Sinus Node Dysfunction in Acute Myocardial Infarction
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Sinus Node Ischemia—A Unique Presentation
International Journal of Clinical Medicine, 2015, 6, 50-54 Published Online January 2015 in SciRes. http://www.scirp.org/journal/ijcm http://dx.doi.org/10.4236/ijcm.2015.61007 Sinus Node Ischemia—A Unique Presentation Jwalit Morakhia1, Padmakumar Ramachandran1, Naveen Chandra Ganiga Sanjeeva1, Harikrishna Damodaran2, Shivani Kothari3, Ashok Thakkar3 1Department of Cardiology, Kasturba Medical College & Hospital, Karnataka, India 2Department of Cardiology, Pariyaram Medical College, Kerala, India 3Department of Clinical Trials, Sahajanand Medical Technologies Pvt. Ltd., Gujarat, India Email: [email protected] Received 27 December 2014; accepted 13 January 2015; published 20 January 2015 Copyright © 2015 by authors and Scientific Research Publishing Inc. This work is licensed under the Creative Commons Attribution International License (CC BY). http://creativecommons.org/licenses/by/4.0/ Abstract Sinus node dysfunction, as the sole manifestation of an acute coronary syndrome, is rare. We re- port a case of ischemic dysfunction of the sinus node in a patient who had previously undergone coronary artery bypass grafting for triple vessel disease. Intermittent rest angina with a junctional rhythm was noted in spite of patent grafts to all three vessels, which resolved after percutaneous revascularization of the right coronary artery. Keywords Sinus Node, Angina, Acute Coronary Syndrome, Thrombus Aspiration 1. Introduction Patients presenting with acute coronary syndromes, with atypical symptoms, are frequently misdiagnosed and under-treated. Embolic phenomena are sometimes overlooked by interventionalists as percutaneous coronary intervention is a specialty which primarily focuses on stenosis and occlusions [1]. We report a case of reversible sinus node dysfunction in the unique setting of post-coronary artery bypass grafting (CABG) status with patent grafts. -

An Extremely Rare Cause of Wolff-Parkinson
108 Erciyes Med J 2019; 41(1): 108–10 • DOI: 10.14744/etd.2018.18165 An Extremely Rare Cause of Wolff-Parkinson-White Syndrome: Rhabdomyoma in Association With Tuberous Sclerosis CASE REPORT Özlem Elkıran , Cemşit Karakurt , Damla İnce ABSTRACT Rhabdomyomas are the most common primary cardiac tumors in infants and children. They are usually associated with tuberous sclerosis (TS). As the tumors tend to regress spontaneously, surgical intervention is not usually performed unless they become obstructive or cause incessant arrhythmias. We report an extremely rare case of rhabdomyoma serving as a substrate for Wolff-Parkinson-White (WPW) syndrome and intractable supraventricular tachycardia accompanied by TS. Our case is particularly interesting because it was diagnosed prenatally. The signs of WPW syndrome disappeared from the elec- trocardiogram with the regression of the tumor. Keywords: Wolff-Parkinson-White Syndrome, child, rhabdomyoma INTRODUCTION Rhabdomyomas are the most common cardiac tumors in infants and children, and they are closely related with tuberous sclerosis (TS). A significant part of rhabdomyomas is asymptomatic, and they regress on follow-up. However, symptoms of cardiac failure, arrhythmias, and obstruction can be observed depending on their location in the heart. They require urgent medical or surgical treatment (1, 2). Cite this article as: Elkıran Ö, Karakurt C, İnce D. An Extremely Rhabdomyoma-related arrhythmias are reported as premature atrial and ventricular contractions, supraventricular Rare Cause of and ventricular tachycardia, sinus node dysfunction, atrioventricular block, and Wolff-Parkinson-White (WPW) Wolff-Parkinson-White syndrome (1, 3, 4). There are only a few studies of WPW syndrome occurring in association with TS, with and Syndrome: Rhabdomyoma in Association With without rhabdomyoma. -
