Lumbar Microdiscectomy: a Historical Perspective and Current Technical Considerations
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Anterior Reconstruction Techniques for Cervical Spine Deformity
Neurospine 2020;17(3):534-542. Neurospine https://doi.org/10.14245/ns.2040380.190 pISSN 2586-6583 eISSN 2586-6591 Review Article Anterior Reconstruction Techniques Corresponding Author for Cervical Spine Deformity Samuel K. Cho 1,2 1 1 1 https://orcid.org/0000-0001-7511-2486 Murray Echt , Christopher Mikhail , Steven J. Girdler , Samuel K. Cho 1Department of Orthopedics, Icahn School of Medicine at Mount Sinai, New York, NY, USA Department of Orthopaedics, Icahn 2 Department of Neurological Surgery, Montefiore Medical Center/Albert Einstein College of Medicine, Bronx, School of Medicine at Mount Sinai, 425 NY, USA West 59th Street, 5th Floor, New York, NY, USA E-mail: [email protected] Cervical spine deformity is an uncommon yet severely debilitating condition marked by its heterogeneity. Anterior reconstruction techniques represent a familiar approach with a range Received: June 24, 2020 of invasiveness and correction potential—including global or focal realignment in the sagit- Revised: August 5, 2020 tal and coronal planes. Meticulous preoperative planning is required to improve or prevent Accepted: August 17, 2020 neurologic deterioration and obtain satisfactory global spinal harmony. The ability to per- form anterior only reconstruction requires mobility of the opposite column to achieve cor- rection, unless a combined approach is planned. Anterior cervical discectomy and fusion has limited focal correction, but when applied over multiple levels there is a cumulative ef- fect with a correction of approximately 6° per level. Partial or complete corpectomy has the ability to correct sagittal deformity as well as decompress the spinal canal when there is an- terior compression behind the vertebral body. -

Spinal Interventional Pain Management and Lumbar Spine Surgery
Spinal Interventional Pain Management and Lumbar Spine Surgery Policy Number: Original Effective Date: MM.06.024 01/01/2014 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 12/15/2017 Section: Surgery; Medicine Place(s) of Service: Office; Outpatient; Inpatient I. Description The following spinal interventional pain management and lumbar spine surgery procedures require precertification through Magellan Hawaii, formally known as National Imaging Associates, Inc. (NIA): A. Spinal Epidural Injections B. Paravertebral Facet Joint Denervation (radiofrequency neurolysis) C. Paravertebral Facet Joint Injections or Blocks D. Sacroiliac joint injections E. Lumbar Spinal Fusion Surgery II. Administrative Guidelines A. The ordering physician can obtain precertification or consult with Magellan Hawaii by accessing their website at http://www.radmd.com/ or by calling 1 (866) 306-9729, from 6 a.m. to 6 p.m., weekdays, Hawaii Time. Refer to the e-library for instructions on navigating the radmd.com website (RadMD Get Started) and requesting precertification/checking the status of a request (RadMD QuickStart). B. For access to the latest clinical guidelines used for precertification, go to www.radmd.com and click on the link entitled View Clinical Guidelines. C. For interventional pain management procedures (epidural injections, facet joint denervation neurolysis, facet joint injections and sacroiliac joint injections), if more than one procedure is planned, a separate precertification number must be obtained for each procedure planned. D. For spinal surgeries (lumbar fusions, lumbar decompressions, and lumbar microdiscectomy), one precertification number should be obtained for the most invasive surgery to be performed. E. Precertification requirements for injection procedures apply only to office and outpatient services (POS 11, 22, or 24). -

