Upper Urinary Tract Trauma
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Nuclear Medicine for Medical Students and Junior Doctors
NUCLEAR MEDICINE FOR MEDICAL STUDENTS AND JUNIOR DOCTORS Dr JOHN W FRANK M.Sc, FRCP, FRCR, FBIR PAST PRESIDENT, BRITISH NUCLEAR MEDICINE SOCIETY DEPARTMENT OF NUCLEAR MEDICINE, 1ST MEDICAL FACULTY, CHARLES UNIVERSITY, PRAGUE 2009 [1] ACKNOWLEDGEMENTS I would very much like to thank Prof Martin Šámal, Head of Department, for proposing this project, and the following colleagues for generously providing images and illustrations. Dr Sally Barrington, Dept of Nuclear Medicine, St Thomas’s Hospital, London Professor Otakar Bělohlávek, PET Centre, Na Homolce Hospital, Prague Dr Gary Cook, Dept of Nuclear Medicine, Royal Marsden Hospital, London Professor Greg Daniel, formerly at Dept of Veterinary Medicine, University of Tennessee, currently at Virginia Polytechnic Institute and State University (Virginia Tech), Past President, American College of Veterinary Radiology Dr Andrew Hilson, Dept of Nuclear Medicine, Royal Free Hospital, London, Past President, British Nuclear Medicine Society Dr Iva Kantorová, PET Centre, Na Homolce Hospital, Prague Dr Paul Kemp, Dept of Nuclear Medicine, Southampton University Hospital Dr Jozef Kubinyi, Institute of Nuclear Medicine, 1st Medical Faculty, Charles University Dr Tom Nunan, Dept of Nuclear Medicine, St Thomas’s Hospital, London Dr Kathelijne Peremans, Dept of Veterinary Medicine, University of Ghent Dr Teresa Szyszko, Dept of Nuclear Medicine, St Thomas’s Hospital, London Ms Wendy Wallis, Dept of Nuclear Medicine, Charing Cross Hospital, London Copyright notice The complete text and illustrations are copyright to the author, and this will be strictly enforced. Students, both undergraduate and postgraduate, may print one copy only for personal use. Any quotations from the text must be fully acknowledged. It is forbidden to incorporate any of the illustrations or diagrams into any other work, whether printed, electronic or for oral presentation. -

Nuclear Pharmacy Quick Sample
12614-01_CH01-rev3.qxd 10/25/11 10:56 AM Page 1 CHAPTER 1 Radioisotopes Distribution for Not 1 12614-01_CH01-rev3.qxd 10/25/1110:56AMPage2 2 N TABLE 1-1 Radiopharmaceuticals Used in Nuclear Medicine UCLEAR Chemical Form and Typical Dosage P Distribution a b HARMACY Radionuclide Dosage Form Use (Adult ) Route Carbon C 11 Carbon monoxide Cardiac: Blood volume measurement 60–100 mCi Inhalation Carbon C 11 Flumazenil injection Brain: Benzodiazepine receptor imaging 20–30 mCi IV Q UICK Carbon C 11 Methionine injection Neoplastic disease evaluation in brain 10–20 mCi IV R Carbon C 11 forRaclopride injection Brain: Dopamine D2 receptor imaging 10–15 mCi IV EFERENCE Carbon C 11 Sodium acetate injection Cardiac: Marker of oxidative metabolism 12–40 mCi IV Carbon C 14 Urea Diagnosis of Helicobacter pylori infection 1 µCi PO Chromium Cr 51 Sodium chromate injection Labeling red blood cells (RBCs) for mea- 10–80 µCi IV suring RBC volume, survival, and splenic sequestration Cobalt Co 57 Cyanocobalamin capsules Diagnosis of pernicious anemia and 0.5 µCi PO Not defects of intestinal absorption Fluorine F 18 Fludeoxyglucose injection Glucose utilization in brain, cardiac, and 10–15 mCi IV neoplastic disease Fluorine F 18 Fluorodopa injection Dopamine neuronal decarboxylase activity 4–6 mCi IV in brain Fluorine F 18 Sodium fluoride injection Bone imaging 10 mCi IV Gallium Ga 67 Gallium citrate injection Hodgkin’s disease, lymphoma 8–10 mCi IV Acute inflammatory lesions 5 mCi IV Indium In 111 Capromab pendetide Metastatic imaging in patients with biopsy- -

