Stomach Tumors Benign Tumors Fundic Gland Polyps Benign
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Parietal Cell Hyperplasia Induced by Long-Term Administration of Antacids to Rats
Gut: first published as 10.1136/gut.19.9.798 on 1 September 1978. Downloaded from Gut, 1978, 19, 798-801 Parietal cell hyperplasia induced by long-term administration of antacids to rats G. MAZZACCA1, F. CASCIONE, G. BUDILLON, L. D'AGOSTINO, L. CIMINO, AND C. FEMIANO From the Division of Gastroenterology, 2nd School ofMedicine, University ofNaples, and the Department ofPathology, Institute for Tumoral Diseases, Naples, Italv SUMMARY Suspension of magnesium and aluminum hydroxide (30-60 mEq/24 h) or a comparable volume of water was orally administered by gastric intubation to two groups of 20 male wistar rats each over 60 days. The antacid treatment led to a significant increase in the height (0-464 + 0-02 mm v. 0-318 ± 0 06) and in the volume (472 ± 32 mm3 v. 328 ± 45) of the fundic mucosa ofthe stomach, in the average count of parietal cells per unit area of the mucosa (32-37 ± 1 8 v. 22-3 + 1 6), and in the total parietal cell population of the stomach (53-6 + 3.5 x 106 v. 43-2 + 3.7 x 106). Furthermore fasting serum gastrin concentration was significantly higher in the antacid treated rats (81.2 + 7.4 pg/ml) than in control animals (56-9 ± 6-9 pg/ml). It is known that a feedback mechanism governs the The animals of group B received each time and by relationship between antral gastrin release and the same procedure a comparable volume of water. intraluminal gastric pH (Walsh et al., 1975). During the night each animal was housed in a Furthermore, gastrin exerts a trophic influence on separate cage and the antacid suspension was the the gastric mucosa with increase in the parietal cell only drinking fluid available to the rats of group A. -

Overview of Gastrointestinal Function
Overview of Gastrointestinal Function George N. DeMartino, Ph.D. Department of Physiology University of Texas Southwestern Medical Center Dallas, TX 75390 The gastrointestinal system Functions of the gastrointestinal system • Digestion • Absorption • Secretion • Motility • Immune surveillance and tolerance GI-OP-13 Histology of the GI tract Blood or Lumenal Serosal Side or Mucosal Side Structure of a villus Villus Lamina propria Movement of substances across the epithelial layer Tight junctions X Lumen Blood Apical membrane Basolateral membrane X X transcellular X X paracellular GI-OP-19 Histology of the GI tract Blood or Lumenal Serosal Side or Mucosal Side Motility in the gastrointestinal system Propulsion net movement by peristalsis Mixing for digestion and absorption Separation sphincters Storage decreased pressure GI-OP-42 Intercellular signaling in the gastrointestinal system • Neural • Hormonal • Paracrine GI-OP-10 Neural control of the GI system • Extrinsic nervous system autonomic central nervous system • Intrinsic (enteric) nervous system entirely with the GI system GI-OP-14 The extrinsic nervous system The intrinsic nervous system forms complete functional circuits Sensory neurons Interneurons Motor neurons (excitatory and inhibitory) Parasympathetic nerves regulate functions of the intrinsic nervous system Y Reflex control of gastrointestinal functions Vago-vagal Afferent reflex Salivary Glands Composition of Saliva O Proteins α−amylase lactoferrin lipase RNase lysozyme et al mucus O Electrolyte solution water Na+ , K + - HCO3 -

