Gastritis Important Information Regarding Your Health
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

IRRITABLE BOWEL SYNDROME by Michael Sperling MD
IRRITABLE BOWEL SYNDROME By Michael Sperling MD Irritable bowel syndrome (IBS) involves vague symptoms of abdominal pain, diarrhea, constipation, gas and bloating for which there is no understandable cause. Incredibly, IBS affects up to 20% of the population but only three- quarters of those people actually seek medical attention. It is the second most common reason for work absenteeism. Irritable bowel symptoms may also be related to other complaints such as belching, heartburn, swallowing problems, fullness after eating, nausea, frequent urination, painful menstruation and pain during intercourse. Extremely severe cases can sometimes be related to a history of traumatic abuse. Some common associations or factors: Michael Sperling, MD 1. ‘Spastic colon’ is frequently found along with irritable bowel syndrome. Spastic colon consists of painful muscle contractions which can be relieved by bulk agents or anti- spasm drugs. 2. Post-infectious IBS occurs when irritable bowel follows a gastrointestinal infection, such as the stomach flu. These recurrent symptoms can last up to two years. 3. Stress and anxiety can worsen IBS symptoms so occasionally anti-anxiety agents may be helpful. 4. Food intolerances classically worsen symptoms of irritable bowel in some people. Common “offending foods” include lactose, legumes (beans) and cruciferous vegetables like brussel sprouts, cauliflower, broccoli and cabbage. 5. Hypersensitivity of the bowel wall: Normal colon activity is not usually noticed however in “visceral hypersensitivity”, the bowel wall reacts painfully to normal activity. This condition may be helped by the use of low dose antidepressants, which can block these painful stimuli. Careful and selective testing of patients with these symptoms and the development of a long-term doctor/patient relationship is the key to diagnosing and managing these symptoms. -

Dyspepsia (Indigestion)
Indigestion (dydpepsia). Indigestion information - Patient | Patient Page 1 of 5 View this article online at https://patient.info/health/dyspepsia-indigestion Dyspepsia (Indigestion) Dyspepsia (indigestion) is a term which describes pain and sometimes other symptoms which come from your upper gut (the stomach, oesophagus or duodenum). There are various causes (described below). Treatment depends on the likely cause. Understanding digestion Food passes down the gullet (oesophagus) into the stomach. The stomach makes acid which is not essential but helps to digest food. Food then passes gradually into the first part of the small intestine (the duodenum). In the duodenum and the rest of the small intestine, food mixes with chemicals called enzymes. The enzymes come from the pancreas and from cells lining the intestine. The enzymes break down (digest) the food. Digested food is then absorbed into the body from the small intestine. What is dyspepsia? Dyspepsia is a term which includes a group of symptoms that come from a problem in your upper gut. The gut (gastrointestinal tract) is the tube that starts at the mouth and ends at the anus. The upper gut includes the oesophagus, stomach and duodenum. Various conditions cause dyspepsia. The main symptom is usually pain or discomfort in the upper tummy (abdomen). In addition, other symptoms that may develop include: • Bloating. • Belching. • Quickly feeling full after eating. • Feeling sick (nausea). • Being sick (vomiting). Symptoms are often related to eating. Doctors used to include heartburn (a burning sensation felt in the lower chest area) and bitter-tasting liquid coming up into the back of the throat (sometimes called 'waterbrash') as symptoms of dyspepsia. -

