Blepharoplasty, Reconstructive Eyelid Surgery, and Brow Lift
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Multipurpose Conical Orbital Implant in Evisceration
Ophthalmic Plastic and Reconstructive Surgery Vol. 21, No. 5, pp 376–378 ©2005 The American Society of Ophthalmic Plastic and Reconstructive Surgery, Inc. Multipurpose Conical Orbital Implant in Evisceration Harry Marshak, M.D., and Steven C. Dresner, M.D. Doheny Eye Institute, Keck School of Medicine, University of Southern California, Los Angeles, California, U.S.A. Purpose: To evaluate the safety and efficacy of the porous polyethylene multipurpose conical orbital implant for use in evisceration. Methods: A retrospective review of 31 eyes that underwent evisceration and received the multipurpose conical orbital implant. The orbits were evaluated at 1 week, 1 month, and 6 months after final prosthetic fitting for implant exposure, superior sulcus deformity, and prosthetic motility. Results: There were no cases of extrusion, migration, or infection. All patients had a good cosmetic result after final prosthetic fitting. Prosthetic motility was good in all patients. Exposure developed in one eye (3%) and a superior sulcus deformity developed in one eye (3%). Conclusions: Placement of an multipurpose conical orbital implant in conjunction with evisceration is a safe and effective treatment for blind painful eye that achieves good motility and a good cosmetic result. visceration has proved to be effective for the treat- forms anteriorly to the sclera to be closed over it, without Ement of blind painful eye from phthisis bulbi or crowding the fornices, and extends posteriorly through endophthalmitis. By retaining the sclera in its anatomic the posterior sclerotomies, providing needed volume to natural position, evisceration has the advantage of allow- the posterior orbit. ing the insertions of the extraocular muscles to remain intact, promoting better motility. -

Ocular Surface Changes Associated with Ophthalmic Surgery
Journal of Clinical Medicine Review Ocular Surface Changes Associated with Ophthalmic Surgery Lina Mikalauskiene 1, Andrzej Grzybowski 2,3 and Reda Zemaitiene 1,* 1 Department of Ophthalmology, Medical Academy, Lithuanian University of Health Sciences, 44037 Kaunas, Lithuania; [email protected] 2 Department of Ophthalmology, University of Warmia and Mazury, 10719 Olsztyn, Poland; [email protected] 3 Institute for Research in Ophthalmology, Foundation for Ophthalmology Development, 61553 Poznan, Poland * Correspondence: [email protected] Abstract: Dry eye disease causes ocular discomfort and visual disturbances. Older adults are at a higher risk of developing dry eye disease as well as needing for ophthalmic surgery. Anterior segment surgery may induce or worsen existing dry eye symptoms usually for a short-term period. Despite good visual outcomes, ocular surface dysfunction can significantly affect quality of life and, therefore, lower a patient’s satisfaction with ophthalmic surgery. Preoperative dry eye disease, factors during surgery and postoperative treatment may all contribute to ocular surface dysfunction and its severity. We reviewed relevant articles from 2010 through to 2021 using keywords “cataract surgery”, ”phacoemulsification”, ”refractive surgery”, ”trabeculectomy”, ”vitrectomy” in combina- tion with ”ocular surface dysfunction”, “dry eye disease”, and analyzed studies on dry eye disease pathophysiology and the impact of anterior segment surgery on the ocular surface. Keywords: dry eye disease; ocular surface dysfunction; cataract surgery; phacoemulsification; refractive surgery; trabeculectomy; vitrectomy Citation: Mikalauskiene, L.; Grzybowski, A.; Zemaitiene, R. Ocular Surface Changes Associated with Ophthalmic Surgery. J. Clin. 1. Introduction Med. 2021, 10, 1642. https://doi.org/ 10.3390/jcm10081642 Dry eye disease (DED) is a common condition, which usually causes discomfort, but it can also be an origin of ocular pain and visual disturbances. -

