Watch and Wait in Neurofibromatosis Type 1 Cases
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Neurofibromatosis Type 2 (NF2)
International Journal of Molecular Sciences Review Neurofibromatosis Type 2 (NF2) and the Implications for Vestibular Schwannoma and Meningioma Pathogenesis Suha Bachir 1,† , Sanjit Shah 2,† , Scott Shapiro 3,†, Abigail Koehler 4, Abdelkader Mahammedi 5 , Ravi N. Samy 3, Mario Zuccarello 2, Elizabeth Schorry 1 and Soma Sengupta 4,* 1 Department of Genetics, Cincinnati Children’s Hospital, Cincinnati, OH 45229, USA; [email protected] (S.B.); [email protected] (E.S.) 2 Department of Neurosurgery, University of Cincinnati, Cincinnati, OH 45267, USA; [email protected] (S.S.); [email protected] (M.Z.) 3 Department of Otolaryngology, University of Cincinnati, Cincinnati, OH 45267, USA; [email protected] (S.S.); [email protected] (R.N.S.) 4 Department of Neurology, University of Cincinnati, Cincinnati, OH 45267, USA; [email protected] 5 Department of Radiology, University of Cincinnati, Cincinnati, OH 45267, USA; [email protected] * Correspondence: [email protected] † These authors contributed equally. Abstract: Patients diagnosed with neurofibromatosis type 2 (NF2) are extremely likely to develop meningiomas, in addition to vestibular schwannomas. Meningiomas are a common primary brain tumor; many NF2 patients suffer from multiple meningiomas. In NF2, patients have mutations in the NF2 gene, specifically with loss of function in a tumor-suppressor protein that has a number of synonymous names, including: Merlin, Neurofibromin 2, and schwannomin. Merlin is a 70 kDa protein that has 10 different isoforms. The Hippo Tumor Suppressor pathway is regulated upstream by Merlin. This pathway is critical in regulating cell proliferation and apoptosis, characteristics that are important for tumor progression. -

Information About Mosaic Neurofibromatosis Type 2 (NF2)
Information about mosaic Neurofibromatosis type 2 (NF2) NF2 occurs because of a mutation (change) in the NF2 gene. When this change is present at the time of conception the changed gene will be present in all the cells of the baby. When this mutation occurs later in the development of the forming embryo, the baby will go on to have a mix of cells: some with the “normal” genetic information and some with the changed information. This mix of cells is called mosaicism. Approximately half the people who have a diagnosis of NF2 have inherited the misprinted NF2 gene change from their mother or father who will also have NF2. They will have that misprinted gene in all the cells of their body. When they have their children, there will be a 1 in 2 chance of passing on NF2 to each child they have. However about half of people with NF2 are the first person in the family to be affected. They have no family history and have not inherited the condition from a parent. When doctors studied this group of patients more closely they noticed certain characteristics. Significantly they observed that fewer children had inherited NF2 than expected some people in this group had relatively mild NF2 NF2 tumours in some patients tended to grow on one side of their body rather than both sides that when a blood sample was tested to identify the NF2 gene, the gene change could not be found in 30-40% of people This lead researchers to conclude that this group of people were most likely to be mosaic for NF2 i.e. -

