A Patient's Guide to Clavicle Fractures (Fractures of the Collarbone)
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Body Mechanics As the Rotator Cuff Gether in a Cuff-Shape Across the Greater and Lesser Tubercles the on Head of the Humerus
EXPerT CONTENT Body Mechanics by Joseph E. Muscolino | Artwork Giovanni Rimasti | Photography Yanik Chauvin Rotator Cuff Injury www.amtamassage.org/mtj WORKING WITH CLieNTS AFFecTED BY THIS COmmON CONDITION ROTATOR CUFF GROUP as the rotator cuff group because their distal tendons blend and attach to- The four rotator cuff muscles are gether in a cuff-shape across the greater and lesser tubercles on the head of the supraspinatus, infraspinatus, the humerus. Although all four rotator cuff muscles have specific concen- teres minor, and subscapularis (Fig- tric mover actions at the glenohumeral (GH) joint, their primary functional ure 1). These muscles are described importance is to contract isometrically for GH joint stabilization. Because 17 Before practicing any new modality or technique, check with your state’s or province’s massage therapy regulatory authority to ensure that it is within the defined scope of practice for massage therapy. the rotator cuff group has both mover and stabilization roles, it is extremely functionally active and therefore often physically stressed and injured. In fact, after neck and low back conditions, the shoulder is the most com- Supraspinatus monly injured joint of the human body. ROTATOR CUFF PATHOLOGY The three most common types of rotator cuff pathology are tendinitis, tendinosus, and tearing. Excessive physi- cal stress placed on the rotator cuff tendon can cause ir- ritation and inflammation of the tendon, in other words, tendinitis. If the physical stress is chronic, the inflam- matory process often subsides and degeneration of the fascial tendinous tissue occurs; this is referred to as tendinosus. The degeneration of tendinosus results in weakness of the tendon’s structure, and with continued Teres minor physical stress, whether it is overuse microtrauma or a macrotrauma, a rotator cuff tendon tear might occur. -

Altered Alignment of the Shoulder Girdle and Cervical Spine in Patients with Insidious Onset Neck Pain and Whiplash- Associated Disorder
Journal of Applied Biomechanics, 2011, 27, 181-191 © 2011 Human Kinetics, Inc. Altered Alignment of the Shoulder Girdle and Cervical Spine in Patients With Insidious Onset Neck Pain and Whiplash- Associated Disorder Harpa Helgadottir, Eythor Kristjansson, Sarah Mottram, Andrew Karduna, and Halldor Jonsson, Jr. Clinical theory suggests that altered alignment of the shoulder girdle has the potential to create or sustain symptomatic mechanical dysfunction in the cervical and thoracic spine. The alignment of the shoulder girdle is described by two clavicle rotations, i.e, elevation and retraction, and by three scapular rotations, i.e., upward rotation, internal rotation, and anterior tilt. Elevation and retraction have until now been assessed only in patients with neck pain. The aim of the study was to determine whether there is a pattern of altered alignment of the shoulder girdle and the cervical and thoracic spine in patients with neck pain. A three-dimensional device measured clavicle and scapular orientation, and cervical and thoracic alignment in patients with insidious onset neck pain (IONP) and whiplash-associated disorder (WAD). An asymptomatic control group was selected for baseline measurements. The symptomatic groups revealed a significantly reduced clavicle retraction and scapular upward rotation as well as decreased cranial angle. A difference was found between the symptomatic groups on the left side, whereas the WAD group revealed an increased scapular anterior tilt and the IONP group a decreased clavicle elevation. These changes may be an important mechanism for maintenance and recurrence or exacerbation of symptoms in patients with neck pain. Keywords: neck pain, whiplash, scapula, posture Clinical theory suggests that altered alignment of of Biomechanics. -