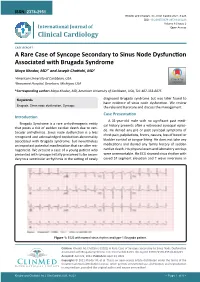
A Rare Case of Syncope Secondary to Sinus Node Dysfunction Associated with Brugada Syndrome Maya Khodor, MD1* and Joseph Chattahi, MD2
ISSN: 2378-2951 Khodor and Chattahi. Int J Clin Cardiol 2021, 8:223 DOI: 10.23937/2378-2951/1410223 Volume 8 | Issue 2 International Journal of Open Access Clinical Cardiology CASE REPORT A Rare Case of Syncope Secondary to Sinus Node Dysfunction Associated with Brugada Syndrome Maya Khodor, MD1* and Joseph Chattahi, MD2 1 American University of Caribbean, USA Check for 2Beaumont Hospital, Dearborn, Michigan, USA updates *Corresponding author: Maya Khodor, MD, American University of Caribbean, USA, Tel: 407-353-8875 diagnosed Brugada syndrome but was later found to Keywords have evidence of sinus node dysfunction. We review Brugada, Sinus node dysfunction, Syncope the relevant literature and discuss the management. Case Presentation Introduction A 31-year-old male with no significant past medi- Brugada Syndrome is a rare arrhythmogenic entity cal history presents after a witnessed syncopal episo- that poses a risk of sudden cardiac death due to ven- de. He denied any pre or post syncopal symptoms of tricular arrhythmias. Sinus node dysfunction is a less chest pain, palpitations, fevers, nausea, loss of bowel or recognized and acknowledged conduction abnormality associated with Brugada syndrome, but nevertheless bladder control or tongue biting. He does not take any an important potential manifestation that can alter ma- medications and denied any family history of sudden nagement. We present a case of a young patient who cardiac death. His physical exam and laboratory workup presented with syncope initially presumed to be secon- were unremarkable. His ECG showed sinus rhythm with dary to a ventricular arrhythmia in the setting of newly coved ST segment elevation and T wave inversions in Figure 1: ECG with normal sinus rhythm and type-1 Brugada pattern. -

Sick Sinus Syndrome After the Maze Procedure Performed
ORIGINAL RESEARCH Sick Sinus Syndrome After the Maze Procedure Performed Concomitantly With Mitral Valve Surgery Min Soo Cho, MD; Ran Heo, MD; Xin Jin, MD; Jung-Bok Lee, PhD; Sahmin Lee, MD, PhD; Dae-Hee Kim, MD, PhD; Joon Bum Kim, MD, PhD; Jun Kim, MD, PhD; Sung-Ho Jung, MD, PhD; Suk Jung Choo, MD, PhD; Jong-Min Song, MD, PhD; Gi-Byoung Nam, MD, PhD; Kee-Joon Choi, MD, PhD; Duk-Hyun Kang, MD, PhD; Cheol Hyun Chung, MD, PhD; Jae Won Lee, MD, PhD; You-Ho Kim, MD, PhD; Jae-Kwan Song, MD, PhD Background-—To characterize the development of sick sinus syndrome (SSS) after the additive maze procedure (MP) during mitral valve surgery. Methods and Results-—Follow-up data (median, 3.6 years) of 750 patients with a prevalence of rheumatic cause of 57.6% were analyzed. SSS occurred in 35 patients with a time-dependent increase: the incidence rates at 1, 2, and 4 years after surgery were 2.9%, 3.7%, and 4.3%, respectively. The additive MP showed higher risks of SSS development (hazard ratio, 7.44; 95% confidence interval, 3.45–16.05; P<0.001) and pacemaker implantation (hazard ratio, 3.61; 95% confidence interval, 1.95–6.67; P<0.001). Patients who developed SSS showed higher 4-year rates of clinical events (death, stroke, and hospital admission) (67.5Æ8.5% versus 33.0Æ1.9%; P<0.001). After adjustment for age and preoperative peak systolic pulmonary artery pressure, the lesion extent (biatrial versus left atrial MP), not the underlying cause (rheumatic versus nonrheumatic), was independently associated with SSS development (hazard ratio, 3.58; 95% confidence interval, 1.08–11.86; P=0.037). -