Adrenal Neuroblastoma Mimicking Pheochromocytoma in an Adult With
Khalayleh et al. Int Arch Endocrinol Clin Res 2017, 3:008 Volume 3 | Issue 1 International Archives of Endocrinology Clinical Research Case Report : Open Access Adrenal Neuroblastoma Mimicking Pheochromocytoma in an Adult with Neurofibromatosis Type 1 Harbi Khalayleh1, Hilla Knobler2, Vitaly Medvedovsky2, Edit Feldberg3, Judith Diment3, Lena Pinkas4, Guennadi Kouniavsky1 and Taiba Zornitzki2* 1Department of Surgery, Hebrew University Medical School of Jerusalem, Israel 2Endocrinology, Diabetes and Metabolism Institute, Kaplan Medical Center, Hebrew University Medical School of Jerusalem, Israel 3Pathology Institute, Kaplan Medical Center, Israel 4Nuclear Medicine Institute, Kaplan Medical Center, Israel *Corresponding author: Taiba Zornitzki, MD, Endocrinology, Diabetes and Metabolism Institute, Kaplan Medical Center, Hebrew University Medical School of Jerusalem, Bilu 1, 76100 Rehovot, Israel, Tel: +972-894- 41315, Fax: +972-8 944-1912, E-mail: [email protected] Context 2. This is the first reported case of an adrenal neuroblastoma occurring in an adult patient with NF1 presenting as a large Neurofibromatosis type 1 (NF1) is a genetic disorder asso- adrenal mass with increased catecholamine levels mimicking ciated with an increased risk of malignant disorders. Adrenal a pheochromocytoma. neuroblastoma is considered an extremely rare tumor in adults and was not previously described in association with NF1. 3. This case demonstrates the clinical overlap between pheo- Case description: A 42-year-old normotensive woman with chromocytoma and neuroblastoma. typical signs of NF1 underwent evaluation for abdominal pain, Keywords and a large 14 × 10 × 16 cm left adrenal mass displacing the Adrenal neuroblastoma, Neurofibromatosis type 1, Pheo- spleen, pancreas and colon was found. An initial diagnosis of chromocytoma, Neural crest-derived tumors pheochromocytoma was done based on the known strong association between pheochromocytoma, NF1 and increased catecholamine levels. -
A Case of Intramedullary Spinal Cord Astrocytoma Associated with Neurofibromatosis Type 1
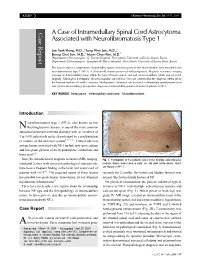
KISEP J Korean Neurosurg Soc 36 : 69-71, 2004 Case Report A Case of Intramedullary Spinal Cord Astrocytoma Associated with Neurofibromatosis Type 1 Jae Taek Hong, M.D.,1 Sang Won Lee, M.D.,1 Byung Chul Son, M.D.,1 Moon Chan Kim, M.D.2 Department of Neurosurgery,1 St. Vincent Hospital, The Catholic University of Korea, Suwon, Korea Department of Neurosurgery,2 Kangnam St. Mary's Hospital, The Catholic University of Korea, Seoul, Korea The authors report a symptomatic intramedullary spinal cord astrocytoma in the thoracolumbar area associated with neurofibromatosis type 1 (NF-1). A 38-year-old woman presented with paraparesis. Magnetic resonance imaging revealed an intramedullary lesion within the lower thoracic spinal cord and conus medullaris, which was removed surgically. Pathological investigation showed anaplastic astrocytoma. This case confirms that the diagnosis criteria set by the National Institute of Health Consensus Development Conference can be useful to differentiate ependymoma from astrocytoma when making a preoperative diagnosis of intramedullary spinal cord tumor in patients of NF-1. KEY WORDS : Astrocytoma·Intramedullary cord tumor·Neurofibromatosis. Introduction eurofibromatosis type 1 (NF-1), also known as von N Recklinghausen's disease, is one of the most common autosomal dominant inherited disorders with an incidence of 1 in 3,000 individuals and is characterized by a predisposition to tumors of the nervous system5,6,12,16). Central nervous system lesions associated with NF-1 include optic nerve glioma and low-grade gliomas of the hypothalamus, cerebellum and brain stem6,10). Since the introduction of magnetic resonance(MR) imaging, Fig. 1. Photograph of the patient's back shows multiple subcutaneous incidental lesions with uncertain pathological characteristic nodules (black arrow) and a cafe-au-lait spot (white arrow), which have been a frequent finding in the brain and spinal cord of are typical of NF-1. -

Cutaneous Neurofibromas: Clinical Definitions Current Treatment Is Limited to Surgical Removal Or Physical Or Descriptors Destruction
ARTICLE OPEN ACCESS Cutaneous neurofibromas Current clinical and pathologic issues Nicolas Ortonne, MD, PhD,* Pierre Wolkenstein, MD, PhD,* Jaishri O. Blakeley, MD, Bruce Korf, MD, PhD, Correspondence Scott R. Plotkin, MD, PhD, Vincent M. Riccardi, MD, MBA, Douglas C. Miller, MD, PhD, Susan Huson, MD, Dr. Wolkenstein Juha Peltonen, MD, PhD, Andrew Rosenberg, MD, Steven L. Carroll, MD, PhD, Sharad K. Verma, PhD, [email protected] Victor Mautner, MD, Meena Upadhyaya, PhD, and Anat Stemmer-Rachamimov, MD Neurology® 2018;91 (Suppl 1):S5-S13. doi:10.1212/WNL.0000000000005792 Abstract RELATED ARTICLES Objective Creating a comprehensive To present the current terminology and natural history of neurofibromatosis 1 (NF1) cuta- research strategy for neous neurofibromas (cNF). cutaneous neurofibromas Page S1 Methods NF1 experts from various research and clinical backgrounds reviewed the terms currently in use The biology of cutaneous fi for cNF as well as the clinical, histologic, and radiographic features of these tumors using neuro bromas: Consensus published and unpublished data. recommendations for setting research priorities Results Page S14 Neurofibromas develop within nerves, soft tissue, and skin. The primary distinction between fi fi Considerations for cNF and other neuro bromas is that cNF are limited to the skin whereas other neuro bromas development of therapies may involve the skin, but are not limited to the skin. There are important cellular, molecular, for cutaneous histologic, and clinical features of cNF. Each of these factors is discussed in consideration of neurofibroma a clinicopathologic framework for cNF. Page S21 Conclusion Clinical trial design for The development of effective therapies for cNF requires formulation of diagnostic criteria that cutaneous neurofibromas encompass the clinical and histologic features of these tumors. -