Uroradiology Tutorial for Medical Students Lesson 3: Cystography & Urethrography – Part 1
Uroradiology Tutorial For Medical Students Lesson 3: Cystography & Urethrography – Part 1 American Urological Association Introduction • Conventional radiography of the urinary tract includes several diagnostic studies: – Cystogram – Retrograde urethrogram – Voiding cystourethrogram • All of these studies answer questions that are essential to urologic patient management Voiding Cystourethrogram (VCUG) • The voiding cystourethrogram is a dynamic test used to define the anatomy and, in part, the function of the lower urinary tract. It is performed by placing a catheter through the urethra into the bladder, filling the bladder with contrast material and then taking x-rays while the patient voids. You can imagine how popular it is among children. Scout Film • Several films are taken when performing a VCUG. The first image is a KUB called the scout film. On this film one can evaluate the bones of the spine and pelvis (injury or congenital anomaly such as spina bifida) and the soft tissues (calcifications, foreign bodies, etc.). • Normal scout image • What gender? Scout Film • Patients with urologic problems (urine infection or incontinence) may have a spinal abnormality that results in abnormal innervation of the bladder. Such anomalies are commonly associated with anomalies of the vertebral column. Let’s look at some spines. • Here is a spine from a normal KUB or scout film. Notice that the posterior processes of all the vertebrae are intact. You can see the posterior process behind and below each vertebral body. • Here is another scout film. Notice that the posterior processes are absent below L-4. This patient has lower lumbar spina bifida. Read This Scout Film • The bones are normal • What about soft tissues (bowel, etc.)? • This child has significant constipation. -

FDA-Approved Radiopharmaceuticals
Medication Management FDA-approved radiopharmaceuticals This is a current list of all FDA-approved radiopharmaceuticals. USP <825> requires the use of conventionally manufactured drug products (e.g., NDA, ANDA) for Immediate Use. Nuclear medicine practitioners that receive radiopharmaceuticals that originate from sources other than the manufacturers listed in these tables may be using unapproved copies. Radiopharmaceutical Manufacturer Trade names Approved indications in adults (Pediatric use as noted) 1 Carbon-11 choline Various - Indicated for PET imaging of patients with suspected prostate cancer recurrence based upon elevated blood prostate specific antigen (PSA) levels following initial therapy and non-informative bone scintigraphy, computerized tomography (CT) or magnetic resonance imaging (MRI) to help identify potential sites of prostate cancer recurrence for subsequent histologic confirmation 2 Carbon-14 urea Halyard Health PYtest Detection of gastric urease as an aid in the diagnosis of H.pylori infection in the stomach 3 Copper-64 dotatate Curium Detectnet™ Indicated for use with positron emission tomography (PET) for localization of somatostatin receptor positive neuroendocrine tumors (NETs) in adult patients 4 Fluorine-18 florbetaben Life Molecular Neuraceq™ Indicated for Positron Emission Tomography (PET) imaging of the brain to Imaging estimate β amyloid neuritic plaque density in adult patients with cognitive impairment who are being evaluated for Alzheimer’s disease (AD) or other causes of cognitive decline 5 Fluorine-18 -

