NF1 with Malignant Transformation of a Neurofibroma
Total Page:16
File Type:pdf, Size:1020Kb

Load more
Recommended publications
-

Neurofibromatosis Type 2 (NF2)
International Journal of Molecular Sciences Review Neurofibromatosis Type 2 (NF2) and the Implications for Vestibular Schwannoma and Meningioma Pathogenesis Suha Bachir 1,† , Sanjit Shah 2,† , Scott Shapiro 3,†, Abigail Koehler 4, Abdelkader Mahammedi 5 , Ravi N. Samy 3, Mario Zuccarello 2, Elizabeth Schorry 1 and Soma Sengupta 4,* 1 Department of Genetics, Cincinnati Children’s Hospital, Cincinnati, OH 45229, USA; [email protected] (S.B.); [email protected] (E.S.) 2 Department of Neurosurgery, University of Cincinnati, Cincinnati, OH 45267, USA; [email protected] (S.S.); [email protected] (M.Z.) 3 Department of Otolaryngology, University of Cincinnati, Cincinnati, OH 45267, USA; [email protected] (S.S.); [email protected] (R.N.S.) 4 Department of Neurology, University of Cincinnati, Cincinnati, OH 45267, USA; [email protected] 5 Department of Radiology, University of Cincinnati, Cincinnati, OH 45267, USA; [email protected] * Correspondence: [email protected] † These authors contributed equally. Abstract: Patients diagnosed with neurofibromatosis type 2 (NF2) are extremely likely to develop meningiomas, in addition to vestibular schwannomas. Meningiomas are a common primary brain tumor; many NF2 patients suffer from multiple meningiomas. In NF2, patients have mutations in the NF2 gene, specifically with loss of function in a tumor-suppressor protein that has a number of synonymous names, including: Merlin, Neurofibromin 2, and schwannomin. Merlin is a 70 kDa protein that has 10 different isoforms. The Hippo Tumor Suppressor pathway is regulated upstream by Merlin. This pathway is critical in regulating cell proliferation and apoptosis, characteristics that are important for tumor progression. -

Malignant Peripheral Nerve Sheath Tumor (MPNST): an Overview with Emphasis on Pathology, Imaging and Management Strategies
Thomas Jefferson University Jefferson Digital Commons Department of Neurosurgery Faculty Papers Department of Neurosurgery 6-2012 Malignant Peripheral Nerve Sheath Tumor (MPNST): An overview with emphasis on pathology, imaging and management strategies Timothy C. Beer 3rd year medical student, Jefferson Medical College Follow this and additional works at: https://jdc.jefferson.edu/neurosurgeryfp Part of the Medical Neurobiology Commons Let us know how access to this document benefits ouy Recommended Citation Beer, Timothy C., "Malignant Peripheral Nerve Sheath Tumor (MPNST): An overview with emphasis on pathology, imaging and management strategies" (2012). Department of Neurosurgery Faculty Papers. Paper 18. https://jdc.jefferson.edu/neurosurgeryfp/18 This Article is brought to you for free and open access by the Jefferson Digital Commons. The Jefferson Digital Commons is a service of Thomas Jefferson University's Center for Teaching and Learning (CTL). The Commons is a showcase for Jefferson books and journals, peer-reviewed scholarly publications, unique historical collections from the University archives, and teaching tools. The Jefferson Digital Commons allows researchers and interested readers anywhere in the world to learn about and keep up to date with Jefferson scholarship. This article has been accepted for inclusion in Department of Neurosurgery Faculty Papers by an authorized administrator of the Jefferson Digital Commons. For more information, please contact: [email protected]. An overview with emphasis -

