Community Ties: UC Health Report on Affiliation Impacts
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Strategies to Increase Health Facility Deliveries: Three Case Studies
Strategies to increase health facility deliveries: Three case studies Strategies to increase health facility deliveries: Three case studies Copyright © 2014 UCSF Global Health Group The Global Health Group Global Health Sciences University of California, San Francisco 550 16th Street, 3rd Floor San Francisco, CA 94158 USA Email: [email protected] Website: globalhealthsciences.ucsf.edu/global-health-group Ordering information This publication is available for electronic download at globalhealthsciences.ucsf.edu/global-health-group/ ghg-publications Recommended citation Butrick, E., Diamond-Smith, N., Beyeler, N., Montagu, D., Sudhinaraset, M. (2014). Strategies to increase health facility deliveries: Three case studies. Global Health Group, Global Health Sciences, University of California, San Francisco. Cover photos courtesy of Photoshare. © 2006 Abhijit Dey (India) and © 2012 Akintunde Akinleye/NURHI (Nigeria). Produced in the United States of America. First Edition, December 2014 This is an open-access document distributed under the terms of the Creative Commons Attribution-Noncommercial License, which permits any noncommercial use, distribution, and repro- duction in any medium, provided the original authors and source are credited. Contents Introduction | 1 Methods | 2 Country selection process | 2 Interviews and recruitment | 2 Description of each case study | 3 Malawi | 3 Nigeria | 3 India | 3 Summary of themes | 4 Lesson learned #1: Political will | 4 Lesson learned #2: Balancing supply, demand and quality | 5 Lesson learned -

Californiachoice® Small Group Advantage PPO Three-Tier Hospital Network
CaliforniaChoice® Small Group Advantage PPO three-tier hospital network With the CaliforniaChoice Advantage PPO plans, you have a choice of tiers (or levels) of hospitals to visit. Tier one hospitals offer the greatest savings to you. Tier two hospitals have the second best level of savings. Tier three hospitals — or out-of-network hospitals — offer the least out-of-pocket savings, but you’ll still be covered. Keep in mind that the tier levels aren’t based on the quality of care given at each hospital. They’re based on which hospitals have shown they’re better able to give quality care that’s also cost effective. Our three-tier levels* are: }}Tier 1 — PPO network hospitals with lower-negotiated hospital reimbursement rates. }}Tier 2 — the remaining PPO network hospitals. }}Tier 3 — non-network hospitals. * The tier levels are not based on the quality of care given at each hospital. Instead, each level stands for the hospitals that show 19685CABENABC 08/15 the best use of health care dollars. CaliforniaChoice® Small Group Advantage PPO three-tier hospital network Here is a list of the Tier-1 and Tier-2 hospitals included in the network. Any hospital not listed is considered out of network. Hospital County Tier St Rose Hospital Alameda 1 Alameda Hospital Alameda 1 Children’s Hospital Oakland Alameda 2 Valleycare Medical Center Alameda 2 Washington Hospital Alameda 2 Sutter Amador Health Center Pioneer 1 Sutter Amador Health Center Plymouth 1 Sutter Amador Hospital Amador 1 Oroville Hospital & Medical Center Butte 1 Feather River Hospital -
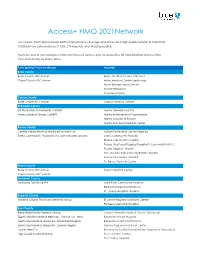
Access+ HMO 2021Network
Access+ HMO 2021Network Our Access+ HMO plan provides both comprehensive coverage and access to a high-quality network of more than 10,000 primary care physicians (PCPs), 270 hospitals, and 34,000 specialists. You have zero or low copayments for most covered services, plus no deductible for hospitalization or preventive care and virtually no claims forms. Participating Physician Groups Hospitals Butte County Butte County BSC Admin Enloe Medical Center Cohasset Glenn County BSC Admin Enloe Medical Center Esplanade Enloe Rehabilitation Center Orchard Hospital Oroville Hospital Colusa County Butte County BSC Admin Colusa Medical Center El Dorado County Hill Physicians Sacramento CalPERS Mercy General Hospital Mercy Medical Group CalPERS Methodist Hospital of Sacramento Mercy Hospital of Folsom Mercy San Juan Medical Center Fresno County Central Valley Medical Medical Providers Inc. Adventist Medical Center Reedley Sante Community Physicians Inc. Sante Health Systems Clovis Community Hospital Fresno Community Hospital Fresno Heart and Surgical Hospital A Community RMCC Fresno Surgical Hospital San Joaquin Valley Rehabilitation Hospital Selma Community Hospital St. Agnes Medical Center Glenn County Butte County BSC Admin Glenn Medical Center Glenn County BSC Admin Humboldt County Humboldt Del Norte IPA Mad River Community Hospital Redwood Memorial Hospital St. Joseph Hospital - Eureka Imperial County Imperial County Physicians Medical Group El Centro Regional Medical Center Pioneers Memorial Hospital Kern County Bakersfield Family Medical -

