Achondrogenesis
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Differential Diagnosis: Brittle Bone Conditions Other Than OI
Facts about Osteogenesis Imperfecta Differential Diagnosis: Brittle Bone Conditions Other than OI Fragile bones are the hallmark feature of osteogenesis imperfecta (OI). The mutations that cause OI lead to abnormalities within bone that result in increased bone turnover; reduced bone mineral content and decreased bone mineral density. The consequence of these changes is brittle bones that fracture easily. But not all cases of brittle bones are OI. Other causes of brittle bones include osteomalacia, disuse osteoporosis, disorders of increased bone density, defects of bone, and tumors. The following is a list of conditions that share fragile or brittle bones as a distinguishing feature. Brief descriptions and sources for further information are included. Bruck Syndrome This autosomal recessive disorder is also referred to as OI with contractures. Some people now consider this to be a type of OI. National Library of Medicine Genetics Home Reference: http://ghr.nlm.nih.gov Ehlers-Danlos Syndrome (EDS) Joint hyperextensibility with fractures; this is a variable disorder caused by several gene mutations. Ehlers-Danlos National Foundation http://www.ednf.org Fibrous Dysplasia Fibrous tissue develops in place of normal bone. This weakens the affected bone and causes it to deform or fracture. Fibrous Dysplasia Foundation: https://www.fibrousdysplasia.org Hypophosphatasia This autosomal recessive disorder affects the development of bones and teeth through defects in skeletal mineralization. Soft Bones: www.softbones.org; National Library of Medicine Genetics Home Reference: http://ghr.nlm.nih.gov/condition Idiopathic Juvenile Osteoporosis A non-hereditary transient form of childhood osteoporosis that is similar to mild OI (Type I) National Osteoporosis Foundation: www.nof.org McCune-Albright Syndrome This disorder affects the bones, skin, and several hormone-producing tissues. -

Prestin, a Cochlear Motor Protein, Is Defective in Non-Syndromic Hearing Loss
Human Molecular Genetics, 2003, Vol. 12, No. 10 1155–1162 DOI: 10.1093/hmg/ddg127 Prestin, a cochlear motor protein, is defective in non-syndromic hearing loss Xue Zhong Liu1,*, Xiao Mei Ouyang1, Xia Juan Xia2, Jing Zheng3, Arti Pandya2, Fang Li1, Li Lin Du1, Katherine O. Welch4, Christine Petit5, Richard J.H. Smith6, Bradley T. Webb2, Denise Yan1, Kathleen S. Arnos4, David Corey7, Peter Dallos3, Walter E. Nance2 and Zheng Yi Chen8 1Department of Otolaryngology, University of Miami, Miami, FL 33101, USA, 2Department of Human Genetics, Medical College of Virginia, Virginia Commonwealth University, Richmond, VA 23298-0033, USA, 3Department of Communication Sciences and Disorders, Auditory Physiology Laboratory (The Hugh Knowles Center), Northwestern University, Evanston, IL, USA, 4Department of Biology, Gallaudet University, Washington, DC 20002, USA, 5Unite´ de Ge´ne´tique des De´ficits Sensoriels, CNRS URA 1968, Institut Pasteur, Paris, France, 6Department of Otolaryngology University of Iowa, Iowa City, IA 52242, USA, 7Neurobiology Department, Harvard Medical School and Howard Hughes Medical Institute, Boston, MA, USA and 8Department of Neurology, Massachusetts General Hospital and Neurology Department, Harvard Medical School Boston, MA 02114, USA Received January 14, 2003; Revised and Accepted March 14, 2003 Prestin, a membrane protein that is highly and almost exclusively expressed in the outer hair cells (OHCs) of the cochlea, is a motor protein which senses membrane potential and drives rapid length changes in OHCs. Surprisingly, prestin is a member of a gene family, solute carrier (SLC) family 26, that encodes anion transporters and related proteins. Of nine known human genes in this family, three (SLC26A2, SLC26A3 and SLC26A4 ) are associated with different human hereditary diseases. -

