbal medications. Allergies should also be verified and documented. -

Angioedema After Long-Term Use of an Angiotensin-Converting Enzyme Inhibitor
J Am Board Fam Pract: first published as 10.3122/jabfm.10.5.370 on 1 September 1997. Downloaded from BRIEF REPORTS Angioedema After Long-Term Use of an Angiotensin-Converting Enzyme Inhibitor Adriana]. Pavietic, MD Angioedema is an uncommon adverse effect of cyclobenzaprine, her angioedema was initially be angiotensin-converting enzyme (ACE) inhib lieved to be an allergic reaction to this drug, and itors. Its frequency ranges from 0.1 percent in pa it was discontinued. She was also given 125 mg of tients on captopril, lisinopril, and quinapril to 0.5 methylprednisolone intramuscularly. Her an percent in patients on benazepril. l Most cases are gioedema did not improve, and she returned to mild and occur within the first week of treat the clinic the following day. She was seen by an ment. 2-4 Recent reports indicate that late-onset other physician, who discontinued lisinopril, and angioedema might be more prevalent than ini her symptoms resolved within 24 hours. Mter her tially thought, and fatal cases have been de ACE inhibitor was discontinued, she experienced scribed.5-11 Many physicians are not familiar with more symptoms and an increased frequency of late-onset angioedema associated with ACE in palpitations, but she had no change in exercise hibitors, and a delayed diagnosis can have poten tolerance. A cardiologist was consulted, who pre tially serious consequences.5,8-II scribed the angiotensin II receptor antagonist losartan (initially at dosages of 25 mg/d and then Case Report 50 mg/d). The patient was advised to report any A 57-year-old African-American woman with symptoms or signs of angioedema immediately copyright. -
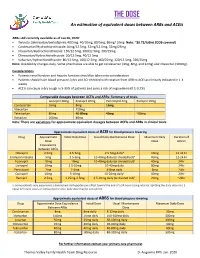
THE DOSE an Estimation of Equivalent Doses Between Arbs and Aceis
THE DOSE An estimation of equivalent doses between ARBs and ACEIs ARBs still currently available as of Jan 26, 2020: Twynsta (telmisartan/amlodipine): 40/5mg. 40/10mg, 80/5mg, 80mg/ 10mg Note: ~$0.73/tablet (ODB covered) Candesartan/Hydrochlorothiazide:16mg/12.5mg, 32mg/12.5mg, 32mg/25mg Irbesartan/Hydrochlorothiazide: 150/12.5mg, 300/12.5mg, 300/25mg Olmesartan/Hydrochlorothiaizde: 20/12.5mg, 40/12.5mg Valsartan/Hydrochlorothiazide: 80/12.5mg, 160/12.5mg, 160/25mg, 320/12.5mg, 320/25mg Note: Availability changes daily. Some pharmacies are able to get candesartan (4mg, 8mg, and 32mg) and irbesartan (300mg). Considerations Patients renal function and hepatic function should be taken into consideration Patients should have blood pressure, lytes and SCr checked with rotation from ARB to ACEI as clinically indicated in 1-4 weeks ACEIs can cause a dry cough in 5-35% of patients and carry a risk of angioedema (0.1-0.2%) Comparable dosages between ACEIs and ARBs- Summary of trials Lisinopril 20mg Enalapril 20mg Perindopril 4mg Ramipril 10mg Candesartan 16mg 8mg 16mg Irbesartan 150mg Telmisartan 80mg 40-80mg 40mg ~80mg Valsartan 160mg 80mg Note: There are variations for approximate equivalent dosages between ACEIs and ARBs in clinical trials. Approximate equivalent doses of ACEI for blood pressure lowering Drug Approximate Initial Daily Dose Usual Daily Maintenance Dose Maximum Daily Duration of Dose Dose Action Equivalence Between ACEIs Cilazapril 2.5mg 2.5-5mg 2.5-5mg dailya 10mg 12-24 hr Enalapril maleate 5mg 2.5-5mg 10-40mg daily (or divided bid)a 40mg 12-24 hr Fosinopril 10mg 10mg 10-40mg daily (or divided bid)a 40mg 24hr Lisinopril 10mg 2.5-10mg 10-40mg daily 80mg 24hr Perindopril 2mg 2-4mg 4-8mg daily 8mg 24hr Quinapril 10mg 5-10mg 10-20mg dailya 40mg 24hr Ramipril 2.5mg 1.25mg-2.5mg 2.5-10mg daily (or divided bid)a 20mg ~24hr a: Some patients may experience a diminished antihypertensive effect toward the end of a 24-hour dosing interval. -