Note on Health Facility and Types Larina Brooklyn * College of Medicine and Health Academy, Nigeria
Health Econ Outcome Res Open Access 2021, Vol.7, Issue 5, e114. Editorial Note on Health Facility and Types Larina Brooklyn * College of Medicine and Health Academy, Nigeria Corresponding Author* clinics are these days staffed by expertly prepared specialists, attendants, paramedical clinicians, and so forth, though truly, this work was typically Larina Brooklyn done by the establishing strict orders or by volunteers. College of Medicine and Health Academy, Nigeria Medical Care Community E-mail: [email protected] Medical care habitats, including facilities, specialist's workplaces, earnest consideration communities and mobile medical procedure places, Copyright: © 2021 Larina Brooklyn . This is an open-access article distributed fill in as first resource with a health proficient and give outpatient clinical, under the terms of the Creative Commons Attribution License, which permits nursing, dental, and different sorts of care administrations. unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. Clinical Nursing Homes Clinical nursing homes, including private therapy places and geriatric Received 18 May 2021; Accepted 20 May 2021; Published 27 May 2021 consideration offices, are medical services foundations which have convenience offices and which take part in giving present moment or long haul clinical therapy of a general or concentrated nature not performed by clinics to inpatients with any of a wide assortment of ailments Introduction Drug Stores and Pharmacies A health facility is, by and large, any area where medical services is Drug stores and pharmacies involve foundations occupied with given. Health offices range from little facilities and specialist's workplaces retailing remedy or nonprescription medications and prescriptions, to dire consideration places and enormous medical clinics with intricate and different kinds of clinical and muscular goods.[4] Regulated drug trauma centers and emergency rooms. -

Operational Considerations for Case Management of COVID-19 in Health Facility and Community Interim Guidance 19 March 2020
Operational considerations for case management of COVID-19 in health facility and community Interim guidance 19 March 2020 Background This document is intended for health ministers, health system administrators, and other decision-makers. It is meant to guide the care of COVID-19 patients as the response capacity of health systems is challenged; to ensure that COVID-19 patients can access life-saving treatment, without compromising public health objectives and safety of health workers. It promotes two key messages: 1. Key public health interventions regardless of transmission scenario; and 2. Key action steps to be taken by transmission scenario to enable timely surge of clinical operations. The public health objectives at all stages of the preparedness and response plan are to: • Prevent outbreaks, delay spread, slow and stop transmission. • Provide optimized care for all patients, especially the seriously ill. • Minimize the impact of the epidemic on health systems, social services, and economic activity. Based on the largest cohort of COVID-19 patients, about 40% of patients with COVID-19 may have mild disease, where treatment is mostly symptomatic and does not require inpatient care; about 40% of patients have moderate disease that may require inpatient care; 15% of patients will have severe disease that requires oxygen therapy or other inpatient interventions; and about 5% have critical disease that requires mechanical ventilation.1 However, the evolution of the outbreak in some countries has shown a higher proportion of severe and critical cases and the need to rapidly increase surge capacity to prevent rapid exhaustion of biomedical supplies and staff. In some countries, doubling rates of cases every 3 days has been observed.2 Scenarios of transmission Countries or subnational areas will have to respond rapidly to one or more epidemiological scenarios. -

