USE of an OXYGEN RESERVOIR with a POCKET MASK by Paul Botkin
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Mapping the Use of Simulation in Prehospital Care – a Literature Review Anna Abelsson1*, Ingrid Rystedt1, Björn-Ove Suserud2 and Lillemor Lindwall1
Abelsson et al. Scandinavian Journal of Trauma, Resuscitation and Emergency Medicine 2014, 22:22 http://www.sjtrem.com/content/22/1/22 REVIEW Open Access Mapping the use of simulation in prehospital care – a literature review Anna Abelsson1*, Ingrid Rystedt1, Björn-Ove Suserud2 and Lillemor Lindwall1 Abstract Background: High energy trauma is rare and, as a result, training of prehospital care providers often takes place during the real situation, with the patient as the object for the learning process. Such training could instead be carried out in the context of simulation, out of danger for both patients and personnel. The aim of this study was to provide an overview of the development and foci of research on simulation in prehospital care practice. Methods: An integrative literature review were used. Articles based on quantitative as well as qualitative research methods were included, resulting in a comprehensive overview of existing published research. For published articles to be included in the review, the focus of the article had to be prehospital care providers, in prehospital settings. Furthermore, included articles must target interventions that were carried out in a simulation context. Results: The volume of published research is distributed between 1984- 2012 and across the regions North America, Europe, Oceania, Asia and Middle East. The simulation methods used were manikins, films, images or paper, live actors, animals and virtual reality. The staff categories focused upon were paramedics, emergency medical technicians (EMTs), medical doctors (MDs), nurse and fire fighters. The main topics of published research on simulation with prehospital care providers included: Intubation, Trauma care, Cardiac Pulmonary Resuscitation (CPR), Ventilation and Triage. -

Resuscitation and Defibrillation
AARC GUIDELINE: RESUSCITATION AND DEFIBRILLATION AARC Clinical Practice Guideline Resuscitation and Defibrillation in the Health Care Setting— 2004 Revision & Update RAD 1.0 PROCEDURE: signs, level of consciousness, and blood gas val- Recognition of signs suggesting the possibility ues—included in those conditions are or the presence of cardiopulmonary arrest, initia- 4.1 Airway obstruction—partial or complete tion of resuscitation, and therapeutic use of de- 4.2 Acute myocardial infarction with cardio- fibrillation in adults. dynamic instability 4.3 Life-threatening dysrhythmias RAD 2.0 DESCRIPTION/DEFINITION: 4.4 Hypovolemic shock Resuscitation in the health care setting for the 4.5 Severe infections purpose of this guideline encompasses all care 4.6 Spinal cord or head injury necessary to deal with sudden and often life- 4.7 Drug overdose threatening events affecting the cardiopul- 4.8 Pulmonary edema monary system, and involves the identification, 4.9 Anaphylaxis assessment, and treatment of patients in danger 4.10 Pulmonary embolus of or in frank arrest, including the high-risk de- 4.11 Smoke inhalation livery patient. This includes (1) alerting the re- 4.12 Defibrillation is indicated when cardiac suscitation team and the managing physician; (2) arrest results in or is due to ventricular fibril- using adjunctive equipment and special tech- lation.1-5 niques for establishing, maintaining, and moni- 4.13 Pulseless ventricular tachycardia toring effective ventilation and circulation; (3) monitoring the electrocardiograph and recogniz- -