LIST of APPROVED DRUG from 01-01-2011 to 31-12-2011
LIST OF APPROVED DRUG FROM 01-01-2011 to 31-12-2011 Date of Sr. No. Name of Drug Indication Issue Alpha Lipoic Acid USP 100mg + Methylcobalamin 1500mcg + Vitamin B6 IP 3mg + Folic Acid IP 1.5mg + Benfotiamine For the treatment of diabetic 1. 03.01.11 50mg + Biotin USP 5mg + Chromium neuropathy Picolinate USP Eq. to Chromuim 200mcg Capsule Ropinirole ER Tablet 1 mg. 2. Same as approved 04.01.11 (Additional Strength) Monotherapy for the Maintenance Treatment of Patients with locally advanced metastatic Erlotinib HCl Tablet 150 mg 3. non-small lung cancer whose disease has not 04.01.11 (Additional Indication) progressed after four cycles of Platinum based First Line Chemotherapy. Moxifloxacin HCl BP 0.5% w/v + Bromfenac For the reduction of post operative 4. 05.01.11 Sodium 0.09% w/v Eye drop inflammatory conditions of the eye Ferrous Ascorbate 100mg + Folic Acid IP 1.5mg + Cyanocobalamin IP 15mcg + Zinc 5. For the treatment of iron deficiency anaemia 05.01.11 Sulphate Monohydrate Eq. to Elemental Zinc 22.5mg Tablet S (+) Etodolac 300mg +Thiocolchicoside 8mg For the treatment of patients with acute 6. 05.01.11 Tablet painful musculoskeletal conditions Beclomethasone Dipropionate IP 100mcg + For the treatment of bronchial asthma where Formoterol Fumarate Dihydrate BP Eq. to 7. use of inhaled corticosteroid therapy found 05.01.11 Formoterol Fumarate 6 mcg Metered Dose appropriate Inhaler Amlodipine Besilate IP Eq. to Amlodipine For the treatment of mild to moderate 8. 05.01.11 5mg + Indapamide USP SR 1.5mg Tablet hypertension Metformin HCl IP 500mg + Alpha Lipoic Acid For the treatment of patients with diabetic 9. -

Angiotensin-Converting Enzyme (ACE) Inhibitors
Angiotensin-Converting Enzyme (ACE) Inhibitors Summary Blood pressure reduction is similar for the ACE inhibitors class, with no clinically meaningful differences between agents. Side effects are infrequent with ACE inhibitors, and are usually mild in severity; the most commonly occurring include cough and hypotension. Captopril and lisinopril do not require hepatic conversion to active metabolites and may be preferred in patients with severe hepatic impairment. Captopril differs from other oral ACE inhibitors in its rapid onset and shorter duration of action, which requires it to be given 2-3 times per day; enalaprilat, an injectable ACE inhibitor also has a rapid onset and shorter duration of action. Pharmacology Angiotensin Converting Enzyme Inhibitors (ACE inhibitors) block the conversion of angiotensin I to angiotensin II through competitive inhibition of the angiotensin converting enzyme. Angiotensin is formed via the renin-angiotensin-aldosterone system (RAAS), an enzymatic cascade that leads to the proteolytic cleavage of angiotensin I by ACEs to angiotensin II. RAAS impacts cardiovascular, renal and adrenal functions via the regulation of systemic blood pressure and electrolyte and fluid balance. Reduction in plasma levels of angiotensin II, a potent vasoconstrictor and negative feedback mediator for renin activity, by ACE inhibitors leads to increased plasma renin activity and decreased blood pressure, vasopressin secretion, sympathetic activation and cell growth. Decreases in plasma angiotensin II levels also results in a reduction in aldosterone secretion, with a subsequent decrease in sodium and water retention.[51035][51036][50907][51037][24005] ACE is found in both the plasma and tissue, but the concentration appears to be greater in tissue (primarily vascular endothelial cells, but also present in other organs including the heart). -