The Interactions of DNA Repair, Telomere Homeostasis, and P53 Mutational Status in Solid Cancers: Risk, Prognosis, and Prediction
cancers Review The Interactions of DNA Repair, Telomere Homeostasis, and p53 Mutational Status in Solid Cancers: Risk, Prognosis, and Prediction Pavel Vodicka 1,2,3, Ladislav Andera 4,5, Alena Opattova 1,2,3,† and Ludmila Vodickova 1,2,3,*,† 1 Institute of Experimental Medicine, AS CR, 142 20 Prague, Czech Republic; [email protected] (P.V.); [email protected] (A.O.) 2 First Medical Faculty, Charles University, 121 08 Prague, Czech Republic 3 Biomedical Center, Faculty of Medicine in Pilsen, Charles University, 301 00 Pilsen, Czech Republic 4 Institute of Biotechnology, AS CR, 252 50 Vestec, Czech Republic; [email protected] 5 Institute of Molecular Genetics, AS CR, 142 20 Prague, Czech Republic * Correspondence: [email protected] † These authors contribured eaqually to this paper. Simple Summary: p53 is a nuclear transcription factor with a pro-apoptotic function. Somatic mutations in this gene represent one of the most critical events in human carcinogenesis. The disruption of genomic integrity due to the accumulation of various kinds of DNA damage, deficient DNA repair capacity, and alteration of telomere homeostasis constitute the hallmarks of malignant diseases. The main aim of our review was to accentuate a complex comprehension of the interactions between fundamental players in carcinogenesis of solid malignancies such as DNA damage response, telomere homeostasis and TP53. Abstract: The disruption of genomic integrity due to the accumulation of various kinds of DNA Citation: Vodicka, P.; Andera, L.; Opattova, A.; Vodickova, L. The damage, deficient DNA repair capacity, and telomere shortening constitute the hallmarks of malig- Interactions of DNA Repair, Telomere nant diseases. -

Information About Mosaic Neurofibromatosis Type 2 (NF2)
Information about mosaic Neurofibromatosis type 2 (NF2) NF2 occurs because of a mutation (change) in the NF2 gene. When this change is present at the time of conception the changed gene will be present in all the cells of the baby. When this mutation occurs later in the development of the forming embryo, the baby will go on to have a mix of cells: some with the “normal” genetic information and some with the changed information. This mix of cells is called mosaicism. Approximately half the people who have a diagnosis of NF2 have inherited the misprinted NF2 gene change from their mother or father who will also have NF2. They will have that misprinted gene in all the cells of their body. When they have their children, there will be a 1 in 2 chance of passing on NF2 to each child they have. However about half of people with NF2 are the first person in the family to be affected. They have no family history and have not inherited the condition from a parent. When doctors studied this group of patients more closely they noticed certain characteristics. Significantly they observed that fewer children had inherited NF2 than expected some people in this group had relatively mild NF2 NF2 tumours in some patients tended to grow on one side of their body rather than both sides that when a blood sample was tested to identify the NF2 gene, the gene change could not be found in 30-40% of people This lead researchers to conclude that this group of people were most likely to be mosaic for NF2 i.e. -

Network Scan Data
CTEP Protocol No: T-99-0090 CC Protocol No: 01-C-0222 Amendment: J Revised: 4/21/09 IRB Approval Date: A Phase II Randomized, Cross-Over, Double-Blinded, Placebo-Controlled Trial of the Farnesyltransferase Inhibitor R115777 in Pediatric Patients with Neurofibromatosis Type 1 and Progressive Plexiform Neurofibromas Coordinating Center: Pediatric Oncology Branch, NCI Principal Investigator: Brigitte Widemann, M.D.* (POB, NCI) NIH Associate Investigators: Frank M. Balis, M.D. (POB, NCI) Beth Fox, M.D. (POB, NCI) Kathy Warren, M.D. (NOB, NCI) Andy Gillespie, R.N. (ND, CC) Eva Dombi, MD (POB, NCI)** Nalini Jayaprakash, (POB, NCI) Diane Cole, (POB, NCI) Seth Steinberg, Ph.D. (BDMB, DCS, NCI) Nicholas Patronas, M.D. (DR, CC)** Maria Tsokos, M.D., (Laboratory of Pathology, NCI)** Pamela Wolters, Ph.D. (HAMB, NCI) Staci Martin, Ph.D. (HAMB, NCI) Jeffrey Solomon, (NIH and Sensor Systems, Inc.) Non-NIH Associate Investigators: Wanda Salzer, M.D. ** Keesler Air Force Base, Biloxi, Mississippi) 81st MDOS/SGOC 301 Fisher Street, Room 1A132 Keesler AFB, MS 39534-2519 Phone: 228-377-6524 E-mail: [email protected] Bruce R. Korf, M.D., Ph.D. ** Chair, Department of Genetics Univeristy of Alabama at Birmingham 1530 3rd Ave. S. Birmingham, AL 35294 Phone: (205)-934-9411, Fax: (205)-934-9488 E-mail: [email protected] David H. Gutmann, M.D., Ph.D. ** Department of Neurology Washington University School of Medicine St. Louis Children’s Hospital Box 8111, 660 S. Euclid Avenue St. Louis, MO 63110 Phone: (314)-632-7149, Fax: (314)-362-9462 E-mail: [email protected] 1 4/21/2009 T-99-0090, 01-C-0222 Arie Perry, M.D. -