Stomach Flu (Viral Gastroenteritis)
Stomach Flu (Viral Gastroenteritis) The stomach flu (also called viral gastroenteritis) is caused by a virus (rotavirus, adenovirus, Norwalk virus to name a few) that affect the stomach and small intestines. It may come on suddenly or over the course of a few hours. The illness is usually brief, lasting 24-72 hours. Symptoms include: Nausea Vomiting Stomach cramps Diarrhea Mild fever Fatigue Body Chills/Sweats Loss of appetite Muscle aches To help take care of yourself: • The best thing to do is to let your stomach rest from solid foods. • Sip on clear liquids (Hi-C, apple, cranberry, and grape juices, Jell-O, Gatorade- type liquids and ginger-ale or ginger tea). There are special properties in ginger that help soothe the stomach. It is extremely important to keep up your hydration. Water is great for hydration but Gatorade-type products are better because they will restore your electrolytes (Sodium, Potassium and Chloride) which are essential for body functions. You may "stir" the bubbles out of the soda if the carbonation is harsh on your stomach. • Once you have not vomited for a few hours and your stomach is feeling better, you may start to eat solid foods. You may try crackers, plain noodles, eggs, broth, pretzels and yogurt. • The BRAT diet (Bananas, Rice, Applesauce & Toast) includes foods that are low in fiber and are easily digested. • Stay away from dairy products, citric (including orange and grapefruit juices), tomato-based & spicy foods. • SLOWLY increase your dietary intake to include fruits, vegetables and meat once symptoms are gone (usually over 2-3 days). -

Abdominal Pain - Gastroesophageal Reflux Disease
ACS/ASE Medical Student Core Curriculum Abdominal Pain - Gastroesophageal Reflux Disease ABDOMINAL PAIN - GASTROESOPHAGEAL REFLUX DISEASE Epidemiology and Pathophysiology Gastroesophageal reflux disease (GERD) is one of the most commonly encountered benign foregut disorders. Approximately 20-40% of adults in the United States experience chronic GERD symptoms, and these rates are rising rapidly. GERD is the most common gastrointestinal-related disorder that is managed in outpatient primary care clinics. GERD is defined as a condition which develops when stomach contents reflux into the esophagus causing bothersome symptoms and/or complications. Mechanical failure of the antireflux mechanism is considered the cause of GERD. Mechanical failure can be secondary to functional defects of the lower esophageal sphincter or anatomic defects that result from a hiatal or paraesophageal hernia. These defects can include widening of the diaphragmatic hiatus, disturbance of the angle of His, loss of the gastroesophageal flap valve, displacement of lower esophageal sphincter into the chest, and/or failure of the phrenoesophageal membrane. Symptoms, however, can be accentuated by a variety of factors including dietary habits, eating behaviors, obesity, pregnancy, medications, delayed gastric emptying, altered esophageal mucosal resistance, and/or impaired esophageal clearance. Signs and Symptoms Typical GERD symptoms include heartburn, regurgitation, dysphagia, excessive eructation, and epigastric pain. Patients can also present with extra-esophageal symptoms including cough, hoarse voice, sore throat, and/or globus. GERD can present with a wide spectrum of disease severity ranging from mild, intermittent symptoms to severe, daily symptoms with associated esophageal and/or airway damage. For example, severe GERD can contribute to shortness of breath, worsening asthma, and/or recurrent aspiration pneumonia. -

Appendicitis
Appendicitis Your child has abdominal pain, it might be appendicitis. Appendicitis is swelling or infection in the appendix. The appendix is a small organ attached to the large intestine. Appendicitis usually develops over 12-24 hours. It has symptoms such as abdominal pain, nausea, vomiting, fever, and loss of appetite. Most importantly, pain that continues, worsens and moves to the right lower side of the abdomen is common in appendicitis. Appendicitis is the most common childhood “emergency” that must be treated in a timely manner. However, it’s important to know that many conditions have symptoms similar to appendicitis but don’t require surgery. At Hasbro Children’s Hospital (HCH), we evaluate your child’s abdominal pain to determine if appendicitis is the cause. That way, we avoid unnecessary operations. What happens now? Your child will be well cared for. First your child will be seen in the HCH emergency department (ED) by a nurse and doctor trained in pediatric emergency medicine. If necessary, your child will have tests that include blood work and a urinalysis. Your child’s pain will be managed with intravenous (IV) pain medication. Your child will not be allowed to eat or drink and may receive fluids through an intravenous line. Members of the pediatric surgical team will examine your child to help determine whether your child has appendicitis or another condition. We will perform a painless ultrasound on your child and the ultrasound images will be read by pediatric radiology doctors with advanced training in imaging children. Usually, ultrasound is the only imaging required but sometimes an MRI may be needed as well. -

