Multiple Sclerosis Associates with LILRA3 Deletion in Spanish Patients
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Human and Mouse CD Marker Handbook Human and Mouse CD Marker Key Markers - Human Key Markers - Mouse
Welcome to More Choice CD Marker Handbook For more information, please visit: Human bdbiosciences.com/eu/go/humancdmarkers Mouse bdbiosciences.com/eu/go/mousecdmarkers Human and Mouse CD Marker Handbook Human and Mouse CD Marker Key Markers - Human Key Markers - Mouse CD3 CD3 CD (cluster of differentiation) molecules are cell surface markers T Cell CD4 CD4 useful for the identification and characterization of leukocytes. The CD CD8 CD8 nomenclature was developed and is maintained through the HLDA (Human Leukocyte Differentiation Antigens) workshop started in 1982. CD45R/B220 CD19 CD19 The goal is to provide standardization of monoclonal antibodies to B Cell CD20 CD22 (B cell activation marker) human antigens across laboratories. To characterize or “workshop” the antibodies, multiple laboratories carry out blind analyses of antibodies. These results independently validate antibody specificity. CD11c CD11c Dendritic Cell CD123 CD123 While the CD nomenclature has been developed for use with human antigens, it is applied to corresponding mouse antigens as well as antigens from other species. However, the mouse and other species NK Cell CD56 CD335 (NKp46) antibodies are not tested by HLDA. Human CD markers were reviewed by the HLDA. New CD markers Stem Cell/ CD34 CD34 were established at the HLDA9 meeting held in Barcelona in 2010. For Precursor hematopoetic stem cell only hematopoetic stem cell only additional information and CD markers please visit www.hcdm.org. Macrophage/ CD14 CD11b/ Mac-1 Monocyte CD33 Ly-71 (F4/80) CD66b Granulocyte CD66b Gr-1/Ly6G Ly6C CD41 CD41 CD61 (Integrin b3) CD61 Platelet CD9 CD62 CD62P (activated platelets) CD235a CD235a Erythrocyte Ter-119 CD146 MECA-32 CD106 CD146 Endothelial Cell CD31 CD62E (activated endothelial cells) Epithelial Cell CD236 CD326 (EPCAM1) For Research Use Only. -

Proteomic and Functional Characterisation of LILRA3: Role In
Proteomic and Functional Characterisation of LILRA3: Role in Inflammation Terry Hung-Yi Lee A thesis submitted in fulfilment of the requirements for the degree of Doctor of Philosophy Faculty of Medicine The University of New South Wales 2014 PLEASE TYPE THE UNIVERSITY OF NEW SOUTH WALES Thosis/Dissertatlon Sh09t Surname or Fam1ly name L l .... f.- First name / 'f (Z (1. 1 Other name/s H "'" ~ - \'I Abbre111at1on lor degree as given in the University calendar. Pt> .fh •I "!.1 '.j 17 J/ 0 School f t. t,...., ..> I <>f lVI e.~, u1 f <J t.r-UJ Faculty: M e. o1; c.• " e Tlrte Pr,te.;) ""l(. (j. f' il ,: ..... d .;" "' u"'"r &- d·er;..c&.L J .