Central Nervous System Tumors General ~1% of Tumors in Adults, but ~25% of Malignancies in Children (Only 2Nd to Leukemia)
Last updated: 3/4/2021 Prepared by Kurt Schaberg Central Nervous System Tumors General ~1% of tumors in adults, but ~25% of malignancies in children (only 2nd to leukemia). Significant increase in incidence in primary brain tumors in elderly. Metastases to the brain far outnumber primary CNS tumors→ multiple cerebral tumors. One can develop a very good DDX by just location, age, and imaging. Differential Diagnosis by clinical information: Location Pediatric/Young Adult Older Adult Cerebral/ Ganglioglioma, DNET, PXA, Glioblastoma Multiforme (GBM) Supratentorial Ependymoma, AT/RT Infiltrating Astrocytoma (grades II-III), CNS Embryonal Neoplasms Oligodendroglioma, Metastases, Lymphoma, Infection Cerebellar/ PA, Medulloblastoma, Ependymoma, Metastases, Hemangioblastoma, Infratentorial/ Choroid plexus papilloma, AT/RT Choroid plexus papilloma, Subependymoma Fourth ventricle Brainstem PA, DMG Astrocytoma, Glioblastoma, DMG, Metastases Spinal cord Ependymoma, PA, DMG, MPE, Drop Ependymoma, Astrocytoma, DMG, MPE (filum), (intramedullary) metastases Paraganglioma (filum), Spinal cord Meningioma, Schwannoma, Schwannoma, Meningioma, (extramedullary) Metastases, Melanocytoma/melanoma Melanocytoma/melanoma, MPNST Spinal cord Bone tumor, Meningioma, Abscess, Herniated disk, Lymphoma, Abscess, (extradural) Vascular malformation, Metastases, Extra-axial/Dural/ Leukemia/lymphoma, Ewing Sarcoma, Meningioma, SFT, Metastases, Lymphoma, Leptomeningeal Rhabdomyosarcoma, Disseminated medulloblastoma, DLGNT, Sellar/infundibular Pituitary adenoma, Pituitary adenoma, -

Adrenal Neuroblastoma Mimicking Pheochromocytoma in an Adult With
Khalayleh et al. Int Arch Endocrinol Clin Res 2017, 3:008 Volume 3 | Issue 1 International Archives of Endocrinology Clinical Research Case Report : Open Access Adrenal Neuroblastoma Mimicking Pheochromocytoma in an Adult with Neurofibromatosis Type 1 Harbi Khalayleh1, Hilla Knobler2, Vitaly Medvedovsky2, Edit Feldberg3, Judith Diment3, Lena Pinkas4, Guennadi Kouniavsky1 and Taiba Zornitzki2* 1Department of Surgery, Hebrew University Medical School of Jerusalem, Israel 2Endocrinology, Diabetes and Metabolism Institute, Kaplan Medical Center, Hebrew University Medical School of Jerusalem, Israel 3Pathology Institute, Kaplan Medical Center, Israel 4Nuclear Medicine Institute, Kaplan Medical Center, Israel *Corresponding author: Taiba Zornitzki, MD, Endocrinology, Diabetes and Metabolism Institute, Kaplan Medical Center, Hebrew University Medical School of Jerusalem, Bilu 1, 76100 Rehovot, Israel, Tel: +972-894- 41315, Fax: +972-8 944-1912, E-mail: [email protected] Context 2. This is the first reported case of an adrenal neuroblastoma occurring in an adult patient with NF1 presenting as a large Neurofibromatosis type 1 (NF1) is a genetic disorder asso- adrenal mass with increased catecholamine levels mimicking ciated with an increased risk of malignant disorders. Adrenal a pheochromocytoma. neuroblastoma is considered an extremely rare tumor in adults and was not previously described in association with NF1. 3. This case demonstrates the clinical overlap between pheo- Case description: A 42-year-old normotensive woman with chromocytoma and neuroblastoma. typical signs of NF1 underwent evaluation for abdominal pain, Keywords and a large 14 × 10 × 16 cm left adrenal mass displacing the Adrenal neuroblastoma, Neurofibromatosis type 1, Pheo- spleen, pancreas and colon was found. An initial diagnosis of chromocytoma, Neural crest-derived tumors pheochromocytoma was done based on the known strong association between pheochromocytoma, NF1 and increased catecholamine levels. -