Lumbar Spine Schmorl's Nodes; Prevalence in Adults with Back Pain, and Their Relation to Vertebral Endplate Degeneration Israa Mohammed Sadiq
Sadiq Egyptian Journal of Radiology and Nuclear Medicine (2019) 50:65 Egyptian Journal of Radiology https://doi.org/10.1186/s43055-019-0069-9 and Nuclear Medicine RESEARCH Open Access Lumbar spine Schmorl's nodes; prevalence in adults with back pain, and their relation to vertebral endplate degeneration Israa Mohammed Sadiq Abstract Background: In 1927, Schmorl described a focal herniation of disc material into the adjacent vertebral body through a defect in the endplate, named as Schmorl’s node (SN). The aim of the study is to reveal the prevalence and distribution of Schmorl’s nodes (SNs) in the lumbar spine and their relation to disc degeneration disease in Kirkuk city population. Results: A cross-sectional analytic study was done for 324 adults (206 females and 118 males) with lower back pain evaluated as physician requests by lumbosacral MRI at the Azadi Teaching Hospital, Kirkuk city, Iraq. The demographic criteria of the study sample were 20–71 years old, 56–120 kg weight, and 150–181 cm height. SNs were seen in 72 patients (22%). Males were affected significantly more than the females (28.8% vs. 18.8%, P = 0.03). SNs were most significantly affecting older age groups. L1–L2 was the most affected disc level (23.6%) and the least was L5–S1 (8.3%). There was neither a significant relationship between SN and different disc degeneration scores (P = 0.76) nor with disc herniation (P = 0.62, OR = 1.4), but there was a significant relation (P = 0.00001, OR = 7.9) with MC. Conclusion: SN is a frequent finding in adults’ lumbar spine MRI, especially in males; it is related to vertebral endplate bony pathology rather than discal pathology. -

Automated Percutaneous and Endoscopic Discectomy
Corporate Medical Policy Automated Percutaneous and Endoscopic Discectomy File Name: percutaneous_discectomy Origination: 9/1991 Last CAP Review: 5/2021 Next CAP Review: 5/2022 Last Review: 5/2021 Description of Procedure or Service Surgical management of herniated intervertebral discs most commonly involves discectomy or microdiscectomy, performed manually through an open incision. Automated percutaneous discectomy involves placement of a probe within the intervertebral disc under image guidance with aspiration of disc material using a suction cutting device. Removal of disc herniations under endoscopic visualization is also being investigated. Endoscopic discectomy involves the percutaneous placement of a working channel under image guidance, followed by visualization of the working space and instruments through an endoscope, and aspiration of disc material. Back pain or radiculopathy related to herniated discs is an extremely common condition and a frequent cause of chronic disability. Although many cases of acute low back pain and radiculopathy will resolve with conservative care, a surgical decompression is often considered when the pain is unimproved after several months and is clearly neuropathic in origin, resulting from irritation of the nerve roots. Open surgical treatment typically consists of discectomy, in which the extruding disc material is excised. When performed with an operating microscope the procedure is known as microdiscectomy. Minimally invasive options have also been researched, in which some portion of the disc is removed or ablated, although these techniques are not precisely targeted at the offending extruding disc material. Ablative techniques include laser discectomy and radiofrequency (RF) decompression. In addition, intradiscal electrothermal annuloplasty is another minimally invasive approach to low back pain. -
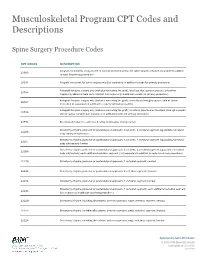
Musculoskeletal Program CPT Codes and Descriptions
Musculoskeletal Program CPT Codes and Descriptions Spine Surgery Procedure Codes CPT CODES DESCRIPTION Allograft, morselized, or placement of osteopromotive material, for spine surgery only (List separately in addition 20930 to code for primary procedure) 20931 Allograft, structural, for spine surgery only (List separately in addition to code for primary procedure) Autograft for spine surgery only (includes harvesting the graft); local (eg, ribs, spinous process, or laminar 20936 fragments) obtained from same incision (List separately in addition to code for primary procedure) Autograft for spine surgery only (includes harvesting the graft); morselized (through separate skin or fascial 20937 incision) (List separately in addition to code for primary procedure) Autograft for spine surgery only (includes harvesting the graft); structural, bicortical or tricortical (through separate 20938 skin or fascial incision) (List separately in addition to code for primary procedure) 20974 Electrical stimulation to aid bone healing; noninvasive (nonoperative) Osteotomy of spine, posterior or posterolateral approach, 3 columns, 1 vertebral segment (eg, pedicle/vertebral 22206 body subtraction); thoracic Osteotomy of spine, posterior or posterolateral approach, 3 columns, 1 vertebral segment (eg, pedicle/vertebral 22207 body subtraction); lumbar Osteotomy of spine, posterior or posterolateral approach, 3 columns, 1 vertebral segment (eg, pedicle/vertebral 22208 body subtraction); each additional vertebral segment (List separately in addition to code for -

