Foreign Body Management
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Siphoning Diesel: a Fatal Mistake
CASE REPORT Siphoning diesel: a fatal mistake Leong Wei Cheng, MRCP, Brian Cheong Mun Keong, FRCP Department of Medicine, Hospital Teluk Intan cervical lymphadenopathy and auscultation of his lungs SUMMARY revealed normal findings. Examination of other systems did Diesel is commonly used as fuel for engines and is distilled not reveal any abnormalities. from petroleum. Diesel has toxic potential and can affect multiple organs. Exposure can occur after ingestion, Initial blood investigations showed evidence of acute kidney inhalation or through the dermal route. The practice of injury (urea: 16.7 mmol/l, sodium 129 mmol/l, potassium 3.7 siphoning diesel using a rubber tubing and the mouth is mmol/l and creatinine 937 µmol/l). There was presence of common in rural communities. This can lead to accidental protein and erythrocytes (2+) in his urine. His full blood count ingestion and aspiration. Here we report a case of a patient showed elevated white cell count of 11,600/µl (neutrophil who accidentally ingested diesel during siphoning, which 85%) with normal haemoglobin concentration (15.9 g/dl) caused extensive erosion of the oral cavity and oesophagus and platelets (185,000/µl). Liver transaminases were normal. leading to pneumomediastinum and severe chemical lung Chest radiograph showed clear lung fields. His provisional injury. The patient responded well initially to steroids and diagnosis was acute tonsillitis with post- infectious Rapidly supportive care but required prolonged hospitalisation. He Progressive Glomerolonephritis (RPGN). Intravenous (IV) developed complications of nosocomial infection and Ceftriaxone 2 g daily was started. succumbed 23 days after admission. He became progressively more tachypnoeic in the ward with KEY WORDS: Diesel; siphon; chemical pneumonitis; oesophageal perforation; worsening renal function and metabolic acidosis. -

Chapter 32 FOREIGN BODIES of the HEAD, NECK, and SKULL BASE
Foreign Bodies of the Head, Neck, and Skull Base Chapter 32 FOREIGN BODIES OF THE HEAD, NECK, AND SKULL BASE RICHARD J. BARNETT, MD* INTRODUCTION PENETRATING NECK TRAUMA Anatomy Emergency Management Clinical Examination Investigations OPERATIVE VERSUS NONOPERATIVE MANAGEMENT Factors in the Deployed Setting Operative Management Postoperative Care PEDIATRIC INJURIES ORBITAL FOREIGN BODIES SUMMARY CASE PRESENTATIONS Case Study 32-1 Case Study 32-2 Case Study 32-3 Case Study 32-4 Case Study 32-5 Case Study 32-6 *Lieutenant Colonel, Medical Corps, US Air Force; Chief of Facial Plastic Surgery/Otolaryngology, Eglin Air Force Base Department of ENT, 307 Boatner Road, Suite 114, Eglin Air Force Base, Florida 32542-9998 423 Otolaryngology/Head and Neck Combat Casualty Care INTRODUCTION The mechanism and extent of war injuries are sig- other military conflicts. In a study done in Croatia with nificantly different from civilian trauma. Many of the 117 patients who sustained penetrating neck injuries, wounds encountered are unique and not experienced about a quarter of the wounds were from gunshots even at Role 1 trauma centers throughout the United while the rest were from shell or bomb shrapnel.1 The States. Deployed head and neck surgeons must be injury patterns resulting from these mechanisms can skilled at performing an array of evaluations and op- vary widely, and treating each injury requires thought- erations that in many cases they have not performed in ful planning to achieve a successful outcome. a prior setting. During a 6-month tour in Afghanistan, This chapter will address penetrating neck injuries all subspecialties of otolaryngology were encountered: in general, followed specifically by foreign body inju- head and neck (15%), facial plastic/reconstructive ries of the head, face, neck, and skull base. -

