1 Differential Expression of Coding and Long Noncoding Rnas In
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Aquaporin Channels in the Heart—Physiology and Pathophysiology
International Journal of Molecular Sciences Review Aquaporin Channels in the Heart—Physiology and Pathophysiology Arie O. Verkerk 1,2,* , Elisabeth M. Lodder 2 and Ronald Wilders 1 1 Department of Medical Biology, Amsterdam University Medical Centers, University of Amsterdam, 1105 AZ Amsterdam, The Netherlands; [email protected] 2 Department of Experimental Cardiology, Amsterdam University Medical Centers, University of Amsterdam, 1105 AZ Amsterdam, The Netherlands; [email protected] * Correspondence: [email protected]; Tel.: +31-20-5664670 Received: 29 March 2019; Accepted: 23 April 2019; Published: 25 April 2019 Abstract: Mammalian aquaporins (AQPs) are transmembrane channels expressed in a large variety of cells and tissues throughout the body. They are known as water channels, but they also facilitate the transport of small solutes, gasses, and monovalent cations. To date, 13 different AQPs, encoded by the genes AQP0–AQP12, have been identified in mammals, which regulate various important biological functions in kidney, brain, lung, digestive system, eye, and skin. Consequently, dysfunction of AQPs is involved in a wide variety of disorders. AQPs are also present in the heart, even with a specific distribution pattern in cardiomyocytes, but whether their presence is essential for proper (electro)physiological cardiac function has not intensively been studied. This review summarizes recent findings and highlights the involvement of AQPs in normal and pathological cardiac function. We conclude that AQPs are at least implicated in proper cardiac water homeostasis and energy balance as well as heart failure and arsenic cardiotoxicity. However, this review also demonstrates that many effects of cardiac AQPs, especially on excitation-contraction coupling processes, are virtually unexplored. -

The Caenorhabditis Elegans Excretory System: a Model for Tubulogenesis, Cell Fate Specification, and Plasticity
| WORMBOOK CELL AND ORGANELLE BIOLOGY The Caenorhabditis elegans Excretory System: A Model for Tubulogenesis, Cell Fate Specification, and Plasticity Meera V. Sundaram*,1 and Matthew Buechner† *Department of Genetics, Perelman School of Medicine, University of Pennsylvania, Philadelphia, Pennsylvania 19104 and †Department of Molecular Biosciences, University of Kansas, Lawrence, Kansas 66045 ABSTRACT The excretory system of the nematode Caenorhabditis elegans is a superb model of tubular organogenesis involving a minimum of cells. The system consists of just three unicellular tubes (canal, duct, and pore), a secretory gland, and two associated neurons. Just as in more complex organs, cells of the excretory system must first adopt specific identities and then coordinate diverse processes to form tubes of appropriate topology, shape, connectivity, and physiological function. The unicellular topology of excretory tubes, their varied and sometimes complex shapes, and the dynamic reprogramming of cell identity and remodeling of tube connec- tivity that occur during larval development are particularly fascinating features of this organ. The physiological roles of the excretory system in osmoregulation and other aspects of the animal’s life cycle are only beginning to be explored. The cellular mechanisms and molecular pathways used to build and shape excretory tubes appear similar to those used in both unicellular and multicellular tubes in more complex organs, such as the vertebrate vascular system and kidney, making this simple organ system a -

Aquaporin-7 Regulates the Response to Cellular Stress in Breast Cancer
Author Manuscript Published OnlineFirst on July 6, 2020; DOI: 10.1158/0008-5472.CAN-19-2269 Author manuscripts have been peer reviewed and accepted for publication but have not yet been edited. Title. Aquaporin-7 Regulates the Response to Cellular Stress in Breast Cancer Authors. Chen Dai1,2*, Verodia Charlestin1,2*, Man Wang1,2, Zachary T. Walker1,2, Maria Cristina Miranda-Vergara1,2, Beth A. Facchine1,2, Junmin Wu1,2, William J. Kaliney2, Norman J. Dovichi1,2, Jun Li2,3, and Laurie E. Littlepage1,2 Affiliations. 1Department of Chemistry and Biochemistry, University of Notre Dame, Notre Dame, IN 46556 2Harper Cancer Research Institute, South Bend, IN 46617 3Department of Applied and Computational Mathematics and Statistics, University of Notre Dame, Notre Dame, IN 46556 *Authors contributed equally Running title. Aquaporin-7 is a metabolic regulator in breast cancer Keywords. Aquaporin, breast cancer, tumor metabolism, correlation-based network analysis Corresponding Author. Laurie Littlepage, Ph.D., Harper Cancer Research Institute, University of Notre Dame, 1234 N Notre Dame Avenue, South Bend, IN 46617; Phone: (574) 631-4804 Fax: (574) 631-1165 Email: [email protected] Conflict of interest disclosure statement. The authors disclose no potential conflicts of interest. 1 Downloaded from cancerres.aacrjournals.org on September 26, 2021. © 2020 American Association for Cancer Research. Author Manuscript Published OnlineFirst on July 6, 2020; DOI: 10.1158/0008-5472.CAN-19-2269 Author manuscripts have been peer reviewed and accepted for publication but have not yet been edited. Abstract The complex yet interrelated connections between cancer metabolism, gene expression, and oncogenic driver genes have the potential to identify novel biomarkers and drug targets with prognostic and therapeutic value. -