Submucosa Precedes Lamina Propria in Initiating Fibrosis in Oral Submucous Fibrosis - Evidence Based on Collagen Histochemistry
SUBMUCOSA PRECEDES LAMINA PROPRIA IN INITIATING FIBROSIS IN ORAL SUBMUCOUS FIBROSIS - EVIDENCE BASED ON COLLAGEN HISTOCHEMISTRY. *Anna P. Joseph ** R. Rajendran Abstract Oral submucous fibrosis is a chronic insidious disease and a well-recognized potentially malignant condition of the oral cavity. It is a collagen related disorder associated with betel quid chewing and characterized by progressive hyalinization of the lamina propria. Objectives: It is traditionally held that in oral submucous fibrosis the hyalinization process starts from the lamina propria and progresses to involve the submucosal tissues. However reports of some investigators suggest that on the contrary, the fibrosis starts in the submucosa and not in the juxta epithelium as previously assumed. Methods: A histochemical study comparing the pattern of collagen deposition and hyalinization in early and advanced cases of oral submucous fibrosis was done using special stain for collagen. Result & Conclusion: The results suggest that in a certain percentage of cases submucosa precedes the lamina propria in initiating fibrosis in this disease. This could have implications on the differences in clinical presentation, biological progression, neoplastic transformation and responsiveness to treatment. Introduction fibrosis (OSF) is an insidious chronic fibrotic disease and a well recognized premalignant Fibrosis, a conspicuous feature of condition that involves the oral mucosa and chronically inflamed tissue is characterized by occasionally the pharynx and the upper progressive -

Normal Gross and Histologic Features of the Gastrointestinal Tract
NORMAL GROSS AND HISTOLOGIC 1 FEATURES OF THE GASTROINTESTINAL TRACT THE NORMAL ESOPHAGUS left gastric, left phrenic, and left hepatic accessory arteries. Veins in the proximal and mid esopha- Anatomy gus drain into the systemic circulation, whereas Gross Anatomy. The adult esophagus is a the short gastric and left gastric veins of the muscular tube measuring approximately 25 cm portal system drain the distal esophagus. Linear and extending from the lower border of the cri- arrays of large caliber veins are unique to the distal coid cartilage to the gastroesophageal junction. esophagus and can be a helpful clue to the site of It lies posterior to the trachea and left atrium a biopsy when extensive cardiac-type mucosa is in the mediastinum but deviates slightly to the present near the gastroesophageal junction (4). left before descending to the diaphragm, where Lymphatic vessels are present in all layers of the it traverses the hiatus and enters the abdomen. esophagus. They drain to paratracheal and deep The subdiaphragmatic esophagus lies against cervical lymph nodes in the cervical esophagus, the posterior surface of the left hepatic lobe (1). bronchial and posterior mediastinal lymph nodes The International Classification of Diseases in the thoracic esophagus, and left gastric lymph and the American Joint Commission on Cancer nodes in the abdominal esophagus. divide the esophagus into upper, middle, and lower thirds, whereas endoscopists measure distance to points in the esophagus relative to the incisors (2). The esophagus begins 15 cm from the incisors and extends 40 cm from the incisors in the average adult (3). The upper and lower esophageal sphincters represent areas of increased resting tone but lack anatomic landmarks; they are located 15 to 18 cm from the incisors and slightly proximal to the gastroesophageal junction, respectively. -

Anatomy, Histology, and Embryology
ANATOMY, HISTOLOGY, 1 AND EMBRYOLOGY An understanding of the anatomic divisions composed of the vomer. This bone extends from of the head and neck, as well as their associ- the region of the sphenoid sinus posteriorly and ated normal histologic features, is of consider- superiorly, to the anterior edge of the hard pal- able importance when approaching head and ate. Superior to the vomer, the septum is formed neck pathology. The large number of disease by the perpendicular plate of the ethmoid processes that involve the head and neck area bone. The most anterior portion of the septum is a reflection of the many specialized tissues is septal cartilage, which articulates with both that are present and at risk for specific diseases. the vomer and the ethmoidal plate. Many neoplasms show a sharp predilection for The supporting structure of the lateral border this specific anatomic location, almost never of the nasal cavity is complex. Portions of the occurring elsewhere. An understanding of the nasal, ethmoid, and sphenoid bones contrib- location of normal olfactory mucosa allows ute to its formation. The lateral nasal wall is visualization of the sites of olfactory neuro- distinguished from the smooth surface of the blastoma; the boundaries of the nasopharynx nasal septum by its “scroll-shaped” superior, and its distinction from the nasal cavity mark middle, and inferior turbinates. The small su- the interface of endodermally and ectodermally perior turbinate and larger middle turbinate are derived tissues, a critical watershed in neoplasm distribution. Angiofibromas and so-called lym- phoepitheliomas, for example, almost exclu- sively arise on the nasopharyngeal side of this line, whereas schneiderian papillomas, lobular capillary hemangiomas, and sinonasal intesti- nal-type adenocarcinomas almost entirely arise anterior to the line, in the nasal cavity. -

