The Genetic Determinants of Cerebral Palsy
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Core Transcriptional Regulatory Circuitries in Cancer
Oncogene (2020) 39:6633–6646 https://doi.org/10.1038/s41388-020-01459-w REVIEW ARTICLE Core transcriptional regulatory circuitries in cancer 1 1,2,3 1 2 1,4,5 Ye Chen ● Liang Xu ● Ruby Yu-Tong Lin ● Markus Müschen ● H. Phillip Koeffler Received: 14 June 2020 / Revised: 30 August 2020 / Accepted: 4 September 2020 / Published online: 17 September 2020 © The Author(s) 2020. This article is published with open access Abstract Transcription factors (TFs) coordinate the on-and-off states of gene expression typically in a combinatorial fashion. Studies from embryonic stem cells and other cell types have revealed that a clique of self-regulated core TFs control cell identity and cell state. These core TFs form interconnected feed-forward transcriptional loops to establish and reinforce the cell-type- specific gene-expression program; the ensemble of core TFs and their regulatory loops constitutes core transcriptional regulatory circuitry (CRC). Here, we summarize recent progress in computational reconstitution and biologic exploration of CRCs across various human malignancies, and consolidate the strategy and methodology for CRC discovery. We also discuss the genetic basis and therapeutic vulnerability of CRC, and highlight new frontiers and future efforts for the study of CRC in cancer. Knowledge of CRC in cancer is fundamental to understanding cancer-specific transcriptional addiction, and should provide important insight to both pathobiology and therapeutics. 1234567890();,: 1234567890();,: Introduction genes. Till now, one critical goal in biology remains to understand the composition and hierarchy of transcriptional Transcriptional regulation is one of the fundamental mole- regulatory network in each specified cell type/lineage. -

Further Delineation of Chromosomal Consensus Regions in Primary
Leukemia (2007) 21, 2463–2469 & 2007 Nature Publishing Group All rights reserved 0887-6924/07 $30.00 www.nature.com/leu ORIGINAL ARTICLE Further delineation of chromosomal consensus regions in primary mediastinal B-cell lymphomas: an analysis of 37 tumor samples using high-resolution genomic profiling (array-CGH) S Wessendorf1,6, TFE Barth2,6, A Viardot1, A Mueller3, HA Kestler3, H Kohlhammer1, P Lichter4, M Bentz5,HDo¨hner1,PMo¨ller2 and C Schwaenen1 1Klinik fu¨r Innere Medizin III, Zentrum fu¨r Innere Medizin der Universita¨t Ulm, Ulm, Germany; 2Institut fu¨r Pathologie, Universita¨t Ulm, Ulm, Germany; 3Forschungsdozentur Bioinformatik, Universita¨t Ulm, Ulm, Germany; 4Abt. Molekulare Genetik, Deutsches Krebsforschungszentrum, Heidelberg, Germany and 5Sta¨dtisches Klinikum Karlsruhe, Karlsruhe, Germany Primary mediastinal B-cell lymphoma (PMBL) is an aggressive the expression of BSAP, BOB1, OCT2, PAX5 and PU1 was extranodal B-cell non-Hodgkin’s lymphoma with specific clin- added to the spectrum typical of PMBL features.9 ical, histopathological and genomic features. To characterize Genetically, a pattern of highly recurrent karyotype alterations further the genotype of PMBL, we analyzed 37 tumor samples and PMBL cell lines Med-B1 and Karpas1106P using array- with the hallmark of chromosomal gains of the subtelomeric based comparative genomic hybridization (matrix- or array- region of chromosome 9 supported the concept of a unique CGH) to a 2.8k genomic microarray. Due to a higher genomic disease entity that distinguishes PMBL from other B-cell non- resolution, we identified altered chromosomal regions in much Hodgkin’s lymphomas.10,11 Together with less specific gains on higher frequencies compared with standard CGH: for example, 2p15 and frequent mutations of the SOCS1 gene, a notable þ 9p24 (68%), þ 2p15 (51%), þ 7q22 (32%), þ 9q34 (32%), genomic similarity to classical Hodgkin’s lymphoma was þ 11q23 (18%), þ 12q (30%) and þ 18q21 (24%). -