A Model Policy for SMART Health Facilities the Model Policy for SMART Health Facilities Was Prepared by Dr
A Model Policy for SMART Health Facilities The Model Policy for SMART Health Facilities was prepared by Dr. Vasantha Chase, et al, (Castries, Saint Lucia), on behalf of the Pan American Health Organization (2013). TABLE OF CONTENTS Foreword . 3 Section I – Defining the Problem . 5 • The vulnerability of health facilities to natural hazards . 5 • The vulnerability of health facilities to climate change and variability . 6 • Damage to health facilities from disasters . 7 • The cost of damage to health facilities in the Caribbean . 8 • Costs related to climate change and variability . 9 • Progress is being made . 10 Section II –Conceptual Framework for a Policy on SMART Health Facilities . 13 Section III – A Model for Developing a SMART Health Facilities Policy . 17 • Purpose of the policy . 17 • Policy guidelines . 17 • Components of the policy . 18 • Policy strategy . 21 • Implementing the policy . 22 • Monitoring, evaluation and reporting . 23 Conclusion . 25 Acronyms . 26 Glossary . 27 List of Tables • Table 1: Impact of Hurricane Tomas (2010) on health facilities in Saint Lucia . 7 • Table 2: Categorization of Energy Supply in Health Facilities in Guyana . 10 List of Figures • Figure 1: SMART Health Facilities Policy: The conceptual framework . 14 • Figure 2: Operationalising the SMART Health Facilities Policy . 16 • Figure 3: Mapping the Policy on SMART Health Facilities . 19 1 FOREWORD he Caribbean is a highly hazard-prone region. Hurricanes Gilbert, Ivan and Tomas are stark reminders of how the direct and indirect impact of weather-related disasters can significantly Tdisrupt access to health services and the sector’s ability to provide care. However, today it also is becoming increasingly clear that the health sector itself is one of many contributors to the impact of climate change, making it imperative to step up efforts to reduce the environmental footprint and increase the resiliency of its health facilities. -

Choosing Hospice Consumer's Guide
Choosing Hospice a consumer’s guide Table of Contents Introduction ............................................................2 What makes hospice care special? .........................4 Minnesota Network of Hospice & Palliative Care (MNHPC) promotes quality of life in Minnesota How will hospice care provide support communities through education and access to resources in advance care planning, palliative for me and my family? ...........................................6 care and hospice care. What if I live alone or don’t have Our vision is that all individuals, families and family nearby? .......................................................7 providers will understand the value of and have access to these resources. Who is eligible for hospice care? ...........................8 With provider members across Minnesota, the work of MNHPC touches communities through- How is my care paid for? .......................................8 out the entire state. How do I find a hospice program? .......................10 Glossary ...............................................................12 Originally written in 1997 with a grant from the Allina Foundation as part of its Project DECIDE Program. © 1997 Minnesota Hospice Organization. All rights reserved. © 2nd Edition, Revised 1998. All rights reserved. © 3rd Edition, Revised 2000. All rights reserved. © 4th Edition, Revised 2009. All rights reserved. © 5th Edition, Revised 2010. All rights reserved. Made accessible in 2016 by funding from a Live Well at Home Grant from Minnesota Department of Human Services. 1 INTRODUCTION The thought that you or someone you love According to the wife of a hospice patient, is dying can be overwhelming. It may seem “Thank you for being “We knew that Mark’s prognosis wasn’t that all is hopeless, that there is nothing honest with me, for good, but we also knew that we had today more you can do. -