1 No. Affymetrix ID Gene Symbol Genedescription Gotermsbp Q Value 1. 209351 at KRT14 Keratin 14 Structural Constituent of Cyto
1 Affymetrix Gene Q No. GeneDescription GOTermsBP ID Symbol value structural constituent of cytoskeleton, intermediate 1. 209351_at KRT14 keratin 14 filament, epidermis development <0.01 biological process unknown, S100 calcium binding calcium ion binding, cellular 2. 204268_at S100A2 protein A2 component unknown <0.01 regulation of progression through cell cycle, extracellular space, cytoplasm, cell proliferation, protein kinase C inhibitor activity, protein domain specific 3. 33323_r_at SFN stratifin/14-3-3σ binding <0.01 regulation of progression through cell cycle, extracellular space, cytoplasm, cell proliferation, protein kinase C inhibitor activity, protein domain specific 4. 33322_i_at SFN stratifin/14-3-3σ binding <0.01 structural constituent of cytoskeleton, intermediate 5. 201820_at KRT5 keratin 5 filament, epidermis development <0.01 structural constituent of cytoskeleton, intermediate 6. 209125_at KRT6A keratin 6A filament, ectoderm development <0.01 regulation of progression through cell cycle, extracellular space, cytoplasm, cell proliferation, protein kinase C inhibitor activity, protein domain specific 7. 209260_at SFN stratifin/14-3-3σ binding <0.01 structural constituent of cytoskeleton, intermediate 8. 213680_at KRT6B keratin 6B filament, ectoderm development <0.01 receptor activity, cytosol, integral to plasma membrane, cell surface receptor linked signal transduction, sensory perception, tumor-associated calcium visual perception, cell 9. 202286_s_at TACSTD2 signal transducer 2 proliferation, membrane <0.01 structural constituent of cytoskeleton, cytoskeleton, intermediate filament, cell-cell adherens junction, epidermis 10. 200606_at DSP desmoplakin development <0.01 lectin, galactoside- sugar binding, extracellular binding, soluble, 7 space, nucleus, apoptosis, 11. 206400_at LGALS7 (galectin 7) heterophilic cell adhesion <0.01 2 S100 calcium binding calcium ion binding, epidermis 12. 205916_at S100A7 protein A7 (psoriasin 1) development <0.01 S100 calcium binding protein A8 (calgranulin calcium ion binding, extracellular 13. -

