Low Milk Supply
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Common Breastfeeding Questions
Common Breastfeeding Questions How often should my baby nurse? Your baby should nurse 8-12 times in 24 hours. Baby will tell you when he’s hungry by “rooting,” sucking on his hands or tongue, or starting to wake. Just respond to baby’s cues and latch baby on right away. Every mom and baby’s feeding patterns will be unique. Some babies routinely breastfeed every 2-3 hours around the clock, while others nurse more frequently while awake and sleep longer stretches in between feedings. The usual length of a breastfeeding session can be 10-15 minutes on each breast or 15-30 minutes on only one breast; just as long as the pattern is consistent. Is baby getting enough breastmilk? Look for these signs to be sure that your baby is getting enough breastmilk: Breastfeed 8-12 times each day, baby is sucking and swallowing while breastfeeding, baby has 3- 4 dirty diapers and 6-8 wet diapers each day, the baby is gaining 4-8 ounces a week after the first 2 weeks, baby seems content after feedings. If you still feel that your baby may not be getting enough milk, talk to your health care provider. How long should I breastfeed? The World Health Organization and the American Academy of Pediatrics recommends mothers to breastfeed for 12 months or longer. Breastmilk contains everything that a baby needs to develop for the first 6 months. Breastfeeding for at least the first 6 months is termed, “The Golden Standard.” Mothers can begin breastfeeding one hour after giving birth. -
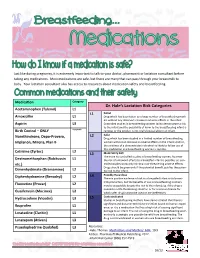
Dr. Hale's Lactation Risk Categories
Just like during pregnancy, it is extremely important to talk to your doctor, pharmacist or lactation consultant before taking any medications. Most medications are safe, but there are many that can pass through your breastmilk to baby. Your lactation consultant also has access to resources about medication safety and breastfeeding. Medication Category Dr. Hale’s Lactation Risk Categories Acetaminophen (Tylenol) L1 L1 Safest Amoxicillin L1 Drug which has been taken by a large number of breastfeeding moth- ers without any observed increase in adverse effects in the infant. Aspirin L3 Controlled studies in breastfeeding women fail to demonstrate a risk to the infant and the possibility of harm to the breastfeeding infant is Birth Control – ONLY Acceptable remote; or the product is not orally bioavailable in an infant. L2 Safer Norethindrone, Depo-Provera, Drug which has been studied in a limited number of breastfeeding Implanon, Mirena, Plan B women without an increase in adverse effects in the infant; And/or, the evidence of a demonstrated risk which is likely to follow use of this medication in a breastfeeding woman is remote. Cetrizine (Zyrtec) L2 L3 Moderately Safe There are no controlled studies in breastfeeding women, however Dextromethorphan (Robitussin L1 the risk of untoward effects to a breastfed infant is possible; or, con- etc.) trolled studies show only minimal non-threatening adverse effects. Drugs should be given only if the potential benefit justifies the poten- Dimenhydrinate (Dramamine) L2 tial risk to the infant. L4 Possibly Hazardous Diphenhydramine (Benadryl) L2 There is positive evidence of risk to a breastfed infant or to breast- milk production, but the benefits of use in breastfeeding mothers Fluoxetine (Prozac) L2 may be acceptable despite the risk to the infant (e.g. -