Cadmium Induced Cell Apoptosis, DNA Damage, De
Int. J. Med. Sci. 2013, Vol. 10 1485 Ivyspring International Publisher International Journal of Medical Sciences 2013; 10(11):1485-1496. doi: 10.7150/ijms.6308 Research Paper Cadmium Induced Cell Apoptosis, DNA Damage, De- creased DNA Repair Capacity, and Genomic Instability during Malignant Transformation of Human Bronchial Epithelial Cells Zhiheng Zhou1*, Caixia Wang2*, Haibai Liu1, Qinhai Huang1, Min Wang1 , Yixiong Lei1 1. School of public health, Guangzhou Medical University, Guangzhou 510182, People’s Republic of China 2. Department of internal medicine of Guangzhou First People’s Hospital affiliated to Guangzhou Medical University, Guangzhou 510180, People’s Republic of China * These authors contributed equally to this work. Corresponding author: Yixiong Lei, School of public health, Guangzhou Medical University, 195 Dongfengxi Road, Guangzhou 510182, People’s Republic of China. Fax: +86-20-81340196. E-mail: [email protected] © Ivyspring International Publisher. This is an open-access article distributed under the terms of the Creative Commons License (http://creativecommons.org/ licenses/by-nc-nd/3.0/). Reproduction is permitted for personal, noncommercial use, provided that the article is in whole, unmodified, and properly cited. Received: 2013.03.23; Accepted: 2013.08.12; Published: 2013.08.30 Abstract Cadmium and its compounds are well-known human carcinogens, but the mechanisms underlying the carcinogenesis are not entirely understood. Our study was designed to elucidate the mech- anisms of DNA damage in cadmium-induced malignant transformation of human bronchial epi- thelial cells. We analyzed cell cycle, apoptosis, DNA damage, gene expression, genomic instability, and the sequence of exons in DNA repair genes in several kinds of cells. -
A Case of Intramedullary Spinal Cord Astrocytoma Associated with Neurofibromatosis Type 1
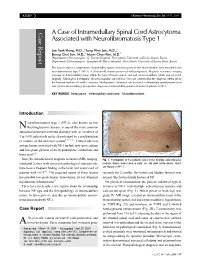
KISEP J Korean Neurosurg Soc 36 : 69-71, 2004 Case Report A Case of Intramedullary Spinal Cord Astrocytoma Associated with Neurofibromatosis Type 1 Jae Taek Hong, M.D.,1 Sang Won Lee, M.D.,1 Byung Chul Son, M.D.,1 Moon Chan Kim, M.D.2 Department of Neurosurgery,1 St. Vincent Hospital, The Catholic University of Korea, Suwon, Korea Department of Neurosurgery,2 Kangnam St. Mary's Hospital, The Catholic University of Korea, Seoul, Korea The authors report a symptomatic intramedullary spinal cord astrocytoma in the thoracolumbar area associated with neurofibromatosis type 1 (NF-1). A 38-year-old woman presented with paraparesis. Magnetic resonance imaging revealed an intramedullary lesion within the lower thoracic spinal cord and conus medullaris, which was removed surgically. Pathological investigation showed anaplastic astrocytoma. This case confirms that the diagnosis criteria set by the National Institute of Health Consensus Development Conference can be useful to differentiate ependymoma from astrocytoma when making a preoperative diagnosis of intramedullary spinal cord tumor in patients of NF-1. KEY WORDS : Astrocytoma·Intramedullary cord tumor·Neurofibromatosis. Introduction eurofibromatosis type 1 (NF-1), also known as von N Recklinghausen's disease, is one of the most common autosomal dominant inherited disorders with an incidence of 1 in 3,000 individuals and is characterized by a predisposition to tumors of the nervous system5,6,12,16). Central nervous system lesions associated with NF-1 include optic nerve glioma and low-grade gliomas of the hypothalamus, cerebellum and brain stem6,10). Since the introduction of magnetic resonance(MR) imaging, Fig. 1. Photograph of the patient's back shows multiple subcutaneous incidental lesions with uncertain pathological characteristic nodules (black arrow) and a cafe-au-lait spot (white arrow), which have been a frequent finding in the brain and spinal cord of are typical of NF-1. -

Depo-Provera
PRODUCT MONOGRAPH INCLUDING PATIENT MEDICATION INFORMATION PR ® DEPO-PROVERA medroxyprogesterone acetate injectable suspension, USP Sterile Aqueous Suspension 50 mg/mL and 150 mg/mL Progestogen Pfizer Canada Inc. Date of Revision: 17,300 Trans-Canada Highway February 13, 2018 Kirkland, Quebec H9J 2M5 Submission Control No: 210121 ® Pharmacia & Upjohn Company LLC Pfizer Canada Inc., Licensee © Pfizer Canada Inc., 2018 Table of Contents PART I: HEALTH PROFESSIONAL INFORMATION......................................................... 3 SUMMARY PRODUCT INFORMATION ........................................................................ 3 INDICATIONS AND CLINICAL USE .............................................................................. 3 CONTRAINDICATIONS ................................................................................................... 4 WARNINGS AND PRECAUTIONS: ................................................................................ 5 ADVERSE REACTIONS ................................................................................................. 18 DRUG INTERACTIONS .................................................................................................. 27 DOSAGE AND ADMINISTRATION .............................................................................. 28 OVERDOSAGE ................................................................................................................ 30 ACTION AND CLINICAL PHARMACOLOGY ............................................................ 30 STORAGE AND -