Ultrastructure of Endocrine-Like Cells in Lamina Propria of Human Gastric Mucosa
Gut: first published as 10.1136/gut.22.7.534 on 1 July 1981. Downloaded from Gut, 1981, 22, 534-541 Ultrastructure of endocrine-like cells in lamina propria of human gastric mucosa* J STACHURA, W J KRAUSE, AND K J IVEYt From the Veterans Administration Medical Center, Long Beach, California; University of California Irvine, Irvine, California; Department of Anatomy, University of Missouri School of Medicine, Columbia, Missouri; and the Institute ofPathology, Copernicus Medical Academy, Krakow, Polantd SUMMARY Endocrine cells of gastric and gut mucosa are commonly thought to be present only within mucosal glands. In a previous report, we described argyrophilic cells in the lamina propria in 40 % of surgical gastric specimens, using light microscopy. All these patients had chronic gastritis. Argyrophilia, however, is a non-specific reaction which could occur in other than endocrine cells. The present study was undertaken to describe the ultrastructure of argyrophil cells in the lamina propria. In five patients with chronic gastritis, endoscopic biopsies were taken from the fundic, intermediate, and pyloric areas of the stomach. Single and/or clustered argyophil cells were seen by light microscopy in the lamina propria of the intermediate and pyloric are.as. On electron- microscopy, these cells had the following characteristics of endocrine-like cells: they were characterised by numerous electron dense granules in the cytoplasm, 100-300 nm in diameter; the cytoplasm contained poorly-developed rough endoplasmic reticulum and well-developed smooth endoplasmic reticulum with occasional vesicles. Immunostaining gave negative results for various gastrointestinal hormones. These ultrastructural characteristics of lamina propria cells are similar to endocrine cells of the APUD series. -

The Gallbladder
The Gallbladder Anatomy of the gallbladder Location: Right cranial abdominal quadrant. In the gallbladder fossa of the liver. o Between the quadrate and right medial liver lobes. Macroscopic: Pear-shaped organ Fundus, body and neck. o Neck attaches, via a short cystic duct, to the common bile duct. Opens into the duodenum via sphincter of Oddi at the major duodenal papilla. Found on the mesenteric margin of orad duodenum. o 3-6 cm aboral to pylorus. 1-2cm of distal common bile duct runs intramural. Species differences: Dogs: o Common bile duct enters at major duodenal papilla. Adjacent to pancreatic duct (no confluence prior to entrance). o Accessory pancreatic duct enters at minor duodenal papilla. ± 2 cm aboral to major duodenal papilla. MAJOR conduit for pancreatic secretions. Cats: o Common bile duct and pancreatic duct converge before opening at major duodenal papilla. Thus, any surgical procedure that affects the major duodenal papilla can affect the exocrine pancreatic secretions in cats. o Accessory pancreatic duct only seen in 20% of cats. 1 Gallbladder wall: 5 histologically distinct layers. From innermost these include: o Epithelium, o Submucosa (consisting of the lamina propria and tunica submucosa), o Tunica muscularis externa, o Tunica serosa (outermost layer covers gallbladder facing away from the liver), o Tunica adventitia (outermost layer covers gallbladder facing towards the liver). Blood supply: Solely by the cystic artery (derived from the left branch of the hepatic artery). o Susceptible to ischaemic necrosis should its vascular supply become compromised. Function: Storage reservoir for bile o Concentrated (up to 10-fold), acidified (through epithelial acid secretions) and modified (by the addition of mucin and immunoglobulins) before being released into the gastrointestinal tract at the major duodenal. -

