Hunter Et Al CLSPN
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Prevalence and Functional Analysis of Sequence Variants in the ATR Checkpoint Mediator Claspin
Published OnlineFirst September 8, 2009; DOI: 10.1158/1541-7786.MCR-09-0033 Prevalence and Functional Analysis of Sequence Variants in the ATR Checkpoint Mediator Claspin Jianmin Zhang,1 Young-Han Song,1 Brian W. Brannigan,1 Doke C.R. Wahrer,1 Taryn A. Schiripo,1 Patricia L. Harris,1 Sara M. Haserlat,1 Lindsey E. Ulkus,1 Kristen M. Shannon,1 Judy E. Garber,2 Matthew L. Freedman,3 Brian E. Henderson,4 Lee Zou,1 Dennis C. Sgroi,1 Daniel A. Haber,1 and Daphne W. Bell1 1Massachusetts General Hospital Cancer Center and Harvard Medical School, Charlestown, Massachusetts; 2Dana-Farber Cancer Institute and Harvard Medical School, Boston, Massachusetts; 3Department of Molecular Biology, Massachusetts General Hospital, Department of Genetics, Harvard Medical School, and Broad Institute for Biomedical Research, Boston, Massachusetts; and 4Department of Preventive Medicine, University of Southern California Keck School of Medicine, Los Angeles, California Abstract mutation, was defective in its ability to mediate CHK1 Mutational inactivation of genes controlling the phosphorylation followingDNA damageand was unable to DNA-damage response contributes to cancer susceptibility rescue sensitivity to replicative stress in CLSPN-depleted within families and within the general population as well as cells. Taken together, these observations raise the to sporadic tumorigenesis. Claspin (CLSPN) encodes a possibility that CLSPN may encode a component of the recently recognized mediator protein essential for the ATR DNA-damage response pathway that is targeted by and CHK1-dependent checkpoint elicited by replicative mutations in human cancers, suggesting the need for larger stress or the presence of ssDNA. Here, we describe a study population-based studies to investigate whether CLSPN to determine whether mutational disruption of CLSPN variants contribute to cancer susceptibility. -

ATR Pathway Inhibition Is Synthetically Lethal in Cancer Cells with ERCC1 Deficiency
Published OnlineFirst March 24, 2014; DOI: 10.1158/0008-5472.CAN-13-3229 Cancer Therapeutics, Targets, and Chemical Biology Research ATR Pathway Inhibition Is Synthetically Lethal in Cancer Cells with ERCC1 Deficiency Kareem N. Mohni, Gina M. Kavanaugh, and David Cortez Abstract The DNA damage response kinase ATR and its effector kinase CHEK1 are required for cancer cells to survive oncogene-induced replication stress. ATR inhibitors exhibit synthetic lethal interactions, with deficiencies in the DNA damage response enzymes ATM and XRCC1 and with overexpression of the cell cycle kinase cyclin E. Here, we report a systematic screen to identify synthetic lethal interactions with ATR pathway–targeted drugs, rationalized by their predicted therapeutic utility in the oncology clinic. We found that reduced function in the ATR pathway itself provided the strongest synthetic lethal interaction. In addition, we found that loss of the structure-specific endonuclease ERCC1-XPF (ERCC4) is synthetic lethal with ATR pathway inhibitors. ERCC1- deficient cells exhibited elevated levels of DNA damage, which was increased further by ATR inhibition. When treated with ATR or CHEK1 inhibitors, ERCC1-deficient cells were arrested in S-phase and failed to complete cell-cycle transit even after drug removal. Notably, triple-negative breast cancer cells and non–small cell lung cancer cells depleted of ERCC1 exhibited increased sensitivity to ATR pathway–targeted drugs. Overall, we concluded that ATR pathway–targeted drugs may offer particular utility in cancers with reduced ATR pathway function or reduced levels of ERCC4 activity. Cancer Res; 74(10); 1–11. Ó2014 AACR. Introduction repair pathway such as homologous recombination or post- – Replicating DNA is sensitive to a wide array of endogenous replicative repair to remove the PARP DNA complexes (7). -
