DOMASYS Standard
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Letters to the Editor
Letters to the Editor Letters to the Editor Need for a New Framework to Understand lactin levels were high (115 mg/L; normal range, 12–30 mg/L). the© MechanismCopyright of All Antipsychotics 2000 PhysiciansAttempts Postgraduate to reduce dosage below Press, 80 mg/day resultedInc. in relapse, with good recovery when dosage was restored. Sir: The advent of atypical neuroleptics has transformed the A SPECT study was performed using a dual-headed camera pharmacologic treatment of schizophrenia. The advent of single and 185 MBq of 123-Iodobenzamide (IBZM). The specific-to- photon emission computed tomography (SPECT) and positron nonspecific binding ratio was measured at 90 minutes postinjec- emission tomography (PET) neuroreceptor imaging makes it tion. The SPECT was performed a week after a PET analysis possible to link biochemical events in the human brain to their was kindly performed in Dr. Kapur’s laboratory while the pa- clinical consequences. Remington and Kapur1 (supplement 10, tient received 90 mg/day of haloperidol. No detectable recep- 1999) have proposed an interesting model based on studies us- tors at this dosage were found with either technique. ing PET that takes in account the serotonin-2/dopamine-2 Our findings lead us to wonder whether there exists a sub- group of chronic patients resistant to conventional and some (5-HT2/D2) occupancy threshold: conventional antipsychotics atypical neuroleptics in normal doses, but who may respond have low 5-HT2/high D2 ratios, olanzapine and risperidone have well to conventional neuroleptics in high doses. Despite a high high 5-HT2/high D2 ratios, clozapine has a high 5-HT2/low D2 2,3 One personal copy maylevel be of printed striatal D occupancy, our patient did not present with ratio, and quetiapine has a low 5-HT2/low D2 ratio. -
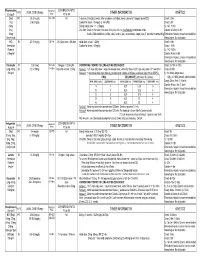
Medication Conversion Chart
Fluphenazine FREQUENCY CONVERSION RATIO ROUTE USUAL DOSE (Range) (Range) OTHER INFORMATION KINETICS Prolixin® PO to IM Oral PO 2.5-20 mg/dy QD - QID NA ↑ dose by 2.5mg/dy Q week. After symptoms controlled, slowly ↓ dose to 1-5mg/dy (dosed QD) Onset: ≤ 1hr 1mg (2-60 mg/dy) Caution for doses > 20mg/dy (↑ risk EPS) Cmax: 0.5hr 2.5mg Elderly: Initial dose = 1 - 2.5mg/dy t½: 14.7-15.3hr 5mg Oral Soln: Dilute in 2oz water, tomato or fruit juice, milk, or uncaffeinated carbonated drinks Duration of Action: 6-8hr 10mg Avoid caffeinated drinks (coffee, cola), tannics (tea), or pectinates (apple juice) 2° possible incompatibilityElimination: Hepatic to inactive metabolites 5mg/ml soln Hemodialysis: Not dialyzable HCl IM 2.5-10 mg/dy Q6-8 hr 1/3-1/2 po dose = IM dose Initial dose (usual): 1.25mg Onset: ≤ 1hr Immediate Caution for doses > 10mg/dy Cmax: 1.5-2hr Release t½: 14.7-15.3hr 2.5mg/ml Duration Action: 6-8hr Elimination: Hepatic to inactive metabolites Hemodialysis: Not dialyzable Decanoate IM 12.5-50mg Q2-3 wks 10mg po = 12.5mg IM CONVERTING FROM PO TO LONG-ACTING DECANOATE: Onset: 24-72hr (4-72hr) Long-Acting SC (12.5-100mg) (1-4 wks) Round to nearest 12.5mg Method 1: 1.25 X po daily dose = equiv decanoate dose; admin Q2-3wks. Cont ½ po daily dose X 1st few mths Cmax: 48-96hr 25mg/ml Method 2: ↑ decanoate dose over 4wks & ↓ po dose over 4-8wks as follows (accelerate taper for sx of EPS): t½: 6.8-9.6dy (single dose) ORAL DECANOATE (Administer Q 2 weeks) 15dy (14-100dy chronic administration) ORAL DOSE (mg/dy) ↓ DOSE OVER (wks) INITIAL DOSE (mg) TARGET DOSE (mg) DOSE OVER (wks) Steady State: 2mth (1.5-3mth) 5 4 6.25 6.25 0 Duration Action: 2wk (1-6wk) Elimination: Hepatic to inactive metabolites 10 4 6.25 12.5 4 Hemodialysis: Not dialyzable 20 8 6.25 12.5 4 30 8 6.25 25 4 40 8 6.25 25 4 Method 3: Admin equivalent decanoate dose Q2-3wks. -