Expression of Cell Membrane Complement Regulatory Glycoproteins Along the Normal and Diseased Human Gastrointestinal Tract
522 Gut 1998;42:522–529 Expression of cell membrane complement regulatory glycoproteins along the normal and diseased human gastrointestinal tract Gut: first published as 10.1136/gut.42.4.522 on 1 April 1998. Downloaded from A E Berstad, P Brandtzaeg Abstract tract. Indeed, activated complement has been Background/Aims—Uncontrolled comple- detected in lesions of inflammatory bowel ment activation may be of immunopatho- disease,2–4 coeliac disease,5 and recently also in logical importance in inflammatory Helicobacter pylori gastritis.6 diseases of the gastrointestinal tract. Ex- Certain complement activation products, pression of membrane bound factors that notably the C3b fragment and the C5b-7 com- regulate complement activation was there- plex, can on their own—that is, without associ- fore studied in situ. ated antibody—bind to any nearby cell Methods—Frozen tissue specimens were membrane.7 Therefore it is crucial that com- obtained from patients with Helicobacter plement activity is tightly regulated. Mam- pylori gastritis, coeliac disease, Crohn’s malian cells are protected from complement disease, or ulcerative colitis, and from induced damage by a family of cell membrane histologically normal controls. Sections complement regulatory glycoproteins that were examined by immunofluorescence downregulate activation of homologous com- with monoclonal antibodies to protectin plement on their cell surface.8 Protectin (CD59), decay accelerating factor (DAF), (CD59) is broadly distributed on cells of and membrane cofactor protein (MCP). haemopoietic and non-haemopoietic origin79; Results—Protectin and MCP were widely it inhibits the formation of terminal comple- expressed in normal and diseased mu- ment complex by preventing the binding of C9 cosae. -

Correlation of Ultrasonographic Small Intestinal Wall Layering with Histology in Normal Dogs
Louisiana State University LSU Digital Commons LSU Master's Theses Graduate School 2015 Correlation of Ultrasonographic Small Intestinal Wall Layering with Histology in Normal Dogs Alexandre Benjamin Le Roux Louisiana State University and Agricultural and Mechanical College, [email protected] Follow this and additional works at: https://digitalcommons.lsu.edu/gradschool_theses Part of the Veterinary Medicine Commons Recommended Citation Le Roux, Alexandre Benjamin, "Correlation of Ultrasonographic Small Intestinal Wall Layering with Histology in Normal Dogs" (2015). LSU Master's Theses. 1148. https://digitalcommons.lsu.edu/gradschool_theses/1148 This Thesis is brought to you for free and open access by the Graduate School at LSU Digital Commons. It has been accepted for inclusion in LSU Master's Theses by an authorized graduate school editor of LSU Digital Commons. For more information, please contact [email protected]. CORRELATION OF ULTRASONOGRAPHIC SMALL INTESTINAL WALL LAYERING WITH HISTOLOGY IN NORMAL DOGS A Thesis Submitted to the Graduate Faculty of the Louisiana State University and Agricultural and Mechanical College in partial fulfillment of the requirements for the degree of Masters of Science in The School of Veterinary Medicine through The Department of Veterinary Clinical Sciences by Alexandre Benjamin Le Roux DrMedVet, Ecole Nationale Vétérinaire de Nantes, 2006 May 2015 To my parents, my family and all my friends, for their continuous support… ii ACKNOWLEDGMENTS Foremost, I would like to express my deepest gratitude to the members of my committee, Drs. Lorrie Gaschen, Frederic Gaschen, Abbigail Granger and Nathalie Rademacher for the continuous support and guidance that they gave me through my residency and Master program research, as well as during the preparation of this manuscript. -
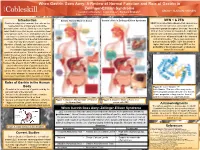
A Review of Normal Function and Role of Gastrin in Zollinger-Ellison
When Gastrin Goes Awry: A Review of Normal Function and Role of Gastrin in Zollinger-Ellison Syndrome Leigha LaTourette1, Janel Cross2, Barbara Brabetz2 Department of Plant and Animal Science1, Department of Natural Sciences and Mathematics2 Introduction Gastrin: Normal Mode of Action Gastrin’s Role in Zollinger-Ellison Syndrome MEN 1 & ZES Gastrin is a digestive hormone that acts on the MEN1 is an inheritable disease that causes over neuroendocrine and parietal cells of the secretion of hormones via tumors on the gastrointestinal tract to ultimately secrete gastric endocrine glands throughout the body.4 Around a acid. Gastrin secretion begins even before food 30% of these tumors are found to be malignant. is consumed, as the mere anticipation of a meal ZES is commonly associated with the MEN1 due can lead to a series of events ending in the to the presence of tumors found in the stomach creation of the gastric acid needed to breakdown and small intestine.4 These gastrointestinal foods. Not only does Gastrin support the tumors caused by MEN 1 give the person a digestion of foods, but it also stimulates growth, higher likelihood of contracting ZES, as the secretion, blood flow, and acts as a defense probability of having pancreatic or duodenal mechanism against bacteria in the tumors is increased.4 gastrointestinal system. When the production of Gastrin becomes overt, major consequences like that of Zollinger Ellison Syndrome (ZES). ZES is an extremely rare disease occurring in people between the ages of 30-60.4 ZES is related to the uncontrolled secretion of gastrin due to the presence of certain pancreatic or duodenal tumors. -