4 Isolation Rooms
4 Isolation Rooms 4 Isolation Rooms 4.1 General An isolation facility aims to control the airflow in the room so that the number of airborne infectious particles is reduced to a level that ensures cross-infection of other people within a healthcare facility is highly unlikely. This may be achieved by: . Control of the quantity and quality of intake or exhaust air. Maintain different air pressures between adjacent areas. Designing airflow patterns for specific clinical procedures. Diluting infectious particles with large air volumes. Air filtration – HEPA filters, etc. Isolation facilities include the following types: . Neutral or standard room air pressure, for example standard air conditioning, also known as Class S . Positive room air pressure where an immune-compromised patient is protected from airborne transmission of any infection, Class P . Negative room air pressure, where others are protected from any airborne transmission from a patient who may be an infection risk, Class N . Negative room air pressure with additional barriers including an Anteroom, also known as Class Q for quarantine isolation. Isolation rooms have fairly high rates of air exchange relative to other patient areas. This applies to both ventilation air supply and exhaust flow rates. Potential draughts within the patient room can result, therefore thermal comfort of the patient needs special attention. Consideration should be given to installing individual thermostats in each room so that air temperature and relative humidity can be controlled from within the room. Isolation rooms do not necessarily always require the provision of an Anteroom. This should be determined by the proposed operational policy and be included at an early stage of the design process. -

Checklist to Prepare Physician Offices for COVID-19
Checklist to Prepare Physician Offices for COVID-19 ASSUMPTION: Transmission will be primarily through exposure to respiratory droplets and direct contact with patients and their contaminated environments. Universal Early Preparation within six feet of patients with suspected COVID-19 infection. (See approved respirators). Provide training ☐ Educate staff and patients about changes they for staff on respirators to ensure fit and appropriate can expect to be implemented in the office use. during an outbreak or pandemic, and about ways to prepare themselves and their families. • Ensure adherence to standard precautions, including airborne precautions and use of eye protection. Assume that every patient is potentially infected or COVID-19 Education colonized with a pathogen that could be transmitted in • Educate staff about coronavirus disease 2019 a health care setting. (COVID-19), and why it is important to contain the • Implement mechanisms and policies that promptly outbreak. alert key facility staff including infection control, health • Educate staff on facility policies and practices care epidemiology, facility leadership, occupational to minimize chance of exposure to respiratory health, clinical laboratory, and frontline staff about pathogens including SARS-CoV-2, the virus that known suspected COVID-19 patients (i.e. PUI). Keep causes COVID-19. updated lists of staff and patients to identify those at risk in the event of an exposure. • Train and educate staff with job-or task-specific information on preventing transmission of infectious • Staff should follow the CDC guidelines collecting, agents, including refresher training. handling and testing clinical specimens from (PUIs for COVID-19. • Educate staff about COVID-19 evaluation and treatment. • Prepare for office staff illness, absences, and/or quarantine. -