Bruises- Wounds
Henry Shih OD, MD Medical Director Austin Emergency Center- Anderson Mill 13435 US Highway 183 North Suite 311 Austin, TX 78750 512-614-1200 BRUISES- http://austiner.com/ What are bruises? — Bruises happen when blood vessels under the skin break, but the skin isn’t cut. Blood leaks into the tissues under the skin. Bruises start off red in color, and then turn blue or purple. As they heal, bruises can turn green and yellow. Most bruises heal in 1 to 2 weeks, but some take longer. How are bruises treated? — A bruise will get better on its own. But to feel better and help your bruise heal, you can: o Put a cold gel pack, bag of ice, or bag of frozen vegetables on the injured area every 1 to 2 hours, for 15 minutes each time. Put a thin towel between the ice (or other cold object) and your skin. Use the ice (or other cold object) for at least 6 hours after your injury. Some people find it helpful to ice longer, even up to 2 days after their injury. o Raise the area, if possible – Raising the area above the level of your heart helps to reduce swelling. o Take medicine to reduce the pain and swelling – To treat pain, you can take Tylenol. To treat pain and swelling, you can take ibuprofen (sample brand names: Advil, Motrin). But people who have certain conditions or take certain medicines should not take ibuprofen. If you are unsure, ask your doctor or nurse if you can take ibuprofen. -
Foreign Body Insertions: a Review
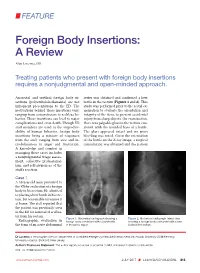
FEATURE Foreign Body Insertions: A Review Alan Lucerna, DO Treating patients who present with foreign body insertions requires a nonjudgmental and open-minded approach. Anorectal and urethral foreign body in- series was obtained and confirmed a beer sertions (polyembolokoilamania) are not bottle in the rectum (Figures 1 and 2). This infrequent presentations to the ED. The study was performed prior to the rectal ex- motivations behind these insertions vary, amination to evaluate the orientation and ranging from autoeroticism to reckless be- integrity of the item, to prevent accidental havior. These insertions can lead to major injury from sharp objects. On examination, complications and even death. Though ED there was palpable glass in the rectum con- staff members are used to the unpredict- sistent with the rounded base of a bottle. ability of human behavior, foreign body The glass appeared intact and no gross insertions bring a mixture of responses bleeding was noted. Given the orientation from the staff, ranging from awe and in- of the bottle on the X-ray image, a surgical credulousness to anger and frustration. consultation was obtained and the patient A knowledge and comfort in managing these cases includes a nonjudgmental triage assess- ment, collective professional- ism, and self-awareness of the staff’s reaction. Case 1 A 58-year-old man presented to the ED for evaluation of a foreign body in his rectum. He admitted to placing a beer bottle in his rec- tum, but was unable to remove it at home. The staff reported that the patient was previously seen in the ED for removal of a vibra- tor from his rectum. -

Foreign Rectal Body – Systematic Review and Meta-Analysis
REVIEW 61 Foreign rectal body – Systematic review and meta-analysis M. Ploner1, A. Gardetto2, F. Ploner3, M. Scharl4, S. Shoap5, H. C. Bäcker5 (1) Department of Anesthesiology and Intensiver Care, Cantonal Spital Lucerne, Lucerne, Switzerland ; (2) Department of Plastic Surgery, Hospital Sterzing, Sterzing, South Tirol, Italy ; (3) Department of Anesthesiology and Emergency Medicine, Hospital Sterzing, South Tirol, Italy ; (4) Department of Gastroenterology and Hepatology, University Hospital Zurich, University of Zurich, Swetzerland ; (5) Department of Orthopaedic Surgery, Columbia University Medical Center, New York, USA. Abstract instrumentation (7). The most common complication is a rectal injury, which can result from a variety of agents and Background : Self-inserted foreign rectal bodies are an objects (8). Often, nonsurgical removal of foreign bodies infrequent occurrence, however they present a serious dilemma to the surgeon, due to the variety of objects, and the difficulty of has been described to be successful – in 11% to 65% – extraction. The purpose of this study is to give a comprehensive (9), however, in many situations, a surgical treatment review of the literature regarding the epidemiology, diagnostic may be essential. There have been a variety of algorithms tools and therapeutic approaches of foreign rectal body insertion. Methods : A comprehensive systematic literature review on introduced for the management of extraction, however, Pubmed/ Medline and Google for ‘foreign bodies’ was performed because of the diversity of foreign bodies, improvisation, on January 14th 2018. A meta-analysis was carried out to evaluate as well creativity of the treating emergency physician the epidemiology, diagnostics and therapeutic techniques. 1,551 abstracts were identified, of which 54 articles were included. -