Melasma (1 of 8)
Melasma (1 of 8) 1 Patient presents w/ symmetric hyperpigmented macules, which can be confl uent or punctate suggestive of melasma 2 DIAGNOSIS No ALTERNATIVE Does clinical presentation DIAGNOSIS confirm melasma? Yes A Non-pharmacological therapy • Patient education • Camoufl age make-up • Sunscreen B Pharmacological therapy Monotherapy • Hydroquinone or • Tretinoin TREATMENT Responding to No treatment? See next page Yes Continue treatment © MIMSas required Not all products are available or approved for above use in all countries. Specifi c prescribing information may be found in the latest MIMS. B94 © MIMS 2019 Melasma (2 of 8) Patient unresponsive to initial therapy MELASMA A Non-pharmacological therapy • Patient education • Camoufl age make-up • Sunscreen B Pharmacological therapy Dual Combination erapy • Hydroquinone plus • Tretinoin or • Azelaic acid Responding to Yes Continue treatment treatment? as required No A Non-pharmacological therapy • Patient education • Camoufl age make-up • Sunscreen • Laser therapy • Dermabrasion B Pharmacological therapy Triple Combination erapy • Hydroquinone plus • Tretinoin plus • Topical steroid Chemical peels 1 MELASMA • Acquired hyperpigmentary skin disorder characterized by irregular light to dark brown macules occurring in the sun-exposed areas of the face, neck & arms - Occurs most commonly w/ pregnancy (chloasma) & w/ the use of contraceptive pills - Other factors implicated in the etiopathogenesis are photosensitizing medications, genetic factors, mild ovarian or thyroid dysfunction, & certain cosmetics • Most commonly aff ects Fitzpatrick skin phototypes III & IV • More common in women than in men • Rare before puberty & common in women during their reproductive years • Solar & ©ultraviolet exposure is the mostMIMS important factor in its development Not all products are available or approved for above use in all countries. -

The Key to Increasing Breastfeeding Duration: Empowering the Healthcare Team
The Key to Increasing Breastfeeding Duration: Empowering the Healthcare Team By Kathryn A. Spiegel A Master’s Paper submitted to the faculty of the University of North Carolina at Chapel Hill In partial fulfillment of the requirements for the degree of Master of Public Health in the Public Health Leadership Program. Chapel Hill 2009 ___________________________ Advisor signature/printed name ________________________________ Second Reader Signature/printed name ________________________________ Date The Key to Increasing Breastfeeding Duration 2 Abstract Experts and scientists agree that human milk is the best nutrition for human babies, but are healthcare professionals (HCPs) seizing the opportunity to promote, protect, and support breastfeeding? Not only are HCPs influential to the breastfeeding dyad, they hold a responsibility to perform evidence-based interventions to lengthen the duration of breastfeeding due to the extensive health benefits for mother and baby. This paper examines current HCPs‘ education, practices, attitudes, and extraneous factors to surface any potential contributing factors that shed light on necessary actions. Recommendations to empower HCPs to provide consistent, evidence-based care for the breastfeeding dyad include: standardized curriculum in medical/nursing school, continued education for maternity and non-maternity settings, emphasis on skin-to-skin, enforcement of evidence-based policies, implementation of ‗Baby-Friendly USA‘ interventions, and development of peer support networks. Requisite resources such as lactation consultants as well as appropriate medication and breastfeeding clinical management references aid HCPs in providing best practices to increase breastfeeding duration. The Key to Increasing Breastfeeding Duration 3 The key to increasing breastfeeding duration: Empowering the healthcare team During the colonial era, mothers breastfed through their infants‘ second summer. -

Breastfeeding Management in Primary Care-FINAL-Part 2.Pptx
Breastfeeding Management in Primary Care Pt 2 Heggie, Licari, Turner May 25 '17 5/15/17 Case 3 – Sore nipples • G3P3 mom with sore nipples, baby 5 days old, full term, Breaseeding Management in yellow stools, output normal per BF log, 5 % wt loss. Primary Care - Part 2 • Mother exam: both nipples with erythema, cracked and scabbed at p, areola mildly swollen, breasts engorged and moderately tender, mild diffuse erythema, no mass. • Baby exam: strong but “chompy” suck, thick ght frenulum aached to p of tongue, with restricted tongue movement- poor lateral tracking, unable to extend tongue past gum line or lower lip, minimal tongue elevaon. May 25, 2017, Duluth, MN • Breaseeding observaon: Baby has deep latch, mom Pamela Heggie MD, IBCLC, FAAP, FABM Addie Licari, MD, FAAFP with good posioning, swallows heard and also Lorraine Turner, MD, ABIHM intermient clicking. Mom reports pain during feeding. Sore cracked nipple Type 1 - Ankyloglossia Sore Nipples § “Normal” nipple soreness is very minimal and ok only if: ü Poor latch § Nipple “tugging” brief (< 30 sec) with latch-on then resolves ü LATCH, LATCH, LATCH § No pain throughout feeding or in between feeds ü Skin breakdown/cracks-staph colonizaon § No skin damage ü Engorgement § Some women are told “the latch looks ok”… but they are in pain and curling their toes ü Trauma from pumping ü § It doesn’t maer how it “looks” … if mom is uncomfortable Nipple Shields it’s a problem and baby not geng much milk…set up for low ü Vasospasm milk supply ü Blocked nipple pore/Nipple bleb § Nipple pain is -