Genetic Causes and Underlying Disease Mechanisms in Early-Onset Osteoporosis
From DEPARTMENT OF MOLECULAR MEDICINE AND SURGERY Karolinska Institutet, Stockholm, Sweden GENETIC CAUSES AND UNDERLYING DISEASE MECHANISMS IN EARLY-ONSET OSTEOPOROSIS ANDERS KÄMPE Stockholm 2020 All previously published papers were reproduced with permission from the publisher. Published by Karolinska Institutet. Printed by Eprint AB 2020 © Anders Kämpe, 2020 ISBN 978-91-7831-759-2 Genetic causes and underlying disease mechanisms in early-onset osteoporosis THESIS FOR DOCTORAL DEGREE (Ph.D.) By Anders Kämpe Principal Supervisor: Opponent: Professor Outi Mäkitie Professor André Uitterlinden Karolinska Institutet Erasmus Medical Centre, Rotterdam Department of Molecular Medicine and Surgery Department of Internal Medicine Laboratories Genetic Laboratory / Human Genomics Facility (HuGe-F) Co-supervisor(s): Examination Board: Associate Professor Anna Lindstrand Professor Marie-Louise Bondeson Karolinska Institutet Uppsala University Department of Molecular Medicine and Surgery Department of Immunology, Genetics and Pathology Associate Professor Giedre Grigelioniene Professor Göran Andersson Karolinska Institutet Karolinska Institutet Department of Molecular Medicine and Surgery Department of Laboratory Medicine Professor Ann Nordgren Minna Pöyhönen Karolinska Institutet University of Helsinki Department of Molecular Medicine and Surgery Department of Medical Genetics Associate Professor Hong Jiao Karolinska Institutet Department of Biosciences and Nutrition ABSTRACT Adult-onset osteoporosis is a disorder that affects a significant proportion of the elderly population worldwide and entails a substantial disease burden for the affected individuals. Childhood-onset osteoporosis is a rare condition often associating with a severe bone disease and recurrent fractures already in early childhood. Both childhood-onset and adult-onset osteoporosis have a large genetic component, but in children the disorder is usually genetically less complex and often caused by a single gene variant. -

Skeletal Dysplasias
Skeletal Dysplasias North Carolina Ultrasound Society Keisha L.B. Reddick, MD Wilmington Maternal Fetal Medicine Development of the Skeleton • 6 weeks – vertebrae • 7 weeks – skull • 8 wk – clavicle and mandible – Hyaline cartilage • Ossification – 7-12 wk – diaphysis appears – 12-16 wk metacarpals and metatarsals – 20+ wk pubis, calus, calcaneus • Visualization of epiphyseal ossification centers Epidemiology • Overall 9.1 per 1000 • Lethal 1.1 per 10,000 – Thanatophoric 1/40,000 – Osteogenesis Imperfecta 0.18 /10,000 – Campomelic 0.1 /0,000 – Achondrogenesis 0.1 /10,000 • Non-lethal – Achondroplasia 15 in 10,000 Most Common Skeletal Dysplasia • Thantophoric dysplasia 29% • Achondroplasia 15% • Osteogenesis imperfecta 14% • Achondrogenesis 9% • Campomelic dysplasia 2% Definition/Terms • Rhizomelia – proximal segment • Mezomelia –intermediate segment • Acromelia – distal segment • Micromelia – all segments • Campomelia – bowing of long bones • Preaxial – radial/thumb or tibial side • Postaxial – ulnar/little finger or fibular Long Bone Segments Counseling • Serial ultrasound • Genetic counseling • Genetic testing – Amniocentesis • Postnatal – Delivery center – Radiographs Assessment • Which segment is affected • Assessment of distal extremities • Any curvatures, fracture or clubbing noted • Are metaphyseal changes present • Hypoplastic or absent bones • Assessment of the spinal canal • Assessment of thorax. Skeletal Dysplasia Lethal Non-lethal • Thanatophoric • Achondroplasia • OI type II • OI type I, III, IV • Achondrogenesis • Hypochondroplasia -

Genes in Eyecare Geneseyedoc 3 W.M
Genes in Eyecare geneseyedoc 3 W.M. Lyle and T.D. Williams 15 Mar 04 This information has been gathered from several sources; however, the principal source is V. A. McKusick’s Mendelian Inheritance in Man on CD-ROM. Baltimore, Johns Hopkins University Press, 1998. Other sources include McKusick’s, Mendelian Inheritance in Man. Catalogs of Human Genes and Genetic Disorders. Baltimore. Johns Hopkins University Press 1998 (12th edition). http://www.ncbi.nlm.nih.gov/Omim See also S.P.Daiger, L.S. Sullivan, and B.J.F. Rossiter Ret Net http://www.sph.uth.tmc.edu/Retnet disease.htm/. Also E.I. Traboulsi’s, Genetic Diseases of the Eye, New York, Oxford University Press, 1998. And Genetics in Primary Eyecare and Clinical Medicine by M.R. Seashore and R.S.Wappner, Appleton and Lange 1996. M. Ridley’s book Genome published in 2000 by Perennial provides additional information. Ridley estimates that we have 60,000 to 80,000 genes. See also R.M. Henig’s book The Monk in the Garden: The Lost and Found Genius of Gregor Mendel, published by Houghton Mifflin in 2001 which tells about the Father of Genetics. The 3rd edition of F. H. Roy’s book Ocular Syndromes and Systemic Diseases published by Lippincott Williams & Wilkins in 2002 facilitates differential diagnosis. Additional information is provided in D. Pavan-Langston’s Manual of Ocular Diagnosis and Therapy (5th edition) published by Lippincott Williams & Wilkins in 2002. M.A. Foote wrote Basic Human Genetics for Medical Writers in the AMWA Journal 2002;17:7-17. A compilation such as this might suggest that one gene = one disease. -