Imaging Findings of Extraventricular Choroid Plexus Papillomas: a Study of 10 Cases
ONCOLOGY LETTERS 13: 1479-1485, 2017 Imaging findings of extraventricular choroid plexus papillomas: A study of 10 cases YUZHEN SHI1*, XIAOSHUANG LI2,3*, XIAO CHEN2, YIMING XU1, GENJI BO1, HAO ZHOU2, YONGKANG LIU2, GUOXING ZHOU4 and ZHONGQIU WANG2 1Department of Medical Imaging, Huai'an First People's Hospital, Nanjing Medical University, Huai'an, Jiangsu 223300; 2Department of Radiology, Affiliated Hospital of Nanjing University of Chinese Medicine, Nanjing, Jiangsu 210029; 3Department of Medical Imaging, Bengbu Medical College, Bengbu, Anhui 233030; 4Department of Radiology, East Hospital, Tongji University School of Medicine, Shanghai 200120, P.R. China Received June 9, 2015; Accepted December 12, 2016 DOI: 10.3892/ol.2016.5552 Abstract. Extraventricular choroid plexus papillomas (CPPs) conclusion, in addition to the typical imaging findings, atypical are rare. In this study, we reveal the imaging findings of CPPs imaging findings, including atypical contours, abnormal signal located in extraventricular sites. The imaging findings of intensity, low enhancement and absence of hydrocephalus were 11 masses [10 masses on magnetic resonance imaging (MRI) also observed in extraventricular CPPs. and one mass on computed tomography (CT)] of extraventric- ular CPP in 10 patients were retrospectively observed. The mass Introduction site, size, contour, signal intensity, cystic or solid appearance, calcification, capsules, degree and pattern of enhancement, Choroid plexus papillomas (CPPs) are rare, histologically and hydrocephalus were evaluated based on CT or MRI. The benign [World Health Organization (WHO) grade I] intra- misdiagnosis rate of CPPs in extraventricular sites was 80.0% cranial neoplasms arising from the choroid epithelium. They (8/10). Solitary masses and multiple masses were observed in represent 0.4‑0.6% of all primary intracranial tumors and nine patients (90.0%, 9/10) and one patient (10%, 1/10), respec- account for 1.5‑4% of pediatric brain tumors (1,2). -

Lhermitte-Duclos Disease Associated with Cowden's Disease
Lhermitte-Duclos Disease Associated with Cowden's Disease Case Report—— Hiroshi YUASA, Takashi MOTOKISHITA, Sumitaka TOKITO, Masayoshi TOKUNAGA*, and Masamichi GOTO** Departments of Neurosurgery and *Pathology, Kagoshima City Hospital, Kagoshima; **2nd Department of Pathology , Kagoshima University School of Medicine, Kagoshima Abstract A 49-year-old Japanese male with Lhermitte-Duclos disease subsequently developed a very rare associa tion with Cowden's disease. Partial tumor removal established the diagnosis of Lhermitte-Duclos dis ease. Follow-up examinations discovered the presence of Cowden's disease. Long-term follow-up of patients with Lhermitte-Duclos disease is essential to identify signs of Cowden's disease, which carries the risk of developing malignancy. Key words: Lhermitte-Duclos disease, cerebellar tumor, magnetic resonance imaging, polyposis , Cowden's disease Introduction examination found his head circumference was large, measuring 61 cm. Neurological examination Lhermitte-Duclos disease is a rare disorder of the demonstrated intention tremor, adiadochokinesis, cerebellum characterized by enlarged cerebellar fo and unskillful finger-nose test on the right side. Com lia containing abnormal ganglion cells, first de puted tomography (CT) of the head revealed moder scribed in 1920.10) It usually presents as a cerebellar ate ventriculomegaly and a low density mass in the mass lesion with headaches, ataxia, and visual dis vermis and the right cerebellar hemisphere, which turbances. Cowden's disease was first described in was not enhanced following intravenous administra 1963.11) It is transmitted in an autosomal dominant tion of contrast medium (Fig. 1). The tumor was par pattern and is characterized by multiple hamartoma tially removed on November 16, 1983. -