Breastfeeding Contraindications
WIC Policy & Procedures Manual POLICY: NED: 06.00.00 Page 1 of 1 Subject: Breastfeeding Contraindications Effective Date: October 1, 2019 Revised from: October 1, 2015 Policy: There are very few medical reasons when a mother should not breastfeed. Identify contraindications that may exist for the participant. Breastfeeding is contraindicated when: • The infant is diagnosed with classic galactosemia, a rare genetic metabolic disorder. • Mother has tested positive for HIV (Human Immunodeficiency Syndrome) or has Acquired Immune Deficiency Syndrome (AIDS). • The mother has tested positive for human T-cell Lymphotropic Virus type I or type II (HTLV-1/2). • The mother is using illicit street drugs, such as PCP (phencyclidine) or cocaine (exception: narcotic-dependent mothers who are enrolled in a supervised methadone program and have a negative screening for HIV and other illicit drugs can breastfeed). • The mother has suspected or confirmed Ebola virus disease. Breastfeeding may be temporarily contraindicated when: • The mother is infected with untreated brucellosis. • The mother has an active herpes simplex virus (HSV) infection with lesions on the breast. • The mother is undergoing diagnostic imaging with radiopharmaceuticals. • The mother is taking certain medications or illicit drugs. Note: mothers should be provided breastfeeding support and a breast pump, when appropriate, and may resume breastfeeding after consulting with their health care provider to determine when and if their breast milk is safe for their infant and should be provided with lactation support to establish and maintain milk supply. Direct breastfeeding may be temporarily contraindicated and the mother should be temporarily isolated from her infant(s) but expressed breast milk can be fed to the infant(s) when: • The mother has untreated, active Tuberculosis (TB) (may resume breastfeeding once she has been treated approximately for two weeks and is documented to be no longer contagious). -

Improving Delayed Lactogenesis and Suppressed Lactation in At-Risk Mothers
Improving Delayed Lactogenesis and Suppressed Lactation in At-Risk Mothers Jean Rucks Rhodes, PhD, CNM, IBCLC High breastfeeding initiation rates show that most mothers in the U.S. want to breastfeed and are trying to do so. However, low breastfeeding rates among infants who are six and 12 months of age indicate that many mothers do not continue breastfeeding as recommended. These rates suggest that mothers, in part, may not be getting the support they need, such as from healthcare provid- ers, family members, and employers.... The early postpartum period is a critical time for establishing and supporting breastfeeding. CDC 2016 Breastfeeding Report Card 1 WHITE PAPER EXECUTIVE SUMMARY Although breastfeeding initiation is at an all-time high New evidence suggests babies’ feeding behaviors of 81%, rates of breastfeeding exclusivity and du- have an important role in determining lactation suc- ration lag behind national goals. Women who stop cess. These unique infant sucking patterns in the first breastfeeding before meeting their goals often report few days of life appear to program mothers’ breasts they did not have enough milk. for optimal milk production. New breast pump initia- tion technology that mimics early newborn sucking The ability to initiate, build and maintain breast milk is a potentially viable and safe intervention to provide volumes sufficient to meet an infant’s needs are de- at-risk mothers with additional breast stimulation for pendent on complex interwoven factors. Additionally, optimal milk production outcomes. there are multiple maternal risk factors for delayed milk production and suppressed lactation: In many lactation situations, interventions aren’t start- ed until a mother reports problems. -