Treatment of Congenital Ptosis
13 Review Article Page 1 of 13 Treatment of congenital ptosis Vladimir Kratky1,2^ 1Department of Ophthalmology, Queen’s University, Kingston, Canada; 21st Medical Faculty, Charles University, Prague, Czech Republic Correspondence to: Vladimir Kratky, BSc, MD, FRCSC, DABO. Associate Professor of Ophthalmology, Director of Ophthalmic Plastic and Orbital Surgery, Oculoplastics Fellowship Director, Queen’s University, Kingston, Canada; 1st Medical Faculty, Charles University, Prague, Czech Republic. Email: [email protected]. Abstract: Congenital ptosis is an abnormally low position of the upper eyelid, with respect to the visual axis in the primary gaze. It can be present at birth or manifest itself during the first year of life and can be bilateral or unilateral. Additionally, it may be an isolated finding or part of a constellation of signs of a specific syndrome or systemic associations. Depending on how much it interferes with the visual axis, it may be considered as a functional or a cosmetic condition. In childhood, functional ptosis can lead to deprivation amblyopia and astigmatism and needs to be treated. However, even mild ptosis with normal vision can lead to psychosocial problems and correction is also advised, albeit on a less urgent basis. Although, patching and glasses can be prescribed to treat the amblyopia, the mainstay of management is surgical. There are several types of surgical procedure available depending on the severity and etiology of the droopy eyelid. The first part of this paper will review the different categories of congenital ptosis, including more common associated syndromes. The latter part will briefly cover the different surgical approaches, with emphasis on how to choose the correct condition. -

Corneal Ectasia
Corneal Ectasia Secretary for Quality of Care Anne L. Coleman, MD, PhD Academy Staff Nicholas P. Emptage, MAE Nancy Collins, RN, MPH Doris Mizuiri Jessica Ravetto Flora C. Lum, MD Medical Editor: Susan Garratt Design: Socorro Soberano Approved by: Board of Trustees September 21, 2013 Copyright © 2013 American Academy of Ophthalmology® All rights reserved AMERICAN ACADEMY OF OPHTHALMOLOGY and PREFERRED PRACTICE PATTERN are registered trademarks of the American Academy of Ophthalmology. All other trademarks are the property of their respective owners. This document should be cited as follows: American Academy of Ophthalmology Cornea/External Disease Panel. Preferred Practice Pattern® Guidelines. Corneal Ectasia. San Francisco, CA: American Academy of Ophthalmology; 2013. Available at: www.aao.org/ppp. Preferred Practice Pattern® guidelines are developed by the Academy’s H. Dunbar Hoskins Jr., MD Center for Quality Eye Care without any external financial support. Authors and reviewers of the guidelines are volunteers and do not receive any financial compensation for their contributions to the documents. The guidelines are externally reviewed by experts and stakeholders before publication. Corneal Ectasia PPP CORNEA/EXTERNAL DISEASE PREFERRED PRACTICE PATTERN DEVELOPMENT PROCESS AND PARTICIPANTS The Cornea/External Disease Preferred Practice Pattern® Panel members wrote the Corneal Ectasia Preferred Practice Pattern® guidelines (“PPP”). The PPP Panel members discussed and reviewed successive drafts of the document, meeting in person twice and conducting other review by e-mail discussion, to develop a consensus over the final version of the document. Cornea/External Disease Preferred Practice Pattern Panel 2012–2013 Robert S. Feder, MD, Co-chair Stephen D. McLeod, MD, Co-chair Esen K. -

The Simplified Trachoma Grading System, Amended Anthony W Solomon,A Amir B Kello,B Mathieu Bangert,A Sheila K West,C Hugh R Taylor,D Rabebe Tekeraoie & Allen Fosterf
PolicyPolicy & practice & practice The simplified trachoma grading system, amended Anthony W Solomon,a Amir B Kello,b Mathieu Bangert,a Sheila K West,c Hugh R Taylor,d Rabebe Tekeraoie & Allen Fosterf Abstract A simplified grading system for trachoma was published by the World Health Organization (WHO) in 1987. Intended for use by non-specialist personnel working at community level, the system includes five signs, each of which can be present or absent in any eye: (i) trachomatous trichiasis; (ii) corneal opacity; (iii) trachomatous inflammation—follicular; (iv) trachomatous inflammation—intense; and (v) trachomatous scarring. Though neither perfectly sensitive nor perfectly specific for trachoma, these signs have been essential tools for identifying populations that need interventions to eliminate trachoma as a public health problem. In 2018, at WHO’s 4th global scientific meeting on trachoma, the definition of one of the signs, trachomatous trichiasis, was amended to exclude trichiasis that affects only the lower eyelid. This paper presents the amended system, updates its presentation, offers notes on its use and identifies areas of ongoing debate. Introduction (ii) corneal opacity; (iii) trachomatous inflammation—fol- licular; (iv) trachomatous inflammation—intense; and (v) tra- Trachoma is the most important infectious cause of blindness.1 chomatous scarring.19 Trachomatous inflammation—follicular Repeated conjunctival infection2 with particular strains of and trachomatous inflammation—intense are signs of active Chlamydia trachomatis3–5 -