Management of Asymptomatic Arrhythmias
Europace (2019) 0, 1–32 EHRA POSITION PAPER doi:10.1093/europace/euz046 Downloaded from https://academic.oup.com/europace/advance-article-abstract/doi/10.1093/europace/euz046/5382236 by PPD Development LP user on 25 April 2019 Management of asymptomatic arrhythmias: a European Heart Rhythm Association (EHRA) consensus document, endorsed by the Heart Failure Association (HFA), Heart Rhythm Society (HRS), Asia Pacific Heart Rhythm Society (APHRS), Cardiac Arrhythmia Society of Southern Africa (CASSA), and Latin America Heart Rhythm Society (LAHRS) David O. Arnar (Iceland, Chair)1*, Georges H. Mairesse (Belgium, Co-Chair)2, Giuseppe Boriani (Italy)3, Hugh Calkins (USA, HRS representative)4, Ashley Chin (South Africa, CASSA representative)5, Andrew Coats (United Kingdom, HFA representative)6, Jean-Claude Deharo (France)7, Jesper Hastrup Svendsen (Denmark)8,9, Hein Heidbu¨chel (Belgium)10, Rodrigo Isa (Chile, LAHRS representative)11, Jonathan M. Kalman (Australia, APHRS representative)12,13, Deirdre A. Lane (United Kingdom)14,15, Ruan Louw (South Africa, CASSA representative)16, Gregory Y. H. Lip (United Kingdom, Denmark)14,15, Philippe Maury (France)17, Tatjana Potpara (Serbia)18, Frederic Sacher (France)19, Prashanthan Sanders (Australia, APHRS representative)20, Niraj Varma (USA, HRS representative)21, and Laurent Fauchier (France)22 ESC Scientific Document Group: Kristina Haugaa23,24, Peter Schwartz25, Andrea Sarkozy26, Sanjay Sharma27, Erik Kongsga˚rd28, Anneli Svensson29, Radoslaw Lenarczyk30, Maurizio Volterrani31, Mintu Turakhia32, -

Management for a Girl with LQTS and Sinus Bradycardia
2015 춘계통합학술대회 Management for a Girl With LQTS and Sinus Bradycardia 아주 의대 황 교 승 Management for a Girl With Long QT syndrome (LQTS) and Sinus Bradycardia Management for a Girl With LQTS and Sinus Bradycardia Action Potential and Electrocardiogram Normal Values for Durations of ECG Waves and Intervals in Adults Braunwald’s Heart Disease, 8th The corrected QT interval (QTc)= QT interval/√RR (Bazett’s formula) Congenital LQTS Historical features • Syncope • Congenital deafness • Family history of long QT syndrome • Unexplained sudden death in family member b age 30 ECG features • Prolonged QTc interval • Torsades de pointes • T-wave alternans • Notched T-waves in 3 or more leads • Bradycardia * The best example of genotype-phenotype correlation Notched T Waves T Wave Alternans Eur Heart J. 2013 Molecular Basis of LQTS J Am Coll Cardiol. 2013 July 16; 62(3): 169–180 P J Schwartz Circulation. 1993;88:782-784 European Heart Journal (2013) 34, 3109–3116 LQTS Diagnosis Europace (2013) 15, 1389–1406 Distribution of QTc Values Among Individuals With and without LQTS Circulation. 2007;115:2613-2620 Epinephrine QT Stress Test * 25% to 50% of patients with LQT1, LQT2, or LQT3: nondiagnostic resting QTc Circulation. 2006;113:1385-1392 * One-third of patients with LQTS: normal QT interval on at least one ECG Circulation 2007;115:2613 1. A 25-minute infusion protocol (0.025 to 0.3 g · kg1 · min1). Circulation. 2006;113:1385-1392 2. A bolus injection of epinephrine (0.1 g/kg)--- continuous infusion (0.1 g/kg/min) Heart Rhythm (2004) 3, 276–283 Diagnostic Outcome of LQTS Referral Cohort Circulation. -

Normal, Skipped, Or Irregular Heart Beats: Does My Heart Rate Determine My Fate?