RFX2 Antibody Cat
RFX2 Antibody Cat. No.: 25-404 RFX2 Antibody Specifications HOST SPECIES: Rabbit SPECIES REACTIVITY: Human Antibody produced in rabbits immunized with a synthetic peptide corresponding a region IMMUNOGEN: of human RFX2. TESTED APPLICATIONS: ELISA, WB RFX2 antibody can be used for detection of RFX2 by ELISA at 1:1562500. RFX2 antibody APPLICATIONS: can be used for detection of RFX2 by western blot at 1 μg/mL, and HRP conjugated secondary antibody should be diluted 1:50,000 - 100,000. POSITIVE CONTROL: 1) 721_B Cell Lysate PREDICTED MOLECULAR 80 kDa WEIGHT: Properties PURIFICATION: Antibody is purified by peptide affinity chromatography method. CLONALITY: Polyclonal CONJUGATE: Unconjugated PHYSICAL STATE: Liquid September 30, 2021 1 https://www.prosci-inc.com/rfx2-antibody-25-404.html Purified antibody supplied in 1x PBS buffer with 0.09% (w/v) sodium azide and 2% BUFFER: sucrose. CONCENTRATION: batch dependent For short periods of storage (days) store at 4˚C. For longer periods of storage, store RFX2 STORAGE CONDITIONS: antibody at -20˚C. As with any antibody avoid repeat freeze-thaw cycles. Additional Info OFFICIAL SYMBOL: RFX2 ALTERNATE NAMES: RFX2, FLJ14226, ACCESSION NO.: NP_000626 PROTEIN GI NO.: 19743881 GENE ID: 5990 USER NOTE: Optimal dilutions for each application to be determined by the researcher. Background and References RFX2 is a member of transcription factors that contain a highly-conserved winged helix DNA binding domain. RFX2 is structurally related to regulatory factors X1, X3, X4, and X5. It is a transcriptional activator that can bind DNA as a monomer or as a heterodimer with other RFX family members. This protein can bind to cis elements in the promoter of the IL-5 receptor alpha gene.This gene is a member of the regulatory factor X gene family, which encodes transcription factors that contain a highly-conserved winged helix DNA BACKGROUND: binding domain. -

Targeted Resequencing Identifies Genes with Recurrent Variation In
www.nature.com/npjgenmed ARTICLE OPEN Targeted resequencing identifies genes with recurrent variation in cerebral palsy C. L. van Eyk 1,2, M. A. Corbett 1,2, M. S. B. Frank 1,2, D. L. Webber1,2, M. Newman3, J. G. Berry 1,2, K. Harper1,2, B. P. Haines1,2, G. McMichael1,2, J. A. Woenig1,2, A. H. MacLennan1,2 and J. Gecz 1,2,4* A growing body of evidence points to a considerable and heterogeneous genetic aetiology of cerebral palsy (CP). To identify recurrently variant CP genes, we designed a custom gene panel of 112 candidate genes. We tested 366 clinically unselected singleton cases with CP, including 271 cases not previously examined using next-generation sequencing technologies. Overall, 5.2% of the naïve cases (14/271) harboured a genetic variant of clinical significance in a known disease gene, with a further 4.8% of individuals (13/271) having a variant in a candidate gene classified as intolerant to variation. In the aggregate cohort of individuals from this study and our previous genomic investigations, six recurrently hit genes contributed at least 4% of disease burden to CP: COL4A1, TUBA1A, AGAP1, L1CAM, MAOB and KIF1A. Significance of Rare VAriants (SORVA) burden analysis identified four genes with a genome-wide significant burden of variants, AGAP1, ERLIN1, ZDHHC9 and PROC, of which we functionally assessed AGAP1 using a zebrafish model. Our investigations reinforce that CP is a heterogeneous neurodevelopmental disorder with known as well as novel genetic determinants. npj Genomic Medicine (2019) ; https://doi.org/10.1038/s41525-019-0101-z4:27 1234567890():,; INTRODUCTION is likely also due in part to the stringent criteria used to select Cerebral palsy (CP) is the most common motor disability of causative variants. -