The Appendicular Skeleton Appendicular Skeleton
THE SKELETAL SYSTEM: THE APPENDICULAR SKELETON APPENDICULAR SKELETON The primary function is movement It includes bones of the upper and lower limbs Girdles attach the limbs to the axial skeleton SKELETON OF THE UPPER LIMB Each upper limb has 32 bones Two separate regions 1. The pectoral (shoulder) girdle (2 bones) 2. The free part (30 bones) THE PECTORAL (OR SHOULDER) GIRDLE UPPER LIMB The pectoral girdle consists of two bones, the scapula and the clavicle The free part has 30 bones 1 humerus (arm) 1 ulna (forearm) 1 radius (forearm) 8 carpals (wrist) 19 metacarpal and phalanges (hand) PECTORAL GIRDLE - CLAVICLE The clavicle is “S” shaped The medial end articulates with the manubrium of the sternum forming the sternoclavicular joint The lateral end articulates with the acromion forming the acromioclavicular joint THE CLAVICLE PECTORAL GIRDLE - CLAVICLE The clavicle is convex in shape anteriorly near the sternal junction The clavicle is concave anteriorly on its lateral edge near the acromion CLINICAL CONNECTION - FRACTURED CLAVICLE A fall on an outstretched arm (F.O.O.S.H.) injury can lead to a fractured clavicle The clavicle is weakest at the junction of the two curves Forces are generated through the upper limb to the trunk during a fall Therefore, most breaks occur approximately in the middle of the clavicle PECTORAL GIRDLE - SCAPULA Also called the shoulder blade Triangular in shape Most notable features include the spine, acromion, coracoid process and the glenoid cavity FEATURES ON THE SCAPULA Spine - -

Bone Limb Upper
Shoulder Pectoral girdle (shoulder girdle) Scapula Acromioclavicular joint proximal end of Humerus Clavicle Sternoclavicular joint Bone: Upper limb - 1 Scapula Coracoid proc. 3 angles Superior Inferior Lateral 3 borders Lateral angle Medial Lateral Superior 2 surfaces 3 processes Posterior view: Acromion Right Scapula Spine Coracoid Bone: Upper limb - 2 Scapula 2 surfaces: Costal (Anterior), Posterior Posterior view: Costal (Anterior) view: Right Scapula Right Scapula Bone: Upper limb - 3 Scapula Glenoid cavity: Glenohumeral joint Lateral view: Infraglenoid tubercle Right Scapula Supraglenoid tubercle posterior anterior Bone: Upper limb - 4 Scapula Supraglenoid tubercle: long head of biceps Anterior view: brachii Right Scapula Bone: Upper limb - 5 Scapula Infraglenoid tubercle: long head of triceps brachii Anterior view: Right Scapula (with biceps brachii removed) Bone: Upper limb - 6 Posterior surface of Scapula, Right Acromion; Spine; Spinoglenoid notch Suprspinatous fossa, Infraspinatous fossa Bone: Upper limb - 7 Costal (Anterior) surface of Scapula, Right Subscapular fossa: Shallow concave surface for subscapularis Bone: Upper limb - 8 Superior border Coracoid process Suprascapular notch Suprascapular nerve Posterior view: Right Scapula Bone: Upper limb - 9 Acromial Clavicle end Sternal end S-shaped Acromial end: smaller, oval facet Sternal end: larger,quadrangular facet, with manubrium, 1st rib Conoid tubercle Trapezoid line Right Clavicle Bone: Upper limb - 10 Clavicle Conoid tubercle: inferior -
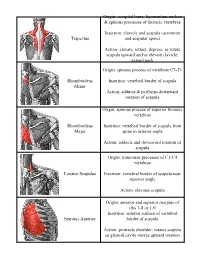
Trapezius Origin: Occipital Bone, Ligamentum Nuchae & Spinous Processes of Thoracic Vertebrae Insertion: Clavicle and Scapul
Origin: occipital bone, ligamentum nuchae & spinous processes of thoracic vertebrae Insertion: clavicle and scapula (acromion Trapezius and scapular spine) Action: elevate, retract, depress, or rotate scapula upward and/or elevate clavicle; extend neck Origin: spinous process of vertebrae C7-T1 Rhomboideus Insertion: vertebral border of scapula Minor Action: adducts & performs downward rotation of scapula Origin: spinous process of superior thoracic vertebrae Rhomboideus Insertion: vertebral border of scapula from Major spine to inferior angle Action: adducts and downward rotation of scapula Origin: transverse precesses of C1-C4 vertebrae Levator Scapulae Insertion: vertebral border of scapula near superior angle Action: elevates scapula Origin: anterior and superior margins of ribs 1-8 or 1-9 Insertion: anterior surface of vertebral Serratus Anterior border of scapula Action: protracts shoulder: rotates scapula so glenoid cavity moves upward rotation Origin: anterior surfaces and superior margins of ribs 3-5 Insertion: coracoid process of scapula Pectoralis Minor Action: depresses & protracts shoulder, rotates scapula (glenoid cavity rotates downward), elevates ribs Origin: supraspinous fossa of scapula Supraspinatus Insertion: greater tuberacle of humerus Action: abduction at the shoulder Origin: infraspinous fossa of scapula Infraspinatus Insertion: greater tubercle of humerus Action: lateral rotation at shoulder Origin: clavicle and scapula (acromion and adjacent scapular spine) Insertion: deltoid tuberosity of humerus Deltoid Action: -