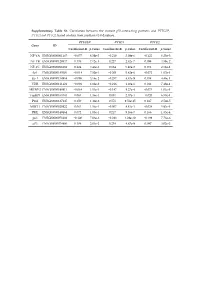
Supplementary Table S1. Correlation Between the Mutant P53-Interacting Partners and PTTG3P, PTTG1 and PTTG2, Based on Data from Starbase V3.0 Database
Supplementary Table S1. Correlation between the mutant p53-interacting partners and PTTG3P, PTTG1 and PTTG2, based on data from StarBase v3.0 database. PTTG3P PTTG1 PTTG2 Gene ID Coefficient-R p-value Coefficient-R p-value Coefficient-R p-value NF-YA ENSG00000001167 −0.077 8.59e-2 −0.210 2.09e-6 −0.122 6.23e-3 NF-YB ENSG00000120837 0.176 7.12e-5 0.227 2.82e-7 0.094 3.59e-2 NF-YC ENSG00000066136 0.124 5.45e-3 0.124 5.40e-3 0.051 2.51e-1 Sp1 ENSG00000185591 −0.014 7.50e-1 −0.201 5.82e-6 −0.072 1.07e-1 Ets-1 ENSG00000134954 −0.096 3.14e-2 −0.257 4.83e-9 0.034 4.46e-1 VDR ENSG00000111424 −0.091 4.10e-2 −0.216 1.03e-6 0.014 7.48e-1 SREBP-2 ENSG00000198911 −0.064 1.53e-1 −0.147 9.27e-4 −0.073 1.01e-1 TopBP1 ENSG00000163781 0.067 1.36e-1 0.051 2.57e-1 −0.020 6.57e-1 Pin1 ENSG00000127445 0.250 1.40e-8 0.571 9.56e-45 0.187 2.52e-5 MRE11 ENSG00000020922 0.063 1.56e-1 −0.007 8.81e-1 −0.024 5.93e-1 PML ENSG00000140464 0.072 1.05e-1 0.217 9.36e-7 0.166 1.85e-4 p63 ENSG00000073282 −0.120 7.04e-3 −0.283 1.08e-10 −0.198 7.71e-6 p73 ENSG00000078900 0.104 2.03e-2 0.258 4.67e-9 0.097 3.02e-2 Supplementary Table S2. -

Curcumin Alters Gene Expression-Associated DNA Damage, Cell Cycle, Cell Survival and Cell Migration and Invasion in NCI-H460 Human Lung Cancer Cells in Vitro
ONCOLOGY REPORTS 34: 1853-1874, 2015 Curcumin alters gene expression-associated DNA damage, cell cycle, cell survival and cell migration and invasion in NCI-H460 human lung cancer cells in vitro I-TSANG CHIANG1,2, WEI-SHU WANG3, HSIN-CHUNG LIU4, SU-TSO YANG5, NOU-YING TANG6 and JING-GUNG CHUNG4,7 1Department of Radiation Oncology, National Yang‑Ming University Hospital, Yilan 260; 2Department of Radiological Technology, Central Taiwan University of Science and Technology, Taichung 40601; 3Department of Internal Medicine, National Yang‑Ming University Hospital, Yilan 260; 4Department of Biological Science and Technology, China Medical University, Taichung 404; 5Department of Radiology, China Medical University Hospital, Taichung 404; 6Graduate Institute of Chinese Medicine, China Medical University, Taichung 404; 7Department of Biotechnology, Asia University, Taichung 404, Taiwan, R.O.C. Received March 31, 2015; Accepted June 26, 2015 DOI: 10.3892/or.2015.4159 Abstract. Lung cancer is the most common cause of cancer CARD6, ID1 and ID2 genes, associated with cell survival and mortality and new cases are on the increase worldwide. the BRMS1L, associated with cell migration and invasion. However, the treatment of lung cancer remains unsatisfactory. Additionally, 59 downregulated genes exhibited a >4-fold Curcumin has been shown to induce cell death in many human change, including the DDIT3 gene, associated with DNA cancer cells, including human lung cancer cells. However, the damage; while 97 genes had a >3- to 4-fold change including the effects of curcumin on genetic mechanisms associated with DDIT4 gene, associated with DNA damage; the CCPG1 gene, these actions remain unclear. Curcumin (2 µM) was added associated with cell cycle and 321 genes with a >2- to 3-fold to NCI-H460 human lung cancer cells and the cells were including the GADD45A and CGREF1 genes, associated with incubated for 24 h. -

Signature of Progression and Negative Outcome in Colorectal Cancer