Molecular Effects of Isoflavone Supplementation Human Intervention Studies and Quantitative Models for Risk Assessment
Molecular effects of isoflavone supplementation Human intervention studies and quantitative models for risk assessment Vera van der Velpen Thesis committee Promotors Prof. Dr Pieter van ‘t Veer Professor of Nutritional Epidemiology Wageningen University Prof. Dr Evert G. Schouten Emeritus Professor of Epidemiology and Prevention Wageningen University Co-promotors Dr Anouk Geelen Assistant professor, Division of Human Nutrition Wageningen University Dr Lydia A. Afman Assistant professor, Division of Human Nutrition Wageningen University Other members Prof. Dr Jaap Keijer, Wageningen University Dr Hubert P.J.M. Noteborn, Netherlands Food en Consumer Product Safety Authority Prof. Dr Yvonne T. van der Schouw, UMC Utrecht Dr Wendy L. Hall, King’s College London This research was conducted under the auspices of the Graduate School VLAG (Advanced studies in Food Technology, Agrobiotechnology, Nutrition and Health Sciences). Molecular effects of isoflavone supplementation Human intervention studies and quantitative models for risk assessment Vera van der Velpen Thesis submitted in fulfilment of the requirements for the degree of doctor at Wageningen University by the authority of the Rector Magnificus Prof. Dr M.J. Kropff, in the presence of the Thesis Committee appointed by the Academic Board to be defended in public on Friday 20 June 2014 at 13.30 p.m. in the Aula. Vera van der Velpen Molecular effects of isoflavone supplementation: Human intervention studies and quantitative models for risk assessment 154 pages PhD thesis, Wageningen University, Wageningen, NL (2014) With references, with summaries in Dutch and English ISBN: 978-94-6173-952-0 ABSTRact Background: Risk assessment can potentially be improved by closely linked experiments in the disciplines of epidemiology and toxicology. -

Dedifferentiation and Neuronal Repression Define Familial Alzheimer’S Disease Andrew B
bioRxiv preprint doi: https://doi.org/10.1101/531202; this version posted November 18, 2019. The copyright holder for this preprint (which was not certified by peer review) is the author/funder, who has granted bioRxiv a license to display the preprint in perpetuity. It is made available under aCC-BY-NC-ND 4.0 International licenseCaldwell. et al. BIORXIV/2019/531202 Dedifferentiation and neuronal repression define Familial Alzheimer’s Disease Andrew B. Caldwell1, Qing Liu2, Gary P. Schroth3, Douglas R. Galasko2, Shauna H. Yuan2,8, Steven L. Wagner2,4, & Shankar Subramaniam1,5,6,7* Affiliations 1Department of Bioengineering, University of California, San Diego, La Jolla, CA, USA. 2Department of Neurosciences, University of California, San Diego, La Jolla, CA, USA. 3Illumina, Inc., San Diego, CA, USA. 4VA San Diego Healthcare System, La Jolla, CA, USA. 5Department of Cellular and Molecular Medicine, University of California, San Diego, La Jolla, CA, USA. 6Department of Nanoengineering, University of California, San Diego, La Jolla, CA, USA. 7Department of Computer Science and Engineering, University of California, San Diego, La Jolla, CA, USA. 8Present Address: N. Bud Grossman Center for Memory Research and Care, Department of Neurology, University of Minnesota, Minneapolis, MN, USA; GRECC, Minneapolis VA Health Care System, Minneapolis, MN, USA. *Correspondence: Correspondence and requests for materials should be addressed to S.S. ([email protected]). Abstract Early-Onset Familial Alzheimer’s Disease (EOFAD) is a dominantly inherited neurodegenerative disorder elicited by over 300 mutations in the PSEN1, PSEN2, and APP genes1. Hallmark pathological changes and symptoms observed, namely the accumulation of misfolded Amyloid-β (Aβ) in plaques and Tau aggregates in neurofibrillary tangles associated with memory loss and cognitive decline, are understood to be temporally accelerated manifestations of the more common sporadic Late-Onset Alzheimer’s Disease. -