Current Overview of Osteogenesis Imperfecta
medicina Review Current Overview of Osteogenesis Imperfecta Mari Deguchi *, Shunichiro Tsuji , Daisuke Katsura , Kyoko Kasahara, Fuminori Kimura and Takashi Murakami Department of Obstetrics & Gynecology, Shiga University of Medical Science, Otsu 520-2192, Shiga, Japan; [email protected] (S.T.); [email protected] (D.K.); [email protected] (K.K.); [email protected] (F.K.); [email protected] (T.M.) * Correspondence: [email protected] Abstract: Osteogenesis imperfecta (OI), or brittle bone disease, is a heterogeneous disorder charac- terised by bone fragility, multiple fractures, bone deformity, and short stature. OI is a heterogeneous disorder primarily caused by mutations in the genes involved in the production of type 1 collagen. Severe OI is perinatally lethal, while mild OI can sometimes not be recognised until adulthood. Severe or lethal OI can usually be diagnosed using antenatal ultrasound and confirmed by various imaging modalities and genetic testing. The combination of imaging parameters obtained by ultrasound, computed tomography (CT), and magnetic resource imaging (MRI) can not only detect OI accurately but also predict lethality before birth. Moreover, genetic testing, either noninvasive or invasive, can further confirm the diagnosis prenatally. Early and precise diagnoses provide parents with more time to decide on reproductive options. The currently available postnatal treatments for OI are not curative, and individuals with severe OI suffer multiple fractures and bone deformities throughout their lives. In utero mesenchymal stem cell transplantation has been drawing attention as a promising therapy for severe OI, and a clinical trial to assess the safety and efficacy of cell therapy is currently ongoing. -

Ultrasonic Demonstration of Fetal Skeletal Dysplasia Case Reports
222 SAMJ VOLUME 67 9 FEBRUARY 1985 Ultrasonic demonstration of fetal skeletal dysplasia Case reports L1NNIE M. MULLER, B. J. CREMIN Toshiba linear array scanners (with 3,5 mHz transducers) and a Philips SDU 7000 Sector/Static scanner. A routine obstetric Summary scan does not involve complete examination of all limbs, but Reports on prenatal diagnosis in cases of skeletal when a bony abnormality is noted a skeletal survey is dysplasia have mostly been in high-risk mothers attempted. Real-time ultrasound offers a flexible technique, with a suspect genetic background where the fetal and when the infant is in the prone vertex position the linear lesion could probably be predetermined. We deal array has the advantage of a wider range of skeletal visualiza with routine ultrasonographic appraisal of the fetal tion. skeleton when dysplasia is not initially suspected, A complete skeletal survey consists of an evaluation of the and relate our experience of the lethal forms of this bones of the skull, spine, thorax and limbs and of correlating these other fetal structures. We first measured the biparietal condition. During the 4-year period 1981 - 1984,6 cases of skeletal dysplasia, including thanatophoric diameter (BPD) and then noted the echogenic characteristics dysplasia, achondrogenesis, the Ellis-van Creveld of the skull and facial contours. A comprehensive evaluation of syndrome (chondro-ectodermal dysplasia) and the spine is possible from 17 weeks' gestation onwards. In a osteogenesis imperfecta, were detected; the ultra longitudinal plane the posterior elements form segmented sonographic findings are discussed. bands of echoes that conform to the fetal kyphosis, but it is not always possible to visualize the whole spine. -

