A Closer Look: Documentation and Coding for Cardiac Conditions
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Follow-Up of 134 Pediatric Patients with Wolff-Parkinson-White Pattern: Natural Outcome and Medical Treatment
ORIGINAL ARTICLE Follow-up of 134 Pediatric Patients with Wolff-Parkinson-White Pattern: Natural Outcome and Medical Treatment AMALIA N. STEFANI, GABRIELA R. DAL FABBRO, MARÍA J. BOSALEH, ROBERTH VÁSQUEZ, GUSTAVO A. COSTA, RICARDO SPERANZA, JORGE L. GENTILE, CLAUDIO DE ZULOAGAMTSAC Received: 01/03/2013 ABSTRACT Accepted: 01/03/2013 Address for reprints: Objective Amalia N. Stefani The aim of the study was to evaluate the outcome of a pediatric population with Almafuerte 1722 ventricular pre-excitation pattern, supraventricular tachycardia, atrial fibrillation, (1650) San Martín, cardiomyopathies, mortality and medical treatment. Pcia. de Buenos Aires e-mail: [email protected] Methods From 1976 to 2011, a descriptive observational study was conducted on patients with ventricular pre-excitation in the electrocardiogram. All patients underwent an echocardiogram, 101(75.3%) Holter monitoring, and 69 (51.5%) an ergometric test. Radiofrequency ablation was performed in selected patients. Data were expressed as mean and standard deviation. Results The study population consisted of 134 patients; 80 (59.7%) were male. Age at diag- nosis ranged from 2 days to 18 years (mean 6.5±5 years). Clinical follow-up lasted 1 month to 20 years (mean 3.6±3.9 years). Thirty five patients (26.1%) consulted for supraventricular tachycardia, 16 (11.9%) for ventricular pre-excitation, and the remaining 83 patients (61.9%) for other abnormalities. Seventy-six patients (56.7%) had left conduction pathway and 3 patients double conduction pathway. Sixteen pa- tients (11.9%) presented supraventricular tachycardia during follow-up. Overall, 51 patients (38%) had orthodromic tachycardia at 6.3±5.8 years, 10 patients during the neonatal period. -

ARIC Cohort Stroke Form Instructions STR, VERSION F Qxq, 01/23/2020
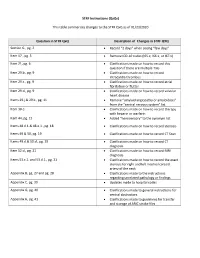
STRF Instructions (QxQs) This table summarizes changes to the STRF QxQ as of 01/23/2020 Question in STRF QxQ Description of Changes in STRF QXQ Section G., pg. 2 Record “2 days” when seeing “few days” Item 17., pg. 5 Remove ICD-10 codes (I65.x, I66.x, or I67.x) Item 21, pg. 6 Clarifications made on how to record this question if there are multiple TIAs Item 29.b., pg. 9 Clarifications made on how to record intracardia thrombus Item 29.c., pg. 9 Clarifications made on how to record atrial fibrillation or flutter Item 29.d., pg. 9 Clarifications made on how to record valvular heart disease Items 29.j.& 29.k., pg. 11 Remove “amyloid angiopathy or amyloidosis” from the “central nervous system” list Item 30.e. Clarifications made on how to record therapy with heparin or warfarin Item 44, pg. 15 Added “hemisensory” to the synonym list Items 48.d.1.& 48.e.1., pg. 18 Clarifications made on how to record stenosis Items 49 & 50, pg. 19 Clarifications made on how to record CT Scan Items 49.d.& 50.d., pg. 19 Clarifications made on how to record CT diagnosis Item 52.d., pg. 21 Clarifications made on how to record MRI diagnosis Items 53.c.1. and 53.d.1., pg. 21 Clarifications made on how to record the exact stenosis for right and left internal carotid artery of the neck Appendix B, pg. 27 and pg. 28 Clarifications made to the instructions regarding unrelated pathology or findings Appendix C, pg. 30 Updates made to hospital codes Appendix G, pg. -

ICD-9-ICD-10 Codes for Cardiology
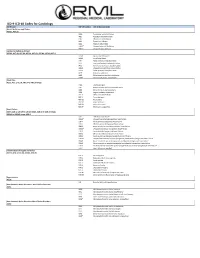