Radionuclide Cystography 138
The American College of Radiology, with more than 30,000 members, is the principal organization of radiologists, radiation oncologists, and clinical medical physicists in the United States. The College is a nonprofit professional society whose primary purposes are to advance the science of radiology, improve radiologic services to the patient, study the socioeconomic aspects of the practice of radiology, and encourage continuing education for radiologists, radiation oncologists, medical physicists, and persons practicing in allied professional fields. The American College of Radiology will periodically define new practice guidelines and technical standards for radiologic practice to help advance the science of radiology and to improve the quality of service to patients throughout the United States. Existing practice guidelines and technical standards will be reviewed for revision or renewal, as appropriate, on their fifth anniversary or sooner, if indicated. Each practice guideline and technical standard, representing a policy statement by the College, has undergone a thorough consensus process in which it has been subjected to extensive review, requiring the approval of the Commission on Quality and Safety as well as the ACR Board of Chancellors, the ACR Council Steering Committee, and the ACR Council. The practice guidelines and technical standards recognize that the safe and effective use of diagnostic and therapeutic radiology requires specific training, skills, and techniques, as described in each document. Reproduction or modification of the published practice guideline and technical standard by those entities not providing these services is not authorized. Revised 2010 (Res. 25)* ACR–SPR–SNM PRACTICE GUIDELINE FOR THE PERFORMANCE OF ADULT AND PEDIATRIC RADIONUCLIDE CYSTOGRAPHY PREAMBLE These guidelines are an educational tool designed to assist Therefore, it should be recognized that adherence to these practitioners in providing appropriate radiologic care for guidelines will not assure an accurate diagnosis or a patients. -
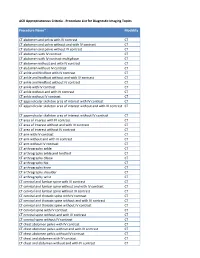
Standard Procedure List – AC Diagnostic Topics
ACR Appropriateness Criteria - Procedure List for Diagnostic Imaging Topics Procedure Name* Modality CT abdomen and pelvis with IV contrast CT CT abdomen and pelvis without and with IV contrast CT CT abdomen and pelvis without IV contrast CT CT abdomen with IV contrast CT CT abdomen with IV contrast multiphase CT CT abdomen without and with IV contrast CT CT abdomen without IV contrast CT CT ankle and hindfoot with IV contrast CT CT ankle and hindfoot without and with IV contrast CT CT ankle and hindfoot without IV contrast CT CT ankle with IV contrast CT CT ankle without and with IV contrast CT CT ankle without IV contrast CT CT appendicular skeleton area of interest with IV contrast CT CT appendicular skeleton area of interest without and with IV contrast CT CT appendicular skeleton area of interest without IV contrast CT CT area of interest with IV contrast CT CT area of interest without and with IV contrast CT CT area of interest without IV contrast CT CT arm with IV contrast CT CT arm without and with IV contrast CT CT arm without IV contrast CT CT arthrography ankle CT CT arthrography ankle and hindfoot CT CT arthrography elbow CT CT arthrography hip CT CT arthrography knee CT CT arthrography shoulder CT CT arthrography wrist CT CT cervical and lumbar spine with IV contrast CT CT cervical and lumbar spine without and with IV contrast CT CT cervical and lumbar spine without IV contrast CT CT cervical and thoracic spine with IV contrast CT CT cervical and thoracic spine without and with IV contrast CT CT cervical and thoracic spine -

Radionuclide Techniques for the Detection of Vesicoureteral Reflux
Review Article Radionuclide techniques for the detection of vesicoureteral reflux and their clinical significance Abstract We discuss and try to evaluate the detection of vesicoureteral reux (VUR) by radionuclide techniques and especially direct radionuclide cystography (DRC). Direct radionuclide cystography is applied for more than half a century mainly in children. Vesicoureteral reux has a complex pathology not yet completely under- Christodoulos Likartsis1 MD, BSc stood and is often related to urinary tract infection (UTI) and renal parenchyma scarring that can lead to 2 long-term renal function impairment. Since there is no consensus on the optimal imaging algorithm after Nikoleta Printza MD, PhD 1 the rst febrile urinary tract infection, many imaging strategies have been proposed for VUR detection in Athanasios Notopoulos MD, the last decade, including or not DRC. Views opposing or accepting its use are also presented. MDA, PhD Hell J Nucl Med 2020; 23(2): 180-187 Epub ahead of print: 27 July 2020 Published online: 24 August 2020 Introduction 1. Nuclear Medicine Department, Hippokration Hospital, Thessaloniki, Greece 2. 1st Pediatric Department, Aristotle University, Thessaloniki, bout 30% to 40% of children diagnosed with urinary tract infection (UTI), have Greece primary vesicoureteral reux (VUR) [1]. Children with VUR have 2.6 times higher Aprevalence of renal scarring compared to children without VUR [2]. For most of children with VUR, treatment involves continuous antibiotic prophylaxis (CAP). Mictura- ting cystourethrography (MCU) and direct radionuclide cystography (DRC) are mainly applied for the detection and follow-up of VUR respectively [3] although some authors are not agreeable as for their indications [4, 5]. -