Neurofibromatosis Type 1 (Nf1) a Guide for Adults and Families
1 NEUROFIBROMATOSIS TYPE 1 (NF1) A GUIDE FOR ADULTS AND FAMILIES Introduction Neurofibromatosis (NF) is a collective name for a group of genetic conditions that affect the nervous system. NF causes benign (non cancerous) lumps to grow on nerves. These lumps can grow on nerve endings in the skin where they can be seen clearly; the lumps can also grow on deeper nerves within the body. Neurofibromatosis occurs all over the world in all races. It affects men and women equally. There are two main types of Neurofibromatosis: Neurofibromatosis type 1 (NF1) and Neurofibromatosis type 2 (NF2). They are two completely different and separate conditions. People who have NF will have one type or the other. NF1 cannot change into NF2. THIS INFORMATION IS ABOUT NF1 ONLY NEUROFIBROMATOSIS TYPE 1 (NF1) is a common genetic condition. A genetic condition is one that can be passed on in families. Approximately 1 in every 2,500/3000 people is born with NF1. In the UK, every day a child is born with NF1. There are about 25000 people in the UK with a diagnosis of NF1. NF1 varies widely in how it affects people. Many people with NF1 will be affected very mildly and may have nothing more than skin changes. A minority of people (about a third) who have NF1 will have health problems linked to the diagnosis at some time in their life. Some of these problems will be mild and easily treated, others will be more severe. 2 At present, doctors cannot predict who is going to develop health problems linked to having a diagnosis of NF1. -

Health Supervision for Children with Neurofibromatosis Joseph H
CLINICAL REPORT Guidance for the Clinician in Rendering Health Supervision for Children With Pediatric Care Neurofibromatosis Joseph H. Hersh, MD, and the Committee on Genetics ABSTRACT Neurofibromatosis 1 is a multisystem disorder that primarily involves the skin and nervous system. Its population prevalence is 1 in 3500. The condition usually is www.pediatrics.org/cgi/doi/10.1542/ peds.2007-3364 recognized in early childhood, when cutaneous manifestations are apparent. Al- though neurofibromatosis 1 is associated with marked clinical variability, most doi:10.1542/peds.2007-3364 affected children do well from the standpoint of their growth and development. All clinical reports from the American Academy of Pediatrics automatically expire Some features of neurofibromatosis 1 are present at birth, and others are age- 5 years after publication unless reaffirmed, related abnormalities of tissue proliferation, which necessitate periodic monitoring revised, or retired at or before that time. to address ongoing health and developmental needs and to minimize the risk of Key Words serious medical complications. This clinical report provides a review of the clinical neurofibromatosis, neurofibromatosis 1, criteria needed to establish a diagnosis, the inheritance pattern of neurofibroma- cafe-au-lait spots, neurofibroma, optic glioma tosis 1, its major clinical and developmental manifestations, and guidelines for Abbreviations monitoring and providing intervention to maximize the growth, development, NF1—neurofibromatosis type 1 and health of an affected child. NF2—neurofibromatosis type 2 NIH—National Institutes of Health CLS—cafe-au-lait spot UBO—unidentified bright object INTRODUCTION PEDIATRICS (ISSN Numbers: Print, 0031-4005; Online, 1098-4275). Copyright © 2008 by the This clinical report was designed to assist the pediatrician in caring for the child in American Academy of Pediatrics whom the diagnosis of neurofibromatosis has been made. -