Complications Associated with Clavicular Fracture
NOR200061.qxd 9/11/09 1:23 PM Page 217 Complications Associated With Clavicular Fracture George Mouzopoulos ▼ Emmanuil Morakis ▼ Michalis Stamatakos ▼ Mathaios Tzurbakis The objective of our literature review was to inform or- subclavian vein, due to its stable connection with the thopaedic nurses about the complications of clavicular frac- clavicle via the cervical fascia, can also be subjected to ture, which are easily misdiagnosed. For this purpose, we injuries (Casbas et al., 2005). Damage to the internal searched MEDLINE (1965–2005) using the key words clavicle, jugular vein, the suprascapular artery, the axillary, and fracture, and complications. Fractures of the clavicle are usu- carotid artery after a clavicular fracture has also been ally thought to be easily managed by symptomatic treatment reported (Katras et al., 2001). About 50% of injuries to the subclavian arteries are in a broad arm sling. However, it is well recognized that not due to fractures of the clavicle because the proximal all clavicular fractures have a good outcome. Displaced or part is dislocated superiorly by the sternocleidomas- comminuted clavicle fractures are associated with complica- toid, causing damage to the vessel (Sodhi, Arora, & tions such as subclavian vessels injury, hemopneumothorax, Khandelwal, 2007). If no injury happens during the ini- brachial plexus paresis, nonunion, malunion, posttraumatic tial displacement of the fractured part, then it is un- arthritis, refracture, and other complications related to os- likely to happen later, because the distal segment is dis- teosynthesis. Herein, we describe what the orthopaedic nurse placed downward and forward due to shoulder weight, should know about the complications of clavicular fractures. -

Evaluation of Humeral and Glenoid Bone Deformity in Glenohumeral Arthritis 5
Evaluation of Humeral and Glenoid Bone Deformity 1 in Glenohumeral Arthritis Brian F. Grogan and Charles M. Jobin Introduction glenoid bone wear helps the surgeon formulate a successful treatment plan and surgical goals Glenohumeral arthritis is the sequela of a vari- to address the pathoanatomy and improve the ety of pathologic shoulder processes, most durability of shoulder arthroplasty. The evalu- commonly degenerative osteoarthritis, but may ation of humeral and glenoid bone deformity also be secondary to post-traumatic conditions, in glenohumeral arthritis has profound surgical inflammatory arthritis, rotator cuff tear arthrop- implications and is fundamental to successful athy, and postsurgical conditions most com- shoulder arthroplasty. monly post-capsulorrhaphy arthritis. Patients with glenohumeral arthritis commonly demon- strate patterns of bony deformity on the glenoid Glenoid Deformity in Osteoarthritis and humerus that are caused by the etiology of the arthritis. For example, osteoarthritis com- Glenoid deformity and glenohumeral subluxation monly presents with posterior glenoid wear, are commonly seen in the setting of primary osteo- secondary glenoid retroversion, and posterior arthritis of the glenohumeral joint. The glenoid humeral head subluxation, while inflammatory wear tends to occur posteriorly and may be best arthritis routinely causes concentric glenoid viewed on axial radiographs or computed tomog- wear with central glenoid erosion. A thorough raphy (CT) axial images. Glenoid erosion, as first history and physical, as well as laboratory and characterized by Walch, is noted to be either central radiographic workup, are keys to understanding or posterior, with varying degrees of wear and pos- the etiology of arthritis and understanding the terior subluxation of the humerus [1, 2] (Fig. -