Skin Care, Hair Care and Cosmetic Treatments in Pregnancy and Breastfeeding
Skin Care, Hair Care and Cosmetic Treatments in Pregnancy and Breastfeeding Information in this leaflet is general in nature and should not take the place of advice from your health care provider. With every pregnancy there is a 3 to 5% risk of having a baby with a birth defect. Issues for pregnancy Many pregnant women have skin and hair concerns just as they did before pregnancy. Sometimes conditions such as acne actually worsen during pregnancy because of hormonal changes and often women notice darkening of their skin (melasma). However, due to concern about potentially hazardous exposures to their unborn babies, pregnant women are often uncertain about which products are safe for them to use. Generally cosmetic treatments are discretionary (not medically necessary) and if safety is uncertain, women should consider whether the product or treatment is really required. There are several considerations when evaluating whether a specific skin or hair product is unsafe in pregnancy. Firstly, the active ingredient in the product needs to be considered unsafe. Secondly, it also has to be able to reach the unborn baby in its mother’s womb by inhalation or absorption through the mother’s skin (topical application). Although there is often limited information about the actual safety of specific ingredients in skin products during pregnancy, if it is known that skin absorption is minimal then the exposure to the unborn baby is generally insignificant and the product or treatment is regarded as safe. Below is a summary of current advice. Cosmetics, Moisturisers and other Skin Care Products Cosmetics and over the counter skin products generally contain ingredients that are unlikely to be harmful in pregnancy as they are used by applying to the skin (rather than swallowing a tablet). -

Breastfeeding Matters
Breastfeeding Matters An important guide for breastfeeding families ACKNOWLEDGEMENTS Best Start by Health Nexus would like to thank the Public Health Units of Ontario who supported the creation and development of this provincial resource and generously shared their resources and expertise. We would also like to thank the parents and the experts who provided input for this booklet. Final review was done by Marg La Salle, RN, BScN, IBCLC, and BFI Lead Assessor. The information in this booklet is current at the time of production but information can change over time. Every effort will be made to ensure the information remains current. Throughout this resource, gender-specific language such as “woman”, “women” and “mother” is used in order to accurately cite the research referred to. We intend these terms to refer to all childbearing individuals, regardless of their gender identity or sexual orientation. Funded by the Government of Ontario. Table of Contents SECTION 1 .......................... 3 SECTION 4 ........................ 27 The Importance of Breastfeeding Important Things to Know • Risks of Not Breastfeeding • Waking a Sleepy Baby • Your Breastfeeding Rights • Calming a Fussy Baby • The Baby-Friendly Initiative • Burping Your Baby • Making an Informed Decision • Growth Spurts • Family Support • Sore Nipples • Peer Support • Using a Pacifier (Soother) • Engorgement SECTION 2 ........................ 11 • Storing Your Breast Milk Helping Your Baby Get a Good Start • Skin-to-Skin SECTION 5 ........................ 33 • Safe Positioning -

In a New Video, the Mom of Two Reveals the Dark Spot Toner She Swears By
In a new video, the mom of two reveals the dark spot toner she swears by. Hilary Duff, who is mom to Luca, 7, and Banks, 1, recently shared her “busy mom makeup routine” with Vogue — including the product she uses to treat her pregnancy melasma. “I’m a busy mom,” the actress says in the video. “I don’t have a ton of time to do my makeup, but this version today is on a day when I have my kids but also have a couple of meetings and I want to look like I put some effort in.” Duff starts off her routine by washing her hands or using hand sanitizer. She then reaches for her toner. “One really ‘cool’ thing that happened to me when I had babies is I got melasma,” she shared, pointing to a dark spot near the top of her forehead. “Every day, I say a little prayer that it’s taking care of that dark spot right there,” she says, rubbing on Ole Henriksen’s Glow2OH Dark Spot Toner ($29; sephora.com). Other products in Duff's kit include REN Clean Skincare Keep Young and Beautiful Anti-Aging Eye Cream ($44; sephora.com) and Perricone MD No Makeup Foundation Broad Spectrum SPF 20 ($60; ulta.com). What is melasma, exactly? Melasma is a common skin condition that causes brown to gray-brown patches to develop, usually on the face. Also referred to as the mask of pregnancy, melasma appears when a sharp rise in estrogen and progesterone levels stimulates excess melanin production, also known as hyperpigmentation. -