OPITO Medical Emergency Response and Planning Requirements (Implementation Date 8Th November 2019)
OPITO Medical Emergency Response and Planning Requirements (Implementation date 8th November 2019) OPITO Medical Emergency Response and Planning Requirements © OPITO The content of this document was developed and reviewed in 2015 by OPITO to improve Emergency Response Arrangements based on accepted industry best practices. It was updated in 2019 to reflect a more risk-based approach towards requirements for each type of Training Centre. Guidance on this document is available by contacting OPITO. © OPITO All rights reserved. No part of this publication may be reproduced, stored in a retrieval or information storage system, or transmitted, in any form or by any means, mechanical, photocopying, recording or otherwise, without the prior permission in writing of the publishers. AMENDMENTS AMENDMENT & DATE PAGES CHANGES CHECKED BY APPROVED MADE BY BY Revision 0 released January Global Technical Industry and Global 2016 Coordinator OPITO Approvals Technical Department Director Rev 1 released August 2019 Approvals Approvals Director, All QA Department Standards Director Any amendments made to this document by OPITO will be recorded above. Revision 1 (August 2019) Page 2 of 29 OPITO Medical Emergency Response and Planning Requirements © OPITO CONTENTS INTRODUCTION ........................................................................................................................ 4 SECTION 1 - RISK BASED PLANNING ..................................................................................... 7 1.1 MEDICAL EMERGENCY RESPONSE AND PLANNING -
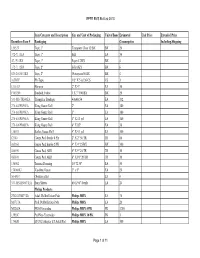
EPFR EMS Bid List 2010
EPFR EMS Bid List 2010 Item Category and Description Size and Unit of Packaging Unit of Issue Estimated Unit Price Extended Price Boundtree Item # Bandaging Consumption Including Shipping 151527 Tape, 1" Transpore Clear 12/BX BX 20 372-7111EA Tape, 1" Silk EA 36 47-1914BX Tape, 1" Paper 12/BX BX 4 372-7112BX Tape, 2" Silk 6/BX BX 6 625-2045033BX Tape, 2" Waterproof 6/BX BX 4 105BLF Hy-Tape 1/2" X 5 yd 36/CS CS 1 1211-209 Hemcon 2" X 4" EA 16 F165200 Bandaid, Fabric 1 X 3" 100/BX BX 20 533-MS-TRI40EA Triangular Bandage 40x40x54 EA 132 276-602PB96EA Kling Gauze Roll 2" EA 180 276-603PB96EA Kling Gauze Roll 3" EA 180 276-604PB96EA Kling Gauze Roll 4" X 4.1 yd EA 180 276-606PB48EA Kling Gauze Roll 6" X 85" EA 36 150031 Kerlex Gauze Roll 4" X 4.1 yd EA 100 J2540 Gauze Pad, Sterile 8 Ply 2" X 2" 50/TR TR 80 085360 Gauze Pad, Sterile 2/PK 4" X 4" 25/BX BX 100 085590 Gauze Pad, ABD 5" X 9" 25/TR TR 10 085810 Gauze Pad, ABD 8" X 10" 20/TR TR 10 150062 Trauma Dressing 10" X 30" EA 50 150066K1 Vaseline Gauze 3" x 9" EA 20 56-0967 Obstetrics Kit EA 4 533-MS-BS0033EA Burn Sheets 60 X 96" Sterile EA 24 Philips Products 2742-ATM3713A Adult Defibrillation Pads Philips MRX EA 70 M3717A Pedi Defibrillation Pads Philips MRX EA 20 M2202A EKG Electrodes Philips MRX 5/PK PK 3200 13955C Ped/Neo Electrodes Philips MRX 30/PK PK 1 174620 ETCO2 Adapter ET Adult/Ped Philips MRX EA 100 Page 1 of 11 EPFR EMS Bid List 2010 M1923A ETCO2 Adapter ET Ped/Infant Philips MRX EA 10 177653 ETCO2 Adapter NC Adult Philips MRX EA 200 M2520A ETCO2 Adapter NC Pediatric Philips -

Washington State First Responder (EMR) Field Protocols
WASHINGTON STATE DEPARTMENT OF HEALTH HEALTH SYSTEMS QUALITY ASSURANCE DIVISION OFFICE OF EMERGENCY MEDICAL AND TRAUMA PREVENTION FIRST RESPONDER FIELD PROTOCOLS DOH Pub. 530-001, (Revised September 2005) These protocols have been reviewed and endorsed by the Medical Program Directors and the Department of Health, Licensing and Certification Advisory Committee. For questions or comments, contact: Licensing and Certification Section Office of Emergency Medical and Trauma Prevention P.O. Box 47853 Olympia, Washington 98504-7853 360-236-2840 These First Responder Field Protocols are State Protocols that establish the standard for field performance. EMS County Medical Program Directors may NOT have protocols that vary from these without specific written approval from the Department of Health. Any deviation from these protocols must be identified to and approved in writing by the Department of Health. THESE FIELD PROTOCOLS WERE DEVELOPED AND WRITTEN WITH THE ASSISTANCE OF THE FOLLOWING INDIVIDUALS: WASHINGTON STATE EM/TP PROTOCOL WORK GROUP Nina Conn Patty Courson Kenny Karnes Dane Kessler Richard Kness Marc Muhr Jim Palmer Terry Patton Jack Pinza Lynn Wittwer, MD 2 Introduction These protocols were developed by the Washington State Protocol Work Group and represent the consolidation of recommendations for emergency pre-hospital patient care from many local and national sources. The assessment information in the First Responder General Orders is intended to be considered with all protocols. These protocols are intended to: 1. Provide a guide to the appropriate emergency medical care procedures to be employed by EMS personnel while working under the direction of the County Medical Program Director; 2. Assist in the standardization of pre-hospital care in Washington State; 3. -