Oncogene (2010) 29, 876–887 & 2010 Macmillan Publishers Limited All rights reserved 0950-9232/10 $32.00 www.nature.com/onc ORIGINAL ARTICLE A ‘DNA replication’ signature of progression and negative outcome in colorectal cancer M-J Pillaire1,7, J Selves2,7, K Gordien2, P-A Gouraud3, C Gentil3, M Danjoux2,CDo3, V Negre4, A Bieth1, R Guimbaud2, D Trouche5, P Pasero6,MMe´chali6, J-S Hoffmann1 and C Cazaux1 1Genetic Instability and Cancer Group, Department Biology of Cancer, Institute of Pharmacology and Structural Biology, UMR5089 CNRS, University of Toulouse, University Paul Sabatier, Toulouse, France; 2INSERM U563, Federation of Digestive Cancerology and Department of Anatomo-pathology, University of Toulouse, University Paul Sabatier, Toulouse, France; 3Service of Epidemiology, INSERM U558, Faculty of Medicine, University of Toulouse, University Paul Sabatier, Alle´es Jules Guesde, Toulouse, France; 4aCGH GSO Canceropole Platform, INSERM U868, Val d’Aurelle, Montpellier, France; 5Laboratory of Cellular and Molecular Biology of Cell Proliferation Control, UMR 5099 CNRS, University of Toulouse, University Paul Sabatier, Toulouse, France and 6Institute of Human Genetics UPR1142 CNRS, Montpellier, France Colorectal cancer is one of the most frequent cancers Introduction worldwide. As the tumor-node-metastasis (TNM) staging classification does not allow to predict the survival of DNA replication in normal cells is regulated by an patients in many cases, additional prognostic factors are ‘origin licensing’ mechanism that ensures that it occurs needed to better forecast their outcome. Genes involved in just once per cycle. Once cells enter the S-phase, the DNA replication may represent an underexplored source stability of DNA replication forks must be preserved to of such prognostic markers. -

Supporting Information
Supporting Information Whittle et al. 10.1073/pnas.0812894106 SI Text range based on analysis on 1.5% agarose gels after reversal of In Vitro Genomic Selection. Recombinant NFI-1-GST fusion pro- cross-linking. DNA-protein complexes were precipitated with tein was immobilized on Glutathione Sepharose 4B (Amersham) anti-NFI immune serum (5 l) or preimmune serum (5 l) as a and C. elegans genomic DNA was used for in vitro genomic control and 5% of the input sample was set aside. Samples were selection. The fusion protein contained the NFI-1 DNA-binding processed using the ChIP assay kit (Upstate). Following reversal domain and a short downstream region. For NFI-1-GST Sepha- of the cross-links, RNase A and Proteinase K treatments, the rose preparation, 400 ml of induced DH5␣ cells expressing immunoprecipitated DNA was purified using phenol-chloro- NFI-1-GST (plasmid pGEXNFI-1) was extracted in buffer L (25 form, precipitated with ethanol, and dissolved in 50 l of DNase, mM Hepes pH 7.5, 10% sucrose, 0.35 M NaCl, 5 mM DTT, 1 mM Rnase-free water. For ChIP-chip, samples were amplified by PMSF, 0.1% Nonidet P-40 and 2 mg/ml of lysozyme). The extract either ligation mediated PCR (5) or a modified Whole Genome (35 ml) was flash-frozen in 5-ml aliquots and stored at –70 °C. To Amplification protocol [Sigma; (6)] as previously described. immobilize NFI-1-GST protein on Glutathione Sepharose 4B, 5 ml of cell extract was incubated with 65 l (bed volume) of Microarrays and Data Extraction. -

Clinicopathological Significance of Claspin Overexpression and Its