Cystography You Will Change in to a Hospital Gown Welcome to VCU Health Diagnostic Imaging
Diagnostic Fluoroscopy Patient Information Cystography You will change in to a hospital gown Welcome to VCU Health Diagnostic Imaging. We are An abdominal x-ray will be obtained located in the Main Hospital 3rd floor, 1200 East Marshall The nurse or physician will insert a catheter into Street. Our hours of operation are Monday through the bladder Friday, 8 am to 5 pm. Advanced scheduling is required for all diagnostic fluoroscopy exams. Please review the You will be laying down on a fluoroscopy table following information about your test. Please call (804) while a contrast agent hooked up to the catheter 628-3580 to schedule your test or if you have any flows in to your bladder. The radiologist will take questions about your diagnostic fluoroscopy exam. images with the fluoroscopy x-ray machine What is it? Once your bladder is full, you will be asked to move in a few different positions Imaging of the urinary system. A bedpan or urinal will be given to you and you Why are you having this test? will be asked to urinate while the radiologist is You are having this study to establish presence or imaging with the fluoroscopy equipment absence, nature or extent of disease affecting the urinary A post void x-ray will be taken if you have not system. Imaging from cystography studies can reveal completely emptied your bladder abnormalities related to: After Care information Hematuria (blood in the urine) You may resume normal activity, eating and Recurring urinary tract infections (UTIs) drinking after exam unless otherwise specified by Leaking Urine your physician. -

Imaging in Pediatric Urology
PEDIATRIC UROLOGY 0031-3955/97 $0.00 + .20 IMAGING IN PEDIATRIC UROLOGY Eglal Shalaby-Rana, MD, Lisa H. Lowe, MD, Anna Nussbaum Blask, MD, and Massoud Majd, MD The pediatric genitourinary tract may be affected by many disor- ders, most of which are congenital and some acquired. Patients pre- senting with signs and symptoms related to the genitourinary tract often need imaging for diagnosis and management. In this article, a problem- oriented approach is used to discuss the following clinical urologic problems: (1) urinary tract infection (UTI), (2) hydronephrosis or hy- droureter, (3) genitourinary trauma, (4) swollen scrotum, and (5) hema- turia. THE CHILD WITH URINARY TRACT INFECTION UTI is one of the most frequently encountered clinical problems in children. Despite the common occurrence of UTI, the diagnostic work- up and management remain a constant challenge for pediatricians. There are many approaches to evaluating children with UTIs; however, the ultimate goal of the diagnostic work-up is to identify kidneys at risk for acute pyelonephritis (AP) and subsequent renal scarring. The task may become simpler by addressing two important questions: Is the infection limited to the bladder, or does it involve the kidney resulting in acute From the Department of Diagnostic Imaging and Radiology, Children’s National Medical Center and The George Washington University Medical School, Washington DC (ESR, A M , MM); and the Department of Radiology, Children’s Medical Center of Dallas, University of Texas-Southwestern, Dallas, Texas (LHL) PEDIATRIC CLINICS OF NORTH AMERICA VOLUME 44 * NUMBER 5 * OCTOBER 1997 1065 1066 SHALABY-RANA et a1 pyelonephritis; and are there underlying anatomic abnormalities in the urinary tract that predispose to infection, most importantly vesicoure- teral reflux (VUR) and obstruction. -