Love Plasma Price List 4 Other Treatments
PLASMA UPPER FACIAL TREATMENTS NECK LIFT / TURKEY NECK £650 NECK LINES / NECK CORDS £350 WRINKLED HANDS £400 (5-8 TREATMENTS, OVERALL FACIAL RESURFACING & REJUVENATION 2 TO 3 WEEKS APART) £700 SKIN TAGS FROM £50 NON-SURGICAL FACELIFT (FULL, MID, MINI) OVERALL FACIAL RESURFACING & REJUVENATION NECK LIFT, TURKEY NECK, NECK LINES / NECK CORDS / BANDING WRINKLED HANDS WWW.LOVEPLASMA.COM PLASMA LOWER FACIAL TREATMENTS JOWL / JAWLINE TIGHTENING & AUGMENTATION £500 VERTICAL LINES / SMOKERS LINES / PERIORAL LINES LIPSTICK LINES £250 SMILE LINES / MARIONETTE LINES £250 LABIOMENTAL CREASE / CHIN LINES £250 LIP FLIP £200 PHILITRAL CREST, VERTICAL LIP LINES / SMOKERS LINES / PERIORAL LINES / PERITONEAL FOLDS / LIPSTICK LINES ORAL COMMISSURES / MOUTH CORNERS SMILE LINES / PARENTHESES JOWL / JAWLINE TIGHTENING & MARIONETTE LINES & AUGMENTATION LABIOMENTAL CREASE, CHIN LINES & CHIN AUGMENTATION WWW.LOVEPLASMA.COM PLASMA MID FACIAL TREATMENTS HORIZONTAL LINES / BUNNY LINES £150 EAR LOBE REJUVENATION £150 NASOLABIAL FOLDS £250 ACCORDION LINES & FOLDS £200 HORIZONTAL LINES / BUNNY LINES & RHINOPHYMA CHEEK LIFT, SKIN TENSION LINES, NASOLABIAL FOLDS ROSACEA & FACIAL REJUVENATION ACCORDION LINES & FOLDS WWW.LOVEPLASMA.COM PLASMA UPPER FACIAL TREATMENTS CROWS FEET £250 NON SURGICAL BLEPHAROPLASTY UPPER EYELIDS £250 NON SURGICAL BLEPHAROPLASTY LOWER EYELIDS £200 NON SURGICAL BLEPHAROPLASTY UPPER & LOWER EYELIDS £430 EYEBROW LIFT £300 HOLLOW TEMPLES CROWS FEET PREORBITAL REGION AND INFRAORBITAL FOLDS / CREASES FROWN / RELAX LINES / CREASES NON-SURGICAL GLABELLA AREA, BETWEEN THE BROW / BLEPHAROPLASTY FOR RADIX UPPER & LOWER EYELIDS / BAGS / HOODS WWW.LOVEPLASMA.COM. -

BOSTON TERRIER EYE DISEASE Corneal Ulcers and Prevention
BOSTON TERRIER EYE DISEASE Corneal Ulcers and Prevention Corneal Ulcers are the single largest eye problem in Boston Terriers. Perhaps 1 dog in 10 will experience a corneal ulcer sometime during its life based on the l903 dogs surveyed in the 2000 Boston Terrier Health Survey. The Boston Terrier Standard for the Breed calls for eyes to be “wide apart, large and round and dark in color. The eyes are set square in the skull and the outside corners are on a line with the cheeks as viewed from the front". The ideal Boston Terrier eye does not protrude but is "set square in the skull". Unfortunately the Boston eye is fairly prone to eye injury because of its large size and prominence. Corneal ulcers are caused initially by injury to the eyes. The common practice of removing Boston Terrier whiskers may be a reason that eyes become injured due to lack of sensory feelers. Some breeders do not trim whiskers once a dog's show career is finished because they know that whiskers can prevent injury to the eye. There are a number of external reasons why an injured eye doesn't heal. These may include irritation from eyelashes or from facial hairs, infection, and lack of moisture in the eye. Some of these reasons are hereditary. Internal reasons for an eye not healing include glaucoma and infection. Corneal ulcers can be difficult and expensive to treat and often result in the loss of the eye. This is a case where an "ounce of prevention is worth a pound of cure". -