<\ ~ l/<.tf. Al: ~ " ' ~ ..... , ...., ~~~"""'" " "'~" Abstract 350 word s ma•imum: (PLEASE TYPE) Se e (f'JicJE' -------- Declaration relating to disposition of project thos tsldissortation I hereby grant to the Un1vers1ty of New South Wales or rts agents the nght to areh1ve and to make avatlabte my theSIS or dissertation '" whole or 1n part 1n the University libranes in all forms of media. now or here after known. subject to the provisions of the Copyright Act 1968 I retain all property nghts such as patent nghts I also retain the right to use in future works (such as artldes or bOOks) all or pan of this thesis or dlssenat1on I also authonse Un1vers1ty Microfilms to use the 350 word abstract of my thesis In Dissertation Abstracts International (this is appticable to doctoral ~~· ~l.A I Po .~.. <j 'I fJs JV VJignatur~ J1 Witness Date The Un1vers1ty recogn•ses that there may be exceptional circumstances requinng restrictions on copying or conditions on use. -

Supplementary Table 1: Adhesion Genes Data Set
Supplementary Table 1: Adhesion genes data set PROBE Entrez Gene ID Celera Gene ID Gene_Symbol Gene_Name 160832 1 hCG201364.3 A1BG alpha-1-B glycoprotein 223658 1 hCG201364.3 A1BG alpha-1-B glycoprotein 212988 102 hCG40040.3 ADAM10 ADAM metallopeptidase domain 10 133411 4185 hCG28232.2 ADAM11 ADAM metallopeptidase domain 11 110695 8038 hCG40937.4 ADAM12 ADAM metallopeptidase domain 12 (meltrin alpha) 195222 8038 hCG40937.4 ADAM12 ADAM metallopeptidase domain 12 (meltrin alpha) 165344 8751 hCG20021.3 ADAM15 ADAM metallopeptidase domain 15 (metargidin) 189065 6868 null ADAM17 ADAM metallopeptidase domain 17 (tumor necrosis factor, alpha, converting enzyme) 108119 8728 hCG15398.4 ADAM19 ADAM metallopeptidase domain 19 (meltrin beta) 117763 8748 hCG20675.3 ADAM20 ADAM metallopeptidase domain 20 126448 8747 hCG1785634.2 ADAM21 ADAM metallopeptidase domain 21 208981 8747 hCG1785634.2|hCG2042897 ADAM21 ADAM metallopeptidase domain 21 180903 53616 hCG17212.4 ADAM22 ADAM metallopeptidase domain 22 177272 8745 hCG1811623.1 ADAM23 ADAM metallopeptidase domain 23 102384 10863 hCG1818505.1 ADAM28 ADAM metallopeptidase domain 28 119968 11086 hCG1786734.2 ADAM29 ADAM metallopeptidase domain 29 205542 11085 hCG1997196.1 ADAM30 ADAM metallopeptidase domain 30 148417 80332 hCG39255.4 ADAM33 ADAM metallopeptidase domain 33 140492 8756 hCG1789002.2 ADAM7 ADAM metallopeptidase domain 7 122603 101 hCG1816947.1 ADAM8 ADAM metallopeptidase domain 8 183965 8754 hCG1996391 ADAM9 ADAM metallopeptidase domain 9 (meltrin gamma) 129974 27299 hCG15447.3 ADAMDEC1 ADAM-like, -

Reascreen™ MAX Kit, Human, FFPE, Version 01 Panel Composition – 89 Antibody Conjugates # 130-127-847
REAscreen™ MAX Kit, human, FFPE, version 01 Panel composition – 89 antibody conjugates # 130-127-847 REAscreen MAX Antibody Plate 1 2 3 4 5 6 7 8 9 10 11 12 IRF-7 CD104 CD158i CD181 CD295 A pS477/ SSRP1 CD45RA ZAP70 TTF-1 CD138 Sox2 (Integrin CD162 (KIR2DS4) (CXCR1) (LEPR) pS479 β4) CD134 B CD240DCE IRF-7 CD15 CD43 AN2 Galectin-3 CD66c TOM22 CD147 CD66acde (OX40) Cyto- CD279 CD234 C Syk Slug LRP-4 IgD Vimentin Dectin-1 Galectin-9 keratin CLA (PD1) (DARC) PAX-5 CD195 CD196 CD88 CD305 D FAK pS910 p53 FcεRIα PCNA CD268 BMI-1 (BSAP) (CCR5) (CCR6) (C5AR) (LAIR-1) CD334 CD45R CD226 AKT Pan E PKCα BATF Bcl-2 CD65 CD223 CD52 CD66abce (FGFR4) (B220) (DNAM-1) (PKB) CD182 CD20 CD326 Cyto- Podo- HLA-DR, F Cyto- CD45 MLC2v CD66b Hsp70 CD45RB (CXCR2) plasmic (EpCAM) keratin 8 planin DP, DQ CD235a α-Actinin CD202b CD317 G Dnmt3b Jak1 SUSD2 EZH2 (Glycopho (Sarco- CD79a CD40 CD99 (TIE-2) (BST2) rin A) meric) p120 CD239 CD271 H Catenin CD44 CD57 CD123 Ki-67 CD233 CD45RO β-Catenin CD100 (BCAM) (LNGFR) pS879 Antigen Clone Fluorochrome Antibody type Plate position AKT Pan (PKB) REA676 PE REAfinity™ E11 AN2 REA989 PE REAfinity B6 BATF REA486 FITC REAfinity E2 1 Antigen Clone Fluorochrome Antibody type Plate position Bcl-2 REA872 FITC REAfinity E5 BMI-1 REA438 FITC REAfinity D10 CD100 REA316 FITC REAfinity H11 CD104 (Integrin β4) REA236 FITC REAfinity A10 CD123 REA918 FITC REAfinity H5 CD134 (OX40) ACT35 FITC Hybridoma B1 CD138 44F9 FITC Hybridoma A8 CD147 REA282 FITC REAfinity B10 CD15 VIMC6 FITC Hybridoma B4 CD158i (KIR2DS4) JJC11.6 PE Hybridoma A1 CD162 REA319 -
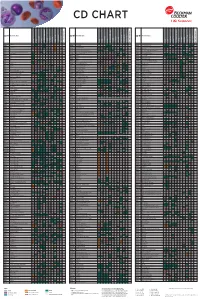
Flow Reagents Single Color Antibodies CD Chart
CD CHART CD N° Alternative Name CD N° Alternative Name CD N° Alternative Name Beckman Coulter Clone Beckman Coulter Clone Beckman Coulter Clone T Cells B Cells Granulocytes NK Cells Macrophages/Monocytes Platelets Erythrocytes Stem Cells Dendritic Cells Endothelial Cells Epithelial Cells T Cells B Cells Granulocytes NK Cells Macrophages/Monocytes Platelets Erythrocytes Stem Cells Dendritic Cells Endothelial Cells Epithelial Cells T Cells B Cells Granulocytes NK Cells Macrophages/Monocytes Platelets Erythrocytes Stem Cells Dendritic Cells Endothelial Cells Epithelial Cells CD1a T6, R4, HTA1 Act p n n p n n S l CD99 MIC2 gene product, E2 p p p CD223 LAG-3 (Lymphocyte activation gene 3) Act n Act p n CD1b R1 Act p n n p n n S CD99R restricted CD99 p p CD224 GGT (γ-glutamyl transferase) p p p p p p CD1c R7, M241 Act S n n p n n S l CD100 SEMA4D (semaphorin 4D) p Low p p p n n CD225 Leu13, interferon induced transmembrane protein 1 (IFITM1). p p p p p CD1d R3 Act S n n Low n n S Intest CD101 V7, P126 Act n p n p n n p CD226 DNAM-1, PTA-1 Act n Act Act Act n p n CD1e R2 n n n n S CD102 ICAM-2 (intercellular adhesion molecule-2) p p n p Folli p CD227 MUC1, mucin 1, episialin, PUM, PEM, EMA, DF3, H23 Act p CD2 T11; Tp50; sheep red blood cell (SRBC) receptor; LFA-2 p S n p n n l CD103 HML-1 (human mucosal lymphocytes antigen 1), integrin aE chain S n n n n n n n l CD228 Melanotransferrin (MT), p97 p p CD3 T3, CD3 complex p n n n n n n n n n l CD104 integrin b4 chain; TSP-1180 n n n n n n n p p CD229 Ly9, T-lymphocyte surface antigen p p n p n -

Snipa Snpcard
SNiPAcard Block annotations Block info genomic range chr19:55,117,749-55,168,602 block size 50,854 bp variant count 74 variants Basic features Conservation/deleteriousness Linked genes μ = -0.557 [-4.065 – AC009892.10 , AC009892.5 , AC009892.9 , AC245036.1 , AC245036.2 , phyloP 2.368] gene(s) hit or close-by AC245036.3 , AC245036.4 , AC245036.5 , AC245036.6 , LILRA1 , LILRB1 , LILRB4 , MIR8061 , VN1R105P phastCons μ = 0.059 [0 – 0.633] eQTL gene(s) CTB-83J4.2 , LILRA1 , LILRA2 , LILRB2 , LILRB5 , LILRP1 μ = -0.651 [-4.69 – 2.07] AC008984.5 , AC008984.5 , AC008984.6 , AC008984.6 , AC008984.7 , AC008984.7 , AC009892.10 , AC009892.10 , AC009892.2 , AC009892.2 , AC009892.5 , AC010518.3 , AC010518.3 , AC011515.2 , AC011515.2 , AC012314.19 , AC012314.19 , FCAR , FCAR , FCAR , FCAR , FCAR , FCAR , FCAR , FCAR , FCAR , FCAR , KIR2DL1 , KIR2DL1 , KIR2DL1 , KIR2DL1 , KIR2DL1 , KIR2DL1 , KIR2DL1 , KIR2DL1 , KIR2DL1 , KIR2DL1 , KIR2DL1 , KIR2DL1 , KIR2DL1 , KIR2DL1 , KIR2DL1 , KIR2DL1 , KIR2DL1 , KIR2DL1 , KIR2DL1 , KIR2DL1 , KIR2DL1 , KIR2DL1 , KIR2DL1 , KIR2DL1 , KIR2DL1 , KIR2DL3 , KIR2DL3 , KIR2DL3 , KIR2DL3 , KIR2DL3 , KIR2DL3 , KIR2DL3 , KIR2DL3 , KIR2DL3 , KIR2DL3 , KIR2DL3 , KIR2DL3 , KIR2DL3 , KIR2DL3 , KIR2DL3 , KIR2DL3 , KIR2DL3 , KIR2DL3 , KIR2DL3 , KIR2DL3 , KIR2DL4 , KIR2DL4 , KIR2DL4 , KIR2DL4 , KIR2DL4 , KIR2DL4 , KIR2DL4 , KIR2DL4 , KIR2DL4 , KIR2DL4 , KIR2DL4 , KIR2DL4 , KIR2DL4 , KIR2DL4 , KIR2DL4 , KIR2DL4 , KIR2DL4 , KIR2DL4 , KIR2DL4 , KIR2DL4 , KIR2DL4 , KIR2DL4 , KIR2DL4 , KIR2DL4 , KIR2DL4 , KIR2DL4 , KIR2DL4 , KIR2DL4 , -

Supplementary Table S4. FGA Co-Expressed Gene List in LUAD
Supplementary Table S4. FGA co-expressed gene list in LUAD tumors Symbol R Locus Description FGG 0.919 4q28 fibrinogen gamma chain FGL1 0.635 8p22 fibrinogen-like 1 SLC7A2 0.536 8p22 solute carrier family 7 (cationic amino acid transporter, y+ system), member 2 DUSP4 0.521 8p12-p11 dual specificity phosphatase 4 HAL 0.51 12q22-q24.1histidine ammonia-lyase PDE4D 0.499 5q12 phosphodiesterase 4D, cAMP-specific FURIN 0.497 15q26.1 furin (paired basic amino acid cleaving enzyme) CPS1 0.49 2q35 carbamoyl-phosphate synthase 1, mitochondrial TESC 0.478 12q24.22 tescalcin INHA 0.465 2q35 inhibin, alpha S100P 0.461 4p16 S100 calcium binding protein P VPS37A 0.447 8p22 vacuolar protein sorting 37 homolog A (S. cerevisiae) SLC16A14 0.447 2q36.3 solute carrier family 16, member 14 PPARGC1A 0.443 4p15.1 peroxisome proliferator-activated receptor gamma, coactivator 1 alpha SIK1 0.435 21q22.3 salt-inducible kinase 1 IRS2 0.434 13q34 insulin receptor substrate 2 RND1 0.433 12q12 Rho family GTPase 1 HGD 0.433 3q13.33 homogentisate 1,2-dioxygenase PTP4A1 0.432 6q12 protein tyrosine phosphatase type IVA, member 1 C8orf4 0.428 8p11.2 chromosome 8 open reading frame 4 DDC 0.427 7p12.2 dopa decarboxylase (aromatic L-amino acid decarboxylase) TACC2 0.427 10q26 transforming, acidic coiled-coil containing protein 2 MUC13 0.422 3q21.2 mucin 13, cell surface associated C5 0.412 9q33-q34 complement component 5 NR4A2 0.412 2q22-q23 nuclear receptor subfamily 4, group A, member 2 EYS 0.411 6q12 eyes shut homolog (Drosophila) GPX2 0.406 14q24.1 glutathione peroxidase -

Supplementary Material DNA Methylation in Inflammatory Pathways Modifies the Association Between BMI and Adult-Onset Non- Atopic