Management of Airway Emergencies (1995)
Reprinted from the July 1995 issue of RESPIRATORY CARE [Respir Care 1995;40(7):749–760] AARC Clinical Practice Guideline Management of Airway Emergencies MAE 1.0 PROCEDURE: Recognition of signs of an impending or actual airway emergency. Initial treatment and continued management of airway emergencies to minimize the likelihood of adverse outcomes, in adults, children, and infants. MAE 2.0 DESCRIPTION/DEFINITION: Management of airway emergencies (MAE) for the purpose of this guideline encompasses all care necessary to deal with sudden and often life-threatening events affecting natural and artificial airways and involves the identification, assessment, and treatment of patients in danger of losing or not being able to maintain an adequate airway, including the newborn. This includes (1) identification of the causes of airway emergencies; (2) management of airway emergencies prior to tracheal intubation; (3) use of adjunctive equipment and special techniques for establishing, maintaining, and monitoring effective ventilation; (4) translaryngeal tracheal intubation, including nasal and oral tracheal intubation; (5) transtracheal catheter ventilation, (6) percutaneous dilational cricothyrotomy, and; (7) surgical cricothyrotomy. MAE 3.0 SETTING: The guideline appliesRETIRED to a variety of settings including but not limited to hospitals and pre- or interhospital transport. MAE 4.0 INDICATIONS: 4.1 Conditions requiring management of the airway, in general, are impending or actual (1) airway compromise, (2) respiratory failure, and (3) need -

The Efficiency of Bag-Valve Mask Ventilations by Medical First Responders and Basic Emergency Medical Technicians
California State University, San Bernardino CSUSB ScholarWorks Theses Digitization Project John M. Pfau Library 2003 The efficiency of bag-valve mask ventilations by medical first responders and basic emergency medical technicians John Vincent Commander Follow this and additional works at: https://scholarworks.lib.csusb.edu/etd-project Part of the Vocational Education Commons Recommended Citation Commander, John Vincent, "The efficiency of bag-valve mask ventilations by medical first responders and basic emergency medical technicians" (2003). Theses Digitization Project. 2310. https://scholarworks.lib.csusb.edu/etd-project/2310 This Project is brought to you for free and open access by the John M. Pfau Library at CSUSB ScholarWorks. It has been accepted for inclusion in Theses Digitization Project by an authorized administrator of CSUSB ScholarWorks. For more information, please contact [email protected]. THE EFFICIENCY OF BAG-VALVE MASK VENTILATIONS BY MEDICAL FIRST RESPONDERS AND BASIC EMERGENCY MEDICAL TECHNICIANS A Project Presented to the Faculty of California State University, San Bernardino In Partial Fulfillment of the Requirements for the Degree Master of Arts in Education: Career and Technical Education by John Vincent Commander September 2003 THE EFFICIENCY OF BAG-VALVE MASK VENTILATIONS BY MEDICAL FIRST RESPONDERS AND BASIC EMERGENCY MEDICAL TECHNICIANS A Project Presented to the Faculty of California State University, San Bernardino by John Vincent Commander September 2003 Approved by: © 2003 John Vincent Commander ABSTRACT• Bag-valve mask (BVM) ventilation maintains a patient's oxygenation and ventilation until a more definitive artificial airway can be established. In the prehospital setting of a traffic collision-or • medical aid scene this is performed by an Emergency Medical Technician or medical first responder. -