Ophthalmic Management of Facial Nerve Palsy
Eye (2004) 18, 1225–1234 & 2004 Nature Publishing Group All rights reserved 0950-222X/04 $30.00 www.nature.com/eye 1 2 3 Ophthalmic V Lee , Z Currie and JRO Collin REVIEW management of facial nerve palsy Abstract The facial nerve travels with the eighth cranial nerve through the internal auditory canal and The ophthalmologist plays a pivotal role in the through the internal fallopian canal in the evaluation and rehabilitation of patients with petrous temporal bone for the longest facial nerve palsy. It is crucial to recognize and interosseus course of any cranial nerve (30 mm). treat the potentially life-threatening The fibres for the pterygopalatine ganglion underlying causes. The immediate ophthalmic leave at the geniculate ganglion as the greater priority is to ensure adequate corneal superficial petrosal nerve. The nerve to the protection. The medium to long-term stapedius and the chorda tympani (innervation management consists of treatment of epiphora, to the salivary glands) leave prior to the nerve hyperkinetic disorders secondary to aberrant exiting through the stylomastoid foramen as a regeneration and poor cosmesis. Patients purely motor nerve to the muscles of facial should be appropriately referred for general expression.2 Within the substance of the parotid 1 facial re-animation. This review aims to Central Eye Service gland, it divides into the five main Central Middlesex Hospital provide a guide to the management of this branchesFthe temporal, zygomatic, buccal, Acton Lane complex condition. Park Royal mandibular, and cervical branches. Facial nerve Eye (2004) 18, 1225–1234. doi:10.1038/sj.eye.6701383 Acton London, UK lesions above the geniculate ganglion classically Published online 16 April 2004 cause more severe ophthalmic symptoms 2Department of because lacrimal secretion and orbicularis Keywords: gold weight; tarsorrhapy; facial Ophthalmology closure are involved. -

The Revised Ghent Nosology; Reclassifying Isolated Ectopia Lentis A
The revised ghent nosology; reclassifying isolated ectopia lentis A. Chandra, D. Patel, A. Aragon-Martin, Amélie Pinard, Gwenaëlle Collod-Béroud, C Comeglio, C. Boileau, L. Faivre, D. Charteris, a H Child, et al. To cite this version: A. Chandra, D. Patel, A. Aragon-Martin, Amélie Pinard, Gwenaëlle Collod-Béroud, et al.. The revised ghent nosology; reclassifying isolated ectopia lentis. Clinical Genetics, Wiley, 2015, 87 (3), pp.284-287. 10.1111/cge.12358. hal-01670143 HAL Id: hal-01670143 https://hal.archives-ouvertes.fr/hal-01670143 Submitted on 21 Dec 2017 HAL is a multi-disciplinary open access L’archive ouverte pluridisciplinaire HAL, est archive for the deposit and dissemination of sci- destinée au dépôt et à la diffusion de documents entific research documents, whether they are pub- scientifiques de niveau recherche, publiés ou non, lished or not. The documents may come from émanant des établissements d’enseignement et de teaching and research institutions in France or recherche français ou étrangers, des laboratoires abroad, or from public or private research centers. publics ou privés. CLINICAL GENETICS doi: 10.1111/cge.12358 Short Report The revised ghent nosology; reclassifying isolated ectopia lentis Chandra A., Patel D., Aragon-Martin J.A., Pinard A., Collod-Beroud´ G., A. Chandraa,b,c, D. Patela, Comeglio P., Boileau C., Faivre L., Charteris D., Child A.H., Arno G. The J.A. Aragon-Martind, revised ghent nosology; reclassifying isolated ectopia lentis. A. Pinarde,f, Clin Genet 2015: 87: 284–287. © John Wiley & Sons A/S. Published by G. Collod-Beroud´ e,f, John Wiley & Sons Ltd, 2014 P. -

Insertion of Aqueous Shunt in Pedicatric Glaucoma
1/29/2018 Challenges of Insertion of Aqueous shunt in paediatric glaucoma Ahmed Elkarmouty MD, FRCS Moorfields Eye Hospital London, UK Classification • Primary Childhood Glaucoma • A- Primary Congenital Glaucoma (PCG) 1: 10,000–18,000 • B- Juvenile Open Angle Glaucoma (JOAG) (5-35 ys,)1 : 50,000. • Secondary Childhood Glaucoma • A- Glaucoma associated with non-acquired ocular anomalies • B- Glaucoma associated with non- acquired systemic disease or syndrome • C- Glaucoma associated with acquired condition • D- Glaucoma following Cataract surgery 1 1/29/2018 Glaucoma associated with non- acquired ocular anomalies • Conditions with predominantly ocular anomalies present at birth which may or may not be associated with systemic signs • Axenfeld Reiger anomaly • Peters anomaly • Ectropion Uvae • Congenital iris hypolplasia • Aniridia • Oculodermal melanocytosis • Posterior polymorphous dystrophy • Microphthalmos • Microcornea • Ectopia Lentis ( et pupillae) • Persistent foetus vasculopathy Glaucoma associated with non- acquired systemic disease or syndrome predominantly associated with known syndrome, systemic anomalies present at birth which may be associated with ocular signs • Down Syndrome • Connective tissue disorder: Marfan syndrome, Weill- Marchesiani syndrome, Stickler syndrome • Metabolic disorder : Homocystenuria, lowe syndrome, Mucoploysacchroidoses • Phacomatoses: Neurofibromatoses, Sturge Weber, Klipple-Trenaunay- weber syndrome, Rubenstein Taybi • Congenital Rubella 2 1/29/2018 Glaucoma associated with acquired condition Conditions -