KANK1 Antibody (N-Terminus) Rabbit Polyclonal Antibody Catalog # ALS16019
10320 Camino Santa Fe, Suite G San Diego, CA 92121 Tel: 858.875.1900 Fax: 858.622.0609 KANK1 Antibody (N-Terminus) Rabbit Polyclonal Antibody Catalog # ALS16019 Specification KANK1 Antibody (N-Terminus) - Product Information Application IF, IHC Primary Accession Q14678 Reactivity Human, Mouse Host Rabbit Clonality Polyclonal Calculated MW 147kDa KDa KANK1 Antibody (N-Terminus) - Additional Information Gene ID 23189 Immunofluorescence of KANK1 in human Other Names kidney tissue with KANK1 antibody at 20 KN motif and ankyrin repeat ug/ml. domain-containing protein 1, Ankyrin repeat domain-containing protein 15, Kidney ankyrin repeat-containing protein, KANK1, ANKRD15, KANK, KIAA0172 Target/Specificity Two alternatively spliced transcript variants encoding different isoforms have been identified. The lower molecular weight band seen in the immunoblot is thought to be non-specific. Reconstitution & Storage Long term: -20°C; Short term: +4°C. Avoid repeat freeze-thaw cycles. Anti-KANK1 antibody IHC staining of human kidney. Precautions KANK1 Antibody (N-Terminus) is for research use only and not for use in KANK1 Antibody (N-Terminus) - diagnostic or therapeutic procedures. Background Involved in the control of cytoskeleton KANK1 Antibody (N-Terminus) - Protein formation by regulating actin polymerization. Information Inhibits actin fiber formation and cell migration. Inhibits RhoA activity; the function Name KANK1 involves phosphorylation through PI3K/Akt signaling and may depend on the competetive Synonyms ANKRD15, KANK, KIAA0172 interaction with 14-3-3 adapter proteins to sequester them from active complexes. Function Inhibits the formation of lamellipodia but not of Page 1/3 10320 Camino Santa Fe, Suite G San Diego, CA 92121 Tel: 858.875.1900 Fax: 858.622.0609 Involved in the control of cytoskeleton filopodia; the function may depend on the formation by regulating actin competetive interaction with BAIAP2 to block polymerization. -
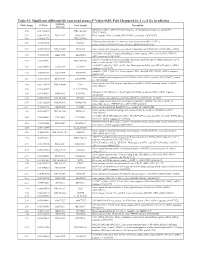
(P -Value<0.05, Fold Change≥1.4), 4 Vs. 0 Gy Irradiation
Table S1: Significant differentially expressed genes (P -Value<0.05, Fold Change≥1.4), 4 vs. 0 Gy irradiation Genbank Fold Change P -Value Gene Symbol Description Accession Q9F8M7_CARHY (Q9F8M7) DTDP-glucose 4,6-dehydratase (Fragment), partial (9%) 6.70 0.017399678 THC2699065 [THC2719287] 5.53 0.003379195 BC013657 BC013657 Homo sapiens cDNA clone IMAGE:4152983, partial cds. [BC013657] 5.10 0.024641735 THC2750781 Ciliary dynein heavy chain 5 (Axonemal beta dynein heavy chain 5) (HL1). 4.07 0.04353262 DNAH5 [Source:Uniprot/SWISSPROT;Acc:Q8TE73] [ENST00000382416] 3.81 0.002855909 NM_145263 SPATA18 Homo sapiens spermatogenesis associated 18 homolog (rat) (SPATA18), mRNA [NM_145263] AA418814 zw01a02.s1 Soares_NhHMPu_S1 Homo sapiens cDNA clone IMAGE:767978 3', 3.69 0.03203913 AA418814 AA418814 mRNA sequence [AA418814] AL356953 leucine-rich repeat-containing G protein-coupled receptor 6 {Homo sapiens} (exp=0; 3.63 0.0277936 THC2705989 wgp=1; cg=0), partial (4%) [THC2752981] AA484677 ne64a07.s1 NCI_CGAP_Alv1 Homo sapiens cDNA clone IMAGE:909012, mRNA 3.63 0.027098073 AA484677 AA484677 sequence [AA484677] oe06h09.s1 NCI_CGAP_Ov2 Homo sapiens cDNA clone IMAGE:1385153, mRNA sequence 3.48 0.04468495 AA837799 AA837799 [AA837799] Homo sapiens hypothetical protein LOC340109, mRNA (cDNA clone IMAGE:5578073), partial 3.27 0.031178378 BC039509 LOC643401 cds. [BC039509] Homo sapiens Fas (TNF receptor superfamily, member 6) (FAS), transcript variant 1, mRNA 3.24 0.022156298 NM_000043 FAS [NM_000043] 3.20 0.021043295 A_32_P125056 BF803942 CM2-CI0135-021100-477-g08 CI0135 Homo sapiens cDNA, mRNA sequence 3.04 0.043389246 BF803942 BF803942 [BF803942] 3.03 0.002430239 NM_015920 RPS27L Homo sapiens ribosomal protein S27-like (RPS27L), mRNA [NM_015920] Homo sapiens tumor necrosis factor receptor superfamily, member 10c, decoy without an 2.98 0.021202829 NM_003841 TNFRSF10C intracellular domain (TNFRSF10C), mRNA [NM_003841] 2.97 0.03243901 AB002384 C6orf32 Homo sapiens mRNA for KIAA0386 gene, partial cds. -