AQP3 and AQP5—Potential Regulators of Redox Status in Breast Cancer
molecules Review AQP3 and AQP5—Potential Regulators of Redox Status in Breast Cancer Lidija Milkovi´c and Ana Cipakˇ Gašparovi´c* Division of Molecular Medicine, Ruder¯ Boškovi´cInstitute, HR-10000 Zagreb, Croatia; [email protected] * Correspondence: [email protected]; Tel.: +385-1-457-1212 Abstract: Breast cancer is still one of the leading causes of mortality in the female population. Despite the campaigns for early detection, the improvement in procedures and treatment, drastic improvement in survival rate is omitted. Discovery of aquaporins, at first described as cellular plumbing system, opened new insights in processes which contribute to cancer cell motility and proliferation. As we discover new pathways activated by aquaporins, the more we realize the complexity of biological processes and the necessity to fully understand the pathways affected by specific aquaporin in order to gain the desired outcome–remission of the disease. Among the 13 human aquaporins, AQP3 and AQP5 were shown to be significantly upregulated in breast cancer indicating their role in the development of this malignancy. Therefore, these two aquaporins will be discussed for their involvement in breast cancer development, regulation of oxidative stress and redox signalling pathways leading to possibly targeting them for new therapies. Keywords: AQP3; AQP5; oxidative stress Citation: Milkovi´c,L.; Cipakˇ 1. Introduction Gašparovi´c,A. AQP3 and Despite the progress in research and treatment procedures, cancer still remains the AQP5—Potential Regulators of Redox leading cause of death. Today, cancer is targeted via different approaches which is deter- Status in Breast Cancer. Molecules mined by diagnosis, tumour marker expression, and specific mutations. -
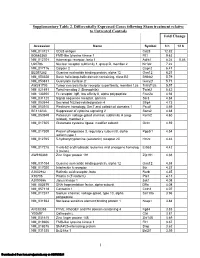
Supplementary Table 2
Supplementary Table 2. Differentially Expressed Genes following Sham treatment relative to Untreated Controls Fold Change Accession Name Symbol 3 h 12 h NM_013121 CD28 antigen Cd28 12.82 BG665360 FMS-like tyrosine kinase 1 Flt1 9.63 NM_012701 Adrenergic receptor, beta 1 Adrb1 8.24 0.46 U20796 Nuclear receptor subfamily 1, group D, member 2 Nr1d2 7.22 NM_017116 Calpain 2 Capn2 6.41 BE097282 Guanine nucleotide binding protein, alpha 12 Gna12 6.21 NM_053328 Basic helix-loop-helix domain containing, class B2 Bhlhb2 5.79 NM_053831 Guanylate cyclase 2f Gucy2f 5.71 AW251703 Tumor necrosis factor receptor superfamily, member 12a Tnfrsf12a 5.57 NM_021691 Twist homolog 2 (Drosophila) Twist2 5.42 NM_133550 Fc receptor, IgE, low affinity II, alpha polypeptide Fcer2a 4.93 NM_031120 Signal sequence receptor, gamma Ssr3 4.84 NM_053544 Secreted frizzled-related protein 4 Sfrp4 4.73 NM_053910 Pleckstrin homology, Sec7 and coiled/coil domains 1 Pscd1 4.69 BE113233 Suppressor of cytokine signaling 2 Socs2 4.68 NM_053949 Potassium voltage-gated channel, subfamily H (eag- Kcnh2 4.60 related), member 2 NM_017305 Glutamate cysteine ligase, modifier subunit Gclm 4.59 NM_017309 Protein phospatase 3, regulatory subunit B, alpha Ppp3r1 4.54 isoform,type 1 NM_012765 5-hydroxytryptamine (serotonin) receptor 2C Htr2c 4.46 NM_017218 V-erb-b2 erythroblastic leukemia viral oncogene homolog Erbb3 4.42 3 (avian) AW918369 Zinc finger protein 191 Zfp191 4.38 NM_031034 Guanine nucleotide binding protein, alpha 12 Gna12 4.38 NM_017020 Interleukin 6 receptor Il6r 4.37 AJ002942 -

Martin Steinhoff Dirk Roosterman, Tobias Goerge, Stefan W
Dirk Roosterman, Tobias Goerge, Stefan W. Schneider, Nigel W. Bunnett and Martin Steinhoff Physiol Rev 86:1309-1379, 2006. doi:10.1152/physrev.00026.2005 You might find this additional information useful... This article cites 963 articles, 265 of which you can access free at: http://physrev.physiology.org/cgi/content/full/86/4/1309#BIBL Medline items on this article's topics can be found at http://highwire.stanford.edu/lists/artbytopic.dtl on the following topics: Biochemistry .. Transient Receptor Potential Channel Biochemistry .. Endopeptidases Biochemistry .. Proteolytic Enzymes Oncology .. Inflammation Medicine .. Neurogenic Inflammation Physiology .. Nerves Updated information and services including high-resolution figures, can be found at: http://physrev.physiology.org/cgi/content/full/86/4/1309 Downloaded from Additional material and information about Physiological Reviews can be found at: http://www.the-aps.org/publications/prv This information is current as of February 8, 2008 . physrev.physiology.org on February 8, 2008 Physiological Reviews provides state of the art coverage of timely issues in the physiological and biomedical sciences. It is published quarterly in January, April, July, and October by the American Physiological Society, 9650 Rockville Pike, Bethesda MD 20814-3991. Copyright © 2005 by the American Physiological Society. ISSN: 0031-9333, ESSN: 1522-1210. Visit our website at http://www.the-aps.org/. Physiol Rev 86: 1309–1379, 2006; doi:10.1152/physrev.00026.2005. Neuronal Control of Skin Function: The Skin as a Neuroimmunoendocrine Organ DIRK ROOSTERMAN, TOBIAS GOERGE, STEFAN W. SCHNEIDER, NIGEL W. BUNNETT, AND MARTIN STEINHOFF Department of Dermatology, IZKF Mu¨nster, and Boltzmann Institute for Cell and Immunobiology of the Skin, University of Mu¨nster, Mu¨nster, Germany; and Departments of Surgery and Physiology, University of California, San Francisco, California I. -