Neurofibromatosis Type 1
Handbook of Clinical Neurology, Vol. 132 (3rd series) Neurocutaneous Syndromes M.P. Islam and E.S. Roach, Editors © 2015 Elsevier B.V. All rights reserved Chapter 4 Neurofibromatosis type 1 JACQUELINE L. ANDERSON AND DAVID H. GUTMANN* Department of Neurology, Washington University School of Medicine, St. Louis, MO, USA INTRODUCTION background (Huson et al., 1989; Rasmussen and Friedman, 2000; Johnson et al., 2013). While NF1 is an History autosomal dominant condition, only 50% of people have Neurofibromatosis type 1 (NF1), previously known as an affected family member with NF1 (familial cases). As von Recklinghausen disease, is a common neurogenetic such, 50% of patients will be the first person in their fam- condition affecting 1:2500 people worldwide. NF1 prob- ily with NF1, arising from a sporadic NF1 gene mutation ably existed in ancient times, with art and literature from (De Luca et al., 2004; Evans et al., 2010). Life expectancy the 3rd century BCE documenting descriptions consistent is reduced by 8–15 years relative to the general popula- with the disease (Zanca, 1980). In 1849, an Irish surgeon tion, with malignancy constituting the major reason named Robert W. Smith differentiated patients with for death prior to the age of 30 (Rasmussen et al., traumatic neuromas from those with cases of multiple, 2001; Evans et al., 2011). With the establishment of an idiopathic neuromas (Smith, 1849). However, it was not online worldwide registry for patients with NF1, new until 1882 that the disease entity was fully recognized: the insights into the epidemiology of this common condition German pathologist Frederick von Recklinghausen first will likely emerge (Johnson et al., 2013). -

Current Understanding of Neurofibromatosis Type 1, 2, And
International Journal of Molecular Sciences Review Current Understanding of Neurofibromatosis Type 1, 2, and Schwannomatosis Ryota Tamura Department of Neurosurgery, Kawasaki Municipal Hospital, Shinkawadori, Kanagawa, Kawasaki-ku 210-0013, Japan; [email protected] Abstract: Neurofibromatosis (NF) is a neurocutaneous syndrome characterized by the development of tumors of the central or peripheral nervous system including the brain, spinal cord, organs, skin, and bones. There are three types of NF: NF1 accounting for 96% of all cases, NF2 in 3%, and schwannomatosis (SWN) in <1%. The NF1 gene is located on chromosome 17q11.2, which encodes for a tumor suppressor protein, neurofibromin, that functions as a negative regulator of Ras/MAPK and PI3K/mTOR signaling pathways. The NF2 gene is identified on chromosome 22q12, which encodes for merlin, a tumor suppressor protein related to ezrin-radixin-moesin that modulates the activity of PI3K/AKT, Raf/MEK/ERK, and mTOR signaling pathways. In contrast, molecular insights on the different forms of SWN remain unclear. Inactivating mutations in the tumor suppressor genes SMARCB1 and LZTR1 are considered responsible for a majority of cases. Recently, treatment strategies to target specific genetic or molecular events involved in their tumorigenesis are developed. This study discusses molecular pathways and related targeted therapies for NF1, NF2, and SWN and reviews recent clinical trials which involve NF patients. Keywords: neurofibromatosis type 1; neurofibromatosis type 2; schwannomatosis; molecular tar- geted therapy; clinical trial Citation: Tamura, R. Current Understanding of Neurofibromatosis Int. Type 1, 2, and Schwannomatosis. 1. Introduction J. Mol. Sci. 2021, 22, 5850. https:// doi.org/10.3390/ijms22115850 Neurofibromatosis (NF) is a genetic disorder that causes multiple tumors on nerve tissues, including brain, spinal cord, and peripheral nerves [1–3]. -

The Pathogenesis of Neurofibromatosis 1 and Neurofibromatosis 2
Chapter_3_p23-42 10/11/04 5:55 PM Page 23 3 The Pathogenesis of Neurofibromatosis 1 and Neurofibromatosis 2 The neurofibromatoses are genetic disorders. NF1 and NF2 are each caused by a mutation in a known specific gene. The quest to understand how these disorders originate and progress (their pathogenesis) received a significant boost when researchers identified the causative genes. The leading theories about the pathogenesis of NF1 and NF2 are discussed in this chapter. Because the search for the biological cause of schwanno- matosis was still underway when this book went to press, less is known about its pathogenesis (see Chapter 12). N A Search for Answers In 1990, two groups of scientists working separately located the NF1 gene on chromosome 17 and characterized its protein product, neurofi- bromin.1–3 In 1993, another two teams working separately identified the NF2 gene on chromosome 22; one named its protein “merlin”4 and the other “schwannomin.”5 Once the genes were identified, work could begin on better understanding how mutations lead to tumor formation and other manifestations. The search for answers, however, has been daunting. There is proba- bly no single answer to the question, What causes NF1 and NF2? Just as 23 Chapter_3_p23-42 10/11/04 5:55 PM Page 24 24 Neurofibromatosis these disorders cause various types of manifestations, so too there appear to be multiple molecular mechanisms at work. When trying to understand the pathogenesis of a disorder, scientists may combine two techniques that approach the question from different directions. The traditional phenotypical approaches analyze the physical manifestations of the disorders, such as what cells are involved and how they function, and then work backward to determine what gene might cause these abnormalities.