How Nevada, Utah Compare
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Colorado History Chronology
Colorado History Chronology 13,000 B.C. Big game hunters may have occupied area later known as Colorado. Evidence shows that they were here by at least 9200 B.C. A.D. 1 to 1299 A.D. Advent of great Prehistoric Cliff Dwelling Civilization in the Mesa Verde region. 1276 to 1299 A.D. A great drought and/or pressure from nomadic tribes forced the Cliff Dwellers to abandon their Mesa Verde homes. 1500 A.D. Ute Indians inhabit mountain areas of southern Rocky Mountains making these Native Americans the oldest continuous residents of Colorado. 1541 A.D. Coronado, famed Spanish explorer, may have crossed the southeastern corner of present Colorado on his return march to Mexico after vain hunt for the golden Seven Cities of Cibola. 1682 A.D. Explorer La Salle appropriates for France all of the area now known as Colorado east of the Rocky Mountains. 1765 A.D. Juan Maria Rivera leads Spanish expedition into San Juan and Sangre de Cristo Mountains in search of gold and silver. 1776 A.D. Friars Escalante and Dominguez seeking route from Santa Fe to California missions, traverse what is now western Colorado as far north as the White River in Rio Blanco County. 1803 A.D. Through the Louisiana Purchase, signed by President Thomas Jefferson, the United States acquires a vast area which included what is now most of eastern Colorado. While the United States lays claim to this vast territory, Native Americans have resided here for hundreds of years. 1806 A.D. Lieutenant Zebulon M. Pike and small party of U.S. -

Dipterous Predators of the Mosquito in Utah and Wyoming
Great Basin Naturalist Volume 9 Number 1 – Number 2 Article 2 12-30-1948 Dipterous predators of the mosquito in Utah and Wyoming Fred C. Harmston United States Public Health Service Follow this and additional works at: https://scholarsarchive.byu.edu/gbn Recommended Citation Harmston, Fred C. (1948) "Dipterous predators of the mosquito in Utah and Wyoming," Great Basin Naturalist: Vol. 9 : No. 1 , Article 2. Available at: https://scholarsarchive.byu.edu/gbn/vol9/iss1/2 This Article is brought to you for free and open access by the Western North American Naturalist Publications at BYU ScholarsArchive. It has been accepted for inclusion in Great Basin Naturalist by an authorized editor of BYU ScholarsArchive. For more information, please contact [email protected], [email protected]. 1)ii'ti^:rous predators of the mosquito in utah and wyoming FRED C. HARMSTOX, S. A. Sanitarian (R) United States Public Healtli Service The brackish marshes bordering the Great Salt Lake are proUtic mosquito breeding areas ; they also are the habitat of predaceous tiies which find a plentiful source of food in the mosquito larvae and pupae that become stranded in shallow water and mud during the dry periods of late spring and early summer. Inspections conducted in this area during May and June of 1945 and 1946 afforded the writer several opportunities to observe five species of predaceous flies vvhich were preying on moscjuito larvae and pupae. The observations were made at a time when the marginal areas of the extensive marshland were rapidly drying out. resulting in a heavy concentration of larvae and pupae in the shallow water of nu- merous pools. -
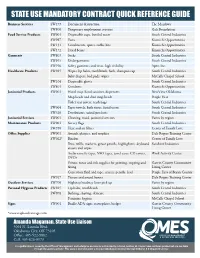
State Use Mandatory Contract Quick Reference Guide
STATE USE MANDATORY CONTRACT QUICK REFERENCE GUIDE Business Services SW177 Document destruction The Meadows SW800 Temporary employment services Galt Foundation Food Service Products SW001 Disposable cups, bottled water South Central Industries SW097 Pasta Kiamichi Opportunities SW131 Condiments, spices, coffee kits Kiamichi Opportunities SW172 Dried beans Kiamichi Opportunities Garments SW803 Socks South Central Industries SW915 Undergarments South Central Industries SW916 Safety garments and vests, high visibility Apex, Inc. Healthcare Products SW015 Wipes, lip balm, toothbrush, bath, shampoo cap South Central Industries Baby diapers, bed pads, wipes McCalls Chapel School SW104 Disposable gloves South Central Industries SW801 Condoms Kiamichi Opportunities Janitorial Products SW001 Hand soap, hand sanitizer, dispensers NewView Oklahoma Mop heads and dust mop heads People First Toilet seat covers, trash bags South Central Industries SW064 Paper towels, bath tissue, facial tissue South Central Industries SW320 Deodorizers, urinal products South Central Industries Janitorial Services SW001 Cleaning, maid, janitorial services Varies by region Maintenance Products SW001 Survey flags South Central Industries SW910 Heat and air filters Center of Family Love Office Supplies SW001 Awards, plaques, and trophies Dale Rogers Training Center SW022* Binders Center of Family Love Pens, refills, markers, grease pencils, highlighters, dryboard Sunshine Industries erasers and wipes Audio cassette tapes, VHS tapes, jewel cases, CD covers, Work Activity -