Gastritis - Symptoms and Causes - Mayo Clinic Visited 11/22/2019
Gastritis - Symptoms and causes - Mayo Clinic Visited 11/22/2019 Request an Appointment Find a Doctor MENU Find a Job Give Now Log in to Patient Account English Patient Care & Health Information Diseases & Conditions Request an Gastritis Appointment Symptoms & causes Diagnosis & treatment Doctors & departments Overview Print Advertisement Gastritis is a general term for a group Mayo Clinic does not endorse companies or of conditions with one thing in common: products. Advertising revenue supports our not- inflammation of the lining of the for-profit mission. stomach. The inflammation of gastritis Advertising & Sponsorship is most often the result of infection with Policy Opportunities Ad Choices the same bacterium that causes most stomach ulcers. Regular use of certain Stomach and pain relievers and drinking too much pyloric valve Mayo Clinic Marketplace alcohol also can contribute to gastritis. Check out these best-sellers and special offers on books and newsletters from Mayo Clinic. Gastritis may occur suddenly (acute gastritis), or appear slowly over time (chronic gastritis). In some cases, gastritis NEW – Guide to Fibromyalgia can lead to ulcers and an increased risk of stomach cancer. Instant access – Mayo Clinic Health Letter For most people, however, gastritis isn't serious and improves quickly with treatment. Diabetes? This diet works … Stop osteoporosis in its tracks The Mayo Clinic Diet Online Products & Services Book: Mayo Clinic on Digestive Health https://www.mayoclinic.org/diseases-conditions/gastritis/symptoms-causes/syc-20355807[11/22/2019 4:16:25 PM] Gastritis - Symptoms and causes - Mayo Clinic Visited 11/22/2019 Symptoms The signs and symptoms of gastritis include: Gnawing or burning ache or pain (indigestion) in your upper abdomen that may become either worse or better with eating Nausea Vomiting A feeling of fullness in your upper abdomen after eating Gastritis doesn't always cause signs and symptoms. -

Nausea and Vomiting (Stomach “Bug” Or Gastroenteritis)
Nausea and Vomiting •(Stomach Nausea and vomiting “Bug” is most commonly or caused Gastroenteritis) by a viral infection and may be associated with diarrhea. • This illness is self-limited with the majority of people finding improvement within 24-hours and are back to normal by 72-hours after onset of the illness. • This illness can be treated at home and does not require a visit to a medical provider. Symptoms: • Nausea with or without vomiting • Muscle aches • Generalized or upper abdominal pain/cramping • Headache • Watery diarrhea (no blood) • Possible fever Self-care measures: • Stop eating solid foods • Rest • Suck on ice chips or sip small amounts of water on a frequent basis • If you vomit, wait about 20 minutes then resume fluid intake • Slowly increase the amount of fluid intake • Water, Pedialyte® or sports drinks are acceptable • Avoid caffeine, alcohol and carbonated beverages • Acetaminophen (Tylenol®) 650 mg every 6 hours as needed for fever, chills, headache or body aches • Use Imodium for diarrhea lasting more than 2 days Recovery: • You may try solid food when: 1) Nausea and vomiting have resolved 2) You are tolerating fluids 3) You feel hungry When you do eat: • Start with small amounts of simple foods (crackers, toast, Jello®, etc.) • Over the next 24-36 hours slowly build up to your normal diet • Add dairy, high-fat foods, raw vegetables, citrus and red meat last Limit spread to others: • Wash hands with soap and water frequently • Stay home (or in your residence hall) for at least the first 24-hours • If you live in a residence hall call 540-568-6949 to get information about obtaining some appropriate food or fluids When to seek medical attention: • If the vomiting persists more than 24-hours • If you develop bloody diarrhea • If you have obvious pain or tenderness isolated to the right lower abdomen UHC self-care guidelines are based on the most recent recommendations of national medical authorities.. -