Avulsion Fracture of Brachioradialis Muscle Origin: an Exceedingly Rare Entity: a Case Report
10-039_OA1 8/13/16 5:34 PM Page 50 Malaysian Orthopaedic Journal 2016 Vol 10 No 2 Behera G, et al http://dx.doi.org/10.5704/MOJ.1607.010 Avulsion Fracture of Brachioradialis Muscle Origin: An Exceedingly Rare Entity: A Case Report Behera G, DNB, Balaji G, MS Ortho, Menon J, MRCS (Edin.), Sharma D, MCH, Komuravalli VK, DNB Jawaharlal Institute of Postgraduate Medical Education and Research (JIPMER), Puducherry, India Date of submission: March 2016 Date of acceptance: June 2016 ABSTRACT lateral supracondylar ridge just proximal to the lateral epicondyle. He had restriction of active terminal elbow Avulsion fracture of the brachioradialis origin at its proximal extension by 10 degrees with near normal active elbow attachment on the lateral supracondylar ridge of the distal flexion, pronation and supination. Active flexion and humerus is exceedingly rare, and only two cases have been extension at wrist were painful along with the painful reported in the literature so far. In this article, we present a terminal elbow extension. There was significant pain at the 38 years old patient who sustained a closed avulsion fracture lateral distal humerus when active elbow flexion against of the lateral supracondylar ridge of left humerus at the resistance was performed in the mid-pronated position of the proximal attachment of brachioradialis following a fall forearm. There was no distal neurovascular deficit. backwards on outstretched hand after being struck by a lorry from behind while riding on a two-wheeler (motorcycle). He Antero-posterior (AP) plain radiograph of the left elbow was managed with above elbow plaster for four weeks showed a fracture of the lateral distal humerus at the followed by elbow and wrist mobilization. -

Humerus Fracture
Portsmouth Hospitals NHS Trust Virtual Fracture Clinic Patient information Humerus Fracture Specialist Support This leaflet can be made available in another language, large print or another format. Please speak to the Virtual Fracture Clinic who can advise you Humerus VFC DCR leaflet 18 5871.indd 1 12/12/2018 09:42:15 This information leaflet follows up your recent conversation with the Fracture Clinic, where your case was reviewed by an orthopaedic Consultant (Bone specialist). You have sustained a fracture (break) to your Humerus (upper arm bone). The Virtual Fracture Clinic letter will detail where the fracture is. This is a very painful injury due to muscle spasms and the bone ends moving. Regular painkillers will be required during your healing stage to aid recovery. The treatment centre you attended will have provided you with a type of sling called a “collar and cuff”. This is the correct type of sling initially for this type of injury. This should be worn at all times. If you are worried that you are unable to follow this rehabilitation plan, or have any questions, then please contact us by using the contact numbers on the front of this leaflet. Healing: It takes approximately 12 weeks to heal. To fully resolve can take up to 1 year. Pain and This can be a painful injury. You are likely to swelling: experience significant swelling & bruising that can track down your chest, arm and into your hand. Take regular painkillers and ensure regular movement of fingers wrist and elbow. You may find it easier to sleep in an upright position. -
Muscles of the Upper Limb.Pdf
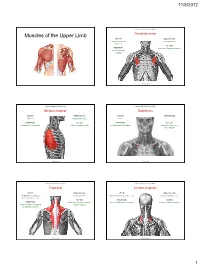
11/8/2012 Muscles Stabilizing Pectoral Girdle Muscles of the Upper Limb Pectoralis minor ORIGIN: INNERVATION: anterior surface of pectoral nerves ribs 3 – 5 ACTION: INSERTION: protracts / depresses scapula coracoid process (scapula) (Anterior view) Muscles Stabilizing Pectoral Girdle Muscles Stabilizing Pectoral Girdle Serratus anterior Subclavius ORIGIN: INNERVATION: ORIGIN: INNERVATION: ribs 1 - 8 long thoracic nerve rib 1 ---------------- INSERTION: ACTION: INSERTION: ACTION: medial border of scapula rotates scapula laterally inferior surface of scapula stabilizes / depresses pectoral girdle (Lateral view) (anterior view) Muscles Stabilizing Pectoral Girdle Muscles Stabilizing Pectoral Girdle Trapezius Levator scapulae ORIGIN: INNERVATION: ORIGIN: INNERVATION: occipital bone / spinous accessory nerve transverse processes of C1 – C4 dorsal scapular nerve processes of C7 – T12 ACTION: INSERTION: ACTION: INSERTION: stabilizes / elevates / retracts / upper medial border of scapula elevates / adducts scapula acromion / spine of scapula; rotates scapula lateral third of clavicle (Posterior view) (Posterior view) 1 11/8/2012 Muscles Stabilizing Pectoral Girdle Muscles Moving Arm Rhomboids Pectoralis major (major / minor) ORIGIN: INNERVATION: ORIGIN: INNERVATION: spinous processes of C7 – T5 dorsal scapular nerve sternum / clavicle / ribs 1 – 6 dorsal scapular nerve INSERTION: ACTION: INSERTION: ACTION: medial border of scapula adducts / rotates scapula intertubucular sulcus / greater tubercle flexes / medially rotates / (humerus) adducts -