Gang Project Brochure Pg 1 020712
Salt Lake Area Gang Project A Multi-Jurisdictional Gang Intelligence, Suppression, & Diversion Unit Publications: The Project has several brochures available free of charge. These publications Participating Agencies: cover a variety of topics such as graffiti, gang State Agencies: colors, club drugs, and advice for parents. Local Agencies: Utah Dept. of Human Services-- Current gang-related crime statistics and Cottonwood Heights PD Div. of Juvenile Justice Services historical trends in gang violence are also Draper City PD Utah Dept. of Corrections-- available. Granite School District PD Law Enforcement Bureau METRO Midvale City PD Utah Dept. of Public Safety-- GANG State Bureau of Investigation Annual Gang Conference: The Project Murray City PD UNIT Salt Lake County SO provides an annual conference open to service Salt Lake County DA Federal Agencies: providers, law enforcement personnel, and the SHOCAP Bureau of Alcohol, Tobacco, community. This two-day event, held in the South Salt Lake City PD Firearms, and Explosives spring, covers a variety of topics from Street Taylorsville PD United States Attorney’s Office Survival to Gang Prevention Programs for Unified PD United States Marshals Service Schools. Goals and Objectives commands a squad of detectives. The The Salt Lake Area Gang Project was detectives duties include: established to identify, control, and prevent Suppression and street enforcement criminal gang activity in the jurisdictions Follow-up work on gang-related cases covered by the Project and to provide Collecting intelligence through contacts intelligence data and investigative assistance to with gang members law enforcement agencies. The Project also Assisting local agencies with on-going provides youth with information about viable investigations alternatives to gang membership and educates Answering law-enforcement inquiries In an emergency, please dial 911. -

State Abbreviations
State Abbreviations Postal Abbreviations for States/Territories On July 1, 1963, the Post Office Department introduced the five-digit ZIP Code. At the time, 10/1963– 1831 1874 1943 6/1963 present most addressing equipment could accommodate only 23 characters (including spaces) in the Alabama Al. Ala. Ala. ALA AL Alaska -- Alaska Alaska ALSK AK bottom line of the address. To make room for Arizona -- Ariz. Ariz. ARIZ AZ the ZIP Code, state names needed to be Arkansas Ar. T. Ark. Ark. ARK AR abbreviated. The Department provided an initial California -- Cal. Calif. CALIF CA list of abbreviations in June 1963, but many had Colorado -- Colo. Colo. COL CO three or four letters, which was still too long. In Connecticut Ct. Conn. Conn. CONN CT Delaware De. Del. Del. DEL DE October 1963, the Department settled on the District of D. C. D. C. D. C. DC DC current two-letter abbreviations. Since that time, Columbia only one change has been made: in 1969, at the Florida Fl. T. Fla. Fla. FLA FL request of the Canadian postal administration, Georgia Ga. Ga. Ga. GA GA Hawaii -- -- Hawaii HAW HI the abbreviation for Nebraska, originally NB, Idaho -- Idaho Idaho IDA ID was changed to NE, to avoid confusion with Illinois Il. Ill. Ill. ILL IL New Brunswick in Canada. Indiana Ia. Ind. Ind. IND IN Iowa -- Iowa Iowa IOWA IA Kansas -- Kans. Kans. KANS KS A list of state abbreviations since 1831 is Kentucky Ky. Ky. Ky. KY KY provided at right. A more complete list of current Louisiana La. La. -