Pharmacologyonline 2: 971-1020 (2009) Newsletter Gabriella Galizia
Pharmacologyonline 2: 971-1020 (2009) Newsletter Gabriella Galizia THE TREATMENT OF THE SCHIZOPHRENIA: AN OVERVIEW Gabriella Galizia School of Pharmacy,University of Salerno, Italy e-mail: [email protected] Summary The schizophrenia is a kind of psychiatric disease, characterized by a course longer than six months (usually chronic or relapsing), by the persistence of symptoms of alteration of mind, behaviour and emotion, with such a seriousness to limitate the normal activity of a person. The terms antipsychotic and neuroleptic define a group of medicine principally used to treat schizophrenia, but they are also efficacious for other psychosis and in states of psychic agitation. The antipsychotics are divided into two classes: classic or typical and atypical. The paliperidone, the major metabolite of risperidone, shares with the native drug the characteristics of receptoral bond and of antagonism of serotonin (5HT2A) and dopamine (D2). It's available in a prolonged release formulation and it allows the administration once daily. Besides, the paliperidone has a pharmacological action independent of CYT P450 and in such way a lot of due pharmacological interactions would be avoided to interference with the activity of the CYP2D6, that is known to have involved in the metabolism of the 25% of the drugs of commune therapeutic employment. Introduction The schizophrenia has been a very hard disease to investigate by the research. This is not surprising because it involves the most mysterious aspects of human mind, as emotions and cognitive processes. According to scientific conventions, the schizophrenia is a kind of psychiatric disease, characterized by a course longer than six months (usually chronic or relapsing), by the persistence of symptoms of alteration of mind, behaviour and emotion, with such a seriousness to limitate the normal activity of a person. -

Neuroprotection by Chlorpromazine and Promethazine in Severe Transient and Permanent Ischemic Stroke
Mol Neurobiol (2017) 54:8140–8150 DOI 10.1007/s12035-016-0280-x Neuroprotection by Chlorpromazine and Promethazine in Severe Transient and Permanent Ischemic Stroke Xiaokun Geng1,2 & Fengwu Li1 & James Yip2 & Changya Peng2 & Omar Elmadhoun2 & Jiamei Shen1 & Xunming Ji1,3 & Yuchuan Ding1,2 Received: 29 June 2016 /Accepted: 31 October 2016 /Published online: 28 November 2016 # Springer Science+Business Media New York 2016 Abstract Previous studies have demonstrated depressive or enhance C + P-induced neuroprotection. C + P therapy im- hibernation-like roles of phenothiazine neuroleptics [com- proved brain metabolism as determined by increased ATP bined chlorpromazine and promethazine (C + P)] in brain levels and NADH activity, as well as decreased ROS produc- activity. This ischemic stroke study aimed to establish neuro- tion. These therapeutic effects were associated with alterations protection by reducing oxidative stress and improving brain in PKC-δ and Akt protein expression. C + P treatments con- metabolism with post-ischemic C + P administration. ferred neuroprotection in severe stroke models by suppressing Sprague-Dawley rats were subjected to transient (2 or 4 h) the damaging cascade of metabolic events, most likely inde- middle cerebral artery occlusion (MCAO) followed by 6 or pendent of drug-induced hypothermia. These findings further 24 h reperfusion, or permanent (28 h) MCAO without reper- prove the clinical potential for C + P treatment and may direct fusion. At 2 h after ischemia onset, rats received either an us closer towards the development of an efficacious neuropro- intraperitoneal (IP) injection of saline or two doses of C + P. tective therapy. Body temperatures, brain infarct volumes, and neurological deficits were examined. -