Hyponatremia Induced by Angiotensin Converting Enzyme Inhibitors and Angiotensin
DOI: 10.7860/JCDR/2018/31983.11754 Original Article Hyponatremia Induced by Angiotensin Converting Enzyme Inhibitors and Angiotensin Pharmacology Section Receptor Blockers-A Pilot Study S BHUVANESHWARI1, PRAKASH VEL SANKHYA SAROJ2, D VIJAYA3, M SABARI SOWMYA4, R SENTHIL KUMAR5 ABSTRACT Results: Among all, 48% (24 out of 50) of the study population Introduction: Hyponatremia, serum sodium <135 mmol/L, can administered with ACEI and ARB developed hyponatremia. result in neurological manifestation in acute cases, may lead Predisposition to develop hyponatremia was high in males to seizures and coma. Angiotensin Converting Enzyme Inhibitor compared to females. Incidence of hyponatremia was 62.5% (10 (ACEI) and Angiotensin II Receptor Blockers (ARB) are drugs out of 16) in the age group of 56-75 years. Though, incidence of that have been commonly prescribed for the treatment of hyponatremia was 54.5% (18 out of 33) in ACEI group compared hypertension and cardiac diseases. It has become important to 35.2% (6 out of 17) in ARB group, but it was not statistically to evaluate and investigate the incidence of hyponatremia on significant. The study also revealed that metosartan had a higher consumption of these drugs. association with hyponatremia compared to other drugs. Aim: To determine the susceptibility of patients on ACEI and Conclusion: Hyponatremia was induced in nearly 50% of ARB to hyponatremia and to ascertain the drug producing patients taking ACEI and ARB. The incidence of hyponatremia notable hyponatremia among ACEI and ARB. among patients on these two drugs did not show statistical variation. Metosartan showed a higher incidence of Materials and Methods: The study was conducted in a tertiary hyponatremia compared to enalapril, ramipril, captopril, care hospital. -

Zestril® (Lisinopril) Tablets Label
HIGHLIGHTS OF PRESCRIBING INFORMATION • Hypersensitivity (4) These highlights do not include all the information needed to use • Co-administration of aliskiren with Zestril in patients with diabetes (4, ZESTRIL safely and effectively. See full prescribing information for 7.4) ZESTRIL ----------------------- WARNINGS AND PRECAUTIONS --------------------- Zestril® (lisinopril) tablets, for oral use Initial U.S. Approval: 1988 • Angioedema: Discontinue Zestril, provide appropriate therapy and monitor until resolved (5.2) WARNING: FETAL TOXICITY • Renal impairment: Monitor renal function periodically (5.3) See full prescribing information for complete boxed warning. • Hypotension: Patients with other heart or renal diseases have increased • When pregnancy is detected, discontinue Zestril as soon as possible. risk, monitor blood pressure after initiation (5.4) (5.1) • Hyperkalemia: Monitor serum potassium periodically (5.5) • Drugs that act directly on the rennin-angiotensin system can cause • injury and death to the developing fetus. (5.1) Cholestatic jaundice and hepatic failure: Monitor for jaundice or signs of liver failure (5.6) ------------------------------ ADVERSE REACTIONS ---------------------------- --------------------------- INDICATIONS AND USAGE -------------------------- Common adverse reactions (events 2% greater than placebo) by use: Zestril is an angiotensin converting enzyme (ACE) inhibitor indicated for: • Hypertension: headache, dizziness and cough (6.1) • Treatment of hypertension in adults and pediatric patients 6 years of age • Heart Failure: hypotension and chest pain (6.1) and older (1.1) • Acute Myocardial Infarction: hypotension (6.1) • Adjunct therapy for heart failure (1.2) To report SUSPECTED ADVERSE REACTIONS, contact AstraZeneca • Treatment of Acute Myocardial Infarction (1.3) Pharmaceuticals LP at 1-800-236-9933 or FDA at 1-800-FDA-1088 or ---------------------- DOSAGE AND ADMINISTRATION --------------------- www.fda.gov/medwatch. -