Artificial Intervertebral Disc: Lumbar Spine Page 1 of 22
Artificial Intervertebral Disc: Lumbar Spine Page 1 of 22 Medical Policy An Independent licensee of the Blue Cross Blue Shield Association Title: Artificial Intervertebral Disc: Lumbar Spine Related Policy: . Artificial Intervertebral Disc: Cervical Spine Professional Institutional Original Effective Date: August 9, 2005 Original Effective Date: August 9, 2005 Revision Date(s): June 14, 2006; Revision Date(s): June 14, 2006; January 1, 2007; July 24, 2007; January 1, 2007; July 24, 2007; September 25 2007; February 22, 2010; September 25 2007; February 22, 2010; March 10, 2011; March 8, 2013; March 10 2011; March 8, 2013; June 23, 2015; August 4, 2016; June 23, 2015; August 4, 2016; May 23, 2018; July 17, 2019; May 23, 2018; July 17, 2019; August 21, 2020; July 1, 2021 August 21, 2020; July 1, 2021 Current Effective Date: September 23, 2008 Current Effective Date: September 23, 2008 State and Federal mandates and health plan member contract language, including specific provisions/exclusions, take precedence over Medical Policy and must be considered first in determining eligibility for coverage. To verify a member's benefits, contact Blue Cross and Blue Shield of Kansas Customer Service. The BCBSKS Medical Policies contained herein are for informational purposes and apply only to members who have health insurance through BCBSKS or who are covered by a self-insured group plan administered by BCBSKS. Medical Policy for FEP members is subject to FEP medical policy which may differ from BCBSKS Medical Policy. The medical policies do not constitute medical advice or medical care. Treating health care providers are independent contractors and are neither employees nor agents of Blue Cross and Blue Shield of Kansas and are solely responsible for diagnosis, treatment and medical advice. -

Biomechanical Evaluation of Relationship of Screw Pullout
ORIGINAL ARTICLE Biomechanical Evaluation of Relationship of Screw Pullout Strength, Insertional Torque, and Bone Mineral Density in the Cervical Spine Charles Alan Reitman, MD, Lyndon Nguyen, and Guy R. Fogel help prevent implant loosening and add rigidity to the plate- Background: Understanding of implant failure mechanisms is im- screw construct. Some screws actually lock to the plate, while portant in the successful utilization of anterior cervical plates. Many in most cases, there is some kind of blocking plate or screw variables influence screw purchase, including the quality of the bone. head expansion to secure the screw to the plate. In these cases, The purpose of this study was to assess the relationship of screw pull- out and screw insertional torque across a wide range of bone mineral the screws are initially placed securely per the surgeon’s own densities (BMDs). perception, in most instances without specific torque control. Screw pullout and stripping (exceeding maximal inser- Methods: A total of 54 cervical vertebrae in 12 cervical spines were tional torque) are possible modes of failure. Some factors af- evaluated for BMD using dual-energy x-ray absorptiometry scan- fecting the pullout strength of a cancellous bone screw are spe- ning. Actual and perceived peak torques of 3.5-mm anterior cervical cific to the screw design and include the major diameter of the screws were determined at each level followed by screw pullout screw, the length of engagement of the thread, and screw strength testing. thread depth and pitch.4 Furthermore, tapping was found to Results: A high correlation was observed between screw pullout reduce pullout force by an average of 8% compared with non- strength and BMD. -