ICD-9-ICD-10 Codes for Cardiology ICD-9 Code ICD-10 Code(s) ICD-10 Descrption(s) Atrial Fibrillation and Flutter 427.31, 427.32 I48.0 Paroxysmal atrial fibrillation I48.1 Persistent atrial fibrillation I48.2 Chronic atrial fibrillation I48.3 Typical atrial flutter I48.4 Atypical atrial flutter I48.91* Unspecified atrial fibrillation I48.92* Unspecified atrial flutter Cardiac Arrhythmias (Other) 427.41, 427.42, 427.60, 427.61, 427.69, 427.81, 427.89, 427.9 I49.01 Ventricular fibrillation I49.02 Ventricular flutter I49.1 Atrial premature depolarization I49.2 Junctional premature depolarization I49.3 Ventricular premature depolarization I49.40 Unspecified premature depolarization I49.49 Other premature depolarization I49.5 Sick sinus syndrome I49.8 Other specified cardiac arrhythmias I49.9* Cardiac arrhythmia, unspecified Chest Pain 411.1, 413.1, 413.9, 786.50 to 786.59 range I20.0 Unstable angina I20.1 Angina pectoris with documented spasm I20.8 Other forms of angina pectoris I20.9 Angina pectoris, unspecified R07.1 Chest pain on breathing R07.2 Precordial pain R07.81 Pleurodynia R07.82 Intercostal pain R07.89 Other chest pain R07.9* Chest pain, unspecified Heart Failure 428.0, 428.1, 428.20 to 428.23 range, 428.30 to 428.33 range, 428.40 to 428.43 range, 428.9 I50.1 Left ventricular failure I50.20* Unspecified systolic (congestive) heart failure I50.21 Acute systolic (congestive) heart failure I50.22 Chronic systolic (congestive) heart failure I50.23 Acute on chronic systolic (congestive) heart failure I50.30* Unspecified diastolic (congestive) -

PAROXYSMAL VENTRICULAR TACHYCARDIA OCCURRING in a NORMAL HEART by DAVID ROMNEY, M.B., B.Ch.(Dub.) Ex-Senior House Officer in Medicine, St
Postgrad Med J: first published as 10.1136/pgmj.31.354.191 on 1 April 1955. Downloaded from I9I -J PAROXYSMAL VENTRICULAR TACHYCARDIA OCCURRING IN A NORMAL HEART By DAVID ROMNEY, M.B., B.Ch.(Dub.) Ex-Senior House Officer in Medicine, St. James's Hospital, Balham It is widely taught-and rightly so-that by sinus pressure will, of course, not affect the paroxysmal ventricular tachycardia is one of the rate in ventricular tachycardia. rarer arrhythmias, and is associated with grave In I953 Froment, Gallavardin and Cahen myocardial damage, with special reference to myo- offered a classification of various forms of cardial infarction. It is the least common, and paroxysmal ventricular tachycardia, and included most serious of the paroxysmal tachycardias, some case report. They described the following which contain four varieties of arrhythmia: supra- groups:- ventricular (auricular and nodal) 60 per cent.; (i) Terminal prefibrillatory ventricular tachy- auricular fibrillation, 30 per cent.; auricular flutter, cardia. 6 per cent.; and ventricular tachycardia, 4 per (ii) Curable and mild monomorphic extra- cent. systoles, with paroxysms of tachycardia. Figures from various sources (Campbell, 1947) (iii) Paroxysmal ventricular tachycardia due toby copyright. would indicate that in the latter group, four-fifths a lesion of the ventricular septum. of the cases had seriously damaged hearts. In (iv) Persistent and prolonged ventricular tachy- the remaining fifth no cause was found for the cardia developing in sound hearts, usually paroxysms. Paroxysmal ventricular tachycardia is in young subjects. more common in men than in women in the proportion of about 3.2. This arrhythmia was Case Report first identified by Sir Thomas Lewis in I909 and A married woman, aged 48, first became aware Gallavardin (1920, I921, 1922) emphasized the in 1948 of a paroxysm which caused alarm, faint- seriousness of the 'terminal ven- ness and It lasted a short pre-fibrillatory collapse. -

Pub 100-04 Medicare Claims Processing Centers for Medicare & Medicaid Services (CMS) Transmittal 3054 Date: August 29, 2014 Change Request 8803