A Brief History of Utah's Utes
Timponogos - Ute A BRIEF HISTORY OF UTAH’S UTES Deep Creek Mountains - Goshute ANCESTRAL UTE TERRITORY CURRENT UTE RESERVATIONS Ute tradition suggests that the Ute people were brought here from the south in a magic sack carried by Sinauf, a god who was half wolf and half man. Anthropologists argue that the Utes began using the northern Colorado Plateau between one and two thousand years ago. Historically, the Ute people lived in several family groups, or bands, and inhabited 225,000 square miles covering most of Utah, western Colorado, southern Wyoming, and northern Arizona and New Mexico. Each of these bands was independent, but the Ute people were bound by a common language, close trade relationships, intermarriage, temporary military alliances, and important social and religious events. The major event for the Utes was, and still is, the Bear Dance, an annual gathering to celebrate the coming of spring. The Ute people ranged over a wide but well-known area to engage in a sophisticated gather- ing and hunting economy. They gathered seeds, berries, and roots, and hunted deer, rabbits, birds, Monument Valley - Navajo squashes, and potatoes. and fish. Long before white settlers arrived in Utah, many of the Utes raised corn, beans, pumpkins, The introduction of the horse in the 1600s brought major changes to the Ute way of life, although some Ute bands used the horse more than others. The horse allowed the Utes to travel farther and more quickly, and the Utes began to adopt many aspects of Plains Indian culture, living in mobile teepees and hunting buffalo, elk, and deer over long distances. -

Azar V. Azar, 146 N.W.2D 148 (N.D
N.D. Supreme Court Azar v. Azar, 146 N.W.2d 148 (N.D. 1966) Filed Nov. 4, 1966 [Go to Documents] IN THE SUPREME COURT STATE OF NORTH DAKOTA James J. Azar, Plaintiff and Respondent, v. Betty Azar, Defendant and Appellant. Case No. 8257 [146 N.W.2d 149] Syllabus of the Court 1. Extreme cruelty as a ground for divorce is an infliction of grievous bodily injury or grievous mental suffering. Section 14-05-05, N.D.C.C. 2. Whether one party to a divorce action has inflicted grievous mental suffering upon the other is a question of fact to be determined from all the circumstances in the case. 3. Upon a trial de novo on appeal, the findings of fact of the trial judge are entitled to appreciable weight. 4. When a divorce is granted, the trial court has continuing jurisdiction with regard to the custody, care, education, and welfare of the minor children of the marriage. Section 14-05-22, N.D.C.C. 5. In the matter of awarding custody of the children of the parties to an action for divorce, the trial court is vested with a large discretion, and its discretion will ordinarily not be interfered with except for an abuse thereof. 6. In a divorce proceeding the court shall make such equitable distribution of the real and personal property of the parties as may seem just and proper. Section 14-05-24, N.D.C.C. Appeal from a judgment of the District Court of Burleigh County, Honorable C. F. Kelsch, Special Judge. -

The Salvage of the USS Oklahoma & the USS Utah
SALVAGESALVAGE OFOF THETHE BATTLESHIPBATTLESHIP USSUSS OKLAHOMAOKLAHOMA FOLLOWINGFOLLOWING THETHE ATTACKATTACK ONON PEARLPEARL HARBORHARBOR 19421942--4646 The USS Oklahoma was our first battleship equipped with 14-inch rifle main battery Second unit of the Nevada Class, built at Camden, New Jersey in 1914-16. Commissioned in May 1916 The Oklahoma was 583 feet long with a maximum beam of 95 feet. She had a maximum displacement of 27,500 Tons. This shows gunnery training in 1917, during World War I USSUSS OklahomaOklahoma - -The Oklahoma was extensively modernized in 1927-29 to make her less vulnerable to air and torpedo attack -In July 1936, she was dispatched to Europe to evacuate US citizens during the Spanish Civil War AttackAttack onon PearlPearl HarborHarbor Japanese torpedo exploding against hull of the Oklahoma The Oklahoma’s berth provided the clearest approach path for Japanese torpedo bombers along battleship row ATTACKATTACK ONON BATTLESHIPBATTLESHIP ROWROW TheThe OklahomaOklahoma waswas hithit byby 99 torpedoestorpedoes becausebecause ofof herher positionposition oppositeopposite thethe innerinner harbor,harbor, whichwhich allowedallowed JapaneseJapanese bombersbombers aa clearclear approachapproach pathpath Each torpedo struck the Oklahoma’s port side at higher levels because the ship began listing soon after the first torpedo detonated. This plot was assembled by John F. DeVirgilio (1991). Capsized hull of the Oklahoma outboard of the battleship Maryland, which received almost no damage Damage Assessment: Aerial view of -