Answers to Chapter Review Exercises, Appendix D
Appendix D text AC200610: Basic CPT and HCPCS Coding Page 1 of 26 Answers to Chapter Review Exercises, Appendix D Chapter 1: Introduction to Clinical Coding Chapter 1 Review 1. The American Medical Association (AMA) updates the CPT codes, and the Centers for Medicare and Medicaid Services (CMS) updates the HCPCS National Codes (Level II). 2. Four 3. ICD-9-CM and CPT/HCPCS 4. a. Diagnosis: ICD-9-CM Procedure: CPT/HCPCS b. Diagnosis: ICD-9-CM Procedure: CPT/HCPCS c. UB-04 (CMS-1450) 5. ICD-9-CM 6. Procedure code 11440 is linked with diagnosis code #1 (216.3). Procedure code 82951 is linked with diagnosis code #3 (790.29). Note: Depending on the carrier, you may link more than one reference number in block 24E, whereas some payers require just one. When reporting more than one code on a CMS-1500 claim, enter the code with the highest fee in line 1 of block 24 and the remaining in descending order of charges. Chapter 2: Application of the CPT System Exercise 2.1 Organization of CPT 1. Surgery 2. Evaluation and Management 3. Pathology and Laboratory 4. Category II codes 5. Medicine 6. Radiology 7. Anesthesia 8. Category III codes 9. Maternity Care and Delivery 10. StandbyServices Appendix D text AC200610: Basic CPT and HCPCS Coding Page 2 of 26 11. Radiation Oncology 12. Surgical Pathology Exercise 2.2 CPT Conventions 1. Repair blood vessel, direct; hand, finger 2. Two 3. Revised descriptor 4. Esophagoscopy, rigid or flexible, with insertion of plastic tube or stent 5. -

Extravasation from the Unused Bladder During Cystography
Paraplegia 24 (1986) 385-388 © 1986 International Medical Society of Paraplegia Extravasation froID the Unused Bladder During Cystography: Case Report Mary M. Staffa, M.D. and Allan Naitnark, M.D. C.M., F.R.C.P.(C) Department of Radiology, University Hospital, Boston University School of Medicine, Boston, MA, U.S.A. Sutntnary Spontaneous, asymptomatic extravasation during retrograde cystography occurred in a quadraplegic patient who had been maintained on constant Foley catheter drainage for 7 years. This phenomenon has recently been described in a few anuric patients being studied prior to renal transplant and is probably related to the chronic disuse status of the bladder. It is a self-limiting process and, in the absence of a clinical reaction, only observation is warranted. Key words: Spinal cord injuries; Retrograde cystography; Urinary bladder rupture. Introduction Asymptomatic, uncomplicated extravasation of contrast material from the urinary bladder during cystography has recently been described in anuric patients with unused bladders being evaluated as potential renal transplant recipients (Caroline 1985, Day 1985, O'Neal 1986). This phenomenon has not been described in a patient with normal renal function. We describe a patient from a totally different patient population in whom this phenomenon was observed-a patient with a neuropathic bladder on constant Foley catheter drainage. Case report A 59-year-old female developed C5 quadriplegia in May, 1978 after surgery for an epidural abscess. She had been treated with constant Foley catheter drainage for a neuropathic bladder since 1978 and had developed multiple episodes of urinary tract infections. The patient was currently being evaluated for re habilitation as her functional level had improved. -

2018-PED Abdomen
CLINICAL GUIDELINES Pediatric Abdomen Imaging Policy Version 20.0.2018 Effective May 17, 2018 eviCore healthcare Clinical Decision Support Tool Diagnostic Strategies: This tool addresses common symptoms and symptom complexes. Imaging requests for individuals with atypical symptoms or clinical presentations that are not specifically addressed will require physician review. Consultation with the referring physician, specialist and/or individual’s Primary Care Physician (PCP) may provide additional insight. CPT® (Current Procedural Terminology) is a registered trademark of the American Medical Association (AMA). CPT® five digit codes, nomenclature and other data are copyright 2016 American Medical Association. All Rights Reserved. No fee schedules, basic units, relative values or related listings are included in the CPT® book. AMA does not directly or indirectly practice medicine or dispense medical services. AMA assumes no liability for the data contained herein or not contained herein. © 2018 eviCore healthcare. All rights reserved. Imaging Guidelines V20.0.2018 Pediatric Abdomen Imaging Guidelines eviCore Code Management for BCBS AL ............................................. 3 PEDAB-1: General Guidelines ............................................................... 6 PEDAB-2: Generalized Abdominal Pain .............................................. 12 PEDAB-3: Right Lower Quadrant Pain ................................................ 13 PEDAB-4: Flank Pain, Renal Stone ..................................................... 14 PEDAB-5: