Blepharoplasty
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Blepharoplasty, Ptosis and Canthoplasty
ENVOLVE VISION BENEFITS, INC. INCLUDING ALL ASSOCIATED SUBSIDIARIES CLINICAL POLICY AND PROCEDURE DEPARTMENT: Utilization DOCUMENT NAME: Blepharoplasty, Ptosis Management and Canthoplasty PAGE: 1 of 8 REFERENCE NUMBER: OC.UM.CP.0007 EFFECTIVE DATE: 01/01/2017 REPLACES DOCUMENT: 118-UM-R6 RETIRED: REVIEWED: 10/25/2017 SPECIALIST REVIEW: Yes REVISED: 11/7/2016 PRODUCT TYPE: COMMITTEE APPROVAL: 01/09/2018 IMPORTANT REMINDER: This Clinical Policy has been developed by appropriately experienced and licensed health care professionals based on a thorough review and consideration of generally accepted standards of medical practice, peer-reviewed medical literature, government agency/program approval status, and other indicia of medical necessity. The purpose of this Clinical Policy is to provide a guide to medical necessity. Benefit determinations should be based in all cases on the applicable contract provisions governing plan benefits (“Benefit Plan Contract”) and applicable state and federal requirements including Local Coverage Determinations (LCDs), as well as applicable plan-level administrative policies and procedures. To the extent there are any conflicts between this Clinical Policy and the Benefit Plan Contract provisions, the Benefit Plan Contract provisions will control. Clinical policies are intended to be reflective of current scientific research and clinical thinking. This Clinical Policy is not intended to dictate to providers how to practice medicine, nor does it constitute a contract or guarantee regarding results. Providers are expected to exercise professional medical judgment in providing the most appropriate care, and are solely responsible for the medical advice and treatment of members. SUBJECT: Medical necessity determination of eyelid procedures for treatment of dermatochalasis and ptosis. -

National Study of Microphthalmia, Anophthalmia, and Coloboma (MAC
16 ORIGINAL ARTICLE J Med Genet: first published as 10.1136/jmg.39.1.16 on 1 January 2002. Downloaded from National study of microphthalmia, anophthalmia, and coloboma (MAC) in Scotland: investigation of genetic aetiology D Morrison, D FitzPatrick, I Hanson, K Williamson, V van Heyningen, B Fleck, I Jones, J Chalmers, H Campbell ............................................................................................................................. J Med Genet 2002;39:16–22 We report an epidemiological and genetic study attempting complete ascertainment of subjects with microphthalmia, anophthalmia, and coloboma (MAC) born in Scotland during a 16 year period beginning on 1 January 1981. A total of 198 cases were confirmed giving a minimum live birth preva- lence of 19 per 100 000. One hundred and twenty-two MAC cases (61.6%) from 115 different fami- See end of article for lies were clinically examined and detailed pregnancy, medical, and family histories obtained. A authors’ affiliations simple, rational, and apparently robust classification of the eye phenotype was developed based on ....................... the presence or absence of a defect in closure of the optic (choroidal) fissure. A total of 85/122 Correspondence to: (69.7%) of cases had optic fissure closure defects (OFCD), 12/122 (9.8%) had non-OFCD, and Dr D FitzPatrick, MRC 25/122 (20.5%) had defects that were unclassifiable owing to the severity of the corneal or anterior Human Genetics Unit, chamber abnormality. Segregation analysis assuming single and multiple incomplete ascertainment, Western General Hospital, respectively, returned a sib recurrence risk of 6% and 10% in the whole group and 8.1% and 13.3% Edinburgh EH4 2XU, UK; in the OFCD subgroup. -

Policy 96018: Blepharoplasty, Blepharoptosis Repair, and Brow
Policy: 96018 Initial Effective Date: 11/22/1996 SUBJECT: Blepharoplasty, Blepharoptosis Repair, and Annual Review Date: 11/16/2020 Brow Ptosis Repair Last Revised Date: 11/16/2020 Prior approval is required for some or all procedure codes listed in this Corporate Medical Policy. Definition: The term blepharoplasty refers to a collection of surgical procedures that involve removal of redundant eyelid tissue (skin, muscle, and fat). Although the primary indication for blepharoplasty is to improve the eyelid appearance, redundant lax eyelid tissue (dermatochalasis) can obstruct the superior visual field and interfere with activities of daily living in some individuals. In these cases, blepharoplasty may be considered in order to produce functional improvement in vision. The pathophysiology of dermatochalasis has not been well described, but much of the process appears to involve skin changes associated with the aging process. Less commonly, systemic disorders such as Ehlers-Danlos syndrome may predispose patients to develop dermatochalasis at a younger age. Clinical manifestations are mainly cosmetic, but in severe cases eyelid tissue may obstruct the superior visual field. The most common symptoms include difficulty reading and loss of peripheral vision when driving. Blepharoplasty may help to improve function for patients with clinically significant dermatochalasis. Blepharochalasis is sometimes confused with dermatochalasis. Though similar in nomenclature, these two disorders are quite different in presentation and etiology. Blepharochalasis is a rare condition characterized by intermittent, recurrent eyelid edema, resulting in relaxation of the eyelid tissue and resultant atrophy. The lower eyelids are less commonly involved. Blepharochalasis typically presents in adolescence or young adulthood, with intermittent attacks that occur less commonly as the person ages. -
Lid and Lash Conditions
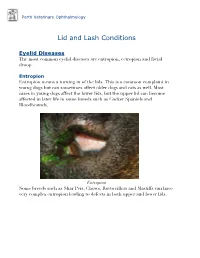
Perth Veterinary Ophthalmology Lid and Lash Conditions Eyelid Diseases The most common eyelid diseases are entropion, ectropion and facial droop. Entropion Entropion means a turning in of the lids. This is a common complaint in young dogs but can sometimes affect older dogs and cats as well. Most cases in young dogs affect the lower lids, but the upper lid can become affected in later life in some breeds such as Cocker Spaniels and Bloodhounds. Entropion Some breeds such as Shar Peis, Chows, Rottweillers and Mastiffs can have very complex entropion leading to defects in both upper and lower lids. A Shar Pei with severe upper and lower lid entropion Entropion is painful and can be potentially blinding. The rolling in of the lid leads to hair coming into contact with the cornea, leading to pain, ulceration and scarring (which can affect vision). In severe cases this can even lead to perforation of the eye. There are many causes of entropion. It can be primary or secondary to other problems affecting the lids (such as ectopic cilia, distichiasis etc. - see below). Some possible causes include the lid being too long, the lid being too tight, instability of the lateral canthus (outer cornea of the eyelids), misdirection of the lateral canthal tendon, brachycephalic anatomy (big eyes and short nose - e.g. Pekingese, Pugs, Shih Tsus, Persian cats etc.), diamond eye defects, loose or too much skin, facial droop etc. Often these cases are referred to a veterinary ophthalmologist for proper assessment and treatment to provide the best outcome. Entropion requires surgical correction. -

Congenital Ocular Anomalies in Newborns: a Practical Atlas
www.jpnim.com Open Access eISSN: 2281-0692 Journal of Pediatric and Neonatal Individualized Medicine 2020;9(2):e090207 doi: 10.7363/090207 Received: 2019 Jul 19; revised: 2019 Jul 23; accepted: 2019 Jul 24; published online: 2020 Sept 04 Mini Atlas Congenital ocular anomalies in newborns: a practical atlas Federico Mecarini1, Vassilios Fanos1,2, Giangiorgio Crisponi1 1Neonatal Intensive Care Unit, Azienda Ospedaliero-Universitaria Cagliari, University of Cagliari, Cagliari, Italy 2Department of Surgery, University of Cagliari, Cagliari, Italy Abstract All newborns should be examined for ocular structural abnormalities, an essential part of the newborn assessment. Early detection of congenital ocular disorders is important to begin appropriate medical or surgical therapy and to prevent visual problems and blindness, which could deeply affect a child’s life. The present review aims to describe the main congenital ocular anomalies in newborns and provide images in order to help the physician in current clinical practice. Keywords Congenital ocular anomalies, newborn, anophthalmia, microphthalmia, aniridia, iris coloboma, glaucoma, blepharoptosis, epibulbar dermoids, eyelid haemangioma, hypertelorism, hypotelorism, ankyloblepharon filiforme adnatum, dacryocystitis, dacryostenosis, blepharophimosis, chemosis, blue sclera, corneal opacity. Corresponding author Federico Mecarini, MD, Neonatal Intensive Care Unit, Azienda Ospedaliero-Universitaria Cagliari, University of Cagliari, Cagliari, Italy; tel.: (+39) 3298343193; e-mail: [email protected]. -

Eleventh Edition
SUPPLEMENT TO April 15, 2009 A JOBSON PUBLICATION www.revoptom.com Eleventh Edition Joseph W. Sowka, O.D., FAAO, Dipl. Andrew S. Gurwood, O.D., FAAO, Dipl. Alan G. Kabat, O.D., FAAO Supported by an unrestricted grant from Alcon, Inc. 001_ro0409_handbook 4/2/09 9:42 AM Page 4 TABLE OF CONTENTS Eyelids & Adnexa Conjunctiva & Sclera Cornea Uvea & Glaucoma Viitreous & Retiina Neuro-Ophthalmic Disease Oculosystemic Disease EYELIDS & ADNEXA VITREOUS & RETINA Blow-Out Fracture................................................ 6 Asteroid Hyalosis ................................................33 Acquired Ptosis ................................................... 7 Retinal Arterial Macroaneurysm............................34 Acquired Entropion ............................................. 9 Retinal Emboli.....................................................36 Verruca & Papilloma............................................11 Hypertensive Retinopathy.....................................37 Idiopathic Juxtafoveal Retinal Telangiectasia...........39 CONJUNCTIVA & SCLERA Ocular Ischemic Syndrome...................................40 Scleral Melt ........................................................13 Retinal Artery Occlusion ......................................42 Giant Papillary Conjunctivitis................................14 Conjunctival Lymphoma .......................................15 NEURO-OPHTHALMIC DISEASE Blue Sclera .........................................................17 Dorsal Midbrain Syndrome ..................................45 -

Presumptive Unilateral Anophthalmia Recorded in Coronella Austriaca Laurenti, 1768
Herpetology Notes, volume 8: 459-460 (published online on 13 August 2015) Presumptive unilateral anophthalmia recorded in Coronella austriaca Laurenti, 1768 Daniel Jablonski* and Peter Mikulíček Different kinds of morphological anomalies were specimens of C. austriaca and other snake species recorded in snakes, most of them in captive-bred (Natrix natrix, N. tessellata, Zamenis longissimus) individuals (Mulder, 1995). According to this author, the have been previously found on the same locality, but all main cause of anomalies seemed to be wrong incubation were without ocular anomaly or other deformities (pers. temperature conditions during embryo development. observation). According to our best knowledge, this is However, little is known about variety of anomalies the first report of presumptive unilateral anophthalmia from snakes born in the wild probably due to their high observed in C. austriaca in nature. mortality rate during early life (Mulder, 1995). Smooth As for reptiles, several kinds of ocular abnormalities snake, Coronella austriaca Laurenti, 1768, is a small, are known: microphthalmia, cystic globe, cyclopia/ viviparous, nonvenomous colubrid snake occurring synophthalmia, coloboma or aphakia (Sabater and in the most of Europe and some parts of Asia (Arnold Pérez, 2013), but their etiology is difficult to explain and Ovenden, 2002). It lives in heathlands, hedgerows, (Da Silva et al., 2015). Anophthalmia, either unilateral wood-edges, open woods and bushy and rocky slopes or bilateral, is defined as the congenital total absence of (Arnold and Ovenden, 2002). Except several types of ocular tissue and results from a failure of the primary colour anomalies (see Lauš and Burić, 2012), no other optic vesicle to develop or from a complete regression anomalies or deformities have been recorded so far in of the optic vesicle (Millichamp, Jacobson and Wolf, this species. -

Freedman Eyelid Abnormalities
1/16/2018 1 1/16/2018 Upper Lid Lower Lid Protractors Retractors: Levator m. 3rd nerve function Muller’s m. Cranial Nerve VII function Sympathetic Function Inferior Tarsal Muscle Things to Note Lid Apposition to Globe Position of Lid Margins MRD = 3‐5 mm Canthal Insertions Brow Positions 2 1/16/2018 Ptosis Usually age related levator dehiscence, but sometimes a sign of neurologic, mechanical orbital or inflammatory disease Blepharospasm Sign of External Irritation or Neurologic Disease 3 1/16/2018 First Consider Underlying Orbital Disease Orbital Cellulitis, Pseudotumor, Wegener’s Graves Ophthalmopathy, Orbital Varix Orbital Tumors that can mimic inflammatory process: Lacrimal Gland CA, Lymphoma, Lymphangioma, etc. Lacrimal Gland – Dacryoadenitis or tumor Sinus Mucocele Without Inflammatory Appearance, consider above but also… Allergic Eyelid Edema Hormonal Shifts Systemic Disorder – Cardiac, Renal, Hepatic, Thyroid with edema Cutaneous Lymphoma Graves Ophthalmopathy –can just have lid edema w/o inflammatory appearance Lymphedema after trauma, surgery to lids or orbit (e.g. lymphatics in lateral canthus) Traumatic Leak of CSF into upper eyelid (JAMA Oph 2014;312:1485) Blepharochalasis Not True Edema, but might mimic it: Dermatochalasis, Hidden Eyelid or Sub‐Conjunctival Mass, Prolapsed Orbital Fat When your concerned about: Orbital Cellulitis Orbital Pseudotumor Orbital Malignancy Vascular – e.g. CC fistula Proptosis Chemosis Poor Motility Poor Vision Pupil abnormality – e.g. RAPD Orbital Pseudotumor 4 1/16/2018 Good Vision Good Motility -

Use of Next Generation Sequencing for Isolated and Syndromic Anophthalmia, Microphthalmia and Coloboma (MAC): a New Approach to Molecular Genetic Diagnosis
View metadata, citation and similar papers at core.ac.uk brought to you by CORE provided by Archivio della ricerca- Università di Roma La Sapienza Use of Next Generation Sequencing for isolated and syndromic Anophthalmia, Microphthalmia and Coloboma (MAC): a new approach to molecular genetic diagnosis Department of Cellular Biotechnologies and Hematology PhD in Human Biology and Medical Genetics XXX° cycle 2014-2017 Candidate Dr. Iapichino Giuseppe 1235269 Supervisor Correlator Prof. Pizzuti Antonio Prof. Novelli Antonio A/A 2016/2017 1. INTRODUCTION 1.1 Eye embryogenesis 1.2 MAC: Mixed group of diseases 1.2.1 Microphthalmia, Anophthalmia and Coloboma 1.2.2 Syndromic diseases: CHARGE syndrome Cornelia de Lange syndrome Axenfeld-Rieger syndrome Lenz’s Microphtalmia Papillorenal syndrome 1.3 Molecular Diagnosis: Next Generation Sequencing 2. AIM OF THE STUDY 3. MATERIALS AND METHODS 3.1 Patients Recruitment 3.2 Molecular Analysis 3.2.1 Blood collection, DNA extraction and quantification 3.2.2 NGS panel construction: Design Studio 3.2.3 NextSeq-500: features and workflow Libraries preparation: Nextera Rapid Capture Custom Enrichment Cluster generation Sequencing 3.2.4 Sanger Sequencing 3.2.5 Data Analysis 4. RESULTS 5. DISCUSSION 6. CONCLUSION 7. BIBLIOGRAPHY 1. INTRODUCTION 1.1 The eye: embryogenesis Eye development begins around the 4th week of gestation and can be summarized in four main stages [Zagozewski J.L. et al.; 2014]: Optic vesicle formation Induction of crystalline lens Retinal tissue formation Optic fissure closure Each of these events is highly regulated and coordinated by various transcription factors and circulating molecules [Adler R. et al.; 2007]. -

SOX2 Anophthalmia Syndrome
SOX2 anophthalmia syndrome Description SOX2 anophthalmia syndrome is a rare disorder characterized by abnormal development of the eyes and other parts of the body. People with SOX2 anophthalmia syndrome are usually born without eyeballs ( anophthalmia), although some individuals have small eyes (microphthalmia). The term anophthalmia is often used interchangeably with severe microphthalmia because individuals with no visible eyeballs typically have some remaining eye tissue. These eye problems can cause significant vision loss. While both eyes are usually affected in SOX2 anophthalmia syndrome, one eye may be more affected than the other. Individuals with SOX2 anophthalmia syndrome may also have seizures, brain abnormalities, slow growth, delayed development of motor skills (such as walking), and mild to severe learning disabilities. Some people with this condition are born with a blocked esophagus (esophageal atresia), which is often accompanied by an abnormal connection between the esophagus and the trachea (tracheoesophageal fistula). Genital abnormalities have been described in affected individuals, especially males. Male genital abnormalities include undescended testes (cryptorchidism) and an unusually small penis (micropenis). Frequency SOX2 anophthalmia syndrome is estimated to affect 1 in 250,000 individuals. About 10 percent to 15 percent of people with anophthalmia in both eyes have SOX2 anophthalmia syndrome. Causes Mutations in the SOX2 gene cause SOX2 anophthalmia syndrome. This gene provides instructions for making a protein that plays a critical role in the formation of many different tissues and organs during embryonic development. The SOX2 protein regulates the activity of other genes, especially those that are important for normal development of the eyes. Mutations in the SOX2 gene prevent the production of functional SOX2 protein. -

The Management of Congenital Malpositions of Eyelids, Eyes and Orbits
Eye (\988) 2, 207-219 The Management of Congenital Malpositions of Eyelids, Eyes and Orbits S. MORAX AND T. HURBLl Paris Summary Congenital malformations of the eye and its adnexa which are multiple and varied can affect the whole eyeball or any part of it, as well as the orbit, eyelids, lacrimal ducts, extra-ocular muscles and conjunctiva. A classification of these malformations is presented together with the general principles of treatment, age of operating and surgical tactics. The authors give some examples of the anatomo-clinical forms, eyelid malpositions such as entropion, ectropion, ptosis, levator eyelid retraction, medial canthus malposition, congenital eyelid colobomas, and congenital orbital abnormalities (Craniofacial stenosis, orbi tal plagiocephalies, hypertelorism, anophthalmos, microphthalmos and cryptophthalmos) . Congenital malformations of the eye and its as echography, CT-scan and NMR, enzymatic adnexa are multiple and varied. They can work-up or genetic studies (Table I). affect the whole eyeball or any part of it, as Surgical treatment when feasible will well as the orbit, eyelids, lacrimal ducts extra encounter numerous problems; age will play a ocular muscles and conjunctiva. role, choice of a surgical protocol directly From the anatomical point of view, the fol related to the existing complaints, and coop lowing can be considered. eration between several surgical teams Position abnormalities (malpositions) of (ophthalmologic, plastic, cranio-maxillo-fac one or more elements and formation abnor ial and neurosurgical), the ideal being to treat malities (malformations) of the same organs. Some of these abnormalities are limited to Table I The manag ement of cong enital rna/positions one organ and can be subjected to a relatively of eyelid s, eyes and orbits simple and well recognised surgical treat Ocular Findings: ment. -

Novel Mutations in ALDH1A3 Associated with Autosomal Recessive Anophthalmia/ Microphthalmia, and Review of the Literature Siying Lin1, Gaurav V
Lin et al. BMC Medical Genetics (2018) 19:160 https://doi.org/10.1186/s12881-018-0678-6 RESEARCH ARTICLE Open Access Novel mutations in ALDH1A3 associated with autosomal recessive anophthalmia/ microphthalmia, and review of the literature Siying Lin1, Gaurav V. Harlalka1, Abdul Hameed2, Hadia Moattar Reham3, Muhammad Yasin3, Noor Muhammad3, Saadullah Khan3, Emma L. Baple1, Andrew H. Crosby1 and Shamim Saleha3* Abstract Background: Autosomal recessive anophthalmia and microphthalmia are rare developmental eye defects occurring during early fetal development. Syndromic and non-syndromic forms of anophthalmia and microphthalmia demonstrate extensive genetic and allelic heterogeneity. To date, disease mutations have been identified in 29 causative genes associated with anophthalmia and microphthalmia, with autosomal dominant, autosomal recessive and X-linked inheritance patterns described. Biallelic ALDH1A3 gene variants are the leading genetic causes of autosomal recessive anophthalmia and microphthalmia in countries with frequent parental consanguinity. Methods: This study describes genetic investigations in two consanguineous Pakistani families with a total of seven affected individuals with bilateral non-syndromic clinical anophthalmia. Results: Using whole exome and Sanger sequencing, we identified two novel homozygous ALDH1A3 sequence variants as likely responsible for the condition in each family; missense mutation [NM_000693.3:c.1240G > C, p. Gly414Arg; Chr15:101447332G > C (GRCh37)] in exon 11 (family 1), and, a frameshift mutation [NM_000693.3:c. 172dup, p.Glu58Glyfs*5; Chr15:101425544dup (GRCh37)] in exon 2 predicted to result in protein truncation (family 2). Conclusions: This study expands the molecular spectrum of pathogenic ALDH1A3 variants associated with anophthalmia and microphthalmia, and provides further insight of the key role of the ALDH1A3 in human eye development.