Supplementary Material DNA Methylation in Inflammatory Pathways Modifies the Association between BMI and Adult-Onset Non- Atopic Asthma Ayoung Jeong 1,2, Medea Imboden 1,2, Akram Ghantous 3, Alexei Novoloaca 3, Anne-Elie Carsin 4,5,6, Manolis Kogevinas 4,5,6, Christian Schindler 1,2, Gianfranco Lovison 7, Zdenko Herceg 3, Cyrille Cuenin 3, Roel Vermeulen 8, Deborah Jarvis 9, André F. S. Amaral 9, Florian Kronenberg 10, Paolo Vineis 11,12 and Nicole Probst-Hensch 1,2,* 1 Swiss Tropical and Public Health Institute, 4051 Basel, Switzerland; [email protected] (A.J.); [email protected] (M.I.); [email protected] (C.S.) 2 Department of Public Health, University of Basel, 4001 Basel, Switzerland 3 International Agency for Research on Cancer, 69372 Lyon, France; [email protected] (A.G.); [email protected] (A.N.); [email protected] (Z.H.); [email protected] (C.C.) 4 ISGlobal, Barcelona Institute for Global Health, 08003 Barcelona, Spain; [email protected] (A.-E.C.); [email protected] (M.K.) 5 Universitat Pompeu Fabra (UPF), 08002 Barcelona, Spain 6 CIBER Epidemiología y Salud Pública (CIBERESP), 08005 Barcelona, Spain 7 Department of Economics, Business and Statistics, University of Palermo, 90128 Palermo, Italy; [email protected] 8 Environmental Epidemiology Division, Utrecht University, Institute for Risk Assessment Sciences, 3584CM Utrecht, Netherlands; [email protected] 9 Population Health and Occupational Disease, National Heart and Lung Institute, Imperial College, SW3 6LR London, UK; [email protected] (D.J.); [email protected] (A.F.S.A.) 10 Division of Genetic Epidemiology, Medical University of Innsbruck, 6020 Innsbruck, Austria; [email protected] 11 MRC-PHE Centre for Environment and Health, School of Public Health, Imperial College London, W2 1PG London, UK; [email protected] 12 Italian Institute for Genomic Medicine (IIGM), 10126 Turin, Italy * Correspondence: [email protected]; Tel.: +41-61-284-8378 Int. -

Whole Exome Sequencing in Families at High Risk for Hodgkin Lymphoma: Identification of a Predisposing Mutation in the KDR Gene
Hodgkin Lymphoma SUPPLEMENTARY APPENDIX Whole exome sequencing in families at high risk for Hodgkin lymphoma: identification of a predisposing mutation in the KDR gene Melissa Rotunno, 1 Mary L. McMaster, 1 Joseph Boland, 2 Sara Bass, 2 Xijun Zhang, 2 Laurie Burdett, 2 Belynda Hicks, 2 Sarangan Ravichandran, 3 Brian T. Luke, 3 Meredith Yeager, 2 Laura Fontaine, 4 Paula L. Hyland, 1 Alisa M. Goldstein, 1 NCI DCEG Cancer Sequencing Working Group, NCI DCEG Cancer Genomics Research Laboratory, Stephen J. Chanock, 5 Neil E. Caporaso, 1 Margaret A. Tucker, 6 and Lynn R. Goldin 1 1Genetic Epidemiology Branch, Division of Cancer Epidemiology and Genetics, National Cancer Institute, NIH, Bethesda, MD; 2Cancer Genomics Research Laboratory, Division of Cancer Epidemiology and Genetics, National Cancer Institute, NIH, Bethesda, MD; 3Ad - vanced Biomedical Computing Center, Leidos Biomedical Research Inc.; Frederick National Laboratory for Cancer Research, Frederick, MD; 4Westat, Inc., Rockville MD; 5Division of Cancer Epidemiology and Genetics, National Cancer Institute, NIH, Bethesda, MD; and 6Human Genetics Program, Division of Cancer Epidemiology and Genetics, National Cancer