Summary of State Child Access Prevention Laws
SUMMARY OF STATE CHILD ACCESS PREVENTION LAWS States with Child Access Prevention Laws California Colorado Connecticut Delaware District of Columbia Florida Georgia Hawaii Illinois Indiana Iowa Kentucky Maryland Massachusetts Minnesota Mississippi Missouri Nevada New Hampshire New Jersey North Carolina Oklahoma Rhode Island Tennessee Texas Utah Virginia Wisconsin State Laws Based on Negligent Storage California Connecticut Florida Hawaii Illinois Iowa Maryland Massachusetts Minnesota New Hampshire New Jersey North Carolina Rhode Island Texas States Imposing Criminal Liability for Allowing a Child to Gain Access to the Firearm, Regardless of Whether the Child Uses the Firearm or Causes Injury Hawaii Maryland Massachusetts Minnesota New Jersey Texas States Imposing Criminal Liability Only if a Child Uses or Possesses the Firearm California Connecticut Florida Illinois Iowa New Hampshire North Carolina Rhode Island States Imposing Criminal Liability for Negligent Storage of Unloaded Firearms California Hawaii Massachusetts State Laws Prohibiting Intentional, Knowing or Reckless Provision of Firearms to Minors Colorado Delaware Georgia Indiana Kentucky Mississippi Missouri Nevada Oklahoma Tennessee Utah Virginia Wisconsin Description of State Child Access Prevention Laws The majority of states have laws designed to prevent children from accessing firearms. The strongest laws impose criminal liability when a minor gains access to a negligently stored firearm. The weakest prohibit persons from directly providing a firearm to a minor. There is a wide range of laws that fall somewhere between these extremes, including laws that impose criminal liability for negligently stored firearms, but only where the child uses the firearm and causes death or serious injury. Weaker laws impose liability only in the event of reckless, knowing or intentional conduct by the adult. -

List of Surrounding States *For Those Chapters That Are Made up of More Than One State We Will Submit Education to the States and Surround States of the Chapter
List of Surrounding States *For those Chapters that are made up of more than one state we will submit education to the states and surround states of the Chapter. Hawaii accepts credit for education if approved in state in which class is being held Accepts credit for education if approved in state in which class is being held Virginia will accept Continuing Education hours without prior approval. All Qualifying Education must be approved by them. Offering In Will submit to Alaska Alabama Florida Georgia Mississippi South Carolina Texas Arkansas Kansas Louisiana Missouri Mississippi Oklahoma Tennessee Texas Arizona California Colorado New Mexico Nevada Utah California Arizona Nevada Oregon Colorado Arizona Kansas Nebraska New Mexico Oklahoma Texas Utah Wyoming Connecticut Massachusetts New Jersey New York Rhode Island District of Columbia Delaware Maryland Pennsylvania Virginia West Virginia Delaware District of Columbia Maryland New Jersey Pennsylvania Florida Alabama Georgia Georgia Alabama Florida North Carolina South Carolina Tennessee Hawaii Iowa Illinois Missouri Minnesota Nebraska South Dakota Wisconsin Idaho Montana Nevada Oregon Utah Washington Wyoming Illinois Illinois Indiana Kentucky Michigan Missouri Tennessee Wisconsin Indiana Illinois Kentucky Michigan Ohio Wisconsin Kansas Colorado Missouri Nebraska Oklahoma Kentucky Illinois Indiana Missouri Ohio Tennessee Virginia West Virginia Louisiana Arkansas Mississippi Texas Massachusetts Connecticut Maine New Hampshire New York Rhode Island Vermont Maryland Delaware District of Columbia -