Pflugers Final
CORE Metadata, citation and similar papers at core.ac.uk Provided by Serveur académique lausannois A comprehensive analysis of gene expression profiles in distal parts of the mouse renal tubule. Sylvain Pradervand2, Annie Mercier Zuber1, Gabriel Centeno1, Olivier Bonny1,3,4 and Dmitri Firsov1,4 1 - Department of Pharmacology and Toxicology, University of Lausanne, 1005 Lausanne, Switzerland 2 - DNA Array Facility, University of Lausanne, 1015 Lausanne, Switzerland 3 - Service of Nephrology, Lausanne University Hospital, 1005 Lausanne, Switzerland 4 – these two authors have equally contributed to the study to whom correspondence should be addressed: Dmitri FIRSOV Department of Pharmacology and Toxicology, University of Lausanne, 27 rue du Bugnon, 1005 Lausanne, Switzerland Phone: ++ 41-216925406 Fax: ++ 41-216925355 e-mail: [email protected] and Olivier BONNY Department of Pharmacology and Toxicology, University of Lausanne, 27 rue du Bugnon, 1005 Lausanne, Switzerland Phone: ++ 41-216925417 Fax: ++ 41-216925355 e-mail: [email protected] 1 Abstract The distal parts of the renal tubule play a critical role in maintaining homeostasis of extracellular fluids. In this review, we present an in-depth analysis of microarray-based gene expression profiles available for microdissected mouse distal nephron segments, i.e., the distal convoluted tubule (DCT) and the connecting tubule (CNT), and for the cortical portion of the collecting duct (CCD) (Zuber et al., 2009). Classification of expressed transcripts in 14 major functional gene categories demonstrated that all principal proteins involved in maintaining of salt and water balance are represented by highly abundant transcripts. However, a significant number of transcripts belonging, for instance, to categories of G protein-coupled receptors (GPCR) or serine-threonine kinases exhibit high expression levels but remain unassigned to a specific renal function. -

Beyond Water Homeostasis: Diverse Functional Roles of Mammalian Aquaporins Philip Kitchena, Rebecca E. Dayb, Mootaz M. Salmanb
CORE Metadata, citation and similar papers at core.ac.uk Provided by Aston Publications Explorer © 2015, Elsevier. Licensed under the Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International http://creativecommons.org/licenses/by-nc-nd/4.0/ Beyond water homeostasis: Diverse functional roles of mammalian aquaporins Philip Kitchena, Rebecca E. Dayb, Mootaz M. Salmanb, Matthew T. Connerb, Roslyn M. Billc and Alex C. Connerd* aMolecular Organisation and Assembly in Cells Doctoral Training Centre, University of Warwick, Coventry CV4 7AL, UK bBiomedical Research Centre, Sheffield Hallam University, Howard Street, Sheffield S1 1WB, UK cSchool of Life & Health Sciences and Aston Research Centre for Healthy Ageing, Aston University, Aston Triangle, Birmingham, B4 7ET, UK dInstitute of Clinical Sciences, University of Birmingham, Edgbaston, Birmingham B15 2TT, UK * To whom correspondence should be addressed: Alex C. Conner, School of Clinical and Experimental Medicine, University of Birmingham, Edgbaston, Birmingham B15 2TT, UK. 0044 121 415 8809 ([email protected]) Keywords: aquaporin, solute transport, ion transport, membrane trafficking, cell volume regulation The abbreviations used are: GLP, glyceroporin; MD, molecular dynamics; SC, stratum corneum; ANP, atrial natriuretic peptide; NSCC, non-selective cation channel; RVD/RVI, regulatory volume decrease/increase; TM, transmembrane; ROS, reactive oxygen species 1 Abstract BACKGROUND: Aquaporin (AQP) water channels are best known as passive transporters of water that are vital for water homeostasis. SCOPE OF REVIEW: AQP knockout studies in whole animals and cultured cells, along with naturally occurring human mutations suggest that the transport of neutral solutes through AQPs has important physiological roles. Emerging biophysical evidence suggests that AQPs may also facilitate gas (CO2) and cation transport. -