Institute, NIH, Bethesda, MD, USA ©2016 Ferrata Storti Foundation. This is an open-access paper. doi:10.3324/haematol.2015.135475 Received: August 19, 2015. Accepted: January 7, 2016. Pre-published: June 13, 2016. Correspondence: [email protected] Supplemental Author Information: NCI DCEG Cancer Sequencing Working Group: Mark H. Greene, Allan Hildesheim, Nan Hu, Maria Theresa Landi, Jennifer Loud, Phuong Mai, Lisa Mirabello, Lindsay Morton, Dilys Parry, Anand Pathak, Douglas R. Stewart, Philip R. Taylor, Geoffrey S. Tobias, Xiaohong R. Yang, Guoqin Yu NCI DCEG Cancer Genomics Research Laboratory: Salma Chowdhury, Michael Cullen, Casey Dagnall, Herbert Higson, Amy A. -

(Lilrs) on Human Neutrophils: Modulators of Infection and Immunity
MINI REVIEW published: 13 May 2020 doi: 10.3389/fimmu.2020.00857 Leukocyte Immunoglobulin-Like Receptors (LILRs) on Human Neutrophils: Modulators of Infection and Immunity Alexander L. Lewis Marffy and Alex J. McCarthy* MRC Centre for Molecular Bacteriology and Infection, Imperial College London, London, United Kingdom Neutrophils have a crucial role in defense against microbes. Immune receptors allow neutrophils to sense their environment, with many receptors functioning to recognize signs of infection and to promote antimicrobial effector functions. However, the neutrophil Edited by: Nicole Thielens, response must be tightly regulated to prevent excessive inflammation and tissue damage, UMR5075 Institut de Biologie and regulation is achieved by expression of inhibitory receptors that can raise activation Structurale (IBS), France thresholds. The leukocyte immunoglobulin-like receptor (LILR) family contain activating Reviewed by: and inhibitory members that can up- or down-regulate immune cell activity. New ligands Debby Burshtyn, University of Alberta, Canada and functions for LILR continue to emerge. Understanding the role of LILR in neutrophil Tamás Laskay, biology is of general interest as they can activate and suppress antimicrobial responses University of Lübeck, Germany of neutrophils and because several human pathogens exploit these receptors for immune *Correspondence: Alex J. McCarthy evasion. This review focuses on the role of LILR in neutrophil biology. We focus on the [email protected] current knowledge of LILR expression -

LILRA3): a Novel Marker for Lymphoma Development Among Patients with Young Onset Sjogren’S Syndrome
Journal of Clinical Medicine Article Leukocyte Immunoglobulin-Like Receptor A3 (LILRA3): A Novel Marker for Lymphoma Development among Patients with Young Onset Sjogren’s Syndrome Evangelia Argyriou 1,2,† , Adrianos Nezos 1,†, Petros Roussos 1, Aliki Venetsanopoulou 3 , Michael Voulgarelis 3, Kyriaki Boki 2, Athanasios G. Tzioufas 3,4, Haralampos M. Moutsopoulos 5 and Clio P. Mavragani 1,3,4,* 1 Department of Physiology, Medical School, National and Kapodistrian University of Athens, 11527 Athens, Greece; [email protected] (E.A.); [email protected] (A.N.); [email protected] (P.R.) 2 Rheumatology Unit, Sismanogleio General Hospital, 15126 Athens, Greece; [email