Is Aristada (Aripiprazole Lauroxil) a Safe and Effective Treatment for Schizophrenia in Adult Patients? Kyle J
Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Student Dissertations, Theses and Papers Scholarship 2017 Is Aristada (Aripiprazole Lauroxil) a Safe and Effective Treatment For Schizophrenia In Adult Patients? Kyle J. Knowles Philadelphia College of Osteopathic Medicine Follow this and additional works at: https://digitalcommons.pcom.edu/pa_systematic_reviews Part of the Psychiatry Commons Recommended Citation Knowles, Kyle J., "Is Aristada (Aripiprazole Lauroxil) a Safe and Effective Treatment For Schizophrenia In Adult Patients?" (2017). PCOM Physician Assistant Studies Student Scholarship. 381. https://digitalcommons.pcom.edu/pa_systematic_reviews/381 This Selective Evidence-Based Medicine Review is brought to you for free and open access by the Student Dissertations, Theses and Papers at DigitalCommons@PCOM. It has been accepted for inclusion in PCOM Physician Assistant Studies Student Scholarship by an authorized administrator of DigitalCommons@PCOM. For more information, please contact [email protected]. Is Aristada (Aripiprazole Lauroxil) a Safe and Effective Treatment For Schizophrenia In Adult Patients? Kyle J. Knowles, PA-S A SELECTIVE EVIDENCE BASED MEDICINE REVIEW In Partial Fulfillment of the Requirements For The Degree of Master of Science In Health Sciences- Physician Assistant Department of Physician Assistant Studies Philadelphia College of Osteopathic Medicine Philadelphia, Pennsylvania December 16, 2016 ABSTRACT OBJECTIVE: The objective of this selective EBM review is to determine whether or not “Is Aristada (aripiprazole lauroxil) a safe and effective treatment for schizophrenia in adult patients?” STUDY DESIGN: Review of three randomized controlled studies. All three trials were conducted between 2014 and 2015. DATA SOURCES: One randomized, controlled trial and two randomized, controlled, double- blind trials found via Cochrane Library and PubMed. -

Potential Drug-Drug Interactions and Adverse Drug Reactions Associated with Hydroxychloroquine
Original Article Potential Drug-drug Interactions and Adverse Drug Reactions Associated with Hydroxychloroquine Arjun Singh1, Richa Chaudhary1, Prayas Verma2, Nilanchal Trivedi3,*, Md. Shamim4 1Department of Pharmacy Practice, Teerthanker Mahaveer College of Pharmacy, TMU, Moradabad, Uttar Pradesh, INDIA. 2Teerthanker Mahaveer Dental College and Research Centre, TMU Moradabad, Uttar Pradesh, INDIA. 3Department of Pharmacology, Teerthanker Mahaveer College of Pharmacy, TMU, Moradabad, Uttar Pradesh, INDIA. 4LCP College of Pharmacy Baghpat, Abdul Kalam Technical University (AKTU), Uttar Pradesh, INDIA. ABSTRACT Introduction: COVID-19 is a pandemic disaster and a health emergency of prime focus for all the world economies. Various prophylactic treatments are considered to combat the disease. Hydroxychloroquine drug is one such option that is given much attention as an armor against SARS COV-2 pandemic. Evaluation and assessment of drug interactions and ADRs is required from ethical concern to justify the use of HCQ on such large scale. Methods: We have performed an analysis of HCQ drug interactions on Micromedex®. We have reviewed literature of HCQ pharmacokinetic properties, ADRs/ ADEs and toxicities associated with the use of HCQ drug on PubMed, Google Scholar and CDC database. Results: There are around 180 drug interactions possible with HCQ. Out of them 13 are of contraindicated severity level and other 165 are of major severity and 2 of them are moderately severe. Most of the interactions are coupled with QT prolonging agents (170), Cardiac arrhythmias is possible with the concomitant use of at least 2 drugs, 4 drugs leads to Torsade de points. System organ level ADRs are also evaluated along with various precautions, warnings and contraindications. -