Human Pathology (2019) 84,8–17 www.elsevier.com/locate/humpath Original contribution Clinicopathological significance of claspin overexpression and its association with spheroid formation in gastric cancer☆,☆☆ Go Kobayashi MBBS a,b,KazuhiroSentaniMD,PhDa,⁎, Takuya Hattori MD, PhD a, Yuji Yamamoto MD a, Takeharu Imai MD c, Naoya Sakamoto MD, PhD a, Kazuya Kuraoka MD, PhD d, Naohide Oue MD, PhD a, Naomi Sasaki MD, PhD b, Kiyomi Taniyama MD, PhD d,WataruYasuiMD,PhDa aDepartment of Molecular Pathology, Graduate School of Biomedical and Health Sciences, Hiroshima University, Hiroshima, 734-8551 Japan bDepartment of Pathology, Kure-Kyosai Hospital, Federation of National Public Service Personnel Mutual Aid Associations, Hiroshima, 737-8505 Japan cDepartment of Surgical Oncology, Graduate School of Medicine, Gifu University, Gifu, 501-1194 Japan dDepartment of Pathology, National Hospital Organization Kure Medical Center and Chugoku Cancer Center, Kure-City, Hiroshima, 737-0023 Japan Received 27 May 2018; revised 31 August 2018; accepted 6 September 2018 Keywords: Summary Gastric cancer (GC) is one of the leading causes of cancer-related death worldwide. Spheroid colony Cancer stem cell; formation is a useful method to identify cancer stem cells (CSCs). The aim of this study was to identify a novel CD44; prognostic marker or therapeutic target for GC using a method to identify CSCs. We analyzed the microarray Claspin; data in spheroid body–forming and parental cells and focused on the CLSPN gene because it is overexpressed Gastric cancer; in the spheroid body–forming cells in both the GC cell lines MKN-45 and MKN-74. Quantitative reverse- Spheroid transcription polymerase chain reaction analysis revealed that CLSPN messenger RNA expression was up- regulated in GC cell lines MKN-45, MKN-74, and TMK-1. -

A Review of Prostate Cancer Genome-Wide Association Studies (GWAS)
Published OnlineFirst January 18, 2018; DOI: 10.1158/1055-9965.EPI-16-1046 Review Cancer Epidemiology, Biomarkers A Review of Prostate Cancer Genome-Wide & Prevention Association Studies (GWAS) Sarah Benafif1, Zsofia Kote-Jarai1, and Rosalind A. Eeles1,2, on behalf of the PRACTICAL Consortium Abstract Prostate cancer is the most common cancer in men in for population-based risk stratification to target prostate Europe and the United States. The genetic heritability of cancer screening to men with an increased genetic risk of prostate cancer is contributed to by both rarely occurring disease development, while for those who develop prostate genetic variants with higher penetrance and moderate cancer, identifying genetic variants could allow treatment to commonly occurring variants conferring lower risks. to be tailored based on a genetic profile in the early disease The number of identified variants belonging to the latter setting. Functional studies of identified variants are needed category has increased dramatically in the last 10 years with to fully understand underlying mechanisms of disease the development of the genome-wide association study and identify novel targets for treatment. This review will (GWAS) and the collaboration of international consortia outline the GWAS carried out in prostate cancer and the that have led to the sharing of large-scale genotyping data. common variants identified so far, and how these may be Over 40 prostate cancer GWAS have been reported, with utilized clinically in the screening for and management of approximately 170 common variants now identified. prostate cancer. Cancer Epidemiol Biomarkers Prev; 27(8); 845–57. Clinical utility of these variants could include strategies Ó2018 AACR. -

A Systems-Wide Screen Identifies Substrates of the SCF Ubiquitin Ligase