protected] 3 Department of Pathophysiology, Medical School, National and Kapodistrian University of Athens, 11527 Athens, Greece; [email protected] (A.V.); [email protected] (M.V.); [email protected] (A.G.T.) 4 Joint Academic Rheumatology Program, School of Medicine, National and Kapodistrian University of Athens, 11527 Athens, Greece 5 Athens Academy, Chair Medical Sciences/Immunology, 10679 Athens, Greece; [email protected] * Correspondence: [email protected]; Tel.: +30-210-746-2714 † Equally contributed. Abstract: Background: Primary Sjogren’s syndrome (SS) is an autoimmune disease with a strong predilection for lymphoma development, with earlier disease onset being postulated as an independent Citation: Argyriou, E.; Nezos, A.; risk factor for this complication. Variations of the Leukocyte immunoglobulin-like receptor A3 (LILRA3) gene Roussos, P.; Venetsanopoulou, A.; have been previously shown to increase susceptibility for both SS and non-Hodgkin B-cell lymphoma Voulgarelis, M.; Boki, K.; Tzioufas, A.G.; Moutsopoulos, H.M.; (B-NHL) in the general population. -
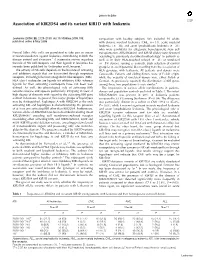

Association of KIR2DS4 and Its Variant KIR1D with Leukemia
Letters to the Editor 2129 Association of KIR2DS4 and its variant KIR1D with leukemia Leukemia (2008) 22, 2129–2130; doi:10.1038/leu.2008.108; comparison with healthy subjects. We included 90 adults published online 8 May 2008 with chronic myeloid leukemia (CML, n ¼ 31), acute myeloid leukemia ( n ¼ 38), and acute lymphoblastic leukemia (n ¼ 21) who were candidates for allogeneic hematopoietic stem cell Natural killer (NK) cells are postulated to take part in innate transplantation. KIR2DS4n001 and KIR1D alleles were detected immunosurveillance against leukemia, contributing to both the according to previously described methodology5 in patients as disease control and clearance.1 A systematic review regarding well as in their HLA-matched related (n ¼ 31) or unrelated the role of NK cell receptors and their ligands in leukemia has (n ¼ 59) donors, serving as controls. Such selection of control recently been published by Verheyden and Demanet.1 group let us avoid potential bias resulting from the association of The activity of NK cells depends on the balance of activating HLA genotype with leukemia. All patients and donors were and inhibitory signals that are transmitted through respective Caucasoids. Patients and sibling donors were of Polish origin, receptors, including killer immunoglobulin-like receptors (KIRs). while the majority of unrelated donors were either Polish or HLA class I molecules are ligands for inhibitory KIRs, whereas German. As previously reported, the distribution of KIR genes ligands for their activating counterparts have not been well among these two populations is very similar.6 defined. As well, the physiological role of activating KIRs The frequencies of various allele combinations in patients, remains obscure and appears particularly intriguing in view of donors and population controls are listed in Table 1.