Redefining Lumbar Spinal Stenosis As a Developmental Syndrome
CLINICAL ARTICLE J Neurosurg Spine 29:654–660, 2018 Redefining lumbar spinal stenosis as a developmental syndrome: an MRI-based multivariate analysis of findings in 709 patients throughout the 16- to 82-year age spectrum Sameer Kitab, MD,1 Bryan S. Lee, MD,2,3 and Edward C. Benzel, MD2,3 1Scientific Council of Orthopedics, Baghdad, Iraq; 2Department of Neurosurgery, Cleveland Clinic Lerner College of Medicine of Case Western Reserve University, Cleveland Clinic; and 3Center for Spine Health, Neurological Institute, Cleveland Clinic, Cleveland, Ohio OBJECTIVE Using an imaging-based prospective comparative study of 709 eligible patients that was designed to as- sess lumbar spinal stenosis (LSS) in the ages between 16 and 82 years, the authors aimed to determine whether they could formulate radiological structural differences between the developmental and degenerative types of LSS. METHODS MRI structural changes were prospectively reviewed from 2 age cohorts of patients: those who presented clinically before the age of 60 years and those who presented at 60 years or older. Categorical degeneration variables at L1–S1 segments were compared. A multivariate comparative analysis of global radiographic degenerative variables and spinal dimensions was conducted in both cohorts. The age at presentation was correlated as a covariable. RESULTS A multivariate analysis demonstrated no significant between-groups differences in spinal canal dimensions and stenosis grades in any segments after age was adjusted for. There were no significant variances between the 2 cohorts in global degenerative variables, except at the L4–5 and L5–S1 segments, but with only small effect sizes. Age- related degeneration was found in the upper lumbar segments (L1–4) more than the lower lumbar segments (L4–S1). -

The Effectiveness of Lumbar Spinal Perineural Analgesia (LSPA) for Various Causes of Low Back Ache
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-ISSN: 2279-0853, p-ISSN: 2279-0861.Volume 19, Issue 6 Ser.19 (June. 2020), PP 08-13 www.iosrjournals.org The Effectiveness of Lumbar Spinal Perineural Analgesia (LSPA) For Various Causes of Low Back Ache Dr. Biju Bhadran MS MCh1, Dr. Arvind K R MS MCh2, Dr. Krishnakumar MS MCh3, Dr. Harrison MS MCh4, Dr. Raghunath MCh5 1Department of Neurosurgery, Govt. TD Medical College, Alappuzha, Kerala, India 2Department of Neurosurgery, Govt. TD Medical College, Alappuzha, Kerala, India 3Department of Neurosurgery, Govt. TD Medical College, Alappuzha, Kerala, India 4Department of Neurosurgery, Govt. TD Medical College, Alappuzha, Kerala, India 5Department of Neurosurgery, Govt. TD Medical College, Alappuzha, Kerala, India Abstract: Background: Back pain is a common medical problem and predominant cause for medical consultations. The concept of lumbar spinal perineural analgesia (LSPA) is to achieve reduction of pain and desensitization of irritated neural structures and not complete analgesia or paralysis of lumbar spinal nerves. This article is intended to study the effectiveness of lumbar spinal perineural analgesia (LSPA) for various causes of low back ache on the basis of degree of pain relief following the procedure. Materials and Methods: This was a prospective study comprising of 50 patients who had undergone appropriate investigations before assessment for eligibility, confirming the existence of lumbar disc disease and these selected patients underwent lumbar perineural analgesia for different causes of low back ache not relieved with other conservative modalities of treatment. Pre procedure and post procedure, the severity of pain level was assessed with standard verbal rating scale (VRS), with a score of 1 = no pain, 2 = mild pain, 3 = moderate pain, 4 = severe pain and 5 = intolerable pain. -

The Costs and Benefits of Moving to the ICD-10 Code Sets
CHILDREN AND ADOLESCENTS This PDF document was made available from www.rand.org as a public CIVIL JUSTICE service of the RAND Corporation. EDUCATION ENERGY AND ENVIRONMENT Jump down to document HEALTH AND HEALTH CARE 6 INTERNATIONAL AFFAIRS POPULATION AND AGING The RAND Corporation is a nonprofit research PUBLIC SAFETY SCIENCE AND TECHNOLOGY organization providing objective analysis and effective SUBSTANCE ABUSE solutions that address the challenges facing the public TERRORISM AND HOMELAND SECURITY and private sectors around the world. TRANSPORTATION AND INFRASTRUCTURE U.S. NATIONAL SECURITY Support RAND Purchase this document Browse Books & Publications Make a charitable contribution For More Information Visit RAND at www.rand.org Explore RAND Science and Technology View document details Limited Electronic Distribution Rights This document and trademark(s) contained herein are protected by law as indicated in a notice appearing later in this work. This electronic representation of RAND intellectual property is provided for non-commercial use only. Permission is required from RAND to reproduce, or reuse in another form, any of our research documents for commercial use. This product is part of the RAND Corporation technical report series. Reports may include research findings on a specific topic that is limited in scope; present discus- sions of the methodology employed in research; provide literature reviews, survey instruments, modeling exercises, guidelines for practitioners and research profes- sionals, and supporting documentation; -