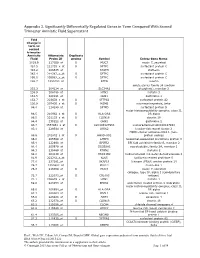
Appendix 2. Significantly Differentially Regulated Genes in Term Compared with Second Trimester Amniotic Fluid Supernatant
Appendix 2. Significantly Differentially Regulated Genes in Term Compared With Second Trimester Amniotic Fluid Supernatant Fold Change in term vs second trimester Amniotic Affymetrix Duplicate Fluid Probe ID probes Symbol Entrez Gene Name 1019.9 217059_at D MUC7 mucin 7, secreted 424.5 211735_x_at D SFTPC surfactant protein C 416.2 206835_at STATH statherin 363.4 214387_x_at D SFTPC surfactant protein C 295.5 205982_x_at D SFTPC surfactant protein C 288.7 1553454_at RPTN repetin solute carrier family 34 (sodium 251.3 204124_at SLC34A2 phosphate), member 2 238.9 206786_at HTN3 histatin 3 161.5 220191_at GKN1 gastrokine 1 152.7 223678_s_at D SFTPA2 surfactant protein A2 130.9 207430_s_at D MSMB microseminoprotein, beta- 99.0 214199_at SFTPD surfactant protein D major histocompatibility complex, class II, 96.5 210982_s_at D HLA-DRA DR alpha 96.5 221133_s_at D CLDN18 claudin 18 94.4 238222_at GKN2 gastrokine 2 93.7 1557961_s_at D LOC100127983 uncharacterized LOC100127983 93.1 229584_at LRRK2 leucine-rich repeat kinase 2 HOXD cluster antisense RNA 1 (non- 88.6 242042_s_at D HOXD-AS1 protein coding) 86.0 205569_at LAMP3 lysosomal-associated membrane protein 3 85.4 232698_at BPIFB2 BPI fold containing family B, member 2 84.4 205979_at SCGB2A1 secretoglobin, family 2A, member 1 84.3 230469_at RTKN2 rhotekin 2 82.2 204130_at HSD11B2 hydroxysteroid (11-beta) dehydrogenase 2 81.9 222242_s_at KLK5 kallikrein-related peptidase 5 77.0 237281_at AKAP14 A kinase (PRKA) anchor protein 14 76.7 1553602_at MUCL1 mucin-like 1 76.3 216359_at D MUC7 mucin 7, -

EGR1 and FOSB Gene Expressions in Cancer Stroma Are Independent Prognostic Indicators for Epithelial Ovarian Cancer Receiving Standard Therapy
GENES, CHROMOSOMES & CANCER 51:300–312 (2012) EGR1 and FOSB Gene Expressions in Cancer Stroma Are Independent Prognostic Indicators for Epithelial Ovarian Cancer Receiving Standard Therapy Fumio Kataoka,1 Hiroshi Tsuda,1* Tokuzo Arao,2 Sadako Nishimura,3 Hideo Tanaka,1 Hiroyuki Nomura,1 Tatsuyuki Chiyoda,1 Akira Hirasawa,1 Tomoko Akahane,1 Hiroshi Nishio,1 Kazuto Nishio,2 and Daisuke Aoki1 1Departmentof Obstetrics and Gynecology,School of Medicine,Keio University,Tokyo,Japan 2Departmentof Genome Biology,Kinki University School of Medicine,Osaka,Japan 3Departmentof Obstetrics and Gynecology,Osaka City General Hospital,Osaka,Japan Stromal components interact with cancer cells to promote growth and metastasis. The purpose of this study was to iden- tify genes expressed in stroma, which could provide prognostic information in epithelial ovarian cancer (EOC). Seventy- four patients were included. We performed gene expression profiling and confirmed array data using RT-PCR and immuno- histochemistry. By microarray analysis, 52 candidate genes associated with progression free survival (PFS) were identified (P < 0.005). Expression of the early growth response 1 (EGR1) and FBJ murine osteosarcoma viral oncogene homolog B (FOSB) genes was further analyzed. Array data were confirmed by RT-PCR and multivariate analysis demonstrated that both EGR1 and FOSB expression in cancer stroma, and EGR1 expression in cancer are independent prognostic factors in EOC. Immunohistochemically, EGR1 protein is localized in cancer cells and a-smooth muscle actin positive stromal fibro- blasts. The EGR1 and FOSB expression in stromal cells and EGR1 expression in cancer cells are prognostic indicators in EOC. VC 2011 Wiley Periodicals, Inc. INTRODUCTION ior, including invasion or metastasis and response Epithelial ovarian cancer (EOC) is a common to therapy (Bhowmick and Moses, 2005; Kim et al., cause of cancer death in women. -