Drugs Affecting Milk Supply During Lactation
VOLUME 41 : NUMBER 1 : FEBRUARY 2018 ARTICLE Drugs affecting milk supply during lactation Treasure M McGuire SUMMARY Assistant director Practice and Development There are morbidity and mortality benefits for infants who are breastfed for longer periods. Mater Pharmacy Services Occasionally, drugs are used to improve the milk supply. Mater Health Services Brisbane Maternal perception of an insufficient milk supply is the commonest reason for ceasing Conjoint senior lecturer breastfeeding. Maternal stress or pain can also reduce milk supply. School of Pharmacy University of Queensland Galactagogues to improve milk supply are more likely to be effective if commenced within three weeks of delivery. The adverse effects of metoclopramide and domperidone must be Associate professor Pharmacology weighed against the benefits of breastfeeding. Faculty of Health Sciences Dopamine agonists have been used to suppress lactation. They have significant adverse effects and Medicine and bromocriptine should not be used because of an association with maternal deaths. Bond University Gold Coast nipple stimulation. Its release is inhibited by dopamine Introduction Keywords Breast milk is a complex, living nutritional fluid from the hypothalamus. Within a month of delivery, breastfeeding, that contains antibodies, enzymes, nutrients and basal prolactin returns to pre-pregnant levels in non- cabergoline, domperidone, galactagogues, lactation, hormones. Breastfeeding has many benefits for breastfeeding mothers. It remains elevated in nursing metoclopramide, prolactin babies such as fewer infections, increased intelligence, mothers, with peaks in response to infant suckling. probable protection against overweight and diabetes Drugs that act on dopamine can affect lactation. and, for mothers, cancer prevention.1 The World In response to suckling, oxytocin is released from Aust Prescr 2018;41:7-9 Health Organization recommends mothers breastfeed the posterior pituitary to enable the breast to https://doi.org/10.18773/ exclusively for six months postpartum. -

Breastfeeding Support Credentials
Who’s Who? A glance at breastfeeding support in the United States Lactation support is often needed to help mothers initiate and continue breastfeeding. There are many kinds of help available for breastfeeding mothers including peer counselors, certified breastfeeding educators and counselors, and lactation professionals such as the International Board Certified Lactation Consultant (IBCLC®). Breastfeeding support is valuable for a variety of reasons, from encouragement and emotional support to guidance and assistance with complex clinical situations. Mothers benefit from all kinds of support, and it is important to receive the right kind at the right time. The breastfeeding support categories listed below each play a vital role in providing care to mothers and babies. Breastfeeding Support Prerequisites Training Required Scope of Practice Type • 90 hours of lactation-specific education Recognized health Provide professional, • College level health science professional or evidence based, clinical courses Professional satisfactory completion lactation management; • 300-1000 clinical practice hours (International Board Certified of collegiate level educate families, health Lactation Consultant, IBCLC®) • Successful completion of a health sciences professionals and others criterion-referenced exam offered coursework. about human lactation. by an independent international board of examiners. Certified • 20-120 hours of classroom training Provide education and • Often includes a written exam guidance for families (i.e. Certified Lactation N/A Counselor, Certified or “certification” offered by the on basic breastfeeding Breastfeeding Educator, etc. ) training organization issues. Provide breastfeeding information, Peer Personal breastfeeding • 18-50 hours of classroom training encouragement, and (i.e. La Leche League, WIC experience. Peer Counselor, etc.) support to those in their community. Copyright © 2016 by USLCA.