NEISS Coding Manual January 2018
NNEEIISSSS CCooddiinngg MMaannuuaall JJaannuuaarryy 22001188 NEISS – National Electronic Injury Surveillance System January 2018 Table of Contents Introduction ................................................................................................................................................. 1 General Instructions ................................................................................................................................... 1 General NEISS Reporting Rule .................................................................................................................. 1 Do Report .................................................................................................................................................. 1 Definitions .............................................................................................................................................. 2 Do Not Report ........................................................................................................................................... 3 Specific Coding Instructions ..................................................................................................................... 4 Medical Information Codes ........................................................................................................................ 4 Date of Treatment ..................................................................................................................................... 4 (8 spaces)................................................................................................................................................. -

Injury Description Codes Nature of Injury
Injury Description Codes Nature of Injury Code Narrative Description I. Specific Injury * 01. No Physical Injury i.e., Glasses, contact lenses, artificial appliance, replacement of artificial appliance 02. Amputation Cut off extremity, digit, protruding part of body, usually by surgery, i.e. leg, arm 03. Angina Pectoris Chest pain 04. Burn (Heat) Burns or scald. The effect of contact with hot substances. (Chemical) burns. tissue damage resulting from the corrosive action chemicals, fume, etc., (acids, alkalies) 07. Concussion Brain, cerebral 10. Contusion Bruise - intact skin surface hematoma 13. Crushing To grind, pound or break into small bits 16. Dislocation Pinched nerve, slipped/ruptured disc, herniated disc, sciatica, complete tear, HNP subluxtion, MD dislocation 19. Electric Shock Electrocution 22. Enucleation Removal of organ or tumor 25. Foreign Body * 28. Fracture Breaking of a bone or cartilage 30. Freezing Frostbite and other effects of exposure to low temperature 31. Hearing Loss or Impairment Traumatic only. A separate injury, not the sequelae of another injury 32. Heat Prostration Heat stroke, sun stroke, heat exhaustion, heat cramps and other effects of environmental heat. does not include sunburn 34. Hernia The abnormal protrusion of an organ or part through the containing wall of its cavity 36. Infection The invasion of a host by organisms such as bacteria, fungi, viruses, mold, protozoa or insects, with or without manifest disease. 37. Inflammation The reaction of tissue to injury characterized clinically by heat, swelling, redness and pain *Description intentionally left blank. May 25, 2021 Injury Description Codes Nature of Injury 38. Adverse reaction to a vaccination or * inoculation 40. -