MECHANISMS in ENDOCRINOLOGY: Novel Genetic Causes of Short Stature
J M Wit and others Genetics of short stature 174:4 R145–R173 Review MECHANISMS IN ENDOCRINOLOGY Novel genetic causes of short stature 1 1 2 2 Jan M Wit , Wilma Oostdijk , Monique Losekoot , Hermine A van Duyvenvoorde , Correspondence Claudia A L Ruivenkamp2 and Sarina G Kant2 should be addressed to J M Wit Departments of 1Paediatrics and 2Clinical Genetics, Leiden University Medical Center, PO Box 9600, 2300 RC Leiden, Email The Netherlands [email protected] Abstract The fast technological development, particularly single nucleotide polymorphism array, array-comparative genomic hybridization, and whole exome sequencing, has led to the discovery of many novel genetic causes of growth failure. In this review we discuss a selection of these, according to a diagnostic classification centred on the epiphyseal growth plate. We successively discuss disorders in hormone signalling, paracrine factors, matrix molecules, intracellular pathways, and fundamental cellular processes, followed by chromosomal aberrations including copy number variants (CNVs) and imprinting disorders associated with short stature. Many novel causes of GH deficiency (GHD) as part of combined pituitary hormone deficiency have been uncovered. The most frequent genetic causes of isolated GHD are GH1 and GHRHR defects, but several novel causes have recently been found, such as GHSR, RNPC3, and IFT172 mutations. Besides well-defined causes of GH insensitivity (GHR, STAT5B, IGFALS, IGF1 defects), disorders of NFkB signalling, STAT3 and IGF2 have recently been discovered. Heterozygous IGF1R defects are a relatively frequent cause of prenatal and postnatal growth retardation. TRHA mutations cause a syndromic form of short stature with elevated T3/T4 ratio. Disorders of signalling of various paracrine factors (FGFs, BMPs, WNTs, PTHrP/IHH, and CNP/NPR2) or genetic defects affecting cartilage extracellular matrix usually cause disproportionate short stature. -

Orphanet Report Series Rare Diseases Collection
Marche des Maladies Rares – Alliance Maladies Rares Orphanet Report Series Rare Diseases collection DecemberOctober 2013 2009 List of rare diseases and synonyms Listed in alphabetical order www.orpha.net 20102206 Rare diseases listed in alphabetical order ORPHA ORPHA ORPHA Disease name Disease name Disease name Number Number Number 289157 1-alpha-hydroxylase deficiency 309127 3-hydroxyacyl-CoA dehydrogenase 228384 5q14.3 microdeletion syndrome deficiency 293948 1p21.3 microdeletion syndrome 314655 5q31.3 microdeletion syndrome 939 3-hydroxyisobutyric aciduria 1606 1p36 deletion syndrome 228415 5q35 microduplication syndrome 2616 3M syndrome 250989 1q21.1 microdeletion syndrome 96125 6p subtelomeric deletion syndrome 2616 3-M syndrome 250994 1q21.1 microduplication syndrome 251046 6p22 microdeletion syndrome 293843 3MC syndrome 250999 1q41q42 microdeletion syndrome 96125 6p25 microdeletion syndrome 6 3-methylcrotonylglycinuria 250999 1q41-q42 microdeletion syndrome 99135 6-phosphogluconate dehydrogenase 67046 3-methylglutaconic aciduria type 1 deficiency 238769 1q44 microdeletion syndrome 111 3-methylglutaconic aciduria type 2 13 6-pyruvoyl-tetrahydropterin synthase 976 2,8 dihydroxyadenine urolithiasis deficiency 67047 3-methylglutaconic aciduria type 3 869 2A syndrome 75857 6q terminal deletion 67048 3-methylglutaconic aciduria type 4 79154 2-aminoadipic 2-oxoadipic aciduria 171829 6q16 deletion syndrome 66634 3-methylglutaconic aciduria type 5 19 2-hydroxyglutaric acidemia 251056 6q25 microdeletion syndrome 352328 3-methylglutaconic -