Department of Health & CMS Manual System Human Services (DHHS) Pub 100-04 Medicare Claims Processing Centers for Medicare & Medicaid Services (CMS) Transmittal 3054 Date: August 29, 2014 Change Request 8803 SUBJECT: Ventricular Assist Devices for Bridge-to-Transplant and Destination Therapy I. SUMMARY OF CHANGES: This Change Request (CR) is effective for claims with dates of service on and after October 30, 2013; contractors shall pay claims for Ventricular Assist Devices as destination therapy using the criteria in Pub. 100-03, part 1, section 20.9.1, and Pub. 100-04, Chapter 32, sec. 320. EFFECTIVE DATE: October 30, 2013 *Unless otherwise specified, the effective date is the date of service. IMPLEMENTATION DATE: September 30, 2014 Disclaimer for manual changes only: The revision date and transmittal number apply only to red italicized material. Any other material was previously published and remains unchanged. However, if this revision contains a table of contents, you will receive the new/revised information only, and not the entire table of contents. II. CHANGES IN MANUAL INSTRUCTIONS: (N/A if manual is not updated) R=REVISED, N=NEW, D=DELETED-Only One Per Row. R/N/D CHAPTER / SECTION / SUBSECTION / TITLE D 3/90.2.1/Artifiical Hearts and Related Devices R 32/Table of Contents N 32/320/Artificial Hearts and Related Devices N 32/320.1/Coding Requirements for Furnished Before May 1, 2008 N 32/320.2/Coding Requirements for Furnished After May 1, 2008 N 32/320.3/ Ventricular Assist Devices N 32/320.3.1/Postcardiotomy N 32/320.3.2/Bridge-To -Transplantation (BTT) N 32/320.3.3/Destination Therapy (DT) N 32/320.3.4/ Other N 32/320.4/ Replacement Accessories and Supplies for External Ventricular Assist Devices or Any Ventricular Assist Device (VAD) III. -

View Pdf Copy of Original Document
Phenotype definition for the Vanderbilt Genome-Electronic Records project Identifying genetics determinants of normal QRS duration (QRSd) Patient population: • Patients with DNA whose first electrocardiogram (ECG) is designated as “normal” and lacking an exclusion criteria. • For this study, case and control are drawn from the same population and analyzed via continuous trait analysis. The only difference will be the QRSd. Hypothetical timeline for a single patient: Notes: • The study ECG is the first normal ECG. • The “Mildly abnormal” ECG cannot be abnormal by presence of heart disease. It can have abnormal rate, be recorded in the presence of Na-channel blocking meds, etc. For instance, a HR >100 is OK but not a bundle branch block. • Y duration = from first entry in the electronic medical record (EMR) until one month following normal ECG • Z duration = most recent clinic visit or problem list (if present) to one week following the normal ECG. Labs values, though, must be +/- 48h from the ECG time Criteria to be included in the analysis: Criteria Source/Method “Normal” ECG must be: • QRSd between 65-120ms ECG calculations • ECG designed as “NORMAL” ECG classification • Heart Rate between 50-100 ECG calculations • ECG Impression must not contain Natural Language Processing (NLP) on evidence of heart disease concepts (see ECG impression. Will exclude all but list below) negated terms (e.g., exclude those with possible, probable, or asserted bundle branch blocks). Should also exclude normalization negations like “LBBB no longer present.” -

Polymorphic Catecholergic Ventricular Tachycardia