Occupational Dusts Other Than Silica* by Kenneth M
Thorax: first published as 10.1136/thx.2.2.91 on 1 June 1947. Downloaded from Thorax (1947), 2, 91. DISEASES OF THE LUNG RESULTING FROM OCCUPATIONAL DUSTS OTHER THAN SILICA* BY KENNETH M. A. PERRY London It is only in recent years that considerable interest has been given to the dusts to which men are exposed at their work, even though silicosis is known to have occurred in prehistoric times. Many dusts are now recognized as dangerous, and in the extreme it may even be doubted whether any dust can be regarded as harmless. It is rational at least to suppose that the lung cannot become a physiological dust trap and yet retain its elasticity. It seems possible that any dust, no matter how innocuous in small concentrations, would in large enough quantity eventually overwhelm the defences of the lung and accumulate in such amounts as to impair function; such a form of lung disease would be the result of causes of a mechanical nature-the physical presence of large amounts of inert foreign material. The term "benign pneumoconiosis " has been given to this type of disease in order to contrast it with diseases resulting http://thorax.bmj.com/ from the inhalation of siliceous matter. But besides this group of conditions occupational dust may give rise to inflammatory lesions, allergic responses, and neoplastic changes. INFLAMMATORY CHANGES Inflammatory changes may be caused by inorganic metals, such as manganese, on September 24, 2021 by guest. Protected copyright. beryllium, vanadium, and osmium, giving.rise to a chemical pneumonitis; and by organic matter, such as decaying hay and grain, bagasse, cotton fibre, and similar substances where the aetiology is somewhat obscure, though fungi are frequently blamed. -

Foreign Body Imaging-Experience with 6 Cases of Retained Foreign Bodies in the Emergency
Arch Clin Med Case Rep 2020; 4 (5): 952-968 DOI: 10.26502/acmcr.96550285 Case Series Foreign Body Imaging-Experience with 6 Cases of Retained Foreign Bodies in the Emergency Radiology Unit Muniraju Maralakunte MD1, Uma Debi MD1*, Lokesh Singh MD1, Himanshu Pruthi MD1, Vikas Bhatia MD, DNB DM1, Gita Devi MD1, Sandhu MS MD1 2Department of Radio diagnosis, PGIMER, Chandigarh, India *Corresponding Author: Dr. Uma Debi, Radiodiagnosis and Imaging, PGIMER, Chandigarh, India, Tel: 0091- 172-2756381; Fax: 0091-172-2745768; E-mail: [email protected] Received: 22 June 2020; Accepted: 14 August 2020; Published: 21 September 2020 Abstract Introduction: Retained foreign bodies are the external objects lying within the body, which are placed with voluntary or involuntary intentions. The involuntarily or accidentally, and complicated cases with the retained foreign body may come to the emergency services, which may require rapid and adequate imaging assessment. Materials and methods: We share our experience with six different cases with retained foreign bodies, who visited emergency radiological services with acute presentation of symptoms. The choice of radiological investigation considered based on the clinical presentation of the subjects with a retained foreign body. Conclusion: Patients with the retained foreign body may present acute symptoms to the emergency medical or surgical services, radiologists play a central role in rapid imaging evaluation. Radiological investigation plays a crucial role in identification, localization, characterization, and reporting the complication of the retained foreign bodies, and in many scenarios, radiological investigations may expose the unsuspected or concealed foreign bodies in the human body. Ultimately radiological services are useful rapid assessment tools that aid in triage and guide in the medical or surgical management of patients with a retained foreign body. -

Using Injury Narrative with Tri-Code to Obtain Accurate Diagnosis Codes and Scoring
Injury Coding – Using Injury Narrative with Tri-Code to Obtain Accurate Diagnosis Codes and Scoring Injury Coding Webinar Series James Pou Product Strategy - Product Manager Digital Innovation - eso.com powered by Copyright © 2020 ESO Inc. All Rights Reserved. powered by Objectives • Search for and abstract the additional detail to support ICD10 Injury coding. • Enter narrative and code using Tri-Code to accurately assign ICD10-CM and AIS. © Copyright 2020 ESO Inc. All Rights Reserved. Tri-Code and Injury Coding in ICD10 powered by • Two methods of coding in Tri-Code • Code by narrative description of injury. Consists of the following: • One injury per line which includes: • Organ or body part • Description of injury • Extent of injury • Code by ICD10 injury code: • Enter each ICD10 Injury Diagnosis on a separate lines © Copyright 2020 ESO Inc. All Rights Reserved. Using Tri-Code powered by • Narrative Based Coding: • Complete set of Guidelines available –Tri-Code for ICD10 Guidelines – ICD10-CM with AIS 2005 Update 2008 • Includes detailed guidelines by AIS chapter. © Copyright 2020 ESO Inc. All Rights Reserved. powered by Narrative Development Guidelines • Cornerstone of accurate injury coding – Good abstraction of injuries from the medical record. • Abstraction Recommendations • Read entire patient chart – In particular focus on: • Radiological results • Operative reports (tells you what has been fixed that was injured) • Consult reports • Discharge abstracts • Autopsy reports (if can be obtained for deaths) © Copyright 2020 ESO Inc. -