Amlodipine 5Mg and 10Mg Tablets Amlodipine Mesilate Monohydrate
Package leaflet: Information for the patient Amlodipine 5mg and 10mg tablets Amlodipine mesilate monohydrate Read all of this leaflet carefully before you start • have recent heart attack taking this medicine because it contains important • have heart failure information for you. • are elderly, your doctor may monitor you closely. • have/suffer from severe increase in blood pressure (hypertensive • Keep this leaflet. You may need to read it again. crisis) • If you have any further questions, please ask your doctor, pharmacist or nurse. Children and adolescents • This medicine has been prescribed for you. Do not pass Safety and effectiveness have been studied in 6-17 year old boys and it on to others. It may harm them, even if their signs of in girls. Amlodipine should only used for hypertension in children and illness are the same as yours. adolescents from 6 years to 17 years of age. Amlodipine has not been studied in children under the age of 6 years. For more information, talk • If you get any side effects, talk to your doctor, to your doctor. pharmacist or nurse. This includes any possible side effects not listed in this leaflet. See section 4. Other medicines and Amlodipine tablets Tell your doctor or pharmacist if you are taking, have recently taken or What is in this leaflet might take any other medicines, including: • ketoconazole or itraconazole (antifungal drugs) 1 What Amlodipine tablets are and what • ritonavir, indinavir, nelfinavir (so called protease inhibitors used to they are used for treat HIV) • rifampicin, erythromycin, clarithromycin (antibiotic drug) 2 What you need to know before you take • hypericum perforatum (St. -

Lisinopril (Ethics) Lisinopril Tablets 5 Mg, 10 Mg, 20 Mg
New Zealand Data Sheet Lisinopril (Ethics) Lisinopril Tablets 5 mg, 10 mg, 20 mg 1. NAME OF THE MEDICINAL PRODUCT LISINOPRIL (Ethics) 5 mg, tablet LISINOPRIL (Ethics) 10 mg, tablet LISINOPRIL (Ethics) 20 mg, tablet 2. QUALITATIVE AND QUANTITATIVE COMPOSITION Lisinopril (Ethics) tablets come in three strengths and contain lisinopril dihydrate equivalent to 5 mg, 10 mg or 20 mg lisinopril. 3. PHARMACEUTICAL FORM 5 mg tablet: A light pink coloured, circular, biconvex uncoated tablet. The tablet has a break line and is embossed with ‘5’ on one side and embossed with ‘BL’ on the other side. 10 mg tablet: A light pink coloured, circular, biconvex uncoated tablet. The tablet is embossed with ‘10’ on one side and embossed with ‘BL’ on the other side. 20 mg tablet: A pink, circular, biconvex uncoated tablet. The tablet is embossed with ‘20’ on one side and embossed with ‘BL’ on the other side. Lisinopril dihydrate. The chemical name for lisinopril dihydrate is N-[N-[(1S)-1-carboxy-3- phenylpropyl]-L-lysyl]-L-proline dihydrate. Its structural formula is: C21H31N3O5.2H2O, Molecular weight: 441.53, CAS No.: 83915-83-7 Lisinopril dihydrate is a white to off-white crystalline powder that is soluble in water, sparingly soluble in methanol and practically insoluble in ethanol. A synthetic peptide derivative, lisinopril dihydrate is an oral long acting angiotensin converting enzyme inhibitor. It is a lysine analogue of enalaprilat (active metabolite of enalapril). 4. CLINICAL PARTICULARS 4.1 Therapeutic indications Lisinopril is indicated in the treatment of essential hypertension and in renovascular hypertension. It may be used alone or concomitantly with other classes of antihypertensive agents.