Grand Circle
Salt Lake City Green River - Moab Salt Lake City - Green River 60min (56mile) Grand Junction 180min (183mile) Colorado Crescent Jct. NM Great Basin Green River NP Arches NP Moab - Arches Goblin Valley 10min (5mile) SP Corona Arch Moab Grand Circle Map Capitol Reef - Green River Dead Horse Point 100min (90mile) SP Moab - Grand View Point NP: National Park 80min (45mile) NM: National Monument NHP: National Histrocal Park Bryce Canyon - Capitol Reef Canyonlands SP: State Park Capitol Reef COLORADO 170min (123mile) NP NP Moab - Mesa Verde Monticello Moab - Monument Valley 170min (140mile) NEVADA UTAH 170min (149mile) Bryce Cedar City Canyon NP Natural Bridges Canyon of the Cedar Breaks NM Blanding Ancients NM Mesa Verde - Monument Valley NM Kodacrome Basin SP 200min (150mile) Valley of Hovenweep 40min 70min NM Cortez (24mile) (60mile) Grand Staircase- the Gods 100min Escalante NM Durango Mt. Carmel (92mile) Muley Point Snow Canyon Jct. SP Goosenecks SP Zion NP Kanab Lake Powell Mexican Hat Mesa Verde Rainbow Monument Valley NP Coral Pink Sand Vermillion Page Bridge NM Four Corners Las Vegas - Zion Dunes SP Cliffs NM Navajo Tribal Park Aztec Ruins NM 170min (167mile) Antelope Pipe Spring NM Horseshoe Shiprock Aztec Bend Canyon Mesa Verde - Chinle 200min (166mile) Mt.Carmel Jct. - North Rim Navajo NM 140min (98mile) Kayenta Farmington Monument Valley - Chinle Mesa Verde - Chaco Culture Valley of Fire Page - North Rim Page - Cameron Page - Monument Valley 140min (134mile) 230min (160mile) SP 170min (124mile) 90min (83mile) Grand Canyon- 130min -

By Handcart to Utah: the Account of C C a Christensen
Nebraska History posts materials online for your personal use. Please remember that the contents of Nebraska History are copyrighted by the Nebraska State Historical Society (except for materials credited to other institutions). The NSHS retains its copyrights even to materials it posts on the web. For permission to re-use materials or for photo ordering information, please see: http://www.nebraskahistory.org/magazine/permission.htm Nebraska State Historical Society members receive four issues of Nebraska History and four issues of Nebraska History News annually. For membership information, see: http://nebraskahistory.org/admin/members/index.htm Article Title: By Handcart to Utah: The Account of C C A Christensen Full Citation: Richard L Jensen, translator, “By Handcart to Utah: The Account of C C A Christensen,” Nebraska History 66 (1985): 332-348 URL of article: http://www.nebraskahistory.org/publish/publicat/history/full-text/NH1985Handcart.pdf Date: 3/04/2014 Article Summary: In journal entries and pictures Christensen recorded his family’s difficult 1857 trip to Salt Lake City. His account provides rare, detailed vignettes of the travelers’ life on the way west. Cataloging Information: Names: Carl Christian Anton Christensen, Carl Christian Nikolai Dorius, Johan Frederik Ferdinand Dorius, Orson Pratt, James P Park, Christian Christiansen, Brigham Young Place Names: Iowa City, Iowa; Florence, Nebraska Keywords: Carl Christian Anton Christensen, Latter-day Saints, Perpetual Emigrating Fund, handcart Photographs / Images: C C A Christensen about 1867; Christensen paintings: “Handcart Pioneers Coming Through the Mountains” and “Handcart Pioneer’s First View of the Salt Lake Valley” C. C. A. Christensen, about 1867. Courtesy of Historical Department, Church of Jesus Christ of Latter-day Saints.