Antipsychotic Combinations
Graylands Hospital DRUG BULLETIN Pharmacy Department Brockway Road Mount Claremont WA 6010 Telephone (08) 9347 6400 Email [email protected] Fax (08) 9384 4586 Antipsychotic Combinations Graylands Hospital Drug Bulletin 2008 Vol. 15 No. 3 February ISSN 1323-1251 Antipsychotic combinations Reasons for antipsychotic combinations Despite the development of efficacious medications for the treatment of schizophrenia, many people do There are a number of theoretical benefits and not respond adequately. To address this problem, reasons cited for antipsychotic combination the use of two or more antipsychotics simultaneously prescribing, these include: is a commonly employed treatment strategy. Although the use of combination antipsychotics is Complementary mechanisms of action4 (e.g. common in clinical practice, the risks and benefits adding an antipsychotic with strong dopamine have not been systematically evaluated to date. As a D2 blockade to a weak D2 blocker) result, current Australian treatment algorithms Partial replacement of antipsychotic action for including the Royal Australian and New Zealand drugs with intolerable adverse effects at higher College of Psychiatry Schizophrenia Guidelines and 5 doses (e.g. adding quetiapine to clozapine to the Western Australian Therapeutic Advisory Group minimise metabolic adverse effects) Antipsychotic Guidelines advise against the use of combined antipsychotics, except for short periods of Alternative where clozapine cannot be used6 changeover1,2. Most data on antipsychotic -

New Drugs Are Not Enough‑Drug Repositioning in Oncology: an Update
INTERNATIONAL JOURNAL OF ONCOLOGY 56: 651-684, 2020 New drugs are not enough‑drug repositioning in oncology: An update ROMINA GABRIELA ARMANDO, DIEGO LUIS MENGUAL GÓMEZ and DANIEL EDUARDO GOMEZ Laboratory of Molecular Oncology, Science and Technology Department, National University of Quilmes, Bernal B1876, Argentina Received August 15, 2019; Accepted December 16, 2019 DOI: 10.3892/ijo.2020.4966 Abstract. Drug repositioning refers to the concept of discov- 17. Lithium ering novel clinical benefits of drugs that are already known 18. Metformin for use treating other diseases. The advantages of this are that 19. Niclosamide several important drug characteristics are already established 20. Nitroxoline (including efficacy, pharmacokinetics, pharmacodynamics and 21. Nonsteroidal anti‑inflammatory drugs toxicity), making the process of research for a putative drug 22. Phosphodiesterase-5 inhibitors quicker and less costly. Drug repositioning in oncology has 23. Pimozide received extensive focus. The present review summarizes the 24. Propranolol most prominent examples of drug repositioning for the treat- 25. Riluzole ment of cancer, taking into consideration their primary use, 26. Statins proposed anticancer mechanisms and current development 27. Thalidomide status. 28. Valproic acid 29. Verapamil 30. Zidovudine Contents 31. Concluding remarks 1. Introduction 2. Artesunate 1. Introduction 3. Auranofin 4. Benzimidazole derivatives In previous decades, a considerable amount of work has been 5. Chloroquine conducted in search of novel oncological therapies; however, 6. Chlorpromazine cancer remains one of the leading causes of death globally. 7. Clomipramine The creation of novel drugs requires large volumes of capital, 8. Desmopressin alongside extensive experimentation and testing, comprising 9. Digoxin the pioneer identification of identifiable targets and corrobora- 10. -