Gastroesophageal Reflux Disease (GERD)
Guidelines for Clinical Care Quality Department Ambulatory GERD Gastroesophageal Reflux Disease (GERD) Guideline Team Team Leader Patient population: Adults Joel J Heidelbaugh, MD Objective: To implement a cost-effective and evidence-based strategy for the diagnosis and Family Medicine treatment of gastroesophageal reflux disease (GERD). Team Members Key Points: R Van Harrison, PhD Diagnosis Learning Health Sciences Mark A McQuillan, MD History. If classic symptoms of heartburn and acid regurgitation dominate a patient’s history, then General Medicine they can help establish the diagnosis of GERD with sufficiently high specificity, although sensitivity Timothy T Nostrant, MD remains low compared to 24-hour pH monitoring. The presence of atypical symptoms (Table 1), Gastroenterology although common, cannot sufficiently support the clinical diagnosis of GERD [B*]. Testing. No gold standard exists for the diagnosis of GERD [A*]. Although 24-hour pH monitoring Initial Release is accepted as the standard with a sensitivity of 85% and specificity of 95%, false positives and false March 2002 negatives still exist [II B*]. Endoscopy lacks sensitivity in determining pathologic reflux but can Most Recent Major Update identify complications (eg, strictures, erosive esophagitis, Barrett’s esophagus) [I A]. Barium May 2012 radiography has limited usefulness in the diagnosis of GERD and is not recommended [III B*]. Content Reviewed Therapeutic trial. An empiric trial of anti-secretory therapy can identify patients with GERD who March 2018 lack alarm or warning symptoms (Table 2) [I A*] and may be helpful in the evaluation of those with atypical manifestations of GERD, specifically non-cardiac chest pain [II B*]. Treatment Ambulatory Clinical Lifestyle modifications. -
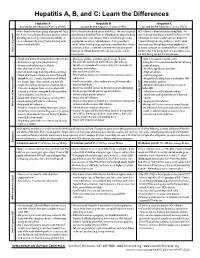
Hepatitis A, B, and C: Learn the Differences
Hepatitis A, B, and C: Learn the Differences Hepatitis A Hepatitis B Hepatitis C caused by the hepatitis A virus (HAV) caused by the hepatitis B virus (HBV) caused by the hepatitis C virus (HCV) HAV is found in the feces (poop) of people with hepa- HBV is found in blood and certain body fluids. The virus is spread HCV is found in blood and certain body fluids. The titis A and is usually spread by close personal contact when blood or body fluid from an infected person enters the body virus is spread when blood or body fluid from an HCV- (including sex or living in the same household). It of a person who is not immune. HBV is spread through having infected person enters another person’s body. HCV can also be spread by eating food or drinking water unprotected sex with an infected person, sharing needles or is spread through sharing needles or “works” when contaminated with HAV. “works” when shooting drugs, exposure to needlesticks or sharps shooting drugs, through exposure to needlesticks on the job, or from an infected mother to her baby during birth. or sharps on the job, or sometimes from an infected How is it spread? Exposure to infected blood in ANY situation can be a risk for mother to her baby during birth. It is possible to trans- transmission. mit HCV during sex, but it is not common. • People who wish to be protected from HAV infection • All infants, children, and teens ages 0 through 18 years There is no vaccine to prevent HCV. -

Travelers' Diarrhea
Travelers’ Diarrhea What is it and who gets it? Travelers’ diarrhea (TD) is the most common illness affecting travelers. Each year between 20%-50% of international travelers, an estimated 10 million persons, develop diarrhea. The onset of TD usually occurs within the first week of travel but may occur at any time while traveling and even after returning home. The primary source of infection is ingestion of fecally contaminated food or water. You can get TD whenever you travel from countries with a high level of hygiene to countries that have a low level of hygiene. Poor sanitation, the presence of stool in the environment, and the absence of safe restaurant practices lead to widespread risk of diarrhea from eating a wide variety of foods in restaurants, and elsewhere. Your destination is the most important determinant of risk. Developing countries in Latin America, Africa, the Middle East, and Asia are considered high risk. Most countries in Southern Europe and a few Caribbean islands are deemed intermediate risk. Low risk areas include the United States, Canada, Northern Europe, Australia, New Zealand, and several of the Caribbean islands. Anyone can get TD, but persons at particular high-risk include young adults , immunosuppressed persons, persons with inflammatory-bowel disease or diabetes, and persons taking H-2 blockers or antacids. Attack rates are similar for men and women. TD is caused by bacteria, protozoa or viruses that are ingested by eating contaminated food or beverages. For short-term travelers in most areas, bacteria are the cause of the majority of diarrhea episodes. What are common symptoms of travelers’ diarrhea? Most TD cases begin abruptly. -