ABC of Resuscitation
Using over 100 illustrations and clear explanation, this fifth edition of the ABC of Resuscitation ABC FIFTH OF RESUSCITATION EDITION is a comprehensive and accessible guide containing practical information on all aspects of resuscitation including the latest advances in drugs, automated external defibrillators, and advanced life support. It has been revised in accordance with the latest guidelines from the European Resuscitation Council. Chapters include: ABC • Basic life support OF • Automated external defibrillators • Resuscitation in pregnancy • Resuscitation of infants and children • Cardiopulmonary resuscitation in primary care • Resuscitation of the patient with major trauma RESUSCITATION • Drugs and their delivery • The ethics of resuscitation Fifth edition The ABC of Resuscitation is an invaluable text for medical and paramedical practitioners, students, and all healthcare workers who need up to date information on resuscitation issues. Related titles from BMJ Books ABC of Intensive Care Acute Medical Emergencies Advanced Paediatric Life Support Major Incident Medical Management and Support Major Incident Management System Safe Transfer and Retrieval of Patients Special Incident Medical Management and Support Paediatric and Neonatal Critical Care Transport Pre-Hospital Paediatric Life Support Resuscitation Rules Colquhoun, Handley and Evans General Practice Edited by M C Colquhoun, A J Handley and T R Evans www.bmjbooks.com ABC OF RESUSCITATION Fifth Edition ABC OF RESUSCITATION Fifth Edition Edited by M C Colquhoun Chairman of the Resuscitation Council (UK) A J Handley Past chairman of the Resuscitation Council (UK) and Chairman of ILCOR working party on basic life support and T R Evans Past chairman of the Resuscitation Council (UK) © BMJ Publishing Group 2004 All rights reserved. -

Battlefield Advances Trauma Life Support (BATLS) Chapters 3 and 4
J R Army Med Corps 2000; 146: 215-227 J R Army Med Corps: first published as 10.1136/jramc-146-03-12 on 1 October 2000. Downloaded from BATLS Battlefield Advanced Trauma Life Support (BATLS) logistic capabilities (JSP 110). In these CHAPTER 3 TRIAGE circumstances the aim of the medical services must be to give care to the greatest Aim benefit of the largest number - that is ‘to do 0301. On successfully completing this most for the most’. topic you will have a sound understanding 0308. The term mass casualties is of how to prioritise casualties for treatment reserved for a situation when medical and evacuation, so that the survival of the resources are overwhelmed.When resources maximum number is ensured. are adequate, the incident is said to be ‘compensated’. In a military setting, an Introduction ‘uncompensated’ situation may exist 0302. The management of a single temporarily or over a prolonged period. It seriously injured casualty in peacetime may be appropriate for the local military or civilian practice is frequently commander to introduce mass casualty problematic. On the battlefield, problems triage without a formal declaration having are compounded by: environment, difficult been made by a higher authority. terrain and tactical constraints. The 0309. The triage system in an situation is even more difficult when faced uncompensated situation thus becomes; with large numbers of casualties. • P1 - Immediate Treatment. Those needing 0303. If a system for prioritisation of care emergency life-saving treatment. of the injured is not in place, many Procedures should not be time salvageable casualties may die consuming and concern only those with a unnecessarily.Triage (from the French verb high chance of good quality survival. -