RESEARCH RESOURCE PROTEOMICS A systems-wide screen identifies substrates of the SCFbTrCP ubiquitin ligase Teck Yew Low,1,2 Mao Peng,1,2* Roberto Magliozzi,3* Shabaz Mohammed,1,2† Daniele Guardavaccaro,3 Albert J. R. Heck1,2‡ Cellular proteins are degraded by the ubiquitin-proteasome system (UPS) in a precise and timely fashion. Such precision is conferred by the high substrate specificity of ubiquitin ligases. Identification of substrates of ubiquitin ligases is crucial not only to unravel the molecular mechanisms by which the UPS controls protein degradation but also for drug discovery purposes because many established UPS substrates are implicated in disease. We developed a combined bioinformatics and affinity purification– mass spectrometry (AP-MS) workflow for the system-wide identification of substrates of SCFbTrCP,a member of the SCF family of ubiquitin ligases. These ubiquitin ligases are characterized by a multi- subunit architecture typically consisting of the invariable subunits Rbx1, Cul1, and Skp1, and one of 69 F-box proteins. The F-box protein of this member of the family is bTrCP. SCFbTrCP binds, through the WD40 b repeats of TrCP, to the DpSGXX(X)pS diphosphorylated motif in its substrates. We recovered 27 pre- Downloaded from viously reported SCFbTrCP substrates, of which 22 were verified by two independent statistical proto- cols, thereby confirming the reliability of this approach. In addition to known substrates, we identified 221 proteins that contained the DpSGXX(X)pS motif and also interacted specifically with the WD40 repeats of bTrCP. Thus, with SCFbTrCP, as the example, we showed that integration of structural infor- mation, AP-MS, and degron motif mining constitutes an effective method to screen for substrates of ubiquitin ligases. -

PRMT1-Dependent Regulation of RNA Metabolism and DNA Damage Response Sustains Pancreatic Ductal Adenocarcinoma ✉ Virginia Giuliani 1 , Meredith A
ARTICLE https://doi.org/10.1038/s41467-021-24798-y OPEN PRMT1-dependent regulation of RNA metabolism and DNA damage response sustains pancreatic ductal adenocarcinoma ✉ Virginia Giuliani 1 , Meredith A. Miller1,17, Chiu-Yi Liu1,17, Stella R. Hartono 2,17, Caleb A. Class 3,13, Christopher A. Bristow1, Erika Suzuki1, Lionel A. Sanz2, Guang Gao1, Jason P. Gay1, Ningping Feng1, Johnathon L. Rose4, Hideo Tomihara4,14, Joseph R. Daniele1, Michael D. Peoples1, Jennifer P. Bardenhagen5, Mary K. Geck Do5, Qing E. Chang6, Bhavatarini Vangamudi1,15, Christopher Vellano1, Haoqiang Ying 7, Angela K. Deem1, Kim-Anh Do3, Giannicola Genovese4,8, Joseph R. Marszalek1, Jeffrey J. Kovacs1, Michael Kim9, 1234567890():,; Jason B. Fleming9,16, Ernesto Guccione10, Andrea Viale4, Anirban Maitra 11, M. Emilia Di Francesco5, Timothy A. Yap 12, Philip Jones 5, Giulio Draetta 1,4,5, Alessandro Carugo 1, Frederic Chedin 2 & ✉ Timothy P. Heffernan 1 Pancreatic ductal adenocarcinoma (PDAC) is an aggressive cancer that has remained clini- cally challenging to manage. Here we employ an RNAi-based in vivo functional genomics platform to determine epigenetic vulnerabilities across a panel of patient-derived PDAC models. Through this, we identify protein arginine methyltransferase 1 (PRMT1) as a critical dependency required for PDAC maintenance. Genetic and pharmacological studies validate the role of PRMT1 in maintaining PDAC growth. Mechanistically, using proteomic and transcriptomic analyses, we demonstrate that global inhibition of asymmetric arginine methylation impairs RNA metabolism, which includes RNA splicing, alternative poly- adenylation, and transcription termination. This triggers a robust downregulation of multiple pathways involved in the DNA damage response, thereby promoting genomic instability and inhibiting tumor growth. -

Resveratrol Inhibits Cell Cycle Progression by Targeting Aurora Kinase a and Polo-Like Kinase 1 in Breast Cancer Cells