Polymorphic catecholergic ventricular tachycardia Author: Doctor Vincent Lucet1 Creation Date: March 2000 Update: August 2002 January 2004 Scientific Editor: Doctor Damien Bonnet 1pédiatrie générale, Château des Côtes, 78350 Les Loges En Josas, France. [email protected] Abstract Keywords Name of the disease and its synonyms Names of excluded diseases Diagnostic criteria/Definition Differential diagnosis Frequence Clinical description Management/treatment Etiology Biological diagnostic method Genetic counseling Unresolved questions and comments References Abstract Identified in 1978, catecholaminergic polymorphic ventricular tachycardia mainly occurs in children over 3 years old with apparently healthy hearts. It is a primary dysrhythmia usually discovered during the work-up conducted after syncope with or without seizure. Syncopes mainly occur during exertion or emotional experiences. The electrocardiogram is normal (particularly the QT interval). During exercise or acceleration of the sinus rhythm, stereotyped and repetitive ventricular extrasystoles appear: first isolated and monomorphic, they become polymorphic and occur in salvos, with bidirectional ventricular tachycardia. Ventricular arrhythmia may be very rapid and interspersed with bursts of supraventricular or junctional tachycardia. During the paroxysms, torsade en pointes and ventricular fibrillation may appear and sometimes revert spontaneously. The same arrhythmia can be induced by stress tests or injecting small doses of isoprenaline. Patients are treated with powerful beta-blockers with delayed action. The spontaneous outcome is poor: half of the untreated patients die before age of 20 years. The disorder, recently assigned to the group of rhythm channelopathies, is familial in 1/3 cases. Somes cases are associated with abnormal transmembrane calcium transport (a mutation of the cardiac ryanodine-receptor gene, RyR2, has been found in several families). -

Paroxysmal Auricular Tachycardia with Block Ralph M
Henry Ford Hospital Medical Journal Volume 3 | Number 3 Article 10 9-1955 Paroxysmal Auricular Tachycardia With Block Ralph M. Denham Follow this and additional works at: https://scholarlycommons.henryford.com/hfhmedjournal Part of the Life Sciences Commons, Medical Specialties Commons, and the Public Health Commons Recommended Citation Denham, Ralph M. (1955) "Paroxysmal Auricular Tachycardia With Block," Henry Ford Hospital Medical Bulletin : Vol. 3 : No. 3 , 154-160. Available at: https://scholarlycommons.henryford.com/hfhmedjournal/vol3/iss3/10 This Article is brought to you for free and open access by Henry Ford Health System Scholarly Commons. It has been accepted for inclusion in Henry Ford Hospital Medical Journal by an authorized editor of Henry Ford Health System Scholarly Commons. For more information, please contact [email protected]. PAROXYSMAL AURICULAR TACHYCARDIA WITH BLOCK RALPH M. DENHAM, M.D.* Paroxysmal auricular tachycardia is a relatively common arrhythmia. The rate is usually between 150 and 220 per minute and the ventricles usuafly respond to each auricular beat. The attacks are usually of abrupt onset and last a few minutes or a few hours. Rarely they may last several days. Vagal stimulation, digitalis and quinidine usually wifl stop the attack. Barker and co-workers^ point out that auricular tachycardia seldom occurs in patients who have had previous attacks of auricular flutter or fibrillation, and that these disturbances, which are caused by circus rhythm are uncommon in patients who have had auricular paroxysmal tachycardia. In 1943 Barker and co-workers^ stated that, "In rare instances of auricular paroxys mal tachycardia, the ventricles do not respond to each auricular beat in the usual manner." In their paper they reviewed seventeen previously reported cases and added eighteen additional cases of auricular tachycardia with block. -