Diagnosis and Treatment of Lumbar Disc Herniation with Radiculopathy
Y Lumbar Disc Herniation with Radiculopathy | NASS Clinical Guidelines 1 G Evidence-Based Clinical Guidelines for Multidisciplinary ETHODOLO Spine Care M NE I DEL I U /G ON Diagnosis and Treatment of I NTRODUCT Lumbar Disc I Herniation with Radiculopathy NASS Evidence-Based Clinical Guidelines Committee D. Scott Kreiner, MD Paul Dougherty, II, DC Committee Chair, Natural History Chair Robert Fernand, MD Gary Ghiselli, MD Steven Hwang, MD Amgad S. Hanna, MD Diagnosis/Imaging Chair Tim Lamer, MD Anthony J. Lisi, DC John Easa, MD Daniel J. Mazanec, MD Medical/Interventional Treatment Chair Richard J. Meagher, MD Robert C. Nucci, MD Daniel K .Resnick, MD Rakesh D. Patel, MD Surgical Treatment Chair Jonathan N. Sembrano, MD Anil K. Sharma, MD Jamie Baisden, MD Jeffrey T. Summers, MD Shay Bess, MD Christopher K. Taleghani, MD Charles H. Cho, MD, MBA William L. Tontz, Jr., MD Michael J. DePalma, MD John F. Toton, MD This clinical guideline should not be construed as including all proper methods of care or excluding or other acceptable methods of care reason- ably directed to obtaining the same results. The ultimate judgment regarding any specific procedure or treatment is to be made by the physi- cian and patient in light of all circumstances presented by the patient and the needs and resources particular to the locality or institution. I NTRODUCT 2 Lumbar Disc Herniation with Radiculopathy | NASS Clinical Guidelines I ON Financial Statement This clinical guideline was developed and funded in its entirety by the North American Spine Society (NASS). All participating /G authors have disclosed potential conflicts of interest consistent with NASS’ disclosure policy. -

Utilization Management Policy Title: Lumbar Spine Surgeries
Medica Policy No. III-SUR.34 UTILIZATION MANAGEMENT POLICY TITLE: LUMBAR SPINE SURGERIES EFFECTIVE DATE: January 18, 2021 This policy was developed with input from specialists in orthopedic spine surgery and endorsed by the Medical Policy Committee. IMPORTANT INFORMATION – PLEASE READ BEFORE USING THIS POLICY These services may or may not be covered by all Medica plans. Please refer to the member’s plan document for specific coverage information. If there is a difference between this general information and the member’s plan document, the member’s plan document will be used to determine coverage. With respect to Medicare and Minnesota Health Care Programs, this policy will apply unless these programs require different coverage. Members may contact Medica Customer Service at the phone number listed on their member identification card to discuss their benefits more specifically. Providers with questions about this Medica utilization management policy may call the Medica Provider Service Center toll-free at 1-800-458-5512. Medica utilization management policies are not medical advice. Members should consult with appropriate health care providers to obtain needed medical advice, care and treatment. PURPOSE To promote consistency between Utilization Management reviewers by providing the criteria that determine medical necessity. BACKGROUND I. Prevalence / Incidence A. It is reported that the lifetime incidence of low back pain (LBP) in the general population within the United States is between 60% and 90%, with an annual incidence of 5%. According to a National Center for Health Statistics study (Patel, 2007), 14.3% of new patient visits to primary care physicians per year are for LBP.