California Hospitals: an Evolving Environment
California Hospitals: An Evolving Environment AUGUST 2015 California Hospitals Introduction Overview California’s general acute care (GAC) hospitals discharged more than 3.3 million patients and had nearly 44 million outpatient visits in 2013. California Hospitals: An Evolving Environment examines the state’s GAC CONTENTS hospitals, including bed supply and capacity, use of services, financial health, and selected quality measures. Supply and Capacity .................... 3 Use of Services .........................11 KEY FINDINGS INCLUDE: • The number of general acute care hospitals declined by 4% between 2004 and 2013, while Finances ................................25 the number of beds remained largely unchanged. Critical Access Hospitals ................33 • Skilled nursing and acute psychiatric beds declined significantly during that decade, while both adult and newborn intensive care beds increased. Quality .................................35 • The eight largest hospital systems accounted for 40% of hospitals and beds in California. Seismic Safety ..........................40 • A larger percentage of hospitals were profitable in 2013 than in 2014 as reflected by both Methodology ...........................41 total and operating margins. Appendices ............................42 • The costs of uncompensated care, as measured by charity care and bad debt, rose by 45% between 2004 and 2013 to $2.8 billion. • Preventable adverse events reported at California hospitals increased each year from 2009 to 2013. • California performed slightly -
![Health Facility Checklist Section 1226 [Oshpd 3] Clinics 1226.6 Primary](https://docslib.b-cdn.net/cover/5175/health-facility-checklist-section-1226-oshpd-3-clinics-1226-6-primary-745175.webp)
Health Facility Checklist Section 1226 [Oshpd 3] Clinics 1226.6 Primary
Compliance Checklist: [OSHPD 3] Primary Care Clinics Page 1 of 11 HEALTH FACILITY CHECKLIST SECTION 1226 [OSHPD 3] CLINICS 1226.6 PRIMARY CARE CLINICS Primary Care Clinics are Health Facilities licensed under Section 1200 of the California Health & Safety Code that provide services limited to those listed in California Building Code Section 1226.6. Outpatient clinical services of a hospital providing services, licensed under Section 1250 of the California Health & Safety Code, which are equivalent to a primary care clinic, shall also comply with California Building Code Section 1226.6 and be considered a primary care clinic. Primary care clinics are subject to the provisions of Section 1226 [OSHPD 3] CLINICS, of the California Building Code and all amendments to the California Building Standards Code (CBSC) under the banner [OSHPD 3]. OSHPD requirements apply to all facilities described above and are not dependent upon Occupancy Group designations. While Examination Rooms are required in Primary Care Clinics, the provision of Treatment Rooms is optional and dependent upon the intended delivery of care. Examination Rooms are intended for diagnostic examinations, where Treatment Rooms are intended for clinical/interventional procedures and include appropriate size and finish requirements to accommodate treatment/procedures that do not require a restricted (sterile) environment but may use sterile instruments or equipment. All new buildings and additions, alterations or repairs to existing buildings, and conversion of space to a clinic use within existing buildings, subject to Licensing and Certification, California Department of Public Health, shall comply with applicable provisions of the California Building Code (CBC), California Electrical Code (CEC), California Mechanical Code (CMC), California Plumbing Code (CPC), California Energy Code, California Green Building Standards Code and California Fire Code (Parts 2, 3, 4, 5, 6, 9, and 11 of Title 24). -

Operational Considerations for Community Isolation Centers for COVID-19 in Low-Resource Settings
Operational Considerations for Community Isolation Centers for COVID-19 in Low-Resource Settings Accessible version: https://www.cdc.gov/coronavirus/2019-ncov/global-covid-19/operational-considerations-isolation-centers.html Background The coronavirus disease 2019 (COVID-19) pandemic has presented numerous challenges to health systems, including large numbers of patients that can overwhelm health facilities and staff. Community isolation centers (CICs) can give people experiencing mild to moderate symptoms (e.g. fever, fatigue, cough, muscle pain, sore threat, new loss of smell or taste, nasal congestion, shortness of breath or headache) a safe place to voluntarily isolate, while conserving healthcare facility resources. Guiding principles: • Community isolation centers generally do not care for severely ill patients or those with increased risk for severe disease. These patients should seek care at a health facility or hospital where advanced care, treatment and constant monitoring can be provided. However, in cases where no hospital beds are available, CICs can accept such people when feasible to prevent household transmission that could occur if they stayed home. CICs also support linkage to higher level care. • People with mild or moderate illness who have been tested and are waiting for their results should isolate at home until they know their status to avoid becoming infected by other patients at a CIC. In cases where safely isolating at home is not possible, people waiting for results may isolate in a CIC. This document gives operational considerations for CDC country offices, ministries of health, and other partners about establishing and operating CICs for people with suspected or laboratory-confirmed COVID-19.