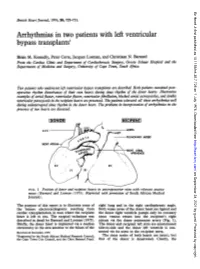
Arrhythmias in Two Patients with Left Ventricular Bypass Transplants'
Br Heart J: first published as 10.1136/hrt.38.7.725 on 1 July 1976. Downloaded from British Heart Journal, 1976, 38, 725-731. Arrhythmias in two patients with left ventricular bypass transplants' Brian M. Kennelly, Peter Corte, Jacques Losman, and Christiaan N. Barnard From the Cardiac Clinic and Department of Cardiothoracic Surgery, Groote Schuur Hospital and the Departments of Medicine and Surgery, University of Cape Town, South Africa Two patients who underwvent left ventricular bypass transplants are described. Both patients sustained post- operative rhythm disturbances of their own hearts during sinus rhythm of the donor hearts. Illustrative examples of atrialflutter, ventricular flutter, ventricular fibrillation, blocked atrial extrasystoles, and double ventricular parasystole in the recipient hearts are presented. The patients tolerated all these arrhythmias well during uninterrupted sinus rhythm in the donor heart. The problems in interpretation of arrhythmias in the presence of two hearts are discussed. [DONOR I IRECIPIENTI Sv C..AOT A ;PULMONARY ARRY http://heart.bmj.com/ RIGHTATRIU_gXARA t,.Y APPENDAGE R.V R.V on September 28, 2021 by guest. Protected copyright. FIG. 1 Position of donor and recipient hearts in anteroposterior view with relevant anasta- moses (Barnard and Losman (1975). Reprinted with permission of South African Medical Journal). The purpose of this report is to illustrate some of right lung and in the right cardiophrenic angle. the bizarre electrocardiograms resulting from Both venae cavae of the donor heart are ligated and cardiac transplantation in man where the recipient the donor right ventricle pumps only its coronary heart is left in situ. The surgical technique was sinus venous return into the recipient's right described in detail by Barnard and Losman (1975). -

Short-Term Exposure to Air Pollution and Cardiac Arrhythmia: a Meta-Analysis and Systematic Review
Int. J. Environ. Res. Public Health 2016, 13, doi:10.3390/ijerph13070642 S1 of S7 Supplementary Materials: Short-Term Exposure to Air Pollution and Cardiac Arrhythmia: A Meta-Analysis and Systematic Review Xuping Song, Yu Liu, Yuling Hu, Xiaoyan Zhao, Jinhui Tian, Guowu Ding and Shigong Wang Figure S1. Flow chart of the literature screening process. Int. J. Environ. Res. Public Health 2016, 13, doi:10.3390/ijerph13070642 S2 of S7 Figure S2. Association between particulate and gaseous components with hospitalization or mortality due to arrhythmia. Int. J. Environ. Res. Public Health 2016, 13, doi:10.3390/ijerph13070642 S3 of S7 Table S1. Search Strategy for PubMed. No. Search Strategy air pollution*/or air pollutant*/or air polluted/or air contamination*/or atmosphere pollution*/or atmosphere pollutant*/ or atmosphere contamination*/or atmospheric pollution*/or atmospheric #1 pollutant*/or atmospheric contamination*/or “particulate matter”/or “PM10”/or “PM2.5”/or ozone/ or “O3”/or “carbon monoxide”/or carbonmonoxide/or “CO“/or “nitrogen dioxide”/or “NO2”/or “sulphur dioxide”/or “sulphur dioxyde”/or “sulfurous anhydride“/or “SO2”.ti,ab. Air Pollution/or Particulate Matter/or Ozone/or Carbon Monoxide/or Nitrogen Dioxide/or Sulfur #2 Dioxide.sh. #3 or/1,2 #4 arrhythmia* /or dysrhythmia* /or “CA”.ti,ab. #5 Arrhythmias, Cardiac.sh. “Sick Sinus Syndrome”/or “SSS”/or “Sick Sinus Node Syndrom”/or Sinus Node Dysfunction*/or #6 Sinus Node Disease*/or Sinus Arrest*.ti,ab. #7 Arrhythmia, Sinus/or Sick Sinus Syndrome/or Sinus Arrest, Cardiac.sh. #8 atrial fibrillation*/or auricular fibrillation*/or “AF".ti,ab. #9 Atrial Fibrillation.sh. -

The Roles of Electrical Cardiac Systole Sudden Death