Characterization of Membrane Proteins: from a Gated Plant Aquaporin to Animal Ion Channel Receptors
Characterization of Membrane Proteins: From a gated plant aquaporin to animal ion channel receptors Survery, Sabeen 2015 Link to publication Citation for published version (APA): Survery, S. (2015). Characterization of Membrane Proteins: From a gated plant aquaporin to animal ion channel receptors. Department of Biochemistry and Structural Biology, Lund University. Total number of authors: 1 General rights Unless other specific re-use rights are stated the following general rights apply: Copyright and moral rights for the publications made accessible in the public portal are retained by the authors and/or other copyright owners and it is a condition of accessing publications that users recognise and abide by the legal requirements associated with these rights. • Users may download and print one copy of any publication from the public portal for the purpose of private study or research. • You may not further distribute the material or use it for any profit-making activity or commercial gain • You may freely distribute the URL identifying the publication in the public portal Read more about Creative commons licenses: https://creativecommons.org/licenses/ Take down policy If you believe that this document breaches copyright please contact us providing details, and we will remove access to the work immediately and investigate your claim. LUND UNIVERSITY PO Box 117 221 00 Lund +46 46-222 00 00 Printed by Media-Tryck, Lund University 2015 SURVERY SABEEN Characterization of Membrane Proteins - From a gated plant aquaporin to animal ion channel -

Review—Current Concepts in Inflammatory Skin Diseases
International Journal of Molecular Sciences Review Review—Current Concepts in Inflammatory Skin Diseases Evolved by Transcriptome Analysis: In-Depth Analysis of Atopic Dermatitis and Psoriasis Julius Schwingen * , Mustafa Kaplan and Florian C. Kurschus * Department of Dermatology, Heidelberg University Hospital, 69120 Heidelberg, Germany; [email protected] * Correspondence: [email protected] (J.S.); fl[email protected] (F.C.K.) Received: 16 December 2019; Accepted: 16 January 2020; Published: 21 January 2020 Abstract: During the last decades, high-throughput assessment of gene expression in patient tissues using microarray technology or RNA-Seq took center stage in clinical research. Insights into the diversity and frequency of transcripts in healthy and diseased conditions provide valuable information on the cellular status in the respective tissues. Growing with the technique, the bioinformatic analysis toolkit reveals biologically relevant pathways which assist in understanding basic pathophysiological mechanisms. Conventional classification systems of inflammatory skin diseases rely on descriptive assessments by pathologists. In contrast to this, molecular profiling may uncover previously unknown disease classifying features. Thereby, treatments and prognostics of patients may be improved. Furthermore, disease models in basic research in comparison to the human disease can be directly validated. The aim of this article is not only to provide the reader with information on the opportunities of these techniques, but to outline potential pitfalls and technical limitations as well. Major published findings are briefly discussed to provide a broad overview on the current findings in transcriptomics in inflammatory skin diseases. Keywords: inflammatory skin diseases; transcriptomics; RNA-Seq; microarray; scRNA-Seq; psoriasis; atopic dermatitis; contact dermatitis; acne; eczema 1. -

Mechanisms of Aquaporin-Facilitated Cancer Invasion and Metastasis
REVIEW published: 25 April 2018 doi: 10.3389/fchem.2018.00135 Mechanisms of Aquaporin-Facilitated Cancer Invasion and Metastasis Michael L. De Ieso and Andrea J. Yool* Department of Physiology, Adelaide Medical School, University of Adelaide, Adelaide, SA, Australia Cancer is a leading cause of death worldwide, and its incidence is rising with numbers expected to increase 70% in the next two decades. The fact that current mainline treatments for cancer patients are accompanied by debilitating side effects prompts a growing demand for new therapies that not only inhibit growth and proliferation of cancer cells, but also control invasion and metastasis. One class of targets gaining international attention is the aquaporins, a family of membrane-spanning water channels with diverse physiological functions and extensive tissue-specific distributions in humans. Aquaporins−1,−2,−3,−4,−5,−8, and−9 have been linked to roles in cancer invasion, and metastasis, but their mechanisms of action remain to be fully defined. Aquaporins are implicated in the metastatic cascade in processes of angiogenesis, cellular dissociation, migration, and invasion. Cancer invasion and metastasis are proposed to be potentiated by aquaporins in boosting tumor angiogenesis, enhancing cell volume regulation, regulating cell-cell and cell-matrix adhesions, interacting with actin cytoskeleton, regulating proteases and extracellular-matrix degrading molecules, Edited by: Graça Soveral, contributing to the regulation of epithelial-mesenchymal transitions, and interacting Universidade de Lisboa, Portugal with signaling pathways enabling motility and invasion. Pharmacological modulators of Reviewed by: aquaporin channels are being identified and tested for therapeutic potential, including Ali Mobasheri, compounds derived from loop diuretics, metal-containing organic compounds, plant University of Surrey, United Kingdom Miriam Echevarria Irusta, natural products, and other small molecules.