PERPHENAZINE and AMITRIPTYLINE HYDROCHLORIDE- Perphenazine and Amitriptyline Hydrochloride Tablet, Film Coated Mylan Pharmaceuticals Inc
PERPHENAZINE AND AMITRIPTYLINE HYDROCHLORIDE- perphenazine and amitriptyline hydrochloride tablet, film coated Mylan Pharmaceuticals Inc. ---------- WARNING Increased Mortality in Elderly Patients with Dementia-Related Psychosis Elderly patients with dementia-related psychosis treated with antipsychotic drugs are at an increased risk of death. Analyses of seventeen placebo-controlled trials (modal duration of 10 weeks), largely in patients taking atypical antipsychotic drugs, revealed a risk of death in drug-treated patients of between 1.6 to 1.7 times the risk of death in placebo-treated patients. Over the course of a typical 10-week controlled trial, the rate of death in drug- treated patients was about 4.5%, compared to a rate of about 2.6% in the placebo group. Although the causes of death were varied, most of the deaths appeared to be either cardiovascular (e.g., heart failure, sudden death) or infectious (e.g., pneumonia) in nature. Observational studies suggest that, similar to atypical antipsychotic drugs, treatment with conventional antipsychotic drugs may increase mortality. The extent to which the findings of increased mortality in observational studies may be attributed to the antipsychotic drug as opposed to some characteristic(s) of the patients is not clear. Perphenazine and amitriptyline hydrochloride is not approved for the treatment of patients with dementia- related psychosis (see WARNINGS). Suicidality and Antidepressant Drugs Antidepressants increased the risk compared to placebo of suicidal thinking and behavior (suicidality) in children, adolescents and young adults in short-term studies of major depressive disorder (MDD) and other psychiatric disorders. Anyone considering the use of perphenazine and amitriptyline or any other antidepressant in a child, adolescent, or young adult must balance this risk with the clinical need. -

Use of Antipsychotic Drugs and Lithium in Mania
BRITISHJOURNAL OF PSYCHIATRY %20%2001), 01), 178 %suppl. 41), s14s148^ 8^ s156 Use of antipsychotic drugs and lithium in mania experience over the following 30 years indi- cated that lithium is far short of an ideal treatment, even when administered expertly JOHN COOKSON to `concordant' patients. There is a striking difference between the results of early con- trolled trials and the outcome on lithium in open clinical practice, where a smaller pro- portion of patients appear to be `lithium re- sponders'; some even doubt the validity of the clinical trials %Moncrieff, 1997). The benefits of lithium therapy have to be balanced against the difficulties in its Background Studies highlighting the Mania or a manic episode is a severe phase management ± with poor compliance in pa- difficulties associated withlithium suggest in the course of bipolar disorders, the con- tients with bipolar disorder and the occur- dition termed `manic±depressive illness' by rence of withdrawal mania ± and the risks that the role of antipsychotic drugs and Kraepelin in the 19th century. A contem- of side-effects and toxicity %Cookson, mood stabilisersin bipolardisorder should porary textbookdescribed the difficulty of 1997). The latter includes the possibility be reconsidered. managing a patient with mania ± using of permanent neurological sequelae with drugs of limited efficacy, mainly sedative cerebellar damage %Schou, 1984). Aims Toreview the efficacyandmode or anaesthetic, such as chloral and ur- Since the 1970s anticonvulsant drugs, of action of antipsychotic drugsin mania, ethane, or potentially toxic drugs, such as first carbamazepine and more recently and to consider the differences between potassium bromide. The sedative anticon- valproate and, in open studies, lamotrigine officialguidelines and routine clinical vulsant paraldehyde was also used. -