Airbag Pneumonitis
Hindawi Publishing Corporation Case Reports in Medicine Volume 2010, Article ID 498569, 2 pages doi:10.1155/2010/498569 Case Report Airbag Pneumonitis Raghav Govindarajan, Gustavo Ferrer, Laurence A. Smolley, Eduardo Araujo Oliveira, and Franck Rahaghi Department of Pulmonary Medicine, Cleveland Clinic Florida, 2950 Cleveland Clinic Boulevard, Weston, FL 33331, USA Correspondence should be addressed to Raghav Govindarajan, [email protected] Received 29 June 2010; Accepted 13 September 2010 Academic Editor: Steven A. Sahn Copyright © 2010 Raghav Govindarajan et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. The widespread and mandatory use of airbags has resulted in various patterns of injuries and complications unique to their use. Airbags have been implicated in a spectrum of pulmonary conditions ranging from exacerbation of asthma, reactive airway diseases to new onset asthma. We report a case of inhalational chemical pneumonitis that developed after exposure to the airbag fumes. 1. Introduction room air. There were no significant electrolyte abnormalities. Chest X-ray PA and lateral view revealed left lower lobe and ffi The 2001 United States national highway tra csafety retocardiac infiltrate. CT chest noncontrast revealed tree in administration report estimated that airbags reduce driver bud opacities in the right middle lobe, left lingual. Ground fatality by 12%–14% [1].The widespread and mandatory glass opacity was also seen in the posterior basal segment of use of airbags has resulted in various patterns of injuries the left lower lobe (Figure 1). -

Thirty Workers in Missouri Popcorn Plant Diagnosed With
Occupational Lung SSSEEENNNSSSOOORRR Disease Bulletin Massachusetts Department of Public Health Occupational Health Surveillance Program, 250 Washington Street, 6th Floor, Boston, MA 02108 Tel: (617) 624-5632 Fax: (617) 624-5696 www.mass.gov/dph/ohsp June 2006 Dear Health Care Provider, An investigation of the workplace revealed that diacetyl, Welcome to the June issue of the SENSOR an artificial butter flavoring ingredient, was linked with the Occupational Lung Disease Bulletin! In this issue, we employees’ symptoms. Animal studies conducted by focus on the topic of bronchiolitis obliterans, a severe lung flavoring manufacturers as early as 1993 showed that disease that can occur in workers that make or handle inhalation of diacetyl resulted in severe lung injury. food flavoring. Bronchiolitis obliterans has been linked to Additional studies completed in 2002 confirmed these diacetyl, an artificial butter flavoring ingredient. The findings1. The National Institute for Occupational Safety illness has been called “popcorn lung disease” because of and Health (NIOSH) issued an alert in 2004, warning of the clusters of workers in popcorn plants that have been the danger posed by vapors, dusts or sprays of flavorings diagnosed with the disease. However, workers in plants and recommending controls to ensure worker safety in making food ranging from pastries and frozen food to plants using or making flavorings. NIOSH recommended nacho chips and candy may be exposed to the chemicals substituting less hazardous flavoring ingredients as the in food flavorings, and therefore may be at risk for best option for controlling health risks to workers. bronchiolitis obliterans. In addition, workers who use Additional options include local exhaust ventilation or, if diacetyl to produce artificial flavorings are also at risk.