Terminology: Nomenclature of Mucosa-Associated Lymphoid Tissue
nature publishing group ARTICLES See COMMENTARY page 8 See REVIEW page 11 Terminology: nomenclature of mucosa-associated lymphoid tissue P B r a n d t z a e g 1 , H K i y o n o 2 , R P a b s t 3 a n d M W R u s s e l l 4 Stimulation of mucosal immunity has great potential in vaccinology and immunotherapy. However, the mucosal immune system is more complex than the systemic counterpart, both in terms of anatomy (inductive and effector tissues) and effectors (cells and molecules). Therefore, immunologists entering this field need a precise terminology as a crucial means of communication. Abbreviations for mucosal immune-function molecules related to the secretory immunoglobulin A system were defined by the Society for Mucosal Immunolgy Nomenclature Committee in 1997, and are briefly recapitulated in this article. In addition, we recommend and justify standard nomenclature and abbreviations for discrete mucosal immune-cell compartments, belonging to, and beyond, mucosa-associated lymphoid tissue. INTRODUCTION for dimers (and larger polymers) of IgA and pentamers of It is instructive to categorize various tissue compartments IgM was proposed in 1974. 3,4 The epithelial glycoprotein involved in mucosal immunity according to their main function. designated secretory component (SC) by WHO in 1972 However, until recently, there was no consensus in the scientific (previously called “ transport piece ” or “ secretory piece ” ) turned community as to how these compartments should be named and out to be responsible for the receptor-mediated transcytosis classified. This lack of standardized terminology has been particu- of J-chain-containing Ig polymers (pIgs) through secretory larly confusing for newcomers to the mucosal immunology field. -

Gastric Fundic Gland Polyps: Can Histology Be Useful to Predict Proton Pump Inhibitors Use?
AG-2018-75 ORIGINAL ARTICLE dx.doi.org/10.1590/S0004-2803.201800000-82 Gastric fundic gland polyps: can histology be useful to predict proton pump inhibitors use? Hugo Leite de Farias BRITO, Cynthia BARROS, Marcelle Vieira FREIRE, Miraldo Nascimento da SILVA FILHO and Tereza Virgínia NASCIMENTO Received 17/6/2018 Accepted 15/10/2018 ABSTRACT – Background – Fundic gland polyps allegedly increased in frequency in recent decades, and had attracted great attention due to possible association with prolonged proton pump inhibitor therapy. Prolonged use of this drug could cause parietal cell hyperplasia, obstruction of glandular lumen and cystic dilation of the gland. Objective – This study aims to analyze clinical and pathological features of fundic gland polyps in patients with and without proton pump inhibitor therapy in a selected population from Brazil. Methods – It was selected a sample of 101 Brazilian patients (78 females and 23 males), from a five years retrospective search of the files from a private pathology laboratory. The patients had an average age of 57 years and we included patients with a histological diagnosis of fundic gland polyp. The clinical data were obtained from their files and all histological slides were reviewed and examined with hematoxylin and eosin (HE) and Giemsa. Results – Information about the use or non-use of proton pump inhibitors (PPI) was obtained in 84 patient files. In 17 cases we could not determine if PPI were used or not. Among those in which the information was available, a positive history of anti-acid therapy was observed in 63 (75.0%) patients. Parietal cell hypertrophy/hyperplasia and parietal cell protrusions were detected in most slides.