Herpes Simplex Virus Type 2: Bystander Or Active Player in Cervical Carcinogenesis?
Journal of Gynecology and Women’s Health ISSN 2474-7602 Mini Review J Gynecol Women’s Health Volume 12 Issue 2 - October 2018 Copyright © All rights are reserved by Jude Ogechukwu Okoye DOI: 10.19080/JGWH.2018.12.555832 Herpes Simplex Virus Type 2: Bystander or Active Player in Cervical Carcinogenesis? Jude Ogechukwu Okoye* Department of Medical Laboratory Science, Babcock University, Nigeria Submission: September 19, 2018 ; Published: October 05, 2018 *Corresponding author: Jude Ogechukwu Okoye, Department of Medical Laboratory Science, Babcock University, Nigeria, Tel: ; Email: Abstract More emphasis have been placed on producing vaccines that prevent host cell entry by Human Papillomavirus (HPV) while less attention andhas beenits potential given to to Herpes up-modulate Simplex both virus HPV type regulatory 2 (HSV-2) andwhich oncogenic potentially gene promotes and downregulate acquisition hostand co-habitationtumour suppressor of human suggest immunodeficiency that it is not a virus (HIV), HPV and Epstein-Barr virus (EBV). The tendency for HSV-2 to induce ulcerations and chronic inflammation following reactivation, to reduce cervical cancer related mortality. bystander in cervical carcinogenesis. Thus, efforts geared towards finding HSV-2 effective microbicide and vaccine should be intensified so as Keywords: Herpes Simplex virus type 2; Human papillomavirus; Epstein-Barr virus; Cervical cancer Abbreviations: HPV: Human Papillomavirus; HIV: Human Immune virus; SSC: Squamous Cell Carcinoma; LMP1: Latent Membrane Protein 1; EBV: Epstein-Barr virus; CIN: Cervical Intraepithelial Neoplasia Introduction Cervical cancer is the second most common type of cancer in a woman’s lifetime and may also facilitate EBV infection, a (9.8%) affecting women worldwide [1-3]. -

UCSD Moores Cancer Center Neuro-Oncology Program
UCSD Moores Cancer Center Neuro-Oncology Program Recent Progress in Brain Tumors 6DQWRVK.HVDUL0'3K' 'LUHFWRU1HXUR2QFRORJ\ 3URIHVVRURI1HXURVFLHQFHV 0RRUHV&DQFHU&HQWHU 8QLYHUVLW\RI&DOLIRUQLD6DQ'LHJR “Brain Cancer for Life” Juvenile Pilocytic Astrocytoma Metastatic Brain Cancer Glioblastoma Multiforme Glioblastoma Multiforme Desmoplastic Infantile Ganglioglioma Desmoplastic Variant Astrocytoma Medulloblastoma Atypical Teratoid Rhabdoid Tumor Diffuse Intrinsic Pontine Glioma -Mutational analysis, microarray expression, epigenetic phenomenology -Age-specific biology of brain cancer -Is there an overlap? ? Neuroimmunology ? Stem cell hypothesis Courtesy of Dr. John Crawford Late Effects Long term effect of chemotherapy and radiation on neurocognition Risks of secondary malignancy secondary to chemotherapy and/or radiation Neurovascular long term effects: stroke, moya moya Courtesy of Dr. John Crawford Importance Increase in aging population with increased incidence of cancer Patients with cancer living longer and developing neurologic disorders due to nervous system relapse or toxicity from treatments Overview Introduction Clinical Presentation Primary Brain Tumors Metastatic Brain Tumors Leptomeningeal Metastases Primary CNS Lymphoma Paraneoplastic Syndromes Classification of Brain Tumors Tumors of Neuroepithelial Tissue Glial tumors (astrocytic, oligodendroglial, mixed) Neuronal and mixed neuronal-glial tumors Neuroblastic tumors Pineal parenchymal tumors Embryonal tumors Tumors of Peripheral Nerves Shwannoma Neurofibroma