Expanding the Phenotypic Spectrum of PAX6 Mutations: from Congenital Cataracts to Nystagmus
G C A T T A C G G C A T genes Article Expanding the Phenotypic Spectrum of PAX6 Mutations: From Congenital Cataracts to Nystagmus Maria Nieves-Moreno 1,* , Susana Noval 1 , Jesus Peralta 1, María Palomares-Bralo 2 , Angela del Pozo 3 , Sixto Garcia-Miñaur 4, Fernando Santos-Simarro 4 and Elena Vallespin 5 1 Department of Ophthalmology, Hospital Universitario La Paz, 28046 Madrid, Spain; [email protected] (S.N.); [email protected] (J.P.) 2 Department of Molecular Developmental Disorders, Medical and Molecular Genetics Institue (INGEMM) IdiPaz, CIBERER, Hospital Universitario La Paz, 28046 Madrid, Spain; [email protected] 3 Department of Bioinformatics, Medical and Molecular Genetics Institue (INGEMM) IdiPaz, CIBERER, Hospital Universitario La Paz, 28046 Madrid, Spain; [email protected] 4 Department of Clinical Genetics, Medical and Molecular Genetics Institue (INGEMM) IdiPaz, CIBERER, Hospital Universitario La Paz, 28046 Madrid, Spain; [email protected] (S.G.-M.); [email protected] (F.S.-S.) 5 Department of Molecular Ophthalmology, Medical and Molecular Genetics Institue (INGEMM) IdiPaz, CIBERER, Hospital Universitario La Paz, 28046 Madrid, Spain; [email protected] * Correspondence: [email protected] Abstract: Background: Congenital aniridia is a complex ocular disorder, usually associated with severe visual impairment, generally caused by mutations on the PAX6 gene. The clinical phenotype of PAX6 mutations is highly variable, making the genotype–phenotype correlations difficult to establish. Methods: we describe the phenotype of eight patients from seven unrelated families Citation: Nieves-Moreno, M.; Noval, with confirmed mutations in PAX6, and very different clinical manifestations. -
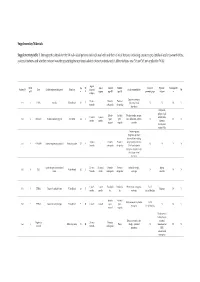
Solved/Unsolved
Supplementary Materials: Supplementary table 1. Demographic details for the 54 individual patients (solved/unsolved) and their clinical features including cataract type, details of ocular co-morbidities, systemic features and whether cataract was the presenting feature (non-isolated cataract patients only). Abbreviations: yes (Y), no (N), not applicable (N/A). Age at Famil Ag M/ Age at Cataract Cataract Cataract Systemic Consanguinit Patient ID Gene Confirmed genetic diagnosis Ethnicity diagnosi Ocular co-morbidities FH y ID e F surgery type RE type LE presenting sign features y s (days) Aniridia, nystagmus, 23 years Posterior Posterior 1-1 1 PAX6 Aniridia White British 25 F - glaucoma, foveal N N N Y 4 months subcapsular subcapsular hypoplasia Cleft palate, epilepsy, high Aphakia Aphakia Macular atrophy, myopia, 7 years 9 7 years 8 arched palate, 2-1 2 COL11A1 Stickler syndrome, type II Not Stated 34 F (post- (post- lens subluxation, vitreous N N N months months flattened surgical) surgical) anomaly maxilla, short stature (5'2ft) Anterior segment dysgenesis, pupillary abnormalities including 12 years Posterior Posterior ectopic pupils, ectropion 3-1 3 CPAMD8 Anterior segment dysgenesis 8 Other, Any other 27 F - N N Y N 5 months subcapsular subcapsular UVAE and irodensis, nystagmus, dysplastic optic discs, large corneal diameters Gyrate atrophy of choroid and 23 years 29 years 1 Posterior Posterior Retinal dystrophy, Bipolar 4-1 4 OAT White British 42 F N N N retina 7 months month subcapsular subcapsular exotropia disorder 1 year 6 1 year