Right Or Left Bones? Clavicle Ulna
Right or Left Bones? Clavicle Ulna . Together, the clavicles make a . Lay the ulna on the table. “handlebar” shape (low at the middle . Can you see the radial notch? of the chest, higher near the shoulders). o If yes, the open side of the . The blunt tip (sternal end) touches the trochlear (semilunar) notch tells sternum at the middle of the chest. you the bone orientation (see . The round tip (acromial end) touches the photo 1). scapula at the shoulder. o If no, the open side of the . The bumpy side of the clavicle faces the trochlear (semilunar) notch is the rib cage. opposite of the bone orientation . The smooth side of the clavicle faces (see photo 2). outward Radius Fibula . The styloid process always touches the . The smoother tip (head of the fibula) thumb. touches the knee. If the lower end of the radius (near the . The rougher tip (lateral malleolus) styloid process) is rough, you are touches the ankle. looking at the back of the wrist. The point of the lateral malleolus points . If the lower end of the radius is smooth, to the pinkie toe, not the middle of the you are looking at the inside of the wrist. foot. The front of the fibula (anterior view) has an edge. The back of the fibula (posterior view) is flat. References: University of Liverpool Faculty of Health and Life Sciences. (2013). Radius and ulna (right forearm) [Digital photograph]. Retrieved from https://www.flickr.com/photos/liverpoolhls/10819145494. . -

Discharge Instructions After Humerus/Clavicle Surgery
DISCHARGE INSTRUCTIONS AFTER HUMERUS/CLAVICLE SURGERY INCISIONAL CARE: •Dressings are to be kept clean and dry. A small amount of clear drainage or bleeding may take place. The dressing should be changed daily as instructed by the nursing staff. •Some swelling around the incision is normal. You will find it more comfortable to wear loose clothing to avoid pressure on the incision. •You may shower in 3 days. •Never, ever remove your own stitches or trim what may appear to be excess suture material. We will remove your stitches in the office at your post-op appointment. If you are concerned about your stitches or if they are bothering you, please call us. ICE THERAPY •Apply ice to your shoulder to help decrease pain and swelling. Use your Iceman machine 2-3 times per day for 20 minutes per session. Instructions are on the lid of the Iceman and in handout. ACTIVITY: •The arm should be kept in the shoulder sling until you are seen in the office. •You may want to place a pillow behind your elbow when seated or lying down to keep the surgery area forward to help decrease pain. •Don’t use the arm to push yourself up in bed or from a chair because this requires forceful contraction of muscles. Use the opposite arm. •Don’t lift anything heavier than a glass of water for the first 6 weeks after surgery. •Remember that you will probably tire more easily than usual. You may want to plan a rest period of 30 to 60 minutes mid-morning and midafternoon.