Normal, Skipped, or Irregular Heart Beats: Does my Heart Rate Determine My Fate? Gregory M Marcus, MD, MAS Professor of Medicine University of California, San Francisco Disclosures • Research: – NIH – PCORI – TRDRP – Medtronic – Jawbone – Eight Sleep – Baylis • Consulting and Equity: – InCarda Therapeutics – Talaria Therapeutics Disclaimer • This is a lot of information • Many of my individual slides are full lectures (if not deserve their own courses and textbooks) • I will hit the highlights • When not to worry versus when to do something (more relevant with new wearable technologies) • I am happy to answer more detailed questions at the end Normal Sinus Rhythm Normal Heart Rate? • Conventional answer: – 60-100 beats per minute • How to check your heart rate – Find your pulse (wrist or neck—wrist preferred) – Count for a minute, or count for 15 seconds and multiply by four Normal Heart Rate? • Let’s break down this 60-100 beats per minute – Implies lower than 60 (called “bradycardia”) is a problem – Implies that faster than 100 (called “tachycardia”) is a problem • Cut to the chase: the great majority of the time, heart rates <60 or >100 are NORMAL What determines the heart rate? The autonomic nervous system The sympathec The nervous system parasympathe,c nervous system AKA: [ Adrenaline AKA: Fight or Flight [ Vagal tone [ [ Exercise Res,ng/ Sleeping Anxiety Eang/ Digesng Excitement Heart Rate Too Fast? • Faster than 100 beats per minute: – Normal—HEALTHY/ EXPECTED– if exercising or nervous or excited • What number is too fast? – Generally -

Sinoatrial Disease in Acute Myocardial Infarction' Long-Term Prognosis
Br Heart J: first published as 10.1136/hrt.38.4.410 on 1 April 1976. Downloaded from British Heart Journal, 1976, 38, 410-414. Sinoatrial disease in acute myocardial infarction' Long-term prognosis L. Hatle, J. Bathen, and R. Rokseth From the Section of Cardiology, Medical Department, University Hospital, Trondheim, Norway Of 32 patients with acute myocardial infarction complicated by sinoatrial disease, 23 survived All 23 had inferior infarction. Duringfollow-up lasting 4 to 6 years only one patient developed severe chronic sinoatrial disease (sick sinus syndrome) necessitating permanent pacemaker treatment; twelve others died during this time. In 2 of them death was sudden 5 and 6 months after infarction. Atrial pacing studies in 7 of the 11 patients still alive showed no gross abnormalities. A review of 71 patients with chronic sinoatrial disease treated with a permanent pacemaker revealed only 5 with previous documented infarction. The present data suggest that sinus node dysfunction in patients surviving acute infarction is most often only temporary as is atrioventricular block. Occasionally, however, severe chronic sinoatrial disease requiring a permanent pacemaker may develop later, and this course of events is most likely to occur in those patients who had additional complications during the acute infarct. The incidence and course of sinoatrial disease one had inferior infarction. Nine died during their stay complicating acute myocardial infarction have been in hospital. The remaining 23 patients were followed up reported (Rokseth and Hatle, 1971), but the long- from 4 to 6 years. There were 4 women and 19 men http://heart.bmj.com/ term prognosis is not well known. -

Sinus Node Dysfunction and Atrial Fibrillation Associated with Isolated Sinoatrial Node Artery Ectasia