2 Achondrogenesis, Type IB A
Achondrogenesis,Type IB 579 2 Achondrogenesis,Type IB A Fraccaro type Extremities • Extremely short tubular bones, with squared, Severely shortened long bones with loss of longitudi- trapezoid, or stellate appearance nal orientation; unossified fibulas; deficient ossifica- • Wide and cupped ends of the long bones, with lat- tion of vertebral bodies, pelvis, and sacrum eral spurs • Unossified fibulas Frequency: 1 in 50,000 births. Skull • Ossified or only mildly underossified calvarium Genetics Autosomal recessive (OMIM 600972), caused by mutations in the DTDST gene at 5q32-q33 Bibliography Clinical Features Beluffi G. Achondrogenesis, type I. Rofo Fortschr Geb Rönt- • Fetal hydrops, polyhydramnios genstr Nuklearmed 1977; 127: 341–4 • Borochowitz Z, Lachman R, Adominan GE, Spear G, Jones K, Premature birth, stillbirth or death within min- Rimoin DL. Achondrogenesis type I: delineation of further utes in large proportion of cases heterogeneity and identification of two distinct subgroups. • Marked micromelic dwarfism J Pediatr 1988; 112: 23–31 • Normocephaly, but head appearing large because Jaeger HJ, Schmitz-Stolbrink A, Hulde J, Novak M, Roggen- of small body kamp K, Mathias K. The boneless neonate: a severe form of • achondrogenesis type I. Pediatr Radiol 1994; 24: 319–21 Severe midface hypoplasia Maroteaux P, Lamy M: Le diagnostic des nanismes chrondro- • Low nasal bridge dystrophiques chez les nouveau-nés. Arch Fr Pediatr 1968; • Micrognathia 25: 241–62 • Short neck Spranger JW, Langer LO, Wiedemann HR. Bone dysplasias. An • Short trunk, barrel-shaped chest atlas of constitutional disorders of skeletal development. • W.B. Saunders Company, Philadelphia, 1974, pp. 24–5 Overdistended abdomen Superti-Furga A, Hastbacka J, Wilcox WR, Cohn DH, van der • Edema of soft tissues Harten HJ, Rossi A, Blau N, Rimoin DL, Steinmann B, Lan- • Prenatal detection of micromelia by ultrasound der ES, Gitzelmann R. -

Kniest Dysplasia Natural History
Richard M. Pauli, M.D., Ph.D., Midwest Regional Bone Dysplasia Clinics revised 8/2009 KNIEST DYSPLASIA NATURAL HISTORY INTRODUCTION: The following summary of the medical expectations in Kniest Dysplasia is neither exhaustive nor cited. It is based upon the available literature as well as personal experience in the Midwest Regional Bone Dysplasia Clinics (MRBDC). It is meant to provide a guideline for the kinds of problems that may arise in children with this disorder, and particularly to help clinicians caring for a recently diagnosed child. For specific questions or more detailed discussions, feel free to contact MRBDC at the University of Wisconsin – Madison [phone – 608 262 6228; fax – 608 263 3496; email – [email protected]]. Kniest Dysplasia is an infrequent bone dysplasia, which is particularly characterized by progressive stiffness and enlargement of various joints. In addition, it shares many other medical risks with other disorders of type II collagen (such as Spondyloepiphyseal Dysplasia, Congenita). Individuals will typically have both a short trunk and a constricted chest from birth and arms and legs that appear to be disproportionately long. MEDICAL ISSUES AND PARENTAL CONCERNS TO BE ANTICIPATED PROBLEM: GROWTH EXPECTATIONS: Marked short stature is typical; ultimate adult height is usually between 100 and 140 cm (about 39 in to 55 in). MONITORING: No diagnosis-specific growth grid is available. INTERVENTION: No known treatment is effective. Growth hormone is not likely to be effective since this disorder is secondary to intrinsic abnormality of bone growth. Limb lengthening, suggested but controversial in other short stature syndromes, is probably not an option since much of the effects of this disorder is on spine growth not primarily the limbs. -
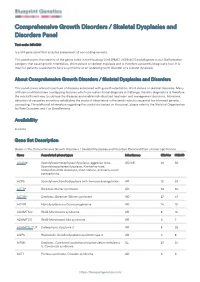
Blueprint Genetics Comprehensive Growth Disorders / Skeletal
Comprehensive Growth Disorders / Skeletal Dysplasias and Disorders Panel Test code: MA4301 Is a 374 gene panel that includes assessment of non-coding variants. This panel covers the majority of the genes listed in the Nosology 2015 (PMID: 26394607) and all genes in our Malformation category that cause growth retardation, short stature or skeletal dysplasia and is therefore a powerful diagnostic tool. It is ideal for patients suspected to have a syndromic or an isolated growth disorder or a skeletal dysplasia. About Comprehensive Growth Disorders / Skeletal Dysplasias and Disorders This panel covers a broad spectrum of diseases associated with growth retardation, short stature or skeletal dysplasia. Many of these conditions have overlapping features which can make clinical diagnosis a challenge. Genetic diagnostics is therefore the most efficient way to subtype the diseases and enable individualized treatment and management decisions. Moreover, detection of causative mutations establishes the mode of inheritance in the family which is essential for informed genetic counseling. For additional information regarding the conditions tested on this panel, please refer to the National Organization for Rare Disorders and / or GeneReviews. Availability 4 weeks Gene Set Description Genes in the Comprehensive Growth Disorders / Skeletal Dysplasias and Disorders Panel and their clinical significance Gene Associated phenotypes Inheritance ClinVar HGMD ACAN# Spondyloepimetaphyseal dysplasia, aggrecan type, AD/AR 20 56 Spondyloepiphyseal dysplasia, Kimberley