Chapter 34 • Drugs Used to Treat Nausea and Vomiting
• Chapter 34 • Drugs Used to Treat Nausea and Vomiting • Learning Objectives • Compare the purposes of using antiemetic products • State the therapeutic classes of antiemetics • Discuss scheduling of antiemetics for maximum benefit • Nausea and Vomiting • Nausea : the sensation of abdominal discomfort that is intermittently accompanied by a desire to vomit • Vomiting (emesis): the forceful expulsion of gastric contents up the esophagus and out of the mouth • Regurgitation : the rising of gastric or esophageal contents to the pharynx as a result of stomach pressure • Common Causes of Nausea and Vomiting • Postoperative nausea and vomiting • Motion sickness • Pregnancy Hyperemesis gravidarum: a condition in pregnancy in which starvation, dehydration, and acidosis are superimposed on the vomiting syndrome • Common Causes of Nausea and Vomiting (cont’d) • Psychogenic vomiting: self-induced or involuntary vomiting in response to threatening or distasteful situations • Chemotherapy-induced emesis (CIE) Anticipatory nausea and vomiting: triggered by sight and smell associated with treatment Acute CIE: stimulated directly by chemotherapy 1 to 6 hours after treatment Delayed emesis: occurs 24 to 120 hours after treatment; may be induced by metabolic by-products of chemotherapy • Drug Therapy for Selected Causes of Nausea and Vomiting • Postoperative nausea and vomiting (PONV) • Antiemetics include: Dopamine antagonists Anticholinergic agents Serotonin antagonists H2 antagonists (cimetidine, ranitidine) • Nursing Process for Nausea and Vomiting -

In Patients with Crohn's Disease Gut: First Published As 10.1136/Gut.38.3.379 on 1 March 1996
Gut 1996; 38: 379-383 379 High frequency of helicobacter negative gastritis in patients with Crohn's disease Gut: first published as 10.1136/gut.38.3.379 on 1 March 1996. Downloaded from L Halme, P Karkkainen, H Rautelin, T U Kosunen, P Sipponen Abstract In a previous study we described upper gastro- The frequency of gastric Crohn's disease intestinal lesions characteristic of CD in 17% has been considered low. This study was of patients with ileocolonic manifestations of undertaken to determine the prevalence of the disease.10 Furthermore, 40% of these chronic gastritis and Helicobacter pylori patients had chronic, non-specific gastritis. infection in patients with Crohn's disease. This study aimed to determine the prevalence Oesophagogastroduodenoscopy was per- of chronic gastritis and that of H pylori infec- formed on 62 consecutive patients suffer- tion in patients with CD who had undergone ing from ileocolonic Crohn's disease. oesophagogastroduodenoscopy (OGDS) at the Biopsy specimens from the antrum and Fourth Department of Surgery, Helsinki corpus were processed for both histological University Hospital between 1989 and 1994. and bacteriological examinations. Hpylori antibodies of IgG and IgA classes were measured in serum samples by enzyme Patients and methods immunoassay. Six patients (9.70/o) were During a five year period from September 1989 infected with H pylorn, as shown by histo- to August 1994, OGDS was performed on 62 logy, and in five of them the infection consecutive patients with CD to establish the was also verified by serology. Twenty one distribution of their disease. During the study patients (32%) had chronic H pyloni period, the OGDS was repeated (one to seven negative gastritis (negative by both times) - on three patients because of anaemia histology and serology) and one of them and on five patients because of upper gastroin- also had atrophy in the antrum and corpus.