Case Report Eur J Gen Med 2013; 10 (Suppl 1):69-71 Sinus Node Dysfunction and Atrial Fibrillation Associated with Isolated Sinoatrial Node Artery Ectasia Ahmet Karabulut, Bülent Uzunlar ABSTRACT A 74 year-old female patient was admitted to emergency service with a complaints of dizziness and shortness of breath. Complete atrioventricular block was observed and patient was followed up two days with transient transvenous cardiac pacemaker. Afterthat, atrial fibrillation (AF) was progressed and then, coronary angiography was scheduled. Although all three main coro- nary arteries was free of the stenotic lesion and coronary ectasia, there was a local ectatic segment with prominent slow flow in the sinoatrial node artery that originated from proximal right coronary artery. Patient was treated with dual anti-agregants and enoxaparine in the hospitalization period. Bradiarrhtymias did not recur and AF was reverted to sinusal rhythm with medical therapy. Classical risk factors for AF progression was absent in the patient. We thought that, ectasia and slow flow in the sinoatrial node artery could trigger the bradiarrhtymia and AF by the mechanism of ischemic sinus node dysfunction. Key words: Coronary ectasia, sinoatrial node artery, atrial fibrillation İzole sinoatriyal nod arteri ektazisine bağlı sinüs nodu disfonksiyonu ve atriyal fibrillasyon ÖZET Yetmişdört yaşında kadın hasta baş dönmesi, nefes darlığı şikayetleriyle acil polikliniğe başvurdu. Atrioventriküler tam blok sap- tanan hasta iki gün geçici transvenöz kalp pili ile takip edildi. Sonrasında atriyal fibrillasyon gelişen hastaya, koroner anjiyografide uygulandı. Her üç ana koroner arterlerde kritik darlık ve koroner ektazi olmamasına karşın; proksimal sağ koroner arterden köken alan sinoatrial nod arterinde izole lokal ektazi ve ektazik segmentte belirgin yavaş akım izlendi. -

Elderly Woman Carries Symptomatic Sinus Node Dysfunction (SND) Or Sick Sinus Syndrome (SSS)
Elderly Woman Carries Symptomatic Sinus Node Dysfunction (SND) or Sick Sinus Syndrome (SSS) Mulher idosa portadora de Doença do Nó Sinusal Sintomática Which is the appropriate approach? Raimundo Barbosa-Barros M.D. [email protected] Specialist in Cardiology by the Brazilian Society of Cardiology (SBC). Specialist in Intensive Care by the Sociedade Brasileira de Terapia Intensiva. Chief of the Coronary Center of the Hospital de Messejana Dr. Carlos Alberto Studart Gomes. Fortaleza - Brazil. Case report English Master, whenever you have a spare minute, present this case to the forum. 71-year-old woman with (biological) mitral valve replacement from 2 years ago. History of pre-syncope and palpitations for 2 months. Taking warfarin, enalapril maleate and espironolactone. Should she be indicated ablation of atrial tachycardia with the aim of improving sinus node function? Or, Should we indicate permanent pacemaker and then try to stabilize the atrium with drugs? Raimundo Barbosa-Barros M.D. Fortaleza Ceará Maestro,quando tiver tempo suba para o foro este caso. Mulher de 71 anos con substituição da válvula mitral (por prótese biológica) há 2anos. História de pré-síncope e palpitações por 2 meses. Em uso regular de warfarina, enalapril e aldactone. Têm indicação de ablação da taquicardia atrial com o intuito de melhorar a função do Nó sinusal? ou melhor indicar implante de marcapasso definitivo e depois tratar de estabilizar o átrio com fármacos? Raimundo Greater pause: 6.7 seconds with pre-syncope (already awake) Pausa maior: 6,7 segundos con pré-sincope (ya había despertado) Pré-síncope Pre-syncope Pre-syncope Pré-síncope Bioprosthesis in the mitral position with good mobility of mobile elements. -