Basic Life Support Ventilation in Mountain Rescue
ICAR REC M 0021 E International Commission for Alpine Rescue Commission for Mountain Emergency Medicine Recommendation REC M 0021 of the Commission for Mountain Emergency Medicine of January 3, 2007 about Basic Life Support Ventilation in Mountain Rescue 1 BASIC LIFE SUPPORT VENTILATION IN MOUNTAIN RESCUE Official recommendations of the International Commission for Mountain Emergency Medicine (ICAR MEDCOM) Peter Paal MDa,b,c,*, John Ellerton MRCGPc,d, Günther Sumann MDa,c, Florian Demetz MDb,c,e, Peter Mair MDa,c, Hermann Brugger MDb,c,f a* Department of Anesthesiology and Division of General and Surgical Critical Care Medicine, Innsbruck Medical University, Anichstrasse 35, A-6020 Innsbruck, Austria; E-mail: [email protected], [email protected] and [email protected] b Mountain Rescue Service provided by the South Tyrolean Alpine Association, Brauereistrasse 18, 39010 Vilpian, Italy c International Commission for Mountain Emergency Medicine, ICAR MEDCOM d Mountain Rescue Council England and Wales, Pinfold, Nicholson Lane, Penrith, Cumbria CA11 7UL, England; E-mail: [email protected] e Clinic for Anesthesiology, LMU University Munich, Marchioninistrasse 15, 81377 Munich, Germany; E-mail: [email protected] f President of ICAR MEDCOM, Europastrasse 17, I-39031 Bruneck, Italy ; E-mail: [email protected] *Corresponding author: Dr. Peter Paal, Department of Anesthesiology and Critical Care Medicine, Innsbruck Medical University, Anichstrasse 35, 6020 Innsbruck, Austria; Phone +43-512-504-80448; Fax: +43-512-504-22450; E-mail: [email protected] This article reflects the consensus of opinion of the International Commission for Mountain Emergency Medicine which has full responsibility for the content. -
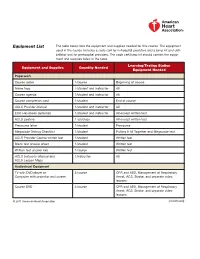
Acls-Equipment-List.Pdf
Equipment List The table below lists the equipment and supplies needed for this course. The equipment used in the course includes a code cart for in-hospital providers and a jump kit and defi- brillator unit for prehospital providers. The code cart/jump kit should contain the equip- ment and supplies listed in the table. Learning/Testing Station Equipment and Supplies Quantity Needed Equipment Needed Paperwork Course roster 1/course Beginning of course Name tags 1/student and instructor All Course agenda 1/student and instructor All Course completion card 1/student End of course ACLS Provider Manual 1/student and instructor All ECC Handbook (optional) 1/student and instructor All except written test ACLS posters 1 set/class All except written test Precourse letter 1/student Precourse Megacode Testing Checklist 1/student Putting It All Together and Megacode test ACLS Provider Course written test 1/student Written test Blank test answer sheet 1/student Written test Written test answer key 1/course Written test ACLS Instructor Manual and 1/instructor All ACLS Lesson Maps Audiovisual Equipment TV with DVD player or 2/course CPR and AED, Management of Respiratory Computer with projector and screen Arrest, ACS, Stroke, and separate video lessons Course DVD 2/course CPR and AED, Management of Respiratory Arrest, ACS, Stroke, and separate video lessons © 2011 American Heart Association (continued) 90-1011_ACLS_Part_1.indd 4 12/22/10 2:57 PM (continued) Learning/Testing Station Equipment and Supplies Quantity Needed Equipment Needed CPR and AED -

American Red Cross Guidelines Highlights 2020 Resuscitation Suite BLS, ALS, PALS
American Red Cross Guidelines Highlights 2020 Resuscitation Suite BLS, ALS, PALS You Now Have a Choice in Resuscitation Education Healthcare providers now have a scientifically equivalent and educationally superior choice from the first provider of resuscitation and first aid training in the United States. Flexible Learning That’s Scientifically Equivalent and Educationally Superior American Red Cross Resuscitation SuiteTM courses deliver the science that will save lives while streamlining the education experience. Our BLS, ALS, and PALS courses will provide the solutions you need while saving you time and money. • Adaptive learning lets participants test out of sections in Blended Learning by demonstrating competency. • Shorter overall course times resulting from more efficient course designs and personalized learning. • Real healthcare providers demonstrate content in real hospital settings with no gamification. • Clinical scenarios specific to those that might be encountered by EMS providers in field settings. • Focus is on critical thinking, decision-making, and team concepts. • Online/streaming videos available at no additional cost. • Digital student certificate immediately available. A better solution at • Feedback devices recommended but not mandatory. • ADA compliant for Blended Learning students. a better price. • Access Blended Learning on any device—computer, tablet, or mobile. Go to Red Cross courses offer a curriculum based on the same ILCOR science and ECC guidelines as other resuscitation courses. redcross.org/healthcare to learn more. A Full Portfolio to Meet All Needs • Certification courses: BLS, ALS, PALS in Instructor-Led and Blended Learning formats. • Streamlined certification course renewal options for experienced BLS, ALS, PALS providers: Review Option (brief skills review before testing) and Challenge Option (test-only).