Role and Regulation of the P53-Homolog P73 in the Transformation of Normal Human Fibroblasts
Role and regulation of the p53-homolog p73 in the transformation of normal human fibroblasts Dissertation zur Erlangung des naturwissenschaftlichen Doktorgrades der Bayerischen Julius-Maximilians-Universität Würzburg vorgelegt von Lars Hofmann aus Aschaffenburg Würzburg 2007 Eingereicht am Mitglieder der Promotionskommission: Vorsitzender: Prof. Dr. Dr. Martin J. Müller Gutachter: Prof. Dr. Michael P. Schön Gutachter : Prof. Dr. Georg Krohne Tag des Promotionskolloquiums: Doktorurkunde ausgehändigt am Erklärung Hiermit erkläre ich, dass ich die vorliegende Arbeit selbständig angefertigt und keine anderen als die angegebenen Hilfsmittel und Quellen verwendet habe. Diese Arbeit wurde weder in gleicher noch in ähnlicher Form in einem anderen Prüfungsverfahren vorgelegt. Ich habe früher, außer den mit dem Zulassungsgesuch urkundlichen Graden, keine weiteren akademischen Grade erworben und zu erwerben gesucht. Würzburg, Lars Hofmann Content SUMMARY ................................................................................................................ IV ZUSAMMENFASSUNG ............................................................................................. V 1. INTRODUCTION ................................................................................................. 1 1.1. Molecular basics of cancer .......................................................................................... 1 1.2. Early research on tumorigenesis ................................................................................. 3 1.3. Developing -

Stroke Genetics and Genomics
Faculdade de Medicina da Universidade de Lisboa Unidade Neurológica de Investigação Clínica PhD Thesis Stroke Genetics and Genomics Tiago Krug Coelho Host Institution: Instituto Gulbenkian de Ciência Supervisor at Instituto Gulbenkian de Ciência: Doctor Sofia Oliveira Supervisor at Faculdade de Medicina da Universidade de Lisboa: Professor José Ferro PhD in Biomedical Sciences Specialization in Neurosciences 2010 Stroke Genetics and Genomics A ciência tem, de facto, um único objectivo: a verdade. Não esgota perfeitamente a sua tarefa se não descobre a causa do todo. Chiara Lubich i Stroke Genetics and Genomics ii Stroke Genetics and Genomics A impressão desta dissertação foi aprovada pela Comissão Coordenadora do Conselho Científico da Faculdade de Medicina de Lisboa em reunião de 28 de Setembro de 2010. iii Stroke Genetics and Genomics iv Stroke Genetics and Genomics As opiniões expressas são da exclusiva responsabilidade do seu autor. v Stroke Genetics and Genomics vi Stroke Genetics and Genomics Abstract ABSTRACT This project presents a comprehensive approach to the identification of new genes that influence the risk for developing stroke. Stroke is the leading cause of death in Portugal and the third leading cause of death in the developed world. It is even more disabling than lethal, and the persistent neurological impairment and physical disability caused by stroke have a very high socioeconomic cost. Moreover, the number of affected individuals is expected to increase with the current aging of the population. Stroke is a “brain attack” cutting off vital blood and oxygen to the brain cells and it is a complex disease resulting from environmental and genetic factors.