Neonatal and Pediatric Guidelines for Arrhythmia Management What the Neonatal and Pediatric Critical Care Nurse Needs to Know
Neonatal and Pediatric Guidelines for Arrhythmia Management What the Neonatal and Pediatric Critical Care Nurse Needs to Know Cecilia St. George-Hyslop, M Ed, RN, CNCCP(C), The Hospital for Sick Children, Toronto, Canada Candace Morton, MSN, CPNP-PC/AC, Children’s Hospital of Wisconsin Elizabeth Daley, BA, BSN, RN, CCRN, Children’s Hospital of Los Angeles Introduction to the Problem: Arrhythmias are relatively common in the pediatric cardiac intensive care unit. Grosse-Wortmann et al studied 494 patients revealing 59% of neonates and 79% of older children have arrhythmias within 24 hrs of surgery. Of these arrhythmias, junctional ectopic tachycardia (JET) was seen in 9% of neonates and 5% of older children. Ventricular tachycardia was found in 3% of neonates and 15% of older children (Gross-Wortmann, 2010). In terms of specific arrhythmias, sinus tachycardia is the most frequently seen arrhythmia, with supraventricular tachycardia being the next most common, followed by sinus bradycardia (Hanash, 2010). Reentrant tachycardia is common in infants and children with congenital heart disease (CHD). Some arrhythmias in the early post operative period like premature atrial contraction’s (PAC’s) and premature ventricular beats (bigeminy) are usually transient and well tolerated. Others like junctional ectopic tachycardia (JET) and atrial flutter may cause significant hemodynamic instability and compromise or even sudden cardiac death. Primary arrhythmias occur in children without structural heart disease, although they may be secondary to ion channel diseases that are still being elucidated. Risk factors that predispose children for secondary arrhythmias include congenital cardiac malformations, surgical repair and scarring, long cardiopulmonary bypass times, or exposure to chronic hemodynamic stress (Brugada, 2013). -

Arrhythmias in Children
Future of Pediatrics June 20, 2019 Arrhythmias: When to Worry? Elizabeth (Libby) Sherwin, MD Pediatric Cardiologist and Electrophysiologist Arrhythmias in Pediatrics: Objectives 1. Review and refresh the basics of arrhythmias 2. Have a healthy relationship with arrhythmias: – Awareness – Curiosity – Respect – Balance of confidence and knowledge with a healthy dose of concern 3. Breathe easier knowing when and how to refer & manage patients Context is key Vasovagal syncope Context: ECG strips leading up to that moment: ST and T wave changes during sinus rhythm Arrhythmias: ElectricalMANY ( MOSTHeart) ARE Disease BENIGN OR HEMODYNAMICALLY WELL TOLERATED (AT LEAST IN THE SHORT TERM) • Benign ectopy: – Premature atrial contractions (PAC) – Premature junctional contractions (PJC) – Premature ventricular contractions (PVC) • Tachyarrhythmias: – Supraventricular tachycardia (SVT) – Ventricular arrhythmias • Bradycardia: – Sinus bradycardia – Heart block Classification of Arrhythmias • Sporadic – SVT, some ventricular tachycardia • Congenital heart defects - Pressure or volume overload - Post-operative - Late arrhythmias related to scars from suture lines • Familial = inherited = genetic – Long QT syndrome (LQTS) – Brugada syndrome – Catecholaminergic polymorphic ventricular tachycardia (CPVT) • Muscle disorders (Structural + inherited) – Hypertrophic, arrhythmogenic, and other cardiomyopathies • Other: Acquired, Infectious, Autoimmune – Myocarditis, Chagas, Lupus * Examples only! Not a complete list Why worry? Implications of Arrhythmias • Symptoms