Journal of Cardiology & Current Research The Roles of Electrical Cardiac Systole Sudden Death Abstract Review Article The definition of sudden death had to be explained in many other chapters of Volume 3 Issue 3 - 2015 this book. So I will not go into more details regarding it. The sudden death in the absence of structural heart disease is uncommon, but when it appears, has a very Francisco R Breijo Marquez* significant clinical impact because many of the victims are young. In relatively School of Medicine, Commemorative Hospital, USA recent form it has given special attention to particular conditions expressed in repolarization electrocardiographies on the QT interval, whose relationship with *Corresponding author: Francisco R Breijo Marquez, the functionality of some ion channels in the membrane cell has prompted its School of Medicine, Commemorative Hospital, USA; designation as “channelopathies”. But the QT-interval alteration is not unique. Email: Keywords: Electrical cardiac systole disturbances; Long and Short QT-Syndromes; Received: August 11, 2014 | Published: August 27, 2014 The short PR-interval disturbances; Sudden cardiac death Abbreviations: ECG: Electrocardiography; WPW: Wolff- Parkinson-White; TSH: Thyroid-Stimulating; LBBB: Left Bundle Branch Block Bundles The Electrical Cardiac Systole Disorders in the electrical cardiac systole can be very dangerous for sudden death, as some cardiac entities previously cited in this book. Its role in sudden death is very important. Before anything else, it is essential to know what is considered as “electrical cardiac systole”. For some authors it would be from the beginning of the Q-wave until the end of T-wave. In contrast, for other authors, including us, it would be from the beginning of the P-wave until the end of T-wave, including the P- wave and the PR- interval (Figure 1). -

Abnormal P Waves and Paroxysmal Tachycardia
Brit. Heart J., 1963, 25, 570. Br Heart J: first published as 10.1136/hrt.25.5.570 on 1 September 1963. Downloaded from ABNORMAL P WAVES AND PAROXYSMAL TACHYCARDIA BY L. G. DAVIES* AND I. P. ROSSt From The National Heart Hospital, London Received January 28, 1963 Specific changes in the P wave of the electrocardiogram have been recognized in mitral stenosis (Lewis and Gilder, 1912), pulmonary heart disease (Winternitz, 1935), left ventricular failure (Wood and Selzer, 1939), and congenital heart disease (Paul, Myers, and Campbell, 1951). These changes are believed to be the result of right or left atrial hypertrophy (Reynolds, 1953; Thomas, and Dejong, 1954). We have noticed P wave abnormalities in some patients with paroxysmal tachycardia, an observation that does not appear to have been reported by other workers. In our patients the abnormal P waves were prolonged, usually to 0@12 second or more, and were frequently notched. These abnormalities were not due to any of the recognized causes for these hearts were clinically normal. As a pilot study 50 electrocardiograms from patients with paroxysmal tachy- cardia and 50 from normal controls were mixed together and studied independently by four obser- vers. The results confirmed our preliminary observations and we decided to study a larger series. copyright. SUBJECTS AND METHODS We examined the records of patients in whom a firm clinical diagnosis of paroxysmal tachycardia had been made. Those patients with organic heart disease were excluded, so were a number with normal hearts where the electrocardiograms were unsatisfactory because of sinus tachycardia or tremor. The series there- fore consisted of 200 patients where the clinical record and electrocardiogram were suitable for analysis.