3696 ONCOLOGY REPORTS 35: 3696-3704, 2016 Resveratrol inhibits cell cycle progression by targeting Aurora kinase A and Polo-like kinase 1 in breast cancer cells RUBICELI MEDINA-AGUILAR1, LAURENCE A. Marchat2, ELENA ARECHAGA OCAMPO3, Patricio GARIGLIO1, JAIME GARCÍA MENA1, NICOLÁS VILLEGAS SEPÚlveda4, MACARIO MartÍNEZ CASTILLO4 and CÉSAR LÓPEZ-CAMARILLO5 1Department of Genetics and Molecular Biology, CINVESTAV-IPN, Mexico D.F.; 2Molecular Biomedicine Program and Biotechnology Network, National School of Medicine and Homeopathy, National Polytechnic Institute, Mexico D.F.; 3Natural Sciences Department, Metropolitan Autonomous University, Mexico D.F.; 4Department of Molecular Biomedicine, CINVESTAV-IPN, Mexico D.F.; 5Oncogenomics and Cancer Proteomics Laboratory, Universidad Autónoma de la Ciudad de México, Mexico D.F., Mexico Received December 4, 2015; Accepted January 8, 2016 DOI: 10.3892/or.2016.4728 Abstract. The Aurora protein kinase (AURKA) and the MDA-MB-231 and MCF-7 cells. By western blot assays, we Polo-like kinase-1 (PLK1) activate the cell cycle, and they confirmed that resveratrol suppressed AURKA, CCND1 and are considered promising druggable targets in cancer CCNB1 at 24 and 48 h. In summary, we showed for the first time therapy. However, resistance to chemotherapy and to specific that resveratrol regulates cell cycle progression by targeting small-molecule inhibitors is common in cancer patients; thus AURKA and PLK1. Our findings highlight the potential use of alternative therapeutic approaches are needed to overcome resveratrol as an adjuvant therapy for breast cancer. clinical resistance. Here, we showed that the dietary compound resveratrol suppressed the cell cycle by targeting AURKA Introduction and PLK1 kinases. First, we identified genes modulated by resveratrol using a genome-wide analysis of gene expression Cancer development results from the interaction between in MDA-MB-231 breast cancer cells. -

Original Article Screening Several Novel Biomarkers for Predicting the Survival of Patients with Lung Adenocarcinoma
Int J Clin Exp Med 2019;12(8):9845-9857 www.ijcem.com /ISSN:1940-5901/IJCEM0092123 Original Article Screening several novel biomarkers for predicting the survival of patients with lung adenocarcinoma Mingzhu Li, Shenyu Wang Department of Integrated Traditional Chinese and Western Medicine, Cancer Hospital of China Medical Univer- sity, Liaoning Cancer Hospital & Institute, No.44 Xiaoheyan Road, Dadong District, Shenyang 110042, Liaoning Province, PR China Received January 31, 2019; Accepted May 9, 2019; Epub August 15, 2019; Published August 30, 2019 Abstract: Background: Increasing evidence has confirmed that long non-coding RNAs (lncRNAs) could regulate pro- tein levels of genes as well as the cellular biological behavior in the competing endogenous RNA (ceRNA) network as miRNA sponges. Our study aimed to explore the role and regulatory mechanisms of lncRNA-mediated ceRNA net- work in lung adenocarcinomas (LUAD), as well as their potential to predict the prognosis of LUAD. Methods: A total of 568 samples with LUAD were downloaded from The Cancer Genome Atlas (TCGA). Differentially expressed lncRNAs (DElncRNAs), miRNAs (DEmiRNAs) and mRNAs (DEmRNAs) were identified with EdgeR package in R according to |log fold change| > 2 and a corrected p-value < 0.05. DElncRNA-DEmiRNA pairs were predicted by the online data- base of miRcode, while DEmRNA-DEmiRNA pairs were predicted through “miRDB”, “miRTarBase” and “TargetScan”. And the ceRNA network was visualized through Cytoscape 3.6. After calculating the degrees of lncRNA nodes, we constructed the ceRNA sub-network. Finally, overall survival analysis was utilized to assess prognostic performance of differentially expressed genes in sub-network. Results: 1503 DElncRNAs, 118 DEmiRNAs and 2501 DEmRNAs were identified associated with LUAD.