Screening of 300 Drugs in Blood Utilizing Second Generation
Forensic Screening of 300 Drugs in Blood Utilizing Exactive Plus High-Resolution Accurate Mass Spectrometer and ExactFinder Software Kristine Van Natta, Marta Kozak, Xiang He Forensic Toxicology use Only Drugs analyzed Compound Compound Compound Atazanavir Efavirenz Pyrilamine Chlorpropamide Haloperidol Tolbutamide 1-(3-Chlorophenyl)piperazine Des(2-hydroxyethyl)opipramol Pentazocine Atenolol EMDP Quinidine Chlorprothixene Hydrocodone Tramadol 10-hydroxycarbazepine Desalkylflurazepam Perimetazine Atropine Ephedrine Quinine Cilazapril Hydromorphone Trazodone 5-(p-Methylphenyl)-5-phenylhydantoin Desipramine Phenacetin Benperidol Escitalopram Quinupramine Cinchonine Hydroquinine Triazolam 6-Acetylcodeine Desmethylcitalopram Phenazone Benzoylecgonine Esmolol Ranitidine Cinnarizine Hydroxychloroquine Trifluoperazine Bepridil Estazolam Reserpine 6-Monoacetylmorphine Desmethylcitalopram Phencyclidine Cisapride HydroxyItraconazole Trifluperidol Betaxolol Ethyl Loflazepate Risperidone 7(2,3dihydroxypropyl)Theophylline Desmethylclozapine Phenylbutazone Clenbuterol Hydroxyzine Triflupromazine Bezafibrate Ethylamphetamine Ritonavir 7-Aminoclonazepam Desmethyldoxepin Pholcodine Clobazam Ibogaine Trihexyphenidyl Biperiden Etifoxine Ropivacaine 7-Aminoflunitrazepam Desmethylmirtazapine Pimozide Clofibrate Imatinib Trimeprazine Bisoprolol Etodolac Rufinamide 9-hydroxy-risperidone Desmethylnefopam Pindolol Clomethiazole Imipramine Trimetazidine Bromazepam Felbamate Secobarbital Clomipramine Indalpine Trimethoprim Acepromazine Desmethyltramadol Pipamperone -

Drug and Medication Classification Schedule
KENTUCKY HORSE RACING COMMISSION UNIFORM DRUG, MEDICATION, AND SUBSTANCE CLASSIFICATION SCHEDULE KHRC 8-020-1 (11/2018) Class A drugs, medications, and substances are those (1) that have the highest potential to influence performance in the equine athlete, regardless of their approval by the United States Food and Drug Administration, or (2) that lack approval by the United States Food and Drug Administration but have pharmacologic effects similar to certain Class B drugs, medications, or substances that are approved by the United States Food and Drug Administration. Acecarbromal Bolasterone Cimaterol Divalproex Fluanisone Acetophenazine Boldione Citalopram Dixyrazine Fludiazepam Adinazolam Brimondine Cllibucaine Donepezil Flunitrazepam Alcuronium Bromazepam Clobazam Dopamine Fluopromazine Alfentanil Bromfenac Clocapramine Doxacurium Fluoresone Almotriptan Bromisovalum Clomethiazole Doxapram Fluoxetine Alphaprodine Bromocriptine Clomipramine Doxazosin Flupenthixol Alpidem Bromperidol Clonazepam Doxefazepam Flupirtine Alprazolam Brotizolam Clorazepate Doxepin Flurazepam Alprenolol Bufexamac Clormecaine Droperidol Fluspirilene Althesin Bupivacaine Clostebol Duloxetine Flutoprazepam Aminorex Buprenorphine Clothiapine Eletriptan Fluvoxamine Amisulpride Buspirone Clotiazepam Enalapril Formebolone Amitriptyline Bupropion Cloxazolam Enciprazine Fosinopril Amobarbital Butabartital Clozapine Endorphins Furzabol Amoxapine Butacaine Cobratoxin Enkephalins Galantamine Amperozide Butalbital Cocaine Ephedrine Gallamine Amphetamine Butanilicaine Codeine